Introduction
Interleukin-1β (IL-1β) is a proinflammatory cytokine implicated in the pathogenesis of ischaemic brain damage. In experimental models of cerebral ischaemia, IL-1β expression is up-regulated and administration of IL-1β intracerebroventricularly or into the brain parenchyma exacerbates ischaemic damage. Conversely, administration of the IL-1 receptor antagonist is neuroprotective 1 . IL-1β expression is also elevated in systemic inflammatory conditions, such as atherosclerosis, and acute infection 2 , which are risk factors for stroke 3 . However, the effects of increased systemic IL-1β levels on ischaemic brain damage have not been studied. The present study determined the effects of peripheral IL-1β administration on outcome after transient focal ischaemia in mice.
Methods
Transient focal ischaemia (30 min) was induced in C57Bl/6J mice (25 – 28 g) by intraluminal filament occlusion. Anaesthesia was induced with 3% halothane in 70% N2O and 30% O2 and maintained with 1.5–2% halothane in the same mixture. A 6-0 nylon monofilament, coated at the tip (2 mm; 180 μm diameter) with “thermo-melting” glue, was positioned to occlude the middle cerebral artery. At the onset of occlusion, mice received an intraperitoneal injection of vehicle (0.5% bovine serum albumin in PBS; n = 5) or recombinant human IL-1β (4 μg/mg; n = 6). The filament was withdrawn after 30 min to allow reperfusion. Neurological deficit 4 was assessed at 4 h and 24 h after occlusion. Brains were removed 24 h after occlusion and frozen in isopentane (−42°C). Coronal sections (20 μm) were cut at 200 μm intervals, stained with cresyl violet and the volume of ischaemic damage measured as described 5 .
Results
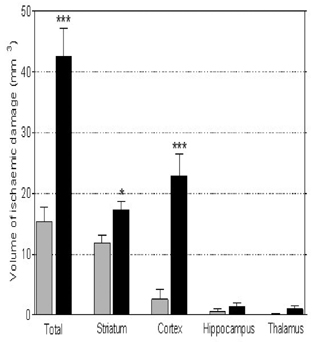
Peripheral IL-1β treatment significantly increased the total volume of ischaemic damage compared to vehicle treatment (43 ± 5 mm3 vs. 15 ± 3 mm3, P < 0.001). IL-1β treatment also significantly increased the volume of ischaemic damage in the striatum (17 ± 1 mm3 vs. 12 ± 1 mm3, P < 0.05) and cerebral cortex (23 ± 3 mm3 vs. 3 ± 2 mm3, P < 0.001). The neurological deficit score was greater at 4 h and 24 h after occlusion in the IL-1β-treated group compared to the vehicle-treated group, although this reached statistical significance only at 24 h (2 ± 0.3 vs. 1 ± 0.2, P < 0.05).
Conclusions
These data show that peripheral IL-1beta administration exacerbates ischaemic brain damage and neurological deficit after transient focal ischaemia and suggest that the systemic inflammatory status may be an important modulator of outcome to ischaemic brain injury. Further characterisation of the peripheral inflammatory response after cerebral ischaemia may reveal novel targets for therapeutic intervention (Figure 1).