Introduction
Pro-inflammatory cytokines such as interleukin-1 (IL-1) have been strongly implicated in the pathogenesis of ischaemic brain damage. After all forms of cerebral ischemia the expression of IL-1 is rapidly up-regulated. Furthermore, exogenous IL-1, given via the intracerebroventricular (icv) route, has been shown to markedly increase ischaemic brain damage. In contrast, the naturally occurring IL-1 receptor antagonist (IL-1ra), which binds to the IL-1R1 and blocks actions of IL-1, has been shown to be effective in reducing lesion volume when given either directly into the brain parenchyma or icv 1 . Clinically, it is not feasible to deliver IL-1ra directly into the brain of patients suffering brain ischemia. However, some clinical studies have shown that peripherally administered IL-1ra does indeed cross the blood brain barrier in patients suffering from subarachnoid haemorrhage, which likely involves cytokines in the pathogenesis of the cerebral ischaemia that develops 2 . To date such studies have been too small to show efficacy and the aim of this study therefore was to examine the efficacy of intravenous IL-1ra on ischaemic brain damage in rodents.
Methods
Experiments were performed on Sprague-Dawley rats (310–380 g). Cerebral ischaemia was induced in anaesthetised rats according to the intraluminal filament occlusion model 3 . Briefly, the right carotid artery and its branches were exposed. A monofilament was advanced until resistance was felt at around 20 mm, to block the origin of the right middle cerebral artery. After 90 minutes, the filament was withdrawn to allow reperfusion. Immediately prior to induction of ischaemia, a bolus of 10 mg of IL-1ra was given via an external jugular cannula and an osmotic minipump (8 ul/hr- to deliver 0.8 mg/h for 24 h) filled with IL-1ra (100 mg/ml) was connected to the tubing. Controls received identical volumes of NaCl (0.9%). After 24 h of IL-1ra infusion, animals were sacrificed. Brains were removed, processed and infarct volumes calculated using an image analysis program, the final volumes being adjusted for oedema. Groups were compared using an unpaired students T-test.
Results
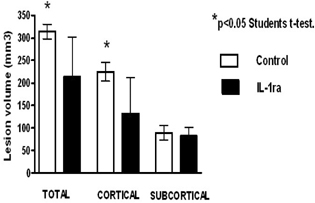
Intravenous delivery of IL-1ra for a period of 24 h after the onset of middle cerebral artery occlusion resulted in a significant decrease in both total (313±9 mm3 vs. 216±92 mm3 p<0.05) and cortical (229±18 mm3 vs. 140±78 mm3 p<0.05) lesion volumes. The subcortical lesion was not affected by IL-1ra treatment (85±17 mm3 vs. 86±22 mm3 p>0.05).
Conclusion
IL-1ra reduces ischaemic damage as measured by lesion volumes after transient MCAO when given intravenously. Further work will determine plasma levels and corresponding CSF levels of IL-1ra required for neuroprotection, in support of pharmacokinetic data in subarachnoid haemorrhage patients. This is further evidence to support the use of IL-1ra in the clinical setting as a neuroprotective agent (See Figure 1).