Introduction
The enhancement of NMDA receptor-mediated glutamatergic neurotransmission has recently gained acceptance as a promising strategy for the treatment of schizophrenia. Because of obvious concerns over excitotoxicity, current research is focused on NMDA receptor activation through modulatory sites rather than the development of glutamate site agonists. In particular, inhibition of glycine reuptake at the GlyT1 transporter has been shown to upregulate NMDA receptor function via the strychnine-insensitive glycine site, but the side effect liability of this approach has not been explored. We therefore investigated the effect of three structurally different GlyT1 inhibitors (R)-NPTS 1 , Org 24461 2 and SSR504734 3 on ischemic infarct development in the rat.
Methods
Focal cerebral ischemia was induced in fasted male Long Evans rats under sevoflurane/nitrous oxide anesthesia by permanent distal ligation of the right middle cerebral artery just above the rhinal fissure. The rats were pretreated with a single intraperitoneal injection of the GlyT1 inhibitor either 30 min ((R)-NPTS and Org 24461) or 60 min (SSR504734) before the onset of ischemia. Twenty-two hours after vessel occlusion the animals were sacrificed and cerebral infarct volume was determined on triphenyltetrazolium chloride-stained serial coronal sections by image analysis. Each treatment group (n = 8 to 11) was compared to its own vehicle-treated controls by unpaired two-tailed t-test. Differences with P < 0.05 were considered statistically significant.
Results
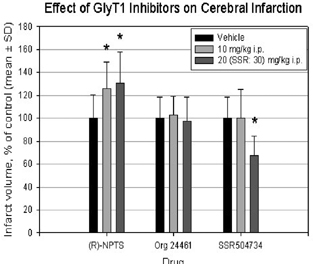
Pretreatment with 10 or 20 mg/kg (R)-NPTS led to an increase in infarct volume by 26% and 31%, respectively, without any noticeable change in the behavior of the animals. The administration of Org 24461 (10 or 20 mg/kg) had no effect on the final extent of ischemic infarction although it resulted in deep and protracted sedation. Preischemic therapy with 30 mg/kg SSR504734 reduced infarct volume by 32% while 10 mg/kg was without effect. The infarct reduction achieved by the higher dose was accompanied only by a small decrease in the volume of edema, indicating genuine neuroprotection afforded by the compound. Treatment was not associated with any obvious behavioral effects.
Conclusion
Although the reasons for the disparate impact of GlyT1 inhibitors on infarct development is unclear at present, the findings nevertheless suggest that the pharmacologically efficacious upregulation of NMDA receptor function via inhibition of the GlyT1 transporter does not necessarily lead to an enhancement of ischemia-induced acute excitotoxic cell death. (See Figure 1).