Introduction
Oestrogen's neuroprotective effect in stroke models has been challenged recently with reports of the hormone exacerbating ischaemic damage1, 2, 3. What controls stroke outcome in the presence of oestrogen remains unclear but may relate to the severity and duration (permanent or transient) of the ischaemic insult. The present work examined the effects of oestrogen on ischaemic damage induced by either transient or maintained (permanent) focal cerebral ischaemia using the intraluminal thread (ILT) model.
Methods
In Study 1, female, ovariectomised Sprague-Dawley rats were pre-treated with a high physiological dose of 17beta-oestradiol (0.25 mg, 21-day release pellet) or placebo 14 days before 24 hours of permanent focal ischaemia using the ILT model. In Study 2, ovariectomised Lister Hooded rats received 14 days of pre-treatment with 17beta-oestradiol (0.25 mg or 0.025 mg) or placebo pellet then underwent transient focal ischaemia by ILT: 2 hours ischaemia and 7 days reperfusion. Infarct volume, cortical blood flow (laser Doppler) and neurological deficits were compared between 17beta-oestradiol and placebo treated groups in each study.
Results
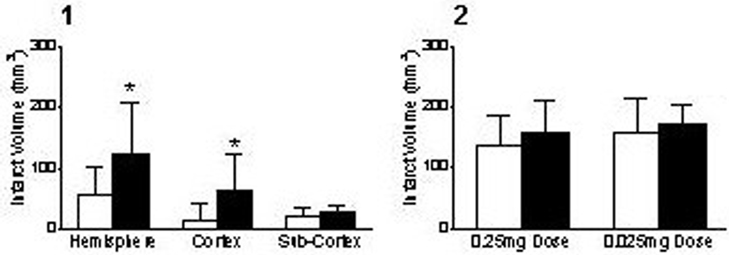
17beta-Oestradiol significantly increased infarct volume by 118% 24 hours after permanent ischaemia (Figure 1(1)) but had no effect on ischaemic blood flow or neurological deficit. Transient ischaemia produced no overall effect at either dose of 17beta-oestradiol on infarct volume (Figure 1(2)), blood flow or neurological deficit.
Conclusion
Oestrogen can induce detrimental effects on the ischaemic brain as displayed in Study 1. Most studies reporting neuroprotective effects of oestrogen involve models of transient ischaemia. The lack of effect of oestradiol in Study 2 may be due to detrimental effects of oestrogen (evident in the permanent ischaemia model), counteracting any beneficial effects during reperfusion, resulting in no overall influence of oestrogen on stroke outcome. The results of Study 1 clearly demonstrate that oestrogen has the capacity to promote detrimental actions in the stroke-injured brain. In line with recent large clinical trials (e.g. Womens Health Initiative), our studies reveal a detrimental influence of oestrogen on stroke and indicate the need for further research on more selective oestrogen receptor agonists and selective oestrogen receptor modulators (SERMs).
Footnotes
Acknowledgements
The authors thank Prof. DI Graham, Dr. E Irving and J McGill for their expertise. KG is supported by a Research into Ageing PhD studentship.
