Abstract
Introduction
We aim to provide better insights into the demographic, epidemiological, and seasonal characteristics of scorpion envenomation reported in the Rio Doce Valley, Brazil.
Methods
We conducted this monocentric retrospective descriptive study with data on Investigation Forms of Accidents by Venomous Animals, only envenoming cases of scorpion stings, between January 1, 2017 and December 31, 2020, belonging to the compulsory notification system of the Municipal Hospital of Governador Valadares.
Results
There were 3032 accidents, and the male-to-female ratio was 1.17:1 (male, 54%; females, 46%). Accidents occurred every month, but there was an increase in June, July, and October to January. In most cases, the time between the scorpion sting and medical care was between 1 and 3 h (n=1304; 43%). The most frequent clinical and systemic manifestations were pain at the bite site (94%) and vagal symptoms (7%). Cases were mild (n=2750, 91%), moderate (n=221, 7%), and severe (n=56, 2%). Children younger than 10 y constituted the most cases, 522 (17%). There was a significant difference between clinical severity and age (P<0.01). Ten patients developed acute pulmonary edema. Two 4-y-old children died. All severely envenomated patients as well as 74% and 2% of mild and moderately envenomated patients, respectively, received specific scorpion antivenoms.
Conclusions
Scorpion envenomation is of greater severity in children aged <10 y. The clinical presentation includes mainly local pain associated with vagal symptoms. Accidents occur every month, but there was an increase in June, July, and October to January.
Introduction
Globally, scorpion stings are one of the most important types of potential envenomation. Annually, an estimated 1.5 million people are victims of scorpion stings worldwide, and approximately 2.3 billion people live in regions that carry an increased risk of scorpion sting.1,2 The Brazilian scorpion fauna is diverse, but the most medically important and widely geographically distributed genus is Tityus.1,3 Especially in the state of Minas Gerais, there are registered cases of scorpion envenomation involving T serrulatus, T bahiensis, T trivittatus, T mattogrossensis, T confluens, and T costatus. 3
T serrulatus venom can cause local and systemic symptoms from immediate pain at the bite site to vomiting, sweating, hypersalivation, psychomotor agitation, cardiac arrhythmias, hypertension, pulmonary edema, and circulatory failure, sometimes leading to death. 4 -7 Tityus species cause the most severe and lethal human envenomation in Brazil 3 and, consequently, impact public health.3,8,9 T serrulatus is the species of greatest medical importance due to its dangerous potential to cause severe envenomation, 10 mostly in children. 11 Studied Tityus venoms commonly contain sodium-channel toxins and potassium-channel toxins, which cause clinical effects resulting from excitation of sympathetic and parasympathetic nervous system, causing systemic symptoms.4,12-14 In addition, in some cases, the envenoming involving Tityus species can cause severe muscle spasms frequently refractory to the serum treatment. 15
In Brazil, according to the Ministry of Health, 16 the clinical manifestations are classified as mild (local manifestations), moderate (local pain, cholinergic/adrenergic symptoms), or severe (including moderate symptoms plus heart failure, pulmonary edema, and shock). This classification is similar to the Scorpion Consensus Expert Group classes, which include 4 classes: local manifestations, minor systemic manifestations, major systemic manifestations, and lethal envenomation. 6 Antivenom is indicated when the envenomation is classified as moderate or severe, showing systemic manifestations, especially when the accident is caused by T serrulatus. 16 The Instituto Butantan (São Paulo, Brazil), produces anti–T serrulatus antivenom that is used in the Hospital Municipal of Governador Valadares, where this study was conducted. The antiscorpion serum is the first-line treatment in these cases, while the antiarachnid antivenom (also produced by Instituto Butantan; prepared against venoms of Loxosceles, Phoneutria, and Tityus) is used when the former is unavailable. 17
Minas Gerais is the Brazilian state with the highest number of scorpion accidents. 3 There were approximately 28,191 in 2017, and in 2020, they exceeded 35,000 accidents. 3 Therefore, in this descriptive study, we aim to provide better insights into the demographic, epidemiological, and seasonal characteristics of scorpion envenomation reported in a public hospital located in a city in the Rio Doce Valley, eastern Minas Gerais.
Methods
Study Design
We conducted this monocentric retrospective descriptive study with data on Investigation Forms of Accidents by Venomous Animals between January 1, 2017 and December 31, 2020, belonging to the compulsory notification system of the Municipal Hospital of Governador Valadares (MHGV), which is analyzed and filed at the Epidemiological Surveillance Department. Those data were reported in the mandatory, non-nominal secondary database public domain Notifiable Diseases Information System (SINAN) of the Ministry of Health of Brazil. The Epidemiological Surveillance Department of Governador Valadares provided the data from SINAN for this study. The MHGV is located in the most populous city in the macroregion of Rio Doce Valley. It is one of the reference medical centers with availability of scorpion antivenom. This hospital receives a large volume of patients daily from different cities in the Rio Doce Valley, which comprises 102 municipalities and a population of more than 1.7 million inhabitants.18,19
All reports of scorpion sting accidents treated at the MHGV from municipalities in the Rio Doce Valley were included. We excluded notifications of scorpion stings from cities belonging to other regions.
Scorpion Sting Data
Demographic, epidemiological, and clinical data from patients were analyzed, such as place of occurrence, age, gender, sting site, the elapsed time between the accident and medical care, specific clinical classification (mild, moderate, or severe), presence of local and systemic signs and symptoms, treatment administered, local and systemic complications, and outcome (cure or death). The severity of envenomation was assessed according to the classification of the Ministry of Health
16
since in the SINAN database, the classification of cases was made according to this ministry as follows: Mild: local pain, edema, hyperemia, or paresthesia. Moderate: local pain and systemic manifestations, including vomiting, agitation, prostration or malaise, sudoresis, tachypnea, tachycardia, and mild arterial hypertension. Severe: including moderate symptoms plus heart failure, pulmonary edema, and shock.
In the SINAN investigation form for venomous animals, it is necessary to identify the type of accident, whether snake, spider, scorpion, caterpillar, bee, other, or unknown, but it is not necessary to specify the species. All sheets provided to us were marked with option 3—scorpion. The MHGV reported that images of scorpions or sighted specimens presented by patients are generally not registered, even when they occur, as they are not part of the compulsory notification form at SINAN, with the largest number of notifications being made through the medical records of the professionals who attended to the patient.
Antivenom
Scorpion antivenom is used for scorpion stings. However, we found other antivenoms that were used for this purpose, such as antiarachnidic antivenom (Loxosceles, Phoneutria, and Tityus), antielapidic serum (Micrurus frontalis and Micrurus corallines), and combinations of bothropic-crotalic antivenom (Bothrops sp and Crotalus durissus ssp), and all of them were manufactured by Instituto Butantan. According to the Manual of Diagnosis and Treatment of Accidents by Venomous Animals of the Department of Epidemiological Surveillance (Ministry of Health, Brazil), antiarachnidic serum can be administered to patients with moderate and severe forms of scorpionism. However, there is no mention of another type of antivenom that can be used in cases of scorpion stings. This manual recommends that antielapidic serum and antibothropic-crotalic serum combinations be administered in cases of accidents with snakes of the Elapidae family, genus Micrurus, and family Viperidae, genera Bothrops and Crotalus, respectively.
Statistical and Geographical Analysis
We performed statistical analysis using the R software (R Core Team and the R Foundation, Vienna, Austria) 20 through descriptive statistics, presented as absolute and relative frequencies. The correlation coefficient was used to verify the relationship between the population size of each city and the respective number of stings. The Fisher exact test was also used to compare groups of patients aged <10 y and >9 y. The significance level was set at P<0.05. GeoDa was used to build the maps to present the spatial distribution of the incidence of scorpionism.
Ethics Statement
The data are from a non-nominal secondary database in the public domain, made available by the Ministry of Health through SINAN, provided by the Department of Health Surveillance of the Municipal Health Department of Governador Valadares, through the Epidemiology Department. According to National Health Council Resolution 510/2016, 21 research that uses publicly accessible information, under the terms of Law No. 12,527, of November 18, 2011, 22 will not be evaluated by the Research Ethics Committee/National Research Ethics Committee system.
Results
Three thousand thirty-two cases of scorpion stings reported in the hospital were included in the present study. The lowest number of reported cases (n=683) was reported in 2017, and the highest number of reported cases (n=844) in 2019.
The male-to-female ratio of patients was 1.17:1 (1634 males or 54% and 1398 females or 46%). The mean age was 35 to 37 y, with a median of 33 years (quartile [Q] 1=15 y; Q3=54 y). Stratification by age showed that children younger than 10 y constituted the most cases, 522 (17%), and in 88 cases, patients were older than 80 y (3%). Most of the scorpion stings affected hands/arms (64%), followed by stings in legs (25%), thorax (7%), head (2%), and neck (1%). The anatomical regions most affected by stings were the upper limbs, especially the fingers (n=727, 24%). However, the lower limbs also received a large number of stings, with the foot being the most affected anatomical region (Table 1).
Clinical and epidemiological characteristics of scorpion envenomation in Rio Doce Valley, Minas Gerais, Brazil
We found that the municipalities with the highest incidence per 100,000 inhabitants of scorpion accidents were, in order of incidence from 2017 to 2020, as follows: Alpercata with 269, 297, 512, and 403 stings; Engenheiro Caldas with 346, 389, 485, and 214 stings; and Capitão Andrade with 355, 258, 421, and 145 stings (Figure 1). Among the 3 cities, Engenheiro Caldas is located farthest (46.4 km) from the municipality of Governador Valadares. All of them have a tropical climate and economic activity with a predominance of agriculture, livestock, and retail minimarkets. The incidence was less than 486 accidents per 100,000 inhabitants per year in all cities, with the exception of Alpercata, which had an incidence of 512 in 2019. The correlation between the number of scorpion stings per city and population size was not significant (P>0.05, 2017–20). There were 84 (82%), 83 (81%), 85 (83%), and 87 (85%) cities with fewer than 50 cases as well as 5 (5%), 6 (6%), 7 (7%), and 5 (5%) cities with more than 200 cases per year, respectively, that had scorpion stings treated at the MHGV (Figure 1). Cities with more than 200 scorpion stings per year belong to the microregion of Governor Valadares or Ipatinga.
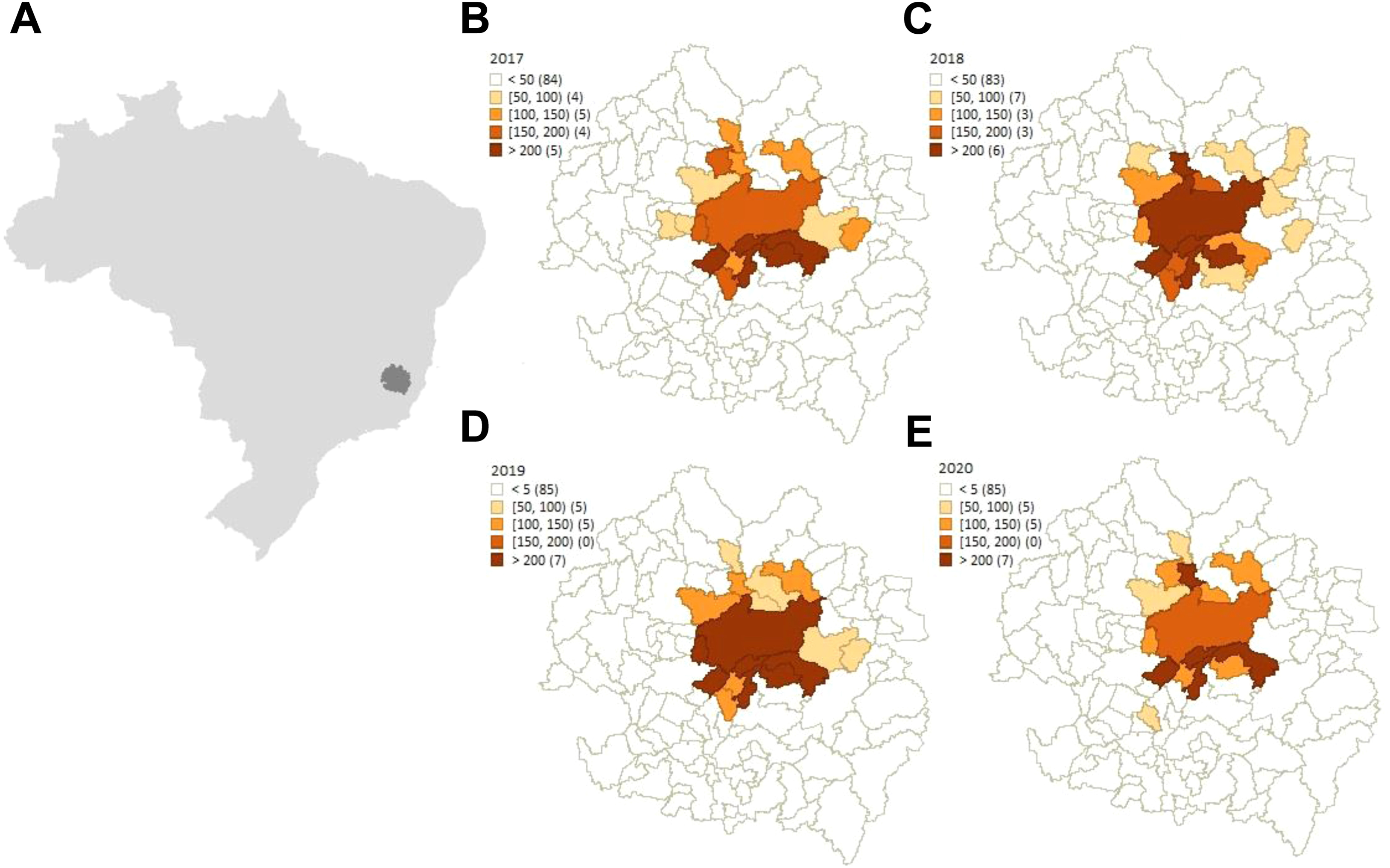
Spatial distribution map of scorpion sting in the Rio Doce Valley. A, Map of Brazil (pale gray) and Rio Doce Valley (gray). B to E, Incidence of scorpionism in the years 2017 to 2020, respectively, in the Rio Doce Valley.
Scorpion stings occurred during all months of the year, but July had the highest monthly frequency of recorded cases, followed by June and October to January (Figure 2). Fifty percent of severe cases occurred in these months. In a 6-mo interval, there was an oscillation in the number of scorpion stings, and in most years, except 2020, January had high incidence peaks.
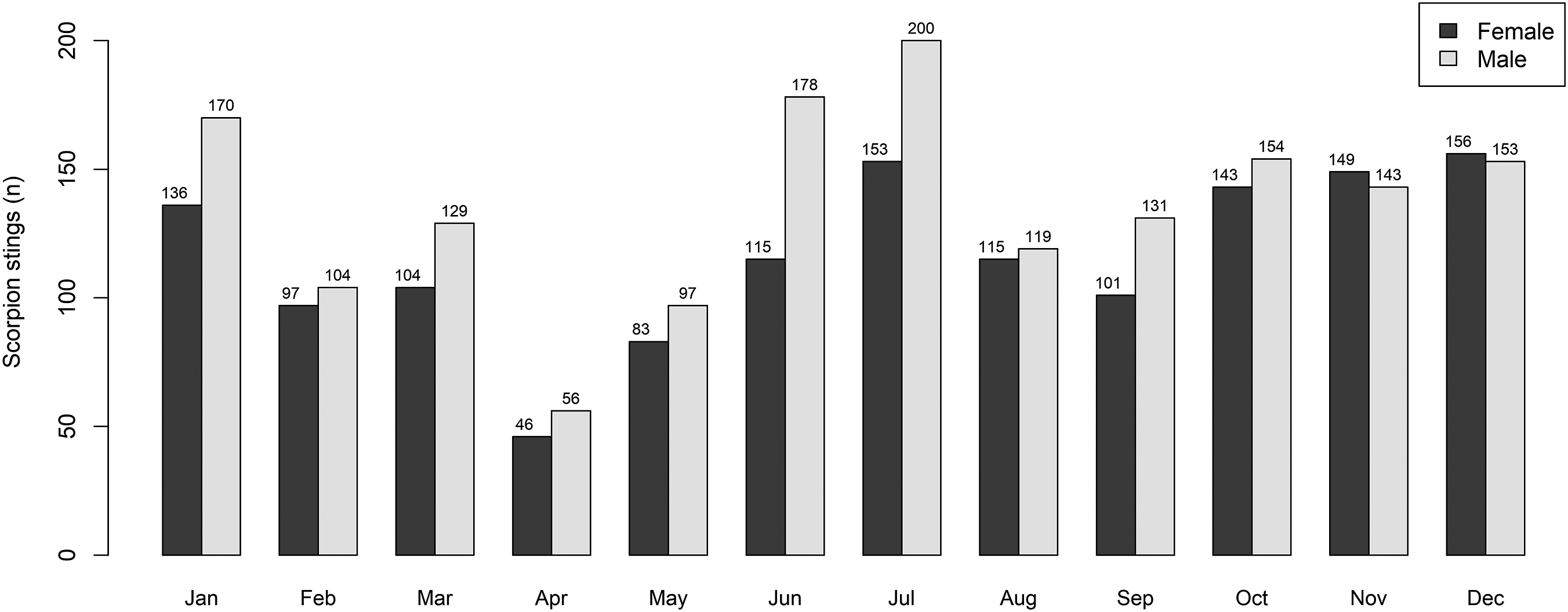
The monthly number of recorded scorpion sting cases in Rio Doce Valley in the period 2017 to 2020.
In most cases, the time elapsed between the scorpion sting and medical care was between 1 and 3 h (n=1304; 43%), followed by up to 1 h after the sting (n=1106; 36%) and between 3 and 6 h (n=287; 10%). In 165 cases (5%), the time elapsed between the accident and medical care was unknown (Table 1). In this study, the database did not provide the time of the stings.
The relative frequency of symptoms presented is shown in Table 2. The most common symptoms presented included local pain (94%), local edema (13%), vomiting and diarrhea (7%), paresthesia (2%), numbness (2%), blurred vision (1%), nausea (1%), sweating (1%), headache (1%), erythema, high blood pressure, and myalgia or anemia (<1%); oliguria/anuria was rarely present. Eleven patients had systemic complications, of whom 10 developed acute pulmonary edema; of these, 4 patients developed pulmonary edema and shock. Among the victims who had pulmonary edema or pulmonary edema and shock, 2 died.
Local and systemic clinical manifestations of scorpionism in the Rio Doce Valley
Cases were classified as mild (91%), moderate (7%), and severe (2%). The hospital length of stay of severely envenomed patients was between 0 and 205 d (the records did not include the clinical basis for the prolonged 205-d inpatient period). The average number of severe cases was 9.16 d, with a median of 6 d (Q1=3 d; Q3=13 d) (Table 1). Two deaths occurred in 4-y-old children 24 h after hospital care. One of these children was stung in the torso and the other was stung in the toe. Both had pain at the bite site, while the other also had numbness and swelling. Both had vomiting and diarrhea, and one reportedly was agitated. They developed pulmonary edema, and one had shock. Children aged <10 y constituted 520 of cases and 44 had severe symptoms of scorpionism, while 2507 patients were aged ≥10 y and 12 had severe symptoms (Table 3). The Fischer exact test showed a significant difference between these groups (P<0.01).
Number of cases in the different classes of envenoming in groups of up to 9 y old and over 9 y old
Patients with severe envenoming as well as 164 patients (74%) with moderate cases and 67 patients (2%) with mild cases received specific scorpion antivenom. The scorpion antivenom consisted of an injectable solution of the F (ab`)2 fraction of specific and purified heterologous immunoglobulins. Each mL of serum neutralizes at least 1.0 mg of T serrulatus venom, totaling at least 5.0 mg of venom per 5-mL ampoule. 23 In total, 187 ampoules were used in mild cases, 494 in moderate cases, and 256 in severe cases. However, in 9 cases, the number of ampoules was not specified, and in 2 unknown cases, 2 ampoules were used (Table 1). The average use of ampoules in mild cases was 2.8 (median, 3), in moderate cases 3 (median, 3) and in severe cases 5.5 (median, 6). In Brazil, the Ministry of Health recommends serum only for moderate (2–3 ampoules) and severe (4–6 ampoules) cases, but 34 people received more than 3 ampoules in moderate cases and 27 people received more than 6 ampoules in severe cases. 16 In addition, we identified 27 cases in which antiarachnid serum was used. Bothropic antivenom was incorrectly used in 2 cases, as were antielapidic antivenom and bothropic-crotalic antivenom.
Aside from antivenom, the database did not indicate any other treatment that was provided to the envenomated patients. The Ministry of Health 16 recommends that symptomatic treatment must consist of pain relief and that electrolyte imbalance and acid-base disorders must be treated according to appropriate measures in each case. Patients with systemic manifestations, especially children (moderate and severe cases), should be kept under continuous observation of vital functions, aiming at early diagnosis and treatment of complications.
Discussion
In this study, we evaluated all envenoming cases of local scorpionism that occurred over the 4-y period from 2017 to 2020 treated in the MHGV from cities of the Rio Doce Valley. There was an increase in the number of accidents. T serrulatus is distributed throughout this region. 3
Stratification of scorpion sting victims by gender showed a predominance of males, while stratification by age revealed that children are more affected than adults. We hypothesize that in 2020, due to the COVID 19 pandemic, children remained in or near their homes for long periods of time. In backyards, it is possible for children to play with dry leaves, tree trunks, and rubble, and scorpions hide in these places. A monocentric retrospective study in French Guiana demonstrated that pediatric scorpionism is closely associated with child activities and climatic conditions. 24 They suggest specific periods when most of the stings occur and that in these periods, children are stung because they are not aware or do not pay attention to the presence of the scorpion. 24
Among the Brazilian regions and states, there are differences in the periods with the highest occurrence of accidents. 25 In this study, we found that although accidents occur every month of the year, there is an increase in warmer and rainy months (October to January) and in the dry months (June and July). We think this increase during warmer and rainy months probably occurs because the precipitation inundates the burrows where scorpions live, forcing them to look for new refuges, 26 while in the dry months, it may be related to agricultural activities and school holidays, as many children help their parents with agricultural activities during this period. Another possible explanation may be favorable local environmental conditions throughout the year and in different months, including food in abundance and ideal temperatures for scorpions. 27 In addition, a recent study using data on the occurrence of the species and climatic variables predicted that climate change, with its steady increase in global warming, should have a significant impact on the patterns of distribution of Tityus species that will clearly extend to more southern latitudes. 28
The majority of cases were mild, in agreement with the results of other South American studies. 29 -32 Most of the individuals were admitted to the hospital within 3 h for medical care (77%), suggesting no significant association between patient delay and clinical severity. This differs from the findings of studies in Minas Gerais and Mexico.26,33 In severe cases, the number of patients attended between 0 to 1 and 1 to 3 h was the same (46% each). Among the severe cases, 2 deaths occurred in 4-y-olds, in line with a study carried out in the state of Bahia, in which 70% of deaths occurred in children aged 1 to 9 y. 29 In scorpion accidents, a higher risk of death is associated with young age and occurs in children up to 14 y of age with severe cases of scorpion sting, as the inoculation of the venom tends to cause more severe effects in a victim with lower body weight/volume. 31 Our study showed that the highest number of accidents reported involved patients aged 0 to 9 y, unlike some other Brazilian studies in which the age group with the highest occurrence of accidents was between 20 and 40 y.34,35 In agreement with Chowell et al 26 (2006) and De Roodt et al 36 (2003), we found a significant association between clinical severity and age, whereby the 0- to 9-y age group presented a higher proportion of cases in clinical severity when compared with those aged >9 y and elderly. Guerra et al 33 (2008) found that scorpion accidents in children and adolescents in the period from 2001 to 2005 in the state of Minas Gerais occurred predominantly with children aged between 5 and 9 y.
Mild envenomation does not require antivenom administration, but we found that 56 mildly envenomed patients received it. The use of antivenom therapy in mild cases may introduce unnecessary risks and expenses for patients and institutions. 33 Moreover, a randomized trial study carried out by Aksel et al 37 showed that to treat scorpion stings associated with pain in patients with no systemic signs and symptoms, topical lidocaine is safe and its effects last several hours after envenomation.
Treatment of scorpion envenomation has 2 components: antivenom administration and supportive care. 38 In 26% of moderate cases, no antivenom was used, and in some patients with severe or moderate symptoms, the number of ampoules was higher than that recommended by the Ministry of Health. This finding suggests that there is a need to review regional criteria in current antivenom therapy schemes. From January 1984 to May 1994, Bucaretchi et al39,40 studied 239 children aged <15 y stung by Tityus spp who presented with severe envenoming. All of them received IV scorpion antivenom. The frequency of early reactions to antivenom was much lower when compared with that in children aged 2 to 14 y who were victims of snake bites and received pretreatment with histamine antagonists H1 and H2 and hydrocortisone before antivenoms. A systematic review of all controlled clinical trials related to scorpion sting management conducted by Rodrigo and Gnanathasan 41 concluded that antivenoms against Centruroides spp are effective in reversing the clinical syndrome of scorpionism faster than without antivenom treatment in children. In addition, antivenom against the Indian red scorpion, Hottentotta tamulus, and prazosin in combination is better than prazosin alone for faster resolution of symptoms.
On the other hand, the administration of dexamethasone is controversial. Reis et al 42 (2020) encourage the use of dexamethasone in situations in which delayed antivenom treatment increases the risk of death. Unlike the results of other studies, corticosteroids have not shown any benefit in the management of scorpion stings. 42 -44
Limitations
The present study has several limitations. This is a retrospective study and may suffer from incomplete or inconsistent information. In addition, this is a local study carried out with data from a single center and lack of information about treatment in medical records. The species of scorpion was not identified, although T serrulatus causes most accidents in Minas Gerais. There were no specific data about whether scorpions or images of scorpions were visualized by medical staff.
Conclusion
The data indicate that severe scorpion envenomation in the Rio Doce Valley (Minas Gerais) is more likely to affect children younger than 10 y. The clinical presentation includes local pain associated with vagal symptoms. Systemic complications consist of respiratory failure/acute pulmonary edema and shock. Accidents occur every month, but there was an increase in June, July, and October to January. The unnecessary administration of scorpion antivenom in mildly envenomed patients is of considerable concern and reinforces the need for review of the regional criteria for antivenom therapy. Antivenom for mildly envenomed patients is not recommended. It is also inappropriate and wholly ineffective to use antivenoms against snake venoms in the case of a scorpion sting. An educational campaign can be valuable in order to inform the public about the potential dangers of scorpion stings and the importance of receiving prompt attention after a scorpion sting.
Footnotes
Acknowledgment
This research would not be possible without the data provided by the surveillance department of Governador Valadares.
Author Contributions: data collection (RCO, LDS); analysis and interpretation of data (LRdM, IMdM); drafting of manuscript (IMdM); review of manuscript (RCO, LDS, LRdM, IMdM); approval of final manuscript (RCO, LDS, LRdM, IMdM).
Financial/Material Support: None.
Disclosures: None
