Abstract
Objective
Scorpion stings are registered worldwide, but the incidence and the features of the envenomations vary depending on the region. The aim of this review was to summarize the epidemiological, clinical, diagnostic, and therapeutic data worldwide regarding humans stung by scorpions.
Methods
A systematic review of the literature was conducted through the online databases of the Virtual Health Library (VHL), which hosts Medline and the Latin American and Caribbean Center on Health Sciences Informational (LILACS) database. We selected articles published between January 1, 2002 and July 31, 2014.
Results
Scorpion envenomation reports were found throughout the world, mainly in subtropical and tropical regions. The clinical manifestations were sympathetically and parasympathetically mediated, depending on the species of scorpion. Some of the most common severe complications of scorpionism included respiratory distress syndrome, pulmonary edema, cardiac dysfunction, impaired hemostasis, pancreatitis, and multiple organ failure. Scorpion envenomation could be classified as mild, moderate, and severe, and the therapeutic approach was based on the case severity. The treatment comprised 3 components: symptomatic measures, vital functions support, and injection of antivenom. Moreover, the time that elapsed between the sting and administration of the appropriate medical care was extremely important to the patient’s prognosis.
Conclusions
The large number of scorpion stings worldwide is concerning and reaffirms the need for new prevention measures and policies to reduce the incidence, prevalence, morbidity, and mortality rates from these poisonous arachnids.
Introduction
Scorpion envenomation, or scorpionism, remains a serious health problem worldwide. 1 Although scorpion stings occur on all continents (except Antarctica), the epidemiology of scorpionism is still poorly known.2,3
Accidents seem to be more common in some world areas, and there is considerable geographical variation, either in incidence or severity.2,3 Scorpionism is relevant in at least 7 limited areas of the world. The incidence and severity of envenomation are higher in the northern Sahara; the southern and eastern regions of Africa; the Middle East; south India; Mexico; Brazil; and the Amazonian basin area (Guyanas, Venezuela, and northern Brazil). 3
Scorpion envenomation is a life-threatening emergency and can cause serious health problems, such as cardiac dysfunction and respiratory failure, in tropical and subtropical regions. 4 Despite the global occurrence and the hazard of scorpionism, epidemiological data are still limited due to unreported cases and few studies regarding this issue.3,4
Accordingly, the aim of this review was to summarize the epidemiological, clinical, diagnostic, and therapeutic data regarding humans stung by scorpions around the world. Our hypothesis is that the clinical manifestations are not widely known or clearly specified and that there are many variations in therapeutic management, therefore requiring a better systemic analysis.
Methods
A systematic review of articles on incidents involving scorpion stings in humans, published in the electronic databases previously referred to, was performed. This study followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement. Our search was conducted through the online literature available on the Virtual Health Library (VHL) database, which hosts Medline and the Latin American and Caribbean Center on Health Sciences Informational (LILACS) database, taking into account articles published between January 1, 2002 and July 31, 2014. This time frame was chosen because the articles published in this period were more expressive and relevant to our research than those published earlier. Also, these articles addressed the incidents involving scorpions and humans more directly.
For the search on the VHL, the following descriptors were used in English, from Medical Subject Headings (MeSH): 1) “Scorpions”; 2) “Prevalence”; and 3) “Public Health.”
The search strategy used on VHL was 1 AND 2 OR 3. In addition, the search was conducted by combining the filters “title, abstract, subject.” This strategy was performed by 3 independent researchers, and disagreements were resolved by the senior researcher.
Data compilation took place between September and October 2014. The following inclusion criteria were adopted: 1) publications written in English, Spanish, or Portuguese; 2) studies regarding incidents in humans involving scorpions; 3) studies about epidemiology, signs and symptoms, diagnosis, and/or therapeutics of incidents involving scorpions; 4) original articles fully accessible through the portal of electronic journals of the Coordination for the Improvement of Higher Education Personnel (CAPES), a virtual library connected to the Brazilian Ministry of Education with content restricted to authorized users; and 5) prospective or retrospective observational studies (descriptive or analytical). The exclusion criteria were other study designs (eg, case reports, literature reviews, comments, and nonoriginal studies, including editorials, reviews, forewords, short or brief communications, and letters to the editor).
Although the inclusion of articles published in English would have been considered adequate to ensure a reliable sampling of studies, Spanish and Portuguese articles were also included in the study.
Each article was read in its entirety. We then compared the findings and divided the results obtained into 4 main categories: epidemiological aspects, clinical aspects, diagnostics, and therapeutics.
The geographic map was constructed using the QGIS software, version 2.12, released on October 23, 2015. QGIS is an open source geographic information system licensed under the GNU General Public License. QGIS is an official project of the Open Source Geospatial Foundation.
Results
Initially, the aforementioned search strategies identified 109 references. After analysis of the articles retrieved based on the eligibility criteria adopted, 87 articles were excluded and 22 were analyzed further and then included in the final sample (Figure 1). Articles from Medline and the LILACS database matched the inclusion criteria of the present study. These criteria were established to diminish the risk of analysis bias.
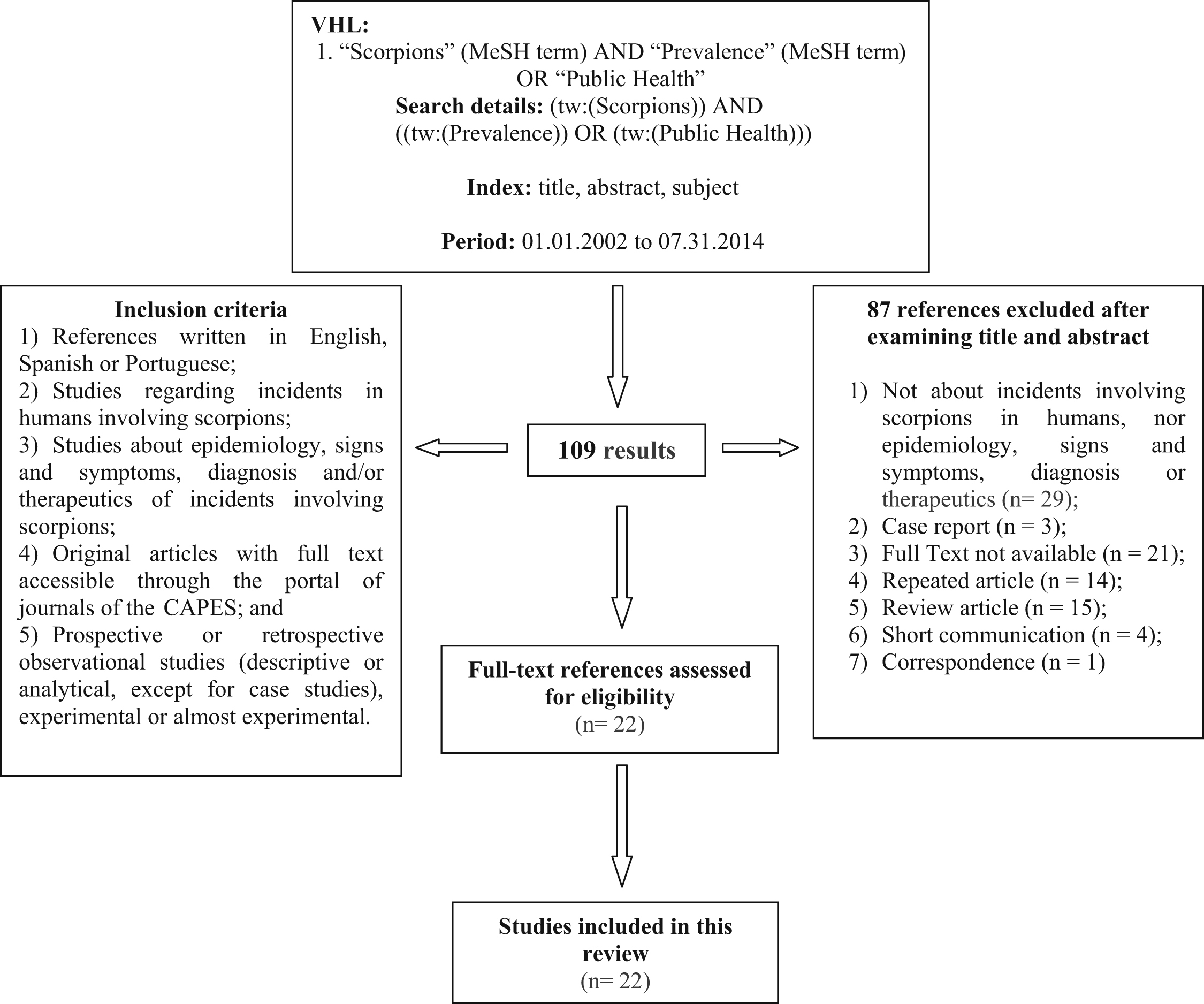
Flow chart showing study selection for the review.
The findings obtained from the 22 studies were divided into the previously determined 4 categories. Some of the included studies were referenced in more than 1 category. The categorization of studies aimed to achieve a better organizational quality of the present systematic review, and it was not compulsory that the articles be referenced only on their respective category.
It is important to note that we had difficulties compiling and organizing all data because there was wide variation in the way results were presented among the articles included in this analysis. The majority of studies did not report details in their results and were often overly generalized. Those articles reporting more details in their results were used to construct Tables 1 and 2. Additionally, not all articles demonstrated enough information regarding treatment modalities to allow inclusion of another table in our review. We address these issues in the Discussion section.
Description of key clinical local aspects of medical importance in humans stung by scorpions
NR, not reported.
Description of the main systemic and neurological effects of medical importance observed in humans stung by scorpions
NR, not reported.
The first column shows the retrospective data (n=80), while the second presents the prospective analysis (n=12) from the same study. All cases have involved the species T. asthenes.
Discussion
Epidemiological Aspects
Scorpions are venomous arthropods, members of the Arachnida class and of the order Scorpiones. Among 1500 described species, the venom of 50 species are dangerous for humans, and most of these species belong to genus Buthus, Parabuthus, Mesobuthus, Tityus, Leiurus, Androctonus, or Centruroides; all of them belong to the same family, Buthidae.5,6 Figure 2 shows the distribution of scorpion species throughout the world, according to the studies included.
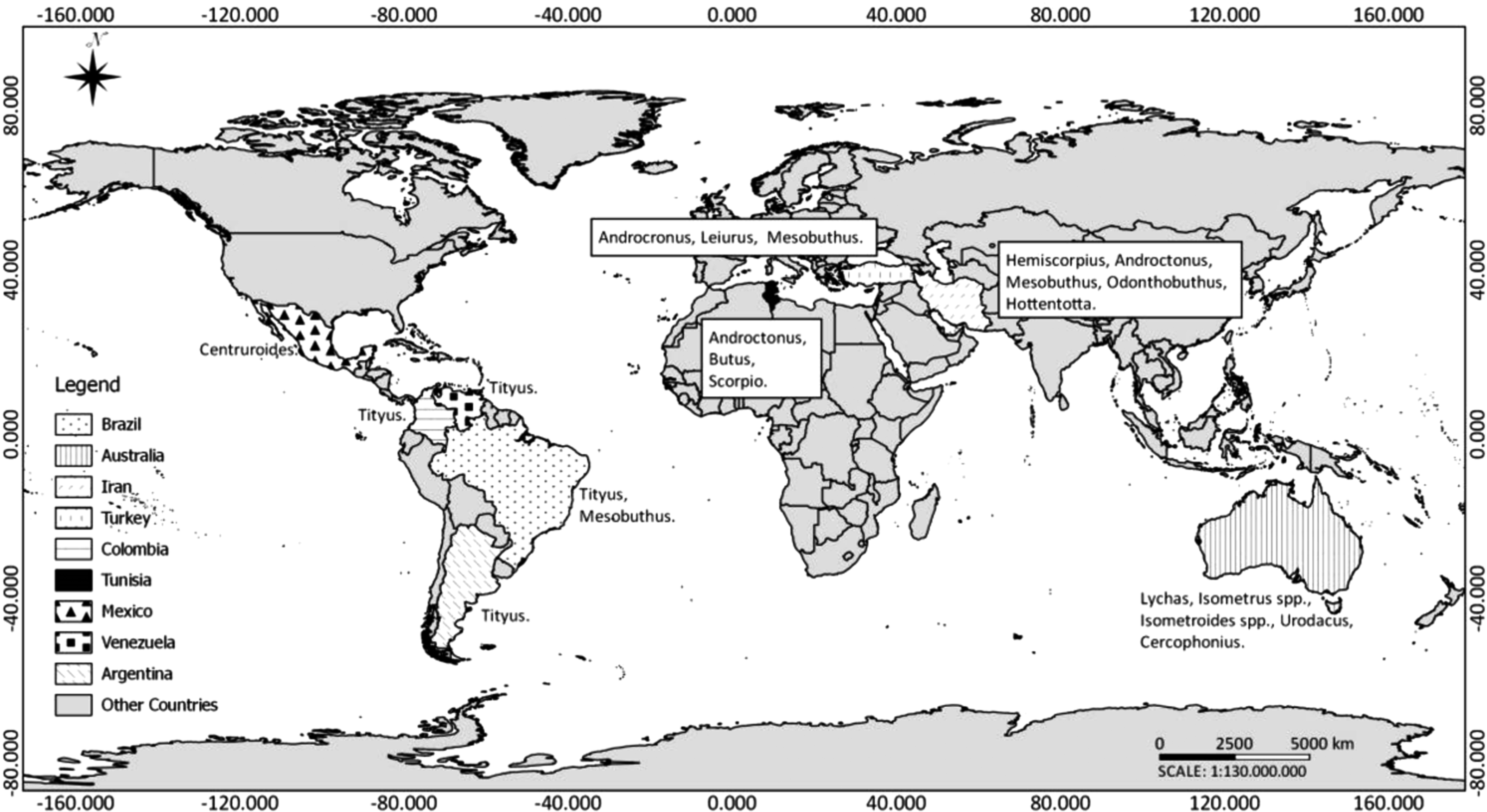
Main scorpions of medical importance found around the world, according to the studies retrieved in the present review.
Envenomation by scorpion stings is a major public health problem in several tropical countries because of the frequent incidence and the potential severity. In South America, scorpions that are dangerous to humans belong particularly to the genus Tityus. Table 3 summarizes the epidemiological aspects of scorpionism in the most affected world regions.
Epidemiological aspects of scorpionism in the most affected world areas
There are few epidemiological population-based studies about scorpions in urban areas where this problem is considered endemic or studies investigating characteristics of the etiological agents responsible for the accidents. Among the studies with the scope of this article, Spirandeli-Cruz et al 7 developed a noteworthy study in an endemic area of the state of São Paulo, Brazil, while De Sousa et al 8 did research in the state of Sucre, Venezuela.
As mentioned, the epidemiology of scorpionism globally remains underreported.2,3 Scorpionism should be a constant object of public action mainly aiming to provide better information and promote population behavior change. The high number of stings occurring throughout the year has important consequences for the design of prevention strategies targeting the reduction of the incidence of scorpionism. 9 Therefore, understanding the epidemiology of this injury is of utmost relevance. 10
Envenomation by scorpions depends on several factors in both the scorpion and the victim. From the former, species, size, types of toxins, status of the telson venom ducts, number of stings, and quantity of venom injected could be mentioned. 11 From the victims, the anatomical location of the sting should be considered, as well as the victim’s age, weight, and health status. It is worth mentioning that children and elderly people are more susceptible to this kind of incident. 12 –15
The temporal incidence of scorpion stings shows a strong seasonal pattern correlated to climatological variables. Increasing scorpion activity in the warmer months has been observed in the state of Guanajuato, Mexico, which the dangerous scorpion species Centruroides infamatus infamatus inhabits. 11 Similarly, in Argentina, increasing scorpion sting incidence caused by Tityus trivittatus was observed in the warmer months, from October to April. 16 Dehesa-Dávila 17 associates the beginning of the rainy season with a decrease in the number of scorpion stings.17,18 Most scorpions are nocturnally active and hide in leaf litter, rocks, or burrows during the day. 19 However, Chowell et al 18 indicate a strong and positive association between minimum temperature and scorpion activity in Mexico. The highest scorpion sting incidence occurred when a minimum temperature of 19.4°C was reached in 2000 and 18.8°C in 2001. This correlation is in agreement with other studies carried out in Brazil and Argentina.11,16 The authors observed “threshold” behavior between pluvial precipitation and scorpion sting incidence. 18 When rainfall was lower than 30 mm/month, there were very few scorpion stings; when rainfall was higher than 30 mm/month, incidence of scorpion sting was independent of the actual rainfall. This could be because of rainfall, which disturbs the scorpions, forcing them to find new refuges.
Clinical Aspects
The clinical manifestations of scorpion envenomation are predominantly mediated by the sympathetic and parasympathetic systems and depend on the scorpion species. Systemic effects of scorpion envenomation include massive autonomic neurotransmitter release (adrenergic or cholinergic autonomic storm) as a result of the excitatory neurotoxins of the scorpion venom. It is known that neurotoxins present in scorpion venoms allow calcium channels at presynaptic nerve terminals to open and thereby initiate autonomic storm. 5 Table 1 summarizes the main local manifestations of medical importance reported in humans stung by scorpions.
High morbidity and lethality rates in children have usually been associated with immune system vulnerability and the ratio between venom dosage and patient body weight.12,13 Children under 7 years old and the elderly constitute a risk group because the immune system is still developing or weakened, but healthy adults are not immune to scorpion stings; fatal cases can also occur in this group.14,15 Beside patient age and susceptibility, other reported aspects that can influence the signs and symptoms of scorpion envenomation include the scorpion species, patient sex, sting site, and the period elapsed between the time of the sting and first medical aid. For this reason urgency of care is extremely important because a possible systemic situation may be established in a patient in a few minutes or hours. 16 ,20,21 Moreover, clinical reports of victims stung by scorpions also described cardiac dysfunction and respiratory failure, which may be fatal. 4 ,22–25
Medically significant scorpion envenomation is almost universally characterized by intense local pain, usually without local tissue injury. Systemic effects occur in a small proportion of scorpion envenomation. Effects depend on the scorpion species involved and are caused by a variety of excitatory neurotoxins.5,19
Regarding the anatomical site affected by scorpion sting, the percentage of lower limb involvement ranged from 15% to 60.4%, while upper limb involvement varied from 12.3% to 73.7%. The percentage in the trunk ranged from 3.8% to 17.3%, and head and neck from 0.9% to 8.6%. 1 ,2,16,26–30
The severity of envenomation can be classified into 3 categories: 1) mild, when patients only present local signs, such as edema, erythema, sweating, numbness, and twitching; 2) moderate, when patients also present with vomiting, abdominal pain, tachypnea, tachycardia or bradycardia, mild hypertension, generalized sweating, agitation, hypersalivation (sialorrhea), dysphagia, fever, priapism, and/or hyperglycemia; and 3) severe, when patients present with cardiovascular complications, such as myocardial failure or dilated cardiomyopathy, congestive heart failure, shock, arrhythmia, or severe hypertension; pulmonary complications, such as pulmonary edema or adult respiratory distress syndrome; gastrointestinal complications, such as acute pancreatitis or peptic ulcer bleeding; metabolic complications, such as hyperglycemia, hypocalcemia, hyperkalemia, or acid-base imbalance; and neurological symptoms, such as hypertensive encephalopathy, stupor, coma, or convulsions, 26 as well as impaired hemostasis and multiple organ failure. 31 Table 2 lists the main systemic and neurological effects of medical importance noted in humans stung by scorpions.
Severe scorpion envenomation may be accompanied by gastrointestinal manifestations and metabolic acidosis even in the absence of hypoxia.32,33 The incidence of gastrointestinal manifestation varies from 11% to 100% according to the species of scorpion and the age of the patient. 16 ,19,34,35 Nevertheless, in Tunisia, Bahloul et al 2 found that 507 (74%) patients had gastrointestinal signs or symptoms. Diarrhea was seen in 36 (5.3%) patients and mortality was significantly higher in this group (P = .023). Bahloul et al 33 observed nausea in 24 patients (2.5%), vomiting in 687 (72.2%), and diarrhea in 41 (4.3%). Furthermore, the presence of diarrhea was associated with respiratory failure (P = .01), neurological failure (P <.0001), and liver failure (P <.0001).
In a retrospective study performed in Colombia, envenomation was mild in 71 cases (88.8%) and moderate in 9 (11.2%). Moderate envenomation was significantly more frequent in children (7/25 [28%]; P = .004) than in adults (2/55 [3.6%]). At the end of a prospective study, envenomation was mild in 4 (33%) and moderate in 8 patients (67%); of these, 6 were children under 15 years old. 26
Bahloul et al 2 revealed that the most observed abnormality was sinus tachycardia. T-wave changes were observed on electrocardiogram in 130 (19%) patients. Other electrocardiography abnormalities were also observed, including ST segment depression or elevation in 94 (13.7%) patients. Moreover, in 3 patients who underwent echocardiography and scintigraphy, the cardiogenic nature of the pulmonary edema was confirmed by a low left ventricular ejection fraction (less than 45%). Uluğ et al 5 found that electrocardiographic changes were not seen much in their series (in Turkey), except for sinus tachycardia and ST segment alterations and prolonged QT interval in 6 (6.1%) and 1 (1%) of the cases, respectively.
In another Turkish study, Cesaretli and Ozkan 4 reported that localized symptoms were observed in 77.9% of cases. In the study by Pardal et al 28 in Brazil, symptoms and local signs represented 91.7% of victims and systemic manifestations were present in 98.6% of the cases of envenomation. However, in another study, 5 scorpion stings caused both local and systemic effects, but the former were more frequent (86.2%) than the latter, as shown by Barbosa et al. 10 In this study carried out in Brazil, only 8.99% of victims had systemic symptoms, with moderate or severe clinical manifestations; 1.85% of victims who received medical care did not show any symptoms.
In the study by Bahloul et al 2 systemic inflammatory response syndrome was observed in 555 patients (81%), and 552 patients (80.6%) developed organ failure in at least 1 organ. Cardiac failure was observed in 542 (79.1%) patients, respiratory failure in 444 (64.8%), neurological signs and symptoms in 25 (3.6%), renal failure in 13 (1.9%), and hematologic or hepatic failure in 7 (1%). Moreover, most patients (64.7%) had organ failure in more than 2 organs. In another study, 33 liver failure was observed in 17 patients (1.8%) and was correlated with a worse prognosis, with a mortality rate of 41.1% in the liver failure group vs 7.4% in the remaining group (P < .0001).
According to Bahloul et al, 2 80.2% of patients had priapism and 26.4% had cyanosis, while according to Adiguzel et al 1 only 1.8% presented with cyanosis. Additionally, Bosnak et al 30 state that patients simultaneously presented with priapism (17.3%) and other symptoms, such as cold extremities (38.4%) and autonomic storm (38.4%).
Pardal et al 28 investigated scorpionism in a northern state of Brazil and found that neurological manifestation predominated over general manifestations. Nevertheless, electric shock sensation in the body was the more common symptom (88.9%), whereas the most frequent signs were myoclonus (93%), dysmetria (86.1%), dysarthria (80.6%), and gait ataxia (70.8%).
Bahloul et al 2 also evidenced that 580 patients (84.7%) had neurological manifestations. Consciousness abnormalities (Glasgow Coma Scale <14) were observed in 177 (25.8%) patients; 123 (18%) of these patients had coma (Glasgow Coma Scale <12). A computed tomography scan of the brain was performed in 9 patients; cerebral edema and/or brain ischemia were observed in 7 patients. Furthermore, the authors also presented more information about neurological manifestations, such as squint (16%), bilateral myosis (5.7%), bilateral mydriasis (2%), and anisocoria (0.6%).
In Iran, Shahbazzadeh et al
29
registered that 3 patients died after being stung by scorpions: 1 case involved a 13-year-old girl envenomed by Hemiscorpius lepturus at 2:00
Albuquerque et al 9 found that most scorpion envenomation cases were successfully treated, but 3 children who were under 5 years old died because of scorpion stings during the analyzed period. Similarly, 2 deaths occurred in children who were 4 and 6 years old. 10 Soares et al 15 found that 1994 was the year that presented the largest number of deaths, with 4 male deaths (1.04%). These studies were conducted in Brazil. In Venezuela, Mejías et al 37 reported 11 deaths due to scorpionism within the period 1995 to 2000. Bahloul et al 2 registered 8.9% of deaths.
Diagnostics
Identification of the scorpion may be considered a very useful epidemiological tool in order to determine the incidence and the risk of envenomation.4,27 Bosnak et al 30 have reported that in hospital admission, scorpion species identification was difficult because of the information provided by the patients and/or their guardians; however, a description of the scorpion’s color was obtained in 6209 (53.3%) of cases as yellow and 2025 (17.4%) as black. The diagnosis of scorpion envenomation was based on a positive history of scorpion sting and when the scorpion was seen or killed by relatives or a bystander. 30
In addition to the information provided by the patient or other person, physicians should keep in mind that victims can exhibit some of the local and/or systemic manifestations as shown in Tables 1 and 2. Additionally, several laboratory tests have been shown to be useful in the diagnostic and the follow-up of these patients.
According to Mohseni et al, 27 urine analysis data, through monitoring hemoglobinuria, was considered the most important examination in following up scorpion victims and during their recovery period. There was severe hemoglobinuria in 95% of H lepturus victims and in 17% of Androctonus crassicauda victims. 27 In another study, the most common laboratory findings were high aspartate transaminase (n = 38), alanine transaminase (n = 26), lactate dehydrogenase (n = 16), and creatine phosphokinase (n = 15) levels. While 92 patients (92.9%) had normal white blood cell count, leukocytosis was present in 6 cases (6.1%) and leukopenia in 1 case (1%). Thrombocytopenia was seen in 21 patients (21.2%). Serum glucose level was higher than 140 mg/dL in 3 cases, and sodium level was lower than 132 mmol/L in 2 events. 5
Mohseni et al 27 found in their research that the maximum levels of serum glucose in the victims of H lepturus, A crassicauda, and other scorpion species were recorded as 270 mg/dL, 220 mg/dL, and 245 mg/dL, respectively. The maximum blood urea nitrogen levels were recorded as 29 mg/dL, 16 mg/dL, and 31 mg/dL, respectively. These results suggest that the venom of scorpions in Ramhormoz, Iran, increased the levels of serum glucose in some victims. This effect might be caused by pancreatic damage promoted by the scorpion toxins; however, this is not completely confirmed. Finally, based on their results, the authors assert the levels of glycemia, blood urea nitrogen, and creatinine in scorpion victims could be considered as paraclinical markers.
A prospective study 26 showed leukocytosis, hypertension, and abnormal electrocardiography in 25% (3/12) of cases; bradycardia, intercostal retractions, and neutrophilia in 16.7%; and arrhythmias and ataxia in 8.3%. All patients were stung by Tityus asthenes. Shahbazzadeh et al 29 observed hemoglobinuria in 1763 (14.5%) patients, in which 145 (8.2%) of the cases showed a positive result even after 24 hours. The intensive degree of hemoglobinuria was reported in 1193 envenomed patients. Mohseni et al 27 stated that red blood cell count in the H lepturus, A crassicauda, and unknown scorpion victims were in the normal levels.
Therapeutics
Some authors report that first aid for scorpion sting incidents included application of ice or a cold pack on the affected site and analgesic intake; however, considering the risk involved it is important that the victims seek medical care to avoid complications.5,19
Scorpion envenomation treatment has 2 components: antivenom administration and supportive care. Antivenom must be administered as soon as possible and through the venous route.2,3 Different approaches have been advocated by different investigators. Some recommend that mild envenomation cases be treated by symptomatic measures with or without antivenom,4,38 and severe cases by symptomatic measures, vital functions support, and intravenous administration of antivenom. 4 ,25,38 Regarding the time elapsed between the scorpion sting and antivenom therapy, a fast treatment (less 2 hours) results in a better prognosis, due to the rapid scorpion venom distribution throughout the victim’s body.9,38 Species-specific antivenom therapy is a widely accepted strategy for scorpion envenomation. 1 ,39,40
The antivenom treatment, initially introduced in 1897, is still the single main therapeutic strategy against scorpion envenomation.1,40 The antivenom dose depends on the severity of symptoms and the amount of inoculated venom. When the latter is about 30 to 50 LD50 of neutralized venom per milliliter of antivenom, the treatment requires from 5 mL in mild envenomation to 20 mL or more in severe cases. 2
Mohseni et al 27 suggest the application of alkaline diuresis to regulate urine alkalosis as a medical approach to prevent renal failure due to the hemolysis effects of H lepturus and antivenom treatments to reduce neurotoxic effects of A crassicauda venom. 27 ,41,42
In addition to antivenom therapy, Uluğ et al 5 report that first aid or treatment included intravenous hydration, analgesia, and ice or cold pack, and they were applied in all cases. Antihistamines and steroids were administered in almost all patients (89.9% for both). There were no adverse reactions to any of the drugs administered, including antivenom. Delayed medical assistance constituted a negative effect on envenomation prognosis; hence, cases that arrived to the hospital more than 2 hours after the sting presented an increased risk of unfavorable evolution.5,43
Once stung, the systemic effects in terms of hematotoxicity and neurotoxicity vary based on species. Specific antivenom is the primary medical treatment, but due to real-world conditions where species may not be identified, polyvalent antivenom is maintained in major treatment facilities. 44
Isbister et al 19 describe the circumstances and clinical effects of stings by Australian scorpions. First aid or treatment was applied in 60 of the 95 cases (63%). The most common treatment was ice or cold pack, in 45 cases (47%). Twenty patients took oral analgesia (paracetamol, paracetamol/codeine phosphate, ibuprofen, and unknown). There was complete relief in only 1 patient, partial improvement in 8 of the 20 patients, and minimal or no effects in the remainder. 19
The importance of antivenom treatment is also verified in a study involving a total of 52 child cases presenting with scorpion envenomation at a single hospital in southeastern Turkey. Antivenom was given at the primary or secondary health center before arrival at the hospital in 44 (84.6%) patients, without any apparent difference in the number of patients presenting mild, moderate, and severe cases. All patients but 1 recovered after treatment; mechanical ventilation was not needed in any patient except for 1 child who died due to severe pulmonary edema. Surviving patients were discharged from the hospital in 2.5 (±1.2) days in apparent good condition. 30
Conclusions
Concerns about accidents of medical importance involving scorpions are relevant throughout the world, mainly in tropical and subtropical regions. Scorpionism is a medical emergency and therefore a life-threatening condition that can cause serious health problems, especially in more vulnerable and susceptible victims such as children and the elderly, if not treated properly and quickly. Potential complications include cardiac dysfunction, respiratory distress syndrome, pancreatitis, impaired hemostasis, neurological and metabolic disorders, and/or multiple organ dysfunction that ultimately can cause death. Urgency of care is extremely important because the life-threatening clinical condition may be established in patients as soon as they are stung or in the hours after the sting. The severity of the case is determined by the scorpion species involved, the number of stings, the body site affected, the amount of venom inoculated, and the general health status of the victim.
Despite the wide variety of species found in the different areas of the world, studies found that all scorpions of medical interest belong to the same family, Buthidae. Stings occur predominantly in the warmer months, in males, and on the limbs. In addition to the main local and systemic manifestations that can be observed in stung patients, some laboratory tests were found to be useful in diagnosis (eg, glycemia, blood urea nitrogen, and hemoglobinuria concentrations). Furthermore, scorpion envenomation can be classified as mild, moderate, and severe, based on the signs and symptoms exhibited by the victim. The therapeutic approach depends on the grade of severity of each case. In general, treatment of scorpionism comprises symptomatic measures, support of vital functions, and antivenom usage. The time elapsed since the moment of the sting until receipt of appropriate medical care is extremely important to the prognosis.
Finally, the large number of scorpion stings worldwide is concerning and reaffirms the need for new prevention measures and policies to reduce the incidence, prevalence, morbidity, and mortality rates from these poisonous arachnids.
Author Contributions: Study concept and design (MSVS, MAPL, CGLS); obtaining funding (MSVS); acquisition of the data (CRPGJ, VHGL, DAB, JVCPL); analysis of the data (CRPGJ, VHGL, DAB, JVCPL, JBC, JGL, BSN, AGTJ); drafting of the manuscript (MAPL, CRPGJ, VHGL, DAB, JVCPL); critical revision of the manuscript (MSVS, MAPL, CGLS); and approval of final manuscript (all authors).
Financial/Material Support: This work was supported by Institutional Program for Scientific Initiation (PIBIC), National Council for Scientific and Technological Development (CNPq), Ministry of Science and Technology, Brazil.
Disclosures: None.
Footnotes
Submitted for publication February 11, 2016.
Accepted for publication August 20, 2016.
