Abstract
Ingestion of Amanita muscaria mushrooms results in transient central nervous system excitation and depression mediated by its components, ibotenic acid and muscimol. The mushroom is distributed worldwide and ingestions occur with some frequency. Although these ingestions have traditionally been considered benign, serious complications can occur. We present 2 cases of serious toxicity, including a fatality. The first case was a 44-y-old man who presented to the emergency department (ED) after cardiopulmonary arrest approximately 10 h after ingesting 4 to 5 dried A muscaria mushroom caps, which he used for their mind-altering effects. Despite successful resuscitation, he remained unresponsive and hypotensive and died 9 days later. The second case was a 75-y-old man who presented to the ED after accidentally consuming one large A muscaria mushroom cap he foraged in Eastern Turkey. The patient initially presented to the ED with hallucinations followed by lethargy, and he was intubated for airway protection. The patient’s condition gradually improved, and he made a full recovery. A muscaria ingestion should not be considered benign as serious outcomes do occur. An understanding of how the main neuroactive chemicals, ibotenic acid and muscimol, affect the brain can help anticipate outcomes. Several high-risk features that portend a more serious course are identified.
Introduction
Amanita muscaria (Figure 1), also called “fly agaric” in reference to its use as an insecticide, is a mushroom found throughout both the northern and southern hemispheres in temperate and boreal climates. 1 Historically, A muscaria has been used by shamans in religious ceremonies to enter a trance state after ingestion. 2

Amanita muscaria, Nelson Lakes National Park, New Zealand (photo by E. Meisel). A muscaria have a distinctive red to orange cap that can fade over time. These mushrooms are covered in white scales and have striate margins with white gills. They can grow up to 20 cm (8 in) tall and often have rings below the annulus that extend up the stipe from the bulbous volva.
The genus Amanita consists of an estimated 900 to 1000 species of which approximately 500 have been described. 3 Due to the toxicity associated with various Amanita species, specifically those containing amatoxin, it is the best studied genus of all mushrooms. Despite the name, however, most species within the Amanita genus, including A muscaria, do not contain amatoxin. 4
A muscaria ingestion causes euphoria and psychotropic effects that are owing to 2 neurotoxins, ibotenic acid and muscimol. As a result, A muscaria is often consumed purposefully and ranks second after the psilocybin-containing mushrooms for mushrooms ingested intentionally. 5 –12
In contrast to other psychoactive mushrooms, A muscaria is often not regulated and is readily available for purchase over the internet. The mushroom is legal in many countries including the United States where it is legal in all states except for Louisiana, which banned it in 2005. 13
A muscaria can produce central nervous system (CNS) excitation and depression that is usually brief. Although usually mild, there are rare reports of more severe outcomes. From 2011 to 2018, the American Association of Poison Control Centers reported 312 exposures to ibotenic acid-containing mushrooms. Of these, only 15 had a major outcome with 1 death. 5 –12 A review of 6 case series accounted for 98 patients of which 7 were intubated without any deaths reported. 14 –18
We present 2 cases of A muscaria toxicity with a severe outcome. We follow this with a discussion of the toxicity associated with the ingestion of these mushrooms based on the current literature.
Case Reports
Case 1
A 44-y-old man with no past medical history presented to an emergency department (ED) in the United States following a cardiac arrest after ingesting 6 to 10 dried mushrooms identified as A muscaria earlier in the day (Figure 2). The mushrooms were given to him by a friend who had purchased them online from a website called
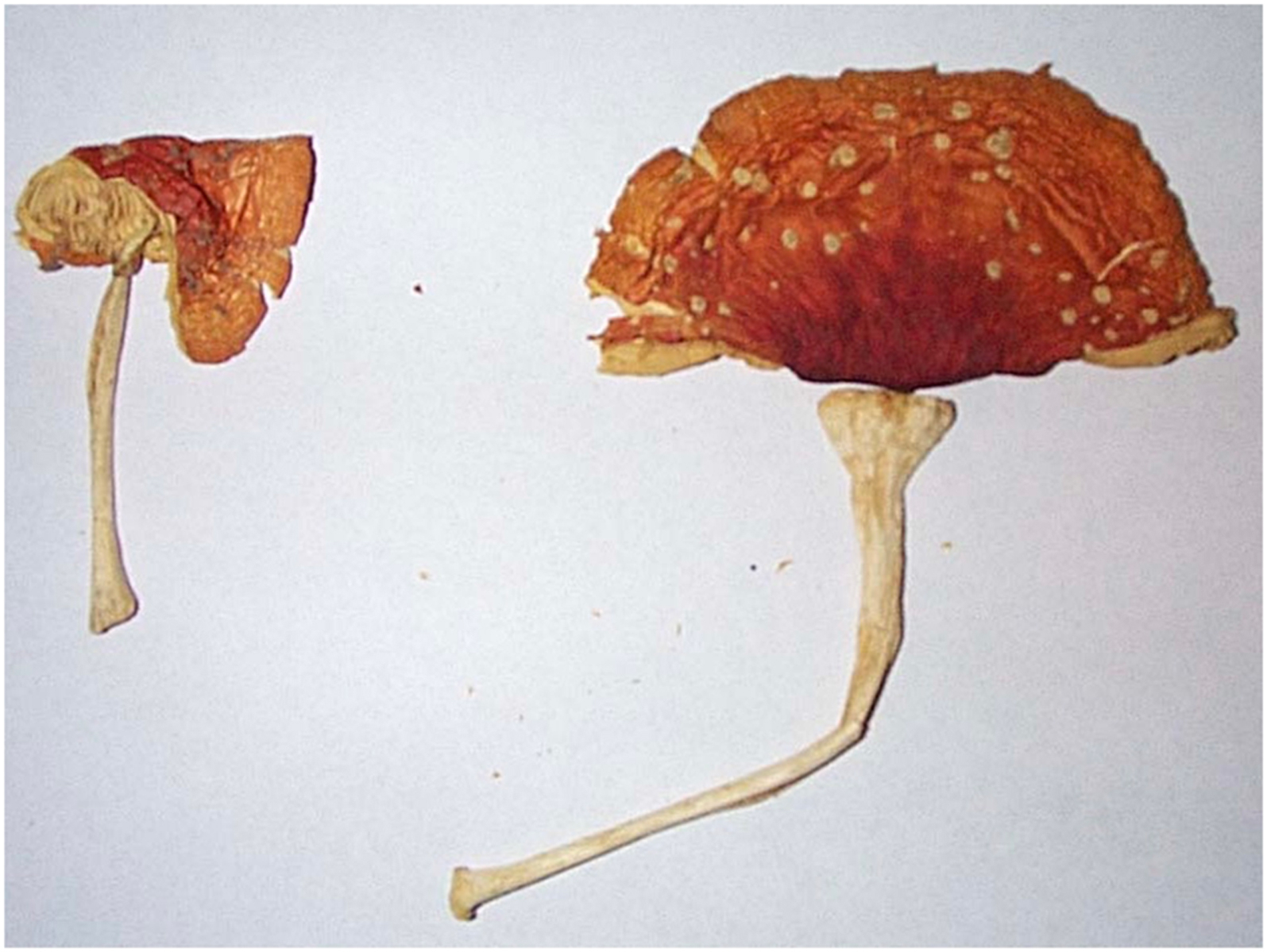
Photo of ingested mushroom retrieved from law enforcement in case 1.
Approximately 30 min after ingestion, the patient was described having fallen asleep. Over the course of the next several hours, the patient developed generalized extremity jerking, shivering, and an episode of emesis. The friend took measures to warm him up by laying him in the sun and then moved him to a warm bath.
Approximately 9 to 11 h after the ingestion, the patient was found in asystole. Cardiopulmonary resuscitation was initiated by prehospital providers with a return of spontaneous circulation after endotracheal intubation and administration of 3 rounds of epinephrine and atropine.
In the ED, vital signs revealed a pulse of 135 beats·min-1, blood pressure of 78/37 mm Hg, and oxygen saturation of 100% on 100% oxygen. Despite the absence of sedation, the patient was unresponsive to noxious stimuli with flaccid limbs. Both corneal and gag reflexes were absent and there were no spontaneous respirations. The pupils were pinpoint and fixed. An electrocardiogram (ECG) showed a narrow complex tachycardia with ST depressions in the inferior leads. Laboratory analysis revealed an elevated white blood cell count of 17.0x103µL-1, a hemoglobin of 13.7 g·dL-1, a hematocrit of 41%, and a platelet count of 173x103µL-1. Additional laboratory values included a serum glucose of 170 mg·dL-1, a blood urea nitrogen of 17 mg·dL-1, creatinine of 2.4 mg·dL-1, a sodium of 155 mmol·L-1, a CO2 of 16 mmol·L-1, a potassium of 2.8 mmol·L-1, and a calcium of 7.6 mg·dL-1. Serum ethanol, acetaminophen, and salicylates were undetectable, as were drugs of abuse as shown through an immunoassay for the presence of cocaine, opioids, THC, and amphetamines. A serum tricyclic antidepressant screen was also undetectable.
The patient ultimately died on day 9 after life support was discontinued because of lack of any improvement in his neurological status.
Results of the autopsy revealed no alternative explanation for the patient’s demise and concluded that the probable cause of death was A muscaria poisoning and the manner of death was accidental.
Case 2
A 75-y-old man with diabetes mellitus and chronic obstructive pulmonary disease presented to an ED in northeastern Turkey with nausea and vomiting 30 min after consuming a wild mushroom cap collected from his backyard for a family dinner. On presentation, he had stable vital signs and a normal exam except for visual and auditory hallucinations. Five hours later he became confused, his Glasgow Coma Score (GCS) score decreased to 8, his blood pressure decreased to 70/50 mm Hg, and his heart rate decreased to 45 beats·min-1. He was intubated for airway protection, received 2 mg of atropine for bradycardia, and was started on a norepinephrine infusion. On repeat exam, his GCS was 3 without sedation and his pupils were 1 mm bilaterally. Laboratory analysis was unremarkable except for elevated blood urea nitrogen of 45 mg·dL-1 and serum creatinine of 1.45 mg·dL-1. An ECG revealed a right bundle block. Imaging studies, including brain computed tomography and magnetic resonance imaging, were normal and an infiltrate was noted on his chest x-ray. Twenty-four hours after arrival, the patient’s GCS improved to 14; however, he had a prolonged hospital stay because he developed aspiration pneumonia that later resolved. Muscimol and ibotenic acid were detected in the collected mushroom samples as well as the patient’s blood samples using liquid chromatography with tandem mass spectrometry. A mycologist identified the mushroom to be A muscaria.
Discussion
Between 1999 and 2018 there were >145,000 mushroom exposures reported to US poison centers. Fortunately, most cases were not severe with only 0.04% resulting in death.5,6,16 Over the last 8 y, of the 23 reported deaths related to mushroom ingestion, only 1 was related to mushrooms containing ibotenic acid. 5 –12
A muscaria, Amanita pantherina, and Amanita gemmata, along with several other species, belong to a group of mushrooms that can produce a poisoning syndrome known as pantherina-muscaria syndrome. 17 Due to its distinctive appearance, poisoning with A muscaria is unlikely to be accidental when compared to A pantherina and A gemmata, although sometimes it can be mistaken for Amanita Caesarea, a highly sought-after flavorful mushroom.1,5–12,17–19 Usually ingestion is intentional because of the mushroom’s psychoactive properties. A pantherina, with its brown coloring and white warts, has a less distinctive appearance and ingestion is typically related to misidentification. 17 Reviewing US poison center data over the last 8 y, which categorizes both A muscaria and A pantherina together with all other ibotenic acid and muscimol containing mushrooms, found that 46% of reported ingestions were intentional. 5 –12
The toxic effect of these mushrooms is attributed to the psychoactive isoxazoles, ibotenic acid and muscimol, which act on the glutamic acid receptors and gamma-aminobutyric acid receptors respectively.20,21 Furthermore, ibotenic acid undergoes decarboxylation to muscimol thereby increasing the concentration of the latter.22,23 Other components have been isolated in smaller concentrations from these mushrooms including muscazone, choline, acetylcholine, betaine, muscarine, hyoscyamine, atropine, scopolamine, and bufotenine and may contribute to the overall toxidrome as well as the occasionally observed cholinergic and anticholinergic manifestations. 24 These other components may also account for the bradycardia and hypotension experienced by our patient in the second case.
After ingestion, symptom onset is rapid, occurring within 30 min to 2 h.14,16,17 The toxidrome is primarily neurological, with the excitatory effects of ibotenic acid seen first, including hallucinations, confusion, and agitation. Convulsions, although not common, have been reported.14,15 The CNS depressive effects of muscimol follow this excitatory stage with progression to lethargy and coma. Multisystem dysfunction is not observed, and symptoms resolve within 24 h.16,18
Gastrointestinal symptoms, consisting of mostly nausea and vomiting, are reported in approximately 50% of poisonings and appear more frequent with A pantherina.14,17,18 Toxicity with A pantherina has less of an excitatory stage with decreased level of consciousness being more common and often the initial presenting symptom. 17 This is likely due to higher concentrations of muscimol relative to ibotenic acid. 20
Cholinergic and anticholinergic manifestations, attributed to muscarine and other neuroactive compounds present in smaller amounts, have also been inconsistently described with both A muscaria and A pantherina. These characterizations are more prevalent in earlier literature and mostly anecdotal. Review of more recent cases, including the 2 largest case series to date, reveal cholinergic and anticholinergic symptoms to be rare.17,18
Seizures, which may be more common in children, pose a unique challenge. 14 Benzodiazepines are the treatment of choice, but given that CNS toxicity typically progresses from an excitation to depression state, patients are already at high risk for profound CNS depression. Not surprisingly, there is an association between benzodiazepine administration and the need for intubation. In the case series by Moss et al, 5 of 34 patients required intubation, of which 4 received benzodiazepines beforehand. There was also one intubation reported in a 9-patient pediatric case series as well as a separate publication reporting a single case requiring intubation.14,15 Despite the lack of a control group in these studies, CNS depression with resultant need for intubation should be anticipated, especially in patients presenting with seizure and in patients receiving benzodiazepines.
Although toxicity from A muscaria and A pantherina share similarities, there can be a spectrum of clinical effects leading some experts to suggest that they be classified as 2 separate toxidromes. The different ratios of ibotenic acid and muscimol between the 2 species is certainly a contributing factor to the differing onset and progression of toxicity between the 2 species. Whether the ingestion was intentional or not may also affect the dose and resultant toxicity. The active toxins, although not heat labile, are water soluble, so boiling or soaking in water prior to consumption may alter the toxic effects. 20 Toxicity from fresh mushrooms, which are higher in ibotenic acid, will be different from than that of dried mushrooms which will contain higher concentrations of muscimol related to increased conversion of ibotenic acid to muscimol during the drying process. 23 It has also been suggested that, along with geographical variation, the season can affect the concentrations of the various neurotoxins. 14
In the first case, we were able to obtain the mushroom samples, and ingestion of A muscaria was confirmed by a mycologist and coroner examination. Unfortunately, confirmation by qualitative testing of preserved specimens in this case was not performed, which does pose limitations. In the second case, we were able to confirm the presence of ibotenic acid and muscimol in both the serum and mushroom samples with liquid chromatography with tandem mass spectrometry.
Conclusion
Toxicity from Amanita mushrooms that contain ibotenic acid and muscimol is generally considered low-risk; however, our cases and a review of the literature demonstrated that severe outcomes do occur. Central nervous system excitation followed by CNS depression with complete resolution of symptoms within 24 h is typical, but the possibility of more deleterious effects, including seizure and respiratory depression, should be anticipated and patients should be monitored closely until symptoms have completely resolved. An understanding of the main neuroactive chemicals is necessary to understanding the resultant toxidrome and anticipating symptoms. The number of mushrooms consumed, how the mushrooms were prepared, and when and where the mushrooms were picked, can potentially affect the resultant toxicity.
Footnotes
Acknowledgements
Author Contributions: Study concept and design (EMM, ZK BM); data acquisition (EM, ZK, AS, HC); data analysis (HC, MS); drafting, critical revision, and approval of final manuscript (all authors).
Financial/Material Support: None.
Disclosures: None.
