Abstract
Centipede bites are a constant risk throughout tropical regions and have the rare potential for systemic side effects. We report a case of multiple centipede bites in South Sudan that was complicated by severe pain refractory to opioid analgesia and an unusual association with acute involuntary muscle contractions. Treatment with local anesthetic, antihistamines, and corticosteroids was effective. This report aims to add to the local literature; because of decades of internal conflict and poor infrastructure, reporting of health data from South Sudan is severely lacking. Further investigation into the pharmacological variation and activity of toxic peptides in centipede venom is recommended. As it stands, this case provides additional information on potential effects of centipede envenomation that should be useful to any healthcare providers preparing for the delivery of remote medical care throughout the Great Upper Nile region.
Introduction
Centipede species are common throughout tropical and subtropical regions. Although the majority of bites heal with supportive treatment, they carry the potential for systemic side effects. Presentation of symptoms can vary substantially and therefore poses a constant challenge to management in remote locations. 1
Because of decades of internal conflict, little is understood about the epidemiology and mechanism of action for biting arthropods throughout South Sudan. This case describes an incident of multiple centipede bites experienced by a single soldier supporting the United Nations Mission in South Sudan and managed in a remote area of the Upper Nile State, in close proximity to the White Nile river. Access to secondary healthcare can be difficult in this region and is often weather dependent.
Case report
We report the case of a normally healthy 21-y-old infantry soldier who experienced a centipede bite while on duty with the United Nations Mission in South Sudan. The bite occurred during the night when a centipede fell from an improvised defense structure onto the patient's left hand and stung the lateral edge of the little finger. Rapid withdrawal of the hand toward the chest caused the centipede to fall inside the soldier's body armor where, unable to remove it, he was stung multiple times across the upper left chest.
Initial symptoms included tachycardia of 120 to 130 beats·min-1, shortness of breath (>30 breaths·min-1), and marked anxiety. The patient reported severe pain in the left hand and across the chest. The left hand and forearm demonstrated intermittent periods of painful involuntary spasm with fasciculation evident across the upper left chest wall in close vicinity to the bites. Specifically, contraction was seen of the flexor carpi ulnaris, hypothenar, and flexor digiti minimi muscles. Contraction was into full flexion, lasting 10 to 15 s and punctuated by short 5 to 10 s periods of relative relaxation. Typical hemorrhagic chevron marks and the remains of the centipede were clearly identifiable. Pain and spasm were worse in the hand, where development of localized edema and erythema was immediate. Lymphangitis across the upper chest wall developed in the 15 min after exposure. The patient was cannulated, and 5 mg intravenous chlorphenamine was administered. Pain relief was delivered via personal issue of an 800 microgram fentanyl lozenge. Analgesia was reported by the patient to be noneffective, and pain remained severe 20 min later. Local infiltration of 3 mL 2% lidocaine (total 60 mg) was administered via ring block to the left little finger. A wide field block was required to provide pain relief to the chest wall (total 80 mg lidocaine). Five minutes after local anesthetic delivery the patient was pain free, and his itching had subsided substantially. His heart rate reduced to 86 beats·min-1 and respiratory rate dropped to 17 breaths·min-1. The involuntary spasms reduced to muscular twitches that became more intermittent and faded over the subsequent hour.
The patient was recovered to the regimental aid post and given 100 microgram IV hydrocortisone and covered with IV amoxicillin/clavulanic acid, as the most broad-spectrum agent available, against secondary bacterial infection. A tetanus vaccine (Tdap) was delivered. Chest pain resolved, and a 12-lead electrocardiogram was unremarkable. The patient was able to sleep until the following morning. Review on the following day revealed a mildly swollen left hand and generalized but improved erythema that spread out from each bite by approximately 5 cm in an irregular pattern. Repeat 12-lead electrocardiogram remained unremarkable. Urine dip revealed 1+ protein and so was sent for urinalysis at the local Indian Role 2 Hospital. Results showed no sign of acute renal failure; on targeted rehydration, repeat urine dip was negative across all parameters. The patient remained pain free, requiring no further analgesia, and was able to return to active duty 24 h postexposure with no further sequelae.
Discussion
Centipedes are among the most ancient of venomous generalist predators still in existence. 1 From the Chilopoda class, centipede species are arthropods that are broadly connected by the development of forciples, a modified pair of front legs that have evolved for the purpose of envenomation. 2 The Natural History Museum (NHM) in London currently holds one of the most taxonomically complete centipede collections for Africa in the world, yet many species throughout the region remain undescribed. Initial remains were collected at the time of the bite, but identification of the species was unfortunately unsuccessful, and assistance from the UK Centre for Biodiversity (at NHM) 3 was hindered by a complex logistics chain and lengthy delivery time. It is the aim of the authors to engage with future deployments to the region in an effort to collect multiple samples for identification. Description of the centipede, alongside known species inhabiting East Africa, would suggest that it is likely of the genus Scolopendra or Ethmostigmus. Figure 1 provides examples of Scolopendromorpha known to be endemic to Sudan, demonstrating both the forciples of Scolopendra morsitans and a full image of Ethmostigmus trigonopodus as reference points for medical staff operating in the region.
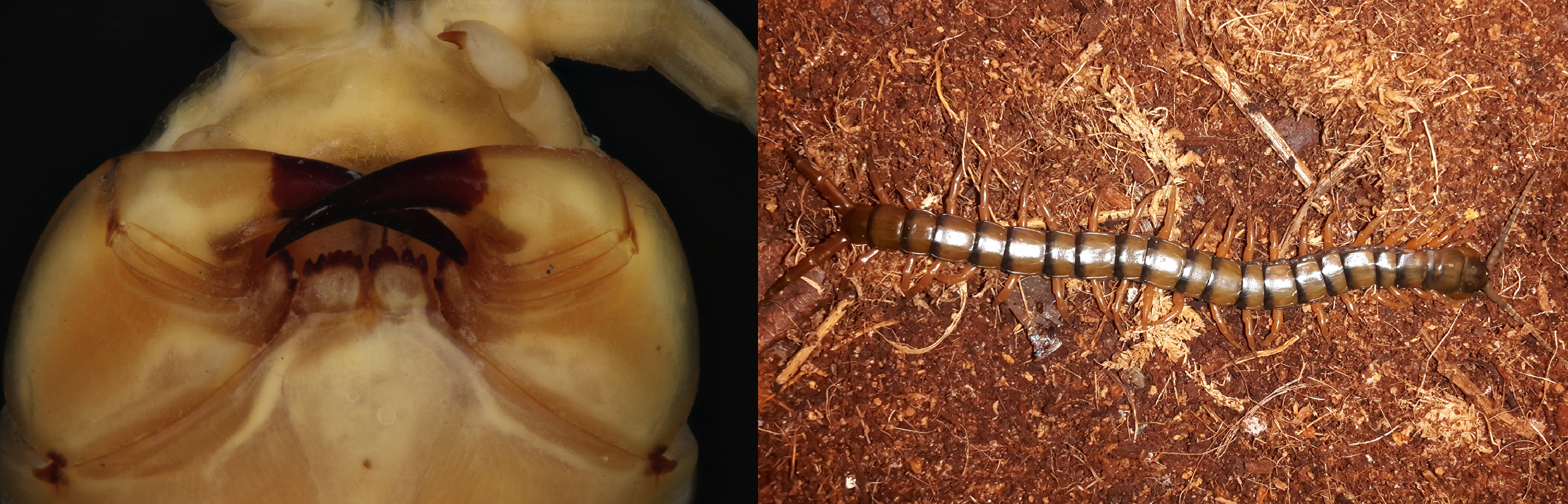
Left: Forciples of Scolopendra morsitans, one of the big Scolopendromorpha known to occur in Sudan. Right: Ethmostigmus trigonopodus, one of the big Scolopendromorpha known to occur in Sudan. Photographs courtesy of Carlos A. Marténez Muñoz (Zoological Museum, University of Turku, Finland), published with permission.
After centipede bites, hemorrhagic marks that appear as a chevron may be seen on the skin and are useful in differentiating the etiology from other biting arthropods if occurring at night. 4 Report of reactions to bites is rare,5,6 and much about the pharmacological structure and function of various centipede venom components remains unknown. 1 This is partly due to the difficulty in obtaining and analyzing the low-yield venom and partly to recognition that the majority of patients recover without complications. 7
Reports of various side effects from centipede bites have been presented from Australia, Southeast Asia, and the Americas. 5 ,6,8,9 Information on the epidemiology and toxic effects of centipedes throughout sub-Saharan Africa is not robust, and there have been no reports of cases in South Sudan. Of the literature available, Scolopendridae family members are recognized as indigenous throughout the Horn of Africa, and there are reports for S morsitans, S mirabilis, and S afar. Review of Scolopenromorph collections from across this part of Africa held at the NHM in 2013 also revealed species of Ethmostigus, Rhysida, and Asanada. 3 Venom proteins from these species are found to be richly diverse and novel; historically, serotonin, phospholipase A2, and histamine components have been identified and partly explain localized effects.10,11 Recent investigation into the cardio- and neurotoxic activity of certain centipede venom proteins, however, has revealed significant variety among species and described several peptide families that have not previously been recognized in arthropod venoms.1,12 It is hoped that recent developments in molecular analysis will generate further interest and a better understanding of the diversity and activity of proteins found in venoms and enable the development of more targeted therapies.
Bites are most commonly reported to cause pain, localized edema, and lymphangitis.13,14 Tachycardia and tachypneic symptoms can be further exacerbated by anxiety. 14 Serious, high-morbidity reactions have been recognized with potential for venom components to cause anaphylaxis 15 and acute myocardial ischemia.16,17 Short-term rhabdomyolysis and acute renal failure can develop, 18 and bacterial superinfection, cellulitis, and necrotizing fasciitis have also been recorded. 19 Neuropathies have been reported after peripheral bites from a variety of athropods 20 ; a centipede bite in particular has been implicated in the onset of a focal dystonia. Development of symptoms occurred shortly after the initiation of treatment, however, making a clear decision on etiology difficult. 21 In contrast, this case developed involuntary contractions within 5 min of the bite and did not demonstrate any signs of central effect. Although this case reports observation of a rare, localized nerve reaction to a centipede bite, this reaction is likely attributable to a separate local mechanism. The potential for various neurotoxic properties has been noted within the Scolopendridae, with recent identification of an S subspinipes mutilans peptide toxin having modulatory activity against voltage-gated potassium and sodium channels.1,22 Voltage-gated sodium channels in peripheral nerves are involved in nociception, and the symptoms observed here could be secondary to toxins causing severe, local pain. Similar responses have been seen with Odontobuthus doriae scorpion venom, where changes to nerve action potentials that are in keeping with activity at sodium and potassium voltage-gated channels are seen on mice hemidiaphragm and lead to contracture. 23 Improvement occurred after local anesthetic administration and may be partly explained by lidocaine's activity on voltage-gated sodium channels. 24
The low level of reporting and poor understanding of different venom components, including neurotoxic compounds, make it difficult to estimate reaction course. Awareness, therefore, of potential side effects in the immediate and short-term postexposure phases is important for healthcare providers to effectively manage bites in subtropical regions.
Remote care poses unique challenges in treating patients with insect bites. Centipedes can be aggressive and may bites multiple times if given the opportunity 14 ; the time taken to move this patient to an area of safety before removal of his body armor resulted in several further bites to his upper chest. Most notably, his pain was initially very difficult to control; opioid analgesia with a fentanyl lozenge was ineffective at 20 min. The remote and potentially unpermissive environment of military operations may preclude the opportunity for testing and time-consuming interventions. It is vital, therefore, that severe pain is quickly and effectively reduced to allow accurate assessment of other symptoms. Although there is no recognized protocol, treatment is often primarily supportive, with anesthetic, antihistamines, and anti-inflammatory medications all having been recommended. 25 We report that local infiltration of lidocaine was completely effective at managing pain through a ring block of the small finger and a wide field block to superficial tissue across the upper chest. Intravenous chlorphenamine was effective at reducing itching symptoms, and some reduction in edema was noted. Local anesthetic as an effective pain management intervention may therefore be the most appropriate initial management for severe pain in remote environments to provide a suitable window in which to recover to a semipermissive environment. Once in a resource-supported location, application of heat is thought to be effective in denaturing some proteins, and subsequent application of ice may aid with local swelling.14,25 Insect envenomation is known to cause myocardial ischemia in a small number of cases, and there are reported incidences of acute myocardial infarction after centipede bites. 17 More thorough assessment is required when possible and should include provision for 12-lead electrocardiogram for acute ischemic changes and urinalysis.
Despite the recognition that some centipede toxins are antibacterial in nature, secondary bacterial infection has been noted and antibiotics should be considered if there are developing signs of infection.19,25 Tetanus prophylaxis should be considered. 25 As with the majority of reported cases, our patient recovered without further issue and was able to return to active duty 24 h later. It is advised that patients be actively followed up for review, which should include wound site assessment and urinalysis.
Summary
We report here the management of a centipede bite in South Sudan that was complicated by management in a remote, semipermissive environment and severe pain with peripheral involuntary muscle contraction that was nonresponsive to opioid analgesia. Use of local anesthetic was effective and should be included in the medications of medics deploying to forward locations for this purpose, especially where the current security situation means recovery to an established healthcare facility can be difficult and unpredictable.
This report is a valuable addition to the local literature; because of decades of internal conflict and poor infrastructure, reporting of health data from South Sudan is lacking. Further investigation into the pharmacological variation and activity of toxic peptides in centipede venom is recommended for the development of a standardized and targeted approach to therapy. This case adds information to the literature on the potential side effects of centipede envenomation that should be useful to military and civilian healthcare providers preparing for the delivery of remote medical care throughout the Great Upper Nile region.
Footnotes
Acknowledgment
The authors are grateful to Carlos A. Martínez Muñoz (Zoological Museum, University of Turku, Finland) and to two other anonymous reviewers for improving the final draft of this work. The authors also thank the staff at he UK Centre for Biodiversity (NHM) for early offers of assistance with identifying the centipede species.
