Abstract
Objective
Scorpionism is an endemic public health problem in Jordan encountered by health providers in all parts of the country. This study updates epidemiological data on scorpion sting encounters in Jordan.
Methods
Data on scorpion sting encounters were obtained from government and military hospitals around the country, and the National Drug and Poison Information Center (NDPIC). P values and 95% confidence intervals (CIs) were calculated using SPSS Professional Statistics Package version 22 (IBM Corp., Armonk, NY) program.
Results
Epidemiological data on 1205 scorpion sting cases reported between 2006 and 2012 are reported. Male to female ratio was 1.18:1, aged 23.3±16 (mean±SD) and 26.4±16.9 years for males and females, respectively. Age groups between 1 to 20 years old constituted 44.6% of the total sting encounters, while adults aged >30 years constituted 30%. Scorpion sting encounters peaked in July (22.5%) and August (23%), with the lowest numbers of recorded cases in February and January (1.6 and 1.9%, respectively). Scorpion stings occurred mostly outdoors (66%). Medical complications associated with scorpion sting cases included fever, difficulty in breathing, drowsiness and dizziness, and numbness, while severe complications include respiratory failure and tachycardia. Hospitalization required 1 to 3 days among admitted patients with no fatalities.
Conclusions
Scorpion stings remain a medical problem in Jordan that requires more attention by health providers. Reporting of scorpion sting cases should be enforced from all healthcare centers throughout the country to better understand the epidemiology and health implications of human encounters.
Introduction
Scorpionism is an endemic public health problem in Jordan encountered by health providers in all parts of the country. Epidemiological data are incomplete and the exact number of encounters remains largely unknown. Few studies addressed the epidemiology of scorpion stings in Jordan. The earliest report on scorpion stinging encounters was published by Wahbeh. 1 Five hundred forty seven cases of scorpion sting were reported from 1982 through 1985, with 2 fatalities. 2 Additionally, 338 cases of scorpion stings in Ma’an Government Hospital and outpatient clinics in the Irbid area from 1989 through 1992 were reported with no fatalities. 3 Mutair et al. 4 reviewed medical records for 96 patients admitted to 3 hospitals after scorpion sting encounters from 1997 through 1999, with 2 fatalities (2.1%). A comprehensive account on the scorpions of Jordan, with data on scorpion stings was recently published. 5 Moreover, additional records to the scorpions of Jordan was updated. 6
In Jordan, 18 species and subspecies of scorpions belonging to 2 families (Buthidae and Scorpionidae) have been recorded. 2 ,5–7 At least 5 species are considered dangerous (Androctonus amoreuxi, Androctonus bicolour, Androctonus crassicauda, Leiurus hebraeus, and Leiurus jordanensis). Leiurus hebraeus is the most common species with a wide range of distribution.
In the Middle East, the epidemiology of scorpion stings was reported from Saudi Arabia, 8 –10 Turkey, 11 –13 and Iran.14,15
This study updates epidemiological data on human scorpion stings encountered in Jordan from 2006 through 2012.
Methods
Data on scorpion sting encounters were obtained from Princess Haya Hospital (PHH) in Aqaba, southern Jordan (2006–2012); the National Drug and Poison Information Center (NDPIC), Jordan University Hospital, covering the years 2009 through 2012; and the Ministry of Health, Directorate of Environmental Health (DEH) from 2006 through 2012. The DEH data cover cases treated at hospitals and health clinics operated by the Ministry of Health. Data from PHH and NDPIC that was published by Amr 5 was pooled with data obtained from DEH.
The Ministry of Health requires mandatory reporting of scorpion stings and snakebite cases from all its affiliated hospitals and healthcare centers to the DEH. The data include age, sex, date of admission, days required for hospitalization, and other relevant information. Despite these regulations, it is noteworthy that some remote health centers do not report to the DEH. Princess Haya Hospital is affiliated with the Armed Forces and serves both civilians and military personnel in southern Jordan. The NDPIC is affiliated with Jordan University Hospital. Table 1 shows the number of cases reported from each source. P values and 95% confidence intervals (CIs) were calculated using SPSS Professional Statistics Package version 22 (IBM Corp., Armonk, NY) program.
Summary for the source of reported cases of scorpion sting accidents
NDPIC, National Drug and Poison information Center; DEH, Directorate of Environmental Health.
Results
Epidemiological Data
A total of 1205 cases of scorpion stings were reported to PHH, NDPIC, and DEH during the study period (Table 2). The highest number of cases was reported in 2011, while the lowest was in 2010. Male to female ratio was 1.18:1 and was statistically significant (P = .001, 20.99–23.53, 95% CI for males and 22.95–25.78, 95% CI for females), aged 23.3±16 (mean±SD) and 26.4±16.9 years for males and females, respectively, for all groups.
Sex of victims of scorpion stings reported from 2006 through 2012
Victims aged from 1 through 20 years old constituted 44.6% of the total sting encounters, while adults aged >30 years constituted 30% (Figure 1). Females were less vulnerable in age groups between 1 through 30 years, while more vulnerable at age groups aged >30 years. No significant results were found between males and females within the same age group (P = .406). Significant results were found between males and females and their age groups (P = .014, 1.93286–9.66714, 95% CI for males, and P = .034, 0.40968–6.39032, 95% CI for females).
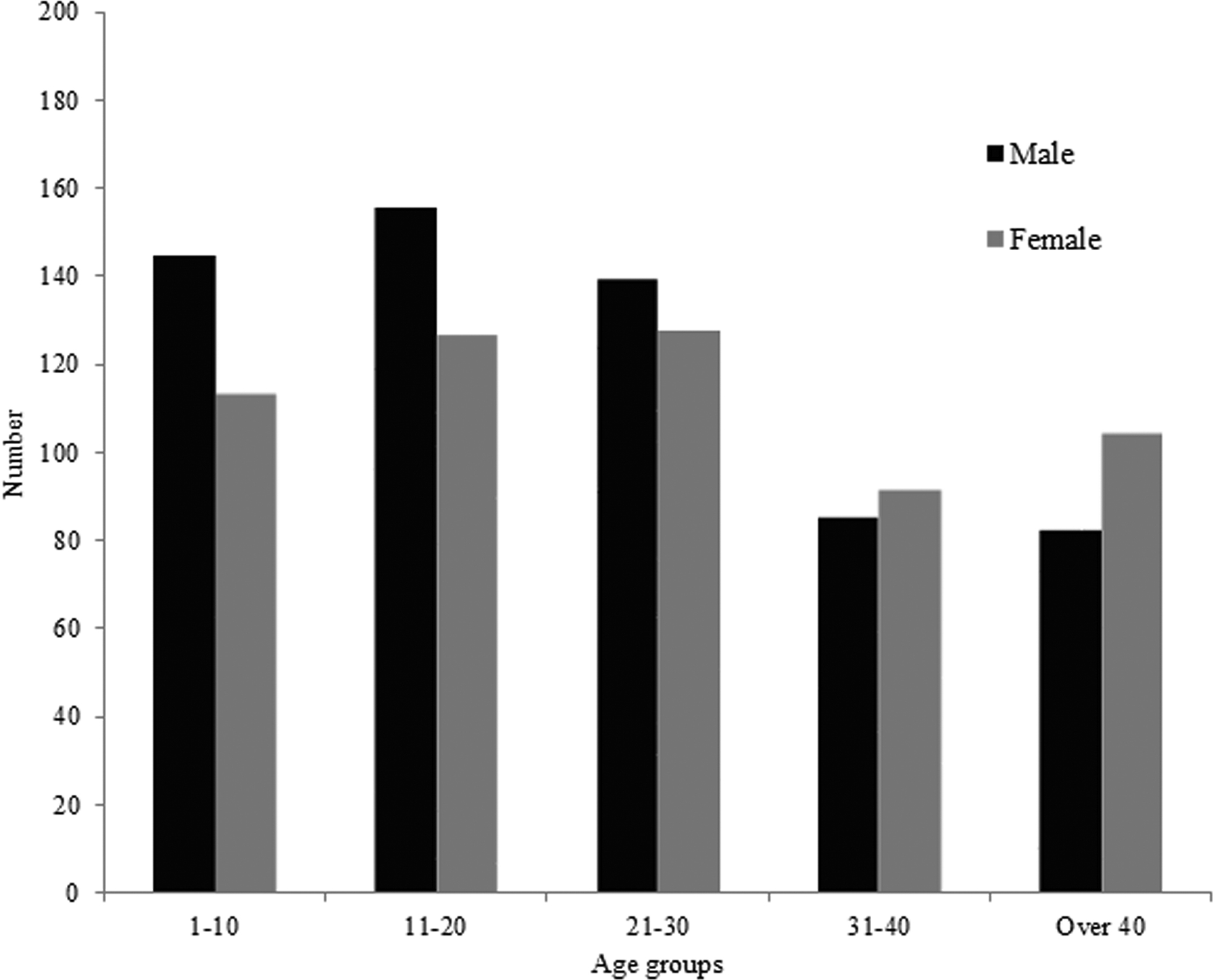
Scorpion sting encounters according to age groups and sex.
Scorpion sting encounters peaked in July (22.5%) and August (23%), with the lowest numbers of recorded cases in February and January (1.6 and 1.9%, respectively) (Figure 2). Significant results were found between the number of cases and the month of the year (P = .002, 152.79–44.38, 95% CI).
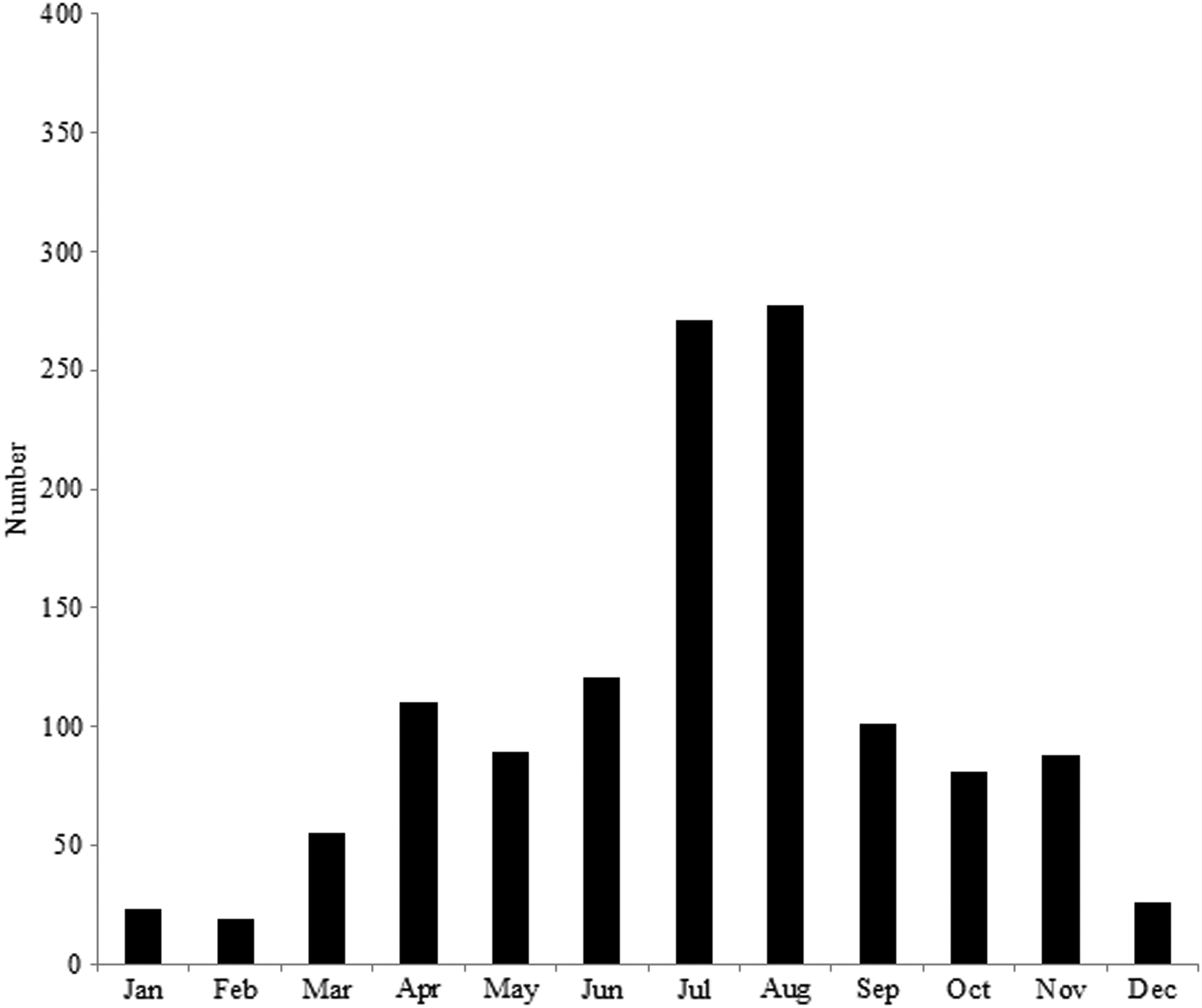
Seasonal distribution of the scorpion stings.
Data obtained from the NDPIC showed that 17 scorpion stings occurred at the patient’s residence (32.2%), 35 occurred outdoors (66%), and 1 case (1.8%) occurred at the workplace. Fingers and toes were the main sites of stings.
We obtained data for the time of exposure to scorpion stings for 64 cases reported to the NDPIC and PHH (Figure 3). Eight cases (12.5%) occurred between midnight and 0900, 30 cases (46.9%) between 0900 and 1600, and 26 cases (40.6%) between 1600 and midnight.
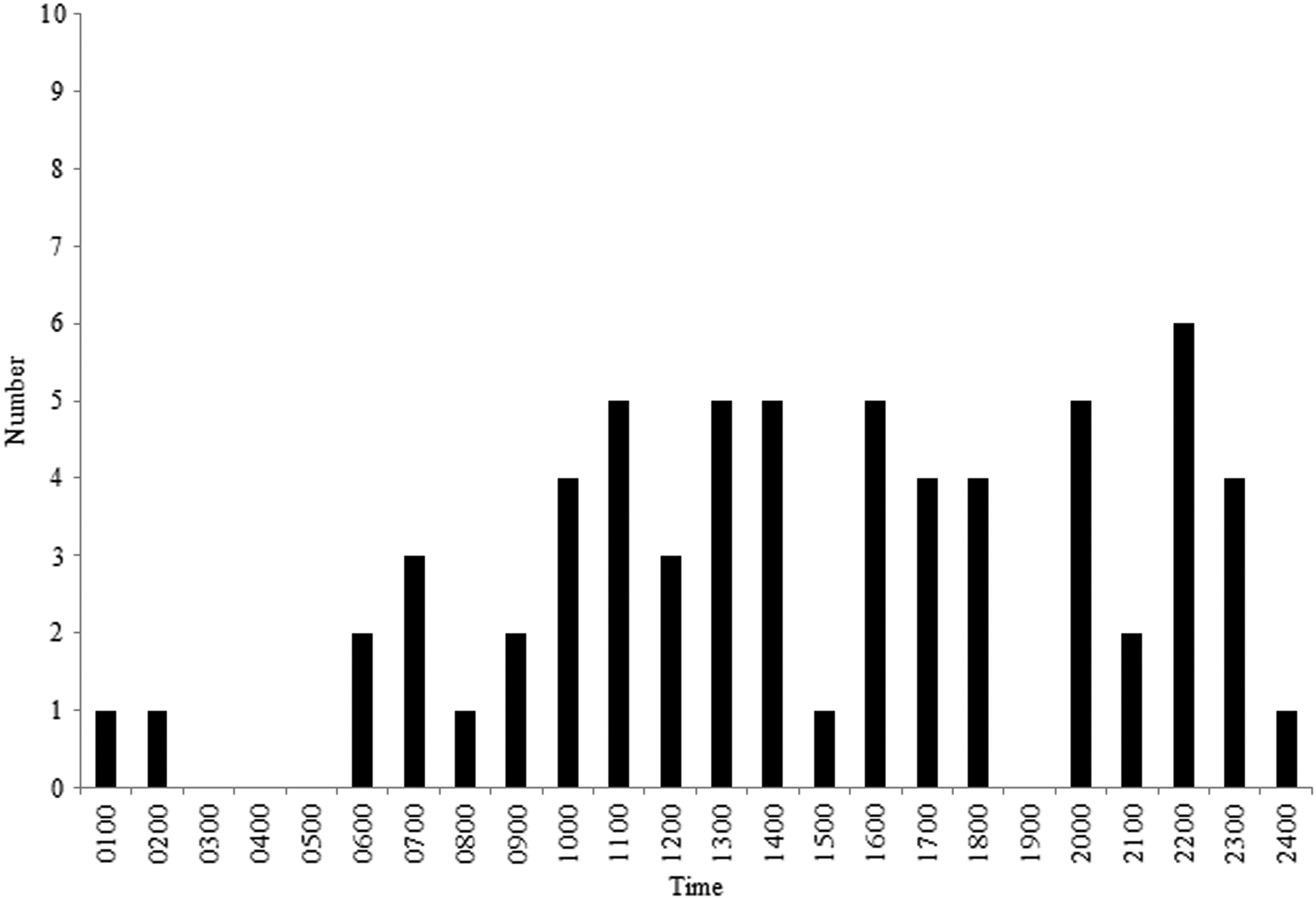
Frequency of scorpion stings and time.
Table 4 and Figure 4 show the number of scorpion sting cases and incidence per 100,000 inhabitants by governorate. Irbid scored the highest number of scorpion sting encounters, followed by Al Balqa Governorate. Lowest numbers were reported from Ma’an and Jarash Governorates. Overall incidence per 100,000 inhabitants was 2.6.
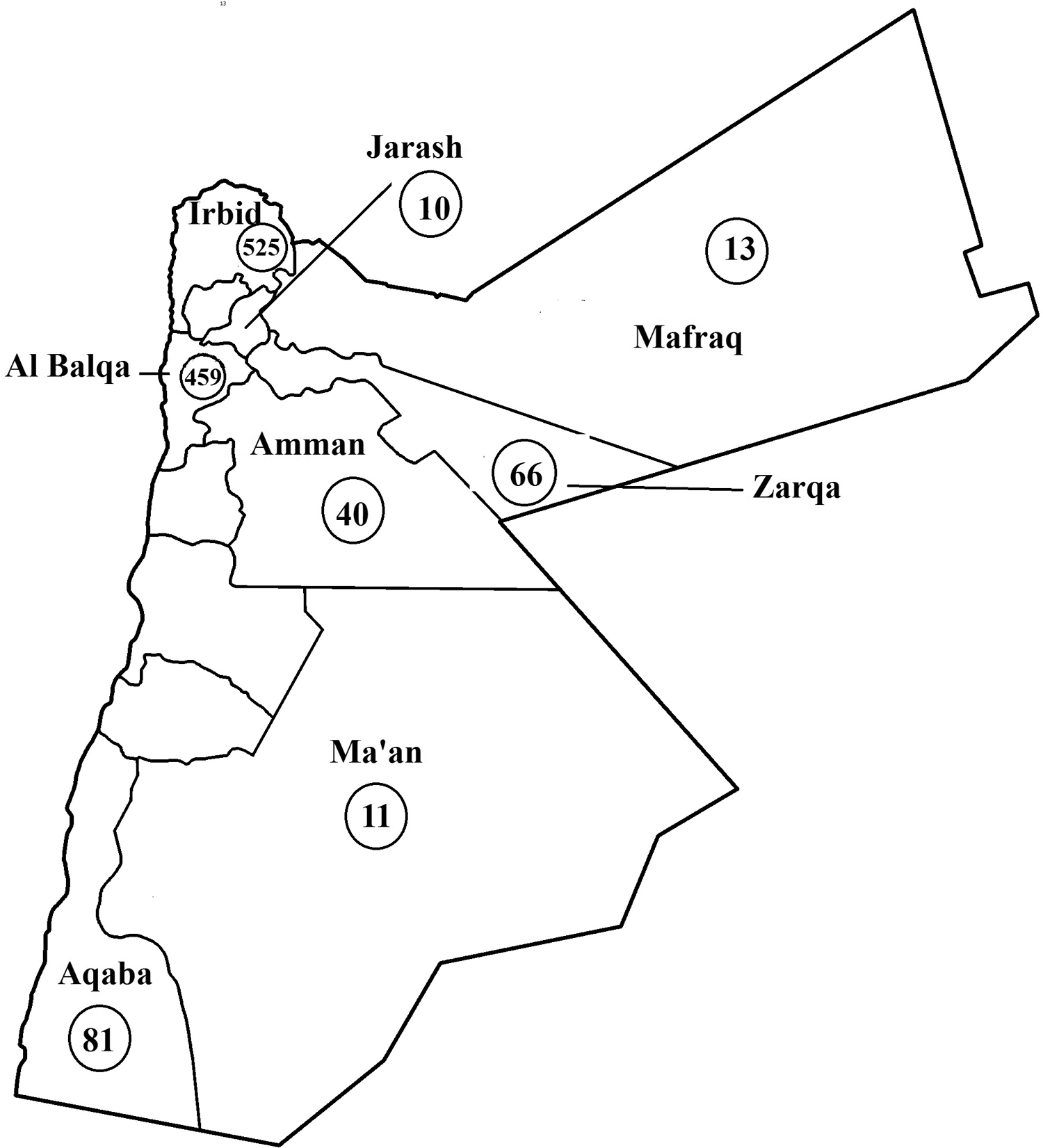
Scorpion sting cases and incidence per 100,000 inhabitants by governorate.
Clinical Data
We obtained clinical data for 53 cases from the NDPIC. Redness and edema at the site of the stings were the most clinical symptoms observed. Other complications included fever, difficulty in breathing, drowsiness and dizziness, and numbness (Table 3). Severe complications included respiratory failure and tachycardia. Hospitalization required 1 to 3 days among admitted patients with no fatalities. Administration of species-specific scorpion antivenom was documented in only 10 cases.
Main clinical symptoms reported in 53 cases of scorpion stings at NDPIC
Scorpion sting cases by governorates and their incidence per 100,000 inhabitants
Scorpion Species
Over the past 15 years, we collected a large number of scorpions from various habitats in Jordan. Eighteen species of scorpions belonging to 3 families (Buthidae, Scorpionade, and Diplocentridae) were identified. Five species are considered highly venomous (Androctonus amoreuxi, Androctonus bicolor, Androctonus crassicauda, Leiurus hebraeus, and Leiurus jordanensis) (Figure 5).

Venomous scorpions of Jordan. A, Androctonus bicolor. B, Androctonus crassicauda. C, Leiurus hebraeus. D, Leiurus jordanensis.
Androctonus amoreuxi was recorded from Wadi Araba and the lower Jordan Valley. This species is known from few localities. Androctonus bicolour was reported from Ma’an, Aqaba, Petra, Karak, and Wadi Rum. Androctonus crassicauda is a desert-adapted species with wide distribution in the eastern desert and Wadi Araba to Aqaba. It was collected from Azraq, Jarash, Νorth Shuna, and Wadi Rum. This species was also collected from the Mediterranean region with dense forests, but in low numbers. Leiurus hebraeus is the most common species in Jordan. It was collected along the Jordan Valley, the eastern desert, the southern mountain range to Aqaba, the southern part of the Dead Sea, and Wadi Rum. Leiurus jordanensis has a rather confined distribution in Southeastern Jordan near the Al Modawrah area. We have no data on the identification of the specific scorpions associated with these sting encounters.
Discussion
Scorpionism is a common medical issue in Jordan. The country is located within the arid Mediterranean region with a relatively high number of scorpion species. Many parts of Jordan are still rural and dependent on agriculture. The rocky terrain of Northern Jordan offers an especially suitable habitat for scorpions. In this setting, children and farmers may suffer scorpion stings when turning over stones and rocks. Fieldstone fences are also very common in Jordan, notably in the mountainous areas of Irbid, Jarash, Karak, Ajlun, and Tafilah, where they offer a perfect habitat for L. hebraeus. In the desert terrain, scorpions were observed using desert rodent burrows: A. crassicauda was seen in many rodent burrows around the Azraq area and Wadi Rum.
The incidence of scorpion stings is related to the seasonal activity of scorpions in Jordan. Highest incidence rates were recorded in rural and agricultural communities in Al Balqa and Irbid Governorates. Fluctuations in the number of recorded cases is certainly related to reporting, especially by the Ministry of Health hospitals and healthcare centers. The increase in the number of reported cases in 2012 may be related to enforcement of mandatory reporting by the Ministry of Health. Our field experience indicated that a higher activity of scorpions occurs during the summer, especially at night, where scorpions become more active to avoid the high temperatures of the daytime and search for food. Stings were more frequent in the summer, peaking in July.2,3 Similar results were obtained from southern Turkey 11 and in Iran, with the highest percentage in August. 14 In Saudi Arabia, however, higher incidence was reported in the months of May through October. 9 This is mainly due to the warm temperatures during these months that affect scorpion activity. Variations in the number of cases per year are attributed to reporting protocols that are not enforced by various health sectors in the country.
A similar pattern was observed among age groups. Amr et al. 2 showed that children were particularly at risk (48.7% of the cases were aged <16 years, and 24.7% were aged <6 years). In a study conducted on scorpion sting encounters in Fidan, a small village in Wadi Araba, with a total of 36 cases, indicated that most occur at night, between 2100 and 0100 hours. 3
Cardiovascular involvement included sinus tachycardia and bradycardia, hypertension, and pulmonary edema, while arterial fibrillation, hypotension, and heart failure were less common. Neurological manifestations included irritability, hypersalivation, and excessive sweating. 12 Also, tachycardia, abdominal pain, dizziness, leukocytosis ranging from 10,450 to 20,000 WBC/mm3, dyspnea, proteinuria, and electrocardiographic evidence of myocarditis were observed among 15 scorpion sting patients referred to the Jordan University Hospital, with 2 fatalities. 2
Scorpion stings remain a medical problem in Jordan that requires more attention by health providers. Reporting of scorpion sting cases should be enforced from all healthcare centers throughout the country to better understand the epidemiology and health implications of human encounters.
Acknowledgments: We are very grateful to Dr. Kamal Hadidi, head of the National Drug and Poison Information Center, Jordan University Hospital and Mr. Salah Al Hiari, head of Department of Environmental Health, Ministry of Health, for providing data on scorpion sting cases.
Author Contributions: Study concept and design (ZSA); acquisition of the data (ZSA, RA); analysis of the data (NA, RBH); drafting of the manuscript (ZSA, NA); critical revision of the manuscript (ZSA, RBH); and approval of final manuscript (ZSA, RA, NA, RBH).
Financial/Material Support: None.
Disclosures: None.
