Abstract
Cancer-related gastrectomy can cause post-gastrectomy syndrome, which includes weight loss, dumping syndrome, and reflux esophagitis and negatively affects the quality of life. Comprehensive and individualized patient management is required; however, there is a limit to Western medicine's ability to treat these symptoms. Kampo, a traditional Japanese medicine, adapts treatments to each individual's symptoms and constitution. We treated a 68-year-old male patient with post-gastrectomy syndrome using senpukukataishasekito, a Kampo medicine. He was diagnosed with Stage II-A gastric cancer at age 66 years and underwent a laparoscopic, pylorus-preserving gastrectomy followed by chemotherapy for 13 months. He visited our clinic for chemotherapy-related fatigue, postsurgical weight loss, and limb numbness. He was prescribed both hachimijiogan and hochuekkito. At the second visit, he complained of stomach discomfort, so we prescribed senpukukataishasekito. As his stomach function improved, his body weight increased and his fatigue decreased. We suggest that senpukukataishasekito may be an effective treatment for post-gastrectomy syndrome.
Introduction
The number of patients with cancer has been increasing worldwide. In Japan, gastrointestinal cancer is the leading type of cancer among men. 1 With developments in therapeutic technique and medicines, patients’ long-term survival has increased. After gastrectomy, however, various gastrointestinal dysfunctions such as acid reflux, regurgitation, and anorexia persist, inducing weight loss and impairing postoperative quality of life (QOL). This is known as post-gastrectomy syndrome. 2 Western-based medical treatment of post-gastrectomy syndrome includes acid secretion inhibitors, gastrointestinal promotility agents, and meal instructions. 2 However, because of the variable and subjective nature of these symptoms, there are limitations to Western medicine–only treatment. Comprehensive and individualized management to improve QOL in patients with cancer is vital.
Kampo is a form of traditional medicine practiced in Japan, adapted from ancient Chinese herbal medicine. It is characterized by treatments that are adapted to each individual's symptoms and constitution. Many Kampo formulas have been used for centuries to effectively treat symptoms such as fatigue, weight loss, and appetite loss. It has been reported that the Kampo herbal formulas rikkunshito and daikenchuto are effective treatments for post-gastrectomy appetite loss, weight loss, diarrhea, constipation, and other symptoms3,4 and that hochuekkito and juzentaihoto improve QOL of cancer patients.5,6 Senpukukataishasekito is traditionally used in Japan for gastrointestinal dysfunction in patients with gastric and esophageal cancer, but few case reports exist. Herein, we report a case of successful treatment of post-gastrectomy syndrome with senpukukataishasekito following the failure of other Kampo treatments.
Presenting Concerns
The patient was a healthy, married 68-year-old man who neither consumed alcohol nor smoked. In July 2010, an upper gastrointestinal endoscopy revealed type 0- IIc lesions according to Japanese classification of gastric carcinoma 7 in his stomach, and he underwent endoscopic submucosal dissection (ESD). Because the margins were positive, the patient underwent laparoscopic pylorus-preserving gastrectomy in September 2010. The histopathology examination revealed a type 0- II c-like advanced lesion that was a poorly differentiated ring cell carcinoma having invasion limited to the muscularis propria, ly (+), UL-IIIs, HM0, VM0, state after ESD, stage IIA, according to the Japanese Classification of Gastric Carcinoma. 7 He was administered tegafur, gimeracil, and oteracil potassium as postoperative adjuvant chemotherapy until October 2011. Although his treatment course went well with no cancer recurrence, he experienced severe fatigue and mild limb numbness following chemotherapy. He visited the Kampo clinic at Keio University Hospital, Tokyo, Japan, in May 2012.
History and Clinical Findings
There were no notable findings in the patient's family history. He was taking 24 mg of sennoside, 0.25 mg of brotizolam, and 7.5 mg of zopiclone before sleep, and 3.9 g of S· M compound powder (Daiichi Sankyo Espha Co, Ltd, Tokyo, Japan; it contains taka-diastase 300 mg, magnesium aluminometasilicate 1200 mg, sodium bicarbonate 900 mg, precipitated calcium carbonate 600 mg, Caryophylli flos [clove] 30 mg, Foeniculi fructus [fennel] 60 mg, Cinnamomi cortex [cinnamon bark] 223.5 mg, Zingiberis rhizoma [ginger] 73.5 mg, Zanthoxili fructus [zanthoxylum fruit] 3 mg, Coptidis rhizome [coptis rhizome] 150 mg, Glycyrrhizae radix [glycyrrhiza] 354 mg) after each meal. He had no allergies. He was 175 cm tall and weighed 57 kg (72 kg before surgery; minimum weight: 54 kg post-gastrectomy). His body mass index was 18.6. He had a body temperature of 97.7° F, blood pressure of 111/69 mm Hg, and a heart rate of 71 beats per minute. A blood exam showed hemoglobin of 13.0 g/dL and glycated hemoglobin of 6.2%.
Diagnostic Focus and Assessment
The patient's subjective symptoms were insomnia, fatigue, weight loss, and limb numbness. The Kampo medical findings concluded the patient had a normal physique, a strong floating and string-like pulse, a pale-red tongue with wrinkles with no coating, and dilated sublingual veins. He exhibited deficient abdominal strength, epigastric discomfort and resistance, rectus muscle tension, lower abdominal weakness, and lower abdominal muscle tension. Cold pattern, qi deficiency pattern, and kidney qi deficiency pattern were diagnosed based on Kampo findings.
Therapeutic Focus and Assessment
The patient was first prescribed hochuekkito (EK-41, Kracie Pharma, Ltd, Tokyo, Japan) and hachimijiogan (TJ-7, Tsumura & Co, Tokyo, Japan) (Figure). Hochuekkito and rikkunshito are variations of shikunshito. Hochuekkito is used for treating qi deficiency pattern and fatigue, and hachimijiogan is used for cold and kidney qi deficiency and limb numbness. The herbal components of the formula are listed in the Table. One month after the first visit, the insomnia had improved and the patient no longer needed hypnotic treatment; however, he complained of a mild bitter taste in his mouth upon waking. We discontinued hachimijiogan as we thought this was caused by the Rehmanniae radix (rehmannia root) in hachimijiogan; this alleviated the symptom. In July 2012, the patient complained of a moderate degree of abdominal fullness, gastric pain after eating, and gastric acid reflux. We thought it was caused by the Zingiberis rhizoma (ginger) in hochuekkito and prescribed instead a decoction of shikunshito without Zingiberis rhizoma, but the symptoms persisted. In August 2012, we changed the prescription to senpukukataishasekito, which is traditionally used for gastrointestinal dysfunction in patients with gastric and esophageal cancer and weaker constitutions. An upper endoscopic examination revealed no abnormalities apart from reflux esophagitis in September 2012. Senpukukataishasekito contains the following drugs in raw form: Pinelliae tuber, 5 g; Inula japonica thumb (dried capitate parts of Inula britannica L subsp japonica Kitamura), 3 g; hematite, 3 g; Zizyphi fructus (jujube), 3 g; Ginseng radix (ginseng), 2 g; Glycyrrhizae radix (glycyrrhiza), 2 g; and Zingiberis rhizoma (ginger), 0.5 g per day. A decoction of these drugs was divided into 3 portions. These herbs included in shikunshito without Zingiberis rhizoma and senpukukataishasekito were products of Uchida Wakanayaku Ltd, Tokyo, Japan.
Follow-Up and Outcomes
Despite the lack of success with other medications, after 1 month of treatment with senpukukataishasekito, the patient's abdominal fullness and gastric pain symptoms improved; after 3 to 4 months, both his gastrointestinal discomfort and his fatigue were reduced. His appetite also improved, and he gained 3 kg. At his initial visit, activities lasting longer than 1.5 h were impossible owing to severe fatigue; 1 year post-treatment, he was able to travel overseas for 2 weeks. In February 2014, he continued to experience concurrent mild limb numbness and mild gastric acid reflux; we added 3 g of Aurantii nobilis pericarpium (citrus Unshiu peel, Uchida Wakanayaku Ltd, Tokyo, Japan) and 1 g of Processi aconiti radix (aconitie root, Uchida Wakanayaku Ltd, Tokyo, Japan) per day to his treatment, which reduced his symptoms. By 2 years post-treatment, he was able to enjoy golf outings 2 or 3 times a month. He continued taking the same formula with no serious adverse effects.
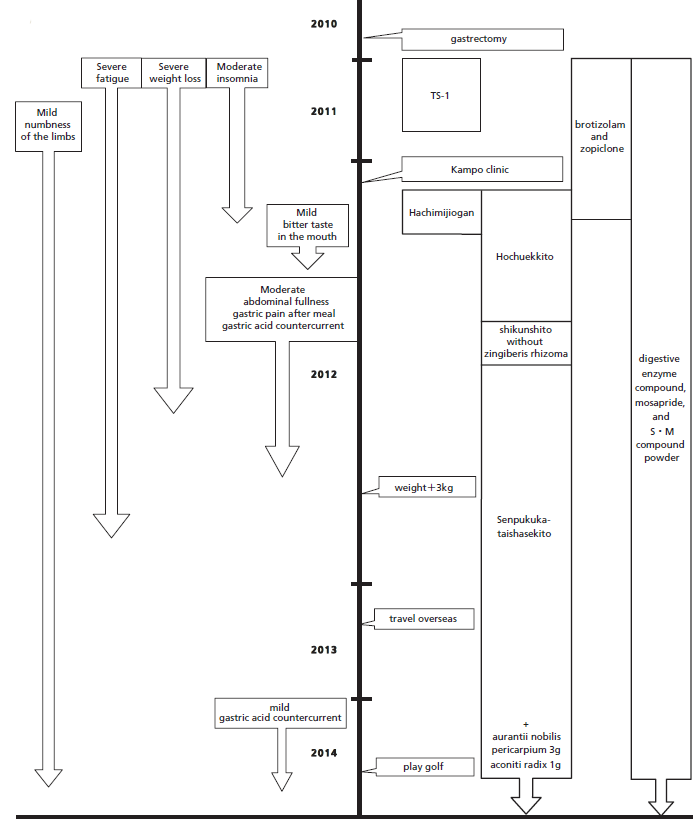
Timeline of interventions and outcomes.
List of the Herbal Components of Hochuekkito, Rikkunshito, Shikunshito, and Senpukukataishasekito

List of the Herbal Components of Hachimijiogan

Discussion
We presented a case suggesting that senpukukataishasekito might have beneficial effects on patients with post-gastrectomy syndrome following cancer treatment. We initially prescribed hachimijiogan and hocyuekkito, but the patient complained of a bitter taste in the mouth, thought to be symptoms of gastric dysfunction caused by the Rehmanniae radix in hachimijiogan. However, his insomnia improved with that treatment, and he no longer required hypnotics. As shikunshito is the base of hochuekkito and rikkunshito, hochuekkito and rikkunshito represent variations of shikunshito. Hochuekkito is useful for fatigue and QOL improvement in patients with cancer, 5 and shikunshito is useful for gastrointestinal dysfunction and for patients with weaker constitutions. In our case, gastrointestinal discomfort occurred with hochuekkito, which we initially attributed to the Zingiberis rhizoma in hochuekkito. We changed the prescription to shikunshito without Zingiberis rhizoma, but the symptoms persisted until the prescription was changed to senpukukataishasekito. We concluded the symptoms were not caused by Zingiberis rhizoma but rather that the previous medicines were not appropriate for this patient.
The structure of senpukukataishasekito is characterized by the raw drugs senpukuka and taishaseki. Senpukuka is the dried capitate parts of Inula britannica L subsp japonica Kitamura (compositae) or closely related plants of the same genus. An old medical text claimed this drug could loosen pressure in the epigastrium and treat hiccups. 8 Taishaseki is soft hematite in earth form, which mainly consists of iron oxide, and is said to supplement blood, constrict veins, and stop bleeding. 8 The effects of the other raw drugs were as follows: Pinelliae tuber to treat gastric heaviness and vomiting; Zizyphi fructus for chest and abdominal pain and cough; Ginseng radix to ease chest pressure and treat poor appetite, abdominal pain, and diarrhea; Glycyrrhizae radix for anti-gastric inflammation, analgesic, expectorant, and anti-tussive effects; and Ingiberis rhizoma for its diaphoretic and antidiarrheal effects. 8 Shanghanlun at the end of the 2nd century CE, described senpukukataishasekito treatment as follows: “Although the sweating, vomiting or purgation method of treatment has relieved the cold damage, there still remained epigastric discomfort and hiccups, senpukukataishasekito should be given.” 9 Keisetsu Otsuka, a Japanese Kampo physician active in the 1900s, argued that senpukukataishasekito can be used postoperatively in patients with gastric cancer or gastric ulcers. 9 It can also be used also for epigastric discomfort, hiccups, and constipation. The target of this medicine is for a weaker type than shikunshito, and our patient exhibited deficient abdominal strength. He also suffered from epigastric discomfort that hochuekkito and shikunshito could not treat, and thus we chose senpukukataishasekito, which proved effective.
Nutritional changes after gastrectomy result from several processes and can lead to micronutrient deficiencies and food intolerance, which cause significant weight loss. Post-gastrectomy conditions, such as dumping syndrome and alkaline reflux gastritis, may intensify these losses and further hinder nutritional recovery.2,10 Further, reduced strength due to weight loss can limit the ability to work, and thus weight loss after gastric cancer resection represents an important QOL measure. Being underweight can potentially lead to a poorer prognosis or an inability to tolerate chemotherapy. 10 According to Aoyama et al, weight loss after gastric cancer surgery is caused by 2 mechanisms 10 : first, storage functions are lost due to diminished stomach size; second, it affects ghrelin, a hormone secreted in the stomach that regulates several physiological activities, including appetite stimulation. 11 It has been reported that ghrelin secretion declines after gastric cancer surgery and that serum ghrelin levels are low in the early postoperative stages. 11 Therefore, the primary cause of weight loss after gastric cancer surgery may be reduced food intake due to decreased ghrelin. 9 While ghrelin replacement therapy is a prime therapeutic candidate, the Kampo formula rikkunshito has received attention for its ability to increase ghrelin secretion. 3 Among its ingredients, Aurantii nobilis pericarpium, Zingiberis rhizoma, and Atractylodes lancea rhizoma have been reported as increasing ghrelin signals. 3 Senpukukataishasekito contains Zingiberis rhizoma, which may stimulate ghrelin secretion. However, it is important to choose the appropriate medicine for the patient's constitution, as some may not tolerate Zingiberis rhizoma.
Due to the variable and subjective nature of post-gastrectomy syndrome symptoms, comprehensive and individualized management is necessary. Kampo is characterized by treatments that are adapted to each individual's symptoms and constitution, making it possible to adjust treatment by adding other raw drugs and modifying quantities. For our patient, we added aurantii nobilis pericarpium and processi aconiti radix to his treatment, as the former is effective for gastric inflammation and the latter is effective for numbness, and his symptoms were gradually reduced. Kampo offers the flexibility to find a matching formula for patients with various medical conditions and therefore allows us to individualize treatment.
In this report, we demonstrated that senpukukataishasekito may be an effective treatment for post-gastrectomy syndrome, by both reducing fatigue and treating gastrointestinal dysfunction. It represents a new understanding of senpukukataishasekito, which is usually used to treat gastrointestinal dysfunction. It also improved patients’ post-gastrectomy QOL. While basic science data for senpukukataishasekito treatment is not yet available, further research is needed to examine the effects of its ingredients on the treatment of post-gastrectomy syndrome.
Patient Consent
The patient gave written permission for the publication of this case report.
