Abstract
Purpose
To assess feasibility and health economic benefits and costs as part of a pilot study for a nurse-led, psychoeducational intervention (NPLI) for prostate cancer in order to understand the potential for cost effectiveness as well as contribute to the design of a larger scale trial.
Methods
Men with stable prostate cancer post-treatment were recruited from two cancer centres in the UK. Eighty-three men were randomised to the NLPI plus usual care or usual care alone (UCA) (42 NLPI and 41 UCA); the NLPI plus usual care was delivered in the primary-care setting (the intervention) and included an initial face-to-face consultation with a trained nurse, with follow-up tailored to individual needs. The study afforded the opportunity to undertake a short-term within pilot analysis. The primary outcome measure for the economic evaluation was quality of life, as measured by the EuroQol five dimensions questionnaire (EQ-5D) (EQ-5D-5L) instrument. Costs (£2014) assessed included health-service resource use, out-of-pocket expenses and losses from inability to undertake usual activities.
Results
Total and incremental costs varied across the different scenarios assessed, with mean cost differences ranging from £173 to £346; incremental effect, as measured by the change in utility scores over the duration of follow-up, exhibited wide confidence intervals highlighting inconclusive effectiveness (95% CI: -0.0226; 0.0438). The cost per patient of delivery of the intervention would be reduced if rolled out to a larger patient cohort.
Conclusions
The NLPI is potentially cost saving depending on the scale of delivery; however, the results presented are not considered generalisable.
Introduction
Prostate cancer incidence, internationally, has steadily increased since the latter half of the twentieth century along with the prevalence of other cancers (1). Prostate cancer survivors can expect longer survival due to earlier diagnosis and improved treatments, but can often experience physical, sexual, psychological and emotional problems, and there is evidence that current follow-up practices fail to meet these men's needs (2). There is also a significant economic burden associated with short- and long-term side effects of prostate cancer treatments (3). Previous studies in cancer survivors suggest that primary-care interventions may reduce psychological and emotional problems and thus improve overall quality of life (4, 5). It has also been evidenced that cancer patients are open to alternative forms of post-treatment follow-up outside the secondary-care setting (6). Therefore, it is suggested that a role exists in primary care for delivering follow-up, survivorship and self-management support and that primary-care-led follow-up may be acceptable to men with prostate cancer. Earlier identification of physical, sexual, psychological and emotional problems may lead to speedier remedial action, thus reducing the need for secondary and tertiary care follow-up.
The aim of the PROSPECTIV trial, a pilot randomised controlled trial, was to explore the feasibility, acceptability and effectiveness of a nurse-led psychoeducational intervention (NLPI) based in primary care, designed to promote self-management and improve health-related quality of life (HRQoL) for men with a diagnosis of prostate cancer in a post-treatment care pathway (7). The benefits, costs and cost effectiveness of the NLPI, consisting of tailored information/advice and support delivered in a primary-care setting compared with usual care alone (UCA), was evaluated. Although previous studies have reviewed the effectiveness of supportive care interventions for men with prostate cancer (8, 9), PROSPECTIV is the first trial to assess a primary-care-led intervention for men providing access to supportive care based on individual needs.
Materials and methods
The intervention
The NLPI involved an initial face-to-face consultation in the patient's own GP practice, with further follow-up tailored to patient's need (either face-to-face or telephone) and a final follow-up telephone call at 6 months. In total, 83 of the 136 patients who were eligible and invited to take part, agreed to be involved in the follow-up phase of the study; 42 men in the intervention and 41 men in the control group. The study had several objectives and the target recruitment for the pilot phase was 80 patients, as this was judged sufficient to enable the study objectives to be met (7). Two of the men in the intervention group were withdrawn from the study during the follow-up period, leaving 81 patients who were included in the health economic evaluation (10). Training for the nurse-led delivery of the NLPI arm consisted of a three-day educational programme. Five nurses attended the programme and costs were estimated for hours spent at the course by nurses and lecturer/presenter fees; accommodation, subsistence and travel costs for both nurses and lecturer/presenters; and course materials.
The knowledge and skills attained during the training programme are not expected to need any further supplementary training for at least a 36-month period, i.e., we anticipated no extra costs associated with training over 3 years but a further refresher training module may be needed after this time. This assumption was made to estimate a training programme cost per month.
Data
A range of clinical and demographic data were collected as part of the baseline assessment including age, time since diagnosis, educational achievement, employment status, marital status, ethnicity and medical treatment history. Several validated instruments were used for measuring disease-specific and generic quality of life, and are discussed in detail elsewhere (7, 10); for this analysis, we used only the generic EuroQol five-dimensions questionnaire (EQ-5D) using 5 level (EQ-5D-5L) described in detail below. The trial participants were asked to record their health service contacts related to their prostate cancer in a patient diary constructed as part of the trial. The frequency and type of health service contacts were self-recorded by patients using the diary completed at three separate time periods; 0-3 months, 3-6 months, 6-7 months. The diary also included questions on over-the-counter medication/device usage and days missed from usual activities, i.e., work and education.
Missing data were assumed missing at random. Due to the varying levels of reporting across the resource use and quality-of-life measures, as well as the small sample size and the investigative nature of the analysis, unconditional mean imputation was used to create a complete dataset for the 81 patients included in the analysis. Missing data are summarised in Supplementary Table A6 (available online at www.grhta.com).
Costs
Total resource use and total and average costs were reported over a 7-month follow-up (30 weeks) time period. Total and average costs were estimated for the intervention (training, implementation including planning, administration and contact time with the patients and nurse travel costs) based on a micro-costing exercise undertaken alongside the trial, patient-reported health resources utilised (PSA testing, contact with health-care providers and medication/devices) and patient productivity losses (time off work and usual activities) associated with sick days reported and attendance time for the intervention. Unit costs were obtained from several sources including, Personal Social Services Research Unit (PSSRU) (11), British National Formulary (12), Boots Chemist (13), NHS Electronic Tariff Database (14) and the literature (15–17). Travel costs were estimated using the AA travel car running costs for 2014/2015 for average priced car assuming 10,000 miles travelled per year (18). The cost of an employed sick day was estimated based on the median full-time gross annual earnings for men in 2014 and the cost of a sick day preventing usual activities, i.e., activities for those who are unemployed or retired, was based on the UK minimum wage rate in 2014 (19, 20). All costs were reported in 2014 (£) using appropriate adjustments for prices retrieved (21).
Effectiveness
The primary outcome measure in the cost-utility analysis was quality-adjusted survival (QAS), using the EQ-5D-5L measure to estimate utility scores across the 7-month trial period, i.e., 6 months of the intervention followed by 1 month of follow-up (22, 23). This EQ-5D-5L was administered to all patients in the intervention and control arms at baseline and after the intervention finished at 6 months. Each of the five dimensions in the EQ-5D-5L (mobility, self-care, activities, pain/discomfort, and anxiety/depression) is scored from 1 (no problem) to 5 (extreme problems), generating a profile (e.g., 11234) that can be used to calculate a single index score (3 level range: -0.594-1.000) (24). A crosswalk algorithm was used to convert the EQ-5D-5L to the 3 level (3L) values as this analysis was undertaken prior to the publication of the 5L UK tariffs (25). The EQ-5D instrument also generates a self-rating of HRQoL scored from 0 to 100 employing a visual analogue scale (VAS). The base-case analysis incorporated survival weighted by the mean EQ-5D index score across the NLPI and UCA cohorts as well as reporting the upper and lower 95% confidence intervals (CIs). The effect reported is the difference in QAS at follow-up from baseline. Scenario analysis employed weighting survival using the mean EQ-VAS score with associated upper and lower 95% CIs.
Analysis
The disaggregated impacts on costs and benefits of the introduction of the NLPI compared to UCA were analysed and reported. A deterministic within pilot cost-effectiveness analysis was also undertaken using average costs and effects across both arms; the base-case analysis adopted the healthcare payer perspective. Incremental cost-effectiveness ratios (ICERs) were estimated and reported for the base-case analysis along with a series of sensitivity and scenario analyses, including the adoption of a societal perspective. ICERs represent the change in mean cost per patient divided by the change in mean QAS per patient associated with the NLPI compared to the UCA arm across the follow-up period. Details of the scenarios adopted are described in Supplementary Table A5 (available online at www.grhta.com). In order to examine the variation in incremental cost and effect, a cost-effectiveness plane was constructed for the base-case analysis adopting a non-parametric approach and incorporating a bootstrapped sample of 1000 cost-effect pairs per trial arm.
Results
Patient-reported health services utilisation varied across trial arms and by type of health service utilised (Tab. I). Reported resource use for prostate-specific antigen (PSA) testing, discussion of treatment side effects and health services utilised were completed for 68/81 men (84%) at various time-points across the follow-up period, 37 in the intervention and 31 in the control group. However, only 58 men (72%) completed all three of the health resource-use questionnaires; 31 in the intervention and 27 in the control group. Medication and medical-device usage was based on patients who completed all three resource-use diaries and also included those who reported >0 medication and medical-device usage across two of the three resource-use diaries, i.e., 33 in the intervention and 31 in the control groups (79% completed across diaries). The reported days unable to carry out usual activities had the lowest completion rate at 49%. This is presumably because in most cases men's usual activities were not affected. Reported HRQoL using the EQ-5D-5L and the EQ-VAS was completed for 71/81 men (88%) included in the economic evaluation for baseline and 6-month follow-up, 37 in the intervention and 34 in the control group.
Frequency of health services usage (HSU) reported *
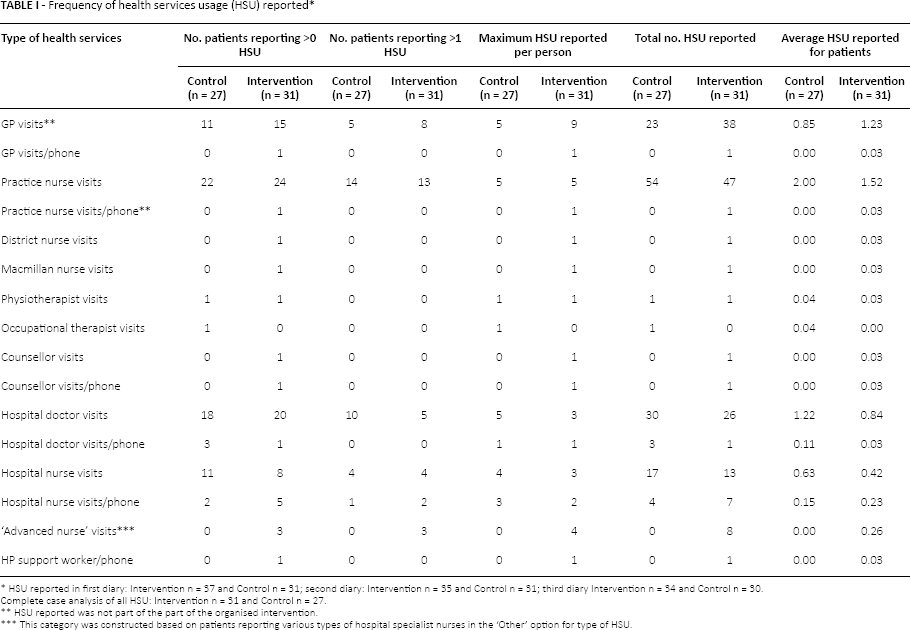
Complete case analysis of all HSU: Intervention n = 31 and Control n = 27.
HSU reported in first diary: Intervention n = 37 and Control n = 31; second diary: Intervention n = 35 and Control n = 31; third diary Intervention n = 34 and Control n = 30.
HSU reported was not part of the part of the organised intervention.
This category was constructed based on patients reporting various types of hospital specialist nurses in the ‘Other’ option for type of HSU.
The average number of visits to a general practitioner throughout the follow-up period was higher for the patients who received the NLPI, 1.23 visits (n = 31), compared to the UCA arm, 0.85 visits (n = 27). In contrast, the average number of outpatient visits were higher in the UCA arm, 1.22 visits (n = 27), compared to the NLPI arm, 0.84 (n = 31). The UCA cohort also reported higher practice-nurse visits than the cohort who received the NLPI, average visits 2 (n = 27) compared to 1.52 (n = 31), respectively.
The average number of patients treated across the five nurses was used to estimate the cost of the NLPI per nurse per patient, £210 (Tab. II). One nurse treated double the average number of patients, i.e., 16 patients compared to an average of 8 overall per nurse; this alternative estimate of £140 per patient, was used to inform the sensitivity analysis as it was thought this represented the overall potential of each nurse across the 7-month follow-up period. The cost associated with nurse travel time and mileage was also included in the overall cost of the intervention. Time spent receiving the intervention was recorded for all patients. This was used to inform productivity losses of the patients associated with average lost earnings due to attendance of the intervention estimated at £19 (both face-to-face and phone consultations included), i.e., the opportunity cost of attendance (see Supplementary Table A1, available online at www.grhta.com). These indirect patient costs were included in the scenario analyses, which incorporated a societal perspective.
Intervention costs — nurse training and implementation
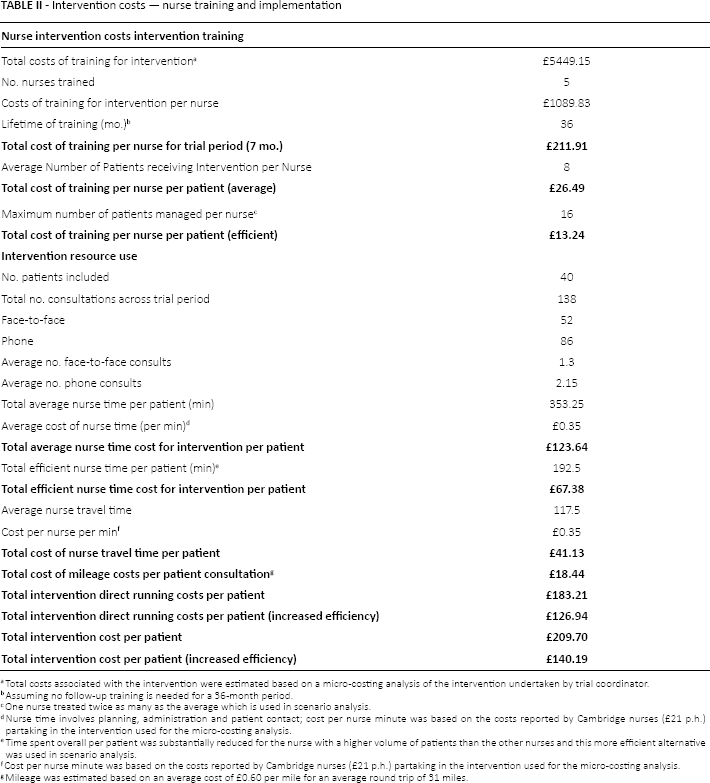
Total costs associated with the intervention were estimated based on a micro-costing analysis of the intervention undertaken by trial coordinator.
Assuming no follow-up training is needed for a 36-month period.
One nurse treated twice as many as the average which is used in scenario analysis.
Nurse time involves planning, administration and patient contact; cost per nurse minute was based on the costs reported by Cambridge nurses (£21 p.h.) partaking in the intervention used for the micro-costing analysis.
Time spent overall per patient was substantially reduced for the nurse with a higher volume of patients than the other nurses and this more efficient alternative was used in scenario analysis.
Cost per nurse minute was based on the costs reported by Cambridge nurses (£21 p.h.) partaking in the intervention used for the micro-costing analysis.
Mileage was estimated based on an average cost of £0.60 per mile for an average round trip of 31 miles.
Total and average costs were estimated for PSA testing, health-services usage, medications and medical-device usage reported across both trial arms. The health services unit costs are presented in Supplementary Table A2 (available online at www.grhta.com) and include the assumed duration of the visit. Average health-services usage was based on the number of patients who fully completed diaries across the 7-month follow-up, i.e., 31 in the intervention and 27 in the control groups (Tab. III). The average cost of health-service usage was £139 and £128 for the NLPI arm and the UCA arm, respectively; the cost difference across the 7-month period being approximately £11 higher in the NLPI arm. The average cost per patient of medications reported by patients in the NLPI arm was double that of the UCA arm, £53 compared to £25 per patient, respectively (Tab. IV). The largest proportion of cost associated with reported medication usage in both groups was for the treatment of sexual dysfunction issues. Similar proportions of men reported usage across the four sub-groups reviewed (medications related to sexual dysfunction, urinary problems, digestive/bowel problems and anxiety/sleeping problems); however, the reported duration of medication usage was far greater in the cohort receiving the NLPI. Medical device usage was minimal and varied across both trial arms (see Supplementary Table A3, available online at www.grhta.com).
Cost analysis of health services usage
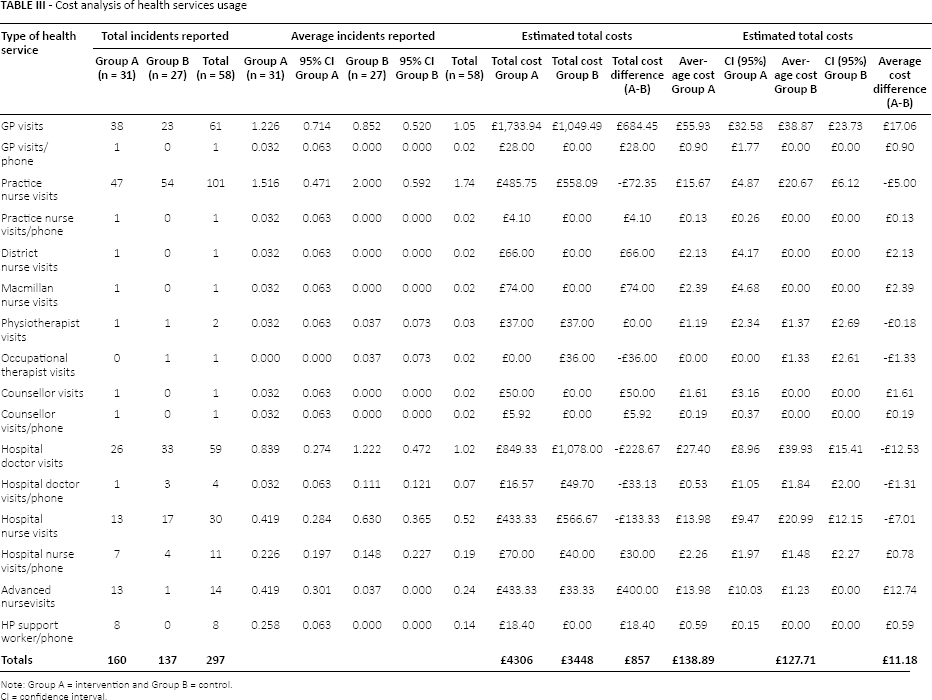
CI = confidence interval.
Analysis of costs for reported medication usage
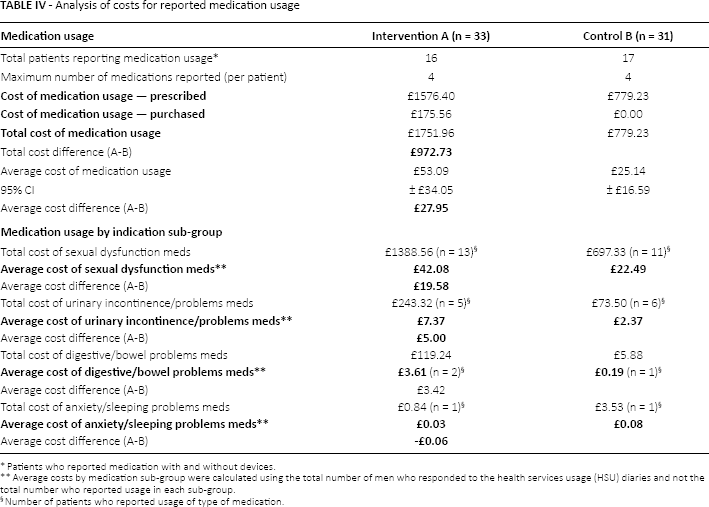
Patients who reported medication with and without devices.
Average costs by medication sub-group were calculated using the total number of men who responded to the health services usage (HSU) diaries and not the total number who reported usage in each sub-group.
Number of patients who reported usage of type of medication.
Average patient-reported sick days, i.e., patients reported being unable to undertake ‘usual activities’, were estimated based on the number of men in each trial arm who reported sick days in at least two of the three diaries collected; 24 in the intervention and 16 in the control group. Overall, there were 66 sick days reported across all patients for the 30-week follow-up period; 57 in the NLPI cohort and 9 in the UCA arm (see Supplementary Table A4, available online at www.grhta.com). An outlier was identified in the cohort receiving the NLPI and was included (in the base-case analysis) and excluded in separate scenario analyses, which included a societal perspective.
The EQ-5D-5L instrument highlighted a reduction in HRQoL across both trial arms in the follow-up period; difference in mean utility from baseline for the intervention group = -0.023 (standard deviation [SD]: 0.15) and for the control group = -0.034 (SD: 0.16) (9). The NLPI cohort yielded a smaller reduction in mean utility over the time-period of the trial, i.e., approximately 32% lower utility decrement than the UCA cohort. The EQ-5D VAS score improved in the cohort that received the NLPI across the follow-up period (+3.61) while the UCA arm highlighted a drop in the reported EQ-5D VAS mean score (-0.72); the difference in HRQoL across both arms was not statistically significant at the 95% confidence level.
The economic evaluation was undertaken to assess the extent to which variability in costs and effects impacted on the ICER. In the base-case analysis the deterministic ICER was £22,950 (95% CI: dominated, £4,850) and at a UK NICE willing-to-pay threshold of £20,000, this would not be considered cost-effective. The incremental effect, i.e., the difference in utility decrement for the intervention relative to the control, was positive at 0.0106 with uncertainty highlighting a positive impact, as high as 0.0438 for the intervention and a negative effect, a higher decrement for the intervention group, at -0.0226; therefore, the effectiveness of the intervention is inconclusive. The cost-effectiveness plane for the base-case analysis (Fig. 1) illustrates the high variability in effect difference with equal proportions of cost-effect pairs present predominantly in the North-East and North-West quadrants. The probability that the NPLI was cost-effective at £20,000 was 45% and at £50,000 was 53%. The economic analysis highlighted high variation in cost-effectiveness estimates based on the assumptions adopted in the scenarios assessed; in particular, the use of the EQ-5D-5L utility score versus the EQ-5D VAS score was one of the main drivers of uncertainty in the results. The assumptions adopted for the base-case analysis and the series of scenario analyses are outlined in Supplementary Table A5. The base-case analysis was not considered cost effective due to inconclusive significance in the incremental effect contributing to wide CIs, i.e., the uncertainty ranges from positive to negative (Tab. V and Fig. 1). The mean incremental cost associated with the NLPI ranges from £173 to £346 across the series of analyses undertaken. Drivers of variation in cost include the intervention training and delivery costs as well as nurse travel costs, all of which would reduce with greater efficiency in delivery. ICERs ranged from £40 per QAS (95% CI: £26, £67) to £32,604 per QAS (95% -£16,976, £7,190 [i.e., dominated]) and due to the uncertainty around the incremental effect, all scenarios employing the EQ-5D-5L to estimate QAS were dominated by the UCA arm. The two scenarios that employed the EQ-5D VAS score to estimate QAS suggested the NLPI to be cost effective.
Cost-effectiveness analysis results
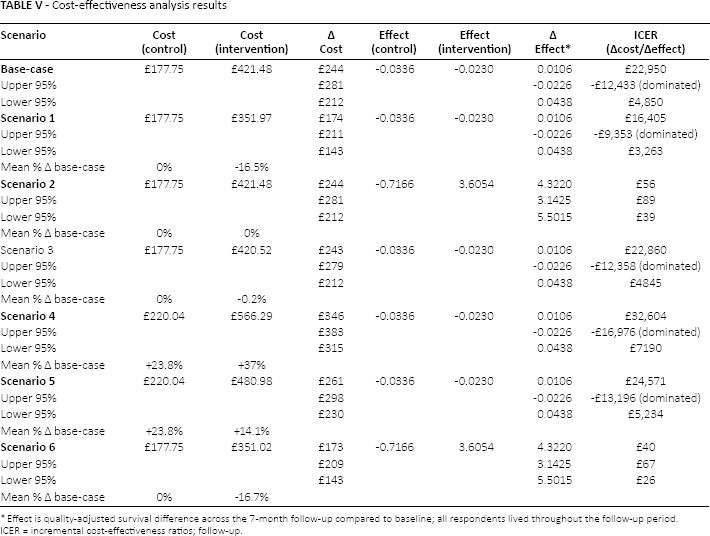
Effect is quality-adjusted survival difference across the 7-month follow-up compared to baseline; all respondents lived throughout the follow-up period.
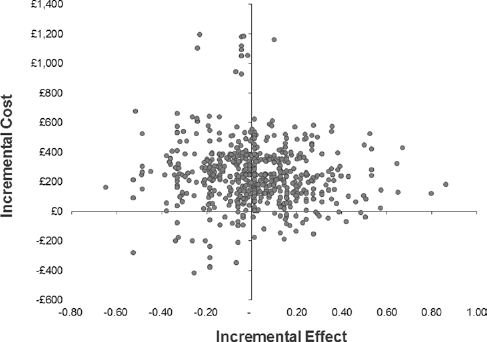
Cost-effectiveness plane for base-case analysis.
Discussion
The purpose of the economic evaluation embedded within the pilot study was to assess the feasibility of resource use and quality-of-life instruments, variations in reporting, analysis of costs and outcomes and to examine the variation therein. Undertaking a preliminary cost-utility analysis facilitated a deeper understanding of the drivers of uncertainty in the NLPI, which will assist with designing the economic evaluation element of the larger trial. Although the base-case ICER is £22,950 (95% CI: dominated, £4,850) the economic evaluation highlighted considerable variation in the incremental cost and effect of the NLPI; in particular, the uncertainty around the effect suggested no significant incremental effect. The extent of the variation, as indicated by the 95% CIs, can be directly related to the small sample size, the limited follow-up period and potential sensitivity issues with the outcome measure for this patient cohort. While the data were not fully complete, the response rates were high suggesting that patients were interested and willing to respond to the resource-use questionnaires, even over an extended period of seven months (10).
Resource use reported in the patient diaries varied across the trial arms and the type of resources utilised. The number of patients reporting more than one health-service resource used across both arms was comparable; however, the categorisation of the resource use differed, with patients receiving the NLPI being represented by a higher number of primary-care visits while the UCA group reported a higher number of secondary-care visits. Thus, costs associated with average resource use for patients undergoing the NLPI in primary care were higher overall but of the total, secondary-care resource use was lower than that in the UCA arm.
The response rate for patients reporting inability to undertake usual activities was the lowest across all data collected, at 49%. We have identified mechanisms to refine this part of the patient diary to increase completion and distinguish between “not applicable” and “incomplete”. The analysis of the productivity losses highlighted an outlier in the NLPI who reported 42 days sick within the trial period; this patient was included in scenario 4 and dropped in scenario 5. Even with the exclusion of the outlier, sick days were higher in the NLPI arm compared to the UCA arm, 15 and 9 days, respectively (n = 39). The increased productivity losses associated with the NLPI arm is mainly due to the small sample size and is more than likely unrelated to the intervention; this will be explored further in the next phase of the trial.
Increased potential for cost effectiveness was indicated when addressing the impact of higher volumes of patients being treated with the intervention using a more efficient nursing staff model (Scenario 1). Therefore, with greater staff experience and a longer follow-up period, there would be a likely reduction in the intervention-related costs. Additionally, nurse travel costs associated with delivery of the intervention would substantially decrease if this intervention were to be offered more widely as nurses in the locality would be trained in delivery of the intervention. Modes of training delivery of the intervention, including online-based initial and continued training, could further reduce the intervention-related costs providing a more efficient delivery model.
The follow-up period for this study was only one month beyond the end of the intervention period, which may not have been sufficient to realise the true benefit of the intervention on reducing costs and improving HRQoL. Costs associated with longer-term treatment-related side effects may well be alleviated due to access to the NLPI. For example, a significant increase in men discussing issues in relation to bowel problems compared to the UCA group was reported; these problems, if left unresolved, may lead to complications over time resulting in higher resource use as well as having implications for self-reported HRQoL.
Therefore, the NLPI may also be acting as a mechanism to diagnose otherwise unrecognised complications that would improve HRQoL and provide cost savings over time. Patients who received the NLPI were also more likely to discuss sexual issues with their general practitioners and were in turn prescribed more medication for sexual dysfunction, potentially improving their HRQoL. The impact on HRQoL, from discussion of and seeking remedies for these types of treatment side effects, may not have been captured over the follow-up period with the generic quality-of-life instruments incorporated in the economic evaluation. In contrast to this, a significantly higher proportion of patients who received UCA discussed PSA testing and changes in tumour growth and disease progression with their hospital consultants in an outpatient setting. There is no evidence to suggest that clinical need differed across the two trial arms and therefore it could be assumed that the NLPI may have aided men in understanding the process of disease management, facilitating them with more information on the clinical pathway and disease monitoring. Therefore, the NLPI may prove to reduce the number of outpatient appointments attended and therefore reduce associated costs over time.
The EuroQol EQ-5D measure of HRQoL did not improve over the trial time-period in either of the trial arms and no statistically significant difference in decrement was evidenced. For men within this age range in a prostate cancer post-treatment care pathway, it is not surprising that adjustments to their lifestyle impact negatively on their HRQoL. That a significant difference in decrement was not evidenced is most likely a function of the small sample size and so should be interpreted with caution. However, the cohort receiving the NLPI yielded a smaller reduction in mean utility over the time-period of the trial, i.e., approximately 32% lower utility decrement than the UCA group. This could suggest that the intervention is acting as a support, diminishing some of the overall impact of treatment and side effects on HRQoL. There is also evidence building across the literature, which suggests the EQ-5D instrument may not be sensitive enough to pick up changes in HRQoL for men with prostate cancer given the average age range of diagnosis (26, 27). Hence the EQ-5D VAS scores may be more applicable to this analysis, which, when utilised, highlighted cost effectiveness.
The men recruited to this study were on average two years post-diagnosis (10) and as such may have not yielded all potential benefits of the intervention. Intervening earlier in the care pathway may increase effectiveness and have implications for quality-of-life and cost effectiveness.
In summary, the results presented indicate that a NLPI delivered in primary care for men treated with prostate cancer may be cost effective depending on the scale of delivery, positioning along the cancer pathway and duration of follow-up; however, these results could not be considered generalisable given the design limitations of the study. The NLPI has had a positive effect on HRQoL relative to UCA and may be potentially cost saving over a longer follow-up period. A larger scale study is feasible and would aid in understanding the variation in cost-effectiveness results evidenced. At the pilot stage, we estimated that the probability that the NLPI was cost-effective at £20,000 was 45%. The addition of economic evaluation techniques to pilot and feasibility studies provides greater understanding of drivers of cost and outcome uncertainty (28). Incorporating a health economic evaluation in the PROSPECTIV pilot study provided valuable insight into the economic impact of the intervention and follow-up care across both arms and aided in identifying key drivers of variation in preliminary economic evaluation. These findings are extremely informative for all stakeholders and afford the opportunity to enhance the design of the next phase of the trial, therefore maximising efficiency of trial delivery.
Footnotes
Appendix
Members of the wider PROSPECTIV study team
We would like to acknowledge members of the wider PROSPECTIV study team for their input:
D Neal1, F Hamdy2, FM Walter3, D Weller4, C Wilkinson5, S Faithfull6, P Sooriakumaran2, C Kastner1, C Campbell4, RD Neal5, H Butcher7, M Matthews7, R Perera8
1 Department of Oncology, Cambridge University Hospitals Trust, Cambridge, CB2 0QQ, UK
2 Nuffield Department of Surgical Sciences, University of Oxford, Oxford, OX3 7DQ, UK
3 Department of Public Health and Primary Care, University of Cambridge, Cambridge, CB1 8RN, UK
4 Centre for Population Health Sciences, University of Edinburgh, Edinburgh, EH8 9AG, UK
5 North Wales Centre for Primary Care Research, Bangor University, Bangor, LL13 7YP, UK
6 School of Health Sciences, University of Surrey, Guildford, Surrey, GU2 7XH, UK
7 Service User Representatives, Resident in UK
8 Department of Primary Health Care Sciences, University of Oxford, New Radcliffe House, 2nd Floor, Radcliffe Observatory Quarter, Woodstock Road, Oxford, OX2 6GG, UK
Financial support: This work was supported by Prostate Cancer UK; grant number PG10-09-SV.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
