Abstract
Aim: To evaluate the relevance of endothelial-derived apoptotic microparticles (EMPs) with inflammatory cytokine outcomes in patients with ischaemic chronic heart failure (CHF).
Methods: A total of 154 patients with moderate-to-severe CHF were enrolled in the study. Flow cytometry analysis was used for quantifying the number of EMPs. All-cause mortality, CHF-related death, and CHD-readmission rates were examined.
Results: During a median follow-up of 2.18 years, 21 participants died and 106 subjects were hospitalized repetitively. Medians of circulating EMPs in survivor and non-survivor patient cohorts were 0.286 n/mL (95% CI = 0.271–0.309 n/mL) and 0.673 n/mL (95% CI = 0.65–0.74 n/mL) (P<0.001). There was a significantly lower concentration of sRANKL, OPG, TNF-alpha, sFAS, and sFAS ligand in the survivor patients when compared with those who met composed endpoints. The sFAS/sFAS ligand ratio in the non-survivor patient cohort was significantly higher than in the survivor cohort (P<0.001). In multivariate model EPMs, NYHA class, NT-pro-BNP, TNF-alpha, sFAS/sFAS ligand ratio, and OPG remained statistically significant for the cumulative endpoint: all-cause mortality, CHF-related death, and CHF-related readmission.
Conclusion: Increased apoptotic circulating EMPs, OPG, and FAS-sFAS ligand ratio independently predicted cumulative survival in CHF patients.
1. Introduction
Chronic heart failure (CHF) is associated with an increased risk of cardiovascular death [1]. Recent investigations suggested that inflammation might play a pivotal role in the pathogenesis of CHF through inducing endothelial dysfunction [2]. As part of this process, hyperproduction of apoptotic endothelial-derived microparticles (EMPs) are reflected in the severity of inflammation and endothelial dysfunction, which is crucial for development CHF [3]. EMPs are defined as a very heterogeneous population of submicronic vesicles that are released in response to cell activation, injury, apoptosis or inflammation [4]. EMPs represent an intercellular communication that leads to realization of an atherothrombosis and proinflammatory effect [5, 6]. Increased circulating EMPs are detectable in cardiovascular and chronic inflammation, as well as metabolic disorders (obesity, diabetes mellitus), immunity, vascular calcification, osteoporosis, and bone remodelling [7–9]. The main cytokines that regulate mobbing and differentiation of EMPs are the receptor activator of nuclear factor-κB ligand (RANKL) and its decoy receptor, osteoprotegerin (OPG), tumour necrosis factor alpha (TNF-alpha), sFas, sFas ligand [10]. While EMPs are considered to be a marker of endothelial dysfunction and tissue remodelling [11], their role as an indicator of inflammatory responses and probably as prognostic biomarkers in CHF is still not clear. The aim of this study was to prospectively evaluate the relevance of EMPs with inflammatory cytokines and outcomes in CHF patients.
2. Methods
2.1 Patient population under study
A total of 154 patients aged 48 to 62 years with ischaemic symptomatic moderate-to-severe CHF were prospectively enrolled in the study. The NYHA class of CHF was determined according current clinical guideline at discharge from the hospital. All patients were haemodynamically stable and they have given their voluntary written informed consent before participation in the study. Cumulative survival related to CHF and all-cause mortality was examined within three years. Re admission reason was defined by source document review, observation of the admitted patient or physician interview.
2.2 Methods for visualization of coronary arteries
Multispiral computed tomography angiography and/or angiographic study was performed for all patients prior to study entry on SOMATOM Volume Zoom scanner (Siemens, Erlangen, Germany) with two detector rows. After preliminary native scanning, non-ionic contrast Omnipaque (Amersham Health, Ireland) was administered for the optimal image of the coronary arteries [12]
2.3 Echocardiography and tissue Doppler imaging
Transthoracic B-mode echocardiography and tissue Doppler imaging were performed using an ACUSON scanner (Siemens, Germany). Left ventricular ejection fraction (LVEF) was measured by modified Simpson's method [13, 14]. Peak systolic (Sm), early diastolic (Em), and late diastolic (Am) myocardial velocities were measured in the mitral annulus area, followed by calculations of the velocity of early diastolic left ventricular filling (E) to Am (E/Am) ratio and to Em (E/Em) ratio.
2.4 Glomerular filtration rate calculation
Glomerular filtration rate (GFR) was calculated using the CKD-EPI formula [15].
2.5 Biomarker determination
All biomarkers were determined at baseline without a blinding procedure. To determine biological marker concentrations, blood samples were drawn in the morning (at 7–8 a.m.) into cooled silicone test tubes with EDTA. Blood samples were assayed immediately after venepuncture according to the recommendations of the manufacturer of the analytical technique used. They were centrifuged upon permanent cooling at 6,000 rpm for 3 min. Plasma was then refrigerated immediately and supernatant was stored at −70°C. Circulating NT-pro-BNP level was measured by immunoelectrochemoluminescent assay using sets by R&D Systems (USA) on Elecsys 1010 analyser (Roche, Mannheim, Germany). Serum concentrations of osteoprotegerin (OPG), sRANKL (serum receptor activator of nuclear factor-kappa B ligand TNF-alpha), sFas, sFas ligand were determined in duplicate with commercially available enzyme-linked immunosorbent assay kits (Bender Med-Systems GmbH, Vienna, Austria). A total of 100 μl serum sample was assayed in parallel to known standard concentrations for each biological marker. The mean intra-assay coefficients of variation were <10% in all cases. Concentrations of total cholesterol (TC) and cholesterol of high-density lipoproteins (HDLP) were measured by a fermentation method. The cholesterol concentration of low-density lipoproteins (LDL-C) was calculated according to the Friedewald formula (1972).
Endothelial-derived apoptotic microparticles were defined as EMPs positively labelled for CD31 and annexin V (CD31+/annexin V+) after were determined by flow cytofluorimetry by phycoerythrin (PE)-conjugated monoclonal antibody against CD31 (BD Biosciences, USA) followed by incubation with fluorescein isothiocyanate (FITC)-conjugated annexin V (BD Biosciences, USA) per HD-FACS (High-Definition Fluorescence Activated Cell Sorter) methodology. We used EDTA as an anti-coagulant for collection of the samples and centrifuged them within 15 min at 1600 g for 30 min at 20°C to pellet the cells. After this the plasma containing the MPs was carefully aspirated, collected, and incubated with 760 μL PBS/calcium buffer. The samples were then analysed on a FC500 flow cytometer (Beckman Coulter) after 400 μL annexin-V binding buffer was added. For each sample, 500,000 events have been analysed (Sigma, St Louis, MO, USA).
2.6 Statistical analysis
Statistical analysis was performed using SPSS for Windows, Version 22 (SPSS Inc., Chicago, IL, USA). The data were presented as mean (M) and error of mean (±m) or 95% confidence interval (CI), median (Me) and interquartile range (IQR). To compare the main parameters of the patient groups (subject to the type of distribution of the parameters analysed), the two-tailed Student t-test or Mann-Whitney U-test was used. To compare categorical variables between groups, Chi2 test (χ2) and Fisher's exact test were used. The factors, which could be potentially associated with circulating EMPs, were determined by logistic regression analysis. A receiver operation characteristic (ROC) curve was constructed to identify the optimal balanced cut-off points of the EMP number with the predicted value. Finding the best cut-off point of EMPs from the ROC curve was performed with a method based on choosing the value that minimizes the Euclidean distance between ROC curve and the upper left corner of obtained graph. Odds ratio (OR) and 95% CI were calculated for all of the independent predictors of survival of the patients. A calculated difference of P<0.05 was considered significant.
3. Results
In a median follow-up of 2.18 years, 21 participants had died and CHF-related death was defined in 18 patients. Additionally, 106 subjects were hospitalized repetitively due to advanced CHF (17 cases in non-survivors cohort and 89 cases in survivors cohort). Table 1 shows a general characteristic of the patients included in the study. No substantial demographic differences, as well as differences in body mass index (BMI), glomerular filtration rate (GFR), HbA1c, fasting blood glucose level, blood creatinine level, total cholesterol (TC), low-density lipoprotein cholesterol (LDL-C) and high-density lipoprotein cholesterol (HDL-C), blood pressure (BP) and heart rate (HR), E/Am and E/Em, numerous of coronary vessels with atheroma were found among non-survivor and survivor persons. The subjects who experienced the composite endpoint demonstrated a higher frequency of hypertension, adherence to smoking, more severe CHF classes, three- and multi-vessel lesion, as well as higher levels of NT-pro-BNP, and lower LVEF and mineralocorticoid receptor antagonist exposure.
General characteristics of patients participating in the study
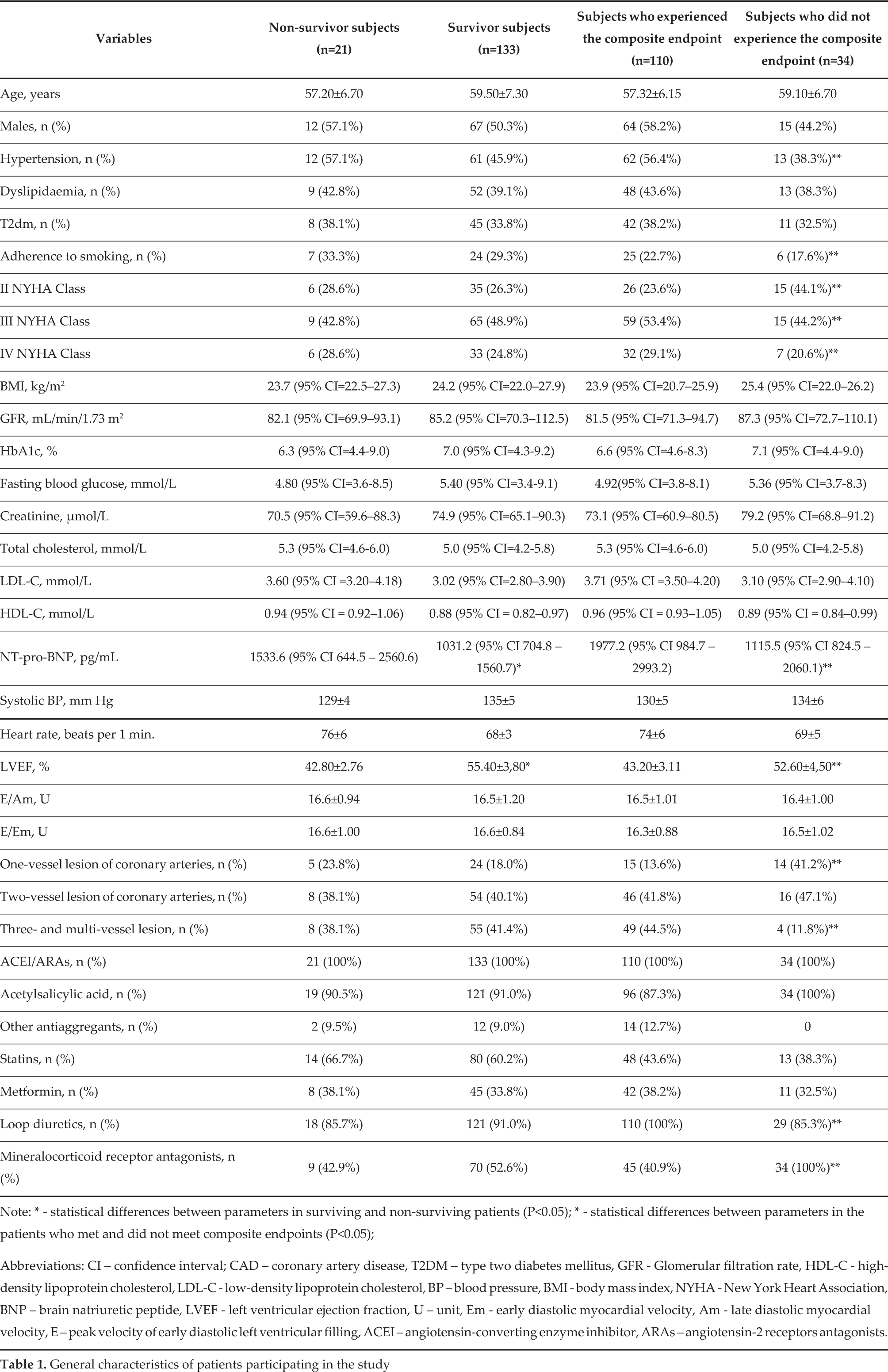
Note: * - statistical differences between parameters in surviving and non-surviving patients (P<0.05); * - statistical differences between parameters in the patients who met and did not meet composite endpoints (P<0.05);
Abbreviations: CI – confidence interval; CAD – coronary artery disease, T2DM – type two diabetes mellitus, GFR - Glomerular filtration rate, HDL-C - high-density lipoprotein cholesterol, LDL-C - low-density lipoprotein cholesterol, BP – blood pressure, BMI - body mass index, NYHA - New York Heart Association, BNP – brain natriuretic peptide, LVEF - left ventricular ejection fraction, U – unit, Em - early diastolic myocardial velocity, Am - late diastolic myocardial velocity, E – peak velocity of early diastolic left ventricular filling, ACEI – angiotensin-converting enzyme inhibitor, ARAs – angiotensin-2 receptors antagonists.
Incidence of type 2 diabetes mellitus in the patients of the two cohorts was 38.1% and 33.8% (P=0.06). The level of circulating NT-pro-BNP was statistically significantly higher in the patients who died than in those who survived. No substantial differences were found between the two cohorts with regard to drug administration.
Medians of circulating EMPs in survivor and non-survivor patient cohorts were 0.286 n/mL (95% CI = 0.271–0.309 n/mL) and 0.673 n/mL (95% CI = 0.65–0.74 n/mL) (P<0.001). The number of circulating MPs was distributed into quartiles (Q): Q1 (< 0.341 n/mL), Q2 (0.342–0.514 n/mL), Q3 (0.521–0.848 n/mL), and Q4 (> 0.850 n/mL). There was a significantly lower concentration of sRANKL, OPG, TNF-alpha, sFAS, and sFAS ligand in surviving patients when compared with those who met composed endpoints (Table 2). The sFAS/sFAS ligand ratio in the non-survivor patient cohort was significantly higher than in the survivor cohort (P<0.001).
The data show that EMP number was positively associated with NYHA class (r = 0.93, P = 0.001), sFAS/sFASl ratio (r = 0.88, P = 0.001), sFAS (r = 0.856, P = 0.001), TNF-alpha (r = 0.827, P = 0.001), OPG (r = 0.796, P = 0.001), sFASl (r = 0.589, P = 0.001), sRANKL (r = 0.692, P = 0.001), NT-pro-BNP (r = 0.689, P = 0.001), T2DM (r = 0.402, P = 0.003), multi-vessel lesion of coronary arteries (r = 0.362, P = 0.001), E/Am (r = 0.360, P = 0.001), and inversely associated with LVEF (r = −0.496, P = 0.001), eGFR (r = −0.408, P = 0.003), and HDL cholesterol (r = −0.221, P = 0.002). No significant association between levels of circulating EMPs with fasting plasma glucose, HbA1c, means systolic and diastolic BP, and medications for both cohorts of the patients was found.
The optimum balance between the sensitivity and specificity cut-off point for EMP number in circulation was 0.514 n/mL (Figure 1). The area under the curve was 0.913 (95% CI = 0.863–0.962), and sensitivity and specificity were 89.6% and 69.7% respectively. The optimal balanced sensitivity and specificity of EMP cut-off point level for other clinical outcomes in the studied patient population are presented in Table 3.
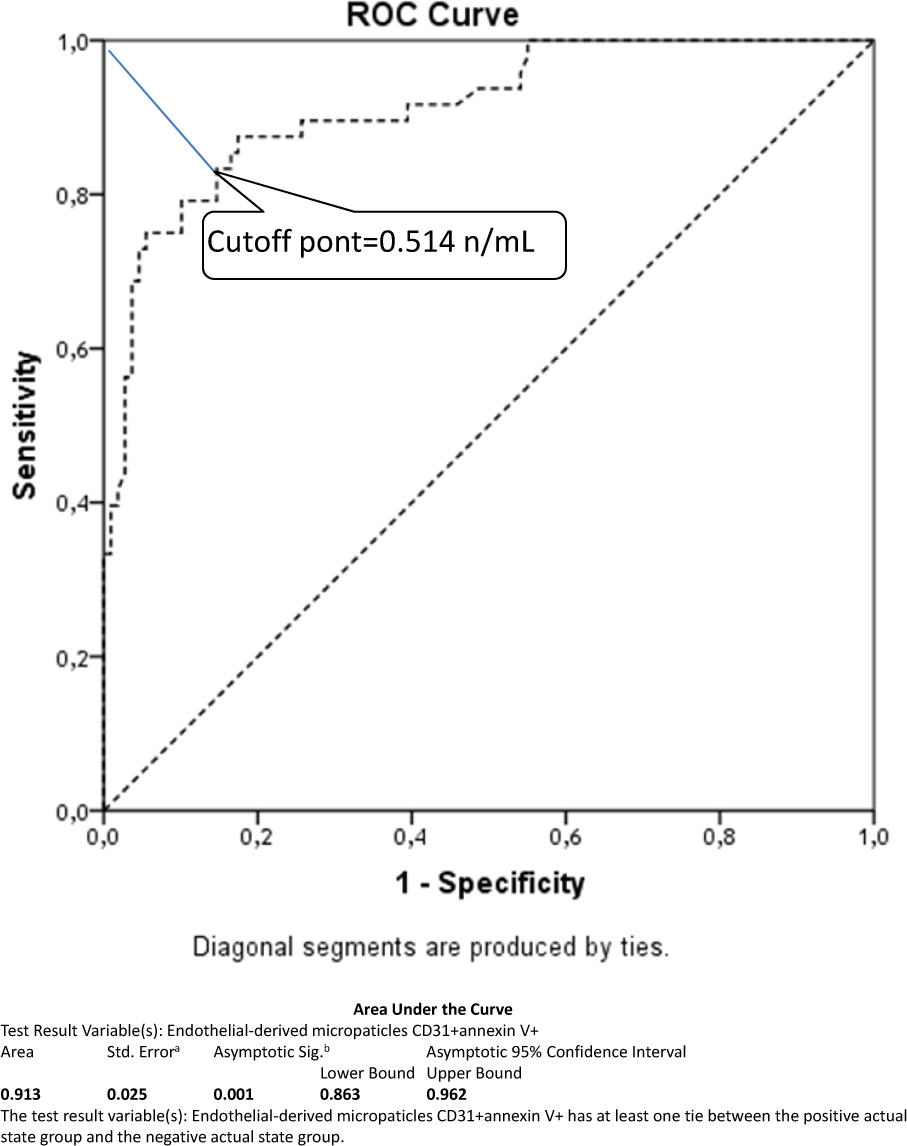
Reliability of the model included EMP number for cumulative survival in the patient population of the study. Results of ROC analysis. The figure shows the ratio of sensitivity and specificity for optimal predicted number of EMPs.
Circulating levels of EMPs, TNF-alpha, sRANKL, OPG, sFAS, and sFAS ligand in both cohort patients
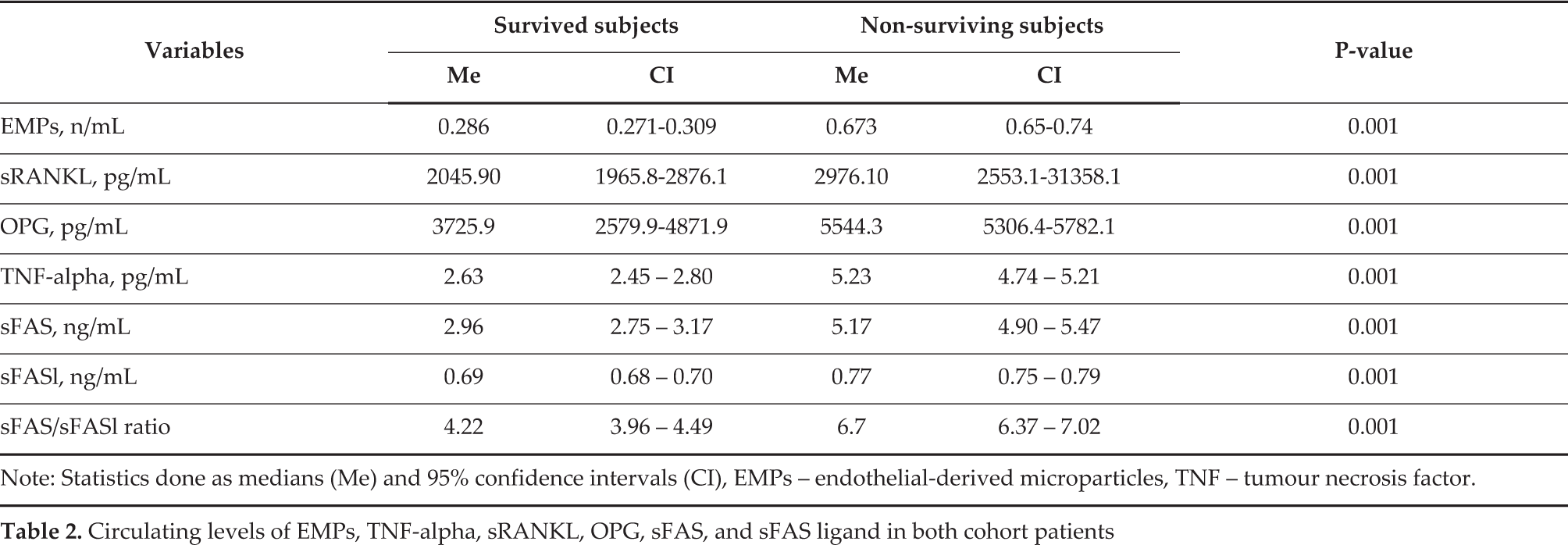
Note: Statistics done as medians (Me) and 95% confidence intervals (CI), EMPs – endothelial-derived microparticles, TNF – tumour necrosis factor.
The optimal balanced sensitivity and specificity of EMPs for clinical outcomes in the patient population studied. Results of receiver operation characteristic analysis.
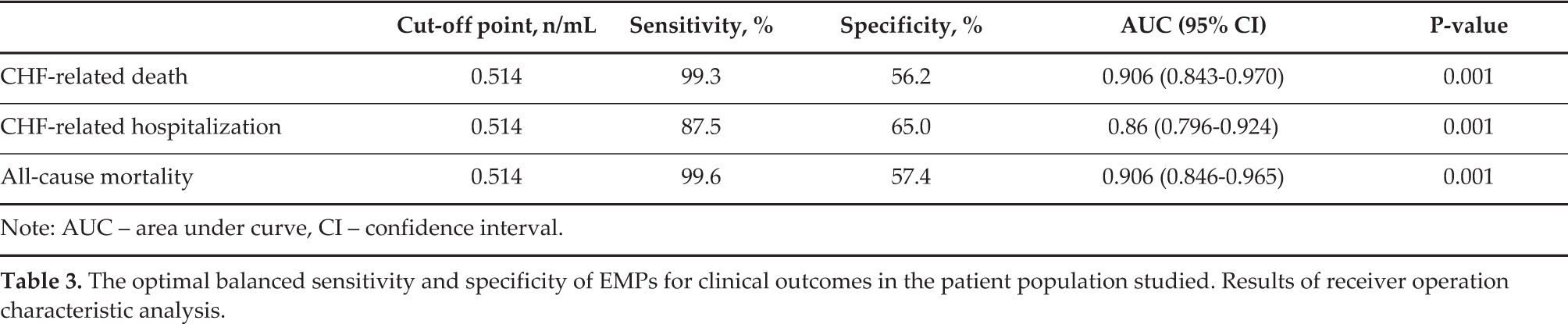
Note: AUC – area under curve, CI – confidence interval.
For all occasions the model was robust, and provided significant results using the optimal cut-off point of EMPs.
A significant divergence of Kaplan-Meier survival curves in patients with high quartiles of EMPs (numbers Q3 and Q4) when compared with low quartiles of the biomarker (Q1 and Q2) was found (Figure 2). The curve's divergence of event accumulation reached statistical significance at 50 weeks of the observation period (P<0.001).
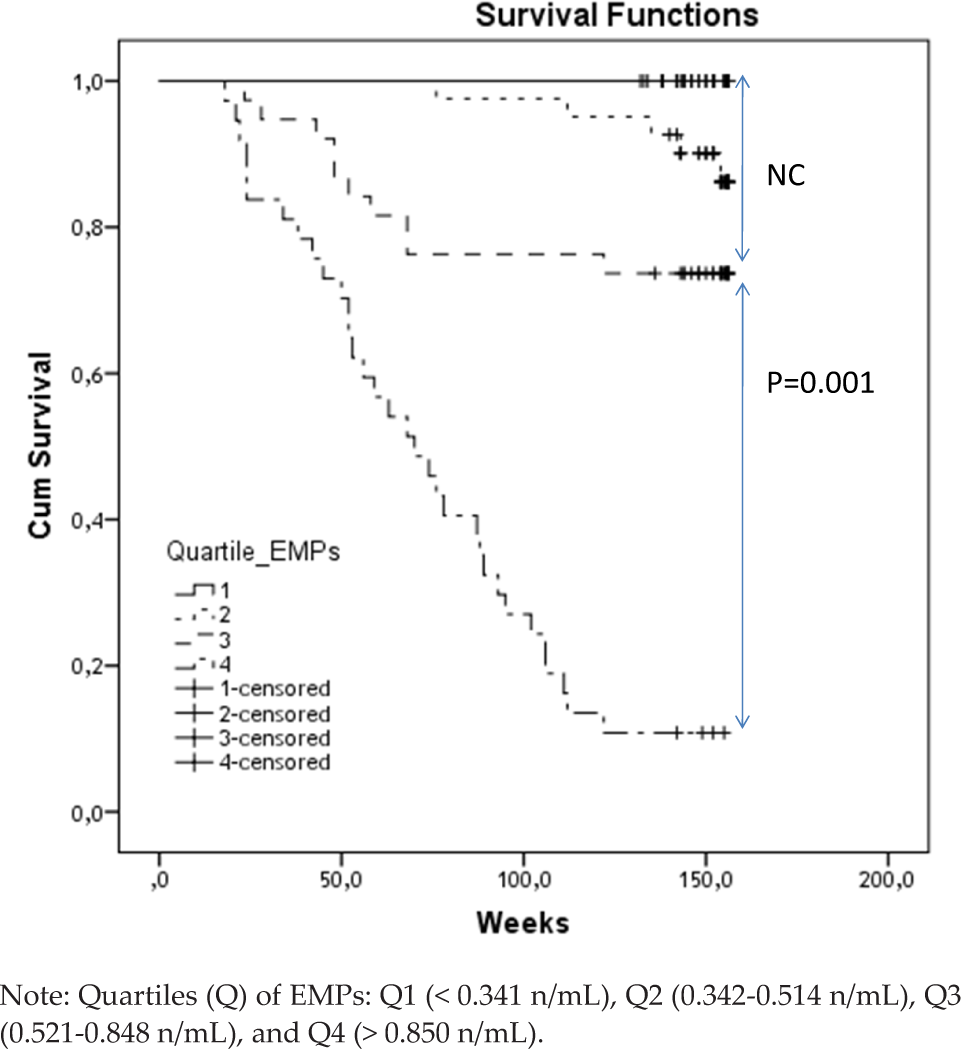
The divergence of Kaplan-Meier survival curves for patient cohorts dependent on quartiles of EMPs
Univariate and multivariate logistic regression were used to assess whether any combination of assays was able to better discriminate between survivors and non-survivors. In univariate logistic regression analysis, the main factors independently related to cumulative endpoints were EPMs, OPG, NT-pro-BNP, NYHA class, TNF-alpha, sFAS/sFAS ligand ratio, decreased LVEF (less 45%), and T2DM (Table 4). In multivariate model EPMs, NYHA class, NT-pro-BNP, TNF-alpha, sFAS/sFAS ligand ratio, and OPG remained statistically significant for the cumulative endpoint: all-cause mortality, CHF-related death, and CHF-related readmission.
Predictors of three-year all-cause mortality, CHF-related death, and CHF-related readmission
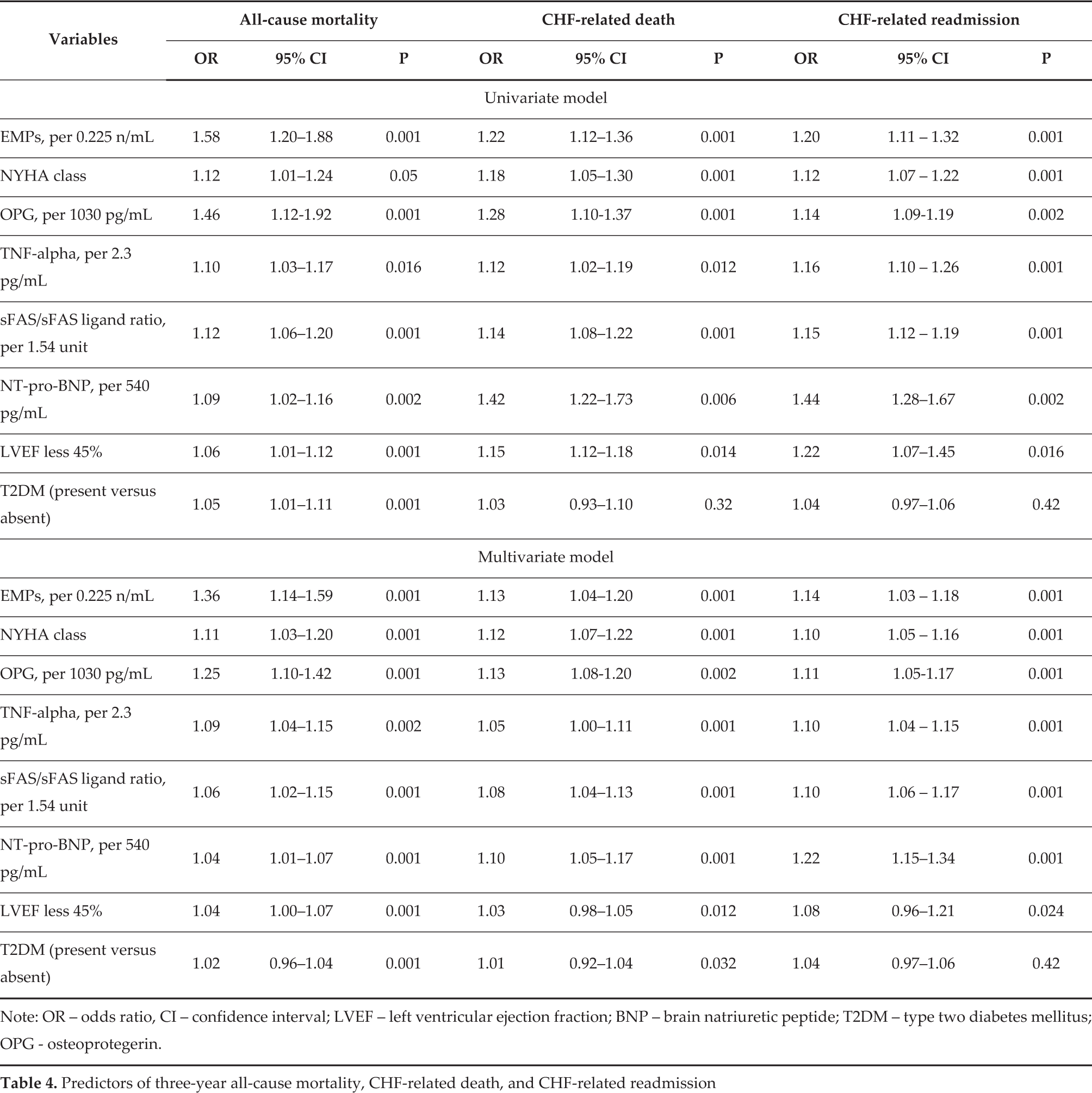
Note: OR – odds ratio, CI – confidence interval; LVEF – left ventricular ejection fraction; BNP – brain natriuretic peptide; T2DM – type two diabetes mellitus; OPG - osteoprotegerin.
Thus, we suggested that EMCs, OPG, FAS-sFAS ligand ratio remained statistically significant predictors for cumulative survival in CHF patients.
4. Discussion
The endothelium is one of the main targets of circulating EMPs; hence, EMPs have been considered as biomarkers of vascular injury, inflammation and stage of progression of cardiovascular disease [17–19]. In fact, serum RANKL, OPG, Fas ligand (FasL), and natriuretic peptides are well-established mutually related biomarkers of CHF, reflecting several faces of the pathogenesis of disease [20]. It is well known that apoptosis or programmed cell death may induce through bound FASl with its membrane receptor and this process promotes impairing survival of endothelial cells, although solubilized form (sFasL) of FAS ligand loses its apoptotic activity after conversion by metalloproteinases from membrane-associated FasL. It is also known that a Fas-Fas ligand system is a representative pathway of the apoptosis-signalling mechanism, activated by TNF-alpha [21]. A recent study has revealed an association between EMPs with cardiovascular outcomes [10]. In our investigation a significant increase of EMP levels in the circulation of ischaemic CHF patients who died was found when compared with those who survived. Because endothelial cells express FasL constitutively and TNF-alpha contributes to apoptosis through affecting the Fas-Fas ligand system [22], we proposed that increasing EMP levels in CHF patients may be related to TNF-alpha induced FAS-sFAS ligands and OPG/sRANKL cooperation.
Recent studies showed OPG to be a member of the tumour necrosis factor receptor superfamily and serum RANK/RANKL have been identified as candidate mediators for paracrine signalling in cell metabolism and extracellular matrix regulation but have also been shown to modulate dendritic cells and activated T cells, as well promoting B-cell maturation and antibody response, which suggests a role in both innate and adaptive immunity [23–25]. Therefore, serum RANKL and OPG as a RANKL inhibitor are increasingly being investigated as markers of cardiovascular risk, subclinical atherosclerosis, and cardiac remodelling and vascular calcification [26–32]. However, the role of the sRANKL/OPG complex in the maintenance of reparative repair potency in people with CHF shows to be very intriguing, while clinical data are limited.
We suggested that a mismatch between apoptotic processes and endothelial cell survival, indirectly determined through the calculation of the FAS/-sFAS ligand ratio and sRANKL/OPG complex, was more profound in subjects who did than in those who survived. Thus, we confirmed that pro-inflammatory activation is dramatically increased in CHF subjects at a high risk of death, it probably associates with endothelial dysfunction, and EMP level might reflect the severity of these disorders. We also noted that CHF patients with low levels of EMPs have demonstrated a superior chance of survival when compared with subjects with a high level of EMPs. Using this data we found that increased EMP number, higher than 0.514 n/mL, independently predicted all-cause mortality, CHF-related death, and CHF-related readmission within the observation period. A multivariable prediction model has shown a high decremented potential of EMP alone in CHF patients in the three years after study entry. These findings suggest that increased EMP number might improve the predictive value of a contemporary model of CHF based on clinical performances and NT-pro-BNP measurements. In this study, levels of EMCs, OPG, FAS-sFAS ligand ratio were sufficient to predict long-term changes in cumulative survival.
In conclusion, increased apoptotic circulating EMP, OPG, and FAS-sFAS ligand ratio independently predicted cumulative survival in CHF patients.
5. Compliance with ethical research standards
All patients given voluntary informed consent from participation in the study. The study was approved by the local ethics committee of State Medical University, Zaporozhye, Ukraine. Authors confirmed that the study was performed in accordance with the Declaration of Helsinki.
Footnotes
6. Acknowledgements
We thank all patients for their participation in the investigation, staff of the Regional Zaporozhye Hospital (Ukraine) and the doctors, nurses, and administrative staff in City Hospital # 6 (Zaporozhye, Ukraine), general practices, and site-managed organizations that assisted with the study. This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Study Restrictions: This study has some restrictions. The authors believe that a greater cohort of patients with more incidences detected would be desirable to improve the power of the study. Because the main limitation of the study was its small size and low frequency of events, we think that this is the reason for the low specificity of EMPs. It should be emphasized that while EMPs have a high diagnostic potential as biomarkers in cardiovascular diseases and cancer, due to current technological limitations in the purification of EMPs and an absence of standardized methods of detection the role of EMPs has become controversial. We think that this is a reason for the low specificity of EMPs and this may negatively bias the ROC curve. The authors suppose that these restrictions might have no significant impact on the study data interpretation.
