Abstract
Osteosarcoma, the most common primary bone malignancy, is characterized by easily relapsing and metastasizing. Hypoxia-inducible factor-1 (HIF-1) plays an essential role in tumorigenesis, affecting tumor metabolism, differentiation, angiogenesis, proliferation and metastasis, and has been found to be associated with survival in patients with osteosarcoma. The possible prognostic value of HIF-1 was investigated in many studies, but the results were inconsistent. We therefore conducted a meta-analysis to elucidate the correlation of HIF-1 expression, analyzed by immunohistochemistry in osteosarcoma tissues, with prognosis. The association degree was assessed by calculation of the hazard ratio (HR) and risk ratio (RR) with corresponding 95% confidence intervals (CIs). Follow-up information was available for 486 patients from 7 studies. The results showed that high HIF-1 expression was associated with a worse prognosis when compared to low or undetectable HIF-1 expression, with an HR of 3.67 (95% CI 2.24-5.99; p<0.001) for overall survival (OS) and an RR of 3.72 (95% CI 2.26-6.13; p<0.001) for OS. The RR of 2.55 for disease-free survival (DFS) did not show any obvious relationship between a high level of HIF-1 and DFS (95% CI 0.95-6.87; p = 0.064). The stability of this result was tested by sensitivity analysis and no significant change was detected. This meta-analysis suggests that HIF-1 is an effective prognostic biomarker to predict OS in patients with osteosarcoma.
Introduction
Osteosarcoma, one of the most common soft tissue and bone cancers, is the leading malignant musculoskeletal disorder that is haunting adolescents and young adults (1, 2). Due to its characteristics of easily relapsing and metastasizing, chemotherapy and surgical removal of metastases and the primary tumor are performed in order to increase the 5-year post-surgery survival rate (3). The genetic and molecular mechanisms involved in the etiology of osteosarcoma (from MMPs and BMPs to miRNAs, etc.) have been widely studied in order to detect predictive and prognostic factors and therapeutic targets (4-5-6).
Hypoxia-inducible factor 1 (HIF-1) is a member of the HIF family. It plays an essential role in transcriptional regulation and protein-protein interactions (7). HIF-1 is a heterodimer composed of 2 subunits, HIF-1α and HIF-1β. HIF-1 has been studied and associated with aggressive tumor behavior (8, 9). Many reports on this subject have been published; the malignancies involved were soft tissue and bone cancer, breast cancer, prostate cancer, colorectal cancer, ovarian cancer and lung cancer (10-11-12-13-14-15-16). Among these cancers, osteosarcoma shows a noticeable correlation with HIF-1 expression (17, 18). Due to osteosarcoma's rare clinical data and the inconsistent poor prognosis among studies (19-20-21-22-23-24-25), it would be worthwhile to discuss whether the expression level of HIF-1 contributes to the prognosis of osteosarcoma patients. We therefore conducted a meta-analysis to clarify and evaluate the relationship between HIF-1 expression as assessed by immunohistochemistry (IHC) in osteosarcoma tissue and osteosarcoma patients’ survival.
Materials and methods
Search Strategy and Article Selection
We conducted a broad search for relevant published articles in the PubMed, Embase, Medline and CNKI (China National Knowledge Infrastructure) databases. The last search was performed on February 10, 2016. Studies were identified by using the following search terms: “osteosarcoma or bone sarcoma” and “hypoxia-inducible factor 1, HIF-1 or HIF-1α”. No search restrictions applied to the date of publication and there were no language limitations. Relevant articles in reference lists were reviewed for further analysis.
Selection Criteria
Selected articles were eligible when they met the following criteria: 1) the diagnosis of osteosarcoma was histologically confirmed; 2) patients’ prognosis and survival outcome were issued; 3) HIF-1 expression level was evaluated by IHC in osteosarcoma tissue and studied in association with patient prognosis and survival outcome. When in a single article different tumors or factors were studied, data were included only when they met the above 3 criteria. The exclusion criteria were as follows: 1) in vitro, in vivo and animal studies; 2) obscure description or absence of clinical outcome; 3) reviews and conference abstracts. In the case of articles from the same author or affiliation with overlapping reports, only the latest or the most comprehensive one was included. Two reviewers carried out data extraction independently. Any disagreement was resolved by consensus.
Primary Outcome and Data Extraction
Overall survival (OS) or disease-free survival (DFS) was taken as the primary outcome in this meta-analysis, indicating the percentage of patients suffering from osteosarcoma within treatment group who are still alive exceeded 20.1-60 months (mean). The following data were extracted from the selected articles: first author, year of publication, patient population, osteosarcoma stages, HIF-1 expression level, and OS or DFS.
Statistical Analysis
The hazard ratio (HR)/risk ratio (RR) and corresponding 95% confidence intervals (Cis) were computed for assessment of the effect of HIF-1 expression on osteosarcoma survival (26). Some of the included studies already provided explicit HR/RR and 95% CI figures. For studies not providing these figures, the heterogeneity of combined HR/RR was assessed by means of Higgins’ I-square (I2) statistics (27). The random-effects model was applied if significant heterogeneity existed after computing the I2 statistics (I2>50%); otherwise the fixed-effects model was applied (28, 29). Both Begg's funnel plot and Egger's test were used for measuring potential publication bias (30, 31). Meanwhile, the stability of the results was assessed by sensitivity analysis. The STATA package version 12.0 (StataCorp LP) was used for all analyses. A 2-tailed p<0.05 was considered statistically significant.
Results
Specifics of the Study
After a primary paper search in the PubMed, Embase, Medline and CNKI databases and further screening and assessment, we identified 7 eligible studies (19-20-21-22-23-24-25) from which we included 486 osteosarcoma patients for meta-analysis (Fig. 1). The patient number per study ranged from 39 to 108, with a mean of 73.5. Three papers were published in English and the other 4 were in Chinese. IHC was performed in all studies. Of all patient samples, 261 showed high expression of HIF-1 and 225 showed low or undetectable expression. However, there was no standard cutoff value among studies (Tab. I).
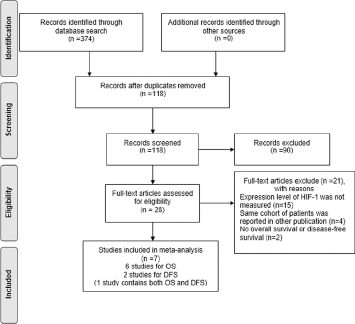
Flow diagram of the identification and selection of studies.
Main characteristics of studies included in the meta-analysis
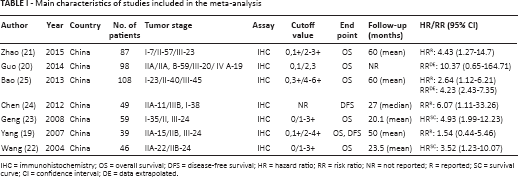
IHC = immunohistochemistry; OS = overall survival; DFS = disease-free survival; HR = hazard ratio; RR = risk ratio; NR = not reported; R = reported; SC = survival curve; CI = confidence interval; DE = data extrapolated.
Meta-Analysis Results
In this meta-analysis, no significant heterogeneity was detected in the analysis of the 7 studies, so a fixed-effects model was applied (I2<50%). Because HR correlates with the instantaneous risk at a particular time while RR refers to the cumulative risk over a time span, and based on the result of each research's survival analysis, we separated HR and RR even if they have a similar statistical interpretation. Six studies presented OS while 2 studies showed DFS: in fact, 1 of the 7 studies presented both OS and DFS. The OS results revealed that high HIF-1 expression was indicative of a worse prognosis compared to low or undetectable HIF-1 expression, with an HR of 3.67 (95% CI 2.24-5.99; p<0.001; I2 = 0.0%) for OS (Fig. 2A) and an RR of 3.72 (95% CI 2.26-6.13; p<0.001; I2 = 23.0%) for OS (Fig. 2B). The RR of 2.55 for DFS did not indicate any obvious relationship between a high level of HIF-1 and DFS in that the 95% CI (95% CI 0.95-6.87; p = 0.064; I2 = 33.9%) overlapped with 1.00; however, it did show a tendency for high HIF-1 expression to be linked to a worse survival (Fig. 2C). The stability of this result was tested through sensitivity analysis by removing one study at a time, and no significant change was detected (Fig. 3).
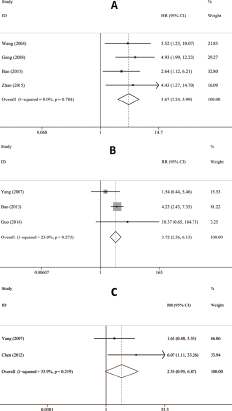

Forest plots of merged analyses for overall survival and disease-free survival associated with HIF-1 expression. (
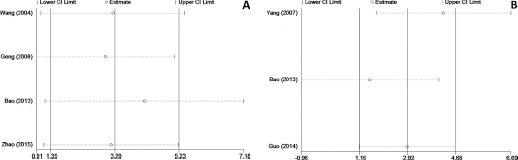
Sensitivity analysis. (
Publication Bias
Publication bias was qualitatively assessed by applying funnel plots and quantitatively by applying Begg's and Egger's tests. The funnel plot showed no distinct evidence of asymmetry among the 7 studies in this meta-analysis (Fig. 4). Egger's test also indicated no publication bias.
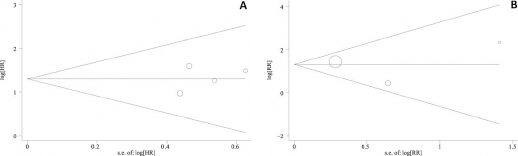
Begg's funnel plots of publication bias test. (
Discussion
The mortality of osteosarcoma is relatively high, and patients often succumb to pulmonary metastases (32). At present no reliable effective treatment is available to cure patients once metastases have developed. It is therefore extremely important to find biomarkers that will identify patients who are more likely to have a poor prognosis, so that appropriate treatment can be given and side effects can be minimized.
HIF-1 is a heterodimer made up of the HIF-1α and HIF-1β subunits, although it is the expression and activity of the HIF-1α subunit that promotes most of the biological processes of HIF-1 (33). HIF-1α protein levels may rise considerably and the fraction that is ubiquitinated reduces under hypoxic conditions (34). HIF-1 mediates physiological and pathophysiological responses in the cellular oxygen-signaling pathway, and plays an essential role in tumorigenesis, affecting tumor metabolism, differentiation, angiogenesis, proliferation and metastasis (35). It can directly activate or regulate the expression of certain factors and genes involved in tumorigenesis, namely VEGF, angiopoietins (ANG-1 and ANG-2), CXCR4 and VHL (36-37-38-39). HIF-1 expression has been found to correlate with malignant growth and poor patient survival in breast, prostate, cervical, pancreatic and gastric carcinomas (10-11-12-13-14-15-16, 40, 41). Collectively, these studies highlight the function of HIF-1 in cancer, suggesting its potential as a biomarker to predict prognosis. Hence, we used a similar approach to analyze the expression level of HIF-1 associated with survival in patients suffering from osteosarcoma.
Meta-analysis, the method of extracting relevant data from myriad individual studies and orderly summarizing them, is widely used for predicting clinical prognosis by evaluating biomarker expression (42). Seven studies were included in our analysis focused on the correlation of HIF-1 expression with osteosarcoma survival outcome. Final analysis suggested that the higher the HIF-1 expression, the worse the survival outcome will be, which indicates that high HIF-1 expression could predict poor prognosis in patients with osteosarcoma. The stability of this result was testified by sensitivity analysis, and no significant change was detected.
However, there are some limitations to this meta-analysis. First, osteosarcoma constitutes a rare subgroup of malignancies, with a limited number of cases reported worldwide. We collected 486 cases of osteosarcoma from 7 studies. Such a relatively small number of cases has the ineludible tendency to produce sample bias and random errors. We expect to enlarge the number of patients for analysis in order to reach more convincing conclusions. Second, studies that meet the specified selection criteria have only been carried out in Chinese populations, but similar research is expected to be done in populations of other origins so that the prognostic value of HIF-1 in osteosarcoma can be validated in larger sets of case-control studies. Third, there is no standard threshold that universally defines a high level HIF-1 expression in osteosarcoma. An appropriate cutoff value is needed to make an accurate evaluation of the relationship between HIF-1 expression and survival outcome. Fourth, we did not conduct subgroup analysis based on patient age, tumor stage, tumor size, etc., because of the limited total sample size. Fifth, there was no uniform interpretation of survival outcome among studies, and few studies addressed both OS and DFS. Thus heterogeneity among studies inevitably exists.
In conclusion, this meta-analysis demonstrated that elevated HIF-1 expression has a remarkable association with adverse prognosis in osteosarcoma. A poorer survival outcome may ensue when a patient presents higher HIF-1 expression. Further standardized prospective studies with more comprehensive analysis are expected to support this association between HIF-1 expression and the clinical prognosis of osteosarcoma.
Footnotes
Financial support: This work was supported by grants from the National Natural Science Foundation of China (No. 81372871 and No. 81502332).
Conflict of interest: None.
