Abstract
Background
Auxetic materials tend to exhibit stretching in the direction of the applied load as well as in the perpendicular direction. This may be an inherent property of the material, or it might be a particular structural characteristic that confers it with auxetic properties. In this study, the auxetic properties of a rotating squares auxetic design were utilized in tandem with a stretching mechanism to manufacture a device that offers the advantages of adjustable pore size and hence tunable drug delivery characteristics.
Methods
An auxetic polyurethane film was fabricated through the polymer casting technique. An acrylonitrile-butadiene-styrene (ABS) plastic mold for polymer casting was made through additive manufacturing. Stereolithography was used for fabrication of the mechanism that controlled pore size of the polymeric auxetic film. A laminate arrangement of the film and the mechanism was devised, through which movement of the mechanism controlled stretching of the auxetic film underneath.
Results
Results were analyzed through image processing. It was observed that a 2-dimensional increase (in length and width) of the auxetic film took place that corresponded to an increase in pore size of the film. Several mathematical correlations were drawn up.
Conclusions
It may be concluded that the first factor controlling drug release kinetics is the pore size of the film. This study explored a prototype mechanism that has the potential for being used in devices for controlled drug delivery or in smart bandage systems that may enhance wound healing in chronic wound treatment.
Introduction
An ideal wound-healing dressing should minimize infection and pain, promote reepithelialization and assist in the maintenance of a relatively moist environment for rapid wound healing. Needless to say, there are several wound dressings on the market that “approach” the definition of ideal, but no currently available dressing fulfills all of the criteria mentioned above (1). For rapid wound healing to take place, it is mandatory that bacterial colonization of the wound is prevented to a large degree; infection can delay wound healing and large vessel angiogenesis, due to prolonged inflammation times (2, 3). Medicated wound dressings have been known to mediate successful wound recovery (4). This is usually achieved through repetitive applications of medicament and frequent dressing changes. However, the process on the whole is inconvenient and painful. Frequent visits to medical centers or hospitals are required to fulfill multiple drug dosing requirements as well.
In many formulations, an initial large dose of drug is released as a bolus dose when the drug comes in contact with the release medium. Thus a burst release phenomenon is observed, which also reduces the lifetime of the drug delivery device. One of the complications of burst release is that it is difficult to control and is unpredictable (5). However, an initial burst release has the effect of providing initial relief, followed by a sustained-release profile (6). In spite of this, in vivo drug concentrations after burst release may reach toxic levels, raising therapeutic and economic concerns (7).
Stringent efforts have been made in the past to optimize drug release so that a locally sustained- or controlled-release pharmacokinetic profile may be attained through transdermal drug permeation instead of through the more common systemic route (8). In chronic wound therapy, controlled drug release from a bandage ensures consistent and sustained delivery of medication to the injured site, at the same time obviating the need for frequent dressing changes (9). In such cases, peak and valley drug profiles are avoided, and drugs with shorter half lives can be delivered. These effects may contribute to improving patient compliance with the treatment regimens (10). Polymeric materials are particularly useful in the fabrication of bandages (11), and also where it is necessary to avoid high systemic doses of antibiotics, while treating the infected wound site with localized concentrations of antibiotics (12, 13).
The necessity of optimizing controlled-release formulations for treatment of disease arises from the therapeutic requisite to reduce the amount of drug concentrations needed to produce desired effects in patients (14). Targeted or controlled-release therapy also improves patient compliance, because of easier dose regimens and the diminished requirements of multiple dosing (15).
To achieve targeted drug release profiles from novel wound dressings, a dual spinneret electrospinning technique has been used in which 2 drugs are used simultaneously, where it was found that the use of 2 drugs simultaneously in 1 matrix changed the release profile of one of the drugs (16). Transdermal drug delivery systems have also employed piezoelectric materials to control the delivery of drugs (17).
Advancements in the field of auxetic biomaterials, however, may pave the way for more convenient possibilities in the field of controlled drug delivery. Auxetic materials have a negative poisons ratio – that is, they increase in cross-section in the directions parallel and perpendicular to the direction of applied load (18, 19). Thus for an auxetic material with a porous morphology, an increase in pore size will take place in response to uniaxial loading. This will also be associated with a large volume change. These properties have been explored with reference to auxetic materials acting as molecular sieves, entrapping a particle and then freeing it in response to pore size changes after directional loading. Such characteristics have the potential to be harnessed for use in fine-tuning the release of drug from a matrix system (20).
In this study, we present a macro-model assembly for possible use in enhanced wound healing and controlled drug delivery applications. The macro-model assembly presented comprises an auxetic film and a mechanism with drug reservoir contained between the 2 opposing interfaces. All of the components of the assembly are arranged in laminar fashion, with the auxetic film and the mechanism conjugated at the ends. Because of this, any extension in the mechanism will ultimately cause extension in the auxetic film, changing pore size and allowing drug particles to pass through. The amount and rate of drug particles that pass through the film may be controlled by actuation of the mechanism at the lever ends (see Fig. 1). The prototype mechanism presented here has adjustable porosity for fine-tuning the amount of drug dispensed to a wound during chronic wound healing.

Macro model of the mechanism fabricated through stereolithography technique (SLA), assembled along with the drug reservoir and auxetic film. The assembly is a laminate arrangement which shows how the mechanism can be utilized in the actual/proposed application.
MATERIALS and methods
For the macro-model design, polyurethane (PU) was the material selected for the fabrication of the auxetic film underlying the mechanism for drug delivery control. PU was chosen because of its excellent biocompatibility and suitable machining characteristics. PU films may also be tailored according to the application by permutation of hard and soft segment ratios. The design used for fabrication of the auxetic film is based on the rotating squares model (21). The behavior of this design may be mapped out on the basis of both the angles formed at the vertices where the rotating squares join, and by the hinging and stretching constants. In addition to these parameters, the direction in which force is applied also plays a role in the stretching characteristics of the film. All of these parameters have been explored with particular reference to the scissor mechanism that controls the stretching behavior of the film. It would be pertinent to note that the mechanism simultaneously limits the stretching behavior of the film and hence the porosity which controls drug elution.
Casting of PU film
The PU used was PMC-744, with hardness 44 Shore ‘A’ (Smooth-On Inc., PA, USA). The 2-part (A and B) PU was mixed at a ratio of 2A to 1B, and then poured over the acrylonitrile-butadiene-styrene (ABS) plastic mold. The standard 18-hour curing period was followed for film casting, after which the film was peeled off the mold and left for another 24 hours in air to achieve full curing.
Manufacture of mold through fused deposition modeling
The mold for polymer casting was prepared through the additive manufacturing technique, FDM (STRATASYS FDM 360 mc machine). The parts extruded through FDM were based on thermoplastic ABS. The 3-D model of the negative replica of rotating square geometry was first designed through PRO/Engineer version Wildfire 5.0. Based on the computer-generated model, the mold was then fabricated by the FDM machine using ABS plastic as the modeling material.
Manufacture of mechanism by stereolithography
The mechanism that controlled the pore size of the auxetic film was manufactured by the stereolithography technique (SLA). In this technique, a computer-added design of the mechanism model was first converted into the StereoLithography (STL) format. Rapid prototyping of the mechanism was carried out based on the given STL format.
The mechanism assembly comprised 14 components, which included 6 bars and 8 pins, which allowed the bars to connect and move with reference to each other. Each part was manufactured separately and then assembled to form a functional mechanism (Fig. 2B). The mechanism functioned with a number of elongated bars that were interlocked with pins. The arrangement of the bars was such that they operated through a scissor-like mechanism. The basic operation depended on the fact that if force was exerted in the x direction (Fig. 2A), the mechanism extension would take place along the y direction. The overall extension of the mechanism was limited by the size of the slits that held 4 of the pins at the extreme ends of the assembly.
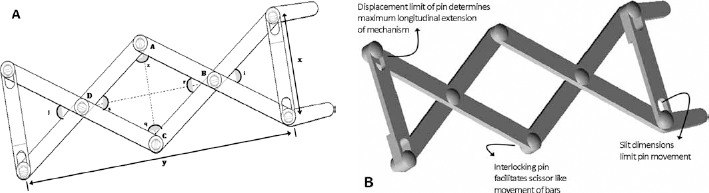
(
Characterization of film extension through image processing
The auxetic film behavior was characterized through image processing software in MATLAB (R 2009b). Measurements of the extended and unextended film were recorded through images taken with a digital camera (DSC-S 750; Sony, China) and characterized after scaling the pixel to centimeter ratio with the image processing toolbox in MATLAB. The images were taken from a fixed distance of 25 cm, so that all images corresponded to the same pixel to centimeter ratio. This was facilitated by the construction of a bridge set-up, in which the camera lens fit through the aperture, and the film was laid out underneath. The pixel to centimeter scale for these images was found to be 37.8:1. Subsequent calculations of film extension were carried out using this scale. Time lapse images of the drug particle being released from expanded pores in the auxetic film were also taken with a Nikon D 3100 camera (see Fig. 3).

Images depicting the release of drug particles from expanded auxetic film pores.
Results and discussion
Figure 4 shows images of the original (unextended) and extended auxetic film. One unit cell in the original film (Fig. 4A) measures 2.5 cm, while measurements for the same unit cell in a stretched condition increased up to 3.0 cm. It is evident from the processed images that a maximum extension of 0.5 centimeters was possible. As shown in Figure 4, the length to width ratios of the 4 unit cells ranged from 1.15 to 1.215, 1.285 and ultimately 1.209. The increase in length of each unit cell of the auxetic film was greater than the increase in width, although a 2-dimensional increase did take place, in both the x and y directions. As discussed earlier, this extension is subject to minor variation throughout the film. However, since the film is constrained (for stretching) from both extremes, the unit cells on both extremes (that is the first and sixth unit cell) were not taken into consideration when measuring maximum extension of the film.

The ratio measurements, length to width (L/W), throughout the length of the film may be patterned as a parabolic curve, as shown in Figure 5. In contrast to this behavior, the L/W ratios of all unit cells in the unextended film followed a relatively linear graph. The curve shown in Figure 5 is significant because even though an equal amount of force was applied at both ends of the film, there was a greater expansion observed in the third and fourth unit cells as compared with the second and fifth unit cells. These measurements support the hypothesis that at the microlevel, a greater amount of drug is likely to elute from this region of the bandage than at the extremes. This has been represented pictorially in Figure 6.
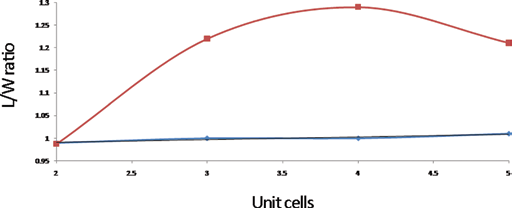
Graph of parabolic pattern that the extended auxetic unit cells follow. As is apparent from the graph, the third and fourth unit cells (middle region of the film) show more expansion than the rest. L/W = length to width.
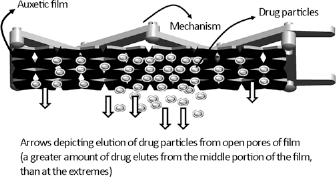
Schematic depicting drug elution from the bandage assembly, with a greater amount of drug eluting from the middle region than at the extremes of the film.
Testing of the macro model
As mentioned earlier, the extension of the film was controlled by the width of the slits at the extremes of the mechanism assembly. As the auxetic film was attached at both ends with corresponding ends of the mechanism, the stretching of the film was controlled by inward flexion of the end levers of the mechanism (Figs. 1 and 2A). Under a similar stress, a tear in a nonauxetic (conventional) material would behave by becoming elongated in the direction of the force applied (or the axial direction) and by contracting in the transverse direction. In this case, if the dimensions of the tear increase in the axial direction, they decrease in the transverse direction and thus there will be negligible increase in size, if any. Hence if the film used in our study had been replaced with a conventional polymeric material, the spherical balls that represent drug particles in this case (Fig. 3) would not have been able to pass through. However, because the film has an auxetic geometry, it will experience an expansion in the pore size in both transverse and axial direction, causing the pore size to increase and thus allowing the passage of the drug particle through the pore. This phenomenon has been represented pictorially in Figure 6. The degree of expansion achieved, however, may still be controlled by the mechanism, and it is this property of the auxetic/drug reservoir/mechanism assembly, which may be utilized for adjustable drug delivery kinetics when tackling chronic infected wounds that require long treatment times and multiple doses.
In the model that we created, the slit width of our mechanism allowed for horizontal movement of the pins, which ultimately translated into a range of possible extension motions for the mechanism on the whole. Because the mechanism controlled pore size in the auxetic film, the particle sizes that could pass through the film depended on, firstly, the degree of extension of the mechanism and, secondly, the slit width, which may be changed or modified in future models to accommodate a larger or different range of particle sizes which might be allowed to pass through the film.
The overall extension of the mechanism has been represented mathematically in mathematical model 1 given below. The condition depicting the range of particle sizes that may be allowed to pass through in the current scenario, have been explored in mathematical model 2 (Tab. I).
Mathematical notations used in text in mathematical models 1 and 2
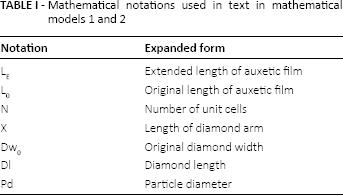
Mathematical model 1
The maximum extension that the auxetic film can achieve may be represented by the equation
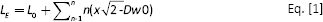
Where LE refers to the extended length of the film, L0 is the original length, n is the number of unit cells, x refers to the diamond arm and Dw0 is the original width of the diamond. Theoretically, substituting values into the expression n (x√2-Dw0) with n taken as 1 would give a total extension the film is subject to of 0.5 cm. Practically this has been demonstrated when the number corresponds to the maximum change in length that is possible when the vertices of the diamond-shaped hollow in 1 unit cell of the film are stretched out to form a square (Figs. 4 and 7).
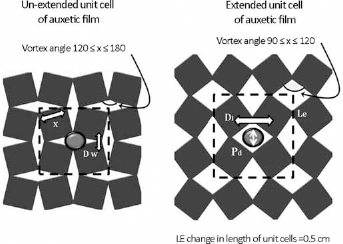
The auxetic film in unexpanded and expanded forms. As seen in the schematic, the drug particle with size Pd is capable of passing through the diamond-shaped pore when the range of angle is between 90° and 120°. Dl = diamond length; Dw = diamond width.
As shown in Figure 7, in the unstretched film, the diamond length (Dl), is greater than diamond width, so that when the condition is Dl>Dw, the drug particle with diameter Pd will not pass through the film. However, when the film is stretched in 1 direction so that the diamond vertex angles move toward 90°, the condition changes – that is, the diamond changes toward a square formation. In this case, when Pd is less than both Dl and Dw, the condition “Dl >Pd and Dw>Pd” is satisfied, and the drug particle passes through the auxetic film. This change in pore size is controlled by manual actuation of the mechanism to which the film is attached, thus providing the advantage of adjustable porosity for controlled drug delivery.
Mathematical model 2
The condition explained in mathematical model 1 depicts an extreme condition – that is, when the film is fully stretched, and the hollow diamond completely attains a square formation. However, another condition may also be explored, in which a range of particle sizes may pass through the film even before it is fully stretched out to maximum pore size.
If we consider the hollow diamond in 1 unit cell (see Fig. 8A) and apply stretching forces on both ends, as discussed earlier, the geometry of the diamond will be distorted to attain a square form (Fig. 8C). When forces are applied vertically on the diamond ABCD (Fig. 8B), the diagonal BD which is equal to Dw, will increase in length, so that the segment AC decreases in length. This will affect the angles at all 4 vertices of the polygon so that the 4 angles move toward 90°, and all of the sides of the polygon align in a square configuration. When the hollow space in the film is in the configuration (shown in Fig. 8B), BDC will be a right-angle triangle. Assuming the base of the triangle to be CD and the perpendicular to be BC and applying the Pythagorean theorem, we can conclude that Dw squared will be equal to the sum of the squares of the lengths of segments CD and BC. Since both of these segment lengths are sides of a square that are equal in length, we can assign them one variable (x). Therefore,
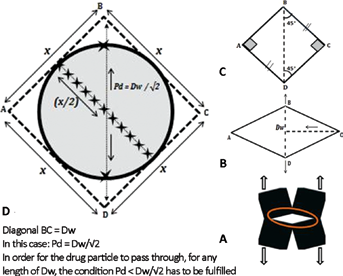
Schematic explaining mathematical model given in the section “Mathematical model 2.” The drug particle can only pass through the film when the condition mentioned above can be fulfilled.



To account for a range in the general size of drug particles that would be able to pass through the film, the following condition has to be satisfied:
If Pd = x, the particle can only pass through when Dw is greater than – that is:

According to this condition, for any measurement of Dw, the particle size should be less than Pd – that is, the following condition should be satisfied:

It may be concluded that the first controlling factor in the release kinetics of drug elution is the pore size of the film, provided that the drug particle sizes satisfy the conditions mentioned above. This may be explored further in a micro-scale study of the same model.
Conclusion
The bandage assembly model may be studied further on a micro scale and in simulated body conditions in vitro to prove the efficacy of this device for use in tunable drug delivery. In the present case scenario, as proven by image processing results and the mathematical models given above, this device offers the opportunity of fine-tuning control of drug delivery to the wound site, through adjustable porosity of the auxetic film and actuation of the mechanism to which it is attached. Further studies may be conducted to bridle the modulation of release kinetics of the drug to be dispensed through this laminate assembly.
Footnotes
Financial support: This work was not funded by any particular funding agency.
Conflict of interest: There are no conflicts of interest.
