Abstract
Background
The purpose of this study was to evaluate the effect of surface pretreatment with 37% phosphoric acid on the enamel bond strength of different universal adhesives.
Methods
One hundred and sixty bovine permanent mandibular incisors freshly extracted were used as a substitute for human teeth. The materials tested in this study included 6 universal adhesives, and 2 self-etch adhesives as control. The teeth were assigned into 2 groups: In the first group, etching was performed using 37% phosphoric acid for 30 seconds. In the second group, no pretreatment agent was applied. After adhesive application, a nanohybrid composite resin was inserted into the enamel surface by packing the material into cylindrical-shaped plastic matrices. After storing, the specimens were placed in a universal testing machine. The normality of the data was calculated using the Kolmogorov-Smirnov test. Analysis of variance (ANOVA) was applied to determine whether significant differences in debond strength values existed among the various groups.
Results
Groups with phosphoric acid pretreatment showed significantly higher shear bond strength values than groups with no enamel pretreatment (p<0.001). No significant variation in shear strength values was detected when comparing the different adhesive systems applied onto enamel after orthophosphoric acid application (p>0.05).
Conclusions
All adhesives provide similar bond strength values when enamel pretreatment is applied even if compositions are different. Bond strength values are lower than promised by manufacturers.
Introduction
The contemporary adhesive systems can be classified, on the basis of underlying adhesion strategy to interact with enamel and dentin substrates, into etch-and-rinse and self-etch adhesives (1). While the etch-and-rinse approach requires a separate acid-etch step to promote dentin and enamel demineralization before monomer infiltration, demineralization and infiltration occur simultaneously in the self-etch approach (2) and the washing process is removed (1, 3). The main disadvantage of etch-and-rinse adhesives is their susceptibility to the complete filling of the interfibrillar spaces by resin monomers thus resulting in areas of exposed demineralized enamel and dentin within the bonded interface (4-5-6-7-8). This incomplete infiltration of resin monomers network may lead to interfacial hydrolysis (9, 10) and postoperative sensitivity (3, 11). Self-etch adhesives incorporate the partially dissolved smear layer, resin, collagen and mineral into the hybrid layer and the superficial portion of the resin tags which may prevent postoperative sensitivity. Their use on dentinal tissue is therefore preferred. However, their etching agents are not as effective as phosphoric acid, and lower enamel bond strengths have been registered (12). Thus, when only enamel is exposed, self-etch adhesives can not ensure adequate enamel shear bond strength both for dental restorations both for bonding orthodontic brackets. To overcome this limitation, enamel acid pretreatment and consequent washing have been recommended prior to the application of self-etch adhesives (13, 14). Facing these technical limitations, in order to simplify adhesive procedures and shorten the application time, new single-stage self-etching adhesive systems have been introduced with improved chemical structure and different application patterns (15, 16). These systems combine acid primer and bond in the same solution which should be applied in 1 step (17, 18). Micromechanical retention provided by resin monomers interlocked in the created porosities is the principal mechanism of adhesion (19), although the hybrid layer has a submicron thickness (20). Self-etch adhesives contain specific monomers characterized by at least 1 polymerizable group and a functional group, which have different purposes, such as wetting and demineralizing the substrate (21, 22). Many universal adhesives have been launched, but few in vitro and clinical studies support and compare the effectiveness of adhesion. Each self-etching adhesive system may have different ingredients which can affect the performance of adhesion (23). The aim of this in vitro laboratory study was to predict the performance of these products both on etched and intact enamel in a short period of time using a shear bond strength test.
We used bovine teeth. Although it is preferable to use extracted human teeth for bonding research (24), it has become increasingly difficult to obtain such samples for laboratory studies in Italy. Bovine teeth have the advantage that bovine enamel is similar to human enamel thus allowing large samples for in vitro studies on enamel bonding (25). Bovine teeth also have large, flat surfaces and are unlikely to have undergone prior caries challenges that could affect the test result. The mineral distribution within the carious lesions in bovine teeth is reportedly similar to that found in human teeth, and the structural changes that occur in human and bovine teeth are also similar (26).
The null hypothesis tested was that there would be no differences between the bond strength of 7 different 1-step self-etch adhesives and a conventional self-etch adhesive, whether they were applied on etched enamel or on intact enamel surfaces.
Methods
One hundred and sixty bovine permanent mandibular incisors freshly extracted and stored in a solution of 0.1% (wt/vol) thymol were used as a substitute for human teeth (26, 27). The criteria for tooth selection included intact buccal enamel with no crack caused by extraction. The teeth were cleansed of soft tissue and embedded in self-curing, fast-setting acrylic resin (Rapid Repair, DeguDent GmbH, Hanau, Germany). Specially fabricated cuboidal Teflon mold was filled with the acrylic resin and allowed to cure, thus encasing each specimen while allowing the buccal surface of enamel to be exposed. Each tooth was oriented so that its labial surface was parallel to the shearing force. The buccal enamel surface of all specimens was flattened with aluminum oxide disks of sequentially decreasing granulation (400, 600, 1200 grit) with copious water coolant to obtain flat enamel/dentin surfaces (28). This process standardizes the orientation of enamel prisms and removes the outer hypermineralized and acid-resistant enamel. It is also consistent with clinical practice when the outer 0.5 mm of labial enamel is removed during beveling or for veneering (29).
The materials tested in this study included 6 universal adhesives (Futurabond M+ by Voco, Scotchbond Universal by 3M ESPE, Adhese Universal by Ivoclar Vivadent, Clearfil Universal Bond by Kuraray, GBU-500 by GC Corporation and Peak Universal Bond by Ultradent) and 2 self-etch adhesives (Clearfil SE Bond 2 by Kuraray and OptiBond XTR by Kerr) as control. The specifications of all adhesive systems are listed in Table I.
Adhesive systems used in study
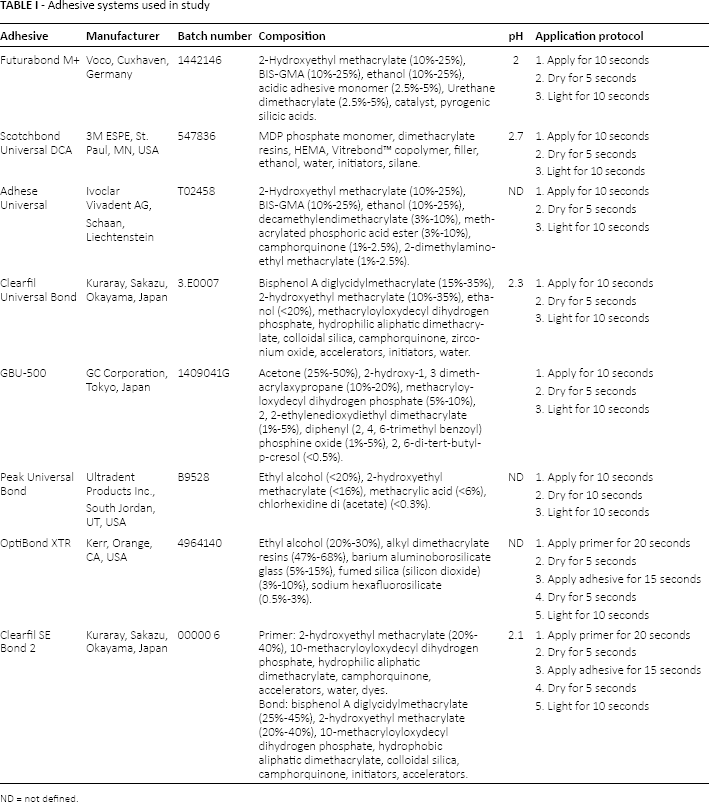
ND = not defined.
The adhesive systems were applied to the demarcated bonding area, following each manufacturer's instructions. Before application of the adhesive systems, the labial surface of each incisor was cleaned for 10 seconds with a mixture of water and fluoride-free pumice in a rubber-polishing cup with a low-speed handpiece. The enamel surface was rinsed with water to remove pumice or debris and then dried with an oil-free air stream.
The teeth were randomly assigned into 2 groups. In the first group (n = 80), etching was performed using 37% phosphoric acid for 30 seconds (Total Etch; Ivoclar Vivadent AG, Schaan, Liechtenstein). In the second group (n = 80), no pretreatment agent was applied. Ten specimens were then randomly assigned for each of the 8 adhesive systems.
All universal adhesives were cured using a light-emitting diode (LED) curing light in soft start–polymerization mode (Celalux 2 High-Power LED curing light; Voco GmbH, Cuxhaven, Germany) for 10 seconds at a light intensity of 1,000 mW/cm2. For Clearfil SE Bond 2 and OptiBond XTR bonding, the application followed primer application (20 seconds) and air-drying for 5 seconds.
After adhesive application, a nanohybrid composite resin (Grandio-Voco GmbH, Cuxhaven, Germany) was inserted into the enamel surface by packing the material into cylindrical-shaped plastic matrices with an internal diameter of 2 mm and a height of 2 mm. Excess composite was carefully removed from the periphery of the matrix with an explorer. The composite was cured with an LED curing light in soft start–polymerization mode (Celalux 2 High-Power LED curing light; Voco GmbH, Cuxhaven, Germany) for 20 seconds at a light intensity of 1,000 mW/cm2 according to manufacturer's instructions. All samples were stored in distilled water at 37°C for 24 hours.
After storing, the specimens were placed in a universal testing machine (Model 3343; Instron Corp., Canton, MA, USA). Specimens were secured in the lower jaw of the machine so that the bonded cylinder base was parallel to the shear force direction. Specimens were stressed in an occluso-gingival direction at a crosshead speed of 1 mm/min (30-31-32). The maximum load necessary to debond was recorded in newtons (N) and calculated in MPa as a ratio of newtons to surface area of the cylinder. Statistical analysis was performed with Stata 9.0 software (Stata, College Station, TX, USA). Descriptive statistics, including the mean, standard deviation, median and minimum and maximum values were calculated for all groups.
The normality of the data was calculated using the Kolmogorov-Smirnov test. Analysis of variance (ANOVA) was applied to determine whether significant differences in debond strength values existed among the various groups. Tukey's test was assessed as post hoc. Significance for all statistical tests was set at a p value <0.05.
Results
Descriptive statistics are presented in Table II. ANOVA showed the presence of significant differences among the various groups (p<0.0001). As shown in Figure 1, post hoc Tukey testing showed that groups with phosphoric acid application showed significantly higher shear bond strength values than groups with no enamel pretreatment (p<0.001).
Descriptive statistics (MPa) for shear bond strengths of the different groups
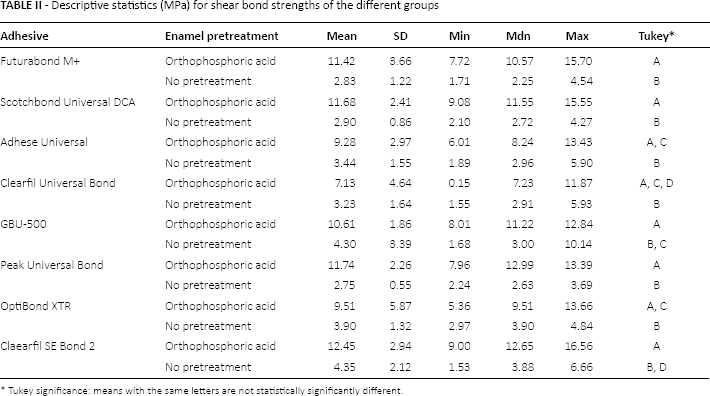
Tukey significance: means with the same letters are not statistically significantly different.
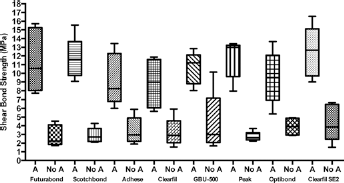
Shear bond strength box plots (MPa) of the different groups. A = 37% phosphoric acid pretreatment; No A = no acid pretreatment.
No statistically significant difference in shear bond strength was reported among various adhesives systems when no enamel pretreatment was performed (p>0.05). Moreover, no significant variation in shear values was detected when comparing the different adhesive systems applied onto enamel after orthophosphoric acid application (p>0.05).
Discussion
Based on our results, the null hypothesis was rejected. Bond strength values obtained after enamel pretreatment with phosphoric acid were significantly higher than values obtained without pretreatment on intact enamel.
When enamel pretreatment with phosphoric acid is applied, nonsignificant variations were obtained among 1-step adhesives. Minor and nonsignificant variations among bond strength values may be related to the different functional monomers the products contain, the filler content and pH value. Combinations of these features have the ability to resolve smear layer and ensure demineralization in dental tissues providing adhesion by binding the tooth substrate with the functional monomer (22). Van Meerbeek et al (16) classified self-etching primaries as strong (pH <1), moderate (pH between 1 and 2) and weak (pH >2) according to pH values (33). However the influence of pH value is considerably reduced if phosphoric acid pretreatment is applied on the tooth surface. On the other hand, when no pretreatment is applied, the pH value is not the only factor influencing bond strength (18).
All adhesives tested contain hydroxyethyl methacrylate (HEMA) except for GBU-500 (GC) and OptiBond XTR (Kerr). However, the constituents of GBU-500 (GC) provide bond strength values comparable with HEMA-based adhesives even if the hypothetical percentage of alcohol content is significantly higher (acetone 25%-50%). OptiBond XTR (Kerr) contains different functional monomers, alkyl dimethacrylate resins (47%-68%) and a remarkable amount of filler content in the form of barium aluminoborosilicate glass (5%-15%) and fumed silica (silicon dioxide). Fillers ensure an high density similar to a flowable resin composite, which promotes filling of the microporosities created on pretreated enamel and elevates the mechanical adhesion. Similar amounts of fillers are included in the composition of Scotchbond Universal (3M ESPE), Clearfil Universal Bond (Kuraray) and Clearfil SE Bond 2 (Kuraray).
Clearfil SE Bond is considered the reference for all other self-etch adhesives (11, 18, 34) because of its high shear bond values and high stability over time. The chemical bonding provided by the 10-methacryloyloxydecyl dihydrogen phosphate (MDP) in the primer, combined with the excellent mechanical properties and high conversion rate of its filled hydrophobic resin resulted in quite low shear bond strength values in the present study if compared with other similar studies (35, 36).
The main limitation of this present study was that long-term clinical follow-up was not investigated, because it is difficult to perform in a standardized manner and is time-consuming. In vitro bond strength tests are thus frequently used to assess properties and quality of dental materials and technical procedures, respectively (37, 38).
Another limitation of this study was the low number of observations. A higher number of observations could show these minor changes among the products and highlight further significant differences. Moreover, the tested adhesives were applied following the manufacturers’ instructions, but the shear bond strength values registered were definitely lower than those promised for each adhesive system.
The main strength of this study was that the direct comparison among different types of adhesive systems was made in 1 stage thus minimizing biases related to procedural errors, environmental influences and time lapses.
Further studies are needed to define the influence of the aging procedures and quantify how much they degrade the adhesion in relation to the composition (i.e., the solvent and filler content). The stability of the adhesion should be maintained over time.
Though the compositions of the adhesive systems are quietly different for functional monomers, filler content, pH values and solvent; the present study did not evidence significantly differences in bond strength values among the adhesives when enamel pretreatment was applied. When orthophosphoric acid was not applied, the bond strength values were significantly lower than the minimum stated for all adhesives tested.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
