Abstract
Background
The purpose of this study was to evaluate the effects of thermal cycling on the surface roughness, hardness and flexural strength of denture resins.
Methods
Polyamide (PA; Deflex and Valplast) and polymethylmethacrylate (PMMA; QC-20 and Acron MC) denture materials were selected. A total of 180 specimens were fabricated and then divided into 3 groups. The first group (group 1) acted as a control and was not thermocycled. The second group (group 2) was subjected to thermocycling for 10,000 cycles in artificial saliva and 5,000 cycles in distilled water. The last group (group 3) was thermocycled for 20,000 cycles in artificial saliva and 10,000 cycles in distilled water. The surface roughness were measured with a profilometer. The hardness of the resins were measured with a Vickers Hardness Tester using a 100-gf load. The flexural strength test was performed using the universal test machine with a crosshead speed of 5 mm/min. Data were analyzed using statistical software. The results of the measurements in the 3 different tests were analyzed by Kruskal-Wallis test with Bonferroni correction. Multiple comparisons were made by Conover and Wilcoxon tests.
Results and conclusions
There was a significant difference between the PMMA and PA groups in terms of surface roughness, hardness and transverse strength before and after thermal cycling (p<0.001). Thermal cycling did not change the surface roughness, hardness and flexural strength values of either the PMMA or PA group (p>0.001).
Introduction
Polymethylmethacrylate (PMMA) has been used as a denture base material since 1937 and has been the primary resin material of choice for the fabrication of denture bases in clinical dentistry (1, 2). PMMA has favorable physical properties, such as accurate fit, aesthetic appearance, polishability and easy manipulation. Although the properties of acrylic denture base resins have been enhanced, factors such as wear, lack of toughness, hypersensitivity and allergic reactions to residual monomer still limit the longevity of prosthetic restorations (3, 4). These conditions have led researchers to reinforce and/or modify PMMA. The addition of a polyfunctional crosslinking agent (5) and the incorporation of a rubber phase (6), metal wire/mesh (7, 8) or fibers (9) has been made to improve the mechanical properties of denture base materials. In addition, alternative materials, such as polyamide resins, have been developed for use in the fabrication of removable prostheses. Polyamide (PA), also known as nylon, is a thermoplastic, crystalline polymer that contains amide groups regularly spaced on the main chain and is produced by a condensation reaction between diamine and dibasic acid (1, 2, 10). High-temperature melt condensation is used for the commercial synthesis of aliphatic polyamides (nylons) (11). Nylon is a generic name used for certain types of thermoplastic polymers belonging to the class known as polyamides. Nylon polyamides were first introduced in the fabrication of denture bases in the 1950s (12) and are currently an alternative to methylmethacrylates, mainly due to their enhanced aesthetic properties, heat and chemical resistance, and toxicological safety for patients allergic to methacrylate monomer and metal-reinforced acrylic resin dentures. Additionally, higher elasticity provides more comfort for patients who have soft and hard tissue undercuts than dentures fabricated with PMMA (10, 13). Although nylon PA resins have superior mechanical properties relative to other nonmetallic denture bases, there remain some limitations, such as processing difficulties, dimensional changes, stain and high water sorption (1, 14).
Some characteristic properties of PAs have been reported by a few previous investigators. Yunus et al (2) studied the effect of a 24-hour immersion in an oxygen-releasing disinfectant solution on the flexural strength of nylon denture base polymers and observed no change in their flexural strength. Ucar et al (15) compared the mechanical properties of PA and PMMA denture base materials and found a significant difference in hardness, but no difference was observed in terms of flexural strength. Takabayashi (16) investigated the mechanical and physical properties of PA, polycarbonate and polyethylene terephthalate resins for nonmetal clasp dentures (PA), and PMMA specimens were prepared as a control. Thermoplastic resins for nonmetal clasp dentures (PA) demonstrated great toughness and strong resistance to fracture, but their flexural strength and modulus of elasticity were lower than those of PMMA. Additionally, the water sorption values of PA indicated that thermoplastic resins for nonmetal clasp dentures have a hygienic nature that reduces the accumulation of plaque. However, the basic properties of commercially available PA-based denture resins after thermal cycling have not been reported in the literature.
During clinical service, prosthetic restorations are usually under conditions of thermal variation and loading in the oral cavity that cause damage to the surface and mechanical properties of the materials. Temperature changes may affect the denture base materials, resulting in a need to improve the longevity of dental restorations. Intraoral temperature changes are produced from routine eating, drinking and breathing, and they have a negative effect on the promotion of crack growth over a prolonged period and can thus change the physical properties of the material (17-18-19). Because of these factors, dental materials should be tested in conditions similar to those they will be encounter in the oral cavity. Thermocycling is an in vitro process used to simulate in vivo events (20) and is often used in these studies (13, 20-21-22) to evaluate the effects of these conditions. Lira et al (21) investigated the effect of thermal cycling on the surface microroughness of PMMA denture base resins and reported significant differences for microwaved resins after thermocycling. Takahashi et al (13) evaluated the effect of thermal shock on the mechanical properties of injection-molded thermoplastic denture base resins and reported significant changes in impact strength. Finally, Machado et al (23) reported that thermocycling did not significantly affect the impact strength of PMMA denture base resins.
No studies have evaluated the effect of thermal cycling on the surface roughness (RA), hardness and flexural strength of PA denture base polymers, all of which are important for the long-term success of dental prostheses. The aim of this study was to compare PA and PMMA denture base resins and to evaluate the effect of thermal cycling on some physical properties of denture base resins. The null hypothesis was that no significant difference occurs between PA and PMMA in terms of RA, hardness and flexural strength before and after thermal cycling.
Materials and methods
Two types of both PA (Deflex and Valplast) and PMMA (QC-20 and Acron MC) denture base materials, commonly used in prosthodontic practice, were selected for investigation. The abbreviations, types, manufacturers and manufacturing methods of the materials used for the experiments are listed in Table I.
Abbreviations, types, manufacturers and polymerization types of materials used for experiments
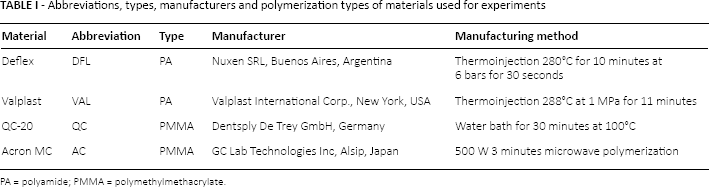

PA = polyamide; PMMA = polymethylmethacrylate.
Fabrication of specimens
Forty-five samples were prepared for each denture base material and divided into 3 subgroups (n = 15). Metal molds and/or wax patterns were fabricated in a rectangular shape (65 x 10 x 2.5 mm) according to the American Dental Association specification no. 12. For PA resins, specimens were flasked according to the manufacturer's instructions with a positioned sprue. Cartridge-formed Deflex (DFL) was heated to a temperature of 280°C for 10 minutes and then injected into the flask at a pressure of 6 bar for 30 seconds. Valplast (VLP) was heated to 288°C and automatically injected to the flask at a pressure of 1 MPa for 11 minutes. The specimens were allowed to bench-cool before deflasking. For PMMA resins, heat-polymerized QC-20 (QC) specimens were polymerized by using conventional flasking and inserting the flask in a boiling water bath for 30 minutes at 100°C (24). Microwave-polymerized Acron MC (AC) specimens were polymerized in a microwave oven (Vestel, Goldstar, Turkey) at 500 W for 3 minutes.
The surfaces of the fabricated samples were finished with 500-grit abrasive paper. A digital caliper (Electronic Digital Caliper, Shan, China) with a precision of 0.05 mm was used to measure the final dimensions of the specimens. All specimens were then stored in distilled water at 37°C for 48 hours before the thermal cycling procedure.
Thermocycling procedure
Initially, all specimens were kept in an artificial saliva bath at 37°C ± 2°C for 24 hours to simulate oral cavity conditions and then dried with absorbent papers before each test. All specimens were then stored in distilled water at 37°C for 48 hours before the thermal cycling procedure. Specimens from each denture base material were equally divided into 3 groups (n = 15). The first group (group 1) served as a control and was not thermocycled. The second group (group 2) was subjected to thermocycling for 10,000 cycles in artificial saliva and 5,000 cycles in distilled water from 5°C to 55°C with a dwell time of 60 seconds using a thermal cycler (MSCT-3 Plus; Marcelo Nucci-ME, Sao Carlos, Brazil). The last group (group 3) was subjected to thermocycling for 20,000 cycles in artificial saliva and 10,000 cycles in distilled water (15, 16). Afterwards, RA, hardness and transverse strength tests were performed.
Surface roughness test
The Ra of each tested material was measured with a profilometer (SJ-201P; Mitutoya Corp, Kawasaki, Japan) using a 0.4-gf load for 5 seconds, in which a diamond stylus transverses the surface of the resin and an amplified trace of the profile is obtained. The resolution of the data was 0.01 µm. Three readings were recorded across the specimen surface, and the average value was calculated.
Hardness test
The Vickers hardness number (VHN) of each test sample was measured with a Vickers Hardness Tester (Struers A/S, Balerup, Denmark) using a 100-gf load for 30 seconds. The diagonals of the pyramid impressed on the specimen by the Vickers diamond indenter were measured and noted. Three measurements were performed on each specimen, and the final value of hardness was calculated by the arithmetic average. All measurements were recorded by 1 operator.
Flexural strength test
The flexural strength test was performed using a universal test machine (Lloyd LRX; Lloyd Instruments, Fareham, Hants, UK). The specimens were placed on jigs that were 50 mm apart, representing the space between the maxillary molars in a complete denture. The load, with a crosshead speed of 5 mm/min, was applied to the center of the specimens until fracture or maximum deflection occurred. The flexural strength (FS) was calculated from the formula FS = 3Fl/2bh2, where F is the maximum load applied, l is the span length (50 mm), b is the width of the specimen (10 mm), and h is the thickness of the specimen (3.3 mm). Flexural strength was calculated in units of MPa as in previous studies (2, 4, 5) that evaluated the flexural strength of denture base resin in this unit; thus, we may compare the results of the present study with those of previous ones.
Statistical Analysis
Data were analyzed with a statistical software package (SPSS, version 11.5; SPSS Inc., Chicago, IL, USA). The Shapiro-Wilk and Levene tests were used to investigate the distribution and homogeneity of the variables. The results of the measurements from the 3 different tests were analyzed using the Kruskal-Wallis test with Bonferroni correction. Multiple comparisons were made using Conover and Wilcoxon tests. Sample sizes were determined with the resource equation method: E = (total number of experimental units) - (number of treatment groups). According to this equation, E = 12-3 = 9. We selected a sample size higher than E for a more balanced design.
Results
The mean values of Ra, hardness and flexural strength of the denture base resins before and after thermocycling, as well as their standard deviations, are given in Tables II, III and IV, respectively.
Mean surface roughness values (Ra, µm) of materials evaluated
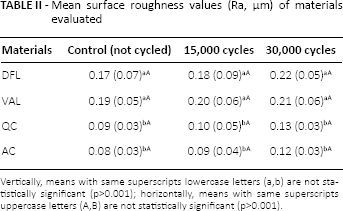
Vertically, means with same superscripts lowercase letters (a,b) are not statistically significant (p>0.001); horizontally, means with same superscripts uppercase letters (A,B) are not statistically significant (p>0.001).
Mean hardness values (kg/mm2) of materials evaluated
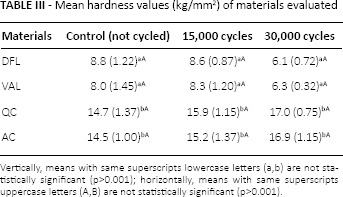
Vertically, means with same superscripts lowercase letters (a,b) are not statistically significant (p>0.001); horizontally, means with same superscripts uppercase letters (A,B) are not statistically significant (p>0.001).
Mean flexural strength values (MPa) of materials evaluated
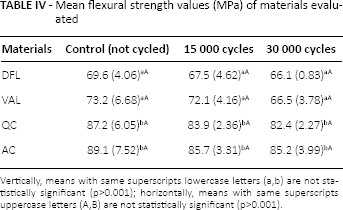
Vertically, means with same superscripts lowercase letters (a,b) are not statistically significant (p>0.001); horizontally, means with same superscripts uppercase letters (A,B) are not statistically significant (p>0.001).
There was a significant difference between the PMMA and PA groups in terms of Ra, hardness and transverse strength before and after thermal cycling (p<0.001).
The Ra of the PMMA resins was significantly lower than that of PA resins (p<0.001) before and after thermal cycling, whereas there were no significant differences between DFL and VAL or QC and AC (p>0.001). The highest Ra was observed in the VAL resins before and after thermal cycling.
The hardness and flexural strength of the PMMA resins were significantly higher than those of the PA resins (p<0.001) before and after thermal cycling, whereas there were no significant differences between DFL and VAL or QC and AC (p>0.001). The PA specimens were not fractured and detached from the supporting jigs during the test, so the flexural yield strength values were taken as the flexural strength. Thermal cycling increased the Ra and decreased the hardness and flexural strength of all resin groups, but these changes were not significantly different (p>0.001). Additionally, no significant differences were found between the control and 15,000 cycles, the control and 30,000 cycles, or 15,000 and 30,000 cycles in any of the denture resins.
Based on the results of the present study, the null hypothesis was rejected because of the significant difference between the PMMA and PA groups in terms of Ra, hardness and flexural strength before and after thermal cycling. PA resins presented the lowest hardness and flexural strength values as well as the highest Ra values relative to those of PMMA. The different chemical structures of PA and PMMA denture base resins may be the reason for these results; nylon is a crystalline polymer, whereas PMMA is amorphous. This crystallinity affects the physical properties of the nylon polymers, such as solubility in solvents, heat resistance, toughness and abrasion resistance (12, 25, 26).
Discussion
Thermal cycling procedure is a routine application for testing the long-term use of dental materials during clinical use. The oral environment may be within the temperature range of 5°C-55°C due to the different types of nutrition, such as cold drinks, hot soup or tea. Additionally, removable dentures are immersed in saliva and, when not in use, may be soaked in water or cleansing agents during clinical use (27). Because of these factors, this study was designed to simulate the maximally identical clinical and oral applications of removable prostheses. Based on these considerations, thermal cycling was performed for 10,000 cycles in artificial saliva and 5,000 cycles in distilled water for the first test group and 20,000 cycles in artificial saliva and 10,000 cycles in distilled water for the second test group, with the aim of simulating both intraoral and extraoral environments. Similarly, Garcia et al (28) studied the influence of artificial accelerated aging on the dimensional stability of acrylic resins and kept the test samples in artificial saliva for 16 hours and distilled water for 8 hours.
In previous studies, various numbers of thermal cycles have been tested, but no definitive relationships have been found. Gale and Darvell (20) reviewed the literature and reported that cycles might occur between 20 and 50 times per day, and some 10,000 cycles might represent a service year. According to that report, we can consider the results of the present study as representing more than 1 year of clinical use.
Ra is an important characteristic in dental materials (29). Dental plaque is related to the adhesion of microorganisms and is a major factor in the etiology of denture-related stomatitis, which occurs due to the increased roughness of denture surfaces (30). Ra of the denture base resin affects the adhesion and colonization of Candida biofilms (31, 32). Candida albicans is the most common pathogen in the oral environment that causes the occurrence of denture stomatitis. Verran and Maryan (33), Quirynen et al (34), Radford et al (35) and Taylor et al (36) reported the relationship between Ra and microbial retention on denture base materials. Additionally, the presence of microorganisms in the oral cavity is a risk factor for respiratory tract infection by aspiration in the elderly population (37). Therefore, providing dentures with low Ra has been recommended as an essential procedure for maintaining healthy oral mucosa. An increase in the roughness of the denture surfaces also may lead to discoloration of the prostheses, causing aesthetic problems. The PA denture base materials had rougher surfaces than PMMA, in agreement with the results of the studies reported by Yunus et al (2), Ucar et al (15) and Kurkcuoglu et al (38). Abuzar et al (39) reported a significant difference in the Ra values of polished PMMA and PA surfaces and explained that the differences may be due to the physical properties of the materials. The significant difference between the 2 types of denture base materials is most likely due to the individual characteristics of PA molecules, which contain amide groups on the main chain and provide the hydrophilic nature of the material. Because nylon is hygroscopic and its moisture content varies with the surrounding conditions (12), immersion in water and artificial saliva during the thermal cycling procedure may produce swelling of the material and increase its Ra. Nevertheless, all materials presented acceptable Ra (40) values, limited to 0.2-µm Ra, before and after thermal cycling. Evaluating Ra is very important for many fundamental problems, such as friction, contact deformation and positional accuracy. The actual surface geometry is sufficiently complicated that a finite number of parameters cannot provide a full description. Ra parameters are normally categorized according to functionality. Ra is the arithmetic average height parameter and is the most universally used roughness parameter for general quality control (41, 42). This parameter is defined and measured easily and provides a good general description of height variations; hence, we selected this parameter in the present study.
Hardness is an important property that enables the use of acrylic materials as denture base resins due to its resistance to occlusal forces. This property also provides resistance to scratching and abrasion (43) and is directly associated with material arrangement, chemistry and polymerization mode (44). Hardness is defined as the resistance to indentation and is determined by measuring the permanent depth of indentation using different test methods. Vickers, Knoop, Brinell, Shore and Rockwell are the commonly used hardness test methods (45). Indentation hardness tests are carried out using a diamond indenter with a specific geometry, usually pyramidal. Sample characteristics such as size, shape, thickness and composition should be considered prior to selecting the hardness testing method. Vickers and Knoop hardness tests are the most commonly used methods for thermoplastic denture base polymers (46). The Vickers test is advantageous because both diagonals are measured, and the average value is used, whereas in the Knoop test, only the longer diagonal is measured (47). The Vickers hardness test method was selected for the present study to obtain accurate results.
In the current study, the 2 types of denture base resins were significantly different in terms of hardness. The PA specimens presented lower values than PMMA before and after thermal cycling. The hardness values of both the PA and PMMA denture base materials were not significantly affected by thermocycling. The hardness of a resin material depends on the nature of the monomers and on the degree of crosslinking (48, 49). This can be attributed to differences in chemistry; PA resins contain amide groups, and PMMA resins have a copolymer structure in their polymer matrix.
In the current study, the PMMA specimens had increased hardness values at both 15,000 and 30,000 thermal cycles, possibly due to the continuous nature of the polymerization reactions during thermal cycling by heat that causes an increase in hardness by the decrease in the number of unreacted monomers (50). In contrast, the hardness of PA was decreased after 30,000 cycles, perhaps indicating that thermal changes affect the surface properties of PA denture base resins negatively during long-term use.
Flexural strength is defined as the ability of a material to resist deformation under load and represents the highest stress experienced within the material at its moment of fracture. The flexural failure of denture base materials is considered the primary mode of clinical failure (51) and is measured by the 3-point flexural (transverse) test, adopting international standards for polymer materials, including ISO 1567:1999 Dentistry-Denture base polymers (52).
Thermal cycling caused a decrease in the flexural strength of denture base materials but without statistically significant differences. The mean flexural strengths of both the PMMA and PA resins after 2 different thermal cycles were lower than those of the control groups. Heat changes may cause an extension of the distance between the polymer chains, resulting in the absorption of water by the material. Water molecules act as a plasticizer in the polymer structure after water immersion, and cyclic temperature changes dissolve unpolymerized PMMA (22). Additionally, the artificial saliva component may have a detrimental effect on the polymer matrix of the resins. Machado et al (53) reported a significant decrease in the flexural and impact strengths of urethane and PMMA base denture materials when the specimens were thermocycled. Archadian et al (54) investigated the flexural properties of denture base materials and observed a decrease in strength after 20,000 thermal cycles. The lower flexural strength value reflects the flexibility of the PA denture base resin. These results are also in agreement with previous studies (2, 15) reporting PA resins to be more flexible than PMMA. This finding may confirm the advice of manufacturers, who suggest the use of PA resins rather than PMMA on patients with soft or hard tissue undercuts to provide comfortable long-term use.
The decrease in the flexural strength of PA denture base resins might be due to the interaction between amide and amine functional groups by heating after thermal cycling, as this reaction may lead to changes in physical properties due to thermal oxidative degradation (55). To our knowledge, there have been no previous reports about the effect of thermal cycling on the flexural strength of PA denture base materials; therefore, we were unable to compare the results of the present study.
Conclusion
PA and PMMA resins can be used in the fabrication of removable prostheses when the patient must use the prostheses for a long period of time. The denture base material should be selected according to the needs of the patients, including anatomic, allergic and aesthetic factors. Further studies should evaluate the improvement of thermoplastic nylon to overcome certain disadvantages and to make PA a useful alternative to PMMA. One limitation of the present study might be the mechanical effect of chewing forces including repeated loads.
Within the limitations of this in vitro study, some conclusions can be drawn. A statistically significant difference was found between PA and PMMA resins in terms of Ra, hardness and transverse strength values before and after thermal cycling. Thermal cycling did not significantly affect the Ra, hardness or transverse strength of either PA or PMMA denture base materials.
Footnotes
Financial support: None received.
Conflict of interest: The authors state that they have no conflict of interest in this study.
