Abstract
Background
Tobacco smoking is the cause of many preventable diseases and premature deaths in the UK and around the world. It poses enormous health- and non-health-related costs to the affected individuals, employers, and the society at large. The World Health Organization (WHO) estimates that, globally, smoking causes over US$500 billion in economic damage each year.
Objectives
This paper examines global and UK evidence on the economic impact of smoking prevalence and evaluates the effectiveness and cost effectiveness of smoking cessation measures.
Study Selection
Search Methods
We used two major health care/economic research databases, namely PubMed and the National Institute for Health Research (NIHR) database that contains the British National Health Service (NHS) Economic Evaluation Database; Cochrane Library of systematic reviews in health care and health policy; and other health-care-related bibliographic sources. We also performed hand searching of relevant articles, health reports, and white papers issued by government bodies, international health organizations, and health intervention campaign agencies.
Selection Criteria
The paper includes cost-effectiveness studies from medical journals, health reports, and white papers published between 1992 and July 2014, but included only eight relevant studies before 1992. Most of the papers reviewed reported outcomes on smoking prevalence, as well as the direct and indirect costs of smoking and the costs and benefits of smoking cessation interventions. We excluded papers that merely described the effectiveness of an intervention without including economic or cost considerations. We also excluded papers that combine smoking cessation with the reduction in the risk of other diseases.
Data Collection and Analysis
The included studies were assessed against criteria indicated in the Cochrane Reviewers Handbook version 5.0.0.
Outcomes Assessed in the Review
Primary outcomes of the selected studies are smoking prevalence, direct and indirect costs of smoking, and the costs and benefits of smoking cessation interventions (eg, “cost per quitter”, “cost per life year saved”, “cost per quality-adjusted life year gained,” “present value” or “net benefits” from smoking cessation, and “cost savings” from personal health care expenditure).
Main Results
The main findings of this study are as follows:
The costs of smoking can be classified into direct, indirect, and intangible costs. About 15% of the aggregate health care expenditure in high-income countries can be attributed to smoking. In the US, the proportion of health care expenditure attributable to smoking ranges between 6% and 18% across different states. In the UK, the direct costs of smoking to the NHS have been estimated at between £2.7 billion and £5.2 billion, which is equivalent to around 5% of the total NHS budget each year. The economic burden of smoking estimated in terms of GDP reveals that smoking accounts for approximately 0.7% of China's GDP and approximately 1% of US GDP. As part of the indirect (non-health-related) costs of smoking, the total productivity losses caused by smoking each year in the US have been estimated at US$151 billion. The costs of smoking notwithstanding, it produces some potential economic benefits. The economic activities generated from the production and consumption of tobacco provides economic stimulus. It also produces huge tax revenues for most governments, especially in high-income countries, as well as employment in the tobacco industry. Income from the tobacco industry accounts for up to 7.4% of centrally collected government revenue in China. Smoking also yields cost savings in pension payments from the premature death of smokers. Smoking cessation measures could range from pharmacological treatment interventions to policy-based measures, community-based interventions, telecoms, media, and technology (TMT)-based interventions, school-based interventions, and workplace interventions. The cost per life year saved from the use of pharmacological treatment interventions ranged between US$128 and US$1,450 and up to US$4,400 per quality-adjusted life years (QALYs) saved. The use of pharmacotherapies such as varenicline, NRT, and Bupropion, when combined with GP counseling or other behavioral treatment interventions (such as proactive telephone counseling and Web-based delivery), is both clinically effective and cost effective to primary health care providers. Price-based policy measures such as increase in tobacco taxes are unarguably the most effective means of reducing the consumption of tobacco. A 10% tax-induced cigarette price increase anywhere in the world reduces smoking prevalence by between 4% and 8%. Net public benefits from tobacco tax, however, remain positive only when tax rates are between 42.9% and 91.1%. The cost effectiveness ratio of implementing non-price-based smoking cessation legislations (such as smoking restrictions in work places, public places, bans on tobacco advertisement, and raising the legal age of smokers) range from US$2 to US$112 per life year gained (LYG) while reducing smoking prevalence by up to 30%–82% in the long term (over a 50-year period). Smoking cessation classes are known to be most effective among community-based measures, as they could lead to a quit rate of up to 35%, but they usually incur higher costs than other measures such as self-help quit-smoking kits. On average, community pharmacist-based smoking cessation programs yield cost savings to the health system of between US$500 and US$614 per LYG. Advertising media, telecommunications, and other technology-based interventions (such as TV, radio, print, telephone, the Internet, PC, and other electronic media) usually have positive synergistic effects in reducing smoking prevalence especially when combined to deliver smoking cessation messages and counseling support. However, the outcomes on the cost effectiveness of TMT-based measures have been inconsistent, and this made it difficult to attribute results to specific media. The differences in reported cost effectiveness may be partly attributed to varying methodological approaches including varying parametric inputs, differences in national contexts, differences in advertising campaigns tested on different media, and disparate levels of resourcing between campaigns. Due to its universal reach and low implementation costs, online campaign appears to be substantially more cost effective than other media, though it may not be as effective in reducing smoking prevalence. School-based smoking prevalence programs tend to reduce short-term smoking prevalence by between 30% and 70%. Total intervention costs could range from US$16,400 to US$580,000 depending on the scale and scope of intervention. The cost effectiveness of school-based programs show that one could expect a saving of approximately between US$2,000 and US$20,000 per QALY saved due to averted smoking after 2–4 years of follow-up. Workplace-based interventions could represent a sound economic investment to both employers and the society at large, achieving a benefit–cost ratio of up to 8.75 and generating 12-month employer cost savings of between $150 and $540 per nonsmoking employee. Implementing smoke-free workplaces would also produce myriads of new quitters and reduce the amount of cigarette consumption, leading to cost savings in direct medical costs to primary health care providers. Workplace interventions are, however, likely to yield far greater economic benefits over the long term, as reduced prevalence will lead to a healthier and more productive workforce.
Conclusions
We conclude that the direct costs and externalities to society of smoking far outweigh any benefits that might be accruable at least when considered from the perspective of socially desirable outcomes (ie, in terms of a healthy population and a productive workforce). There are enormous differences in the application and economic measurement of smoking cessation measures across various types of interventions, methodologies, countries, economic settings, and health care systems, and these may have affected the comparability of the results of the studies reviewed. However, on the balance of probabilities, most of the cessation measures reviewed have not only proved effective but also cost effective in delivering the much desired cost savings and net gains to individuals and primary health care providers.
Keywords
Background
It is a known fact that both active and passive smoking are damaging to human health and have associated economic costs. Cigarette smoking is the cause of many preventable diseases, a leads to premature deaths, and accounts for a significant proportion of many health inequalities. The World Health Organization (WHO) currently estimates that each year smoking accounts for about ~6 million deaths worldwide and causes about half a trillion dollars in economic damage annually. 1 This number of smoking-attributable deaths is expected to rise to 7 million by 2020 and to more than 8 million a year by 2030 if the current rate of smoking continues unabated. 2 According to recent statistics from the Action on Smoking and Health, 3 smoking causes ~80% of deaths from lung cancer, ~80% of deaths from bronchitis and emphysema, and ~17% of deaths from heart disease. More than one quarter of all cancer deaths can be attributed to smoking. These include cancer of the lung, mouth, lip, throat, bladder, kidney, pancreas, stomach, liver, and cervix. It is also estimated that globally 600,000 deaths a year are caused by second-hand smoke, and most of these deaths occur among women and children.
Cigarette smoking is a major contributor to chronic obstructive pulmonary disease, peripheral and cerebrovasular disease, coronary artery disease (CAD), cancer of the lung or pharynx, larynx, oesophagus, pancreas, bladder, kidney and cervix, peptic ulcer disease, and nonmalignant diseases of the mouth,134,135 among other smoking-induced illnesses.
The US center for Disease Control and Prevention also reported that cigarette smoking is the proximate cause of over 440,000 premature deaths annually, of which 50,000 is attributable to second-hand smoke.4–6 Recent statistics from the British National Health Service (NHS) Health and Social Care Information Centre 7 shows that smoking accounts for about 100,000 deaths a year in the UK (79,100 in England, 13,000 in Scotland, 5,600 in Wales, and 2,300 in Northern Ireland). This compares with similar studies for UK in 2009, which showed that there were 109,164 deaths due to smoking (19% of all deaths in the UK), of which 27% deaths in men and 11% deaths in women can be traced to smoking. 8 These figures no doubt show that addiction to cigarette smoking poses a lot of health risk and could be loosely described as a death sentence in disguise. Reducing the prevalence of this menace is thus a worthy cause for health care professionals, the government, and society at large.
This paper reviews the major studies on the economics of tobacco smoking and the economic impact of reducing its prevalence. The paper examines the following research questions:
What are the economic costs and benefits of smoking?
How effective and cost effective are smoking cessation measures in terms of delivering cost savings and net gains to individuals and primary health care providers?
The economic impact of smoking is twofold: the costs of tobacco use itself, and the costs of reducing its prevalence among smokers. Beyond the face value of cigarette purchases, the costs of tobacco use have more far-reaching health and economic implications on private individuals, families, employers, and taxpayers. The costs of smoking have thus been classified as direct, indirect, and intangible. The direct costs of smoking include the cost of illness due to smoking on affected patients, and the health care expenditure involved in the treatment of smoking-related illnesses (eg, cost of drugs and administrative services). In the UK, direct costs of smoking arise from GP consultations, prescriptions for drugs, and various costs related to treating diseases attributable to smoking. 7 Direct costs could also include the resources used up by other agencies and charitable organizations. 9 The World Bank estimates that about 15% of the aggregate health care expenditure in high-income countries can be attributed to smoking.10,11 In the UK, the direct costs of smoking to the NHS have been estimated at between £2.7 billion and £5.2 billion, which is equivalent to around 5% of the total NHS budget each year.3,7,8,12–14 Smoking also poses considerable indirect costs to society and the nonsmoking public, eg, costs of second-hand smoking, costs to employers in the form of loss of productivity and absenteeism of smokers owing to smoking-related illnesses. 15 In addition, smoking-induced fires, sickness/invalidity benefits, litter, etc are all negative externalities of smoking to society. The direct and indirect costs of smoking can be measured b and hence are tangible costs, whereas there are some costs that cannot be easily quantified, such as loss of life, and the burden of pain and suffering caused by smoking-induced illness.16,17 These unquantifiable costs are often referred to as the intangible costs of smoking.
For example, evidence from Kahende et al 5 show that in the US, the medical costs (part of direct costs) and productivity losses (part of indirect costs) caused by cigarette smoking can be estimated to be worth US$193 billion annually.
Just as there are costs emanating from smoking, there are also benefits associated with reducing the incidence or prevalence of smoking. Benefits here refer to the losses that could be avoided by the individuals who quit smoking, such as cost savings from smoking in terms of reduced morbidity and mortality, reductions in the costs of illness, and the marginal risk of disease. 18 Other benefits of reducing smoking prevalence are longevity and improvement in the quality of life of quitters and passive smokers, improved workplace productivity, reduced costs of cleaning up the environment after smoking, reduction in fires caused by smoking, and the resulting damage or destruction, as well as a healthier population, among other benefits. There is a growing body of literature suggesting that smoking cessation interventions, coupled with regulations and legislations, are effective ways to reduce smoking prevalence.16,17,19,20 Furthermore, there is evidence to suggest that smoking cessation interventions are among the most cost-effective and economically reasonable ways of appropriating health care resources.5,9–11,21–27
This study attempts to review the existing evidence on the economic, health-related, and non-health-related impact of reducing smoking prevalence. First, we summarize the search methods and selection procedure used to conduct the systematic review, and then we examine the quality assessment method used in evaluating the study quality. The paper utilizes two main approaches used by medical researchers for economic evaluation c : cost-effectiveness analysis (CEA) and cost–benefit analysis (CBA). These are discussed in detail in Section “Measures of Evaluating Economic Impact”. The aim of this paper is to identify evidence on the effectiveness and cost effectiveness of smoking cessation interventions and also to identify data that may be of use in the economic modeling of the cost savings and net benefits derivable from investing in smoking cessation programs in the UK. Two specific pieces of work are presented in this review. The Section “Global Evidence on the Economics of Smoking” examines the evidence globally on the costs and benefits attributable to smoking, and then reviews the literature on the effectiveness and cost effectiveness of smoking cessation programs across countries. These will be examined under six broad headings: 1) pharmacological treatment interventions, 2) policy-based interventions, 3) community based interventions, 4) telecoms, media, and technology (TMT)-based interventions, 5) school-based interventions, and 6) workplace- or employer-based interventions. The second major segment of this review (“The Economic Impact of Smoking and Smoking-cessation Interventions in UK”) examines the economic impact of smoking in the UK. The rationale for narrowing down to UK is to assess how these various types of interventions are applied in a single country case study. Here, the costs and benefits of smoking in the UK are examined, as well as the effectiveness and cost effectiveness of UK-specific smoking cessation intervention programs. The Section “Discussion” discusses the main findings of the review by comparing results across types of intervention, across countries, and across measurement outcomes, and in some cases, providing the range of costs or cost savings for each intervention by combining costs from multiple sources. The section also discusses some of the known limitations of the study.
Other approaches that are not considered in this analysis include Cost Analysis (CA) and Cost Utility Analysis (CUA)–-see Kahende et al 5 ).
Research Methods
Search Methods and Selection Criteria: Overview
A systematic review produced several studies, out of which a total of 99 literature sources on the economics of smoking and of reducing smoking prevalence were used for the review. We captured major economic studies on the health and economic impact of smoking and cost effectiveness of tobacco policies published between 1992 and 2014, but included only eight relevant studies before 1992. We also performed hand-searching of relevant articles, which produced additional 52 papers, including useful non-economic studies, and health reports and white papers issued by government bodies, international health organizations and health intervention campaign agencies that are usually not included in the electronic databases. This brings the total number of studies included in the review to 151. Of this number, 123 were strictly peer-reviewed medical journals, while 28 were useful government (public health) reports and white papers. This paper benefits strongly from the inclusion and synthesis of high-level evidence from mostly recent studies (eg, 2005–2014), with the implication that newer and better methods, indicators, or measures have been reported in order to aid economic modeling.
Study Outcomes
Primary outcomes of the selected studies are smoking prevalence, direct and indirect costs of smoking, and the costs and benefits of smoking cessation interventions (eg “cost per quitter”, “cost per quality of life year gained”, “cost per life saved”, “present value” or “net benefits” from smoking cessation, and “cost savings” from personal health care expenditure).
Identification of Studies
Two main electronic databases were searched. These are PUBMED (January 1992 to July 2014) and CRD (NIHS) (January 1992 to July 2014). The reason for the selection of these databases is that they are both very comprehensive databases containing health care-related studies. For example, PUBMED contains more than 23 million citations for biomedical literature from MEDLINE. The CRD database also contains the NHS Economic Evaluation Database, the Cochrane Library of Systematic Reviews in health care and health policy, and other health care-related bibliographic sources. To identify relevant studies for this review, we used a detailed search strategy for each database. These were based on the search strategy developed for PUBMED but revised appropriately for each database to take account of differences such as vocabulary and syntax rules. Key terms used were “economic” or “costs”, or “cost effectiveness” and “smoking”, or “tobacco” for the international evidence section, while the search strategy for the UK segment of the study included “UK” to the list of key words (see Supplementary File 1). Other keywords used were “tobacco control”, “smoking reduction”, and “smoking cessation”. We also performed hand searches on other databases such as EconLit, Science Direct, JSTOR, Cochrane Library, and Google Scholar using the same keywords, and this produced most of the papers already contained in PUBMED/MEDLINE and CRD. Unpublished reports, abstracts, brief and preliminary reports were considered for inclusion on the same basis as published reports. There was no restriction based on language or date.
Data Collection and Analysis
Selection of Studies
The authors read all titles and/or abstracts resulting from the search process, and any irrelevant studies were removed. Full copies of the remaining potentially relevant studies were obtained and assessed independently by the authors to ensure that these clearly met all inclusion criteria. Those that were clearly irrelevant or had insufficient information to make a decision were excluded, or the authors were contacted for further information to aid the decision process. Decisions were based on inclusion criteria, ie, types of studies, types of participants, interventions, and outcome measures used. Variations in authors’ opinion were resolved through discussion and consensus.
Under the review of international (non-UK) evidence in Section “Global evidence on the economics of smoking”, we assessed and summarized 36 papers on the costs and benefits of smoking as well as 65 papers on the effectiveness and cost effectiveness of smoking cessation interventions across countries. Though a substantial part of the evidence on the economics of smoking were drawn from the United States, we tried as much as possible to reflect pockets of evidence from other countries around the world, especially from China, the largest producer and consumer of tobacco products, as well as from Australia, Hong Kong, Korea, Thailand, Taiwan, Sweden, France, Belgium, Denmark, India, Turkey, Netherlands, and Canada.26,28–42 These countries appear to be known to have carried out comprehensive tobacco control policies. This study reviewed only relevant papers on the effectiveness and cost effectiveness of smoking cessation under six headings: pharmacological interventions (8), policy-based interventions (19), community-based interventions, (10), TMT-based interventions (12), school-based interventions (5) and workplace- or employer-based interventions (7).
With regard to the UK, in Section “The economic impact of smoking and smoking cessation interventions in UK”, this study reviewed 33 papers, 19 on the costs and benefits of smoking in UK and 14 studies on the effectiveness and cost effectiveness of UK-specific smoking cessation interventions. Cost estimates are mostly expressed in US dollars for international evidence (except where stated otherwise) and in British pounds for UK evidence.
Data Extraction and Management
Data were extracted from published sources using a standard data recording form. Studies that reported primary outcomes were extracted and reviewed. At the first level of screening, we excluded papers that merely described the effectiveness of an intervention without including economic or cost considerations. We also excluded studies that combined smoking cessation with the reduction in the risk of other diseases such as lung cancer, myocardial infarction, chronic obstructive pulmonary disease (COPD), stroke, obesity, diabetes, coronary heart disease, etc. At the second level of screening, we excluded papers in which study design, methods, or outcomes did not appear to be consistent with those of the review as well as publications that appeared more than once in both databases. Figure 1 illustrates the study selection process more clearly.

Flowchart of study selection process.
Risk of Bias
The risk of bias in studies was assessed via the criteria described in version 5.0.0 of Cochrane Reviewers Handbook. 43 This is based on the evaluation of six specific methodological domains (ie, sequence generation, allocation concealment, blinding, incomplete outcome data, selective outcome reporting, and other issues). Generally, the six domains are used by answering a prespecified question about the adequacy of each study in relation to each domain, such that a judgment of “Yes” indicates low risk of bias, “No” indicates high risk of bias, and “Unclear” indicates unclear or unknown risk of bias.
For this review, the following domains were used: sequence generation, allocation concealment (avoidance of selection bias), incomplete outcome data, and selective outcome reporting. Blinding was not possible because of the nature of some of the studies/intervention used.
Measures of Evaluating Economic Impact
We now discuss two methods commonly used by medical researchers for economic evaluation: cost effective analysis (CEA) and cost-benefit analysis (CBA).
Cost Effectiveness Analysis
CEA is a measure of cost savings. It tends to link the cost of an intervention to the health improvements or gains caused by that intervention. Measures of health improvements include cases avoided (CA), hospital days avoided (HDA), deaths averted (DA), and life-years saved (LYS). 5 Other measures include cost per quitter (CPQ) enrolled in community-based cessation programs such as a self-help program, a smoking cessation class, an incentive-based cessation contest, 44 or in a quitline program. 45 The cost effectiveness of a cessation program may not only be looked at in absolute terms but also in relative or comparative terms to other intervention programs because each program may have different dimensions of cost effectiveness. Cost effectiveness is usually measured in ratios. A higher cost effectiveness ratio means that a program is less cost effective than another intervention program. However, Altman et al 44 put forward an argument that the fact that an intervention program yields a high cost effectiveness ratio does not necessarily imply that it is a less desirable outcome. It may well mean that even the most cost-effective program only impacts on a small fraction of the population in need, so that a wiser decision would be to implement as many cost-effective programs that satisfy the needs of more diverse groups of citizens.
Cost–Benefit Analysis
CBA is an economic technique that is used in evaluating the economic soundness or feasibility of an intervention program. CBA measures both the costs and monetary benefits derivable from an intervention, discounted at their present value. Discounting helps to make divergent outcomes of costs and benefits comparable irrespective of the date at which they occur. According to Phillips and Prowle, 22 there are three basic stages involved when conducting a CBA: (1) the costs incurred in the intervention program must be identified, measured, and assessed; (2) the benefits associated with the intervention also has to be identified, measured, and assessed in which case any input–output misalignments or time-dependent outcomes (eg, of a reduction in smoking prevalence) will have to be adjusted; (3) the costs and adjusted benefits are now combined to arrive at a measure of the net present value of outcomes, ie, the difference between the present value of benefits and the present value of costs. If benefits exceed costs, then the intervention is economically viable, and has a positive net benefit. Otherwise, it has a negative net benefit. Another way of looking at this is to estimate the benefit–cost ratio, that is, the present value of benefits divided by the present value of costs. The higher the benefit–cost ratio, the more desirable is the outcome of the intervention. It should be noted that many health researchers find it difficult to attach monetary values to health outcomes, and hence find the technique less useful than CEA and CUA. 5
Global Evidence on the Economics of Smoking
According to the Campaign for Tobacco-Free Kids, 46 the top five cigarette-consuming countries are China, Russia, United States, Japan, and Indonesia. China consumes more than 35% of the world's cigarettes, with 53% of males smoking. Philip Morris International, British American Tobacco, Japan Tobacco International, and Imperial Tobacco are the world's four largest multinational tobacco companies. The largest state tobacco monopoly is the China National Tobacco Corporation, which has the largest share of the global market among all companies. Based on WHO estimates, tobacco use costs the world an estimated $500 billion each year in health care expenditures, productivity losses, fire damage, and other costs. In the US alone, smoking causes more than $193 billion each year in health-related costs, including medical costs and the cost of lost productivity caused by smoking.5,47 New figures from the Campaign for Tobacco-Free Kids show that the social cost of smoking in the US could be estimated at about US$321 billion (ie both smoking-caused health costs of US$170 billion and associated productivity losses of US$151 billion). 59 (See Fig. 2). This section examines the economic costs and benefits of smoking in some detail, citing examples from countries where tobacco is in high demand and use.
Smoking-Attributable Costs and Benefits
As shown earlier, the costs of smoking can be classified into health-related costs and non-health-related costs.
Health-Related Costs
The health care costs associated with tobacco-related illnesses are extremely high. In the United States, total annual public and private health care expenditures caused by smoking amount to approximately US$170 billion. 59 Measured as a proportion of the gross domestic product (GDP), smoking costs in the US are approximately 1% of the GDP. Many studies have estimated the health-related costs of smoking. These costs include medical expenditure on drugs and administration, smoking-attributable morbidity and mortality, medical costs attributable to passive smoking, maternal smoking, and children smoking. Other direct costs include sickness/invalidity benefits attributable to tobacco abuse. A study by Yang et al 48 reveals three ways in which smoking-attributable expenditures could be measured–-average expenditure per in-patient hospitalization (or admission), average expenditure per outpatient visit, and self-medication expenditures. Some other indicators of health care expenditure include smoking-induced emergency and general practitioner visits for adults and children, and use of nursing homes and home-based care. 49
Annual federal and state government smoking-caused Medicaid payments are estimated at US$39.6 billion (federal share: US$22.5 billion; states’ share: US$17.1 billion) (see Fig. 2). State-level estimates from USA revealed that the direct costs of smoking in California in 1999 were US$8.6 billion, with nearly half of this amount (47%) going to hospital care, 24% for ambulatory care, 15% for nursing home care, 13% for prescriptions, and 1% for domestic health care services. 4 Fresh statistics from Campaign for Tobacco-Free Kids 50 on state tobacco-related costs and revenues has revealed that smoking-related medical expenditures in US varied dramatically across states, with a low of US$22.4 million in Wyoming to a high of US$3.31 billion in New York. Another report by Armour et al 51 showed that the proportion of health care expenditure attributable to smoking ranged between 6% and 18% across the different states.

Smoking-attributable expenditure in the United States (USD billion).
The National Drug Strategy in Australia estimated the total social costs of smoking in Australia between 2004 and 2005 at about AUD$31.4 billion, representing 56.2% of total costs of drug abuse in Australia. 16 Of these costs, AUD$12.02 billion or 38.2% was classified as tangible costs, while AUD$19.45 billion or 61.8% was intangible costs. Yang et al 48 estimated the economic burden of smoking for 2008 in China at US$28.9 billion, representing 0.7% of China's GDP and 3% of national health care expenditures. This figure also averaged US$127.30 per smoker. According to the study, mortality costs contributed the most to smoking-attributable costs in China, followed by outpatient expenditures. Results also show that, as a result of high prevalence rate, a whopping 93% of total economic cost of smoking in China was borne by men. Results from Hong Kong reveal that annual health-related cost of smoking in 1998 was US$688 million. 49 The same study shows that about 5,596 deaths in Hong Kong among adults 35 years of age and above in 1998 was attributable to active smoking, while passive smoking accounted for 1,324 deaths. This brings to a total of 6,920 tobacco-related deaths out of 32,847 deaths. In what seems very surprising, passive smoking accounted for 23% of total smoking-related health care costs in Hong Kong, implying a growing risk of the prevalence of passive smoking. In Taiwan, the total smoking-attributable expenditures (SAEs) totaled US$397.6 million, representing 6.8% of the total medical expenditures for people aged 35 years and over. 52 The mean annual medical expenditure per smoker was US$70 more than that of each nonsmoker.
Although the health risks associated with passive smoking d have been well documented in the literature, little is known about the economic costs. Regular exposure to second-hand smoke (SHS) among nonsmokers both at home and in the workplace could be economically costly in as much as it poses enormous health hazards. Following a recent research conducted by Plescia et al 53 on SHS exposure in North Carolina, the total annual cost of treatment for conditions related to such exposure was estimated to be US$293.3 million in 2009. Though the majority of the SHS victims were children, the most common cases were traceable to cardiovascular conditions. In a similar study in Minnesota by Waters et al, 54 the total annual cost of treatment for conditions associated with SHS was estimated to be US$228.7 million in 2008 dollars–-equivalent to US$44.58 per Minnesota resident. Just as passive smoking poses huge health care costs, smoking during pregnancy, otherwise called “maternal smoking”, also has some related cost implications. It is associated with considerably higher child health expenditures as well as increase in overall medical costs. 55 For example, the annual direct medical expenditure for early childhood respiratory illness attributable to maternal smoking totaled US$661 million for all children under the age of six. 56 Further evidence reveals that smoking-attributable neonatal costs in the US represent almost US$367 million in 1996 dollars. 57 Though these costs vary considerably from state to state, they can easily be avoided by implementing temporary cessation programs aimed at pregnant women.
Passive smoking has some causal relationships with coronary heart disease, heart attacks, and chronic respiratory symptoms. For children and infants, SHS exposure can also lead to low birth weight, sudden infant death syndrome (SIDS), childhood respiratory illness and Asthma, amongst others. In US, about 53,000 deaths of non-smokers can be attributed to passive smoking ( 56 :s39).
The foregoing statistics indicate that smoking everywhere is very costly in many respects and takes a huge toll on public finances. For most countries, smoking-attributable costs represent the largest single expenditure in total health care costs, with wider implications for the economy.
Non-Health-Related Costs
Besides the health care costs of smoking, there are other costs that the abuse of tobacco imposes on society, and these costs need not be treated as less important. Tobacco-related illnesses and premature mortality impose high productivity costs to the economy because of sick workers and those who die prematurely during their working years. Lost economic opportunities in highly populated developing countries are likely to be particularly severe as tobacco use is high and growing in those areas. 58 Countries that are net importers of tobacco leaf and tobacco products lose millions of dollars a year in foreign exchanges. Fire damage and the related costs are significant. In 2000, about 300,000 or 10% of all fire deaths worldwide were caused by smoking, and the estimated total cost of fires caused by smoking was US$27 billion. 59 Tobacco production and use also damage the environment and divert agricultural land that could be used to grow food.
The economic loss to employers in the form of workplace absenteeism and the resulting lost productivity of their smoking employees is particularly alarming. In specific terms, employers suffer loss of revenue from the days off work and earnings lost from work owing to smoking-induced illness and premature death of its smoking employees during productive years. It is reported that US smokers are absent from work approximately 6.5 days more per year than nonsmokers. They make about six visits more to the health care centers per year than their nonsmoking counterparts, while dependents of smokers visit health care centers four times more than non-smokers.23,56 Recent US statistics show that the total cost of productivity losses caused by smoking each year amounts to US$151 billion. 47 59 This estimate only includes costs from productive work lives shortened by smoking-caused death, and does not include costs from smoking-caused disability during work lives, smoking-caused sick days, or smoking-caused productivity declines when at work, all of which amount to huge economic losses to the US. In California alone, the annual value of lost productivity owing to smoking-related illness between 2000 and 2004 averaged US$8.54 billion (US$6.87 billion for Florida; US$6.79 billion for Texas, and US$6.05 billion for New York), showing that these US states and many others have lost huge productive hours and potential revenue owing to smoking-induced health problems. These results suggest that, if adequate measures are taken by primary health authorities and employers to promote smoking cessation, there will be huge cost savings from smoking-related illnesses and premature deaths.
Absenteeism and premature deaths represent only a fraction of the aggregate indirect burden of smoking to employers. It may well be that even at work smoking-induced illness could retard the performance of smoking employees and translate into lost time and earnings, which may not be easily quantified. Arguing in this light, Thompson and Forbes 60 noted that productivity losses emanating from smoking for the most part arise from short-term absenteeism or from performance at less than full efficiency due to respiratory problems or other smoking-induced illnesses. However, one cannot overlook the impact of other qualitative factors that lead to absenteeism and reduced productivity such as other health indicators (alcohol, weight, exercise, etc), job characteristics (occupation type, income, employment status, hours worked), and demographic characteristics (age, sex, ethnicity, marital status, education, place of work, etc). Evidence from Bush and Wooden 61 revealed that, even after controlling for these factors, smoking was still highly correlated with work-place absenteeism. In fact, in their 1994 paper on the impact of smoking and alcohol on workplace absence, Bush and Wooden concluded that, after controlling for the effect of other variables, employees on smoking status were found to be 1.4 times more likely to be absent, and ex-smokers were found to be 1.3 times more likely to be absent than nonsmokers. Their results also showed that the probabilities of smoking-induced absenteeism differed considerably by sex. For male smokers, the probability of workplace absence surpassed that of male non-smokers by 1.7 times, while for female smokers the probability of absence fell slightly to 1.2 times more than those females who have never smoked.
Apart from smoking-attributable absenteeism, cigarette smoking and its associated activities can also be economically costly when they are the cause of fires. In the study conducted by Collins and Lapsley, 17 the total cost of smoking-attributable fires in New South Wales, Australia, in 2006/2007 was estimated at AUD$51.4 million, with tangible costs representing over three-quarters of the total cost. In USA, smoking-induced fires lead to the death of 2,300 civilians (men, women, and children inclusive) per year, with additional 5,000 injuries per year.23,56 Besides the health care costs of treating injured or burn victims, direct property damaged from fires induced by tobacco has been valued at US$552 million per year. Other costs to employers of workers who smoke include health care claims and benefits not related to health care. 23 There are also some hidden costs that are economically significant to society but often omitted in most studies for the lack of satisfactory data, eg, costs of paramedical and ambulance services, damage caused by smoking-induced forest fires, toxic effects from tobacco consumption, especially amongst children, as well as accidents and other property loss caused by cigarette smoking apart from fires.
Economic Benefits of Smoking
The cost of smoking notwithstanding, the tobacco industry poses a great deal of benefits, especially to the economy, consumers, and producers. It is therefore imperative to examine the positive economic effects of smoking and, hence, the impact or consequences on these of reducing smoking prevalence. Following previous studies by Thompson and Forbes, 60 Woodfield, 62 and Cohen and Barton, 56 among others, the major benefits of smoking are in economic stimulation, namely income generated from production and consumption, tax yields, employment, and early death of smokers. Taxes on cigarettes have always contributed to government treasury. In 2009, President Barrack Obama signed an act that raised the US federal tax rate on cigarettes from 39 cents to US$1.01 per pack. The 156% tax increase was estimated to earn the US government about US$33 billion in tax over a 4½-year period. There are, however, economic consequences of raising taxes (see “The economics of policy-based interventions” Section).
The World Bank estimates that tobacco farming employs about 33 million people worldwide, and about 15 million of those workers reside in China alone. 63 In China, over 4 million households rely on tobacco for their livelihood, as tobacco farmers, cigarette industry retailers, or employees. 32 In fact, China is the largest producer and consumer of tobacco worldwide. All cigarettes are produced by the Chinese government's tobacco monopoly company, which produces more than 1.7 trillion cigarettes annually. In 2003, the company generated almost US$2 billion in profits and taxes, while income from tobacco represented about 7.4% of centrally collected government revenue. In terms of consumption, China boasts of a smoking population of 350 million active smokers and 460 million passive smokers. In 2010, about 52.9% of Chinese men and 2.4% of women were current smokers. 48 Given that China is the most populous country in the world, this proportion of smokers translates into enormous earning potential.
Apart from the income benefits of tobacco smoking, another source of benefit, especially to the government, of smoking is the substantial cost savings in pension payments from premature death of smokers. This is a highly debated issue in the literature, because it is premised on the thinking that a shorter life expectancy implies a reduced expenditure on pensions. Thus, attempts to promote this will be deemed socially undesirable and hence cannot be incorporated into social policy design.60,62
Clearly, from the above, therefore, if tobacco farming is to be phased out, many households, investors, and the government itself will suffer huge economic losses. Hence there is a need to strike a balance between the costs and benefits of smoking. But this is easier said than done, especially as the health implications of smoking far outweigh any associated economic returns from the perspective of a socially desirable outcome.
Effectiveness and Cost Effectiveness of Smoking Cessation Interventions
Because the health hazards attributable to smoking are very significant, the risks of illness or disease are reduced following smoking-cessation interventions. 19 According to a UK General Household Survey in 1998, about 27% of adults (aged 16 years and above) were smokers, and of this figure about 70% wanted to quit smoking. Data from a similar survey conducted in 1994 by the US health authorities indicated that 46.4% of smokers had made serious attempts to stop in the year preceding the survey, but only 5.7% of smokers managed to abstain from smoking after a period of 1 month or more, and only 2.5% of smokers are able to achieve permanent abstinence each year. The reason for this is smoking is an addiction and can hardly be stopped on the basis of will power alone. Evidence from Feenstra et al 11 shows that only ~3%–7% of smokers who attempt to stop smoking on will power are still abstinent after 1 year. In order to enhance quit rates, there must be some deliberate measures to incentivize cessation. There are different forms of smoking cessation interventions, and they range from pharmacological treatment interventions to policy-based interventions, community-based cessation programs, TMT-based interventions, school-based interventions, and workplace- or employer-based interventions.
The aim of this section is to identify and evaluate cross-country evidence on the effectiveness and cost effectiveness of smoking cessation interventions. The idea of carrying out economic evaluations is to identify which interventions utilize the least resources or have greater cost savings, while being most effective in reducing both the number of smokers and the health- and non-health-related risks associated with smoking. By comparing the costs and outcomes of different alternative interventions, economic evaluations help health care professionals and policy makers in deciding the most efficient use of scarce resources. 24 In estimating the effectiveness of cessation interventions, two major indicators are necessary: the number of long-term quitters and the health gains from smoking cessation, measured according to the age and sex of the quitters. 19 In estimating the cost effectiveness of smoking cessation interventions, emphasis is placed on the impact of such interventions on direct cost reductions with respect to smoking-related morbidity and mortality rates as well as the effect on long-term medical expenditure.
Pharmacological Treatment Interventions
There are several pharmacological agents that are commonly used to aid smokers in their quest to quit smoking. However, we will concentrate on the three major types: nicotine replacement therapy (NRT), bupropion sustained release (SR), and varenicline. These treatment interventions are widely available on prescription, and in the case of NRT as an over-the-counter medication. They are licensed as first-line treatments for use as smoking-cessation aids in the US and the EU, and are widely recommended in many national guidelines. 64
The aim of NRT is to temporarily replace much of the nicotine from cigarettes to reduce motivation to smoke and the physiological and psychological withdrawal symptoms often experienced during a quit attempt, thus easing the transition from cigarette smoking to complete abstinence. It is available in various forms and dosages, including transdermal patches (ie, absorbed slowly through the skin), as chewing gum, oral and nasal sprays, lozenges, sublingual tablets, and inhalers. NRT, in all its commercially available forms, has been found to help people who make a quit attempt to increase their chances of successfully stopping smoking. NRT increase the rate of quitting by as much as 50%–70% regardless of setting. 65
Bupropion was developed as a non-tricyclic antidepressant, and is sometimes preferred by smokers who do not wish to use a nicotine-based treatment, or who have already failed to quit using NRT. The usual dose for smoking cessation is 150 mg once a day for 3 days, increasing to 150 mg twice a day, continued for 7–12 weeks. 64 The quit attempt is generally initiated a week after starting pharmacotherapy. Some studies have shown that bupropion doses up to 300 mg per day does have significant effect in a dose–response fashion on smoking cessation, but does not seem to affect long-term cessation rates (see 66 ).
Varenicline is a selective nicotinic receptor partial agonist, licensed as a prescription-only treatment for smoking cessation in USA in 2006 and in Europe in 2006/2007. The standard regimen is 1 mg twice a day for 12 weeks, with the first week titrated to reduce side effects, and quit date set for the second week. Varenicline has helped ~50% more people to quit than nicotine patch and “other” NRT (tablets, sprays, lozenges, and inhalers) and ~70% more people than nicotine gum. 64 This means that for every 10 people who quit with NRT patch or with “other” NRT, about 15 could be expected to quit with varenicline, and for every 10 who quit with NRT gum, about 17 could be expected to quit with varenicline.
NRT, bupropion, and varenicline all improve the chances of quitting, with low risk of harms, and in some cases, using a combination of these pharmacological treatments could be seen to be even more clinically effective. However, as noted earlier, to justify the investment in any intervention, its effectiveness must be evaluated alongside its cost effectiveness. The cost effectiveness of pharmacological interventions is thus as important as their clinical effectiveness. A review of economic studies on these pharmacological treatment interventions (see Supplementary File 2) showed that varenicline and bupropion (with or without behavioral interventions) are more cost effective than NRT measures such as nicotine gum, patch, lozenge, and inhaler. A recent study by the Canadian Agency for Drugs and Technologies 33 found that, if providers’ willingness to pay (WTP) was greater than US$10,000 per QALY gained, then varenicline was the optimal treatment of choice compared to NRT and bupropion.
Several studies have also found that the use of NRT and/or bupropion SR along with GP counseling is both clinical and cost effective in primary health care. For example, Stapleton et al 67 showed that contingent prescriptions could yield additional life years at a cost between £398 (US$724) and £758 (US$1,380) in 1998 UK pounds compared to brief counseling alone. In a similar estimation of the cost effectiveness of treating nicotine dependence (including NRT and counseling), Croghan et al 68 found the aggregate 1-year smoking rate to be 22% with a cost of $9,231 per net life year gained. This cost compares favorably with other medical services that rely only on GP counseling however brief or intensive. Although NRT products can be purchased over the counter, many people have suggested that free NRT treatments yield more positive results in terms of number of quitters than other cessation interventions. For example, Ong and Glantz 69 found that in Minnesota, a free NRT program would generate 18,500 quitters at a cost of US$4,440 per quality of life adjusted years (QALY) compared to implementing a smoke-free workplace policy, which would generate 10,400 quitters at US$506 per QALY.
Nielsen and Fiore 70 conducted a CBA of bupropion SR and nicotine transdermal patch (NTP) to see which of the two, or whether a combination of both, was more cost effective for smoking cessation. The results revealed that bupropion is more cost beneficial than either NTP or bupropion and NTP together, producing a net benefit in the first post-quit year of up to £338 per employee who attempts to quit compared with US $26 for NTP only, US$178 for the two combined, and US$258 for placebo, another pharmaceutical therapeutic that was used in the clinical trials. Thus, according to this study, bupropion is able to offer the most substantial monetary benefits than any other pharmacological treatment. In a more recent study by Bolin et al, 31 the cost effectiveness of varenicline was compared with nicotine patches for smoking cessation in four European countries (Belgium, France, Sweden, and UK). Surprisingly, the results showed that the use of varenicline for smoking cessation was associated with reduced smoking-related morbidity and mortality more than was the case using NRT. The number of morbidities avoided per 1,000 smokers who made attempts to quit ranged from 9.7 in Belgium to 6.5 in UK. The number of QALY gained, per 1000 smokers, was 23 in Belgium, 19.5 in France, 29.9 in Sweden, and 23.7 in UK. The results of the base-case simulations revealed that, with the exception of France, varenicline treatment appeared to be more cost effective and cost saving than NRT. Thus, funding varenicline as a smoking cessation aid is an economically justifiable use of health care resources in these countries.
The Economics of Policy-Based Interventions
This subsection takes a look at the global evidence on the economic consequences of policy-based measures that aid smoking cessation. These include price-based measures (eg, increase in tobacco taxes, limitations on tobacco crop subsidies) and non-price measures (eg, no smoking regulations at work and in public places, restriction on sales to minors, and bans on promotion and advertising, etc). Legislative bans could either ban smoking completely (comprehensive) or restrict it to designated areas (partial). Both price-based measures and legislation-based smoking bans or restrictions have been found to yield both health and economic gains, including (1) reduction in smoking prevalence though reductions in the demand for and consumption of cigarettes, (2) significant reductions in the incidence of smoking-related diseases and deaths, (3) reduction in smoking-related medical costs, and (4) large gains in cumulative life years and QALYs.23,36,37,71–79
Increase in Tobacco Taxes
The most widely used measure to reduce the demand for tobacco is increase in taxes. This puts an upward pressure on tobacco prices, and higher tobacco prices tend to significantly reduce the consumption of tobacco.74,77 According to a World Bank report, 63 when taxes are raised on tobacco, consumption decreases especially in young people; a 10% cigarette price increase results in a 7% decrease in smoking by young people and 4% by the general public. It has also been hypothesized that a price increase of 10% would reduce smoking by 4% in high-income countries and by about 8% in low-and middle-income countries.23,71 In other words, the price elasticity of demand for tobacco is higher in low- and middle-income countries and among populations of young or teenage smokers who are the most responsive to price changes. Smokers in high-income countries are, however, less responsive to price changes. According to Atkinson and Townsend, 80 low price sensitivity means that the revenue argument against tax increases is rather unconvincing. As long as prices do not respond proportionately to tax increases (ie, price elasticity of less than 1), the revenue from tobacco will surely increase when taxes go up since “a fall in consumption is more than offset by the extra tax paid by those who continue to smoke” (pp. 492). Thus, according to Atkinson and Townsend, so long as the reduction in tobacco consumption is attributable to increased duty, the amount of corporate revenue from tobacco is likely to remain unaffected. The World Bank has recommended that “Governments increase tobacco tax to about 65% of retail price”. 63 Increasing tobacco prices also increases the chances of cigarette theft, smuggling, and counterfeiting. The Mackinac Center on Public Policy estimates that profits made illegally from smuggling cigarettes to the US could amount to be between US$10 billion and US$17 billion. 81 Over the years, tobacco tax increases have brought about increases in revenue for the government, even when the incidence of smuggling and tax evasion are discounted. Currently, in most high-income countries where tobacco control policies are very comprehensive, tobacco taxes represent between two-thirds and four-fifths of the retail price of cigarettes, whereas in low- and middle-income countries, they are generally below 50% of the total price.
Apart from the decline in tobacco consumption via increased prices, raising cigarette taxes also poses some potential health and cost-saving benefits. Reduced tobacco consumption leads to a reduction in health care costs as former smokers and their children do not require as much medical care or treatment as they used to. 23 There is also another argument that says that huge tobacco taxes are equitable in the sense that it makes the tobacco industry pay more for the huge economic burden placed by its products to the health care system as well as the negative externalities of same to society. The income generated from tobacco taxes can also be used to finance community education and advertising against tobacco. In China, the largest producer and consumer of tobacco, a recent tobacco tax adjustment has just been implemented and, if this tax increase passes through to retail prices, it is expected to reduce the number of smokers by 630,000 saving 210,000 lives, at a price elasticity of -0.15. 32 Following the same model, a tax increase of 1RMB (or US$0.13) per pack of cigarettes is expected to increase the revenue accruable to the Chinese government by 129 billion RMB (US$17.2 billion), reduce consumption by 3.0 billion packs of cigarettes, reduce the number of smokers by 3.42 million, and save 1.14 million lives. These figures indicate that tobacco tax increase in China can be construed as the most cost-effective measure of smoking cessation.
In summary, tobacco tax increases reduces tobacco consumption via higher cigarette prices, raises government revenue, saves more lives, preserves employment, and reduces tobacco farming. However, whether or not tax increases lead to loss of revenue in the tobacco industry is still a subject of debate, as smuggling and tax evasion help to minimize any losses arising from taxation.
Smoking Restrictions in the Work Place and in Public Places
It is in recognition of the dangers of passive smoking that many governments institute no smoking restrictions in public places (eg, bars, restaurants, public buses, trains, airports, government buildings, and other public facilities) and private workplaces. Governments are now increasingly sensitive to the need to protect its citizens from the externalities caused by environmental tobacco smoke. Evidence from the US and Canada suggests that smoke-free air policies are associated with a significant reduction in cigarette consumption.23,71,82 In a report issued by the United States Environmental Protection Agency, the costs and benefits of a proposed national smoke-free environment act were modeled to identify its net benefits. The proposed policy was meant to curtail significantly smoking in public places entered by more than 10 people per week. The costs considered were costs of implementing and enforcing the restriction, costs of building and maintaining smoking lounges, among other costs. The benefits included savings from smoking-related medical expenditures, heart diseases averted, the value of lives saved, costs averted by a reduction in smoking-induced fires, and gains in productivity. 83 The net present value to society was estimated to fall between US$42 and US$78 billion, and this range was obtained by considering high and low estimates of costs and benefits. In another study by the Stephens et al, 82 they analyzed the relationship between cigarette prices and no-smoking bylaws to the prevalence of smoking in Canada. Results from a comparison of price and policy differences among Canadian provinces showed that the tendency of being a smoker falls with rising cigarette prices and with widespread no-smoking regulations, even after controlling for age, sex, education, and marital status of respondents. They thus concluded that no smoking regulations should be accompanied by an increase in cigarette prices to be more effective. If either were used in isolation, the outcomes will likely produce a lesser impact than the two measures used together.
Bans on Tobacco Advertisement
Tobacco remains the second most heavily advertised product in the United States besides the automobile industry. 23 Over the years, it has been widely advocated that bans be placed totally on cigarette advertisements and promotional activities. In many countries, this bill has been a subject of controversy or debate. There are those who argue that a partial ban on advertisement has little or no effect on cigarette consumption.71,80 This is because, most adverts, particularly the tobacco-industry-related ones only reveal the brands smoked instead of the quantity smoked. In this sense, therefore, it is difficult to measure the impact of increased or reduced advertising on tobacco consumption. In addition, companies affected by such legislation could seek to utilize alternative forms of media. In an econometric study on high-income countries, Saffer and Chaloupka 84 noted that comprehensive bans on tobacco advertising tend to reduce consumption.
Community-Based Intervention Programs
Smoking cessation programs also come in the form of community-based interventions to educate, inform, and assist smokers in their quitting attempts. According to Secker-Walker et al, 85 a community intervention is defined as “a co-ordinated, multi-dimensional programme aimed at changing adult smoking behaviour, involving several segments of the community and conducted in a defined geographical area, such as a town, city, country, or other administrative district” (pp. 3). These programs could range from community pharmacy-based interventions to group-based counseling, incentive-based smoking cessation contests, use of self-help quit smoking kit, and, in some cases, mass media campaigns directed at certain communities within a defined geographical area. The aim of this section is to identify and assess global evidence on the effectiveness and cost effectiveness of such interventions.
Nine studies on community-based interventions were reviewed, including studies by Altman et al, 44 Secker-Walker et al, 86 Stephens et al, 82 Secker-Walker et al,87,88 Lightwood et al, 89 Hurley and Matthews,26,30 and Simpson and Nonnemaker. 90 Altman et al, as far back as 1987, studied the cost effectiveness and cost distribution of three community-based smoking cessation programs designed for use in the two education communities of the Stanford Five City Project. These programs included (1) smoking cessation class (eight 1-hour training sessions offered to ~8–25 participants where several quitting techniques were taught); (2) incentive-based smoking cessation contest (a 6-week community smoking cessation prize contest where entrants were assessed and rewarded on the basis of their smoking status and habits); and (3) self-help quit smoking kit (included tips on smoking replacement habits, social support available, public commitment, and record keeping and goal setting, among other tips aimed at providing specific actions to aid individual smoking cessation). Results revealed that the self-help quit had the lowest total cost (US$26,190), lowest quit rate (21%), lowest time requirement for participants, and was the most cost effective (with a CER of $50). However, the smoking cessation class was the most effective, requiring the most time from participants, with a quit rate of 35%, but incurring the highest total costs (US$261,589) and was also least cost effective (US$276). The smoking cessation contest was in-between the other two programs, with a total cost of US$82,925, a quit rate of 22%, and a CER of US$151.
A community pharmacy also provides an excellent setting in which to provide a smoking cessation program, as the pharmacy would have regular contact with residents of the area. Thavorn and Chaiyakunapruk 30 evaluated the incremental cost effectiveness of a community-pharmacist-based smoking cessation (CPSC) in Thailand. They found that the CPSC program yielded cost savings and life year gains to the health system. A series of sensitivity analyses, however, demonstrated that both cost savings and life year gains were sensitive to variations in discount rate and long-term smoking quit rate associated with the intervention (see Supplementary File 2 for more details on the results).
Lightwood et al 89 also examined the effect of California's Tobacco Control Program (CTCP) on aggregate personal health expenditures in the state. The CTCP, which was established in 1989, offered a comprehensive approach to smoking cessation by altering the existing social norms and values among tobacco users. The campaign featured an aggressive media campaign with three themes, namely the tobacco industry lies, nicotine is addictive, and second-hand smoke kills. It also included a radical public policy change, especially in the area of promoting smoke free environments. The findings of the study revealed that, between 1989 and 2004, the California program led to a reduction in personal health care expenditures to the tune of US$86 billion (in 2004 dollars), which would have been expected without the program. Using 95% confidence interval, the cost savings ranged between $28 billion and US$151 billion.
Hurley and Matthews 26 also presented evidence on the cost effectiveness of Australia's National Tobacco Campaign (NTC), an intensive mass media antismoking campaign, which was launched in 1997. Using a quit benefits model (QBM), the study predicted that the NTC avoided more than 32,000 cases of COPD, 11,000 cases of acute myocardial infarction, 10,000 cases of lung cancer, and 2,500 cases of stroke. The model also predicted the prevention of about 55,000 deaths, 323,000 life-years gain, and 407,000 QALYs, as well as a health care cost savings of AUD$740.6 million. Thus, the NTC was both effective and cost saving.
The above studies as well as other community-based interventions all reveal that a strong and aggressive tobacco control program do not only reduce the number of smokers and its resulting health benefits but also reduce substantially the health care expenditure associated with smoking prevalence. It is worth noting that the benefits of these initiatives may not have been well established quantitatively in the sense that most of these studies reflect potential uncertainty in the estimates and data used as well as differences in the parameters estimated. In some cases, data sufficient to establish definite causality are also lacking. However, on the balance, the community-based cessation initiatives examined appear to yield substantial net benefits.
Telecoms, Media, and Technology-Based Interventions
TMT-based interventions refer to electronic and mass media-related means aimed at offering support to effect changes in smoking behavior in adults and young adolescents. Examples include telephone counseling offered through “quitlines” or “helplines”; radio, TV, and print media; and computer and Internet-based intervention programs. A summary of the results of related TMT-based cost effectiveness studies can be found in Supplementary File 2.
Telephone Counselling, Quitlines and Text Messaging
Telephone services can provide information and support for smokers. Counseling may be provided proactively or offered reactively to callers to smoking cessation helplines. 91 Support can be given in individual counseling sessions or in a group therapy where clients can share problems and derive support from one another. Counseling may be helpful in planning a quit attempt and could assist in preventing relapse during the initial period of abstinence. Although intensive face-to-face intervention increases quit rates, there are difficulties in delivering it to large numbers. Telephone counseling may be a way of providing individual counseling more affordably.
Tomson et al 45 examined the cost effectiveness of the Swedish quitline, a free-of-charge service offered to the smoking population in Sweden to aid cessation. About 31% of the study population (354 callers) reported abstinence after 1 year of the implementation of the scheme, leading to an accumulated number of life year saved of 2,400. The cost per quitter ranged between US$311 and US$401. In comparison with other smoking cessation interventions, the study concluded that the Swedish quitline was cost effective. A more recent study by Rasmussen 40 assessed the cost effectiveness of the Danish smoking cessation telephone service “quitline”. The study was based on the number of quitline callers in 2005. A total 511 ex-smokers were estimated to have gained 2172 life years based on prolonged abstinence over 12 months. Discounting life years (LYs) at 3% per annum, the costs per LYS are €213 for ex-smokers with continued abstinence and €137 for ex-smokers with point prevalence abstinence. The sensitivity analysis for a worst case scenario indicates that the costs per LYS are €1199. The author concluded that the Danish reactive telephone counseling to aid smoking cessation appears to be cost effective in comparison with other Danish smoking cessation interventions.
Farrelly et al 92 took a rather different dimension to the study of quitlines by assessing the relative effectiveness and cost effectiveness of television, radio, and print advertisements in generating calls to the New York smokers’ quitline. The results showed that there was a positive and statistically significant association between the call volume and expenditures for television (P < 0.01) and radio (P < 0.001) advertisements and a slightly significant effect for expenditures on newspaper advertisement (P < 0.065). Though television advertising had the largest effect on call volume, differences in advertising costs for different media implied that call volume on the quitline was least responsive to increases in expenditure on television advertising (0.1%) per US$1000 increase compared to the other mass media: radio (5.7%) and newspaper (2.8%). While it was difficult to determine the optimal mix of expenditures, the bottom line is that all three mass media effectively raised the number of callers to the New York quitline.
Another telecom-based intervention measure is the use of mobile phone text messaging facilities to aid smoking cessation. A study by Guerriero et al 93 used a cohort simulation model to determine the cost effectiveness of smoking cessation support delivered by mobile phone text messaging in the UK, called “Txt2stop”. The cost effectiveness was measured in terms of cost per quitter, cost per life year gained, and cost per QALY gained. The cost of text-based support per 1,000 enrolled smokers was £16,120, which, given an estimated 58 additional quitters at 6 months, equates to £278 per quitter. However, when the future NHS costs saved (as a result of reduced smoking) are included, text-based support would be cost saving. It is estimated that 18 LYs are gained per 1,000 smokers (0.3 LYs per quitter) receiving text-based support, and 29 QALYs are gained (0.5 QALYs per quitter). The deterministic sensitivity analysis indicated that changes in individual model parameters did not alter the conclusion that this is a cost-effective intervention. Similarly, the probabilistic sensitivity analysis indicated a .90% chance that the intervention will be cost saving.
Mass-Media-Led Interventions
Mass media interventions consist of the dissemination through television, radio, print media, and billboards of cessation-related messages, informing smokers and motivating them to quit. Mass media campaigns can be effective in keeping tobacco control on the social and political agenda, in reinforcing community action, and in triggering other interventions. Campaigns are designed either directly to change individuals’ smoking behavior (the risk factor model) or to catalyze other forces of social change (the social diffusion model), which may then lead to change in the social norms about smoking. 94 Social diffusion campaigns, such as those run in Australia, Canada, UK, Thailand, and in some US states, are designed to de-normalize smoking, thus counteracting the tobacco industry's message that smoking is desirable and harmless.
While many studies have revealed that mass media interventions are effective in reducing smoking prevalence among adults, not many studies have commented on the cost effectiveness of such campaigns. Villanti et al 95 evaluated the cost effectiveness of the American Legacy Foundation's national “EX” campaign, which ran on radio and TV in 2008 and was designed to promote smoking cessation among adult smokers. The incremental societal cost of EX, in 2009 dollars, was US$166 million. Data from eight designated media market areas studied indicate that, in a hypothetical nationwide cohort of 2,012,000 adult smokers ages 18–49, EX resulted in 52,979 additional quit attempts and 4,238 additional quits and saved 4,450 QALYs. Incremental cost-utility estimates comparing EX to the status quo–-that is, the situation that would have existed in eight markets with no campaign and no change in cessation behavior–-ranged from a cost of US$37,355 to US$81,301 per QALY, which suggests that the campaign was cost effective. These findings are consistent with previous evidence that national mass media campaigns for smoking cessation in the US can lower smoking prevalence in a cost-effective manner. However, in a study on the cost effectiveness of online, radio, and print tobacco control advertisements targeting 25–39-year-old males in Australia, Clayforth et al 42 found that online advertising could be more cost effective than other non-television advertising media such as radio and press in reaching and affecting target audiences, implying that online campaigns may be a highly cost-effective channel for low-budget tobacco control media campaigns (see Supplementary File 2 for details).
Computer-And Internet-Based Programs
Personal computers, the Internet, and other electronic aids, which are now an indispensable part of daily life for many people around the world, also offer additional means of effecting changes to smoking behavior. These electronic-based measures have been found to be effective and cost effective in reducing smoking prevalence among adults (see35,96,97). For example, computer-tailored programs that entail the adaption of the content of an intervention to participants’ individual characteristics using computer programs have been found to be both effective and economically efficient. 41 Most often, a questionnaire is used as a screening instrument, in which case answers provided by the smokers on the questions are accumulated into a large data file and are subsequently matched with relevant feedback messages that are ultimately combined into a tailored feedback letter. Tailored interventions are more effective in attracting and keeping a smoker's attention, resulting in better processing of information. Civljak et al 97 found that Internet programs that were interactive and tailored to individual responses led to higher quit rates than usual care or written self-help at 6 months or longer. There are two types of computer-tailored programs: single computer-tailored programs and multiple computer-tailored programs. A single-tailored feedback message is successful in increasing cessation rates, but dynamically tailored feedback provided on multiple occasions can even be more effective. Due to the automatic generation of the tailored feedback and the fact that computer-tailored interventions are increasingly delivered online, the integration of an internet-based computer-tailored program in the general practice setting might limit the burden on health professionals and patients, reduce facility and administrative costs, and could potentially be time and cost saving. 41 However, the Internet may offer additional benefits when combined with usual pharmacological interventions, such as NRT, varenicline, or other pharmacotherapy.
School-Based Interventions
Though the majority of smoking-related deaths occur in people aged 35 years or older, the onset of tobacco use occurs primarily in early adolescence, which makes adolescents a special target for smoking prevention projects. Schools have been identified as an ideal site to deliver tobacco prevention programs since they capture the majority of youth across a large age range, including the ages when most young people initiate smoking. The main perceived advantages of school-based intervention programs are that almost all children can be reached through schools, and a focus on education fits naturally with the daily activities of schools. 98 Researchers often employ five types of school-based intervention programs, each based on a different theoretical orientation: (1) information-only curricula, ie, interventions that provide information to oppose tobacco use (also called normative education). These educational programs provide content and activities that seek to correct inaccurate perceptions regarding high prevalence of tobacco use; (2) social competence curricula, a group of interventions that aim to help adolescents refuse offers to smoke by improving their general social competence–-including training on life skills such as self-control, self-esteem, decision making, and cognitive skills for resisting interpersonal and media influences; (3) social influence curricula, educational programs that seek to inform youths about the effects of outside influences such as advertising on their behavior, teach them that smoking is not the norm, and give them the skills to refuse cigarettes; (4) combined social competence and social influences curricula, methods that draw on both social competence and social influence approaches, and (5) multimodal programs, which combine curricular approaches with wider initiatives within and beyond the school, including programs for parents, schools, communities, and initiatives to change school policies about tobacco, or state policies about the taxation, sale, availability, and use of tobacco.
Although numerous school-based smoking prevention trials have found short-term decreases in smoking prevalence by up to 30%–70%, there is little or no evidence on the long-term effectiveness of school-based smoking prevention programs.98–100 Tengs et al 101 have reported that the effectiveness of anti-tobacco education programs using the “social influences” model tends to dissipate in 1–4 years, raising questions about the long-term economic efficiency of such initiatives. Using a system-dynamics computer simulation model based on secondary data, the authors evaluated the cost effectiveness of an enhanced nationwide school-based anti-tobacco education and found that over 50 years, cost effectiveness is estimated to lie between US$4,900 and US$340,000 per QALY, depending on the degree and longevity of program effectiveness. Assuming a 30% effectiveness that dissipates in 4 years, cost effectiveness is US$20,000/QALY. A similar study on the cost effectiveness of a school-based tobacco use prevention program in the US, known as Toward No Tobacco Use (TNT), showed that the program was highly effective as the government could expect to save US$13,316 per LY saved and a saving of US8,482 per QALY saved. However, a peer-led intervention, known as ASSIST, aimed at reduced smoking among adolescents in England and Wales, was only valued to yield a modest cost saving, with an incremental cost per student not smoking after 2 years of follow-up at £1,500 (CI = £669–£9,947). Other cost-effectiveness studies on school-based smoking cessation programs are summarized in Supplementary File 2. From all of these studies, an issue that remains unresolved is the extent to which reductions in adolescent smoking lead to lower smoking prevalence and/or earlier smoking cessation in adulthood.
Workplace Interventions
There has been growing interest within the business community regarding interventions against smoking in the workplace. Smoking interventions in the workplace particularly have numerous advantages. First, a large number of people can be contacted, canvassed, and enrolled in programs with relative ease, sometimes with the aid of extensive onsite occupational health facilities. 102 Second, worksites have the potential for higher participation rate than non-workplace environments. Third, worksites have the potential to provide sustained peer group support and positive peer pressure for quitting and staying tobacco-free. Fourth, it provides a particular opportunity to target young men, who traditionally have low general practitioner consultation rates and are thus less likely to benefit from opportunistic health promotion activity in primary care. Fifth, in some workplaces, occupational health staff may be on hand to give professional support. Finally, the employee need not travel to attend cessation programs; hence the workplace provides convenience benefits to the employee.103,104 It is worthy of note that many of these assumptions are based on a model of workplace that is rapidly changing. With many generation-Y employees who change jobs frequently or work from multiple locations, the net benefits from workplace cessations could be expected to become marginal in the long run.
Workplace smoking interventions can take numerous forms, including pharmacological interventions, behavioral interventions, or a combination of both. It could target individuals or specific employee groups. The main strategies include smoking prohibition, incentives, competitions, individual and group counseling, self-help materials, pharmacological therapy, and social and environmental support.
Many health economics researchers have found empirical evidence to support the general belief that smoking intervention programs help a firm's bottom line by reducing health care costs, absenteeism, and its attendant productivity losses and other employer-related costs. 105 However, there are serious challenges to the reliability and validity of their findings, as some critics of this literature have cited systematic biases affecting the credibility of some of these studies. These biases often manifest themselves in underestimation of costs and overestimation of benefits. Other researchers who have carried out behavioral workplace interventions have found a strong consistency in the correlation between smoking interventions and reduced cigarette consumption and decreased exposure to environmental tobacco smoke. 106 Smedslund et al 103 also compared the cost effectiveness of behavioral workplace interventions compared to pharmacological interventions and found that controlled smoking cessation trials at the worksite showed initial effectiveness, but the effect seemed to decrease over time and was not present beyond 12 months. Jackson et al, 107 however, showed that pharmacological interventions at the workplace seemed to generate 12-month employer cost savings per nonsmoking employee of between $150 and $540. The authors however found that varenicline was more cost beneficial than placebo because it had higher quit rates. Warner et al 105 also found that smoking cessation is a very sound economic investment for the firm, and is particularly profitable when long-term benefits are included, with an eventual benefit–cost ratio of 8.75. Other studies by Ong and Glantz 108 also showed that the first year effect of making all workplaces in the US smoke-free would produce about 1.3 million new quitters and prevent over 950 million cigarette packs from being smoked annually, worth about US$2.3 billion in pretax sales to the tobacco industry. In addition to preventing the risk of smoking-induced diseases such as myocardial infarctions and strokes, smoke-free work places could result in nearly US$49 million in savings in direct medical costs after 1 year. At steady state, more than US$224 million would be saved in direct medical costs annually (see Supplementary File 2 for summary of results).
Overall, this section has examined evidence across countries on the economic impact of smoking and the effectiveness and cost effectiveness of reducing smoking prevalence through intervention programs. It has examined the health and non-health-related costs and benefits of smoking as well as the effectiveness and cost effectiveness of pharmacological, policy-based, community-based, TMT-based, school-based and workplace- or employer-based smoking cessation interventions carried out through the years by different countries or state public health agencies. Key statistics and examples were drawn from United States, China, Australia, Canada, Hong Kong, Belgium, Taiwan, India, France, and Sweden. Next, this study narrows down by reviewing the economics of smoking in United Kingdom.
The Economic Impact of Smoking and Smoking Cessation Interventions in UK
The Costs and Benefits of Smoking in UK
Smoking has also been responsible for over 100,000 deaths per annum over the last decade in UK. The number of deaths attributable to smoking in 2005 was estimated at 109,164. 8 The financial and health burden of smoking in UK is enormous. Previous studies have estimated the direct costs of treating smoking-related diseases by the NHS to range somewhere between £1.4 and £1.7 billion every year.10,56,109,110 A more recent study conducted by Callum et al 12 showed that smoking-attributable costs to the NHS in 2006 was estimated at £2.7 billion. This includes smoking attributable hospital admissions (£1 billion), outpatient attendances (£190 million), general practitioner (GP) consultations (£530 million), practice nurse consultations (£50 million), and GP prescriptions (£900 million). Allender et al 8 estimates the costs of smoking-induced ill health to the NHS to be £5.2 billion in 2005–2006, representing about 5.5% of the total NHS budget that year e (see also 7 ). The cost of smoking in UK is thus increasing every year. The estimates provided by the above studies, however, are conservative cost estimates because they do not include the indirect costs of passive smoking and productivity losses due to smoking-related morbidity and premature mortality. The costs of informal care, smoking-related fires, cleaning costs, and sickness absence payments were also excluded from these estimates.
The cost of smoking to the NHS Wales has been estimated to be £386 million in 2007/2008, which is equivalent to £129 per head and 7% of total health care expenditure in Wales. 136
Cohen and Barton 56 show that approximately 50 million working days f are lost in UK annually due to smoking, valued at £1.71 billion. The British Medical Association 112 estimates that each year in UK, at least 1,000 deaths are attributable to passive smoking and more than 17,000 children under the age of five are admitted to hospital because of the ill effects of second-hand smoke. Parrott and Godfrey. 10 have estimated that each year in UK the cost of treating childhood illnesses related to smoking is about £410 million. The same study estimates the damage caused by smoking-related fires to be around £151 million each year in England and Wales. If all these indirect costs estimates are included to the NHS figures, the financial burden of smoking in UK will skyrocket. A more recent report by the Policy Exchange in 2010 attempts to sum up the total estimated costs to society of smoking in UK and puts the figure at £13.74 billion. This includes £2.7 billion cost to the NHS but also the loss in productivity from smoking breaks (£2.9 billion), and increased absenteeism (£2.5 billion). Other costs include cleaning up cigarette butts (£342 million), the cost of fires (£507 million), the loss of economic output from the death of smokers (£4.1 billion), and passive smokers (£713 million).
In England and Wales, more than 34 million days are lost through sickness absence resulting from smoking-related ill-health, while in Scotland the cost of productivity loss is ~£400–£450 million. In addition, smoking-induced fires cost about £4 million per annum in Scotland.10,137
The study by Allender et al 8 shows the percentage attributable to smoking of total NHS costs for smoking-related conditions in 2005–2006 by countries in UK (see Table 1). In England, the cost of smoking is £4.3 billion and this represents about 85% of the total smoking attributable costs in UK. For Wales, Scotland, and Northern Ireland, smoking-attributable cost was £234.2 million, £409.4 million and £127.9 million, respectively. Following the analysis made by this study, the smoking-attributable fraction (SAF) in UK was estimated at 23%. The SAF represents the costs attributable to smoking for smoking-related conditions, as a proportion of total NHS expenditure for those conditions. The smoking-related conditions considered included cardiovascular diseases, COPD, other respiratory conditions, lung/bronchus/trachea cancer, mouth and oral cancer and peptic ulcer disease.
Percentage of NHS costs attributable to smoking in 2005–2006 by countries in UK. 8

The smoking-related conditions considered included cardiovascular diseases, COPD, other respiratory conditions, lung/bronchus/trachea cancer, mouth and oral cancer and peptic ulcer disease.
In spite of the costs of smoking in UK, there are potential economic benefits that smoking brings to the economy. Just like in other countries, tobacco is a major revenue earner for the government. Thus, a reduction in the prevalence of smoking will bring about significant loss to the Exchequer. According to the HM Revenue and Customs 112 Tobacco Bulletin and Factsheets, the treasury earned £9.5 billion in revenue from tobacco duties in the financial year 2011–2012 (excluding VAT). This amounts to 2% of the total government revenue. Including VAT at an estimated £2.6 billion, total tobacco revenue was £12.1 billion. 113 The price of a pack of 20 premium brand cigarettes currently costs around £7.98, of which £6.17 (or 77%) is tax. 114 The economic benefits of smoking from taxation alone thus appear to be noticeably higher than the direct costs of smoking in UK. A CBA of the effects of increasing tobacco taxation commissioned by ASH (in 115 ) found that a tobacco price increase of 5% would result in net benefits to the economy as a whole of around £10.2 billion over 50 years. The economic benefits in the first 5 years would be around £270 million per year on average.
Apart from government taxation, tobacco companies make huge profits from sale of tobacco products. In 2012, British American Tobacco, which is the world's second largest tobacco company, produced 694 billion cigarettes worldwide (down from 705 billion in 2011) and reported an operating profit of £5.14 billion, an increase of 15% on 2011. 116 The two major UK tobacco companies–-Imperial Tobacco and Gallaher (the latter now owned by JTI)–-control around 85% of the UK market.
The economic benefits of smoking in UK could also be seen in terms of employment in the tobacco and dependent industries. According to the National Statistics from Tobacco Manufacturers Association, 117 approximately 5,700 people are employed in tobacco manufacturing in UK. It has been argued that a reduction of smoking might not necessarily imply an overall increase in unemployment. It may well boost employment and output.56,118,119 The argument is that, though there will be loss of job in the tobacco industry following smoking cessation, money not expended on tobacco will then be spent elsewhere, thereby increasing the demand for other goods and services, and hence generating employment for some other sectors. The extent, to which this happens, however, depends on the spending patterns of the former smokers. McNicoll and Boyle 118 estimated that a total cessation of cigarette purchases in Glasgow will bring about net benefits to the Scottish economy. They estimated that for every £1 million reduction in cigarette expenditure, there would be a net increase in Scottish output of £1.1 million and a net increase of Scottish employment of 64 jobs. In a similar study by Buck et al, 119 a 40% reduction in smoking–-a target set by the 1992 UK Policy document–-will have estimated effects of increasing jobs in the UK by 150,000. As noted earlier, a smoking population also has the benefit of achieving savings in pension payments from the premature death of smokers. Manning et al. 120 have estimated that every pack of cigarettes smoked reduces the life expectancy by 137 minutes and pension costs by $1.82.
The Effectiveness and Cost Effectiveness of UK-Specific Smoking Cessation Programs
This section takes a look at the effectiveness and cost effectiveness of smoking cessation interventions that are specific to the UK and identifies where there are any cost savings or net benefits to the health care system arising from a reduction in smoking prevalence. It reviews high-quality evidence on the economics of smoking cessation programs implemented in the different parts of UK. In 1998, the UK government for the first time took a comprehensive approach to the reduction of smoking prevalence in England when it published a policy paper (called a White Paper), Smoking Kills. This program was aimed at reducing smoking among children and adolescents, and help adult smokers, particularly the disadvantaged ones (including pregnant women) to quit smoking. The strategy involved ban on tobacco advertising, further increases in tobacco prices g , measures to reduce smoking in workplaces and in public places, measures to restrict the sale of tobacco to minors h , and also, for the first time in the history of NHS, the commitment of huge resources to smoking cessation treatment services. Smoking Kills has been able to reduce the average prevalence of smoking in adults (16 years+) in England from 27% before the implementation period to 21% in 2008. 121
One major issue associated with tax increases is that of smuggling and tax evasion. In the UK, it is estimated that approximately 40% of cigarettes do not have UK duty paid on them. The average cost of such cigarettes is almost half the price of legitimate ones. Taxation policies therefore need to be accompanied by a radical law enforcement mechanism in order to reduce this problem. 122
NHS Smoking Cessation Treatment Services
The White Paper, Smoking kills, sets out guidelines for the provision of specialist smoking cessation services. The United Kingdom was the first country to introduce a national smoking cessation treatment program funded through public taxes. 122 Since then, other countries have implemented similar treatment services, eg, Japan and Taiwan. Since 2000, many smokers have received behavioral support through counseling or special training sessions to aid smoking cessation. In England and other parts of UK, smokers can purchase NRT products from local pharmacies and shops. A report from the National Institute for Clinical Excellence (NICE) 123 in March 2002 showed that NRT and bupropion are some of the most cost-effective treatments of all pharmacological interventions. Their cost effectiveness has been estimated by NICE in terms of cost per life year gained (LYG); NHS treatment services produce a cost of about £3000 per LYG and about £2000 when adjusted using UK discount rates (estimates cited in Ref. 124, pp. 5). Stapleton. 125 reveals that calculations based on the reported performance of the NHS specialist smoking cessation services suggest they are highly cost effective, generating a cost of less than £800 per life-year saved. The same study reveals that during April 2000 and March 2001, about 126,800 smokers made an attempt to quit smoking while attending cessation services. Of these, 48% were abstinent at the end of 4 weeks. The total costs (including treatment and administrative costs) were £21.4 million or £209 when expressed per patient treated.
Like in many countries, the UK government forbid children under the age of 16 from purchasing tobacco products. However, the effectiveness of this restriction has been called to question as children are able to obtain cigarettes from their older friends, siblings, or vending machines.
According to a more recent report for 2005, an estimated 2 million smokers in UK used NRT products (and to a much lesser extent bupropion) to aid in stopping smoking. 122 The effectiveness of these treatment services has also been estimated at ~2%–3% abstinence rates. In all, about 90,000 smokers (out of an estimated 12 million smokers in UK) stopped smoking permanently in 2005, implying that about 0.75% of smokers became ex-smokers due to smoking cessation treatments.
Two very recent studies have also examined the cost effectiveness of NRT, bupropion, and varenicle for preventing or reducing relapse to smoking by abstinent smokers following smoking cessation.27,126 Their findings revealed that, like other interventions, relapse prevention interventions (RPIs) are also likely to be highly cost and clinically effective. When compared to no intervention, using bupropion for relapse prevention resulted in an incremental QALY increase of 0.07 with a concurrent NHS cost saving of £68; NRT and varenicline both caused incremental QALY increases of 0.04 at costs of £12 and £90, respectively. Extensive sensitivity analyses from both studies demonstrated that cost-effectiveness ratios were more sensitive to variations in RPI effectiveness than cost. In addition, even after varying key model parameters, the cost effectiveness of NRT and bupropion generally remained. Cost effectiveness ratios only exceeded the UK NICE benchmark of £20,000 per QALY when drug treatment effects were projected to last for only 1 year.
In summary, NHS treatment services and relapse prevention intervention services have been both clinically and cost effective, generating substantial health and cost savings that are acceptable to health care providers.
Community Pharmacy-Based Smoking Cessation
Crealey et al 127 have looked at the cost effectiveness of a community pharmacy-based smoking cessation program in Northern Ireland. Data from a pilot study conducted in two community pharmacies in Belfast were used as the basis of the current study, which examined the costs and effects associated with a formal counseling program for smoking cessation by community pharmacists across Northern Ireland. The Pharmacists Action on Smoking (PAS) model was the only active intervention used in the study. Findings indicate that the cost per life year saved when using the PAS program ranges from £196.76 to £351.45 in men and from £181.35 to £772.12 for women (1997 values), depending on age. This compares favorably with other disease prevention medical interventions such as screening for hypertension or hypercholesterolemia. More recently, Boyd and Briggs 128 examined the cost effectiveness of pharmacy-based versus group behavioral support in smoking cessation services in Glasgow. This study was based on the premise that smokers attending group-based support for smoking cessation are significantly more likely to be successful than those attending pharmacy-based support. The study was conducted using a combination of observational study data and information from the NHS Greater Glasgow and Clyde smoking cessation services. Findings revealed that incremental cost per 4-week quitter for pharmacy-based support was found to be approximately £772 and £1612 for group support, dismissing the earlier hypothesis. Furthermore, estimated incremental cost per QALY for pharmacy-based service is £4400 and £5400 for group support service. The study, however, concludes that both group support and pharmacy-based support for smoking cessation are highly cost effective.
Action Heart Promotion Program
Action Heart is a cost-effective, community-based heart promotion project, which was implemented between 1991 and 1995 in Wath and Swinton, England. Baxter et al 129 carried out a prospective comparative study to establish whether this community-based coronary heart disease health promotion intervention, undertaken over 4 years, was associated with a reduction in the prevalence in adults of risk factors associated with heart disease, including smoking, as well as to estimate the cost effectiveness of this intervention. Smoking prevalence before and after the intervention was assessed using a questionnaire mailed to residents in both the intervention and control areas. Smoking decreased in the intervention area and increased in the control area between 1991 and 1995. Results showed that the intervention achieved a smoking abstinence rate of 6.9%, while 8.7% more of the sample population consumed low-fat milk between the intervention and control area in the 4-year period. The differences between the areas rose from 4.2% to 9.2%. Total project cost (including allowances for community project officer and worker, consumables and other overheads, other NHS staff, school expenditure, etc) was £110,000. The estimated cost per life year gained was £31.
Heart Beat Wales (HBW)
Phillips and Prowle 22 also appraised the economics of a no-smoking intervention program named Heart Beat Wales (HBW) carried out between 1985 and 1988. Health benefits were estimated as intermediate and final outcomes. Intermediate outcomes were the reduction in the number of smokers and the amount of tobacco consumed. The final outcomes were presented in the terms of reduced morbidity and mortality in three disease groups–-coronary heart disease (CHD), lung cancer, and chronic bronchitis. The program costs included direct cash costs and staff costs. Total cost in year 1 was £72,000, in year 2 £82,000, in year 3 £150,000, and in year 4 £205,000. Results show a net present value of benefits to NHS of £4,134,000. The “economic” appraisal has a present value of benefits of £43,503,000. The estimated cost of a working life year saved is £5.78. The net present value of benefits from reductions in smoking is significantly greater than costs in terms of both the NHS and the economy as a whole in Wales. In addition, the net costs per life year saved reveals that the program generates additional working life years at relatively low cost.
No Smoking Day
More than two decades after the launch of the “No Smoking Day” (NSD) in UK, Owen and Youdan 130 and Kotz et al 131 evaluated the impact and relevance of this national awareness day. Launched in 1984, the campaign seeks to create an enabling environment for smokers to quit smoking. When the campaign began, smoking prevalence in the UK was more than 33% of adults; in 2003 it dropped to 25%. The campaign expenditure ranges somewhere between £470,000 and £550,000 annually. Results show that follow-up after 1 week indicates awareness of NSD is lower in 2004 than in 1986, 2 years after it was launched. However, awareness is still high at 70% for all smokers. Interestingly, the decline in participation from 18% of aware smokers in 1994 to 7% in 2001 was reversed in 2005 when about 19% either gave up or reduced their smoking on NSD. In 2004, NSD awareness had reached 78% of the smoking population. When compared to the 8.5 million smokers in England, the campaign can be deemed to be effective in reaching its target audience. In addition, media coverage has increased regardless of the fact that the campaign expenditure has remained relatively constant and calls to national smokers’ helpline on NSD are typically four times those received on a normal day. The cost of NSD per smoker was £0.088. The discounted life years gained per smoker in the modal age group 35–44 years was 0.00107, resulting in an incremental cost–effectiveness ratio (ICER) of £82.24 (95% CI 49.7–231.6). Thus, the campaign emerges as an extremely effective and cost-effective public health intervention in aiding smoking cessation.
HEBS's Mass Media-Led Intervention
Ratcliffe et al 132 evaluated the costs and outcomes of a mass media-led antismoking campaign in Scotland, which was conducted by the Health Education Board for Scotland (HEBS). The campaign had three elements or features, namely 1) mass media advertising, including television, outdoor posters, and press; 2) Smokeline, a free telephone quitline to aid smoking cessation; and 3) You can stop smoking, a practical handbook aimed at guiding smokers to renounce smoking. At the end of a 12-month period, about 9.88% of individuals in the follow-up sample reported they have renounced smoking since 6 months after the campaign. The costs of the campaign (including the youth campaign costs) ranged from £1,486,101 to £1,546,420. In terms of costs per quitter, estimates ranged from £189 to £369. The costs per life year saved attributable to the campaign ranged from £304 to £656. Another mass media campaign based on behavior change theory and operating through both traditional and new media, known as Stoptober, was launched in England during late 2012. Brown et al 133 found that Stoptober was both effective and cost effective, as it generated up to 350,000 quit attempts and saved 10,400 discounted life years (DLY) at less than £415 per DLY in the modal age group.
This section has reviewed the economic impact of smoking and reducing its prevalence in UK. Though smoking is beneficial to the UK both in terms of tax revenue and employment, the health- and non-health-related costs of smoking to the NHS and the society far outweigh any benefits that might be accruable at least from a socially desirable perspective. Most smoking cessation interventions implemented in the UK have also been highly effective, reducing the number of smokers and any health risks associated with smoking.
Discussion
This study reviews major studies on the economics of tobacco smoking and the economic impact of reducing its prevalence both globally and in UK. The findings from the review reveal that tobacco smoking is the cause of many preventable diseases and premature deaths in UK and around the world. It poses enormous health- and non-health-related costs to the affected individuals, employers, and the society at large. The WHO estimates that, globally, smoking causes over US$500 billion in economic damage each year. In the UK, the total estimated costs of smoking to society could be put at £13.74 billion. In the US, a much larger economy by population and GDP, the social cost of smoking is more than 8 times that of UK–-US$193 billion (or ~£114 billion) according to estimates from Kahende et al, 5 though this figure is even larger when we consider latest estimates from the Campaign for Tobacco-Free Kids, which puts the social cost of smoking at US$321 billion. 59 About 15% of the aggregate health care expenditure in high-income countries can be attributed to smoking. In the US, the proportion of health care expenditure attributable to smoking ranges between 6% and 18% across different states. In the UK, the direct costs of smoking to the NHS have been estimated at between £2.7 billion and £5.2 billion, which is equivalent to around 5% of the total NHS budget each year. The economic burden of smoking estimated in terms of GDP reveals that smoking accounts for approximately 0.7% of China's GDP and approximately 1% of US GDP. As part of the indirect (non-health-related) costs of smoking, the total productivity losses caused by smoking each year in the US have been estimated at US$151 billion. Smoking is therefore considerably expensive to countries where its prevalence is high, particularly high-income countries. The costs notwithstanding, smoking has some potential economic benefits to most economies. The economic activities generated from the production and consumption of tobacco provides economic stimulus. It also produces huge tax revenues for most governments, especially in high-income countries, as well as employment in the tobacco industry. Income from the tobacco industry accounts for up to 7.4% of centrally collected government revenue in China. Smoking also yields cost savings in pension payments from the premature death of smokers.
Several measures have been undertaken by most countries (including UK) over the years in order to reduce the prevalence of smoking in adults, children, and pregnant women. These measures range from pharmacological treatment interventions (such as the use of NRT, bupropion, and varenicle) to policy-based measures (tax increases, smoking restrictions, bans on tobacco advertising, etc), community-based interventions (such as smoking cessation contests, classroom education, self-help quit kit, etc), TMT-based measures (such as quitlines, mass media led interventions, internet- and computer-based measures), school-based measures, and workplace interventions. We now discuss some of the findings from the review by comparing results across types of intervention, implementation countries, and measurement outcomes, where possible.
Comparing the Effectiveness and Cost Effectiveness of Various Interventions
From the review of pharmacological and medical treatment interventions for smoking cessation across countries, it was found that cost per life year saved ranged between US$128 and US$1,450 and up to US$4,400 per QALY saved. Comparing various types of pharmacological interventions, existing studies showed that varenicline (with or without behavioral interventions) seemed to be the most cost-effective therapy, followed by bupropion and NRT. However, the results have a high risk of bias because the manufacturer of varenicline funded most of the studies comparing varenicline with bupropion or NRT. In the UK, it was found that the use of NRT and/or bupropion combined with GP counseling was both clinically effective and cost effective to primary health care providers.
Some studies reveal that pharmacological treatments tend to yield more positive results in terms of number of quitters than other cessation interventions (eg, NRT programs could yield as much as 18,500 quitters at a cost of US$4,440 per QALY compared to implementing a smoke-free workplace policy, which would generate 10,400 quitters at US$506 per QALY). The use of pharmacotherapies such as varenicline when combined with other behavioral treatment interventions (such as proactive telephone counseling and Web-based delivery, or both) is cost effective when measured from both cost per LY and cost per QALY, with costs per additional 6-month nonsmoker and per additional life time quitter ranging from US$1,278 to US$1,617 and from US$2,601 to US$3,291, respectively.
With respect to policy-based measures, increase in tobacco taxes is unarguably the most effective means of reducing the consumption of tobacco and hence the health care costs associated with treating smoking-caused diseases. Findings show that a 10% tax-induced cigarette price increase anywhere in the world reduces smoking prevalence by between 4% and 8%. Apart from reducing the number of smokers and saving lives, increasing tobacco taxes also raise government revenue accruable from tobacco manufacturers and retailers. Thus, as cigarette taxes increase, government tax revenues continue to rise even as smoking prevalence falls. In fact, net public benefits from tobacco tax remain positive only when tax rates are between 42.9% and 91.1%. However, increase in tobacco taxes increases the risk of reduction in employment in tobacco companies and the incidence of cigarette smuggling and tax evasion, further dwindling the net benefits from tax increases. Non-price-based measures (such as smoking restrictions in work places, public places, bans on tobacco advertisement, and raising the legal age of smokers) have also proven to be both effective and cost saving. The health and economic benefits of such measures include reduction in smoking prevalence, reduction in second hand smoke, savings from smoking-related medical expenditures, heart diseases averted, costs averted by a reduction in smoking-induced fires, and gains in productivity. Findings show that the cost–effectiveness ratio of implementing non-price-based smoking cessation legislations range from US$2 to US$112 per LYG, while reducing smoking prevalence by up to 30%–82% in the long term (over 50-year period).
From the perspective of the public health system, community-based intervention programs yield cost savings and life year gains. There are, however, differences in the effectiveness and cost effectiveness of different types of community-based interventions. Smoking cessation classes are known to be most effective among community-based measures since they require more time commitment from participants. They could lead to a quit rate of up to 35%, but they usually incur higher costs. On the other hand, self-help quit smoking kits usually require the lowest time commitment from participants and are usually the most cost effective. Community pharmacies also provide opportunities for regular contact with residents of a local community. On average, community pharmacist-based smoking cessation programs yield cost savings to the health system of between US$500 and US$614 per LYG. Knowledge of the health and economic gains of different community-based measures is highly desirable when health policy decision makers plan the allocation of resources for smoking cessation at the community level. One classic example of an effective community-based campaign is the UK's “No Smoking Day”. After almost three decades of its launch, the campaign has achieved a 78% awareness rate. It has also reduced smoking prevalence by 14%. With the cost of NSD per smoker at £0.088 and ICER of £82.24, NSD emerges as an extremely cost-effective public health intervention.
Since many people are ambivalent about smoking, it has been widely held that advertising media, telecommunications, and other technology-based interventions usually have positive synergistic effects. In fact, as many studies show, an integrated approach involving a combination of multiple media to deliver a message produces greater effects than relying on one medium alone. However, the outcomes on the effectiveness and cost effectiveness of TMT-based measures have been inconsistent. For example, Farrelly et al 92 examined the effects of expenditure on TV, radio, and print advertising and concluded that, while TV advertising produced the greatest overall increase in calls to a Quitline, incremental increases in expenditure on radio advertising yielded proportionally higher increases in the call rate. Clayforth et al 42 found that online-only advertising campaigns can be substantially more cost effective than other non-television advertising media such as radio, and print media, including when an integrated approach is used. Chen et al34,35 also found that making some form of electronic support available to smokers actively seeking to quit (eg, PC, internet, and other electronic aids) is highly likely to be cost effective. This is true whether the electronic intervention is delivered alongside brief advice or more intensive counseling.
The differences in reported cost effectiveness may be partly attributed to varying methodological approaches, including different inputs used to determine model parameters, especially the different dependent variables tested (eg, calls to a quitline versus intention to quit; visits to a quit website versus online registration to smoking cessation services), disparate levels of resourcing between campaigns, differences in national contexts, and differences in advertising campaigns tested on different media. For example, radio is limited to sound, while traditional print media is confined to static pictures. Further, it is difficult to isolate the effects of individual media due to the tendency for campaigns to typically involve the simultaneous use of different media to optimize results. In such circumstances, it is difficult to attribute results to specific media. Some studies have, however, shown that under a wide variety of conditions, the use of personalized smoking cessation service advice, when combined with telephone counseling, mobile phone messages, or other personalized computer-based intervention measures, is both beneficial for health and cost saving to a health system.
In evaluating the effectiveness of school-based intervention programs aimed at preventing smoking in children and adolescents, many studies have conducted analysis of peer-led programs, analysis of social influences, social competences, gender effects, class competitions, and booster sessions, among other measures. Thomas et al 98 found that all these theoretical approaches were very effective in aiding smoking cessation particularly in the number of youths that were prevented from starting smoking. Numerous smoking prevalence trials have found short-term decreases in smoking prevalence of between 30% and 70%. As with other intervention programs, determining that a program is effective may not be sufficient to justify its implementation since the resources to fund school-based smoking prevention programs are limited. Because of limited financial resources, most school-based smoking cessation programs are usually carried out in multiple schools, most times covering thousands of students across communities or regions within the countries of implementation (eg, TNT in USA; ASSIST in England and Wales; MYTRI in India; SFC in Germany). Total intervention costs could range from US$16,400 to US$580,000 depending on the scale and scope of intervention, and these costs usually cover personnel expenses, costs of materials, travel expenses, and program administration costs. Most studies evaluating the cost effectiveness of school-based programs show that one could expect a saving of approximately between US$2,000 and US$20,000 per QALY saved due to averted smoking after 2–4 years of follow-up.
Finally, from the economic evaluation of smoking cessation activities at the workplace, it is evident that employer-based interventions could be beneficial to both employers and the society at large. For example, Warner et al 105 found that smoking cessation is a very sound economic investment for the firm, and is particularly profitable when long-term benefits are included, with an eventual benefit–cost ratio of 8.75. Jackson et al 107 also showed that pharmacological interventions at the workplace seemed to generate 12-month employer cost savings per nonsmoking employee of between $150 and $540. Other studies by Ong and Glantz 108 also showed that the first-year effect of making all workplaces in the US smoke-free would produce about 1.3 million new quitters and prevent over 950 million cigarette packs from being smoked annually, worth about US$2.3 billion in pretax sales to the tobacco industry. In addition to preventing the risk of smoking-induced diseases such as myocardial infarctions and strokes, smoke-free work places could result in nearly US$49 million in savings in direct medical costs after 1 year. At steady state, more than US$224 million would be saved in direct medical costs annually.
From a review of these and other economic studies, it can be safely deduced that the economic benefits of employer-based smoking cessation measures are likely to be far more greater than the costs involved, particularly on a long-range basis, since reduced worksite smoking prevalence translates into reduced absenteeism, increased productivity, lower health insurance costs, higher cost savings, and higher overall benefit–cost ratio in the long run. Moreover, the economic advantages of workplace anti-tobacco policies seem to be more visible when smoking at the workplace is completely prohibited and no smoking areas are set.
Limitations of the Study
Only a few studies examining the long-term effect of smoking cessation interventions were found. Evidence of long-term health and economic benefits of many cessation interventions such as clinical and workplace interventions remains uncertain. A series of sensitivity analyses from many of the studies also show that both cost savings and life year gains are sensitive to variations in the discount rates and the long-term smoking quit rate associated with the intervention. Thus, there is a high risk of uncertainty in some of the cost estimates provided in this study. Another source of error in comparative analysis is the differences in basis for cost comparisons across countries and the impact of inflation on cost estimates. For example, there are significant differences across countries in terms of basic demographic and socioeconomic characteristics, life expectancy of population, and advancements in health care systems. Thus, calculation of life years saved and medical costs of smoking-related diseases are likely to differ significantly across countries. Also, the inflation rates in developing/emerging countries like India, Thailand, Taiwan, and China are likely to be higher than those in developed countries such as USA, UK, Canada, and Australia where inflation rates are known to be somewhat lower. Hence, some studies may overstate the real cost estimates if not properly discounted (ie, adjusted) for inflation, thus making comparisons across time and countries difficult. Finally, it is worth noting that the results of many studies reviewed may not have been well established quantitatively in the sense that most of these studies reflect potential uncertainty in the estimates and data used and, in some cases, data sufficient to establish definite causality are lacking.
Conclusions
Though tobacco smoking may be economically beneficial, its direct costs and externalities to society far outweigh any benefits that might be accruable at least when considered from the perspective of socially desirable outcomes (eg, a healthy population and a vibrant workforce). There are enormous differences in the application and economic measurement of smoking cessation measures across various types of interventions, methodologies, countries, economic settings, and health care systems, and these may have affected the comparability of the results of the studies reviewed. However, on the balance of probabilities, most of the cessation measures reviewed have not only proved effective but also cost effective in delivering the much-desired cost savings and net gains to individuals and primary health care providers.
Author Contributions
Conceived and designed the experiments: VE and AB. Analyzed the data: VE. Wrote the first draft of the manuscript: VE. Contributed to the writing of the manuscript: AB. Agree with manuscript results and conclusions: VE and AB. Jointly developed the structure and arguments for the paper: VE and AB. Made critical revisions and approved final version: VE and AB. All authors reviewed and approved of the final manuscript.
Footnotes
Supplementary Data
Summary of results from selected economic studies by types of intervention.
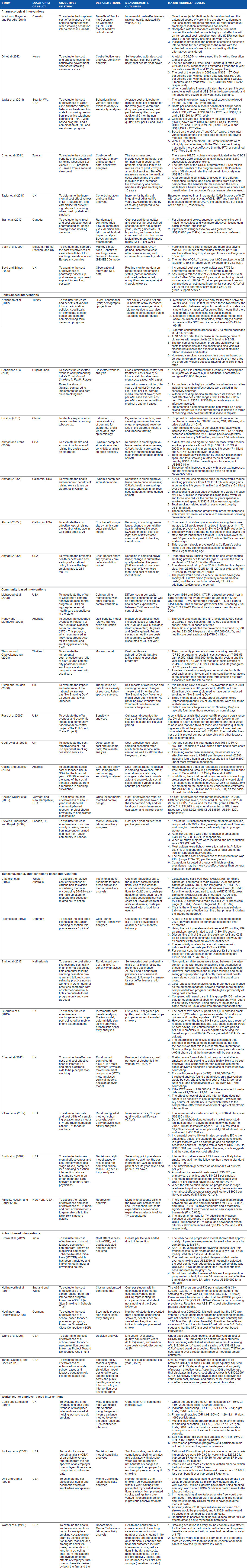
| STUDY | LOCATION(S) OF STUDY | OBJECTIVES OF STUDY | DESIGN/METHODS | MEASUREMENTS/OUTCOMES | MAJOR FINDINGS/RESULTS |
|---|---|---|---|---|---|
|
|
|||||
| Wartburg, Raymond, and Paradis (2014) | Canada | To evaluate the long-term cost effectiveness of varenicline compared with other smoking cessation interventions in Canada | Benefits of Smoking Cessation on Outcomes (BENESCO) model; Markov cohort model | Incremental cost–effectiveness ratio per quality-adjusted life year (QALY) |
Over the subjects’ life time, both the standard and the extended course of varenicline are shown to dominate (eg, less costly and more effective) all other alternative smoking cessation interventions considered. Compared with the standard varenicline treatment course, the extended course is highly cost effective with an incremental cost–effectiveness ratio (ICER) less than US$4,000 per quality-adjusted life year (QALY). Including indirect cost and benefits of smoking cessation interventions further strengthens the result with the extended course of varenicline dominating all other alternatives considered. |
| Oh et al (2012) | Korea | To evaluate the cost and effectiveness of the nationwide government-sponsored smoking cessation clinics | Cost-effectiveness analysis; sensitivity analysis | Self-reported quit rates; cost per quitter; cost per service user; cost per life-year saved |
A total of 354,554 smokers used the Smoking Cessation Clinics in 2009. The self-reported 4-week and 6-month quit rates were 78% and 40%, respectively. Estimated 1-year and 8-year quit rates were 28.1% and 12.9%, respectively. The cost of the service in 2009 was US$21,127. Cost per service user who set a quit date was US$60. Cost per service user who maintained cessation at 4 weeks, 6 months, and 1 year was US$76, US$149 and US$212, respectively. When considering 8-year quit rates, the cost per life year saved was estimated at US$128 in the base scenario and increased to US$230 in the worst case scenario. |
| Javitz et al (2011) | Seattle, WA, USA | To evaluate the cost effectiveness of varencline and three different behavioral treatment formats for smoking cessation: proactive telephone counseling (PTC), Web-based program, and a combination of PTC and web-based program | Behavioral intervention; cost effectiveness analysis; sensitivity analyses | Average cost of telephone minute; costs per enrollee for the Web group; varenicline drug cost per enrollee; cost per lifetime quitter; cost per additional 6 months non-smoker and additional lifetime quitter; cost per LY and QALY |
The Web intervention was the least expensive followed by the PTC and PTC–Web groups. Costs per additional 6-month nonsmoker and per additional lifetime quitter were US$1,278 and US$2,601 for Web, US$1,472 and US$2,995 for PTC, and US$1,617 and US$3,291 for PTC–Web. Cost per life-year (LY) and quality-adjusted life-year (QALY) saved were US$1,148 and US$1,136 for Web, US$1,320 and US$1,308 for PTC, and US$1,450 and US$1,437 for PTC–Web. Based on the cost per LY and QALY saved, these interventions are among the most cost-effective life-saving medical treatments. Web, PTC, and combined PTC–Web treatments were all highly cost effective, with the Web treatment being marginally more cost effective than the PTC or combined PTC–Web treatments. |
| Chen et al (2011) | Taiwan | To evaluate the costs and benefits of the Outpatient Smoking Cessation Services (OSCS) program in Taiwan from a societal view point | Cost–benefit analysis; primary and secondary data; sensitivity analyses | The costs measured include cost to the health sector, non-health sectors, the patients, and their family, as well as loss of productivity as a result of smoking; Benefits measures include the medical costs savings and the earnings due to the increased life expectancy of a person who has stopped smoking for 15 years |
There were 169,761 subjects who participated in the OSCS in the years 2007 and 2008, and, of those cases, 8282 successfully stopped smoking. The total cost of the OSCS program was US$18 million. The total benefits of the program were US$215 million with a 3% discount rate; the net benefit to society was US$196 million. After conducting sensitivity analyses on the different abstinence, relapse, and discount rates, from a societal perspective, the benefits still far exceeded the costs, while from a health care perspective, there was only a net benefit when the respondent's abstinence rate was used. |
| Taylor et al (2011) | UK | To determine the incremental cost effectiveness of NRT, bupropion, and varenicline for preventing relapse to smoking when used by abstinent smokers | Cohort simulation and sensitivity analyses | Incremental health gain in quality of adjusted life years (QALYs) generated by each drug compared to no intervention | Bupropion resulted in an incremental QALY increase of 0.07 with a concurrent cost saving of £68; NRT and varenicline both caused incremental QALYs increases of 0.04 at costs of £12 and £90, respectively. |
| Tran et al (2010) | Canada | To evaluate the clinical and cost effectiveness of pharmacological-based strategies for smoking cessation | Randomized controlled trials (RCTs); meta analyses; decision analytic model; budget impact analysis; Bayesian random effects model | Cost per additional quitter and cost per life-year gained; cost per quality-adjusted life year (QALY) gained of NRT, bupropion, and varenicline compared with no pharmacological treatment; willingness to pay (WTP) per QALY |
For all ages and sexes, bupropion and varenicline dominated (ie, cost less and was more effective) nicotine gum, patch, lozenge, and inhaler. If providers’ willingness to pay was greater than US$10,000 per QALY, then varenicline was preferred. |
| Bolin et al (2009) | Belgium, France, Sweden, and UK | To evaluate and compare the cost effectiveness of varenicle with NRT for smoking cessation in four European countries | Markov simulations, Benefits of smoking cessation on Outcomes (BENESCO) model | Abstinence rates, QALY gained, incremental cost–effectiveness ratios, and incremental cost–utility ratios |
Varenicle is more cost effective and more cost saving than NRT: Number of morbidities avoided, per 1,000 smokers attempting to quit, ranged from 9.7 in Belgium to 6.5 in UK. The number of QALY gained, per 1,000 smokers, was 23 (Belgium), 19.5 (France), 29.9 (Sweden), and 23.7 (UK). |
| Boyd and Briggs (2009) | UK | To examine the cost effectiveness of pharmacy-based support versus group-based support for smoking cessation | Observational study and NHS data | Routine monitoring data on resource use and smoking status (carbon monoxide-validated, self-reported, nonquitters and relapsers) at 4-week follow-up |
Incremental cost per 4-week quitter was £772 for pharmacy support and £1612 for group support. Assuming a relapse rate of 75% from 4 weeks to 1 year and a further 35% beyond 1 year, and combining this with an average of 1.98 QALY gained per permanent cessation provides an estimated incremental cost per QALY of £4400 for the pharmacy service and £5400 for group-support service. |
|
|
|||||
| Arslanhan et al (2012) | Turkey | To evaluate the costs and benefits of various tobacco elimination policies, specifically, an immediate taxation option and eight tax-combined long-term cessation programs | Cost–benefit analysis; demographic projections | Net social cost and net public benefits of tax increases; increase in average price of cigarettes due to tax raise; cigarette consumption due to tax raise; cost per quitter |
Net public benefit is positive only for tax rates between 42.9% and 91.1%. In fact, between these two values, the relationship between net public benefit and tax rates is a single-hump-shaped Laffer curve. This means that there is a tax rate that maximizes net public benefit. Net public benefit reaches its maximum at the tax rate of 84.6%, which, if implemented, would imply a drastic increase of the SCT from its current level of 63.4% to 69.3%. Cigarette consumption drops to 165,763 million packages at 84.6% tax rate. At 91.5% tax rate, the increase in the average price of cigarettes with respect to its 2011 level is 149.3%. The tax-combined cessation programs yield lower net costs to households and the society and also yield significant reductions in the expected number of smoking-related diseases and deaths. However, a smoking cessation class program based on 20-year intervention period is found to be the most effective program, yielding success rates of up to 35% in quit rates. |
| Donaldson et al (2011) | Gujarat, India | To assess the cost effectiveness of implementing India's Prohibition of Smoking in Public Places | Cost effectiveness analysis | Gross intervention costs; AMI treatment costs saved; All tobacco-attributable treatment costs saved; AMI cases |
After 1 year, it is estimated that a complete smoking ban in Gujarat would avert 17,000 additional heart attacks and gain 438,000 life years. |
| Rules the state of Gujarat, compared to implementation of a complete smoking ban | averted; smokers quitting; life years gained (LYG); cost per LYG; cost per LYG without media treatment saved; cost per AMI case averted; cost per AMI case averted without medical treatment saved |
A complete ban is highly cost effective when key variables including legislation effectiveness were varied in the sensitivity analyses. Without including medical treatment costs averted, the cost effectiveness ratio ranges from US$2 to US$112 per LYG and US$37 to US$386 per acute myocardial infarction averted. Implementing a complete smoking ban would be a cost-saving alternative to the current partial legislation in terms of reducing tobacco-attributable disease in Gujarat. |
|||
| Hu et al (2010) | China | To identify key economic issues involved in raising tobacco tax | Estimated price elasticity of demand for cigarettes, prevalence data, and epidemiology | Cigarette consumption, lives saved, government tax revenue, employment, revenue loss in the cigarette industry and tobacco farming |
Proposed tax adjustment in China would reduce the number of smokers by 630,000 saving 210,000 lives, at a price elasticity of -0.15. A tax increase of US$0.13 per pack of cigarettes would increase the government's tax revenue by US$17.2 billion, decrease consumption by 3.0 billion packs of cigarettes, reduce smokers by 3.42 million, and save 1.14 million lives. |
| Ahmad and Franz (2008) | USA | To estimate health and economic outcomes of raising the excise taxes on cigarettes | Dynamic computer simulation model; sensitivity analysis on price elasticity | Reduction in smoking prevalence due to price increases; QALYs; health care savings realized; changes in tax revenues (amount of taxes gained or lost) |
A 40% tax-induced cigarette price increase would reduce smoking prevalence from 21% (in 2004) to 15.2% (in 2025) with large gains in cumulative life years (7 million) and QALYs (13 million) over 20 years. Total tax revenue will increase by US$365 billion in that span, and total smoking-related medical costs would drop by US$317 billion, resulting in total savings of US$682 billion. These benefits increase greatly with larger tax increases, and tax revenues continue to rise even as smoking prevalence falls. |
| Ahmad (2005a) | California, USA | To evaluate the health and economic benefits of raising excise taxes on cigarettes in California | Dynamic computer simulation model | Reduction in smoking prevalence due to price increases; QALYs; health care savings realised; changes in tax revenues (amount of taxes gained or lost) |
A 20% tax-induced cigarette price increase would reduce smoking prevalence from 17% to 11.6% with large gains in cumulative life years (14 million) and QALYs (16 million) over 75 years. Total spending on cigarettes by consumers would increase by US$270 million in that span (all going to tax revenue), and those who reduce the number of years spent as a smoker would spend US$12.5 billion less on cigarettes. Total smoking-related medical costs would drop by US$118 billion. These benefits increase greatly with larger tax increases, with which tax revenues continue to rise even as smoking prevalence falls. |
| Ahmad (2005b) | California, USA | To evaluate the cost effectiveness of raising the legal smoking age in California state to 21 | Cost benefit analysis; dynamic computer simulation model | Reducing in smoking prevalence; change in cumulative quality-adjusted life years (QALYs); medical cost savings; cost of law enforcement; and cost of checking identification |
Compared to a status quo simulation, raising the smoking age to 21 would result in a drop in teen (ages 14–17) smoking prevalence from 13.3% to 2.4% (82% reduction). The policy would generate no net costs, in fact saving the state and its inhabitants a total of US$24 billion over the next 50 years with a gain of 1.47 million QALYs compared to status quo. This research should prove useful to California's policy makers as they contemplate legislation to raise the state's legal smoking age. |
| Ahmad (2005c) | USA | To evaluate the projected health benefits and cost savings of a national policy to raise the legal smoking age to 21 in the US | Cost–benefit analysis; dynamic computer simulation model | Reducing in smoking prevalence; change in cumulative quality-adjusted life years (QALYs); medical cost savings; cost of law enforcement; and cost of checking identification |
Under this policy, raising the smoking age would reduce smoking prevalence for adults (age 18+) from the status quo level of 22.1–15.4% after 50 years. Prevalence would drop from 20% to 6.6% for 14–17-year-olds, from 26.9% to 12.2% for 18–20-year-olds, and from 21.8% to 15.5% for the 21+ group. The policy would produce a net cumulative savings to society of US$212 billion (driven by reduced medical costs), and the accumulation of nearly 13 million additional QALYs over the period. |
|
|
|||||
| Lightwood et al (2008) | USA | To investigate the effect of California's comprehensive tobacco control program (CTCP) on aggregate personal health care expenditures in the state | Cointegrating regressions (with other states as control variables) | Differences in per capita cigarette consumption as well as differences in per capita health care expenditures between California and the control states. | Between 1989 and 2004, CTCP reduced personal health care expenditures by an average of $86 billion (2004 US dollars)–-95% confidence interval [CI] $28 billion to $151 billion. This reduction grew over time, reaching 7.3% (95% CI 2.7%–12.1%) total health care expenditures in 2004. |
| Hurley and Matthews (2008) | Australia | To assess the cost effectiveness of Phase 1 of the Australian National Tobacco Campaign (NTC). This program, which commenced in 1997, cost around A$9 million and reduced smoking prevalence by 1.4% | Quit-benefits model (QBM); Markov-cycle simulation model | Measures of effectiveness included: cases of lung cancer, AMI, and COPD avoided; deaths prevented; life years and QALYs gained. Future savings in health care costs, life years and QALYs were discounted at 3% per year. |
The QBM predicted that the NTC avoided 32,000 cases of COPD, 11,000 cases of AMI, 10,000 cases of lung cancer, and 2500 cases of stroke. The NTC also predicted the prevention of around 55,000 deaths, 323,000 life-years gains, 407,000 QALYs, and health care cost savings of $A740.6 million. |
| Thavorn and Chaiyakunap ruk (2008) | Thailand | To estimate the incremental cost–effectiveness ratio of a structured community pharmacist-based smoking cessation program compared with usual care | Markov model | Cost per life year gained (LYG) attributable to the smoking cessation programm |
The community pharmacist-based smoking cessation (CPSC) programme results in cost savings of 17,503.53 baht (£250; €325; US$500) to the health system and life year gains of 0.18 years for men and; costs savings of 21,499.75 baht (£307; €399; US$614) and life year gains of 0.24 years for women. A series of sensitivity analyses demonstrate that both cost savings and life year gains are sensitive to variations in the discount rate and the long-term smoking quit rate associated with the intervention. |
| Owen and Youdan (2006) | UK | To evaluate the impact and relevance of the national awareness day “No Smoking Day”, 22 years after it was launched | Triangulation of data from a variety of sources; Retrospective surveys. | Self-reports of awareness and smoking behavior changes 1 week and 3 months after “No Smoking Day; Volume of media coverage, visits to “No Smoking Day” Website; and Volume of calls to national smokers’ help lines |
“No Smoking Day” achieved 78% awareness rate in 2004. 14% of smokers in UK (ie, about 1,840,000 out over 12 million UK smokers) claimed to have quit or reduced smoking on “No Smoking Day”. Three months after the day, about 85,000 smokers (representing about 0.7% of UK smokers) were still found in abstinence status. Calls to smokers’ helplines on “No Smoking Day” are typically four times those received on normal days. |
| Ross et al (2006) | USA | To evaluate the effectiveness and economic impact of a community-based tobacco control project (The Full Court Press Project) | Sensitivity analyses | Quit rates; discounted life years gained; real discounted cost per quit and per life year gained | A sensitivity analysis that assumed 5% program persistence (ie, 5% of the program's impact would last forever in the absence of future funding for the program), one-third would relapse and that one-third of those who quit have quit smoking even without the program, suggested a lower cost per discounted life-year saved of US$3,476. The cost effectiveness of this project compares favorably with other tobacco control interventions. |
| Godfrey et al (2005) | UK | To investigate the cost effectiveness of English specialist smoking cessation services | Observational cost and outcome data; Multivariate analysis | Cost–effectiveness ratios; smoking cessation rates attributable to service intervention as well as attributable life-years gained. |
Average cost per life-year gained was £684 (95% CI 557–811), reducing to £438 when future health care costs were counted. Assuming worse case scenarios, the estimate of cost effectiveness rose to £2693 per life-year saved (£2293 including future health care costs) and fell to £227 (£102) under most favorable conditions. |
| Collins and Lapsley (2005) | Australia | To estimate the social cost of tobacco use in NSW for the financial year 1998/99 as well as the value of the social benefits accruable from a reduction in smoking prevalence | Cost–benefit analysis; Demographic methodology; sensitivity analyses | Cost–benefit ratios; reduction in smoking prevalence rates; annual real social costs; changes or decline in avoidable and unavoidable social costs; present value of social benefits per smoker |
Model assumed that if current public policies on smoking were maintained, smoking prevalence in NSW will reduce from 18.1% in 2001 to 13.1% by the end of 2006. In addition, the social benefits from reduction in smoking prevalence in NSW by 5 percentages points would yield a present value of benefits of AUD$2, 366 (or AUD$9,046 per smoker) on the basis of most conservative estimates and AUD$5, 835.5 million (or AUD$22, 311) on the basis of most plausible estimates. |
| Secker-Walker et al (2005) | Vermont and New Hampshire, USA | To estimate the cost effectiveness of a four year, multi-faceted, community-based research project shown previously to help women quit smoking | Quasi-experimental matched control design | Cost-effectiveness ratio, as dollars per life-year saved, for the intervention only and for total grant costs (intervention, evaluation and indirect costs) | The cost-effectiveness ratio for the intervention, in 2002 US$ per life-year saved, discounted at 3%, was US$1,156 (90% CI US$567 to ∞), and for the total grant, US$4022 (90% CI US$1,973 to ∞) when discounted at 5%, these ratios were US$1,922 (90% CI US$3555-US$54,422), respectively. |
| Stevens, Thorogood, and Kayikki (2002) | London, UK | To evaluate the cost effectiveness of a community smoking cessation intervention, aimed at a high risk Turkish community in London | Monte Carlo simulation; sensitivity analyses | Cost per 1 year quitter; cost per life year saved |
57% of the Turkish population were smokers at baseline, compared with 39% in the general population of Camden and Islington. Levels were particularly high in younger women. At follow-up, there was a net reduction in smokers of 6.4% (95% CI 0-13.6%] in responders. When all study subjects were included, the net reduction was 2.9% (CI 0-6.3%). Most quitters were light smokers to start with. At follow-up, 51% of respondents recognized at least one of the Turkish language interventions. The estimated cost effectiveness of this intervention was £105 (range £33-391) per life year gained. Campaigns targeted at groups with high smoking prevalence may be more cost effectiveness than general population campaigns. |
|
|
|||||
| Clayforth et al (2014) | Western Australia | To assess the relative cost effectiveness of various non-television advertising media in encouraging 25-39-year-old male smokers to respond to a cessation-related call to action | Testimonial advertisements for radio, press and online media; sensitivity analysis | Costs per additional call to the quitline; costs per additional visit to the website; costs per additional registrations for QuitCoach; costs per additional registration for the call-back counseling service; costs per unweighted total of additional events; costs per weighted total of additional events |
Costs/quitline calls was lower (AUD$1,106) for online campaign, compared to radio (AUD$5,223) and press campaign (AUD$3,042), and integrated (AUD$4.377). Costs/total visits/calls/registrations was lower (AUD$43) for online media compared to radio (AUD$2,394), press campaign (AUD$1,888) and integrated (AUD$185). Costs/weighted total for online media was lower (AUD$472) compared to radio (AUD$4,267), press campaign (AUD$4,655) and integrated (AUD$1,567). Clearly, the online-only campaign phase was substantially more cost effective than the other phases, including the integrated approach. |
| Rasmussen (2013) | Denmark | To assess the cost effectiveness of the Danish smoking cessation telephone service “quitline” | Cost-benefit analysis, sensitivity analyses | Costs per life-year saved (LYS), point prevalence of abstinence at 12 months follow-up |
A total of 511 ex-smokers have been estimated to gain 2172 life years based on continued abstinence over 12 months. Using the point prevalence abstinence at 12 months, 799 ex-smokers are estimated to gain 3,394 life years. Discounting LYS at 3% p.a., the costs per LYS are €213 for ex-smokers with continued abstinence and €137 for ex-smokers with point prevalence abstinence. The sensitivity analysis for a worst case scenario indicates that the costs per LYS are €1199. For comparison, the average costs per LYS of smoking cessation interventions in other Danish settings are €1592 (95% CI €1547-1636). |
| Smit et al (2013) | Netherlands | To assess the cost effectiveness and cost utility of an internet-based multiple computer tailoring smoking cessation program and tailored counseling by practice nurses working in Dutch general practices compared with an internet-based multiple computer-tailored program only and care as usual | Randomized control trial (RCT), sensitivity analyses | Self-reported cost and quality of life at 12-month follow-up; prolonged abstinence; 24-hour and 7-hour point prevalence abstinence at 12-month follow-up; incremental cost effectiveness ratio (ICER) |
No significant differences were found between the intervention arms with regard to baseline characteristics or effects on abstinence, quality of life, and addiction level. However, participants in the multiple tailoring and counseling group reported significantly more annual health care-related costs than participants in the usual care group. Cost–effectiveness analysis, using prolonged abstinence as the outcome measure, showed that the mere multiple computer-tailored program had the highest probability of being cost effective. Compared with usual care, in this group €5,100 had to be paid for each additional abstinent participant. With regard to cost-utility analyses, using quality of life as the outcome measure, usual care was probably most efficient. |
| Guerriero et al (2013) | UK | To examine the cost effectiveness of smoking-cessation support delivered by mobile phone text messaging | Incremental cost–benefit analysis, Markov model, deterministic sensitivity analyses, probabilistic sensitivity analyses | Life years (LYs) gained per quitter, cost of text based support per number of enrolled smokers |
The cost of text-based support per 1,000 enrolled smokers is £16,120, which, given an estimated 58 additional quitters at 6 months, equates to £278 per quitter. However, when the future NHS costs saved (as a result of reduced smoking) are included, text-based support would be cost saving. It is estimated that 18 LYs are gained per 1,000 smokers (0.3 LYs per quitter) receiving text-based support, and 29 QALYs are gained (0.5 QALYs per quitter). The deterministic sensitivity analysis indicated that changes in individual model parameters did not alter the conclusion that this is a cost-effective intervention. Similarly, the probabilistic sensitivity analysis indicated a >90% chance that the intervention will be cost saving. |
| Chen et al (2012) | UK | To examine the effectiveness and cost effectiveness of internet, PC, and other electronic aids to help people stop smoking | Randomized controlled trials (RCTs); meta analyses; Bayesian mixed-treatment comparison (MTC) meta-analyses; survival models; decision analytic model | Prolonged abstinence; cost per user of electronic intervention; WTP/QALY |
Making some form of electronic support available to smokers actively seeking to quit is highly likely to be cost effective. This is true whether the electronic intervention is delivered alongside brief advice or more intensive counseling. For a willingness to pay (WTP) of £20,000/QALY, threshold analysis found that an electronic intervention would be cost-effective up to a cost of £1,053 per user (with NRT and brief advice) or £1,387 (with NRT and counseling). If the WTP rose to £30,000/QALY, the equivalent thresholds were £1,579 and £2,081 per user. The effectiveness of electronic interventions does not seem to be sensitive to cost differentials. However, the key source of uncertainty is that which relates to the comparative effectiveness of different types of electronic interventions. |
| Villanti et al (2012) | USA | To estimate the costs and cost utility of a smoking essation mass media (TV and radio) campaign called “EX” for adult smokers | Random-digit-dial method; cohort analysis; cost–utility analysis; sensitivity analyses | Intervention costs; Cost per quality-adjusted life-year (QALY) |
The incremental societal cost of EX, in 2009 dollars, was US$166 million. Data from eight designated media market areas studied indicate that in a hypothetical nationwide cohort of 2,012,000 adult smokers ages 18–49, EX resulted in 52,979 additional quit attempts and 4,238 additional quits and saved 4,450 QALYs. Incremental cost–utility estimates comparing EX to the status quo, that is, the situation that would have existed in eight markets with no campaign and no change in cessation behavior–-ranged from a cost of US$37,355 to US$81,301 per quality-adjusted life year, which suggests that the campaign was cost effective. |
| Smith et al (2007) | USA | To evaluate the incremental effectiveness and cost-effectiveness of a stage-based, computerized smoking cessation intervention relative to standard care in an urban managed care network of primary care physicians | Decision-analytic model based on results of a randomized clinical trial (RCT); sensitivity analyses | Seven-day point prevalence abstinence at 6 months post-intervention; QALYs; cost per patient per life year saved and per QALYs saved |
Intervention patients were 1.77 times more likely to be smoke-free at 6 months follow-up than those in standard care (P = 0.078). The intervention generated an additional 3.24 quitters per year. Annualized incremental costs were US$5,570 per primary care practice, and US$40.83 per smoker. The mean incremental cost effectiveness ratio was US1,174 per life year saved (US$869 per QALY). When the intervention impact on progression in stage readiness to quit was also considered, the mean incremental cost effectiveness ratio declined to US$999 per life year saved (US$739 per QALY). |
| Farrelly, Hussin, and Bauer (2007) | New York, USA | To assess the relative effectiveness and cost-effectiveness of TV, radio and print advertisements to generate calls to the New York smokers’ quitline | Regression analysis | Monthly total county calls to the New York smokers’ quitline; TV expenditures; radio expenditures; Newspaper expenditures; elasticity of for TV expenditures |
There was a positive and statistically significant relation between call volume and expenditures for TV (P < 0.01) and radio (P < 0.01) advertisements and a marginally significant effect for expenditures on newspaper advertisements (P < 0.065). The largest effect was for TV advertising. However, because of differences in advertising costs, for every US$1,000 increase in TV, radio, and newspaper expenditures, call volume increased by 0.1%, 5.7%, and 2.8%, respectively. |
|
|
|||||
| Brown et al (2012) | India | To evaluate the cost effectiveness of a youth tobacco use prevention program, known as Mobilizing Youths for Tobacco-Related Initiatives (MYTRI), which has been translated and implemented in India, a developing country | Cost effectiveness ratio (CER), both quality adjusted and non-quality adjusted | Dollars per life year added due to intervention |
The tobacco use progression model showed that approximately 12 people were projected to avert tobacco use by age 26 due to MYTRI. At 2.88 life-years added per averted tobacco user, this translates into 35 life-years added due to MYTRI. If quality-adjusted, this rises to 54 life-years. The cost per quality-adjusted life-year added due to averted smoking was US$2769. If not quality-adjusted, the cost per life year added due to averted smoking was US$4348. If we ignore student time, the cost effectiveness improves by roughly 10%. To put the cost effectiveness of this smoking prevention program in context, it is over 24 times more cost effective than dialysis in the USA, which costs US$50,000 for a life-year. |
| Hollingworth et al (2011) | England and Wales | To evaluate the cost effectiveness of a school-based “peer-led” intervention program known as ASSIST (A Stop Smoking In Schools Trial) | Cluster randomized controlled trial | Cost per student within each school, incremental cost effectiveness ratio (ICER) representing the cost per additional student not smoking at the 2 year follow-up | The ASSIST program cost £32 per student (95% CI = £29.70– £33.80). The incremental cost per student not smoking at 2 years was £1,500 (95% CI = £669–£9,947). Previous work has demonstrated that the ASSIST program achieved a 2.1% (95% CI = 0%–4.2%) reduction in smoking prevalence. Results show ASSIST is cost effective under realistic assumptions. |
| Hoeflmayr and Hanewinkel (2008) | Germany | To evaluate the cost effectiveness of a school-based tobacco prevention program, known as Smoke-free Class Competition (SCF) | Stochastic progression model, sensitivity analyses | Number of students prevented from becoming established smokers, benefits per prevented smoker, direct and indirect costs per prevented smoker | In school year 2001/2002, it is estimated that the SFC prevented 3,076 students from becoming established smokers, with net benefits of 5.59 Mio. Euro (direct net benefits) and 15.00 Mio. Euro (total net benefits). The direct benefit/cost ratio was 8.2 and the total benefit/cost ratio was 3.6. Data suggests that the SFC is a cost-effective school-based intervention. |
| Wang et al (2001) | USA | To determine the cost effectiveness of a school-based tobacco-use prevention program, known as Project Toward No Tobacco Use (TNT) | Decision analysis | Life years (LYs) saved, quality-adjusted life years (QALYs) saved, and medical care costs saved, discounted at 3% | Under base case assumptions, at an intervention cost of US$16,403, TNT prevented an estimated 34.9 students from becoming established smokers. As a result, a saving of US13.316 per LY saved and a saving of US$8,482 per QALY saved could be expected. Results showed TNT to be cost-saving over a reasonable range of model parameter estimates. |
| Tengs, Osgood, and Chen (2001) | USA | To evaluate the cost effectiveness of enhanced nationwide school-based anti-tobacco education relative to the status quo | Tobacco Policy Model, a system dynamics computer simulation model – designed to calculate the expected costs and public health gains of any tobacco policy or intervention over any time frame | Cost per quality-adjusted life year (QALY) | Over 50 years, cost effectiveness is estimated to lie between US$4,900 and US$340,000 per quality-adjusted life-year (QALY), depending on the degree and longevity of program effectiveness. Assuming a 30% effectiveness that dissipates in 4 years, cost effectiveness is US$20,000/QALY. Sensitivity analysis reveals that cost effectiveness varies with cost, survival, and quality of life estimates but cost effectiveness ratios generally remain favorable. |
|
|
|||||
| Cahill and Lancaster (2014) | UK | To evaluate the effectiveness and cost effectiveness of workplace interventions aimed at helping workers to quit smoking | Meta analyses of main workplace interventions, using the generic inverse variance method to generate odds ratios and 95% confidence intervals | Odds ratio (OR), confidence intervals (CI) |
Group therapy programs OR for cessation 1.71, 95% CI 1.05–2.80; eight trials, 1309 participants). Individual counseling (OR 1.96, 95% CI 1.5–2.54; eight trials, 3516 participants). Pharmacotherapies (OR 1.98, 95% CI 1.26–3.11; 5 trials, 1092 participants). Multiple intervention programmes aimed mainly or solely at smoking cessation (OR 1.55, 95% CI 1.13–2.13; six trials, 5018 participants) all increased cessation rates in comparison to no treatment or minimal intervention controls. Self-help materials were less effective (OR 1.16, 95% CI 0.74–1.82; 6 trials, 1906 participants). Two relapse prevention programs (484 participants) did not help to sustain long-term abstinence. |
| Jackson et al (2007) | USA | To conduct a cost–benefit analysis (CBA) of varenicline versus bupropion from the perspective of an employer over a 1 -year time frame, using clinical outcomes data | Decision tree model, sensitivity analyses | Smoking status, medication compliance, abstinence rates and quit rates with placebo, varenicle and bupropion, net benefits of changes in cost savings to employer for each employee who had quit smoking |
Estimated 12-month employer cost savings per nonsmoking employee were $540.60 for varenicline, $269.80 for bupropion SR generic, $150.80 for bupropion SR brand, and $81.80 for placebo. Varenicline was more cost beneficial than placebo, which had quit rates of 16.9% or less. The quit rate with varenicline would have to be <16.9% to lose cost benefit over bupropion SR generic. |
| Ong and Glantz (2004) | USA | To estimate the cardiovascular health and economic effects of smoke-free workplaces | Monte Carlo simulation; sensitivity analyses | Number of quitters after smoke-free workplace policy within 1 year; savings from prevented myocardial infarctions; savings from prevented stroke; savings from prevented myocardial infarctions in previous passive smokers |
The first year effect of making all workplaces smoke free would produce about 1.3 million new quitters and prevent over 950 million cigarette packs from being smoked annually, worth about US$2.3 billion in pretax sales to the tobacco industry. In 1 year, making all workplaces smoke free would prevent about 1500 myocardial infarctions and 350 strokes and result in nearly US$49 million in savings in direct medical costs. At steady state, 6250 myocardial infarctions and 1270 strokes would be prevented, and US$224 million would be saved in direct medical costs annually. Reductions in passive smoking would account for 60% of effects among acute myocardial infarctions. |
| Warner et al (1996) | USA | To examine the health and economic implications of a workplace smoking cessation program by using a simulation model that includes, among its novel features, consideration of long-term as well as short-term implications and evaluation of the effects of employee turnover on benefits derived by both the firm and the broader community. | Cohort model, Monte Carlo simulation, sensitivity analysis | Health and behavioral outcomes: amount of smoking cessation, reductions in number of deaths, gains in life expectancy and reductions in absenteeism. Economic and financial outcomes include: intervention costs, reductions in health care costs, absenteeism costs, on-the-job-productivity losses, and life insurance costs Net cost savings (benefit–cost ratio) |
Smoking cessation is a very sound economic investment for the firm, and is particularly profitable when long-term benefits are included, with an eventual benefit–cost ratio of 8.75. Saving life-years at a cost of $894 each, the program is more cost effective than most of the conventional medical care covered by the firm's insurance. |
