Abstract
Iron oxide contrast agents have been combined with magnetic resonance imaging for cell tracking. In this review, we discuss coating properties and provide an overview of ex vivo and in vivo labeling of different cell types, including stem cells, red blood cells, and monocytes/macrophages. Furthermore, we provide examples of applications of cell tracking with iron contrast agents in stroke, multiple sclerosis, cancer, arteriovenous malformations, and aortic and cerebral aneurysms. Attempts at quantifying iron oxide concentrations and other vascular properties are examined. We advise on designing studies using iron contrast agents including methods for validation.
Introduction
Magnetic resonance imaging (MRI) has been combined with various contrast agents to enhance tissue contrast. Iron oxide nanoparticles are largely used as a negative contrast agent, causing hypointense contrast.1,2 Per mole, iron-based contrast is generally stronger than gadolinium (Gd), the most common contrast agent. 3
MRI cell tracking was introduced in 1993 to look at cell survival and migration after grafting. 4 In 2001, the first in vivo time course of cell migration was reported. 5 As the field developed, in vivo studies tracking cells–-eg, neural cells, 4 stem cells, 5 and dendritic cells (DCs) 6 –-became increasingly popular. The strength of iron oxide is such that researchers have even succeeded in tracking single cells in vivo.7–9
The flexibility of iron oxide particles cannot be understated; they have been used to target specific molecules, 10 track and deliver therapeutic drugs,11,12 label cancer vaccine effecting cells, 6 track inflammation, 13 visualize organs 14 and vasculature, 15 and heat and kill cancers. 16
Iron oxide particles come in a range of types and sizes, including ultrasmall superparamagnetic particles of iron oxide (USPIOs; 5–50 nm), superparamagnetic iron oxide particles (SPIOs; 50–150 nm), 1 and micron-sized iron oxide particles (MPIOs), such as Bangs MC03F particles (≍1 μm).
Coating Properties
Iron nanoparticles interact with each other magnetically and via van der Waals’ interactions. These interactions cause iron nanoparticles to flocculate. This flocculation may be overcome by coating the iron nanoparticles. 17 As clumping is undesirable for imaging applications and makes cell labeling difficult, in biological applications, iron nanoparticles are typically coated. 5 Flocculation can often be predicted by the nanoparticles zeta potential, the potential at its shear layer. 18 Nanoparticles that have strong negative or positive zeta potentials tend to repel and, hence, do not flocculate. 18 The zeta potential is dependent on environmental conditions (eg, pH, temperature, and solvent composition); hence, flocculation is somewhat environment-dependent. The internalization of iron nanoparticles within cells may change both the cells’ and the nanoparticles’ zeta potentials. 19 Negatively charged coatings may have a positive zeta potential, and vice versa. Negatively charged coatings have been reported as having superior ex vivo uptake.20–23 Positively charged coatings have also been used to a great extent.24–28 In an in vivo setting, the blood-pool lifetime of nanoparticles is partially determined by coating. Hydrophobic coatings tend to incur shorter half-lives. 29
Iron nanoparticles are also coated for reasons of cytotoxicity; uncoated iron oxide nanoparticles have been shown to increase the generation of reactive oxygen species (ROS), 30 reduce cellular proliferation, 31 and even induce cell death 30 though typically not at low concentrations. 32 Uncoated SPIOs have been shown to have up to a sixfold increase in cytotoxicity compared to dextran-coated iron nanoparticles. 30 The best characterized coating for iron nanoparticles to date has been dextran, owing perhaps to its early approval for human work, and early biological characterization. 33 Although dextran-coated USPIOs are safe at low concentrations, they have been shown to incur hemolysis, platelet aggregation, and increased immune system activity at high concentrations. 34
Studies of novel coating types commonly compare new coatings to dextran coatings and often report enhancements in cellular uptake.20,35,36 Even coated nanoparticles may incur varied biological effects in labeled cells. For example, ferucarbotran-coated SPIOs increased mesenchymal stem cell (MSC) proliferation, owing to iron nanoparticles peroxidase-like activity. 37 Investigations into biocompatibility of coatings can be at the cellular or at the system levels. For example, citrate-coated USPIOs have been shown to temporarily increase ROS in rat macrophages though without cytotoxic effects, 38 while cationic USPIOs apparently induced no microhemorrhage or thrombus, no inflammatory processes, and no effect on hepatic or renal enzymes. 26 Specialized coatings have also been used to more precisely label cells in vivo. The nanoparticle coating can itself be conjugated with molecules of interest. Experiments have been performed with Herceptin-dextran-coated SPIOs, which provided useful contrast in cancer lines expressing HER2/neu. 39 Similar work has been performed with folic acid-poly(ethylene glycol)-coated SPIOs, which provided contrast in tumors expressing folate receptors, 40 and with prostate-specific membrane antigen (PMSA), which bound to PMSA positive tumors. 41 A thorough review of coatings for iron nanoparticles has been written by Gupta and Gupta. 5
Iron Pharmacokinetics
Upon entering the bloodstream, SPIOs are phagocytosed by the reticuloendothelial system (RES; or macrophage– monocyte system) that removes SPIOs by receptor-mediated endocytosis from the blood pool. These nanoparticles are typically taken up by macrophages and phagocytic cells in the liver, bone marrow, and spleen.
The lysosomal compartments of macrophages gradually degrade the iron nanoparticles, 42 with radioactive tracers showing that the iron is ultimately incorporated into the body's iron store. 43 The degradation rate of MPIOs is significantly slower than that of smaller nanoparticles; under some circumstances, these particles can be observed on MRI months later. 44 The biodegradation rate of these particles can be varied, depending on size and coating. 45
Blood-pool half-life is dependent on several factors, including size, coating, dose, and charge. The half-lives of these nanoparticles are in the order of minutes 46 to hours. 47 The half-life dose dependence is relatively minimal, with clinical dose ranges having similar pharmacokinetic profiles. Smaller SPIOs tend to have longer half-lives. 23 Human blood-pool half-lives are significantly longer than those of small mammals. For example, ferumoxytol's half-life in humans is 24–36 hours, while in rats, it is 2–3 hours. 47 Hence, USPIO experiments in animals typically require significantly higher doses, often on the order of 10 times the human dose per kilogram of body weight.
Magnetic Characterization of Iron Oxides
The paramagnetism induces magnetic field inhomogeneities. There are reductions in T1, T2, and

The magnetic field of an iron-labeled cell and its relation to the main magnetic field: the magnetic field is enhanced in the z direction and suppressed in the × direction. (A) FLASH image showing the bloom effect of iron in the MRI image. (B) RARE T2-weighted image. (A and B have FeREX-labeled ESCs (4000 cells) at the top of the image and 5 μl of FeREX solution at the bottom. ESC labeling was accomplished by incubating a monolayer of ESCs (at 80% confluence) for 24 hours in 5% CO2 at 37°C in a serum-free optimum medium with FeREX and Lipofectamine 2000 at a concentration of 25 μg Fe/mL).
Quantifying the efficiency of MRI contrast agents allows us to assess whether they have sufficient relaxivity for magnetic resonance (MR) visualization. The relaxivity value (r1, r2, and
Relaxation rate changes linearly with the concentration of contrast agent over a wide concentration range (Fig. 2) and is sensitive to field strength. Relaxivity also depends on iron oxide configuration; nanorods have been shown to have significantly greater relaxivity.
49
Nanoparticles with some degree of ferrimagnetism also evidence much stronger relaxivity; this has been used to enable single-cell tracking.
7
Relaxivity graphs for Bangs, FeREX, and Feridex particles and the corresponding MRI phantom images showing the different concentrations of dissolved contrast agents. R2 and 
A comparison between several common iron oxide contrast agents. PSC is polyglucose sorbitol carboxymethylether. Approval in some cases is not for imaging but for treatment of anemia (eg, ferumoxytol). Relaxivities of Feridex, Resovist, and Supravist at 3T are made in H2O at 37°C by the study of Rohrer, Bauer, Mintorovitch, Requardt, and Weinmann. 174 Relaxivity of ferumoxytol 175 and FeREX 176 are more recent.
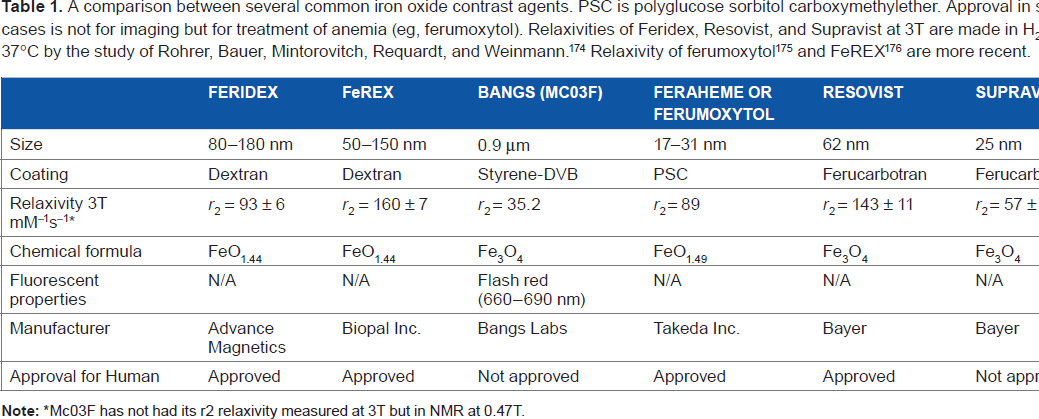
Mc03F has not had its r2 relaxivity measured at 3T but in NMR at 0.47T.
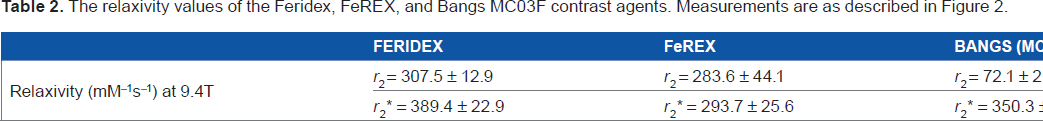
The relaxivity values of the Feridex, FeREX, and Bangs MC03F contrast agents. Measurements are as described in Figure 2.

Overview of Ex Vivo Labeling of Cells
Ex vivo labeling involves cell labeling outside of a living body by culturing cells with iron oxide. Subsequently, these labeled cells are injected or implanted into the organs of interest and imaged using MRI. Histology is used to confirm that iron is present in the loaded cell. It is possible for a labeled cell to die, releasing the iron; in such a situation, the iron could then be taken up by macrophages just as it would be in an in vivo labeling study.
Ex vivo labeling may have the advantage of increased specificity in the target cells. Cells not especially prone to endocytosis of iron nanoparticles, nonetheless, may be saturated in an environment where only the cells of interest may uptake the labeling compound without competition from incidental cells. Experiments examining the utility of a particular species of iron nanoparticle tend to emphasize the characterization of three traits: iron uptake in cultured cells, capacity to label daughter cells, and biological effects (e.g. apoptosis, non-viability of labelled cells, reduced protein production, etc.) of the nanoparticle.
Stem cells
Stem cells are an area of significant research interest as they may provide novel avenues for therapeutic treatments. 54 One appealing aspect of stem cell repair is their capacity to hone in on the site of injury. Thus, it is of interest to track the migration of stem cells to evaluate delivery efficiency without impairing the biological function of the stem cells. Labeling stem cells with iron oxide nanoparticles has grown into a popular technique in recent years, as with the correct biological coating or transfection agents, iron uptake can be accomplished with high efficacy.55,56
While iron nanoparticles, when used in labeling concentrations, do not totally inhibit stem cell function, 57 cellular viability does decrease in a dose-dependent manner at high concentrations in a variety of iron oxides.20,58 While dextran-based coatings remain the most common coating for cellular labeling, citrate, 20 aminosilane, 58 and unfractionated heparin 36 coatings have been shown to improve stem cell uptake of iron nanoparticles. Conjugation with transfection agents, such as the HIV tat peptide, has yielded labeling rates of up to 10–30 pg Fe/cell, allowing for single-cell tracking of stem cells. 59
While it is common to track injected stem cells via iron oxide labeling MRI, MRI does not distinguish between iron encapsulated within a surviving stem cell and iron recovered from apoptotic cells by macrophages. Histology has shown that MR signal from labeled and transplanted cells persists after cell death owing to tissue-bound macrophages. 60 This highlights the necessity of some external measure of validation (usually histology) to confirm that the cells labeled are the ones still being tracked.
A key aspect of stem cells is their proliferative ability. This may make maintaining the iron oxide label over multiple generations challenging. 44 Although this may not be a concern for stem cells that remain fixed while proliferating, it can make migrating stem cells challenging to track. One study that examined neuroblast migration along with the rostral migration stream to the olfactory bulb used MPIOs for their biological longevity and ability to label even with only a few particles. 44 MPIOs may prove ideal for long-term studies of stem cells, especially with MPIOs detectable with only a single particle. 61
A study done by Taha et al
62
labeled embryonic stem cells (ESCs) using FeREX. The labeled ESCs were imaged using fast low angle shot (FLASH) and rapid acquisition with relaxation enhancement (RARE) T2 sequences. In MRI, the 4000 FeREX-labeled ESCs were detectable, appearing as a hypointense area with susceptibility artifacts surrounding it in FLASH and RARE T2 sequences (Fig. 1B and 1C). This was confirmed with Prussian blue (PB) for histology, which showed that iron is inside the cells (Fig. 3).
FeREX-labeled single layer of ESCs. (A & B) stained with PB; iron appears as blue spots. (C) PB-stained section and counterstained with nuclear fast red. Different aggregates of ESCs appear as red areas, and iron appears as blue spots. The cell labeling procedure here is the same as in Figure 1.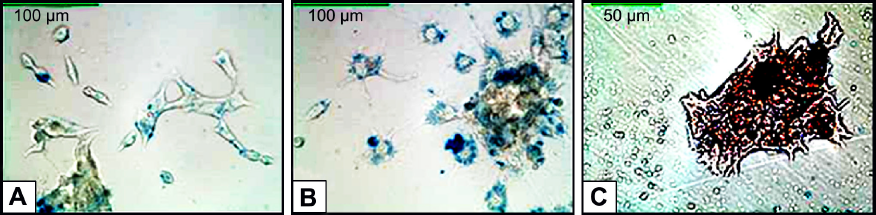
Regenerative therapies using MSCs have been proposed for bone and cartilage repair. The exact role that MSCs play in repair is not fully characterized, so a noninvasive way to monitor stem cell migration would be useful. Histology and mass spectroscopy have shown that it is possible to label human MSCs without adversely impacting viability or proliferation. 63 Adipogenic, osteogenic, and chondrogenic differentiations of labeled cells were shown to be unaffected by gene expression. 63 However, MSC labeling approaches have seen impairment of chondrogenic differentiation with increasing dose of SPIO. 20 That said, the optimization of dosage and loading can minimize such impairment to negligible levels.64,65 Human MSCs have been labeled and visualized by MRI in the collagen hydrogels that are now clinically used for cartilage repair.63,66 MSCs have been used in a rabbit model of cartilage knee injury. 67 The injection of labeled MSCs caused signal decline in the defect, which reached a maximum at 4 weeks and returned to baseline after 12 weeks. Histology found labeled MSCs in the injury at 4 weeks, and none at 12 weeks, though they could be found outside the lesion. Animals treated with MSCs showed enhanced recovery; thus, these MRI results suggested that stem cells recruit native cells for repair.
Demyelination is common to many pathological conditions. Exogenously applied oligodendrocyte progenitors have been shown to support remyelination. 68 Oligodendrocyte progenitors are highly mobile and their movement correlates well with remyelination, 69 so iron labeling is also appropriate here. Bulte et al conjugated MION-46L with transferrin to label CG-4, an oligodendrocyte progenitor. 70 The labeled CG-4 cells were grafted into myelin-deficient rat spinal cords, and showed significant migration along the spine in MRI. 70 Regions of stem cell enhancement correlated strongly with new myelin formation. Improved neural progenitor labeling techniques have since been exactingly described. 71
It may even be possible to use magnetic labeling to direct the delivery of stem cells in vivo. Magnetically labeled cells migrate toward magnets in culture through a phenomenon known as magnetophoresis.72–74 One study injected labeled MSCs intravenously into rats and placed magnets over the livers of a subset of them. Those with magnetic direction had increased stem cell delivery to their livers, which corresponded to MR signal reductions. 72 Over the course of 30 days, MR enhancement faded, yet the MSCs remained fixed. Morphology of iron-labeled cells suggested that they were not simply Kupffer cells but appeared instead to be hepatocytes, perhaps originating as the injected MSCs.
Red blood cells
Contrast agents often clear from the blood within minutes to hours, but in some studies, it is desirable to have an agent that will remain circulating in the blood for days to weeks. A common role of MRI contrast agents is enhancement of the vasculature both to produce angiograms and venograms75,76 and to calculate cerebral blood volume (CBV) by saturating the blood pool with the contrast agent.77–79 However, the biological lifetime of free iron oxides in the blood is usually rather low, typically far less than 24 hours,80,81 and so to do repeated measurements one would need repeated injections.
One approach to overcome this limitation has been the encapsulation of USPIOs within red blood cells (RBCs), which have a biological half-life of 3 months. Half-lives of up to 20 days have been demonstrated with this technique. 82 A variety of USPIOs–-including commercially available Resovist and Sineram and experimental USPIOS–-have been tested for compatibility with this technique. 83 Silicon-coated agents tend to be poorly encapsulated, and citrate agents are unsuitable because of their tendency to adsorb to the cellular membrane, which triggers elimination by the RES.
RBCs tend not to spontaneously load SPIO.84,85 One loading technique requires that the integrity of the RBC's cellular membrane be temporarily compromised by hypotonic swelling in the presence of USPIOs and, after sufficient uptake, be restored. 86 This technique relies on the formation of pores between 50 and 200 nm in diameter, which are sufficient to allow passage of the nanoparticles. When performed successfully, the majority of loaded RBCs are successfully recovered, and these RBCs have similar hemoglobin concentrations, full cellular integrity, and surface properties to unloaded RBCs. 84 The loading procedure tends to reduce cell volume, regardless of whether USPIOs are loaded. 86
Research has shown that encapsulation slightly reduces the relaxivity of loaded USPIOs as compared to the bulk material in solution. 82 One explanation for this phenomenon is that the loading procedure favors the encapsulation of smaller nanoparticle crystals, which would reduce relaxivity slightly. Despite this slight reduction in relaxivity, loaded RBCs remain viable negative contrast agents that are highly compatible for use as a blood-pool enhancement or in magnetic particle imaging.
Overview of in Vivo Labeling of Cells
In vivo labeling involves injecting the contrast agent into an animal and having it taken up by cells. In vivo labeling of cells offers advantages compared to labeling cells in vitro and injecting them into the animal. One major advantage is that it is technically less challenging and less time-consuming, as one does not need to load the cells with USPIO in vitro. In addition, it offers a significant advantage in that it does not significantly introduce a foreign tissue into the animal, allowing one to monitor innate cell processes.
Macrophage–monocyte labeling
Labeling of macrophages has been shown to leave cells’ macrophages viable, with labeled macrophages migrating to the sites of inflammation.
87
SPIOs have been shown to enhance the sites of inflammation. There are several proposed avenues for this enhancement.
88
Macrophages in the blood could uptake SPIOs before migrating to inflamed tissues. Alternatively, SPIOs could be transported by transcytosis across the epithelium at the sites of inflammation prior to endocytosis by macrophages already in situ. Another possibility is that leakage from the vasculature may take place because of vessel dilation, which results in SPIO deposition in the region of inflammation. Blood–brain barrier (BBB) breakdown has been shown to be accompanied by USPIO enhancement without immune cell involvement in stroke.
89
In cases without a leaking vasculature, it has been suggested that the dominant mechanism is endocytosis and subsequent migration of blood monocytes to the sites of inflammation. Mice treated with lipopolysaccharide (LPS), a substance that elicits a massive immune response, showed significant USPIO enhancement compared to the control group (Fig. 4).
90
However, when the monocytes were depleted with clodronate sulfate, the USPIO enhancement was abolished, indicating that iron endocytosis via blood monocytes is critical for USPIO enhancement of inflammation.
90
Regardless of mechanism, long half-life SPIOs appear to be an effective tool for demarking inflammation.

Nonlymphocyte labeling
While iron oxides tend to be taken up by the RES, other cell types may be targeted in vivo. Since MPIOs only require a few particles to be endocytosed, injection of MPIOs into the ventricles has been shown to be sufficient to label endogenous neural stem cells. 44 Tumor models have shown uptake of USPIOs into the intracellular compartment. 91 In nude mice (ie, without macrophages), it was shown that intravenous application of USPIO alone can enhance tumor cells, albeit variably. 92
Targeted nanoparticles are those conjugated to some kind of targeting molecule. 10 The use of antibody coatings has enabled the in vivo labeling of antigen-expressing tumors.39,93 USPIOs conjugated to Aβ1–42 peptides were used to detect amyloid plaque deposition, and could identify Alzheimer's disease mouse models. Injected MPIOs conjugated with antibodies for CD81 have been used to visualize atherosclerotic plaques, 94 and MPIOs conjugated to an antibody for the glycoprotein IIb/IIIa receptor of activated platelets have been used to visualize atherothrombosis 95 in mice. MPIOs may be of value for these targeted applications, as they clear from the blood, deliver a high dose of iron, and rarely leak through the vasculature. In a comparison between Gd and MPIO conjugated to a ligand for intercellular adhesion molecule-1 (ICAM-1), it is found that while both bound to ICAM-1 in vivo (as determined by histology), only the MPIO yielded significant MRI enhancement in vivo. 96 Angiogenesis has been visualized using both USPIO and MPIOs conjugated to arginine-glycine-aspartic acid (RGD), which binds to the sites of angiogenesis. It was found that the RGD-MPIOs had significantly greater specific binding and provided better contrast of regions with angiogenesis. 97
Applications of Cell Tracking with Iron Nanoparticles
Ischemic stroke
Ischemic strokes are caused by a thrombus blocking off a major artery, reducing blood and oxygen delivery to the brain. The reduction of blood flow and oxygen causes acute tissue death (infarct). However, infarct volume continues to grow after the acute stage, suggesting that stroke-induced brain damage is not solely because of ischemia. 98 Blood-borne inflammatory cells infiltrate into the brain parenchyma after the initial ischemic insult; this is associated with the occurrence of postischemic neuronal loss. 98 Hence, monitoring inflammatory cell trafficking could be a useful prognostic marker in the subacute stages of ischemic stroke.
Several groups have shown that it is possible to noninvasively monitor blood monocyte migration by USPIO.99,100 Using a rat photothrombotic model of ischemic stroke, it has been shown that there is USPIO enhancement in the infarct area 6 days postischemia.99,100 Histology confirmed the colabeling of iron and proinflammatory phagocytes, indicating that brain inflammation during the subacute stage of stroke was detected by USPIO. Similar results have been obtained in a rat permanent middle cerebral artery occlusion model, with histology confirming USPIO colocalization with phagocytes on days 28 and 56. 101 One interesting trend was identified: inflamed regions without phagocytes (as imaged by USPIO) on day 7 tended to remain viable. This suggests that iron oxides may offer a noninvasive method of determining prognosis in stroke. Some caution is warranted, however. Stroke has been associated with BBB leakage (confirmed with Gd). Iron might leak through and subsequently be picked up by local macrophages, which could be confused with transiting invasive macropahges.89,102
Multiple sclerosis
Multiple sclerosis (MS) is a demyelinating, immune-mediated disease. Infiltrating macrophages are key players in demyelination 103 and typically tend to cluster in central nervous system (CNS) lesions typical of MS. Studying macrophage infiltration may yield insights into disease progression and treatment response.
Several studies have explored tracking macrophage infiltration with iron nanoparticles in the experimental autoimmune encephalomyelitis (EAE) model of MS in rodents. EAE is a well-characterized disease model that exhibits chronic inflammation and demyelination, similar to human MS.
104
Studies using iron nanoparticles in EAE and MS have been reviewed previously by Nathoo et al.
105
Studies tracking macrophage infiltration using iron nanoparticles in EAE models have demonstrated macrophage accumulation throughout the CNS, including in the spinal cord,22,106 brainstem,106,107 cerebellum,106,107 and cortex.108,109 It is worth noting that in cases where there is a high concentration of internalized iron, it is possible to visualize iron accumulation at the single-cell level,
22
making this a powerful tool for cell tracking. This is also relevant since studies have shown that iron deposition (corresponding to monocyte infiltration) occurs even in areas without BBB breakdown (as determined by Gd enhancement),110–112 suggesting translocation via macrophages. Similar discrepancies have been observed in human MS studies (Fig. 5).113–116 This suggests that not all regions of inflammation are associated with BBB breakdown. Thus, iron oxide nanoparticles allow for measurement of inflammation not possible with other MRI contrast agents.
Discrepancies are present in lesion visualization between Gd-enhanced MRI (for BBB breakdown) and USPIO MRI (for macrophage accumulation). More lesions are observed with USPIO MRI (white arrows) as compared to Gd MRI (white arrows). Figure adapted and reproduced with permission from Ref. 115.
Labeling of monocytes with iron nanoparticles is also used to assess drug treatment response in MS and other conditions associated with inflammation. Studies using iron nanoparticles with MRI to assess drug treatment response have been reviewed by Nathoo et al. 117 In particular, the responses to disease-modifying therapies, such as natalizumab 118 and fingolimod, 119 have been tested using monocyte-labeled USPIOs with MRI. Treatment with natalizumab reduced monocyte infiltration into the CNS of EAE animals but did not prevent it completely, 118 whereas fingolimod treatment prevented the formation of lesions detected by USPIO in EAE animals. 119
The response to lovastatin (a low-density lipoprotein lowering agent, thought to reduce cellular infiltration) has also been assessed in EAE animals using USPIOs. 110 Lovastatin suppresses monocyte infiltration, and it lessened the magnitude of the UPSIO darkening in treated EAE rats compared to untreated EAE rats. Less darkening by USPIOs correlated with improvements in EAE symptom scores. The results of these studies suggest that MRI with USPIOs can be used to track monocyte infiltration in inflammatory conditions and to assess response to treatments related to monocyte trafficking.
Cancer
Several approaches to visualizing tumors using USPIOs have been made. A common study design for cancer therapies entails the injection of a cancer line into a host animal. Some groups have labeled tumor cells, not hoping to visualize the immune cell response but simply to track the proliferation and spread of cancer in response to treatment. With recent advances in single-cell imaging, 120 some groups have managed to image single tumor cells in liver cancer, 121 though this has yet to be performed in a living animal.
Inflammatory immune cells, including tumor-associated macrophages (TAMs), affect cancer development. TAMs have been correlated with cancer prognosis. One group has explored GEH121333 and ferumoxytol, both USPIOs, to identify adenocarcinomas. 122 Persistent enhancement was observed from 24 to 72 hours later. Histology confirmed the internalization of USPIOs within TAMs.
In addition to their macrophage recruitment, tumors in the brain may also have associated microglia. 123 Fluorescently labeled USPIOs have been used to show that microglia internalize iron oxides at a high rate (above that of tumor cells and astrocytes). 124 In vitro work also showed that MR enhancement was dependent on immune cell count. 124 An in vivo rat study was conducted (16.74 mg Fe/kg delivered intravenous therapy with imaging preinjection and 24 hours postinjection) and showed significant tumor enhancement. Consistent with previous results, 125 the boundaries of tumors were enhanced, as phagocytic cells often form a barrier between tumor and brain.
Glioblastoma multiforme (GBM) is an aggressive CNS tumor with poor prognosis. There are some major applications of USPIOs in GBM. The first application is using multifunctional iron oxide nanoparticles to enhance the delivery of cytotoxic drugs to GBM. USPIO coatings can be modified to attach to tumor surface receptors, such as epidermal growth factor receptors, a receptor that is overexpressed in the majority of GBM tumors. 93 The modified iron oxide particles can then be attached to cytotoxic drugs, allowing more efficient delivery to tumor cells. It has been shown that treatment with a modified USPIOs tagged with cetuximab (a cytotoxic drug) resulted in significant antitumor effect compared to nontagged cetuximab, showing increased efficacy of cancer drug delivery to tumor cells. 93 Similar studies have been done, using modified USPIOs to deliver antitumor peptides, such as chlorotoxin. 126 The conjugation of therapeutic compounds to USPIOs is an interesting field with high potential. It opens up the possibility of noninvasively delivering a high-dose, cell-specific strategy to treat this aggressive cancer.
USPIOs are also used as blood-pool agents to differentiate pseudoprogression from true progression of tumors. Pseudoprogression is most commonly caused by radiation necrosis, which appears very similar to the recurrence of tumor on Gd-enhanced T1-weighted scans. 127 The current method of determining pseudoprogression is unreliable, as it does not have good correlation with survival. 127 Pseudoprogression can be determined by using dynamic contrast-enhanced MRI to measure CBV. Abnormalities with high CBV are suggestive of tumor, while abnormalities with normal or low CBV indicate pseudoprogression.127,128
Gd is the most common contrast agent used to measure CBV, but in GBM, the BBB is often broken, which results in contrast agents leaking into the tumor. 128 This yields an inaccurate CBV calculation and requires a leaking factor to be calculated in order to obtain the true CBV. 128 On the other hand, USPIOs, such as ferumoxytol, can act as blood-pool agents but do not exhibit contrast leakage even when the BBB is compromised. 129 Ferumoxytol has been shown to reliably differentiate pseudoprogression from cancer recurrence.127,128 It has been shown that abnormal regions with a low CBV (suggestive of pseudoprogression), as calculated using ferumoxytol, is associated with significantly prolonged survival compared to abnormal regions with high CBV (true progression).127,128 In addition, a leaking correction factor for CBV did not need to be calculated for ferumoxytol, unlike Gd. 128 Ferumoxytol can be a promising blood-pool agent in conditions where the BBB is compromised.
Immune therapy is establishing itself as a new method of treating cancer. The immune system is suppressed in many types of cancer, including GBM.130,131 USPIOs can be a promising tool to label immune cells and assess the efficacy of such types of therapies. It has been shown that amphotericin B (AmpB) can activate innate immunity, suppress GBM, and prolong mice's life span. 132 AmpB increases the total number of circulating monocytes and the number of proinflammatory macrophages in the tumor. 132 By labeling monocytes with USPIOs, drug response of AmpB (ie, upregulation of blood monocytes and infiltration of monocytes into the tumor) could possibly be detected even before there is any evidence of changes in tumor volume.
Iron oxide nanoparticles can also be used in DC-based vaccines to assess the efficacy of cancer immune therapy. 133 The success of DC vaccine therapy depends on the migration of vaccinated DCs to lymph nodes to activate T cells and elicit an antitumor response. Therefore, in vitro labeling of vaccinated DCs using USPIOs to track their location can be a very powerful tool to assess treatment response. USPIOs have been shown to leave DC viability largely unimpaired. 133 A dose-dependent lymph node signal drop has been shown to occur when using magnetically labeled DCs injected into the sites of inflammation, with histology confirming both iron and immune cells in the lymph nodes. 134 One group developed a magnetically labeled cancer vaccine, using a SPIO-labeled tumor mixed with Granulocyte macrophage colony stimulating factor (GM-CSF) secreting bystander cells. 6 This approach showed that signal decreases in lymph nodes three days postinjection, which coincided with the arrival of magnetically labeled DCs in the lymph nodes. These DCs were shown to induce the proliferation of T cells targeting factors expressed by the tumor cells.
Angiogenesis is critical to the development of tumors. RGD acts as a ligand to α v β3 integrin, a marker for angiogenesis. 97 RGD-conjugated MPIOs (2.8 μm diameter) were first examined in vitro in both static and flow chamber cultures with human umbilical vein endothelial cells. 97 The MPIOs had significantly greater specific binding to the activated cells than control cells. Subsequent in vivo work found that RGD-conjugated MPIOs enhanced colorectal- and melanoma-derived tumors. 97 Histology confirmed that MPIOs were colocalized with neovessels. This suggests that targeted MPIOs may serve as a useful tool for tracking tumor growth and potentially as a platform for delivering drugs to the regions of angiogenesis.
Vascular disease (arteriovenous malformations, cerebral aneurysms, and aortic aneurysms)
Iron oxide contrast agents have been used in vascular diseases, such as arteriovenous malformations (AVMs), cerebral aneurysms, and aortic aneurysms for various purposes. In the context of brain AVMs in humans, the USPIO agent ferumoxytol has been used as a blood-pool agent in combination with susceptibility-weighted MRI to help better delineate such vascular alterations in the forms of capillary telangiectasias and cavernomas. 135 With ferumoxytol sequences, 40 lesions were detected, while with pre- and postgadoteridol images, only 35 lesions were detected among the 19 patients in the study. The inclusion of ferumoxytol and susceptibility-weighted MRI enabled the visualization of tributary veins that were not apparent with pre- and postgadoteridol imaging with T1-weighted MRI. A different study used ferumoxytol-enhanced MRI to highlight macrophages in brain AVMs in four patients. As one of the patients in the study underwent surgical resection of their AVM after imaging, staining of tissue for macrophages was compared with MRI findings; these appeared to be present in the same regions in the vascular wall. 136 The results from this small study are encouraging, but more studies are needed to compare ferumoxytol-enhanced MRI with the presence of macrophages in brain AVMs.
Iron oxide contrast agents have also been used in the setting of unruptured abdominal aortic aneurysms (AAAs) and cerebral aneurysms to assess macrophage infiltration in the vessel wall. AAAs are associated with inflammatory activity; thus, imaging such inflammation using iron oxide contrast agents to label macrophages is a possibility. One study used USPIOs to determine the rate of growth of AAAs. Those with asymptomatic aortic aneurysms ranging in size from 4 cm to 6.6 cm were imaged at 3T using
Macrophages are also a significant component of cerebral aneurysms, lending them to being imaged with iron oxide contrast agents. In patients with unruptured cerebral aneurysms, MRI with ferumoxytol has been compared with tissue staining for macrophages (with CD68) and for the uptake of iron particles (with PB), with the finding being that ferumoxytol uptake seen with MRI is well correlated with the presence of macrophages in the aneurysm wall. 138 Furthermore, the optimal time between administration of ferumoxytol and subsequent imaging has also been compared, where more MRI signal changes were seen when there was a three-day delay in imaging postferumoxytol administration as compared to a one-day delay. 138 The same group conducted more research on the significance of early MRI changes with ferumoxytol administration (ie, 24 hours after administration)–-mainly, they wanted to know if this suggests that the aneurysm is unstable. For this study, they investigated 30 unruptured aneurysms, of which 7 showed early uptake of ferumoxytol. 139 Of those seven, four were clipped soon after, while three were not, and of note, all three ruptured within 6 months. It is also worth noting that macrophages were similar in unruptured aneurysms with early uptake of ferumoxytol and ruptured aneurysms, suggesting that early uptake of ferumoxytol may be indicative of pending aneurysm rupture. 139 As the sample size for this study was quite small, it would be interesting to see if future studies come to the same conclusion as this one did. Imaging of cerebral aneurysms, with iron oxide contrast agents, has been reviewed more in depth by Levitt et al. 140
Quantification with Iron Oxide Agents
Determination of iron oxide concentration in a region of interest is desirable for several reasons. The degree of cellular iron uptake can be used to probe cytotoxicity outcome. 141 If quantification can be done in the magnet, it can yield CBV; in nondividing or slowly dividing cells, it can yield cell counts and can quantify iron biodistribution. If iron oxides are functionalized as part of a drug payload 11 or for use in hyperthermia,27,142,143 quantification may aid understanding treatment efficacy.
Relaxivity is dependent on environmental factors that limit the areas in which relaxation rate measurements can be applied. One approach that has thus far only been applied in vitro has been the use of susceptibility imaging to obtain concentration. Susceptibility does not change much between encapsulated and free iron, making iron oxide concentration measurements feasible.
144
Relaxivity changes during encapsulation, with r1 and r2 reduced and
An approach that has seen more success in vivo is the use of electron paramagnetic resonance (EPR) spectroscopy. EPR spectroscopy has been used to assess in vitro iron oxide concentration where it was found to have a 91 ng Fe/mL lower limit of detection and 304 ng Fe/mL lower limit of quantification.
147
This was obtained for loading of the 35 nm USPIO Molday Ion Rhodamine B (MIRB) in RENA-luc (7 pg/cell) and B16F10-luc cells (10–13 pg/cell) at 9 GHz.
147
The same group subsequently injected mice with labeled renal
148
and breast cancer cells.
8
The renal cells lodged in the lungs and liver; EPR was, however, unable to track them in vivo beyond one day, owing to reduced sensitivity of their in vivo system.
148
With breast cancer, cell loading was sufficiently high to enable single-cell tracking using
Apparent diffusion coefficient (ADC) can be changed in the presence of iron. In an in vivo Macaque study, this change in ADC disappears when bipolar pulses are used, allowing the estimation of ξ Fe , a parameter estimating the ADC change because of iron. 149 This method showed sensitivity to regions of the brain known to endemically contain greater iron concentration and to USPIO injection. 149 Since iron is already present in the macaque brain and has been characterized by age and anatomy, 150 a linear mapping between ξ Fe and [Fe] could be made. 149 However, the fit of this map was rather poor: ξ Fe = 0 suggested a negative [Fe] of -371.5 μg/g of brain. The authors speculate that the relationship between the two parameters is not linear, and that further calibration will enable absolute quantification.
Quantification as a blood-pool contrast agent
A common use of contrast agents is in saturating the blood pool to perform angiography and venography75,76 and derive vascular information, including blood volume (BV),
151
vessel diameter,152,153 and water exchange.
154
Owing to iron oxide's blooming effect in
Visualizing the blood via contrast agent yields angiographies and venographies. Iron oxides act as a negative contrast agent for T2 and
One approach to overcome these problems was the use of ultrashort time to echo (UTE) imaging sequences. The short time to echo means that dephasing because of
When performing angiography and interrogating the vasculature, it is sometimes of use to examine other properties of the vasculature. T1, T2, and
Designing Studies using Iron Contrast Agents
A lab intent on employing iron nanoparticles will typically want to perform several steps of validation before attempting a labeling study. Typically, validation will begin with in vitro work. An illustrative paper of this process was published by Engberink et al, in which human leukocytes were loaded with SPIOs and USPIOs. 159 This paper incorporated four common validation steps as follows: i) T2 measurements of solutions at different concentrations of iron were made; ii) cell loading was studied histologically via the colocalization of nuclear fast red and PB staining; iii) MRI signal was examined via an nuclear magnetic resonance phantom consisting of cells in agar and was used to determine optimal culturing and loading parameters; and iv) cell viability was established via measurements of cellular migration, proliferation, and production of extracellular factors (IL-1 and IL-6 in this case). This validation could then be followed by a study using these labeled cells. Indeed, the authors of this article followed this work with an immune cell study ex vivo. 22
Limitations
Even coated nanoparticles have subtle immunological effects 34 and can affect cellular proliferation (negatively 58 or positively 37 ), and nanoparticles can be toxic to certain cells at high concentrations. 31 While cytotoxicity is typically dose dependent, low-dose labeling decreases MR I visibility. For this reason, developing high relaxivity nanoparticles and employing higher field MRIs is useful, so that less iron is required to obtain the same contrast. Exploiting ferrimagnetism, 7 non-spherical geometries, 49 nanocluster, 160 or even simply using MPIOs53,161,162 can meet these requirements. Avoiding the use of transfection agents and still obtaining good labeling are often possible 163 and may prove less toxic. While there are iron oxides that appear to be largely safe at imaging doses, 164 some adverse systemic effects have been reported in human trials. 165 The Food and Drug Administration now warns that ferumoxytol may pose a fatal allergic reaction risk. 166
One challenge with using iron oxides is that their relaxivity changes depending on the environment they find themselves situated in. This poses challenges to their quantification. 144 Quantification also often depends on assumptions of intra-vascularity15,156 or is sensitive to dilution.8,147,148 Cell labeling quality is often degraded as iron oxide becomes dilute by proliferation 8 or by lysosomal action, though MPIOs are more resilient to these effects.44,146,161
Typical imaging schemes with iron oxides use iron as a negative contrast agent. To track iron, two images, such as a precontrast and a postcontrast image, are often used.
167
Some positive contrasts (white marker techniques) do exist, but they deposit more energy and are more complicated.
167
T1 shortening may be employed, but is complicated by rapid
It is difficult to be certain about which cells nanoparticles find themselves in or whether they are in the cellular compartment at all. For example, when studying iron oxides situated in the brain, infiltrating macrophages may be credited with iron oxide presence,110,119 or BBB leakage may be to blame. 89 The presence of iron in a region does not guarantee that the cells they originally labeled are still alive. 60 While histology often shows that iron oxides are localized within immune cells, noninvasively determining whether these are microglia or invasive macrophages remains difficult.101,124
Conclusion
Iron nanoparticles are a versatile tool for cell tracking and targeting cells for imaging. They may be introduced into the body where they provide contrast enhancement associated with macrophages and monocytes. Iron particles enable imaging of the liver, lymph nodes, spleen, and sites of inflammation. They may be introduced to a population of cells ex vivo, which may be tracked upon transplantation into the body. The diversity of available coatings and sizes for iron nanoparticles grants tremendous flexibility for cell and tissue targeting via conjugation with histological agents, antibodies, and transfection agents. The use of iron-based contrast agents for both preclinical and patient studies is on the rise and will be certain to provide novel information in the future.
Author Contributions
Conceived and designed the experiments: MT. Analysed the data: MT, DJK. Wrote the first draft of the manuscript: DJK, MT, RY, NN. Contributed to writing of the manuscript: DJK, MT, RY, NN, JFD. Jointly developed the structure and arguments for the paper: DJK, MT, RY, NN, JFD. Made critical revisions and approved final version: DJK, MT, RY, NN, JFD. All authors reviewed and approved of the final manuscript.