Abstract
Streptococcus pyogenes (S. pyogenes) is the most important causative agent of tonsillopharyngitis. Beta-lactam antibiotics, particularly penicillin, are the drug of first choice and macrolides are recommended for patients who are allergic to penicillin. However, other antibiotics are also used for the treatment of streptococcal tonsillopharyngitis. In recent years, the increase in the incidence of respiratory tract pathogens that are resistant to current antibacterial agents highlights the need to monitor the evolution of the resistance of these pathogens to antibiotics. In this study, we assess the susceptibility of 98 isolates of S. pyogenes to 16 antibiotics. The pathogens were recovered from patients with acute tonsillopharyngitis in Dakar, the Senegalese capital city, who were recruited from May 2005 to August 2006. All strains were susceptible to penicillin with low Minimum Inhibitory Concentration (MIC = 0,016 mg/L). Amoxicillin had high activity (100%) showing its importance in treatment of streptococcal infections. Cephalosporins had MIC90 values ranging from 0.016 to 0.094 mg/L. Macrolides have shown high activity. All strains were resistant to tetracyclin. Other molecules such as teicoplanin, levofloxacin and chloramphenicol were also active and would represent alternatives to treatment of tonsillopharyngitis due to this pathogen. These results indicate that no significant resistance to antibiotics was found among patients with tonsillopharyngitis studied in Dakar. Limitations of this study were that the number of isolates tested was small and all isolates were collected from one hospital in Dakar. Hence, results may not be representative of the isolates found, in the wider community or other regions of Senegal. Further studies are needed in other parts of Dakar and other geographic regions of Senegal, in order to better clarify the antibiotic susceptibility profile of S. pyogenes isolates recovered from patients with tonsillopharyngitis.
Introduction
Acute tonsillopharyngitis is one of the most common infectious diseases particularly in children.
Among the bacteria which are responsible, Streptococcus pyogenes (group A streptococcus) is one of the most common pathogens. 1 Severe forms of this disease have been detected in various parts of the world.2–4 Although penicillin remains active on S. pyogenes, in recent years, the increase in the incidence of strains that are resistant to current antibacterial agents, highlights the need to assess the evolution of resistance of this pathogen to antibiotics.
As data on antimicrobial susceptibility of S. pyogenes to antibiotics are lacking in Senegal, we assessed the susceptibility of different strains of this pathogen isolated from patients with acute tonsillopharyngitis to a broad spectrum of antibiotics using standard susceptibility-testing method (Disk diffusion method) and Epsilometer-test (E-test) to determine MICs.
Material and Methods
Streptococcus pyogenes isolates
From May 2005 to August 2006, throat swabs collected from patients with acute tonsillopharyngitis in the departments of pediatrics and otorhinolaryngology of the university hospital of Aristide Le Dantec in Dakar, Senegal were sent to Biotechnology unit of the bacteriology laboratory of the same hospital. At the laboratory, samples were immediately cultured on trypticase -soy agar supplemented with sheep blood. After incubation for 24–48 hours at 37 °C in a carbondioxide (CO2) atmosphere, strains were identified using conventional procedures (thin smooth colonies, Gram-positive cocci grouped into chains, catalase-negative, growth inhibition around a disk containing 0.04 units of bacitracin) and using microCSB streptococci® galleria. Colonies surrounded by beta-hemolysis were selected for grouping using a streptococcal grouping kit (Slidex Strepto A®, BioRad).
Antibiotic susceptibility testing
Antibiotic susceptibility of group A beta-hemolytic streptococci were analysed with respect to 16 antibiotics belonging to 9 classes (β-lactams, macrolides, lincosamins, streptogramins ketolides, fluoroquinolones, glycopeptides, phenicols and cyclines) using standard disk diffusion method and the Minimum Inhibitory Concentrations(MICs) were determined for 10 antibiotics by E-test (AB Biodisk, Solna, Sweden).
Briefly, for each isolate, a bacterial suspension with final concentration of 105 CFU/ml was used to inoculate a Mueller-Hinton agar plate supplemented with 5% sheep blood for both standard disk diffusion method and E-test. After application of disks (diffusion method) or strips (E-test) containing selected antibiotics, plates were incubated at 37 °C in a CO2 atmosphere for 18–24 hours. The following organisms were used as controls: Staphylococcus aureus ATCC 29213 and Streptococcus pneumoniae ATCC 49612. MIC endpoints were read as the lowest concentration of antimicrobial that totally inhibited macroscopically visible growth of the inoculum. Percentage susceptibilities were calculated based on the Clinical and Laboratory Standards Institute (CLSI) break points. 5
Analysis of results
The WHONET software was used to analyze the results. 6
Results
Streptococcus pyogenes isolates
A total of 98 strains of S. pyogenes were isolated from 11 pediatric patients (less than 15 years of age) and 87 from adults (18–57 years of age) presenting with acute tonsillopharyngitis.
Antimicrobial susceptibility rates
All control strains gave MICs within acceptable values according to CLSI. 5
Susceptibility rates of strains are shown in Table 1.
Susceptibility rates of Streptococcus pyogenes (Disk diffusion) and MIC values (E-test).
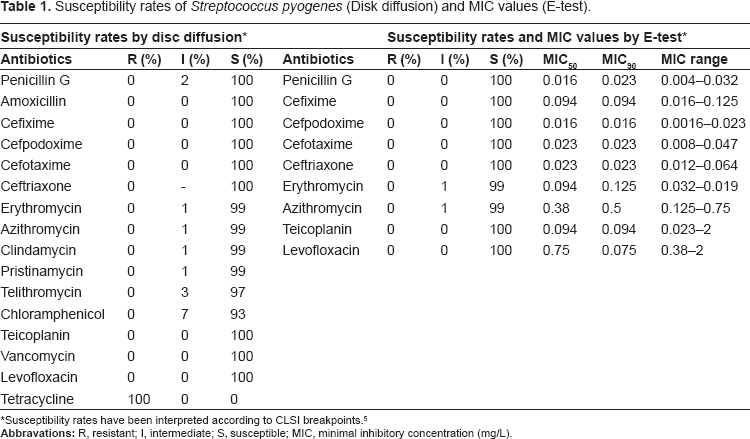
Susceptibility rates have been interpreted according to CLSI breakpoints. 5
Susceptibility to beta-lactams
Penicillin was highly active with MIC90 value of 0.023 mg/L. All strains were susceptible to amoxcillin, cefixime, cefotaxime, cefpodoxime and ceftriaxone. This result was confirmed by E-test with MIC90 ranging from 0.016 to 0.094 mg/L.
Susceptibility to MLSBK
Almost all strains were susceptible to erythromycin and azithromycin. Only one strain showed intermediate susceptibility to these two molecules. MIC90 values were 0.0125 mg/L and 0.5 mg/L respectively for erythromycin and azithromycin. As for macrolides, only one strain showed intermediate susceptibility to Clindamycin and pristinamycin. The susceptibility rate to telithromycin was of 97%.
Susceptibility to Chloramphenicol
By the disk diffusion method, 93% of the strains were susceptible to Chloramphenicol.
Susceptibility to others antibiotics
All strains were susceptible to vancomycin, teicoplanin, levofloxacin and resistant to tetracycline. Fluoroquinolones, phenicols and glycopeptides had low MIC90 values (Table 1).
Discussion
Susceptibility to β-lactam antibiotics
Antimicrobial resistance is an important problem in the management of patients with infectious diseases. Interestingly, S. pyogenes remains susceptible to penicillin in many countries of the world. The reason for this unique lack of development of resistance to penicillin is unknown. 4 On the other hand, numerous reports have demonstrated a significant prevalence of erythromycin- resistant S. pyogenes around the world during the two past decades.7–9
In this study, none of the 98 isolates were resistant to penicillin. This finding is concordant with other studies from around the world.10–12These results confirm once again that penicillin is a reference molecule for treatment of group A streptococcal infections. However, treatment failure observed in more than 20% of patients at the University of Washington, 13 suggested a possible development of resistance to penicillin.
Amoxicillin has been active on all strains (100% of susceptibility) with inhibition diameters ranging from 26–36 mm. All strains were susceptible to cefixime, cefotame, cefpodoxime and ceftriaxone. Clinical and microbiological responses to cephalosporins were equal (or even superior) to those obtained with penicillin. However, cephalosporins have a broader spectrum and are more expensive than penicillin and are, therefore, not recommended as the drug of first choice. They can be used for patients allergic to penicillin.
Susceptibility to MLSBK
Macrolides are an alternative and suitable treatment for patients allergic to penicillin. Studies conducted in many countries have shown a wide heterogeneity of resistance, with high levels of macrolide resistance in Poland (42%), Hong Kong (28%), Italy (25%), and France (14,5%), and no macrolide resistance in Indonesia, Austria, Belgium, the Netherlands or the UK.14,15
In this study, there was no resistance of S. pyogenes to erythromycin. Only one strain showed an intermediate susceptibility. These results suggest that strains of S. pyogenes which are resistant to erythromycin may not yet be circulating in Dakar. But the limitations of our study are that the number of isolates tested was small and that all isolates were collected from one hospital in Dakar. As for erythromycin, high activity of azithromycin (99% of susceptibility rate) had been detected in this study.
Susceptibility to clindamycin was comparable with that of erythromycin and azithromycin with 99% of isolates being susceptible to them and 1% of strains showing intermediate susceptibility. No resistance was noted in this study unlike the one by Soumah who in 2002 reported, 2.7% resistance to this molécule in Dakar (Soumah unpublished data). Tétithromycin showed 97% activity. The same rate was obtained in Dakar in 2002 (Soumah unpublished data). The lack of resistance to erythromycin could justify this result. The rate of susceptibility is comparable to those observed in central and eastern European countries which was 98.5%–100%. 16 Such results justifies the use of the telithromycin in pharyngitis due to group A streptococci and Balfour et al. have shown that 5 days of treatment with telithromycin is as effective as 10 days of treatment with penicillin V. 17
Suceptibility to others antibiotics
In this study, Levofloxacin presented high activity with a susceptibility rate of 100%. This is significantly higher than that obtained by Soumah in Dakar, in 2002, which was of 78.37% (Soumah, unpublish data). Rates of susceptibility comparable to those found in this study have been reported also in the U.S.A with less than 1% resistance. 18 In contrast, resistance to levofloxacin was observed in Spain. 19 However, levofloxacin is an alternative to be considered in case of allergy to penicillin and resistance to macrolides for treatment of group A streptococcal infections.
All isolates tested is this study were completely resistance to tetracycline (100%), thus confirming the results obtained in Dakar in 2002 and 2004 (Soumah unpublished data, Hounkponou, unpublished data) and in other countries such as Iran with 23%–42% resistance to this molecule. 20 Vancomycin and teicoplanin inhibited all isolates with a low MIC90 of less than 1 mg/L for tecoplanin. These results, which confirmed the ones obtained in 2004 (Hounkponou, unpublished data) are also similar the results observed in Brazil, 21 and in Spain. 22 Used for in-patients, teicoplanin is a drug of last choice reserved for severe respiratory infections resistant to penicillin.
Conclusion
Acute respiratory tract infections, despite the antimicrobial therapy, remain frequent and a real health problem. Considered for long as a disease of cold countries, infection with S. pyogenes is currently among the main causes of mortality in developing countries. The diversity and severity of its clinical spectrum should encourage clinicians and microbiologists to pay more attention. For this reason, it is important to always identify and explore susceptibility of this pathogen to antibiotics in order to contribute to the improvement of care.
In this study, susceptibility of 98 strains of S. pyogenes to various antibiotics belonging to several classes (β-lactam antibiotics, macrolides, lincosamines fluoroquinolones, glycopeptides, streptogramins, phenicols and tetracylcines) were determined by two techniques: standard disk diffusion method and E-test. The results obtained have led to several conclusions: all strains of S. pyogenes were sensitive to penicillin; amoxicillin has proved to be the most effective antibiotic. With MIC90 < 0.1 mg/L, no resistance to cephalosporins has been detected. Azithromycin and Erythromycin were very efficient with 99% susceptibility. Clindamycin and pristinamycin have shown a high degree of efficacy on β-hemolytic streptococcus. With 99% susceptibility rate, these two molecules could be used as a second choice of antibiotic. The phenicols (chloramphenicol), glycopeptides (vancomycin and teicoplanin) and fluoroquinolones (levofloxacin) have confirmed their effectiveness with 93%–100% of activity. The resistance to tetracycline, demonstrated throughout this study, is probably due to uncontrolled use of this molecule because of its affordable cost through the Bamako Initiative.
But limitations of our study are that all the isolates were collected from one hospital in Dakar. Hence, the results may not be representative of the isolates found in the wider community or other regions of Senegal. Further studies from other parts of Dakar and other geographic regions of Senegal are needed, in order to better clarify the antibiotic susceptibility profile of S. pyogenes.
Publish with Libertas Academica and every scientist working in your field can read your article
“I would like to say that this is the most author-friendly editing process I have experienced in over 150 publications. Thank you most sincerely.”
“The communication between your staff and me has been terrific. Whenever progress is made with the manuscript, I receive notice. Quite honestly, I've never had such complete communication with a journal.”
“LA is different, and hopefully represents a kind of scientific publication machinery that removes the hurdles from free flow of scientific thought.”
Available to your entire community free of charge
Fairly and quickly peer reviewed
Yours! You retain copyright
Footnotes
The authors report no conflicts of interest.
