Abstract
Background
There is a direct correlation between glycemic load and the risk of developing many malignant neoplasms.
Aims
The aim of this study was to determine the plasma glucose levels in women with cervical cancer.
Methods
The study included 177 women with anatomopathologically diagnosed uterine cervical cancer (stages 0–IV) treated between 1980 and 2008 at the Gynecology and Obstetrics outpatient service of the UFTM, Brazil. The plasma glucose levels of all patients were assayed at the time of diagnosis and correlated with tumor staging.
Results
We statistically compared the plasma glucose levels of group 1 (cervical intraepithelial neoplasia 2–3), group 2 (stage I–II), group 3 (stage III–IV), and group 4 (control group: leiomyomas). Patient groups with poor prognosis (groups 2 and 3) showed significantly higher plasma glucose levels (P < 0.05) than those with less aggressive lesions (group 1). Plasma glucose levels were significantly higher in groups 2 and 3 than in group 4 (P < 0.05). The comparison of number of patients with plasma glucose level >90 mg/dl showed CIN versus I/II: P = 0.0753; OR = 2.018; (95% CI: 0.9236 to 4.410) and CIN versus III/IV: P = 0.0975; OR = 2.400; (95% CI: 0.8335 to 6.911).
Conclusion
We observed an association between high plasma glucose levels and cervical cancer cases with poor prognoses. Plasma glucose tests should be routinely used as additional prognostic parameters in patients with cervical neoplasias.
Introduction
Cervical cancer is a public health problem in developing countries, characterized by high prevalence and mortality rates in premenopausal women of low socioeconomic status. 1 Factors related to glucose metabolism may play an important role in cancer development. The glycemic index has been investigated as a potential etiological and prognostic factor for several types of malignancy. 2
The literature shows a direct correlation between glycemic load/glycemic index and the risk of developing colorectal,2–5 breast,6,7 upper aerodigestive tract, 8 gastric, 9 ovarian,10–12 and endometrial cancer.2,13,14 However, to our knowledge, no published study has investigated plasma glucose level as a cofactor in the progression of noninvasive cervical lesions to invasive carcinomas, or the role of plasma glucose evaluation in the prognosis of this neoplasia. The aim of this study was to examine the relationship between plasma glucose levels and cervical cancer staging, and the applicability of this measure as a prognostic factor.
Patients and Methods
Patients and Controls
This retrospective study was carried out at the Oncological Research Institute (IPON), Discipline of Gynecology and Obstetrics, of the Federal University of Triângulo Mineiro (UFTM). Data were collected from the medical records of 177 women with anatomopathologically diagnosed uterine cervical neoplasia (stages 0–IV) attending the Gynecology and Obstetrics outpatient service of the UFTM between 1980 and 2008. Patients with HIV coinfection, those who had used corticosteroids during the period of the disease, and those diagnosed with diabetes mellitus were excluded from the study. This research was approved by the Research Ethics Committee of the UFTM.
The patients were divided into three groups according to the staging system of the International Federation of Gynecology and Obstetrics (FIGO): group 1 (n = 104): cervical intraepithelial neoplasia (CIN) 2–3 (stage 0); group 2 (n = 48): invasive cervical carcinoma stages I–II; group 3 (n = 25): invasive cervical carcinoma stages III–IV. A fourth group (n = 100) consisted of randomly chosen patients diagnosed with uterine leiomyoma that had been confirmed by postoperative histopathological examination.
Plasma glucose levels
Blood samples were collected from patients during routine preoperative testing for the measurement of plasma glucose levels (mg/dl). The patients fasted for 12 hours before sample collection. Plasma glucose levels were correlated with neoplasm staging in groups 1–3, and these three groups were then compared with group 4.
Statistical analysis and ethical approval
Data were analyzed using GraphPad Instat software. Values were expressed as means ± standard deviations (SD). The unpaired t test was used to compare pairs of groups, with P values of less than 0.05 considered to indicate statistical significance. Plasma glucose cut off level of 90 mg/dl to calculate the Odds Ratio (OR-95% confidence interval-CI). The research was approved by Ethical Committee of UFTM.
Results
Table 1 shows the characteristics of the study patients.
Characteristics of the patients.
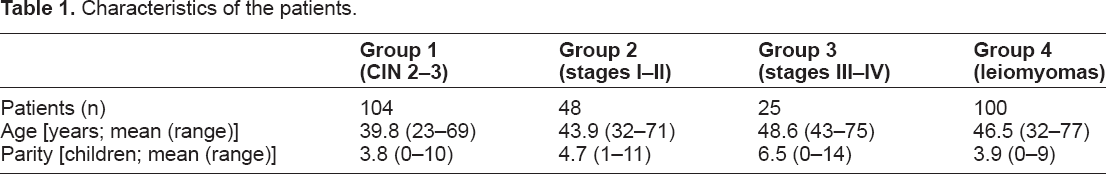
Table 2 presents the mean plasma glucose levels of patients in all groups. Plasma glucose levels (mg/dl) in groups 1–4 were 94.7 ± 14.1, 104.3 ± 31.4, 112.6 ± 56.7, and 94.5 ± 13.4 mg/dl, respectively. We observed that patient groups with poor prognoses (groups 2 and 3) showed significantly higher plasma glucose levels (group 2: P = 0.011, group 3: P = 0.0044) than those with less aggressive lesions (group 1). We also compared patients with cervical neoplasia (groups 1–3) to patients with leiomyomas (group 4). Plasma glucose levels were significantly higher in groups 2 and 3 (P = 0.009, P = 0.0041, respectively) than in the leiomyoma group.
Age and plasma glucose levels in patients with cervical intraepithelial neoplasia (CIN; group 1), uterine cervical cancer (groups 2 and 3), and leiomyomas (group 4).

The OR values are shown in Table 2. There is a tendency to significant difference statistic for comparison of blood glucose above 90 mg/dl in patients with invasive staging in relation to the group with CIN.
Discussion
Diets with high glycemic loads have been directly associated with the risk of diverse chronic conditions, such as diabetes, 15 coronary heart disease, 16 and cancer. 2 Hyperinsulinemia may be implicated in the mechanism by which high glycemic load leads to these diseases. 10
Our study aimed to evaluate glucose levels in patients with cervical cancer, since this parameter is simpler than the dosage load and glycemic index, parameters that are already linked to several types of cancer in the literature. Data of the 177 patients were collected from 1980–2008. During this long period, there were no significant changes in the methods of plasma collection and glucose tests in the clinical laboratory of our university over time. The collection has been carried out with 12 hours of fasting for many years. The main changes that occurred were the cutoff levels for the diagnosis of glucose intolerance or diabetes, but that does not interfere in our study, because it compared glucose levels in each group, no cut off. In the literature, a meta-analysis of the role of glycemic index and load in cancer risk suggested a direct association for colorectal and endometrial cancer and an inconsistent relationship with several other types of cancer. Obesity was a major determinant of insulin resistance and hyperinsulinemia, and physical activity influenced glucose tolerance and insulin sensitivity. 2
Uterine cervical cancer is related to human papillomavirus (HPV), 17 and HPV infection is considered a causal factor in the development of CIN and invasive neoplasia. 18 Persistent infection of the genital tract with oncogenic subtypes of HPV is the leading cause of squamous intraepithelial lesions and invasive carcinoma.19,20 The presence of HPV does not establish clinical disease presence, and rarely persists or progresses to high-grade disease. Progression to invasion depends on additional cofactors, such as nicotine, exogenous estrogen, p53 polymorphism, immune status, or the presence of other infectious agents. 21 Thus, the discovery of other factors in carcinogenesis of cervical cancer could lead to new targets of study for the treatment and prognosis.
The consumption of a diet rich in glucose may lead to chronic hyperinsulinemia and insulin resistance,10,22 which have been shown to reduce concentrations of insulin-like growth factor binding protein (IGFBP) and consequently increase insulin-like growth factor-1 (IGF-1) levels. Some studies have shown that increased IGF-1 activity inhibits apoptosis and stimulates cell proliferation; these factors may lead to the development of cancer. High IGF-1 activity also increases steroid synthesis and inhibits hormone-binding globulin synthesis, contributing to the development of ovarian and endometrial cancer.23,24
In colorectal cancer, insulin receptors activate mitogenic signaling pathways, increasing the risk of cancer in patients with elevated insulin levels (as occurs in insulin resistance and non-insulin-dependent diabetes). 25 Insulin is inversely associated with IGFBP-1.26,27 Several studies have associated indicators of insulin resistance, including serum levels of insulin, C-peptide, glycated hemoglobin, and glucose, with colorectal neoplasia.28–30
Obesity and insulin resistance are the results of compromised insulin signaling in liver, muscle, and adipose tissue, likely due to elevated levels of free fatty acids or cytokines from adipose tissue (eg, tumor necrosis factor-α) that antagonize phosphorylation events at the insulin receptor. 31 The pancreas compensates by up-regulating insulin synthesis, and tissues that express insulin receptors (eg, colon tissue) may be chronically exposed to increased levels of insulin, free fatty acids, and glucose, with subsequent mitogenic and tumor-promoting effects. 32 Since high blood glucose levels may be a predisposing factor for the development of insulin resistance or diabetes mellitus, our findings are consistent with the literature, and a positive association may exist between this parameter and cervical cancer. Besides, we have added group 4 thinking about the interference of age as a factor in the increase of plasma glucose and increased incidence of cancer. Even with a mean age similar to groups 2 and 3, and leiomyoma being a benign disease, we found statistical significance when compared glucose levels with these patients of groups 2 and 3. This finding may suggest a stronger relation with the progression of the disease than with the increasing age of the patients.
Genetic alterations may be associated with insulin resistance and the development of cancer. Preliminary evidence has been shown for the interaction between genetic variation in insulin receptors and body mass index in the risk for advanced left-sided colorectal adenoma. 33
Women with diabetes have been shown to be at higher risk for breast cancer. 34 Their high-glycemic-load diets have reduced the levels of adiponectin, an adipocyte-produced insulin sensitizer 35 that is inversely associated with obesity. Decreased concentrations of adiponectin have been related to an increase in postmenopausal breast cancer risk, independent of IGF-I and IGFBP-3 concentrations.36,37 Lajous et al showed an increase in the risk of estrogen-receptor-negative breast cancer with increasing carbohydrate and dietary glycemic load intakes. 38 Sieri et al found a direct association between glycemic load and breast cancer risk in premenopausal women who reported low levels of physical activity. 39 In contrast, Mulholand et al showed that glycemic load and index were not relevant etiological factors for breast cancer. 40 Diets with high glycemic loads have been associated with an increased risk of endometrial cancer, more pronounced in obese women, but additional research is required to clarify the relationship with ovarian cancer risk. 12
Increased plasma glucose levels have recently been investigated as negative prognostic factors in patients with neoplasms. Our study evaluated plasma glucose levels in patients with various stages of cervical neoplasia. Patients with uterine cervical cancer stages I/II and III/IV had significantly higher plasma glucose levels than those with CIN or leiomyomas. Although some questions arising as does the glucose level decreases when they receive effective treatment? The glucose level goes up when they don't have any treatment and the cancer progresses? Was body mass index measured? And were prediabetes patients excluded? A study limitation is the inability to examine other demographic data, since the study analyzes retrospective data on a large time interval. Therefore, plasma glucose levels were divided into a cut-off level of 90 mg/dl for calculating the odds ratio, showing an increasing trend in glucose levels with the development of cervical lesion. Thus, further prospective studies with a larger number of patients could enhance the relationship of glucose levels with prognosis of cervical cancer.
In conclusion, we have thus demonstrated an association between invasive cervical cancer and higher plasma glucose levels. This blood test is a component of routine examination that should be used as an additional prognostic parameter in patients with cervical neoplasia. Further studies are needed to elucidate the value of plasma glucose levels in the evaluation of the progression and prognosis of uterine cervical cancer.
Disclosure
This manuscript has been read and approved by all authors. This paper is unique and is not under consideration by any other publication and has not been published elsewhere. The authors and peer reviewers of this paper report no conflicts of interest. The authors confirm that they have permission to reproduce any copyrighted material.
Footnotes
Acknowledgments
The authors wish to thank the Conselho Nacional de Desenvolvimento Científco e Tecnológico (CNPq) and the Fundação de Amparo à Pesquisa do Estado de Minas Gerais (FAPEMIG) for providing funding in support of this research.
