Abstract
Background
Valvular heart diseases and mainly rheumatic heart diseases complicate about 1% of pregnancies. During pregnancy physiological hemodynamic changes of the circulation are the main cause of mitral stenosis (MS) decompensation. Prior to introduction of percutaneous mitral balloon commissuroplasty (PTMC), surgical comissurotomy was the preferred method of treatment in patients with refractory symptoms. PTMC is an established non-surgical treatment of rheumatic mitral stenosis. The study aimed to assess the safety and efficacy of PTMC in pregnant women with severs mitral stenosis.
Material and Method
Thirty three consecutive patients undergoing PTMC during pregnancy enrolled in this prospective study. Mitral valve area (MVA), transmitral valve gradient (MVG), and severity of mitral regurgitation (MR) were assessed before and 24 hour after the procedure by transthoracic and transesophageal echocardiography. Mitral valve morphology was evaluated before the procedure using Wilkin's criteria. Patient followed for one month and neonates monitored for weight and height and adverse effect of radiation.
Result
Mitral valve area increased from 0.83 ± 0.13 cm2 to 1.38 ± 0.29 cm2 (P = 0.007). Mean gradient of mitral valve decreased from 15.5 ± 7.4 mmHg to 2.3 ± 2.3 mmHg (P = <0.001). Pulmonary artery pressure decreased from 65.24 ± 17.9 to 50.45 ± 15.33 (P = 0.012). No maternal death, abortion, intrauterine growth restriction was observed and only one stillbirth occurred.
Conclusion
PTMC in pregnant women has favorable outcome and no harmful effect on children noted.
Introduction
Valvular heart diseases complicate 0.5 to 1.5 percent of all pregnancies. 1 Mitral stenosis is the most common form with increased pregnancy and delivery complications for both mother and neonate. 2 During pregnancy physiological hemodynamic changes of the circulation are the main cause of mitral stenosis decompensation. 3 The symptoms are poorly tolerated especially beyond second trimester and in other cases may lead to frank heart failure.4,5 Most pregnant women with mitral stenosis can be adequately treated with medical therapy and sometimes an invasive procedure is mandatory.6–9 Before the introduction of percutaneous transluminal mitral comissurotomy (PTMC) surgical comissurotomy was the sole answer to pregnant women with refractory symptoms. The high mortality rate (1.8% to 33%) of surgery and favorable outcome of PTMC in relieving symptoms plus lower risk of fetal death made PTMC more popular.10–15 Prospective studies on PTMC and its effect on pregnancy outcome and neonate are needed. In this study we aimed to investigate the clinical outcome of pregnant women undergoing PTMC and to assess the neonate condition after one month.
Material and Methods
A consecutive series of thirty three pregnant women undergoing PTMC in Rajaei Heart Center from March 2004 to March 2009 enrolled in this prospective descriptive study. The study was approved by ethical committee of Rajaei Cardiovascular Medical and Research Center.
Patients with severe mitral stenosis and following criteria were scheduled for invasive intervention: Progressive symptoms during first trimester in spite of adequate medical therapy, severe hemoptysis, and history of acute pulmonary edema during pregnancy.
Excluding criteria were severe mitral regurgitation and left atrial thrombus. PTMC was performed using Inoue balloon. Balloon diameters were chosen according to the patient's body surface. Lead shields were used to protect the abdomen during the procedure limiting fetal radiation exposure. Fluoroscopy time was measured during the procedure. Heparin (80 IU/kg, intravenously) was administered twice during the procedure. Mitral valve area, transmitral valve gradient and severity of mitral regurgitation were measured before and 24 hours after the procedure by means of two-dimensional and transesophageal echocardiography to evaluate the efficacy of the procedure. Transthoracic echocardiography was performed with a General Electric Vivid 3 machine with a 2.5-MHz probe, and images obtained in parasternal long and short axis and apical two- and four-chamber views. Mitral valve area, mean transmitral gradient, and severity of mitral regurgitation were assessed before the procedure, 24 hr after it, and during long-term follow-up. Mitral valve morphology was also evaluated before the procedure using criteria by Wilkins et al. 16 Mitral valve velocities were assessed with continuous-wave Doppler and mitral valve area was estimated from the Doppler pressure half-time method. 17 Mitral regurgitation was graded as mild, moderate, or severe according to jet length and area by two independent observers. Clinical follow-up after hospital discharge was accomplished by medical visits one month after discharge and was continued to the next year at the three months intervals. Finally patients were scheduled to be visited every 6 months for life time. Moreover, all babies were examined after delivery for any malformation and their development was assessed after one month. Continuous variables are expressed in mean ± SD. Comparison between the groups was accomplished by Student's two-tailed test. A P value of 0.05 was considered of statistical significance.
Results
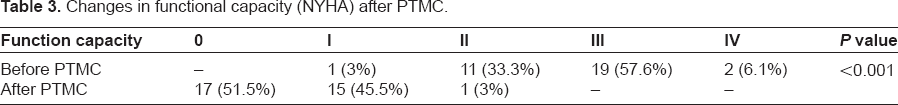
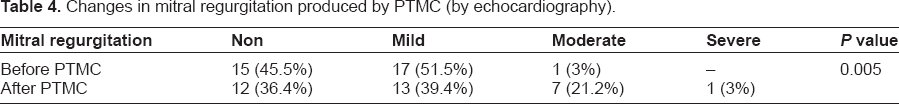
Demographic data are summarized in Table 1. Mean maternal age was 31.55 ± 6.3 years and mean gestational age was 21.85 ± 5.8 weeks. PTMC was performed successfully in all patients. After the procedure, mean MVA increased from 0.83 ± 0.13 cm2 to 1.38 ± 0.29 cm2 (P-value <0.001). Mean MVG significantly decreased from 15.5 ± 7.4 mmHg to 2.3 ± 2.3 mmHg (P-value <0.001). Also a significant decrease in pulmonary artery pressure was detected from 65 ± 18 mmHg to 50 ± 15 mmHg (P = 0.012). Mean left atrial pressure decreased significantly from 28.3 ± 7.2 to 15 ± 5.45. No significant change occurred in left ventricular ejection fraction and left ventricular end diastolic volume before and after procedure (Table 2). Symptoms of heart failure improved in all patients, and none of them experienced NYHA class III or IV (Table 3). Mitral regurgitation in six patients changed from mild to moderate and in one case to severe after procedure (Table 4). No maternal death, abortion, or intrauterine growth retardation was reported. There was one case with stillbirth and four neonates with respiratory distress. Infants assessed after one month by pediatrics and all had normal growth and development.
Baseline characteristics of study population.

Clinical data of patients.

Changes in functional capacity (NYHA) after PTMC.

Changes in mitral regurgitation produced by PTMC (by echocardiography).
Discussion
Pregnancy is characterized by a hyper dynamic state with significant change of hemodynamic especially between the 24th and 26th week of gestation and can explain decompensation in pregnant women with critical mitral stenosis.1,3 However, most patients respond well to adequate medical therapy. In some cases, maximal clinical therapy is not enough and an invasive intervention is required. Surgical mitral commissurotomy was performed during pregnancy with precautions mainly due to the high mortality rates of mother and neonates.15–17 Percutaneous mitral valvuloplasty was first performed in 1984. PTMC proved a safe procedure with outstanding results. However, studies with proper follow-up have not yet been fully described. The present study shows an excellent outcome for the patients after PTMC. After the successful procedure, all of the patients were in FC I or II and none of them required an additional surgical procedure until the end of pregnancy. In addition, there were no deaths related to the procedure. Echocardiographic examinations also showed favorable results, with a significant increase in mitral valve area and decrease in transmitral gradient shortly after the procedure. Only one case of severe mitral regurgitation was observed.
The excellent results observed after PTMC in this study can be attributed to the young age of the group and suitable mitral valve morphology. These parameters are both important predictors of short and long term results.16,18
There were neither maternal nor fetal deaths directly related to the procedure. No fetal abnormalities were found during examination and no clinical abnormalities could be associated with the use of radiation. Concerning the radiation exposure, the maximum safe radiation dose for the mother and the child has been established as 5 rads. Similar fluoroscopy time and the same protection used in other series, reported the total amount of received radiation to be approximately 0.5 rads, therefore far below the established limit.
In summary, due to the favorable results observed, percutaneous mitral valvuloplasty can be considered the procedure of choice to treat pregnant women with mitral stenosis unresponsive to adequate medical therapy.
Conclusion
The present study shows an excellent outcome for the patients after PTMC with no clinical abnormalities associated to the use of radiation in neonates.
Disclosures
Author(s) have provided signed confirmations to the publisher of their compliance with all applicable legal and ethical obligations in respect to declaration of conflicts of interest, funding, authorship and contributorship, and compliance with ethical requirements in respect to treatment of human and animal test subjects. If this article contains identifiable human subject(s) author(s) were required to supply signed patient consent prior to publication. Author(s) have confirmed that the published article is unique and not under consideration nor published by any other publication and that they have consent to reproduce any copyrighted material. The peer reviewers declared no conflicts of interest.
