Abstract
Metastatic lesions in the liver derived from colorectal cancer rarely invade the portal vein macroscopically. Portal vein tumor thrombus is commonly associated with hepatocellular carcinoma. Colorectal liver metastases are usually accompanied by microscopic tumor invasion into the intrahepatic portal vein, and the incidence of macroscopic tumor thrombus in the trunk of the portal vein is rare. Here, we provide unique appearance of metastatic colorectal cancer. To the best of our knowledge, macroscopically, the right portal vein filled with the tumor thrombus without any tumor in liver parenchyma has been quite rare.
Introduction
Tumor thrombus in the portal vein is one of the characteristic growth patterns of hepatocellular carcinoma. 1 Portal vein thrombosis has recently been detected by dynamic computed tomography (CT) in patients with liver cirrhosis, pancreatitis, inflammatory bowel disease, thrombocytemia, and in patients after liver transplantation, splenectomy.2–5 A recent study of resected specimens has shown that microscopic tumor invasion into the intrahepatic portal vein is common with metastatic liver tumor as well. 6 However, macroscopic tumor thrombus in the portal branch is rare and little is known about the incidence, clinical characteristics, or outcome of surgical treatment for patients with such tumor thrombi. 7 Here, we present a case of colorectal liver metastasis with massive portal vein tumor thrombus that required major hepatectomy.
Case Report
A 77-year-old Japanese man was referred to us because of an uncommon portal vein thrombus on an abdominal computed tomography (CT) scan. He had undergone a sigmoidectomy for T4N0 sigmoid colon carcinoma. He had not received any chemotherapy after surgery. Twenty months after primary surgery, a CT scan demonstrated obstruction of the portal vein in the upper posterior section of the liver, but no tumor was evident in the liver parenchyma (Figure 1). The serum carcinoembryonic antigen level was slightly elevated at 7.7 ng/mL (normal range ≤5.0 ng/mL). A positron emission tomography scan showed positive fluorodeoxyglucose uptake in the right lobe of the liver. A metastatic tumor in the portal vein was diagnosed, and a right hepatectomy was performed.
Enhanced computed tomography shows low-density area along the right portal branch, and no definite metastatic mass in the liver parenchyma.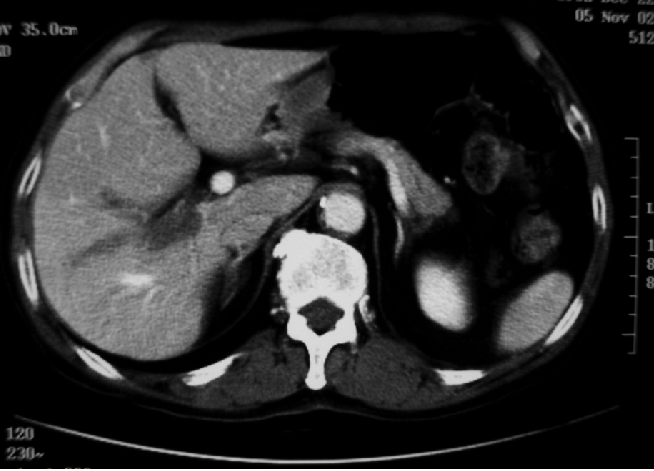
Macroscopic examination of the cut surface of the resected liver specimen showed that the tumor filled the portal vein in a branch-like manner (Figure 2). No definite tumor was recognized at sites other than the portal vein. Microscopic examination revealed that the tumor thrombi in branches of the portal vein were moderately differentiated adenocarcinoma and restricted to the portal vein area (Figure 3a, 3b).
Macroscopically, the right portal vein is filled with the tumor thrombus. No definite tumor was recognized at sites other than the portal vein.
Histologically, the tumor thrombus a) is diagnosed as metastatic tumor from primary resected sigmoid colon cancer; b) well differentiated adenocarcinoma.
Metastasis to the right adrenal gland was diagnosed at month 27 after hepatectomy. Then, after systemic chemotherapy based of CPT-1 and S-1, his adrenal metastasis was resected. At the time of this writing (14 months after adrenal resection), he remains free of recurrence with receiving chemotherapy same as before removal of adrenal metastasis.
Discussion
We present a rare case of colorectal liver metastasis with massive portal vein tumor thrombus treated by major hepatectomy. Portal vein tumor thrombus (PVTT) is commonly associated with hepatocellular carcinoma (HCC), because HCC is a hypervascular tumor with shunt formation from the hepatic artery to the portal vein. Microscopic invasion of the portal vein, hepatic vein, and intrahepatic biliary duct are reportedly present at rates of 22.5%, 7.5%, and 40.0%, respectively. 6 Colorectal liver metastases are usually accompanied by microscopic tumor invasion into the intrahepatic portal vein, and the incidence of macroscopic tumor thrombus in the trunk of the portal vein is estimated to be 2.8%. 8 Most reported cases of PVTT from colorectal cancer had concomitant metastatic nodules in the liver parenchyma, and the PVTT was continuous with the liver nodules, similar to PVTT in HCC.8–10 Characteristics of portal vein involvement by HCC have been well described. 11 In general, tumor cells from the primary lesion reach the hepatic sinusoids via the portal system and form metastatic nodules in the liver parenchyma when tumor cells are able to survive and multiply. PVTTs have been attributed to these metastatic nodules. In our patient, however, the resected specimen showed that the right portal vein was almost completely filled with tumor thrombus, with no metastatic nodules in the liver parenchyma. The present case may thus represent a very rare type of PVTT from colorectal cancer and suggests another unknown mechanism underlying the formation of PVTTs from colorectal cancer.
Even the recent advance in chemotherapy and other treatment modalities, surgical resection is still gold standard for treatment of liver metastasis from colorectal cancer.12,13 Despite in patients with a macroscopic tumor thrombus in the main branch and/or trunk of the portal vein originating from colorectal cancer, a better prognosis may be expected if the tumor can be completely resected en bloc.14,15 Oppositely, the presence of PVTTs indicates a poor prognosis for patient with HCC, because of portal hypertension, rupture of esophageal varices, and liver failure. 11 In general, liver resection for liver metastasis is considered adequate as a 1 cm margin around the tumor is obtained. However, in the presence of portal vein thrombus, a non-anatomic liver resection around the tumor would not be adequate, as the tumor is likely to spread along the portal vein branches. Thus, an anatomic major resection of the liver is considered necessary for curative treatment in this situation as our case. 8 In our case, although the patient suffered recurrence in the adrenal gland, recurrences have not been detected in rest of the liver. The present patient have received chemotherapy after removal of metastatic tumors and still been alive without recurrence. From this point, probably due to long-term survival has been obtained that continued chemotherapy after surgery. Thus, in conclusion, the combination of en bloc removal of the lesion and effective chemotherapy is considered essential for curative treatment for like this case.
