Abstract
Papillary serous cystadenocarcinoma of the ovary is a common tumor but occurrence of ovarian type papillary serous cystadenocarcinoma in the testis is very rare. Herein we report such a case in a 49-year-old man presenting with testicular swelling. In this tumor, mesothelioma of tunica vaginalis should be excluded by immunohistochemistry. The best treatment is radial orchiectomy and it is very resistant to chemoradiation. Our case was well after orchiectomy and now after a year he is doing well and completely symptom free.
Introduction
Ovarian type surface epithelial carcinomas of testis and paratestis are very rare. 1
Histologic classifications of ovarian type surface epithelial tumors of testis are composed of borderline microinvasive serous tumor and serous carcinoma, intra and paratesticular mucinous tumor with different grades, clear cell and endometrioid adenocarcinoma and transitional cell tumors. 2 The most frequent histologic type is serous. 1
To the best of our knowledge, less than 50 cases of testicular and paratesticular serous type have been reported in the English literature so far. 3
Herein we report our experience with a 49-year-old male with testicular serous cystadenocarcinoma.
Case Report
A 49-year-old man presented with chief complaint of left testicular swelling for several months. His past medical history was unremarkable. Laboratory investigation including tumor markers such as CEA, PSA and CA 125 were normal. On palpation, there was left scrotal fullness, and right testis was normal. Ultrasonography showed hyperdense lobulated mass in left hemiscrotum measuring 9 cm in diameter. There was also hydrocele and small-sized left testis but right testis was unremarkable (Figure 1). With the primary diagnosis of testicular tumor, the patient was scheduled for orchiectomy. Gross findings: After orchiectomy the received specimen in the pathology department showed a large testicular mass measuring 9X7X6 cm with an intact capsule and well-defined border with no necrosis or hemorrhage (Figure 2). Microscopic findings: Microscopic examination of the tumor sections showed a testicular tumor with papillary projections lined by atypical cuboidal cells with basophilic cytoplasm. There were many psammoma bodies (Figure 3). All the histologic findings were typically identical to ovarian papillary serous cystadenocarcinoma, however immunohistochemistry was performed for confirmation and to exclude mesothelioma of tunica vaginalis. The tumor cells were reactive for cytokeratin (CK), cytokeratin 7 (CK7), and epithelial membrane antigen (EMA) but nonreactive with CK20, inhibin, calretinin and placental alkaline phosphatase (PLAP).
Ultrasonography of the intratesticular scrotal mass.
Gross picture of the intratesticular mass.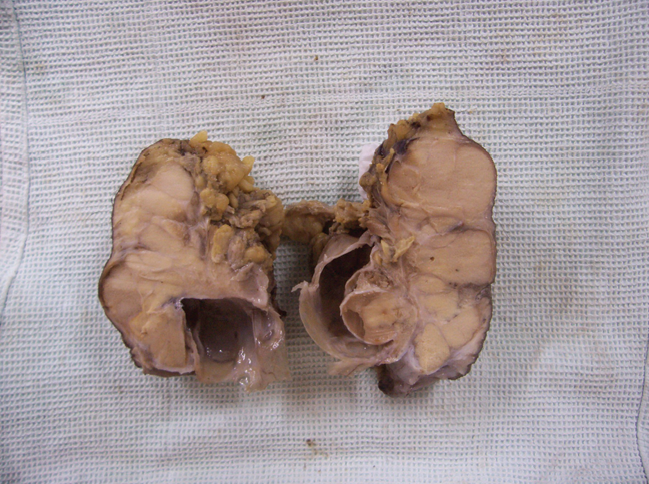
Low power of the mass with papillary projections and psammoma bodies.
Discussion
Mullerian epithelial tumors of testis are uncommon, the most common of which are serous type. 4 These serous papillary tumors are benign, borderline, or invasive (malignant) as their ovarian counterparts and have morphologic, immunohistochemical and ultrastructural features of serous tumors arising in the female genital tract. 5 It has been believed that these tumors develop from mesothelial inclusions or abnormalities in the development of coelomic epithelium 3 i.e. from areas of coelomic epithelium that became trapped in the testicular tissue. 5 The presenting signs and symptoms in the previously reported cases have been hydrocele, 2 and testicular fullness or mass. 5 Our case presented with testicular swelling for several months. Our case showed an intratesticular tumor with gross and microscopic features exactly similar to ovarian serous cystadenocarcinoma, i.e. well-formed papillary structures lined by serous epithelium. There were numerous psammoma bodies. The epithelium showed malignant nuclear features including enlargement, pleomorphism and hyperchromasia. Mitotic figures were inconspicuous. Morpho-logically most important differential diagnosis was mesothelioma arising from tunica vaginalis. 6 However both intratesticular location and immunohistochemical findings were against this diagnosis. Another important issue is the diagnosis of benign, borderline or malignant nature of the papillary serous tumors. 5 In our case overt stromal invasion, made this differential diagnosis easy. Serous cystadenocarcinoma can more commonly occur in paratesticular tissue of rete testis and epididymis with different pathogenesis and same clinical presentation, i.e. scrotal swelling. 7 Reported mean age of serous papillary carcinoma is 56 (14–77) for borderline and 31(16–42) years for invasive forms. 3 The recommended treatment is radical orchiectomy, because the tumor is highly resistant to radiotherapy and chemotherapy. 7 Our case was successfully treated with radical orchiectomy and now after a year he is doing well and completely symptom-free. Long term follow up of the patients with this tumor is important because there is high probability of long term metastasis. 2
In conclusion, serous cystadenocarcinomas of male genital tract are very similar to their ovarian counterpart but their occurrence in the male genital tract is extremely rare. However it should be considered in the differential diagnosis of any malignant testicular tumor with epithelial pictures.
