Abstract
BACKGROUND:
Radical resection of lung cancer and chemotherapy are the main methods for the treatment of early lung cancer, but surgical treatment is still the key and preferred method.
OBJECTIVE:
To evaluate the efficacy and safety of robotic-assisted thoracic surgery (RATS) and video assisted thoracic surgery (VATS) for non-small cell lung cancer (NSCLC).
METHODS:
The clinical cohort studies on the comparison of the effects of RATS and VATS in the treatment of NSCLC published in Web of Science, PubMed, The National Library of Medicine (NLM), China National Knowledge Infrastructure (CNKI) and Wanfang database from January 1, 2015 to December 31, 2022 were searched. Two researchers independently screened the literature, extracted the data, such as operation time, intraoperative conversion rate, intraoperative blood loss, number of lymph nodes dissected, and evaluated the quality of the included literature based on the Newcastle-Ottawa Scale (NOS). RevMan 5.3 software was used for Meat analysis.
RESULTS:
A total of 18 articles and 21,802 subjects were included. The results of the meta-analysis showed that the intraoperative blood loss of RATS was significantly less than that of VAS, and the difference was statistically significant [MD
CONCLUSION:
Compared with VATS, the number of lymph nodes dissected in RATS was significantly more, and the removal of lesions and lymph nodes was more thorough and accurate. More flexible and precise operation avoids the injury of important blood vessels during operation, effectively reduces the amount of blood loss during operation, shortens the indwelling time of thoracic drainage tube, and is conducive to postoperative rehabilitation of patients.
Introduction
According to the global cancer statistics report released by the International Agency for Research on Cancer (IARC) in 2020, the incidence and mortality of lung cancer are still high, which seriously endangers human life and health and brings great challenges to the global disease burden [1]. Radical resection of lung cancer and chemotherapy are the main methods for the treatment of early lung cancer, but surgical treatment is still the key and preferred method [2]. Non-small cell lung cancer (NSCLC) accounts for about 80% of all lung cancers, and about 75% of patients are already in the middle and advanced stage when detected, with a very low 5-year survival rate [3]. Taking NSCLC as an example, the most effective method of treatment is surgical resection of the lesion tissue. Traditional thoracotomy has a greater trauma to patients, and larger surgical incisions increase postoperative pain and affect the prognosis of patients [4]. In recent years, with the emergence and development of thoracoscopic technology, video-assisted thoracic surgery (VATS) has been widely used. Relevant studies have reported that VATS has more obvious advantages than traditional thoracotomy in the treatment of lung cancer [5, 6]. VATS has gradually developed into a routine procedure for the treatment of early lung cancer.
However, in thoracoscopic surgery, the surgeon’s surgical experience is very important and depends on the tacit cooperation between the surgeon and the handrail. However, due to the long running-in time, the learning curve is long. In addition, the lack of flexibility of thoracoscopic surgical instruments and unclear intraoperative vision also limit the further development of thoracoscopic technology [7]. In recent years, with the emergence of robotic surgery system, it has brought another significant change in the history of minimally invasive surgery [8]. In 2002, Melfi et al. [9] firstly reported robot-assisted thoracic surgery (RATS). At present, RATS has been proved to have a more stable and clear 3D vision, unique anti-tremor system and the ability of remote surgery, making it safer when completing fine operations [10]. However, some researchers still propose that RATS is not mature enough, mechanical operation is not stable enough and expensive [11].
With the continuous development of minimally invasive surgery, robotic and thoracoscopic surgery have been widely used in clinical practice and become the main treatment for lung cancer surgery. However, the current research evidence has inconsistent results for the clinical efficacy and safety evaluation of the two procedures, for both VATS and RATS, there are advantages and disadvantages and controversial. Therefore, this study retrieved the literature on robot-assisted and thoracoscopic-assisted treatment of early NSCLC published in the past five years, extracted relevant clinical indicators, and combined analysis to comprehensively and objectively evaluate the effectiveness and safety of robot-assisted and thoracoscopic-assisted surgery for early NSCLC. We intend to use meta-analysis to analyze and compare the real clinical effects of VATS and RATS in the treatment of NSCLC, in order to make a more objective evaluation of the efficacy and safety of the two procedures.
Materials and methods
Search strategy
According to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidance manual, three English databases, PubMed, Web of Science and The National Library of Medicine (NLM), and two Chinese databases, China National Knowledge Infrastructure (CNKI) and Wanfang, were systematically searched. The search time limit was from January 1, 2015 to December 31, 2022. The search was performed using a combination of subject words and free words. The search terms included Da-Vinci, robot, video-assisted, thoracoscopic, lung cancer, pulmonary neoplasm, and pulmonary cancer. In order to avoid literature omission, the target literature was obtained by reading the relevant systematic review.
Inclusion and exclusion criteria
Inclusion criteria: (1) The subjects were NSCLC patients; (2) Intervention measures: the experimental group was treated with Da Vinci robot-assisted thoracic surgery (RATS), and the control group was treated with video assisted thoracic surgery (VATS). (3) Outcome indicators reflecting the effectiveness and safety of surgery were reported, including operation time, intraoperative conversion rate, intraoperative blood loss, number of lymph nodes dissected; postoperative mortality, postoperative recurrence rate, postoperative complication rate, postoperative chest drainage time, postoperative hospital stay.
Exclusion criteria: (1) The study subjects were not simple NSCLC patients, but lymph nodes, mediastinal tumors, esophageal cancer, small cell lung cancer, etc. (2) Conference articles, case reports, systematic reviews and other research literature.
Study selection and data extraction
Two reviewers independently reviewed the abstracts and full text of each article according to inclusion of exclusion criteria. For disagreements between the two reviewers, a third reviewer was recruited for discussion until consensus was achieved. After literature screening, two reviewers independently respectively extracted the following information: (1) The basic characteristics of the included studies: including the first author, the scope of the study year, the year of publication, the country, and the type of research; (2) Baseline data of the included subjects: sample size and average age of the experimental group and the control group; (3) Outcome indicators: including operation time, intraoperative conversion rate, intraoperative blood loss, number of lymph nodes dissected; postoperative mortality, postoperative recurrence rate, postoperative complication rate, postoperative chest drainage time, postoperative hospital stay.
Assessments of methodological quality
The Newcastle-Ottawa Scale (NOS) [12] was used to evaluate the quality of the included literature. The scale was evaluated from eight aspects: the representativeness of the study population, the comparability between groups, the adequacy of the evaluation of the results, the adequacy of the follow-up time and the integrity of the follow-up. The full score was 9 points, and the total score was 7 points and above for high-quality literature, 5 points and below for low-quality articles.
Statistical analysis
Meta-analysis was performed using Revman 5.3 software. The odds ratio (OR) was used as the effect index for qualitative variables, and the mean deviation (MD) was used as the effect index for quantitative variables. Each effect size was expressed as point estimate and 95% confidence interval (CI). If the original literature only provided the median (interquartile range), the formula was used to convert it into mean and standard deviation and included in the analysis [13]. Heterogeneity test was used to determine the size of heterogeneity by the test of
Results
Study characteristics
A total of 2930 relevant literatures were retrieved in this study. After systematic screening, 18 eligible literatures were finally included [2, 7, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29], with a total of 21,802 subjects, 4,862 in the experimental group and 1,6940 in the control group. The flow chart of literature retrieval and screening is shown in Fig. 1.
Literature screening flow chart.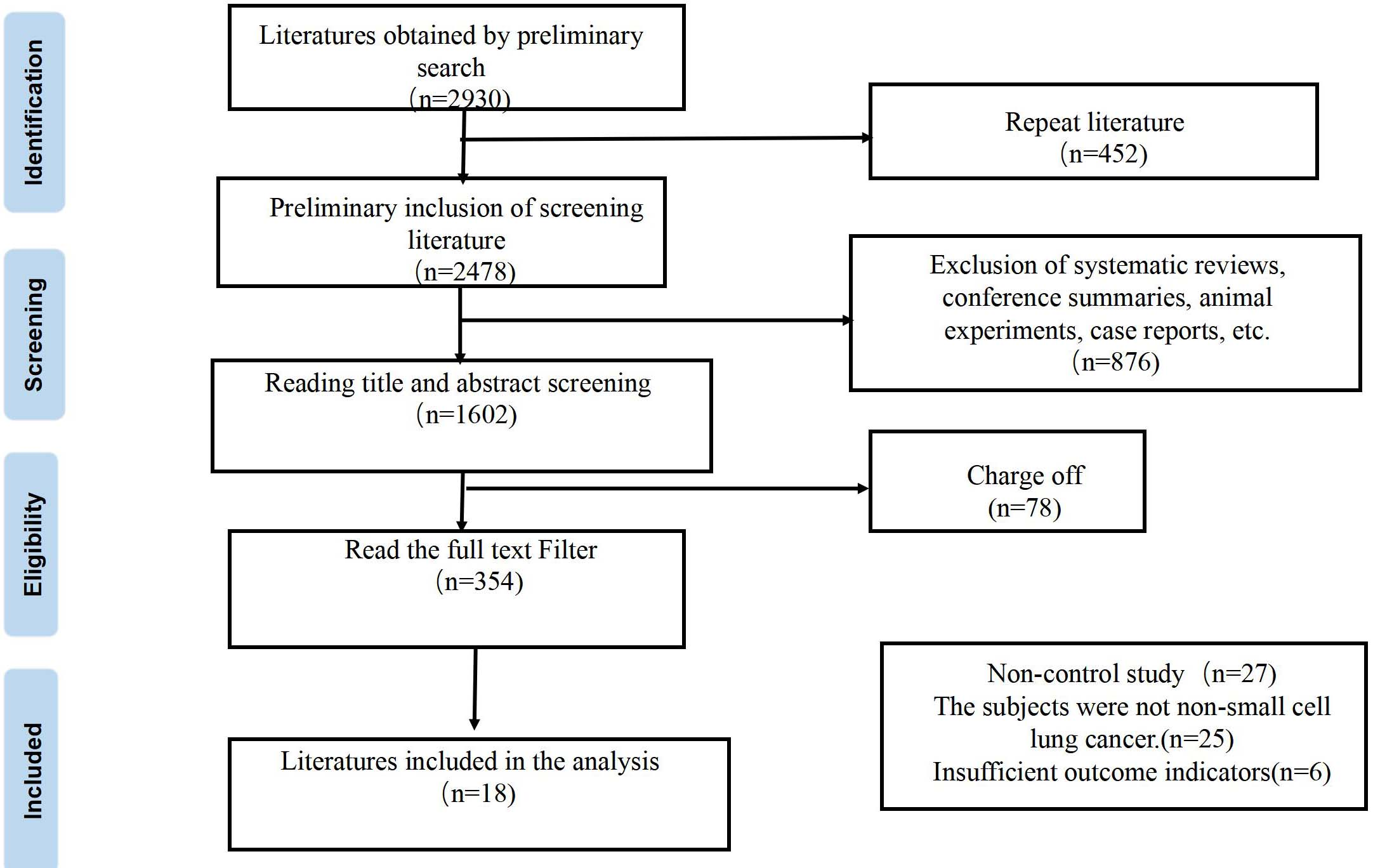
The basic characteristics and quality evaluation of the included literature are shown in Table 1. Finally, 18 articles were included, including 4 prospective cohort studies [13, 23, 24, 28] and 14 retrospective cohort studies [2, 7, 14, 15, 16, 17, 18, 19, 20, 21, 22, 25, 26, 27]. Among them, 1 was from Japan [15], 1 from France [28], 5 from the United States [2, 14, 16, 21, 27], and the rest were from China [7, 13, 17, 18, 19, 20, 22, 23, 24, 25, 26]. Among the included literatures, 17 literatures with NOS score
Basic characteristics of included studies and literature quality evaluation
Basic characteristics of included studies and literature quality evaluation
Note: 1
Operation time
A total of 11 articles compared the operation time of RATS and VATS. The results of heterogeneity evaluation showed that there was a high degree of heterogeneity among the studies (
Meta-analysis of RATS and VATS operation time.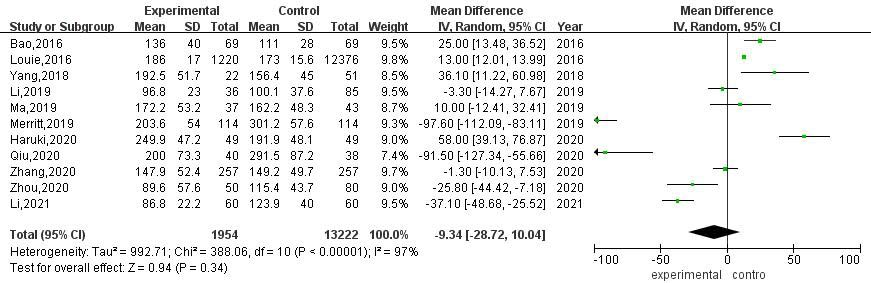
A total of 9 articles compared the intraoperative blood loss between RATS and VATS. The results of heterogeneity evaluation showed that there was a high degree of heterogeneity among the studies (
Meta-analysis of intraoperative blood loss between RATS and VATS.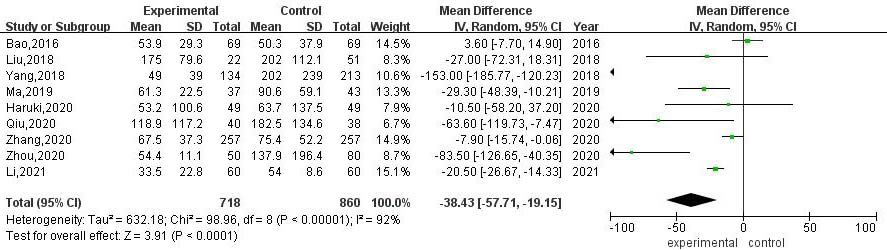
A total of 9 articles compared the number of lymph nodes dissected during RATS and VATS. The results of heterogeneity evaluation showed that there was a high degree of heterogeneity among the studies (
Meta-analysis of the number of lymph nodes dissected during RATS and VATS.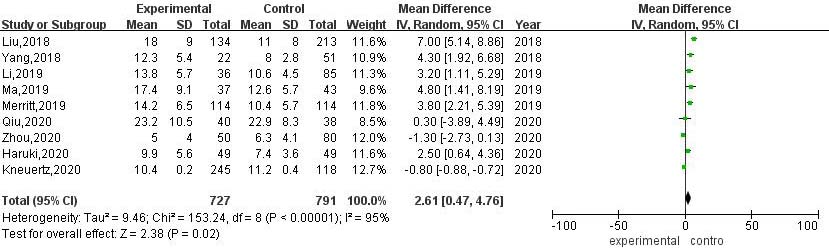
Meta-analysis of the rate of intraoperative conversion to thoracotomy between RATS and VATS.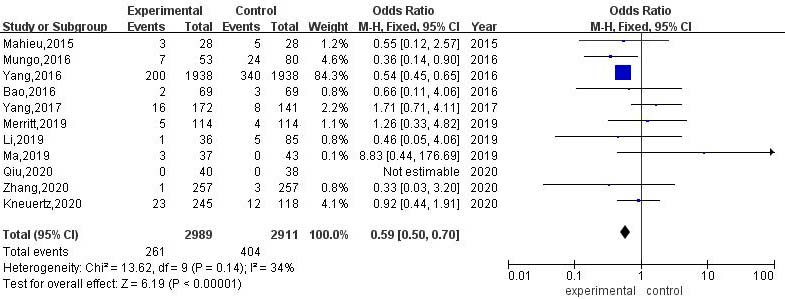
A total of 11 articles compared the rate of conversion to thoracotomy between RATS and VATS. The results of heterogeneity evaluation showed that there was low heterogeneity among the studies (
Postoperative chest drainage time
A total of 8 articles compared the postoperative thoracic drainage time between RATS and VATS. The heterogeneity evaluation results showed that there was moderate heterogeneity among studies (
Meta-analysis of thoracic drainage time after RATS and VATS.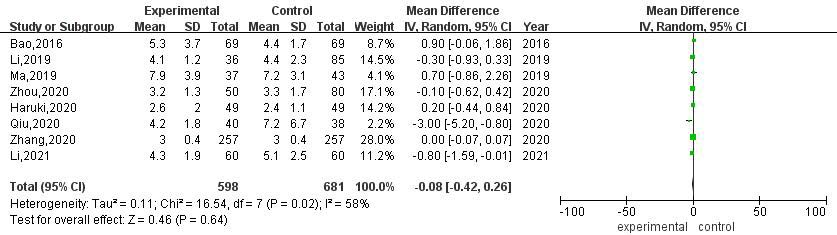
A total of 13 articles compared the postoperative hospital stay between RATS and VATS. The results of heterogeneity evaluation showed that there was a high degree of heterogeneity among the studies (
Meta-analysis of postoperative hospital stay after RATS and VATS.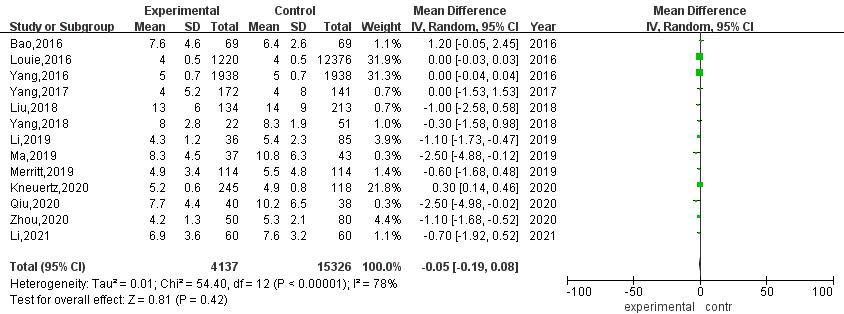
A total of 8 articles compared the postoperative mortality of RATS and VATS. The results of heterogeneity evaluation showed that there was low heterogeneity among the studies (
Meta-analysis of postoperative mortality after RATS and VATS.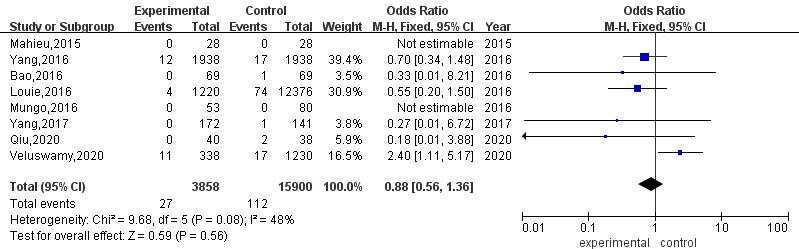
A total of 14 articles compared the incidence of postoperative complications between RATS and VATS. The results of heterogeneity evaluation showed that there was low heterogeneity among the studies (
Meta-analysis of the incidence of postoperative complications after RATS and VATS.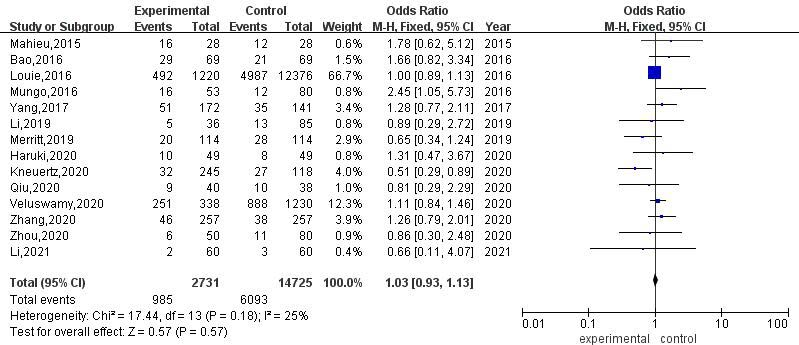
Among the 9 studies that included intraoperative blood loss, after excluding 1 study [23], sensitivity analysis showed that the heterogeneity among the included studies was reduced by 14%, and the intraoperative blood loss of RATS was still significantly lower than that of VATS [MD
Discussion
Systematic lymph node dissection is the most important part of radical resection of lung cancer. The number of dissection groups and the number of dissections not only remove lymph nodes that may have occult metastasis, but also provide more specimens, reduce the rate of missed diagnosis of pathological examination, and improve the accuracy of pathology, so as to obtain more accurate Tumor Node Metastasis staging, provide a reliable basis for postoperative guidance and treatment, and enable patients to obtain better survival benefits [30, 31]. The Da Vinci robotic surgical system manipulator has 7 degrees of freedom, higher flexibility and stability, and can achieve 360∘ surgical operation, which has unique advantages in cleaning lymph nodes. The results of this study showed that compared with VATS, the number of lymph nodes dissected during RATS was significantly higher, and the difference was statistically significant, indicating that RATS was more thorough and accurate in the removal of lesions and lymph node dissection.
The common reasons for conversion to thoracotomy in minimally invasive radical resection of lung cancer include: (1) the operation space is narrow, and the surgeon cannot continue the operation; (2) intraoperative injury of blood vessels, resulting in bleeding; (3) Severe lymph node calcification and extensive pleural adhesions [32]. When the above situation occurs during thoracoscopic surgery, it is mostly converted to thoracotomy, thereby continuing to complete the remaining surgical procedures. The results of this meta-analysis showed that the rate of intraoperative conversion to thoracotomy in RATS was lower than that in VATS, and the difference was statistically significant. The possible reason is that the Da Vinci robotic surgical system can provide the surgeon with a high-definition 3D surgical field that is magnified by 10 to 15 times. The unique inward turning wrist system and the multi-dimensional freely moving robotic arm can make the surgical instruments achieve hand-eye coordination similar to traditional thoracotomy [33, 34]. At the same time, it can filter the adverse effects of the operator’s hand tremor on the operation, making it safer when performing fine operations in small spaces such as pleural roof and diaphragm angle [35]. At the same time, the results of this study showed that the intraoperative blood loss of RATS was significantly less than that of VAS, and the difference was statistically significant, suggesting that RATS surgery is more minimally invasive and less traumatic to the body. This is due to the unique advantages of the RATS surgical system, which can largely avoid the tremor of manual operation, and is more flexible when performing fine operations in deep tissues and narrow spaces, thus greatly reducing damage to surrounding tissues. In addition, the three-dimensional visual field provided by it can clearly show the complex anatomical structure around the mediastinum and hilum of the lung, thus greatly reducing the damage of the operating arm to the blood vessels and surrounding tissues during the operation, effectively reducing the amount of intraoperative blood loss, and also reducing the risk of intraoperative thoracotomy to a certain extent.
This study found that there was no significant difference in the operation time, postoperative thoracic drainage time, postoperative hospital stay, postoperative mortality and postoperative complication rate between RATS and VATS groups. By analyzing the differences of each index, it can be found that in terms of postoperative thoracic drainage time, the time of RATS is shorter than that of VATS, but the difference is not statistically significant, which is consistent with the previous research results [36]. Patients undergoing pneumonectomy need routine indwelling thoracic drainage tube after operation. The purpose is to drain pleural effusion and gas, maintain intrathoracic negative pressure, and promote lung recruitment. However, there is no uniform extubation time. The traditional view is that the thoracic drainage volume is less than 100 mL/d before extubation [37]. According to this standard, it will not only prolong the indwelling time of the thoracic drainage tube, limit the patient ’s early ambulation, but also increase the risk of wound infection, which is not conducive to the postoperative rehabilitation of patients. With the introduction of the concept of enhanced recovery after surgery (ERAS), this traditional extubation time is no longer suitable for clinical work [38]. Most of the studies [39, 40, 41] found that compared with the traditional extubation group (thoracic drainage volum
There are some limitations in this study: (1) The included literature does not involve information on patient race, tumor diameter, and tumor stage; (2) The included literature includes different surgical methods, including lobectomy, segmentectomy and wedge resection of the lung, and the differences in this area will also have a certain impact on the surgical results; (3) The sample size of some studies is small, which may have a certain impact on the final results; (4) The study did not discuss the difference in the cost of RATS and VATS, and the cost of surgery directly affected the choice of surgical methods to a large extent.
Conclusion
The results of this study showed that compared with VATS, the number of lymph nodes dissected during RATS was significantly higher, and the clearance of lesions and lymph node dissection were more thorough and accurate. More flexible and precise operation avoids the damage of important blood vessels during operation, effectively reduces the amount of blood loss during operation, shortens the indwelling time of thoracic drainage tube, and is conducive to postoperative rehabilitation of patients. However, due to the limitations of this study, multi-center randomized controlled trials are still needed to verify the conclusions.
Availability of data and materials
All data generated or analysed during this study are included in this article. Further enquiries can be directed to the corresponding author.
Competing interests
None of the authors have any personal, financial, commercial, or academic conflicts of interest to report.
Funding
This study did not receive funding in any form.
Author contributions
WP conceived the study; FYH, QHF and HP participated in its design, data analysis and statistics; and WHF, LC and LXC helped draft the manuscript. All authors read and approved the final manuscript.
Footnotes
Acknowledgments
Not applicable.
