Abstract
PURPOSE:
Coffin-Siris syndrome (CSS) is a rare genetic disorder characterized by the presence of particular facies, congenital malformations, intellectual developmental disorder, behavioral issues, and speech and language impairment. Thorough neuropsychological assessments in the case of CSS have been reported infrequently, and its subdomains are poorly defined. A detailed description of the clinical, neurocognitive, behavioral, socio-adaptive sequelae of the patient with CSS is provided.
RESULTS:
The clinical diagnosis in the patient was confirmed by genetic analysis, which identified the presence of mutation of ARID1B gene; the parents’ Sanger sequencing reported normal. The neuropsychological assessments revealed borderline intellectual functioning (IQ-75, verbal > performance) with a mild socio-adaptive deficit score of 64 as suggested by the adaptive scale. The behavioral profile reported that the child had significant difficulties in the attention subdomain with concern in social and thought subdomains. The child met the profile for mild severity of Autism Spectrum Disorder and did not meet the criteria for Attention Deficit Hyperactivity Disorder. In addition, the child had scholastic difficulties in reading and mathematical skills.
CONCLUSION:
Neurocognitive, behavioral, socio-adaptive functioning and comorbidity assessment in order to provide holistic management of such children after thorough evaluation is essential for their overall functioning.
Introduction
Global developmental delay is a relatively common pediatric condition. However, its management requires a meticulous approach [1]. A child with developmental delay requires a complete neurocognitive assessment to identify their strengths and weaknesses in order to optimize overall functioning. Then vital interventions can be planned accordingly [2].
Coffin-Siris Syndrome (CSS) is a rare genetic syndrome presenting with characteristic facial features, congenital malformations, intellectual developmental disorder, and behavioral issues [3]. There are around 220 cases reported of CSS worldwide [4] along with a handful of reports from Lower Middle-Income Countries (LMIC).
An illustrative case study of a child with global developmental delay diagnosed as CSS is presented. Also, an attempt is made to further describe the pattern of cognitive and behavioral sequelae of the disorder in addition to socio-adaptive functioning with a holistic perspective.
Case report
A 7 year 9 month old male presented with complaint of developmental delay. He was the only child born from a non-consanguineous marriage. No significant antenatal, perinatal, or birth history was reported. Parents noticed the developmental delay from the early childhood years. As he grew, he had significant behavioral issues in the form of aggression, hyperactivity, and repetitive behavior. He was reported as a clumsy child. His school reports described him having selective friends, self-focused behavior, and hand flapping when excited. On examination, he had coarse facies, hirsutism, alopecia on the posterior part of the scalp, and a short fifth finger and toe. Based on the clinical observations, the child was referred for clinical exome sequencing, which revealed p.Gln452Pro mutation of the ARID1B gene. He met the clinical as well as genetic mutation found in Coffin-Siris Syndrome. As his parents were desirous of having a second child, their Sanger sequencing was done and was reported normal. The child’s hearing, thyroid function, and ophthalmological evaluation turned out to be normal. An MRI of his brain was normal except for thin corpus callosum.
Formal IQ testing of the child using Malin’s Intelligence Scale for Indian Children (MISIC), an Indian adaptation of the Wechsler Intelligence Scale for Children (WISC) [5] revealed borderline intellectual functioning (Full-scale IQ – 75, Performance – 67, Verbal – 83). His performance-based subdomain showed that he had deficits in visual perception abilities.
Vineland Adaptive Behavioral Scale (VABS) [6] was used to observe the adaptive and social skills of the child and to see his strengths and deficits in daily activities and self-sufficiency. His overall adaptive functioning score (composite score) measured by VABS was 64, suggestive of mild deficits. His communication, daily living, socialization, and motor skills were all low in functioning, with socialization and daily living the most affected. Fine motor skills were his strength, and the socialization domain was weak.
In the communication domain, he obtained age equivalents (AEs) as wide as 2.2–6.0 years, with the receptive area being weaker and the written part being stronger. In daily living skills, he obtained the AE from 2.2–4.5 years of age. In the socialization subdomain, his scores were of AE of 1.0–2.5 years. Mainly he had inappropriate socialization with infrequent use of spontaneous gestures reported. His gross motor milestones were delayed with an AE of around 2.1 years. Deficits in motor coordination and clumsy running were observed. Fine motor skills were his relative strength with an age equivalent of around 4.11 years.
His behavioral profile as measured by the Child Behavior Checklist [7] was suggestive of clinical scores (>98 percentile) in the attention subdomain and borderline scores in social and thought subdomains (93–98 percentile). His total scores were in the borderline range with a T score of 62. He did not meet the threshold for the diagnostic criteria for Attention Deficit Hyperactivity Disorder (ADHD).
On the Indian Scale for Assessment of Autism, a diagnostic test for Autism Spectrum Disorder (ASD) based on the DSM-5 [8], his score was 105, which is suggestive of mild autism (70–106). He showed major deficits in social relationships and reciprocity, emotional responsiveness, and behavior patterns.
On the scholastic curriculum test, he had significant difficulties in reading and mathematical skills and was 2 grades below expected for his age.
Discussion
The genetic syndrome evaluation and its management have always been crucial for a clinician [1]. The neuropsychological evaluation plays an important role in formulating a management plan. When the evaluations are administered to younger children, they can be used to formulate a goal-based intervention program [2]. Moreover, re-evaluations can then track progress over time which facilitates follow-up treatment planning as a part of health surveillance of any syndrome [9]. Further, such evaluations are also useful in diagnosing comorbid conditions like ASD and ADHD. This approach was adopted for the patient described.
The child met the clinical criteria for the diagnosis of CSS. These criteria include some degree of developmental delay, hirsutism, coarse facial features, and hypoplastic terminal phalanges of nails of the fifth digits of hands or feet [3]. On molecular testing, he had ARID1B mutation which is observed in the largest number with the phenotypic feature of CSS [10].
Similar to the majority of the children described throughout the literature [11], the patient had an intellectual developmental disorder as per his performance on MISIC, with the verbal domain better than performance. The comparative performance domain impairment could have been due to inattention, which is commonly observed in CSS [9], and poor visuospatial abilities correlating with thin corpus callosum shown via neuroimaging [12]. An accurate, developmentally-appropriate assessment of intellectual functioning is key for securing supportive services both within and outside the school setting. This also serves as a baseline for future testing. Domain-specific tests based on the neurocognitive difficulties that have been associated with CSS are usually advisable, specifically those assessing language, attention, and visuomotor abilities [13].
His overall adaptive functioning score was suggestive of mild deficits similar to other reported studies ranging from mild to moderate deficits [14]. Assessment of functional skills is required for the development of therapeutic goals and future attainment for any child with delayed development. Despite the substantial benefit of identifying socio-adaptive deficits at an early age, there has been little emphasis on this for individuals with CSS.
Clinically, it is very important to recognize the social deficits in the child because of their potential impact on cognitive functioning and educational planning. Approximately 54% of all children with CSS showed autism-related symptoms in the clinical and subclinical ranges [13] such as inappropriate social communication along with problem behaviors like self-stimulation and restricted interests. The child’s social skills were poor as he fit the criteria for ASD. He showed major concerns in social relationship and reciprocity, obsession with objects, and rigid behavior patterns.
Behavioral issues are often reported in children with CSS especially with ARID1B gene mutation [15]. Amongst behavioral issues, inattention has been reported in certain case reports. His behavioral profile was suggestive of clinical scores in the attention subdomain without meeting the threshold for ADHD diagnosis. He had significant difficulties in reading and mathematical skills and was 2 grades below expected for his age. Usually, the objective assessment of learning difficulties is not reported in the literature.
Conclusion
Thorough workup can provide the range of deficits and strengths in any child with developmental delay. This case report gives insight into the developmental sequelae not only in children with CSS but also with other developmental disorders. It provides clinical health practitioners and families an opportunity to work on the developmental goals of the child based on present level of functioning as shown in assessments.
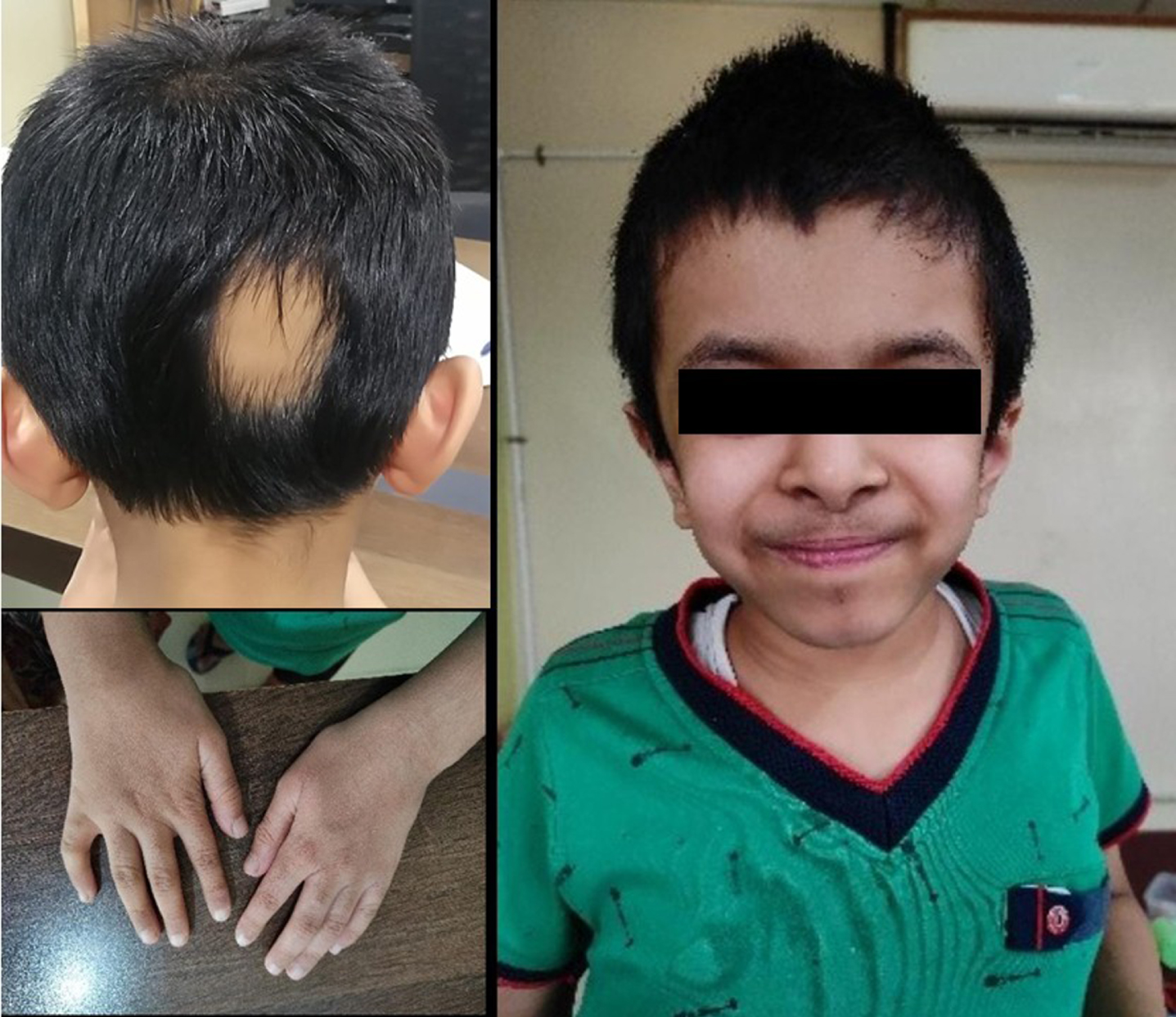
Phenotypic characteristics: excessive hair growth, sparse hair on posterior part of scalp, coarse facies, short fifth digit of hand.
An accurate baseline and future testing on similar concerns and any added ones will help to improve the overall functioning of a child. Also, it will increase the confidence of the families regarding health care availability in settings where resources may be limited, like India (or in LMIC). In India, here are multiple challenges faced in practice when it comes to neurodevelopmental disorders. This includes prioritizing acute illnesses over chronic neurodevelopmental disorders along with a heterogeneous population of doctors who lack the proficiency to cater to the special needs of children. Also, lack of insurance coverage for families with children with neurodevelopmental disorders and limited awareness among parents and the society are hurdles in executing the optimum standard of care for those with developmental disorders. With the help of timely referrals and the multidisciplinary standard of care available at the center along with the parental support, it was possible in this case to provide such care. Remembering the importance of adaptive components in such a population and its importance in classifying children with intellectual disabilities along with IQ is highlighted in this case.
Secondly, it gives an idea about areas of intervention available to make a child more independent and adaptive to society which is neglected in the literature, especially from LMIC. Lastly, a thorough evaluation of psychological, behavioral, and social functioning is necessary, given the elevated risk of ASD in children with CSS.
As CSS is a rare disorder, it is unlikely that a clinician will encounter a child with CSS in their whole career. However, the case presented can be used as a prototype of any child with developmental disorders. Such disorders require a multi-disciplinary team approach in which a developmental pediatrician along with a group of therapists work for the progress and improvement of the functioning of the child and the family.
Footnotes
Acknowledgments
The authors acknowledge the child who participated in the study and his parents. No funding was received for the study.
Conflicts of interest
The authors have no conflict of interest to report.
