Abstract
INTRODUCTION:
Acute Flaccid Myelitis (AFM) is a recently recognized pediatric condition characterized by flaccid paralysis that can cause lifelong deficits. Adhesive Capsulitis (AC) is a chronic condition that causes loss of passive range of motion in the shoulder due to joint contracture.
CASE REPORT:
This is a case report of a 15-year-old male who suffered from shoulder pain with progressive loss of passive range of motion after AFM, diagnosed with AC based on exam and radiology. After failing conservative management, the patient was successfully treated with ultrasound guided corticosteroid injection.
DISCUSSION/CONCLUSION:
AC is uncommonly reported in pediatric patients. However, secondary adhesive capsulitis is frequently associated with disorders of shoulder immobility in adults. This case contributes to the body of literature regarding pediatric frozen shoulder, highlights the successful use of ultrasound guided injections for management, and suggests a relationship between AFM and AC which may be beneficial for pediatric physiatrists in treating patients with shoulder pain or immobility related to this condition.
Keywords
Introduction
Adhesive Capsulitis (AC) is a chronic condition characterized initially by shoulder pain, followed by progressive loss of passive range of motion (PROM). Estimated to affect 2–5% of adults, the pathology of AC is related to loss of glenohumeral joint volume secondary to a thickened hypervascular joint capsule [1, 2]. Primary AC occurs spontaneously or in association with comorbidities such as diabetes. However, secondary AC is often associated with shoulder immobility due to certain disorders, such as stroke, spinal cord injury, or full thickness rotator cuff tears [2, 3, 4, 5]. Though there is a plethora of literature on adult AC, there is very little literature on AC in children, with only a single article identified, describing two cases [6].
Acute Flaccid Myelitis (AFM) is a recently recognized pediatric condition characterized by flaccid paralysis secondary to inflammation of the anterior horn cells, presenting in pediatric patients similar to Poliomyelitis. Patients typically present with a viral prodrome which progresses to asymmetric flaccid limb and trunk weakness, often with cranial nerve involvement. MRI of the spine generally confirms the presence of inflammation in the associated anterior horns [7]. Despite AFM commonly causing a unilateral upper extremity paralysis, there was no identified literature associating AFM with secondary AC.
Initial conservative management for AC typically consists of rehabilitation focused on aggressive PROM exercises and NSAIDs for pain control. Corticosteroid injections into the subacromial bursa or glenohumeral joint have been used in adult cases. If these measures fail, more aggressive surgical means of treatment can be pursued [8]. Ultrasound Guided Capsular Distention (USGCD) has been described as an intermediate step between low-volume injection therapy and surgery [8, 9]. While the comparative efficacy of these treatments is debated in the literature, little data exists to guide management of the exceedingly rare cases of pediatric AC [6].
We present a case of pediatric AC due to severe left shoulder immobility after AFM, which was treated with USGCD.
Case description
This is a case of a 15-year-old boy diagnosed with AFM after presenting to the Emergency Department with a five-day history of viral prodrome, which progressed to head drop and predominantly left sided weakness. Diagnosis of AFM was based on brain and spine MRI and lumbar puncture. Following 35 days of medical stabilization, involving intubation, corticosteroids and IVIG, the patient was discharged to the hospital.
Ultrasound image capture from the USGCD. This image shows the needle (arrow) in the
posterior glenohumeral recess, with fluid distending the overlying capsule and
infraspinatus.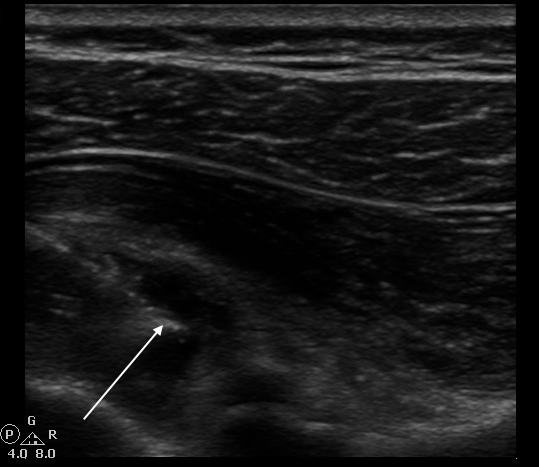
On admission, the patient exhibited hypotonia, areflexia and 0/5 strength in the left upper extremity, but was reported as having antigravity strength in the left leg and 4/5 strength on the right side. His left shoulder had passive abduction to about 90 degrees, and a positive left sulcus sign for glenohumeral instability. The patient complained of substantial left shoulder pain that was aching in quality, worse with PROM and radiated into the trapezius and upper arm. During his stay, he showed improving strength in the left arm, distally to proximally. However, he had no motor recovery in the shoulder and developed worsening shoulder PROM despite aggressive therapy. Three months after disease onset, a left shoulder X-ray showed no significant subluxation, arthritis or heterotopic ossification. Based on these findings, he was presumptively diagnosed with AC secondary to immobility in the setting of AFM. The decision was made to send the patient for a diagnostic and therapeutic USGCD with Sports Medicine after discussion with family regarding the lack of literature on Pediatric AC and the use of USGCD in pediatric patients.
Pre-procedural shoulder PROM in abduction was 20 degrees, flexion was 30 degrees, and external rotation was 10 degrees. For patient comfort and to improve patient tolerance of the procedure, regional anesthesia was obtained with ultrasound-guided blockade of the suprascapular and axillary nerves with 4 cc of Lidocaine 2%, deposited around each nerve. Once sufficient anesthesia was achieved, the patient was placed in the right lateral decubitus position. The posterior glenohumeral joint was visualized with a high-frequency linear probe. Using a lateral-to-medial in-plane approach, a 3 inch 22 gauge needle was introduced into the glenohumeral joint. Once the needle tip was visualized within the posterior glenohumeral recess, deep to the infraspinatus tendon, 4 cc of Ropivicaine 0.5% and 1 cc of triamcinolone acetate 40 mg/cc was injected. The syringe was changed and 10 cc of normal saline was infused against moderate resistance (Fig. 1). While the patient did not report overt pain during the procedure, he noted significant discomfort associated with the pressure sensation. The procedure was terminated with a total volume of 15 cc of solution infused. The glenohumeral joint capsule was notably distended on ultrasound. Of note, no audible “pop” or subjective sensation of a “pop” was reported by the patient, nor was there sonographic evidence of extracapsular extravasation of injectate, indicating that glenohumeral capsular integrity was preserved. The patient was discharged back to the hospital with instructions to engage in aggressive range-of-motion exercises with physical and occupational therapy within 24–48 hours.
Immediately following the injections, the patient demonstrated passive abduction to 80 degrees, flexion to 90 degrees, and external rotation to 30 degrees. He denied any pain at rest, though movement towards end ROM was reportedly uncomfortable. Within one week of the procedure, he demonstrated new active shoulder extension and external rotation, improving from grade 0/5 to 2/5. At the time of discharge, the patient had developed reciprocal arm-swing with gait.
This is a case of a pediatric patient who suffered from shoulder pain with progressive loss of PROM after AFM, which was diagnosed as adhesive capsulitis based on history and exam and by improvement after USGCD. Adhesive capsulitis explained the patient’s lack of PROM, in the context of a negative radiograph for heterotopic ossification or arthritis. Furthermore, the lack of spasticity and the loss of range of motion despite aggressive inpatient therapy made joint contracture unlikely. Lastly, the positive response to capsular distention helped confirm the diagnosis of adhesive capsulitis in this case.
Image-guided capsular distention (also described in the literature as hydrodilation or hydrodilatation) is a treatment option which is more mechanically aggressive than low-volume shoulder injections and less invasive than surgery [8]. First described in 1965 by Andren and Lundberg [9], this procedure involves the infusion of a large volume of solution (often containing normal saline, local anesthetic, and/or corticosteroid) with the goal of distending and stretching the capsule to improve range of motion. Image-guidance is used to confirm needle position and to confirm hydraulic distention of the capsule. Fluoroscopy was the preferred imaging modality for many years, due to real-time imaging capability and the ability to visualize extra-capsular extravasation of contrast-dye and to confirm capsular rupture [10]. With the advent and increased availability of ultrasound for visualization of musculoskeletal tissues and joints, ultrasound has emerged as a point-of-care imaging solution which has substantial benefits in that it is portable and does not expose the patient to radiation. These are particularly advantageous features when considering an intervention in a younger patient. A recent meta-analysis by Amber et al., comparing fluoroscopy and ultrasound suggests ultrasound is the more accurate modality to guide interventions [10].
Another technical consideration of the procedure which has evolved over time is whether rupture of the capsule is necessary for maximum improvement in post-procedural range of motion. Capsule rupture was long considered a desired end point to the distention procedure, however radiographic studies have demonstrated that the location of rupture was often in the biceps tendon sheath or subscapular recess without sufficiently stretching the more thickened areas of the capsule. A study by Kim et al. [11], comparing capsule-preserving distention versus capsule-rupturing distention under ultrasound guidance demonstrated significant improvements in pain and range of motion measurements in both groups. However, the capsule-preserving group was found to have a greater improvement in pain at 3 days follow up, and significantly larger gains in active and total-summed range of motion at 1 month. The proposed mechanism of this benefit is prolonged exposure to a sustained increase in glenohumeral joint pressure resulting in more effective stretching of the capsule when the integrity of the capsule is preserved. In contrast, capsular rupture is often localized to one aspect of the capsule and causes a sharp drop in glenohumeral joint pressure due to extravasation of the injectate [12]. This discussion is particularly germane to our patient, given that the potential long-term negative effects of capsular rupture in pediatric patients are not well studied.
We suggest a relationship between the patient’s AFM related immobility and his AC. AFM causes a flaccid weakness, often worse in a unilateral upper extremity. There is likely a relationship between the patient’s slow recovery of AFM and his frozen shoulder, in the same way that disorders such as stroke, spinal cord injury, or rotator cuff tears are related to secondary adhesive capsulitis. While the etiology of this patient’s AC makes sense in this context, we are unaware of any literature that identifies the development of AC in children with AFM. Also, there is limited literature describing AC in pediatric patients [6]. Therefore, this case is significant because it brings attention to a complication of AFM that may go undiagnosed, and it is the only documented case to our knowledge of USGCD that successfully improved pain and PROM in a pediatric patient with AC.
Conclusion
This report highlights a pediatric case of AC secondary to AFM related immobility, which improved following USGCD with corticosteroid, after failure of conventional conservative management. Given the much higher occurrence rate of AC in adults, there is a lack of literature regarding the utility of USGCD in pediatric patients. This case demonstrates the successful use of USGCD to facilitate the rehabilitation process by improving the PROM in a pediatric patient with AC secondary to AFM. Moreover, the remarkable finding of improved active range of motion suggests that early motor recovery may have been masked by the PROM restrictions caused by AC. We suggest maintaining a high index of suspicion for AC in patients with AFM who develop PROM limitations.
Footnotes
Acknowledgments
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. Informed consent was obtained from the patient’s guardian for the writing of this case report.
