Abstract
Background:
Alpha-synucleinopathies (AS) are characterized by pathologic aggregations of alpha-synuclein (
Objective:
The aim of this study was to further investigate and confirm the presence of cardiac
Methods:
All deceased patients with performed autopsy and with neuropathologically confirmed AS at the Clinical Department of Pathology in Lund 2010–May 2021 were evaluated for inclusion. Cases with insufficiently sampled cardiac tissue or only limited neuropathological investigation were excluded. An age-matched group of individuals with other neurodegenerative diseases, having no
Results:
The AS group had a significantly higher prevalence of cardiac
Conclusion:
This study confirms the association between AS and the presence of cardiac
Keywords
INTRODUCTION
Alpha-synucleinopathies (AS) comprise the clinical disease entities dementia with Lewy bodies (DLB), Parkinson’s disease (PD), and multiple system atrophy (MSA), plus cognitively unimpaired individuals with alpha-synuclein (
The pathological alterations in LBD are believed to originate in one single anatomical location, and then spread to adjacent neuroanatomical regions [7]. One theory proposes transcellular spread of
During the last decades, several studies have found evidence of extra-axial engagement and involvement of nerves in multiple organs, including the heart [13–18]. Studies have reported findings of cardiac, i.e., epicardial nerve
While not all previous studies provided neuropathologic confirmation, some did, and, i.e., the early work of Orimo et al. (2008) [13] did meticulously explore the cardiac nerve proteinopathy which we also have encountered in the clinical investigation of synucleinopathies over the years. Hence, we felt compelled to report on our findings in a slightly larger cohort—cases accessible from clinical diagnostic investigations over 12 years.
Aim of the study
The aim of this study was to investigate the presence of cardiac
MATERIAL AND METHODS
Study design
We analyzed the prevalence of
An approval was obtained from the Regional Ethical Review Board, Lund University, currently the Swedish Ethical Review Authority, nr 631-2015, 944-2017, 00051-2019 and 06582-2019.
Subjects
Neuropathological diagnoses
All deceased patients with neuropathologically confirmed AS at the Clinical Department of Pathology in Lund 2010-May 2021 were evaluated for inclusion (
The neuropathological diagnosis of AS was defined by findings of
Clinical diagnoses
The clinical diagnoses were retrieved from the medical records or referrals to the neuropathological examination. Most individuals had a clinical diagnosis of PD, DLB, or MSA, as determined from a specialist. In a few individuals with AS in the brainstem only, there was cognitive disease of other type.
Control group
The age-matched control group included 32 subjects with any major neurocognitive disorder without
Disease duration
Disease duration was defined as the year of diagnosed cognitive impairment of any type or, when not available, date of first symptoms described in the medical records until time of death. Brainstem LBD and in many cases limbic LBD do not generally exhibit clinical symptoms of the AS, particularly not in the presence of other neurocognitive disorders [26]. Information regarding disease duration was retrieved for these cases as well, but their symptoms were likely due to other pathologies than
Cardiac alpha-synuclein pathology
The myocardial samples were taken from several different locations. The sections stained with hematoxylin-eosin were retrieved and analyzed for selection of the section most clearly harboring nerves. The correlating paraffin-embedded tissue block was re-sectioned at 3 micrometer and immunohistochemically stained with a monoclonal mouse anti-
Cardiac
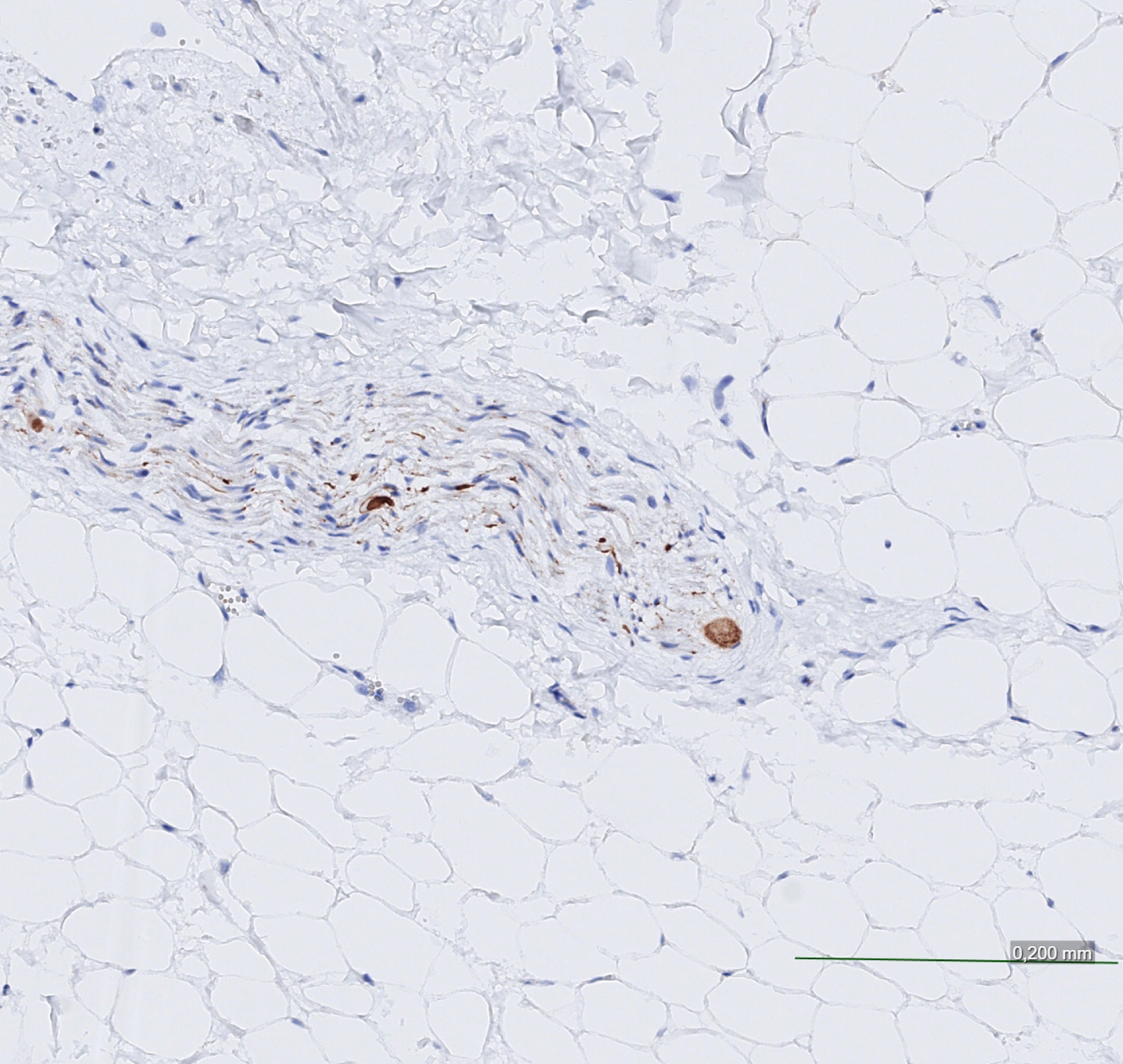
Cardiac (epicardial) nerve strongly positive for alpha-synuclein pathology, with Lewy bodies present.

Cardiac nerve weakly positive for alpha-synuclein pathology.
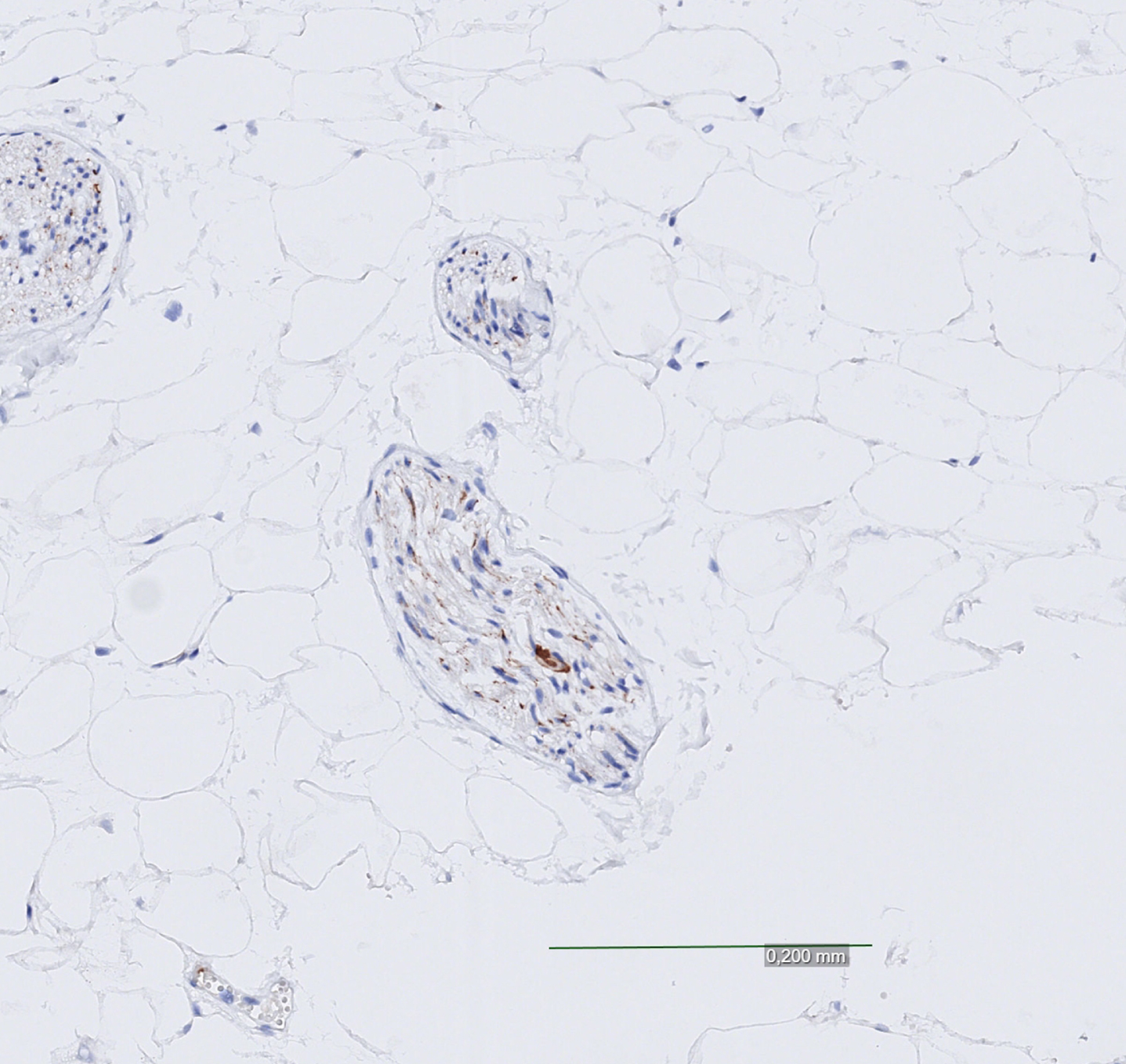
Cardiac Lewy bodies, strong and focal positivity.
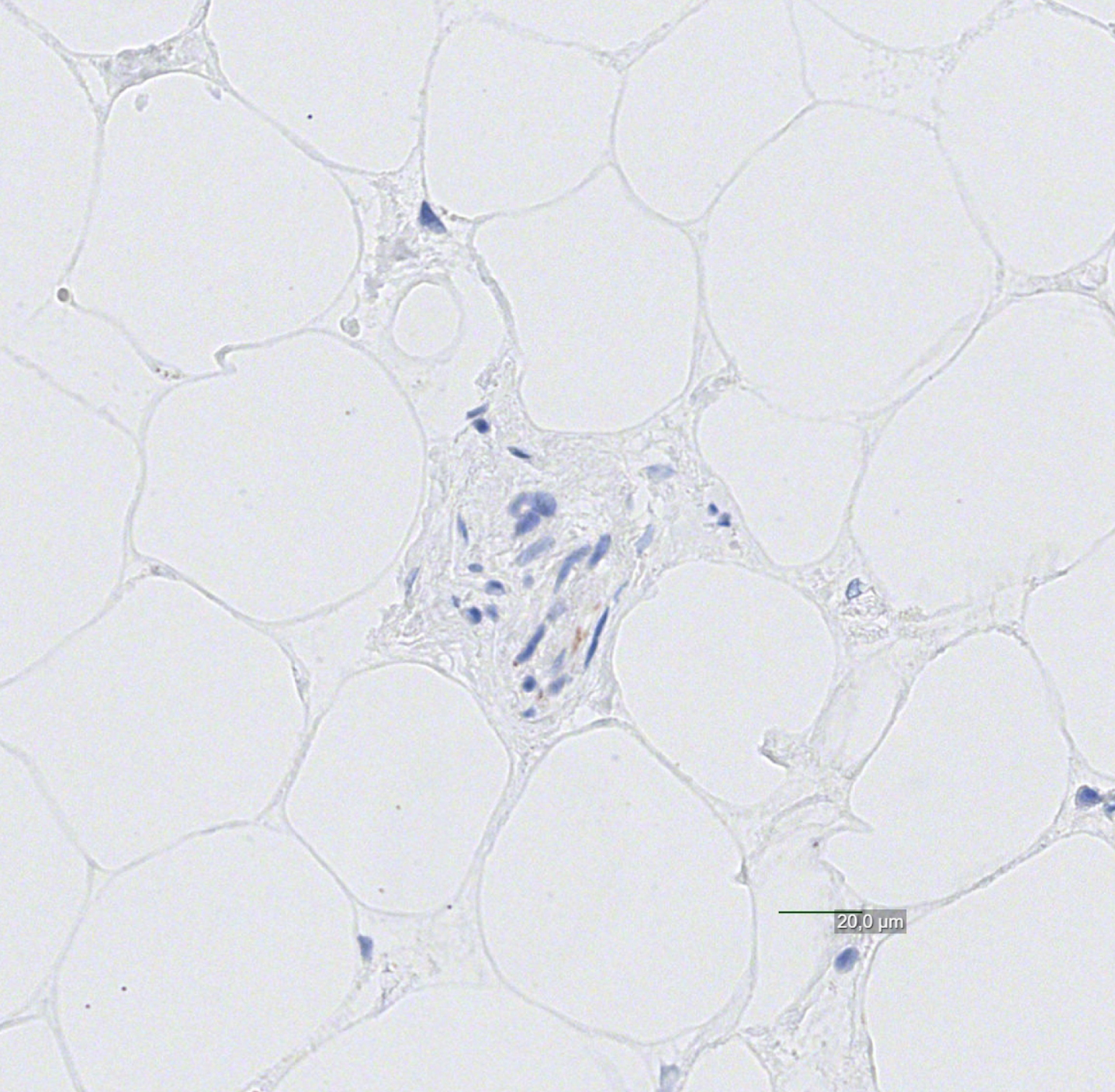
Cardiac nerve negative for alpha-synuclein pathology with questionable/minimal findings.
Data analysis
Statistical analyses were carried out using Microsoft Excel and IBM SPSS Statistics 26. AS and the control group were compared regarding the presence of myocardial
RESULTS
AS subjects
Among the total of 92 subjects reviewed for inclusion, 24 cases were excluded, mainly due to the lack of stainable nerve within the myocardial tissue (often myocardium without epicardial surface) and in a few the lack of sampled heart tissue. Hence, 68 study subjects were included for analysis. For demographic data on the study group, see Table 1.
Demographic data and neuropathological diagnoses for all subjects
AS, alpha-synucleinopathy; LBD, Lewy body disease; MSA, multiple system atrophy, including one MSA-C, MSA-P, MSA-C + P and one undetermined; AD, Alzheimer’s disease; VaD, vascular dementia; FTLD, frontotemporal lobar degeneration. *Including five cases with progressive supranuclear palsy and one with corticobasal degeneration. **Including AD, VaD, and FTLD, whereof 6 had a combination of AD + VaD. aPresented in median years, interquartile range within brackets.
In the AS group, 64 (94%) had LBD and 4 (6%) had MSA. Within the LBD group, 42 had cortical, 9 had limbic and 13 had brainstem LBD (Table 1). In addition to fulfilling the criteria for AS, a total of 25 cases had concomitant AD, VaD, FTLD pathology, or admixtures of these, most frequently concurrent AD pathology (Table 2A). The four MSA cases were of cerebellar, parkinsonian and mixed type, respectively, whereas one could not be specified further due to the lack of representatively sampled brain regions (Table 1). The clinical diagnoses did not indicate an AS in all individuals of the studied group and the clinicopathological concordance was 66% (45 cases with a concordant clinical-neuropathologic diagnosis). The clinical diagnoses were distributed as follows: 17 (25.0%) PD, 12 (17.6%) DLB, 5 (7.4%) MSA, 11 (16.1%) AD, 5 (7.4%) vascular dementia (VaD), 5 (7.4%) frontotemporal lobar degeneration (FTLD), 2 (2.9%) with a mix of AD and VaD, 1 (1.5%) with a mix of AD and LBD, and 1 (1.5%) with a mix of AD and PD. Six individuals (8.8%) were labeled with dementia not otherwise specified (DNOS) and three (4.4%) had no diagnosis at all (Table 2B). All three cases with no clinical diagnosis had a neuropathologically confirmed cortical LBD. All cases with brainstem LBD had been clinically diagnosed with other neurocognitive disorders, which were verified as specific neuropathologic conditions in each case.
Neuropathological comorbidity in the AS group
AS, alpha-synucleinopathy; AD, Alzheimer’s disease; VaD, vascular dementia; FTLD, frontotemporal lobar degeneration. *≥2 of the pathologies mentioned above.
Clinical diagnoses in the AS group
AS, alpha-synucleinopathy; PD, Parkinson’s disease; DLB, Dementia with Lewy bodies; MSA, multiple system atrophy; AD, Alzheimer’s disease; VaD, vascular dementia; LBD, Lewy body disease; FTLD, frontotemporal lobar degeneration; DNOS, dementia not otherwise specified.
Control subjects
A total of 32 subjects were included. For demographic data on the control group, see Table 1. The neuropathological diagnoses in the control group were AD in 10 (31%), VaD in 6 (19%), FTLD in 7 (22%), and mixed pathologies in 9 (28%) (Table 1). In the latter group, the majority had a combination of AD and VaD.
Cardiac alpha-synuclein pathology
Cardiac
The prevalence of cardiac
Cardiac alpha-synuclein pathology in AS and control cases
AS, alpha-synucleinopathy;
DISCUSSION
In this study we investigated the presence of cardiac
Our findings regarding AS are concordant with previous studies reporting involvement of nerves in multiple organs including the heart, suggesting that AS are systemic disorders with primarily neurological manifestations [13–18]. Further, our results lend support to the caudo-rostral spread of
The findings of cardiac
Regarding disease duration, no striking nominal difference was observed between the different AS disorders. However, no results were presented, and no conclusions were drawn as information concerning onset of brainstem LBD and limbic LBD was not judged representative due to coexisting other neurocognitive disease contributing to clinical symptoms.
A strength of this study is the relatively large sample size. Moreover, the confirmation of
Optimally, the control group would be comprised of cases representing the age-matched “general population” instead of cases with major neurocognitive disorders. The brain is however not specifically investigated in cognitively healthy individuals, except for by selective tissue sampling for specific reasons. A control group representative of the general population could thus hardly be obtained. Hence a mere referral for autopsy means a selection of individuals.
A limitation of this study concerns the myocardial tissue sampling, which was targeted to include epicardial tissue only in the smaller, prospectively collected group, while tissue was evaluated retrospectively in most cases. Many heart tissue samples were originally taken with the intention to verify a suspected myocardial infarction, steered by macroscopic findings of discolored myocardium, rather than to analyze nerve tissue, which is best studied in the epicardial tissue [26]. Consequently, some AS cases were excluded from the study, and some cases were included and analyzed despite suboptimal tissue samples with minimal nerve components, likely leading to an under-reporting of cardiac
The finding however of 100% cardiac a-syn positivity in the prospectively sampled cases, indicates that we perhaps could have found cardiac a-syn positivity in all AS cases, had they been sampled in a prospective way.
CONCLUSION
We found an association between AS and cardiac
Footnotes
ACKNOWLEDGMENTS
The Trolle-Wachtmeister Foundation for Medical Research, as well as The Lund University Medical Faculty, are acknowledged for essential funding of this study.
CONFLICT OF INTEREST
MH is a former employee of Biogen and Eli Lilly but has no active financial interest in either company. The other authors have no conflict of interest to report.
