Abstract
Background:
Despite evidence for the benefits of exercise in Parkinson’s disease (PD), many patients remain sedentary for undefined reasons.
Objective:
To compare exercise habits, perceptions about exercise, and barriers to exercise in ‘low’ (<3 h/week) and ‘high’ (≥3 h/week) exercisers with PD.
Methods:
A 48-item survey was administered to PD patients at an outpatient academic center. Chi-squared tests were used to compare the percentage differences between low- and high-exercisers with two-sided tests and a significant level of 0.05.
Results:
243 surveys were collected over three months; 28 were excluded due to incomplete data, leaving 215 to be analyzed. 49.3% reported ‘low’-exercise and 50.7% reported ‘high’-exercise. High-exercisers participated in higher intensity exercise regimens (83.4% versus 32.1%,
Conclusions:
There are significant differences between people with PD who exercise regularly and those who do not in terms of motivators and barriers. These findings should be considered when tailoring recommendations for PD patients to encourage exercise, and in designing future interventions.
INTRODUCTION
Encouraging exercise has become an integral part of the management of Parkinson’s disease (PD) as data on the beneficial effects of different exercise modalities continues to expand. Aerobic [1, 2], strength-training [3, 4], yoga [5, 6], Tai Chi [7], forced exercise [8], and even virtual reality [9] for gait training have been shown to augment motor function, prolong functional independence, and improve quality of life. The National Parkinson Foundation (NPF) has emphasized the importance of exercise as part of the standard-of-care for patients based on data obtained from PD Centers of Excellence (COE) around the United States. Despite the growing evidence and awareness of the importance of exercise, many PD patients do not exercise regularly. Analysis of the NPF QII Registry was able to identify that 56% of PD patients did not exercise regularly, and that these patients had worse quality of life, worse physical function, more progression of disease, and more caregiver burden even after controlling for disease duration, disease severity, cognition, and demographics, both in a cross-sectional and one-year longitudinal analysis [10].
In a clinical setting, discussions of exercise are limited by our incomplete understanding of the variables that most influence activity versus inactivity in this patient population. If we can better understand the differences between regular exercisers and non-exercisers, we may be able to transform the latter population into the former. One cross-sectional study did look at the barriers to engaging in exercise in PD patients and compared an exercise group to a non-exercise group, distinguished based on both patient report and an activity monitor [11]. They found that fear of falling, lack of time, and low-outcome expectation (i.e., participants did not expect to derive benefit from exercise) were significant barriers in the non-exercise group. We were interested in verifying this finding, but also understanding the difference between the two populations with regards to beliefs about exercise and the ideal exercise settings that would lead to increased participation.
The objective of this study was 1) to compare the beliefs and knowledge about exercise and its benefits in PD among exercisers and non-exercisers, 2) to identify the exercise conditions and motivators for exercise that are most likely to lead to exercise compliance, and 3) to assess barriers to exercise and how these differ between groups.
MATERIALS AND METHODS
Design
This was a cross-sectional study in which a 48-item survey was administered to patients with PD between October 2015 and January 2016. There were 215 study participants recruited from the Northwestern University PD & Movement Disorders Center (NUPDMDC) as they presented for their regularly scheduled clinic visits. NUPDMDC is a NPF COE staffed by 4 fellowship-trained Movement Disorders specialists, in which over 2,000 patients with PD are seen annually. Every patient seen for PD between October 2015 and January 2016 was presented with the optional survey which included multiple-choice and Likert-scale-based questions regarding their PD symptoms, exercise habits, perspectives on the benefit of exercise, preferences regarding exercise regimens, and perceived barriers to their own participation in exercise. Subjects were asked to recall an estimate of their average amount of exercise per week using a Likert-scale of ‘none,’ ‘<3 hours,’ and ‘≥3 hours.’ Surveys were completed while waiting for their appointments and then returned to their Movement Disorders specialist who would 1) determine whether the patient met inclusion criteria or any exclusion criteria and separate the surveys accordingly, and 2) answer 5 non-identifying questions regarding the patient’s disease, antidepressant use, and deep-brain stimulation (DBS) status. No patient identifiers were included in the survey.
All participants met the following inclusion criteria: age of 18 years or over and confirmed to have a diagnosis of idiopathic PD by a Northwestern Movement Disorders specialist. Participants were excluded if they had a diagnosis other than idiopathic PD, such as atypical parkinsonism or the diagnosis was in question, if they had a concurrent neurologic condition that rendered them with severe disability (i.e., major stroke or head injury), and/or if they were unable to complete the survey adequately due to severe cognitive impairment or language barrier. Excluded surveys were discarded in a HIPAA-compliant manner by their physician.
This study was approved by the Institutional IRB and a waiver of consent was obtained.
Measures
Based on the survey responses, participants were categorized into two groups: low-exercisers (those who reported less than 3 hours per week) and high-exercisers (those who reported more than or equal to 3 hours per week). This distinction used a slightly higher cutoff than the American Heart Association’s recommended guideline of 150 minutes of moderate exercise per week. All survey responses were compared between these groups.
Data was collected on demographics and basic disease characteristics. This included employment status, living environment, exercise practices, years from PD diagnosis, primary perceived motor symptom, presence of depression, cognitive impairment, or orthostasis, antidepressant use, and DBS status.
Beliefs and knowledge
First, with regards to perceptions regarding exercise and PD, participants were asked how often their Movement Disorders specialist would talk to them about exercise, how their exercise habits changed since their PD diagnosis (i.e., less, more, or same), if they believed there is scientific evidence showing that exercise can slow the progression of PD symptoms, and their view on the potential impact of exercise on motor symptoms of speed of movements, balance and fall risk, and tremor, and non-motor symptoms of mood, memory, fatigue, and sleep.
Optimal exercise conditions and motivators to exercise
Second, participants were asked to indicate their likelihood of participating in exercise under certain conditions on a Likert-scale of ‘less likely,’ ‘does not matter,’ and ‘more likely,’ in order to determine which environmental variables would lead to the best exercise compliance. The 13 options included exercising alone, in a group, with an “exercise buddy,” with a significant other, with a personal trainer, with a group instructor, for <30 minutes, for 30–60 minutes, as a means of transportation, with equipment, with the same routine each time, with a different routine each time, and if their Neurologist told them it was necessary.
Barriers to exercise
And finally, participants were asked what makes it difficult for them to exercise on a 5-item Likert-scale of ‘strongly-agree’ to ‘strongly-disagree,’ in order to identify variables that lead to poor exercise compliance. The 15 options included fear of falling, history of falls, having no one to exercise with or motivate them, hindering PD symptoms, lack of time, fatigue, excessive daytime sleepiness, depression, lack of exercise experience, disliking exercise, low-outcome expectation, lack of necessity, and other hindering medical conditions.
Analysis
Simple descriptive statistics including mean (SD), median (interquartile range) and count (percentage) were reported for the whole sample, as well as for the low- and high-exercise groups. For categorical questions, we performed Chi-squared tests to compare the percentage differences between the low- and high-exercise groups. We used Fisher’s exact tests when the cell count was less than the expected in any of the cross tabulations. The number of barriers had a skewed distribution, thus the non-parametric Wilcoxon rank sum test was used to compare the number of barriers between the groups. Two-sided tests and a significant level of 0.05 were used for all tests. Analyses were performed in R: A language and environment for statistical computing (R Foundation for Statistical Computing, Vienna, Austria, version 3.3.0).
RESULTS
Surveys were completed by 215 PD patients. Surveys from 28 patients were excluded due to incomplete data. There were no patients who refused to complete the survey. The mean age and gender breakdown of the PD patients seen in the NUPDMDC over the period in which data was obtained was 68 years, 63% male, and 37% female, respectively. Of the 215 participants, 49.3% (N = 106) reported low-exercise (i.e., <3 hours/week) and 50.7% (N = 109) reported high-exercise (i.e., ≥3 hours/week). These groups differed significantly only with respect to living arrangements and employment status, with low-exercisers being more likely to live in a retirement community or nursing home and less likely to be employed. There were no significant between-group differences in disease duration or key motor and non-motor symptoms questioned (Table 1). Of note, only 7.9% of our study population had DBS.
Participant demographics and disease characteristics
†Mean age and gender breakdown of the PD patients seen in the NUPDMDC over the period in which data was obtained was 68 years, 63% male, and 37% female, respectively.
Participants engaged in the following exercise regimens: walking (73.5%), strength-training (34.9%), physical therapy (29.8%), cycling (23.3%), yoga (12.6%), swimming (7.9%), running (7%), dance (4.7%), Tai Chi (4.7%), and other (19.1%) (Table 2). Of the various exercise regimens participants engaged in, the most common were those that would be considered low-intensity. High-exercisers had statistically significantly higher participation in both strength-training and cycling, both considered to be higher-intensity regimens (50.5% and 33% versus 18.9% and 13.2%, total 83.4% versus 32.1%,
Participant exercise regimens
Beliefs and knowledge
Participants were generally well-educated about the importance of exercise, but high-exercisers were significantly more likely to change their habits to exercising more since their PD diagnosis (54.2% versus 27.8%,
Perceptions of exercise
Perceptions of non-motor symptoms
Optimal exercise conditions and motivators to exercise
The motivating factors and non-factors that were reported by ≥50% of low-exercisers and high-exercisers are summarized in Fig. 1. Low-exercisers reported 7 of 13 to be motivating factors including having their Neurologist say exercise was necessary, exercising with a personal trainer, significant other, exercise buddy, in a group, or with a group instructor, and exercising shorter durations at a time (<30 minutes compared to 30–60 minutes long). On the other hand, high-exercisers did not report as many motivating factors as did the low-exercisers, only 3 of 13. Like the low-exercisers, high-exercisers were motivated by exercising with a personal trainer or significant other, and having their Neurologist tell them exercise was necessary.
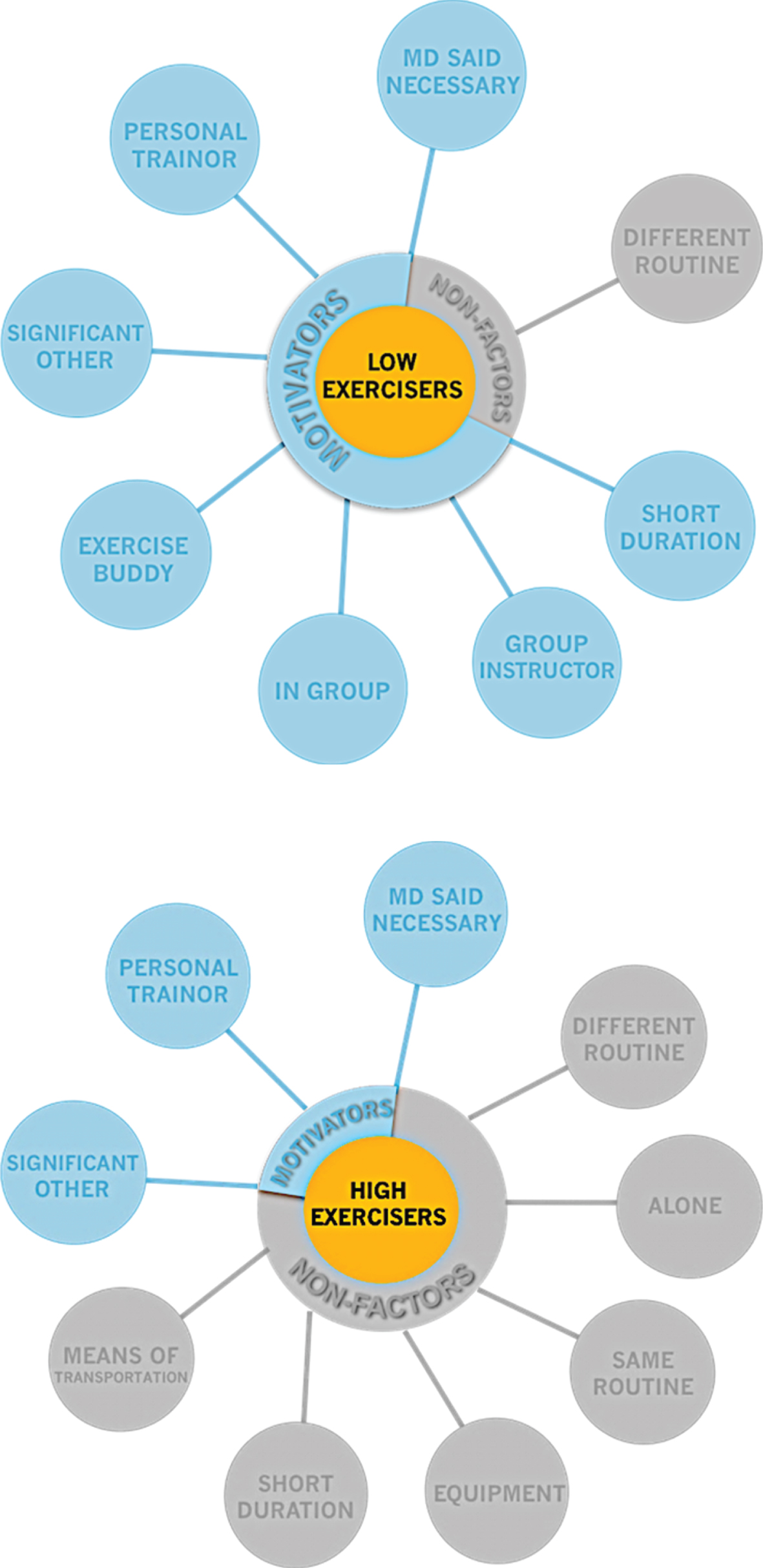
Motivators to exercise: Motivating factors and non-influential factors that were reported by ≥50% of low-exercisers and high-exercisers.
Barriers to exercise
Finally, participants were asked about 15 potential barriers to exercise (Table 4). The median number of barriers to exercise reported by low-exercisers was twice that of high-exercisers (2 versus 1,
Barriers to exercise
DISCUSSION
This study shows that there are significant differences between people with PD who exercise regularly compared to those who do not in terms of their beliefs about exercise, their ideal exercise conditions and motivators for exercise, and their specific barriers to exercise. With the growing evidence that exercise improves PD outcomes and quality of life, it is important for Neurologists to identify motivators and barriers to exercise and provide appropriate recommendations to patients. Likewise, it is important for communities to design exercise programs that meet the needs of PD patients in a way that increases their likelihood of compliance and success with regards to exercise frequency, duration, and intensity. Our study is the first to demonstrate the differences between the beliefs and needs of low- and high-exercisers in PD. The study offers important findings that can lend to evidence-based guidelines for exercise in PD.
Beliefs and knowledge
First, our findings support the concept of self-efficacy as it relates to exercise behavior in PD patients, playing a dual role as a predictor and an outcome of exercise. Since receiving their diagnosis of PD, our high-exercisers were more likely to change their habits to exercising more, whereas our low-exercisers changed their habits to exercising less. High-exercisers were also more likely to participate in higher-intensity exercise regimens, often participating in both aerobic exercise and strength-training. Studies have shown that progressive resistance-training, that is inherently more challenging and generates large forces that further increase neuronal activation in the basal ganglia, can increase not only the strength but also the speed of movements, thereby improving PD motor control [3, 13]. This could be thought of as a “higher dose” of exercise. The heightened benefit from higher-intensity exercise may feedback into higher levels of self-efficacy. In fact, most recently, researchers have examined reward signaling in the ventral striatum of PD patients who are habitual exercisers versus sedentary and participated in aerobic cycling versus controls/stretching only using an fMRI-based monetary incentive task. They have shown that in the habitual exercisers and after three months of aerobic exercise, there was higher fMRI signal in the ventral striatum, suggesting that aerobic exercise alters the function of reward circuitry, potentially through enhanced transmission in the mesolimbic dopamine system [14].
Second, our findings revealed that non-motor PD symptoms could be just as important as motor symptoms in hindering the PD patient in adopting regular exercise. Low-exercisers were less likely to believe that exercise improves mood and sleep, despite considerable evidence in the literature supporting this and the considerable impact non-motor symptoms have on quality of life [15, 16]. High-exercisers, on the other hand, did believe in the benefits of exercise on these symptoms. Low-exercisers reported depression and fatigue as barriers to exercise, and reported a higher incidence of these symptoms compared to the high-exercisers, however they were less likely to believe that exercise could help these symptoms. The number of subjects actually reporting these symptoms as barriers to exercise was a small subset of the entire cohort, and rates of a diagnosis of depression were actually very similar amongst the two groups, as were the rates of antidepressant use: 38.6% and 41.1% among low-exercisers, and 38% and 37.7% among high-exercisers (Table 1). Perhaps a subset of low-exercisers experience either more severe depression or poorly-controlled depression, although these symptoms may also be under-reported and under-recognized. This argues that clinicians should pay special attention to treating mood, fatigue, and sleep as part of their efforts in motivating exercise, not to mention educate patients about the potential non-motor benefits of exercise.
Optimal exercise conditions and motivators to exercise
Low-exercisers required more motivating factors to exercise, whereas high-exercisers reported more factors that were non-influential to their exercise behavior. The motivating factors that were shared by the two groups again highlight how self-efficacy should be harnessed for all of our PD patients; both low- and high-exercisers were motivated by a significant other, a personal trainer, or even their Neurologist telling them it was necessary to exercise, all clearly strategies that can guide PD patients to higher levels of self-efficacy. Recommendations to exercise likely need to be heard more than once, and from multiple healthcare professionals including physical therapists and physiatrists. Educational events discussing the importance of exercise may also be beneficial. There is strong evidence in the primary care community that advice from health professionals significantly influences adoption of healthy lifestyle behaviors including regular physical activity [17]. This underscores the importance of clinicians and physical therapists talking to their patients about their exercise habits, encouraging significant others’ or family members’ involvement, and routinely recommending group PD exercise classes as part of standard-of-care.
Similar findings have been found with other chronic diseases that directly affect movement like PD, such as arthritis, the leading cause of disability in the United States. In one qualitative study of 68 community-dwelling adults with arthritis, the symptoms related to arthritis such as pain, stiffness, fatigue, and mobility issues were perceived as barriers to exercise, but improvement in these outcomes were also seen as potential motivators for exercise. In this focus-group-based study, exercisers identified that they were more likely to make adaptations to their regimens to account for these specific barriers (i.e., modify the type or intensity, take a respite during flares, and work through the pain to attain benefits), whereas non-exercisers were more likely to quit. The findings of this study and ours underlines the importance of aligning our health communication messages and exercise recruitment strategies with expectations [18].
The data depicted in Fig. 1 should be considered in designing future exercise programs for people with PD. At least with regard to this cohort, a group class, led by an instructor, that lasts less than 30 minutes, and allows spouses or significant others to be included, may lead to improved compliance.
Barriers to exercise
Unlike the prior study by Ellis et al., our study did not identify fear of falling, lack of time, and low-outcome expectation as major barriers to exercise. Their cohort had more participants who had a history of falling (50% in the non-exercise group) and perhaps even more balance and gait dysfunction and low-outcome expectation than our low-exercise group (28.1%) [11]. Another possible explanation for the different findings is that most subjects in our low-exercise group were still doing some exercise, and in fact, only 13 (12% of low-exercise group) were not exercising at all. Those who exercise even 1 or 2 hours per week may be noticing benefits, and therefore may not identify low-outcome expectation as a barrier. In the Ellis et al. study, “exercisers” were defined differently, and were compared to “non-exercisers” rather than “low exercisers,” which might account for differences in the results. High-exercisers in our study were also significantly more likely to still be employed, 36.7% versus 18.9% of low-exercisers (
We recognize the limitations of the study include use of self-reported data and lack of objective measures of disease severity such as UPDRS and Hoehn and Yahr staging, non-motor symptoms of mood, fatigue, and sleep, exercise habits, and exact time spent exercising. Since this is a cross-sectional study, the conclusions are merely observational. While there were similar rates of PD patients with a disease duration of >5 years as seen in Table 1, disease duration was also not precisely accounted for in the interpretation of these findings. We acknowledge that we did not use a validated survey to assess exercise barriers, but such a survey specific to the PD population does not exist. Including a validated survey such as the “Self-Efficacy for Exercise Scale” could have been useful in assessing the reliability of our data, but in order to reduce the time to complete the survey we did not include this [19]. Another limitation is that subjects were categorized based on a 3-hour exercise cut-off, while AHA guidelines use 150 minutes. Subjects were being asked to estimate their average amount of exercise per week using recall. They were not completing diaries or calculating actual minutes. Since we did not expect that responders would be specific enough to recall to the half hour, we tried to make it easier by using 3 hours as a general cut-off. In categorizing it this way we recognize that we falsely categorize those who are exercising between 2.5–3 hours as “low-exercisers,” although we expect this is a small group. The fact that hours are estimated rather than calculated with diaries or actigraphy is also a limitation. While assumptions are made about differences in intensity of exercise between groups, these were generalizations about types of exercise, and intensity was not actually assessed. It should be acknowledged that actual behavior is affected by many variables like heredity, overall health, lifestyle, and socioeconomic class which is not being assessed in its entirety in this study. The purpose of this study was to gather data from this unique patient population regarding general exercise behavior, perceptions, and preferences, and draw conclusions on factors influencing exercise adherence. Another limitation of our study is that we did not inquire about apathy from our participants, their caregivers, or their neurologists, which could be another variable particular to PD that could affect exercise perceptions and behavior.
Conclusions
Given the overwhelming evidence of the benefits of exercise in PD and the vital role physicians play in motivating behavior change, we believe our findings represent essential knowledge for the management of patients with PD. In our study, we found that high-exercisers with PD were more likely to engage in multi-modal exercise regimens and believed in the impact of exercise on their motor symptoms, mood, and sleep. Low-exercisers, however, needed more motivation to overcome perceived barriers including having no one to exercise with, fatigue, and depression. This information can guide the design of future exercise interventions and studies for PD patients that aim to increase compliance.
CONFLICTS OF INTEREST
Dr. Afshari and Amy Yang have nothing to disclose. Dr. Bega has served as a consultant for Teva Pharmaceuticals and Cynapsus Therapeutics, Inc. He serves on the speaker’s bureau for Acadia Pharmaceuticals, Inc. He has received grant support from the National Parkinson Foundation.
Footnotes
ACKNOWLEDGMENTS
The authors have no acknowledgements to disclose.
