Abstract
BACKGROUND:
Invariant natural killer T (iNKT) cells are an immune subset that purportedly link the adaptive and the innate arms of the immune system. Importantly, iNKT cells contribute to anti-cancer immunity in different types of hematological and solid malignancies by secreting pro-inflammatory cytokines. Therefore, using such cells in treating different type of tumors would be an ideal candidate for cancer immunotherapy.
OBJECTIVE:
To assess the prognostic effect of iNKT cells across different types of solid and hematological tumors.
METHODS:
In systematic review and meta-analysis, articles assessed the prognostic effect of iNKT cells were systemically searched using the scientific databases including Google Scholar, ScienceDirect, PubMed, Cochrane Central, and Scopus.
RESULTS:
Strikingly, the analysis showed the positive impact of intratumoral or circulating iNKT cells on the survival rate in patients with all studied tumors with overall effect of a pooled hazard ratio of 0.89 (95% CI 0.81 to 0.98;
CONCLUSIONS:
Taken together, this study would present a new insight into the impact of iNKT cells correlate with caner patients’ survival rate and how such cells would be used as a therapeutic target in these patients.
Introduction
Invariant natural killer T (iNKT) cell is a unique population of lymphocytes with shared properties of natural killer cells (NK) and T lymphocytes [1]. iNKT cells are distinct from conventional
iNKT cells known to secrete plethora of cytokines that play a crucial role in inflammatory diseases and maintain immune homeostasis [3]. iNKT cells have a well-known role in anti-tumor immunity. For example, iNKT cells are remodeling the tumor microenvironment through producing cytokines such as IFN-
Importantly, a decrease of iNKT cell counts are associated with worse outcomes in squamous carcinoma and chronic lymphocytic leukemia (CLL), possibly as a result of persistent activation by CLL cells that express CD1d [20, 21]. Notably, myeloma cells decrease CD1d expression as the disease progresses, hence iNKT cell frequency is inextricably linked to cancer progression [13, 15, 22, 23, 24]. Additionally, antigen-presenting cells (APCs) loaded with
Therefore, in this systematic review and meta-analysis, we aimed to assess the prognostic effect of iNKT cells across different types of solid and hematological tumors. Hence, iNKT cells were correlated with patient survival rates. We then explored the factors related to iNKT cells variation in tumors, such as gender, smoking status, number of intratumoral or peripheral iNKT cells and combination therapy with IFN-
Materials and methods
Search strategy and selection criteria
We systematically searched the scientific databases including Google Scholar, ScienceDirect, PubMed, Cochrane Central, and Scopus to select potential studies for this systematic review and meta-analysis. Different key words were used to identify the relevant articles including invariant natural killer T cells (iNKT), clinical application of iNKT, iNKT in immunotherapy as well as iNKT cells in cancer prognosis. Additionally, we were looking in the relevant database for a combination of iNKT cells with cancer key words such as tumor, malignancy, carcinoma, adenocarcinoma, squamous cell carcinoma, sarcoma, myeloma, lymphoma and leukemia. The potential 1017 articles related to iNKT cells and cancer were found in the time span from (2000–2023).
Inclusion and exclusion criteria
In the systematic review and meta-analysis, all studies provided information about association of iNKT cells frequencies either in periphery or at tumor sites and their relationship to cancer prognosis were included. Studies included in this analysis must been published as an original and primary article and assess human subjects as well as published in English language. Articles evaluating the association of either tumor infiltrating iNKT cells or circulating iNKT cells with clinical features of cancer patients such as overall survival (OS), disease free survival (DFS), recurrence free survival (RFS) and relapse free survival (RFS) were included. The eligibility of each study was assessed independently by at least two investigators (AA, FA, RAA, RTA, SA, ZA). Animal studies, in vitro studies using cell lines, interventional studies, using engineered iNKT cells as cellular therapy in cancer, reports published as conference abstracts and letters, and studies reported insufficient data of survival rates were excluded.
Data extraction and assessment
Newcastle-ottawa quality assessment
Newcastle-ottawa quality assessment
The data from included studies was extracted independently by two investigators (RMA, AA, FA, RAA, RTA, SA, ZA). Both of two investigators assessed each study according to the authors’ names, year of publication, sample size, type of study, type of cancer, and iNKT identification (in peripheral blood or intratumoral tissue). The Newcastle-Ottawa quality assessment scale (NOS) was used to assess each study included in this analysis individually by two investigators. The scored of total 8 studies ranged from good quality to fair quality, according to the evaluation criteria detailed in Table 1.
All statistical analysis and graphical representation were analysed and generated using RevMan software version 5.4 version (Cochrane Collaboration, Oxford, United Kingdom). The hazard ratio (HR) and its 95% confidence interval (CI) were extracted from the selected studies in the meta-analysis to assess the association of iNKT cells and patients’ prognosis. A fixed model effect was used to sum up all outcomes from the selected reports. Standard of error (SE) were calculated from given HR and 95% CI. Further, heterogeneity between studies was calculated, where I2 value of 25%, 50% and 75% corresponded to low, moderate, and high degree of heterogeneity.
Results
Study characteristics
Flow chart of searching and study selection (PRISMA).
Initially, a total 1017 relevant articles were systematically identified through the scientific database, however 897 articles were excluded on the first pass based on the title and abstract (Fig. 1). The remaining 120 articles were given a more detailed assessment with evaluating association of iNKT cells with cancer prognosis. Following that, 81 studies were comprehensively assessed against inclusion criteria, however, only 14 articles were eligible studies and met the inclusion criteria. Yet, 5 studies out of 14 eligible articles were excluded as these studies did not report sufficient data to estimate the hazard ratio. Moreover, one study was assessing the NK/iNKT ratio. The final 8 datasets were included in the systematic review and meta-analysis encompassed different types of malignancies, including colorectal cancer, hepatocellular carcinoma, acute myeloid leukemia, head and neck squamous cell carcinoma, neuroblastoma, upper gastrointestinal cancers, and lung cancers.
The basic characteristics for studies included in meta-analysis
The basic characteristics for studies included in meta-analysis
All studies included in the meta-analysis detailed in Table 2 and classified based on of the date of publication from the oldest to newest, type of cancer and
Forest plot of overall survival sorted by year of study.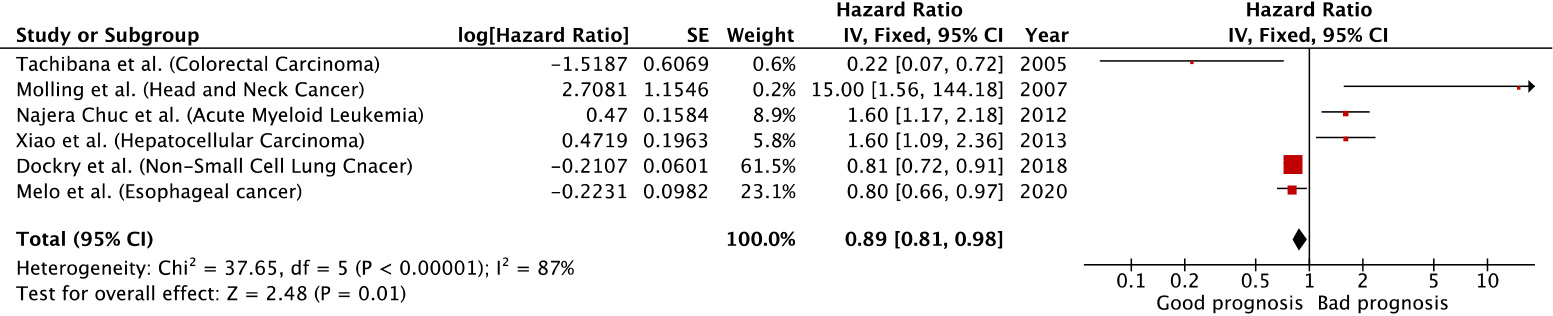
All the studies reported a significant impact of tumor infiltrating or circulating iNKT cells in patients with distinct types of malignancies on overall survival (Table 2). Of note, high density of infiltrating iNKT cells was found to be associated with an improved overall survival in patients with non-small lung cancer, oesophageal cancer and colorectal cancer compared to hepatocellular carcinoma, acute myeloid leukaemia and head and neck squamous cell carcinoma (Fig. 2).
Funnel plot to detect the presence of publication bias in the meta-analysis of overall survival.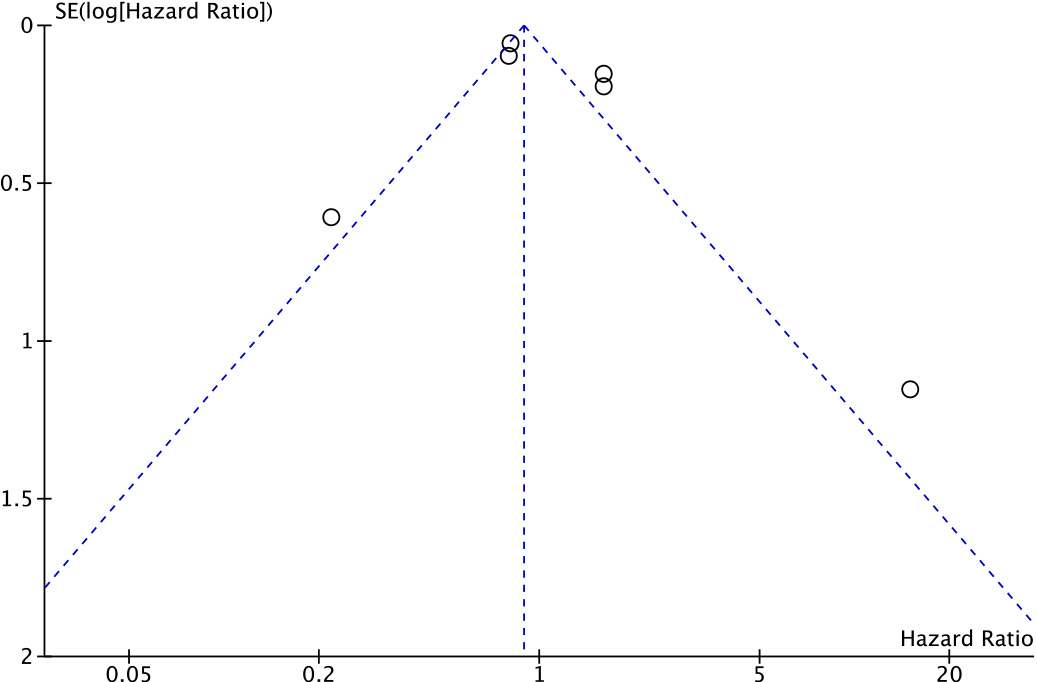
Indeed, the forest plot evaluating the hazard ratio in all studied tumors showed that the positive effect of iNKT cells on the survival rate with a pooled hazard ratio of 0.89 (95% CI 0.81 to 0.98;
Forest plot of recurrence free survival sorted by year of study.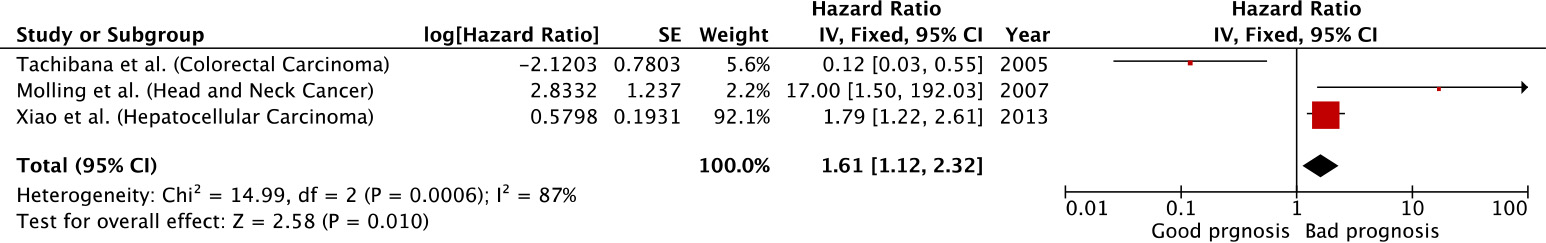
Funnel plot to detect the presence of publication bias in the meta-analysis of recurrence free survival.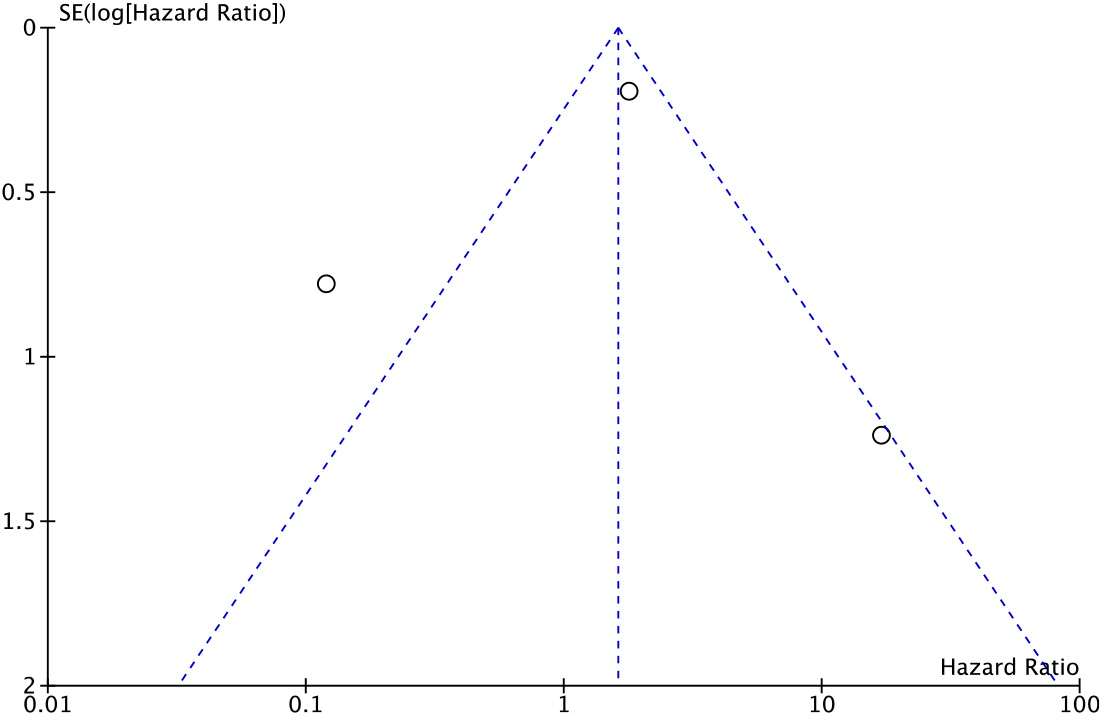
The recurrence-free survival (RFS) was reported only in three studies which had a negatively correlation with hazard ratio of 1.61 (95% CI 1.12 to 2.32) and
Subgroup analysis of iNKT cells impact on different types of cancer
Subgroup analysis of iNKT cells impact on different types of cancer
Several factors might have a potential effect on iNKT cells frequencies within tumor microenvironment. For example, male patients with non-small cell lung carcinoma (NSCLC) had high expression of CD1d molecules which associated with significantly improved of overall survival compared to female patients with
Interferon
The systematic review and meta-analysis were set out to assess the prognostic effect of iNKT cells across different types of solid and hematological tumors and correlate it with patients’ overall survival (OS).This study suggested that iNKT cells have a positive impact on the overall survival rate in different types of cancer including colorectal cancer, oesophageal cancer and lung cancer. This finding is supported by a number of clinical trials showed the potency of iNKT cells to be used as immunotherapeutic agent by increasing the overall survival rate and enhancing anti-tumor activity [31, 32, 33, 34, 35, 36]. For example, activating iNKT cells by administrating
However, combination therapy of administration of
In line with our observation that iNKT had different impact according to types of cancer, many studies demonstrated the influences of these cells depends on the site of cancer. For instance, there was an increase in peripheral iNKT cells number in benign ovarian cancer compared to advanced stage of ovarian cancer [38]. However, intratumoral iNKT cells showed an increase number compared to peripheral iNKT cells in the same cancer patients [38]. Therefore, the overall survival rate or recurrence-free survival may depend on the methods of iNKT cells detection and whether such cell was detected at tumor site or periphery. Having said that, the studies included in this meta-analysis were using different detection methods at different sites which might affect the consistency and accuracy of the study.
In this meta-analysis, the methods of detection varied between immunohistochemistry, real time polymerase chain reaction (RT-PCR) and flow cytometry which might impact on the overall effect. Importantly, different detection techniques would have different sensitivity and specificity. For example, RT-PCR is considered a gold stander for detection a certain type of cell or marker [39]. However, a recent study has been conducted comparing the accuracy of flow cytometry and RT-PCR in children with acute lymphoplastic leukemia [40]. Interestingly, the study showed the feasibility of both methods to be used in diagnosis as well as disease mentoring with no noticeable differences [40].
Other factor might have a noted impact on iNKT cells functionality in tumor microenvironment is their response to either endogenous or exogenous glycolipids such as
To our knowledge, this meta-analysis is the first study to demonstrate the prognostic impact of iNKT cells across different types of both hematological and solid tumors. However, there was a number of limitations associated with this study. First, the number of the studies that have been included and have met our criteria was limited which affect the overall effect and accuracy of this study. Notably, this study was using only observational study where it would be useful to compare the impact of iNKT cells on both observational and interventional studies. However, in all clinical trials were searching, there was a lack of information which limited the use of these studies. More meta-analysis should be done to evaluated different factors might affect the influence of iNKT cells in different sort of cancers.
In conclusion, either circulating or tumor infiltrating iNKT cells have been linked to improved overall survival rate in patients suffering from invasive malignancies such as NSCLC and hepatocellular carcinoma. Therefore, iNKT cells have been found to be a perfect candidate for cancer immunotherapy. However, a number of questions are needed to be answered in order to fully evaluated the use of such cells as a new treatment that might improve the clinical outcomes of cancer patients.
Footnotes
Author contributions
Conception: RMA.
Interpretation or analysis of data: All authors contributed to the interpretation or analysis of data Preparation of the manuscript: All authors contributed to preparation of the manuscript.
Revision for important intellectual content: RMA, NA, YA and HE.
Supervision: RMA.
