Abstract
BACKGROUND:
Pyruvate kinase M2 (PKM2) was overexpressed in many cancers, and high PKM2 expression was related with poor prognosis and chemoresistance.
OBJECTIVE:
We investigated the expression of PKM2 in breast cancer and analyzed the relation of PKM2 expression with chemotherapy resistance to the neoadjuvant chemotherapy (NAC). We also investigated whether PKM2 could reverse chemoresistance in breast cancer cells
METHODS:
Immunohistochemistry (IHC) was performed in 130 surgical resected breast cancer tissues. 78 core needle biopsies were collected from breast cancer patients before neoadjuvant chemotherapy. The relation of PKM2 expression and multi-drug resistance to NAC was compared. The effect of PKM2 silencing or overexpression on Doxorubicin (DOX) sensitivity in the MCF-7 cells
RESULTS:
PKM2 was intensively expressed in breast cancer tissues compared to adjacent normal tissues. In addition, high expression of PKM2 was associated with poor prognosis in breast cancer patients. The NAC patients with high PKM2 expression had short survival. PKM2 was an independent prognostic predictor for surgical resected breast cancer and NAC patients. High PKM2 expression was correlated with neoadjuvant treatment resistance. High PKM2 expression significantly distinguished chemoresistant patients from chemosensitive patients.
CONCLUSION:
PKM2 expression was associated with chemoresistance of breast cancers, and could be used to predict the chemosensitivity. Furthermore, targeting PKM2 could reverse chemoresistance, which provides an effective treatment methods for patients with breast cancer.
Introduction
Chemotherapy for primary breast cancer is frequently given neoadjuvantly to reduce tumor size with the aim of avoiding mastectomy. Although the majority of patients receiving neoadjuvant therapy achieve a clinical response to chemotherapy, only a minority achieve a pathological complete response, and eventually develop chemoresistance despite the on-going treatment, rendering reduced effectiveness of chemotherapeutic agents [1]. Clinical observations have shown that once tumors become resistant to a certain drug in chemotherapy, they will rapidly acquire tolerance to other drugs, suggesting there are mechanisms involved in inducing multi-chemoresistance [2]. Therefore, better understanding of the molecular mechanism of chemotherapy resistance is urgently needed for effective and individualized chemotherapies, and to establish a reliable method for predicting and overcoming the chemoresistance.
Pyruvate kinase is an enzyme that functions in the glycolytic pathway and catalyzes the last, rate-limiting step of glycolysis by converting phosphoenolpyruvate and ADP to pyruvate and ATP [3]. Of the four known isoforms, the muscle-type pyruvate kinase (PKM) gene is expressed ubiquitously and capable of producing two mRNA products through alternative use of exon 9 (PKM1) or exon 10 (PKM2) [4]. While normally PKM1 is present in adult cells, PKM2 is expressed abundantly in embryogenic tissues. During tumorigenesis, however, a major isoform switch occurs that replaces PKM1 with PKM2. Pyruvate kinase M2 (PKM2) is a key glycolytic enzyme that regulates the Warburg effect and is necessary for tumor growth. However, how to target PKM2 in cancer treatment is not conclusive, since both inhibition and activation of PKM2 have been shown to suppress cancer cell growth [5]. This is at least partially due to the fact that in cancer cells, PKM2 can exist as either a tetramer with higher activities or a dimer with lower activities.
PKM2 can also translocate to nucleus and exerts both kinase and non-kinase activities [5]. However, its role in chemoresistance has not been fully elucidated. At present, a few studies on the relationships between PKM2 and cell sensitivity to chemotherapy have been carried out. Fukuda et al. [6] reported that PKM2 expression is associated with esophageal squamous cell carcinoma chemoresistance, and PKM2 inhibition can restore cisplatin sensitivity by inactivating PPP. Similar results were showed in human non-small cell lung cancer (NSCLC) cells [7] and ovarian cancer cells [8]. Shin et al. [9] reported that PKM2 expression increased significantly in 5-fluorouracil (5-FU)-resistant colon cancer cells, but Yoo et al. [10] reported that there was no significant relevance between the expression of PKM2 and resistance to 5-FU. Recent research has indicated that PKM2 upregulation promotes chemosensitivity in colorectal cancer [12]. However, the clinical significance of PKM2 expression in breast cancer and the relation of PKM2 expression with chemosensitvity in breast cancer is currently unknown.
In this study, we detected PKM2 expression in breast cancers and breast cancers before neoadjuvant chemotherapy (NAC) and analyzed the relation of PKM2 expression with clinical data, chemoresistance and chemosensitivity to chemotherapeutic drugs. Using DOX-resistant or sensitive breast cancer cells, we investigated the effect of PKM2 in regulating DOX sensitivity or resistance in breast cancer cells
Materials and methods
Cell culture
The human breast cancer cell line MCF-7 (MCF-7
Patient samples
Breast cancer samples were obtained from Breast disease Center, the affiliated Hospital of Qingdao University. In all, 130 surgical resected tumors and 78 core needle biopsies of breast cancer before neoadjuvant chemotherapy (NAC) were collected from Oct. 2011 to Jan. 2013 and Jan. 2011 to Dec. 2013, respectively. The patients were followed up for 1–106 months and 1–102 months (median follow-up are 64 months and 59 months). Among the 130 tumor samples, there are 51 corresponding adjacent normal tissues. Pathological diagnosis, as well as ER, PR, and HER2 status, were verified by two pathologists independently. All human samples were collected with informed consents from the donors according to the International Ethical Guidelines for Biomedical Research Involving Human Subjects (CIOMS). The study was performed after approval by the institutional review board (IRB) of the affiliated Hospital of Qingdao University. Written informed consent was obtained from each individual or patient.
Immunohistochemistry
Immunohistochemistry (IHC) for PKM2 was performed according to the standard protocol. The IHC score, H-score, or PKM2 score, were determined by combining the percentage of positively stained tumor cells and the staining intensity of positively stained tumor cells. The staining intensity was graded as follows: 0, no staining; 1, weak staining (light yellow); 2, moderate staining (yellow–brown); 3, strong staining (brown). The percentage of cells at each staining intensity level is calculated, and finally, an H-score is assigned using the following formula: [
Lentiviral vector-mediated downexpression of PKM2
PKM2-specific shRNAs originate from the “MISSION shRNA Library” designed and developed at BioLink Biotechnology (Shanghai City, P.R. China). Two PKM2 hairpins (NM_182471.1-1706s1c1-#2 and NM_182471.1-1493s1c1-#4) that showed high efficacy knock-down were selected. Short hairpin RNAs (shRNA) of PKM2 shRNAs were inserted into pLenR-GPH vector (BioLink Biotechnology). Lentiviruses were generated from 293 T cells according to the protocol of Single Oligonucleotide RNAi Technology for Gene Silencing. Stable MCF-7 cells (MCF-7
Lentiviral vector-mediated overexpression of PKM2
EGFP-encoding lentiviral constructs for PKM2 overexpression were manufactured by Sunbio Medical Biotechnology Co., Ltd. (Shanghai City, P.R. China). The cDNA sequence for human PKM2 was cloned into XbaI and BamHI restriction sites of pLenO-GTP vector. Three helper plasmids pMDLg/pRRE, pRSV-REV, and pCMV-VSV-G were cotransfected into 293 T cells (
MTT assay
The MCF-7
Colony formation assay
The stable Lv-PKM2 transfected MCF-7
Western blot assay
The separation of cytoplasmic fractions was performed using the PARIS Kit (Life Technologies) according to the manufacturer’s instructions. Extracted proteins were separated by SDS-PAGE and transferred to a PVDF membrane. The membrane was blocked with 5% non-fat milk and incubated with primary antibodies for PKM2 (CST, 1:200) and a-Turbulin (Beyotime, 1:1000).
PKM2 upregulation indicates worse prognosis in patients with breast cancer. A, Representative immunohistochemistry images of PKM2 expression in the breast cancer (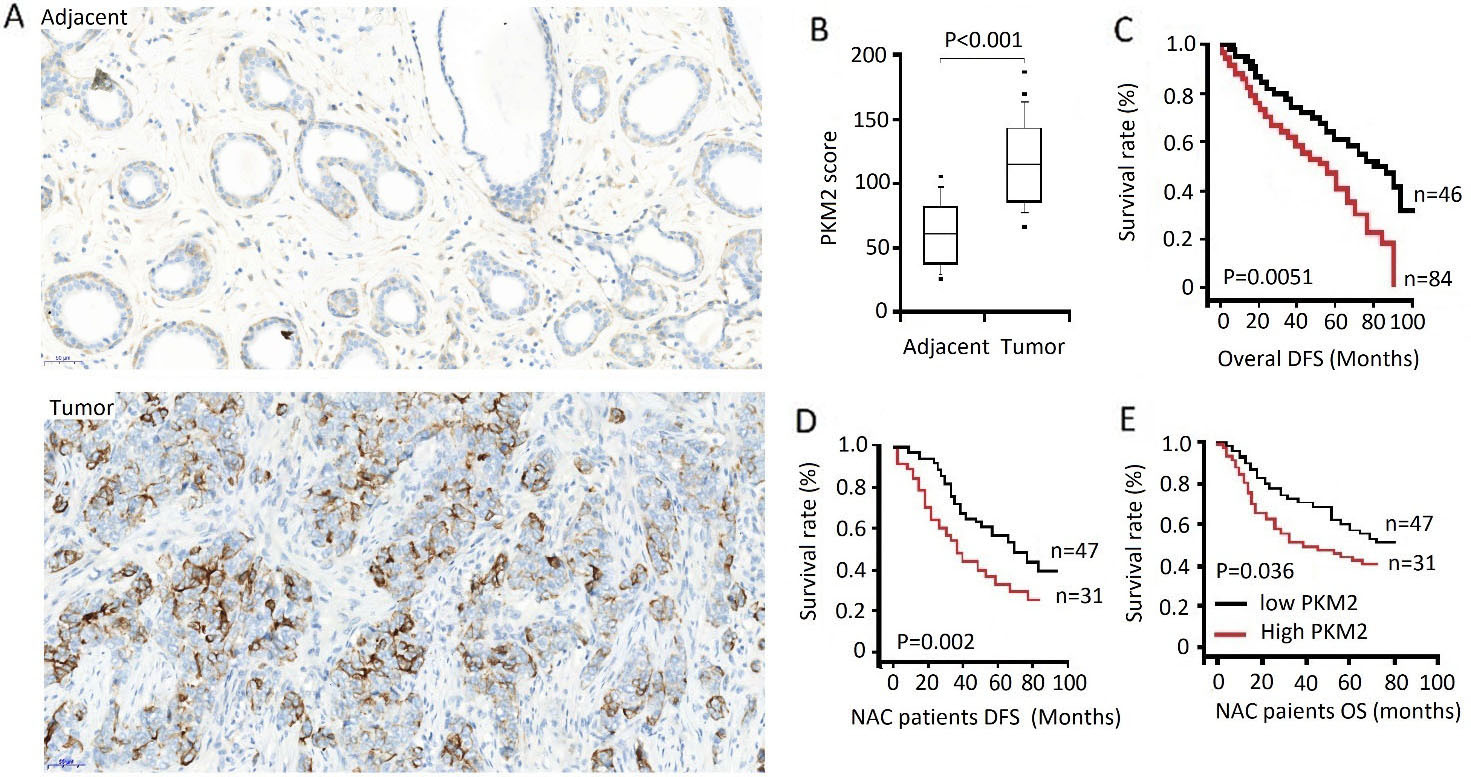
Female BALB/c nude mice (5–6 weeks of age, 16–18 g) were obtained from National Rodent Shanghai Experimental Branch Center, Chinese Academy of Sciences (Shanghai, China). All experimental procedures involving animals were conducted in accordance with the institutional guidelines by the Affiliated hospital of Qingdao University. BALB/c mice (
Statistical analysis
Unpaired two-sided Student’s t test and one-way ANOVA was used to compare cell viability and colony formation and tumor volume with different treatments, and post hoc tests were used to test difference between groups. Chi-square test was used to analyze the relationship between PKM2 expression and clinicopathological status. Kaplan-Meier method was for survival analysis. Value of
Correlations of PKM2 expression with clinicopathological status in 130 cases of patients with breast cancer
Correlations of PKM2 expression with clinicopathological status in 130 cases of patients with breast cancer
Clinical significance of PKM2 expression in surgical excised breast cancer
To further validate the expression of PKM2 in breast cancers, immunohistochemistry (IHC) was performed in 130 surgical excised breast cancer tissues and 51 cases of the adjacent normal tissues. We found that PKM2 was intensively expressed breast cancer tissues compared to the adjacent normal tissues (Fig. 1A). As shown in Fig. 1B, PKM2 score was higher in the breast cancer tissues compared to the adjacent normal tissues (
Multivariate Cox proportional hazard analysis of 130 cases of breast cancer
Multivariate Cox proportional hazard analysis of 130 cases of breast cancer
Multivariate Cox proportional hazard analysis of 78 NAC patients
Chemoresistance was defined as stable disease (SD) or progressive disease (PD) after NAC treatment, while chemosensitive patients had a completed response (CR) or partial response (PR) according to RECIST 1.16 [12]. To further validate the correlation of PKM2 expression with breast cancer chemoresistance, we collected 78 core needle biopsies from breast cancer patients before neoadjuvant chemotherapy, which were then treated with platinum-based drugs, Taxanes, and Doxorubicin. Our clinical studies discovered that patients with high PKM2 expression (Fig. 2A) and high PKM2 score (Fig. 2B) has poor outcome to neoadjuvant treatment in the breast cancer patients. We also compared the relation between PKM2 expression and clinical significance in 78 NAC patients, and found that high PKM2 expression was associated with high
PKM2 upregulation indicates worse neoadjuvant chemotherapy outcome. A, Representative immunohistochemical images showed that PKM2 level was highest expressed in PD (progress disease) tumors (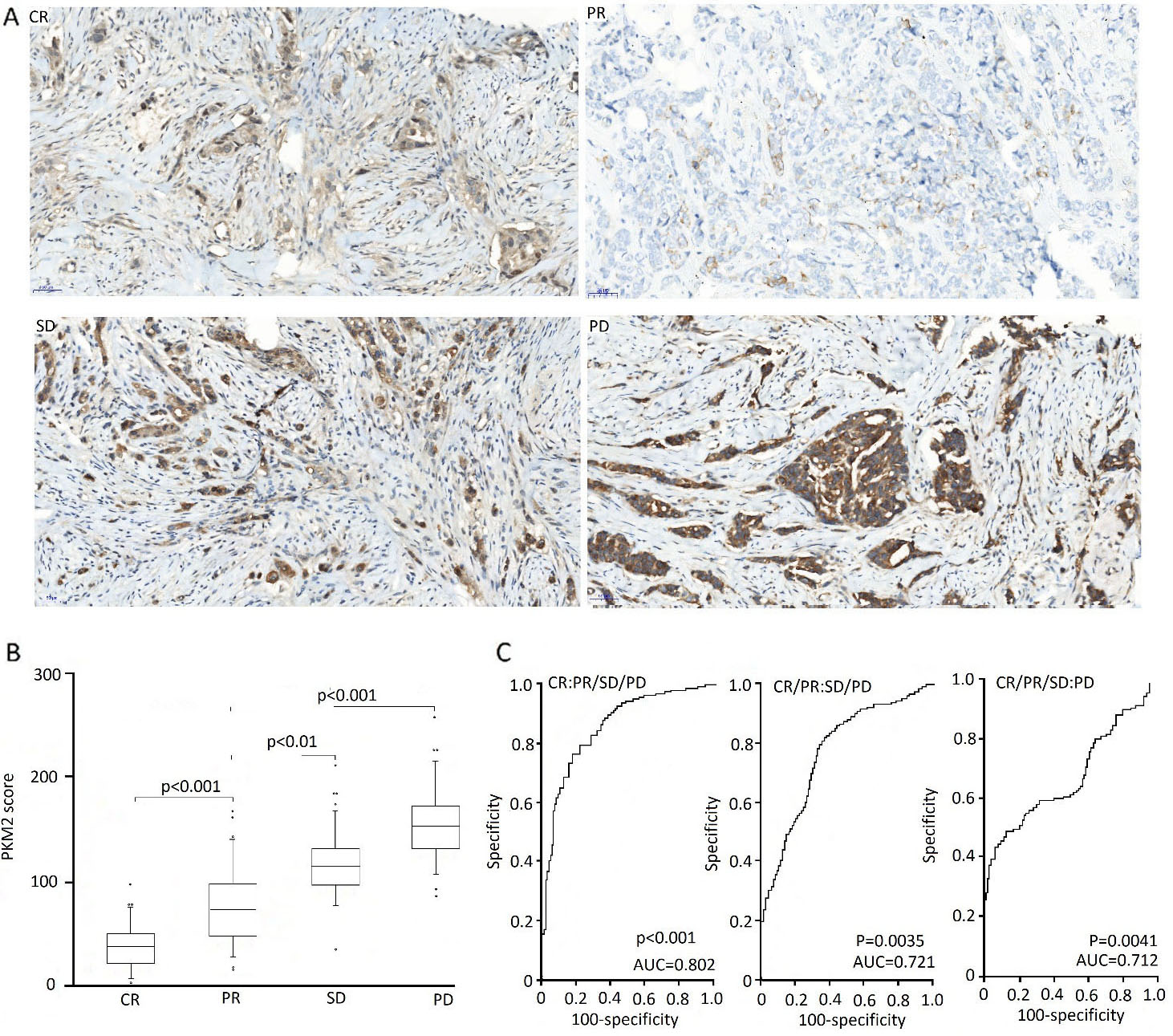
Correlations of PKM2 expression with clinicopathological status in 78 breast cancer patients with Neoadjuvant chemotherapy
To explore the common mechanisms that promote the chemoresistance in breast cancers, we generated DOX-resistant MCF-7 cell line (MCF-7
PKM2 regulates the chemosensitivity of breast cancer cells to DOX in vitro. A, PKM2 protein levels in MCF-7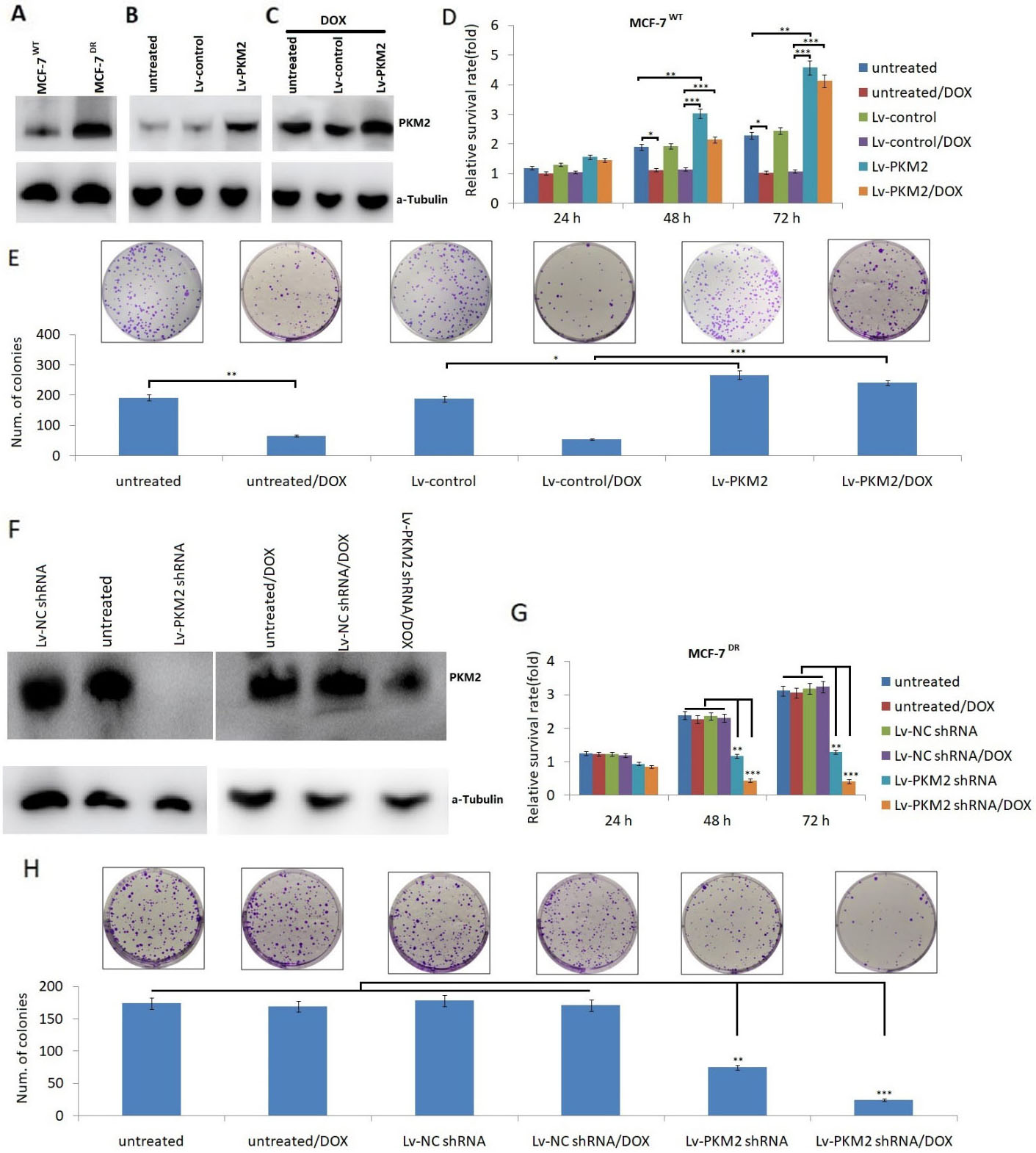
The Lv-PKM2 shRNA or Lv-scrambled shRNA (Lv-NC shRNA) were transfected MCF-7
PKM2 knockdown increases the sensitivity of breast cancer cells to chemotherapies in vivo
To determine whether the effect of targeting PKM2 on chemosensitivity in vitro also extended to tumors growing in vivo, we injected female BALB/c mice with 5
PKM2 expression influences chemosensitivity of MCF-7 breast cancer cells in vivo. MCF-7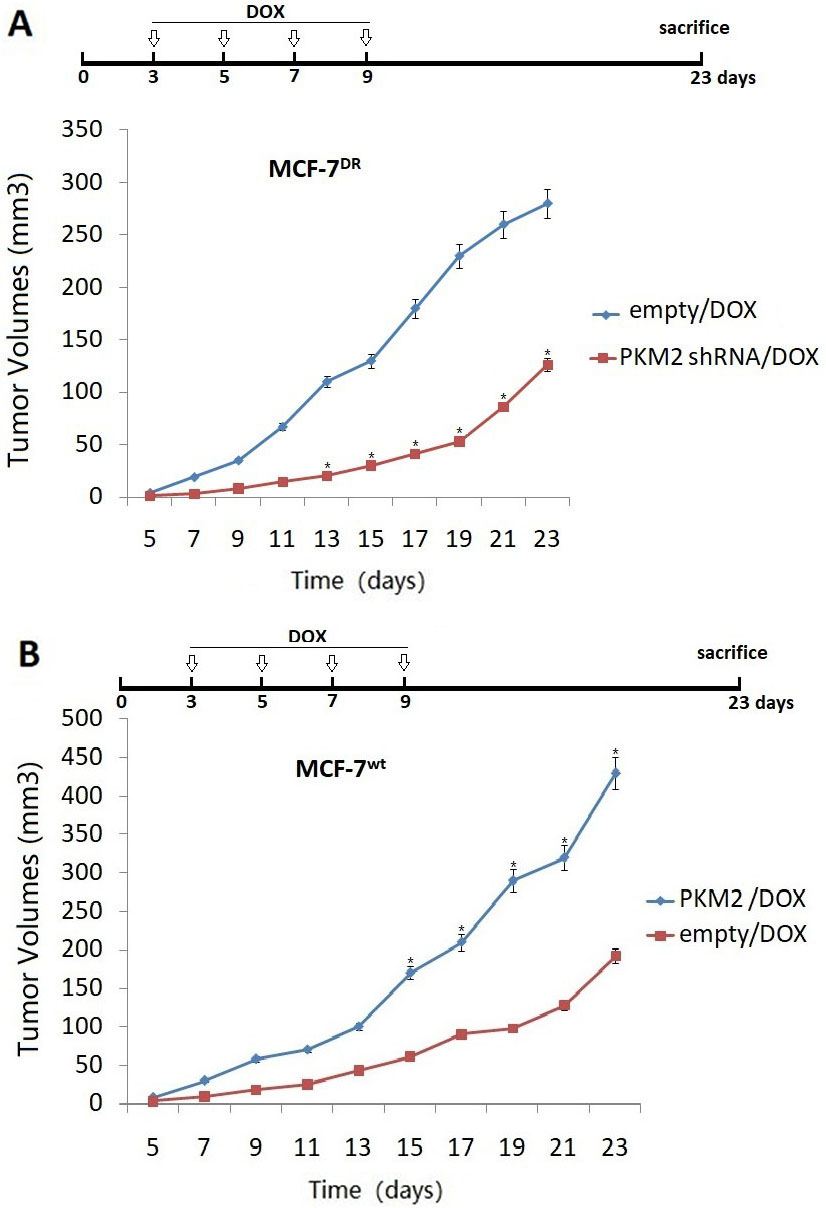
PKM2 was overexpressed in intrahepatic cholangiocarcinoma [13], PDAC [14], gallbladder cancer [15], lung adenocarcinoma [16], and higher PKM2 expression is associated with tumor progression and poor prognosis [13, 14, 15, 16]. In the present study, we found that PKM2 is upregulated breast cancer tissues compared with that in normal breast tissues. Moreover, PKM2 expression is significantly associated with poor progression in patients with breast cancer. Higher PKM2 expression correlated with a shorter survival time, indicating that PKM2 plays an important role in breast cancer progression. Furthermore, higher PKM2 expression was an independent prognostic indicator of shorter survival in breast cancer patients. These findings suggested that lower expression of PKM2 would provide a selective advantage in prognosis for breast cancer patients.
Neoadjuvant chemotherapy (NAC) refers to administration of chemotherapeutic agents before tumor resection, with purpose of downstaging locally advanced breast cancer to an operable tumor, as well as eradicating occult distant metastases [17, 18]. However, a subset of patients might not respond to neoadjuvant chemotherapy, possibly due to intrinsic chemoresistance, resulting in compromise of the treatment efficacy and affecting the success of following surgery [19]. Identification of potential biomarkers to predict the response to NAC might help to guide the chemotherapeutic regimen selection.
PKM2 is strongly upregulated in bladder cancer, and contributes to the cisplatin resistance [20]. PKM2 overexpression is also related chemoresistance in colorectal cancer [21] and multiple myeloma cell [22]. In this study, we demonstrated that PKM2 expression was significantly upregulated in chemoresistant breast cancer or cell lines. High PKM2 expression was correlated with significantly lower disease free survival (DFS) and overall survival (OS). Furthermore, higher PKM2 expression was related to the neoadjuvant chemotherapy resistance. These findings suggest that PKM2 may serve as potential biomarkers to predict chemosensitivity.
To further confirm whether PKM2 expression regulates the chemosensitivity of breast cancer cells to therapeutic drug, the PKM2 downexpressing MCF-7 cells and overexpresssing MCF-7 cells were treated with doxorubicin. As might be predicted from prior studies of doxorubicin, a remarkably decreased cell growth was observed in MCF-7
Conclusion
In conclusion, PKM2 is overexpressed in breast cancer and chemoresistant breast cancers. High PKM2 expression is related with poor prognosis and chemoresistance in patients with breast cancers. Monitoring PKM2 expression and targeting PKM2 may be utilized to predict chemotherapy response and reverse the chemoresistance of breast cancers. PKM2 may be as a useful biomarker and a potential therapeutic target to sensitize breast cancer to chemotherapies.
Footnotes
Author contributions
Conception: Yu Wang and Xingang Wang
Interpretation or analysis of data: Fengyun HaoHan Zhao and Xingang Wang
Preparation of the manuscript: Yu Wang and Xingang Wang
Revision for important intellectual content: Yu Wang and Xingang Wang
Supervision: Xingang Wang
