Abstract
BACKGROUND:
Precise recipient selection optimizes the prognosis of liver transplantation (LT) for hepatocellular carcinoma (HCC). Alpha-fetoprotein (AFP) is the most commonly used biomarker for diagnosis and prognosis of HCC in the clinical context. As a crucial molecule in methionine cycle, homocysteine (Hcy) level has been proved to be related to HCC progression and metastasis.
OBJECTIVE:
We aimed to explore the prognostic capacity of pre-transplant serum Hcy level in LT for HCC.
METHODS:
This study retrospectively enrolled 161 HCC patients who had underwent LT from donation after cardiac death (DCD) in the First Affiliated Hospital of Zhejiang University from 2015.01.01 to 2018.09.01. Pre-transplant serum Hcy level was incorporated into statistical analysis together with other clinical parameters and pathological features.
RESULTS:
From an overall perspective, significant difference was observed in Hcy level between recurrence (
CONCLUSION:
As a classic predictor in HCC prognosis, AFP performed well in our study cohort when combined with Milan criteria. Homocysteine was an effective prognostic biomarker in LT for AFP
Keywords
Introduction
Hepatocellular carcinoma (HCC) [1] is the most common liver cancer worldwide and accounts for majority of cancer-related death. LT is a decent curative option for HCC patients who have no indication for surgical resection though with limited tumor burden. Due to donor organ shortage, technical difficulties, complicated perioperative management and high tumor recurrence rate, the candidate selection for HCC-related LT should be carefully reviewed and optimized. Clinical indexes such as neutrophil-to-lymphocyte ratio, platelet-to-lymphocyte ratio, systemic immune-inflammation index, protein induced by vitamin K absence or antagonist II, as well as AFP showed certain predictive value for tumor recurrence after LT [2, 3, 4, 5, 6, 7, 8]. Thus, we decided to explore other clinical molecules to improve recipient selection before LT for HCC.
Methionine is a metabolic dependency of tumor-initiating cells. It has been reported that methionine cycle had an impact on the epigenetic state of cancer cells and ignited tumor initiation [9]. A previous study showed that switching gene expression of two crucial methionine adenosyltransferases, MAT1A to MAT2A (M1-M2 switch) promoted HCC invasion and metastasis [10]. Homocysteine (Hcy), a critical molecule in methionine cycle, folate metabolism and transsulfuration pathway, is routinely reviewed to evaluate the cardiovascular risk for patients. Liver is the key metabolic center for Hcy biosynthesis and metabolism. In fact, elevated Hcy level has been demonstrated to be related to HCC progression and metastasis [11, 12, 13]. However, the relationship between Hcy level and the outcomes of LT patients remains relatively vague. An in-depth analysis is therefore necessary to explicate the role of Hcy in the prognosis of LT patients.
In present study, we detected the Hcy level in the pre-transplant serum of LT recipients with HCC and carried out multiple factor analysis combining other important clinical features. The ultimate purpose is to disclose the predictive value of Hcy in HCC-related LT recipients and optimize the candidate selection criteria, as well as to provide potential treatment guidelines for them.
Material and methods
Patients and demographics
One hundred and sixty-one HCC patients who underwent LT from donation after cardiac death (DCD) in the First Affiliated Hospital of Zhejiang University from 2015.01.01 to 2018.09.01 were enrolled in this study. HCC was confirmed exclusively based on post-operative result. Pre-transplant factors including demographics, preoperative complications, preoperative serum level of alpha-fetoprotein (AFP,
Endpoint of follow-up was on 2019.09.30, the median follow-up time was 2.75 years (95% CI: [2.26–3.23]). In the 161 patients enrolled, 147 were male and 14 were female. Their ages ranged from 42 to 60 years old, with an average of 51 years old. The average length of survival was 1.83 years. One hundred and fifty-four cases of HCC were derived from HBV infection, 1 from HCV infection, 2 from alcoholic hepatitis and 4 from unknown reason (Table 1).
Demographic and clinical characteristics of enrolled patients with/without tumor recurrence
Demographic and clinical characteristics of enrolled patients with/without tumor recurrence
Note. HBV, hepatitis B virus; HCV, hepatitis C virus; ASH, alcoholic hepatitis; PHB, primary biliary cirrhosis; CVD, cardiovascular diseases; HP, hypertension; DM, diabetes; BMI, Body Mass Index; MELD, Model for end-stage liver disease; MC, Milan criteria; Total diameter, total tumor diameter; AFP, alpha fetal protein; CYC, cystatin; Cr, creatinine; Hcy, homocysteine; BUN, blood urea nitrogen; AG, albumin to globulin ratio; GFR, glomerular filtration rate; NLR, lymphocyte ratio; SII, systemic immune-inflammation index; ST, survival time; RFST, recurrence free survival time; MFT, median follow-up time.
The tumor recurrence-predicting capacity of AFP and Hcy in LT for HCC. A. Recipients with low pre-transplant serum AFP level (
ROC curve and Kaplan-Meier survival analysis of MA score in predicting tumor recurrence after LT. A. ROC curve for HCC recurrence of the MA score, the AUROC 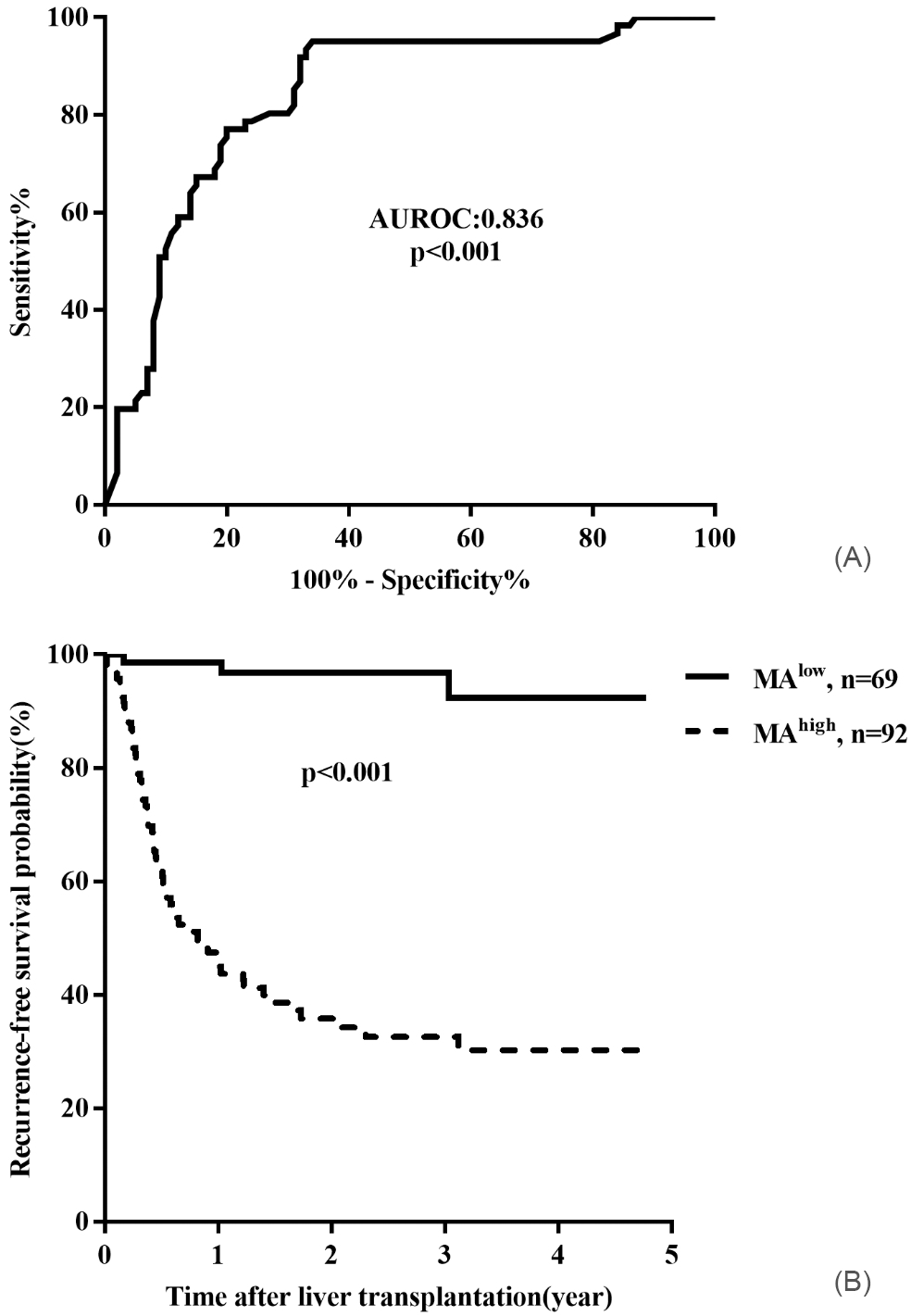
The procedures of this study were in accordance with the Helsinki Declaration. All livers were acquired from deceased donors strictly according to the guidelines of the China donation after citizen’s death. No donor organs were obtained from executed prisoners or other institutionalized persons. The study was approved by China Liver Transplantation Registry (CLTR), the only national registry in Mainland China, according to the Regulations on Human Organ Transplant and national legal requirements. Patient consents were obtained. The study protocol was also approved by the Human Ethics Committee of First Affiliated Hospital, Zhejiang University School of Medicine.
The results were analyzed by SPSS (Version 20.0, inc., Chicago, IL, USA). AUROC curve and Youden index were calculated for optimal cut-off value. Kaplan-Meier method was used for univariate analysis. Student’s
Results
Novel pre-operative tumor recurrence predicting score based on Milan criteria and serum AFP level
All characteristics shown in Table 1 were enrolled to evaluate their correlation with post-transplant tumor recurrence. Among them, pre-operative serum AFP level (
Cox regression analysis of the variables of recurrence-free survival in 161 patients with HCCs after LT
Cox regression analysis of the variables of recurrence-free survival in 161 patients with HCCs after LT
Note. HR, hazard ratio.
Cox regression analysis of the variables of recurrence-free survival in 77 patients with AFP
Note. HR, hazard ratio.
Hcy performed well in predicting post-transplant tumor recurrence of AFP
Then we carried out univariate analysis to reassess the correlation between post-LT tumor recurrence and potential risk variables by Cox regression. Eight variables including lnAFP, MC, tumor number, total tumor diameter, Hcy, Cr, NLR and SII were subsequently enrolled in multivariate Cox regression analysis, the results showed that lnAFP (
As we mentioned above, AFP is the most commonly used clinical biomarker which has strong correlation with the prognosis of HCC patients, we further divided all 161 patients into AFP
Combination of Hcy level and Milan criteria optimized selection of recipients with negative pre-transplant serum AFP level
As shown in Table 3, both Hcy level (
Combination of Hcy level and Milan criteria optimized selection of AFP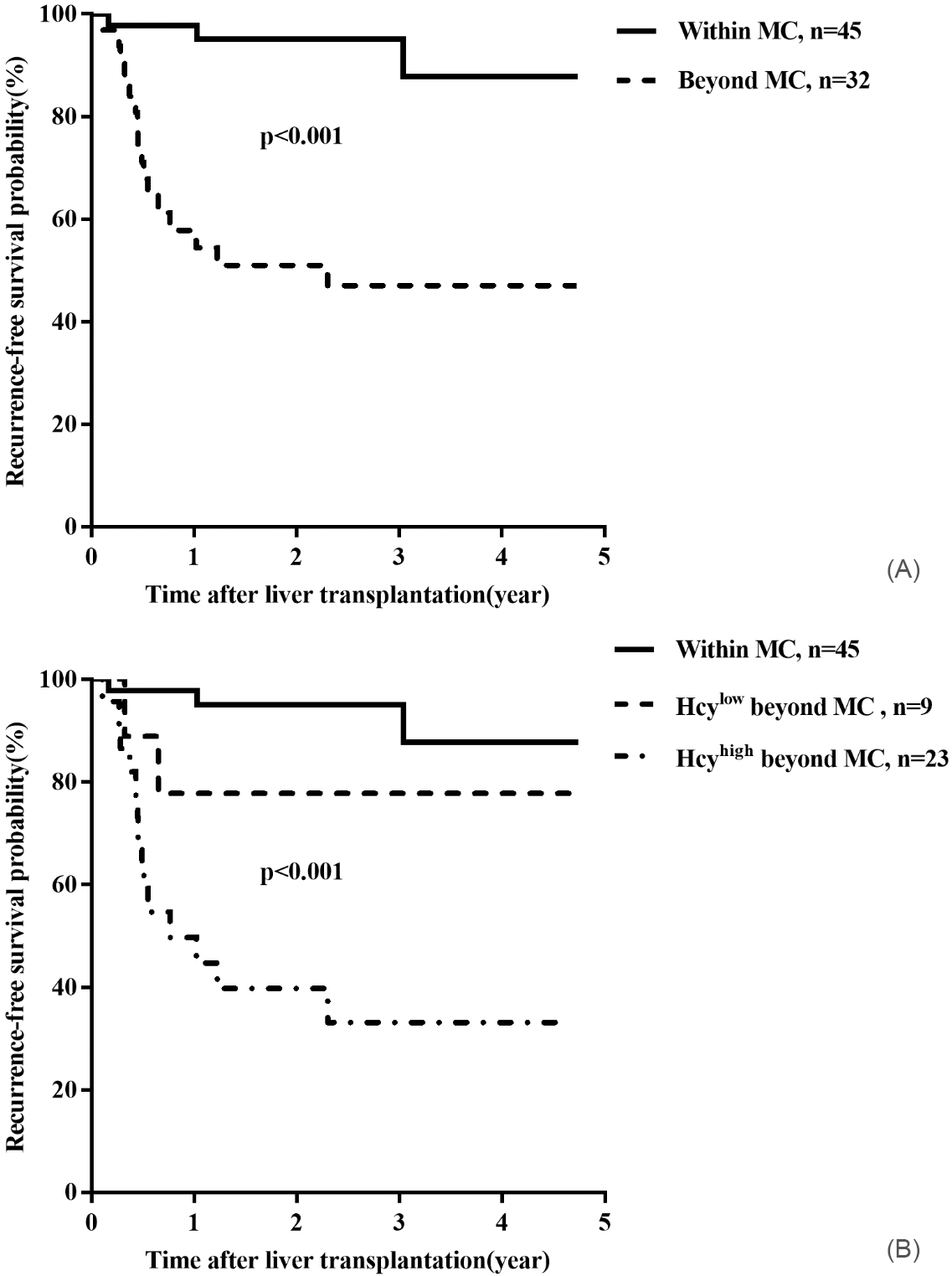
HCC accounts for the majority of liver cancer worldwide and the fourth-leading cause of cancer-related death [1, 14]. LT is an effective curative option for HCC patients with limited tumor burden and optimized recipient selection is of great significance for HCC patients to obtain favorable prognosis. Pre-transplant serum AFP level has been recognized to effectively predict tumor recurrence after LT for HCC patients though HCC recurrence were still observed in some AFP negative recipients [15]. In fact, single biomarker is far from enough to meet with the command of precise selection of LT recipients while multi-biomarker models can bridge the gap by serving as a more effective predictor for post-operative prognosis. Our results showed that pre-transplant serum Hcy level can be applied to distinguish AFP
In the past decade, several prognostic models were established to evaluated the post-transplant HCC recurrence risk for recipients with intent to optimize MC [16]. AFP is a surrogate marker of both tumor differentiation and vascular invasion. Accordingly, high AFP levels have been reported to be associated with high recurrence rates [17]. Thus, AFP was applied to construct predicting models in several researches [18]. In our research, the multivariate analysis showed that MC and lnAFP were independent risk factors for tumor recurrence. We further established a novel prognostic score name MA score which effectively predicting post-transplant HCC recurrence. The MA score is convenient and might be useful in clinical practice after multi-center validation and optimization.
The most significant finding in current article is the tumor-recurrence predicting capacity of homocysteine in certain HCC-related LT recipient group. Homocysteine is an important intermediate product of one-carbon metabolism, which encompasses folic acid and methionine cycle [19]. One-carbon units are essential substances for the proliferation and regeneration of cancer cells by influencing nucleotide synthesis and methylation pathways [20]. HCC is a highly malignant cancer and the needs for one-carbon units is extremely integrant. Previous study of our research team reported that genetic variations in one-carbon metabolism pathway genes of donor liver was associated with increased risk of HCC frecurrence [21]. Butler et al. reported that serum cystathionine, methionine, and S-adenosylmethionine but not HCY were associated with increased HCC risk (
We further demonstrated that in a special HCC-related LT recipient group, which was the AFP
We assumed that as a valid biomarker for SAM metabolism, abnormal elevation of Hcy level reflects increment in Hcy remethylation activity which results in stimulated methionine synthesis and reduced SAM level. This in turn increasing the HCC risk by triggering several tumor-promoting pathways. Previous study demonstrated that the production of SAM, which is the biological methyl donor essential to vast reactions within the cell, relies greatly on methionine adenosyltransferases (MATs) regulation [24]. Impaired biosynthesis of SAM in patients with HCC indicates aberrant M1-M2 switch which subsequently induces genomic instability [25], mitochondrial dysfunction and dysregulated metabolic pathways including RAS/ERK [26], IKK/NF-kB [27], PI3K/AKT [28] and LKB1/AMPK [29] and eventually leads to HCC development. A recent research reported that simultaneous downregulation of MAT1A enhanced osteopontin (OPN) expression which triggered ERK signaling and thereby promoted metastasis [10]. Thus, these findings suggested a promising anticancer treatment since the restoration of SAM level can inhibit stimulation of cancer-promoting signaling pathways and potentially reduce the tumor recurrence risk after LT for HCC recipients.
Molecules which play crucial roles in SAM and HCY regulation are considerable therapeutic targets. At present, there are two ongoing SAM-related clinical trials in HCC treatment. One of which (NCT03178929) is designed to investigate SAM treatment in HCC patients after radical treatment, where tumor recurrence is the endpoint while another (NCT02586285) aims to study the SAM treatment in HCC patients after curative treatment. Inspired by above researches, we believed that Hcy level might be a practical biomarker for peri-transplant management. It’s rational to proactively administer SAM to recipients with high Hcy level in order to decrease the post-transplant tumor recurrence risk. Our research team have also carried out animal experiments to validate our hypothesis.
In a nutshell, we revealed the predicting capacity of homocysteine in post-transplant tumor recurrence risk for HCC recipients and suggested potential novel therapeutic targets for those at high risk. Despite the encouraging results of our study, there are a few shortcomings which need to be improved: 1) limited sample size; 2) no multi-center validation as pre-transplant serum Hcy level is not routinely examined in other medical centers, we plan to generalize the detection of serum Hcy level test in the peri-operative examination and carry out multi-center validation in future; 3) this study focused on clinical phenomenon and further experimental evidence is required to support our hypothesis.
Conclusion
We innovatively came up with that homocysteine was a promising prognostic biomarker in LT for AFP
Footnotes
Acknowledgments
This work was supported by the National Major Scientific and Technological Special Project under Grant No. 2017ZX10203205; the State Key Program of National Natural Science Foundation of China under Grant No. 81930016; the National Natural Science Funds for Distinguished Young Scholar of China under Grant No. 81625003; Zhejiang Provincial Natural Science Foundation under Grant No. LQ19H160030; and Zhejiang Medical and Technological Program of China under Grant No. 2018263185.
