Abstract
BACKGROUND:
Increasing evidence have demonstrated that serum extracellular vesicle microRNAs (EV-miRNAs) are promising noninvasive biomarkers for various cancer types.
OBJECTIVE:
In this study, we aimed to investigate and evaluate the potential clinical significance of serum EV-miR-10b for acute myeloid leukemia (AML).
METHODS:
Blood samples were collected from a cohort of 95 de novo AML patients and 80 healthy individuals. Of all AML patients, 51 patients were considered as cytogenetic normal AML (CN-AML). Quantitative reverse-transcription polymerase chain reaction (qRT-PCR) was performed to measure the expression levels of serum EV-miR-10b.
RESULTS:
The extracellular vesicles we extracted from the serum samples were positive for EV/exosome markers including TSG101, CD63, Flotillin-1 and CD9. The expression levels of serum EV-miR-10b were significantly higher in AML/CN-AML patients than healthy controls. In addition, serum EV-miR-10b expression was strongly correlated with aggressive clinical characteristics. Moreover, receiver operating characteristic analysis showed serum EV-miR-10b yielded an area under the curve of 0.875, with 77.89% specificity and 82.50% sensitivity in identifying AML patients from normal controls. Furthermore, AML patients with higher serum EV-miR-10b expression had significantly shorter survival and serum EV-miR-10b was demonstrated to be an independent prognostic marker for overall survival in AML.
CONCLUSIONS:
Taken together, serum EV-miR-10b might serve as a promising biomarker for predicting the prognosis of AML.
Introduction
Acute myeloid leukemia (AML) is a cytogenetically, molecularly and clinically heterogeneous disease, resulting in aberrant proliferation of clonal neoplastic cells and maturation arrest [1, 2]. Approximately half of AML patients are considered as cytogenetic normal AML (CN-AML). CN-AML patients usually show a cytogenetic uniformity and offer new approaches to AML biomarker screening [3, 4]. Though most AML patients can achieve a complete remission after receiving standard induction chemotherapy, only few cases reach long-term survival [5, 6]. Deregulation of biomarkers that associate with unfavorable clinical outcome indicate the need for alternative or more aggressive therapeutic intervention at earlier time, which might contribute to improve the survival of AML patients. Therefore, it is urgently needed to identify effective and reliable biomarkers for predicting the prognosis of AML.
MicroRNAs (miRNAs) are a class of small (19–25 nucleotide), noncoding RNA that regulate gene expression at the posttranscriptional level, and involve in a variety of biological processes, such as cell growth, proliferation, apoptosis, differentiation, tumor metastasis and tumor angiogenesis. MiRNAs have been found to act as either oncogenes or tumor suppressor genes in various cancers, depending on the tumor types and tumor microenvironment [7, 8]. Extracellular vesicles (EVs) are a heterogeneous group of cell-derived membranous structures comprising exosomes and microvesicles. EVs can be detected in various types of body fluids such as serum, urine, plasma, saliva and breast milk. EVs have been proposed as the major carriers for DNA, RNA, miRNA, lipids, and proteins [9, 10]. They play a critical role in mediating cell-to-cell communication by delivering these macromolecules to their recipient cells. Accumulating evidence have demonstrated that abnormal expression of circulating EVs derived contents have been closely associated with the progression of many cancer types including AML [11, 12]. For instance, alterations in exosomal protein and/or TGF-
The role of miR-10b in AML had been reported by some previous studies. For instance, Wang et al. showed that miR-10b expression was significantly upregulated both in AML cell lines and patients, miR-10b overexpression and HOXD10 inhibition significantly promoted AML cell proliferation, colony formation and suppressed AML cell apoptosis [15]. Bi et al. showed the expression level of miR-10a/b was significantly higher in AML than in normal controls. MiR-10b upregulation greatly stimulated leukemia cell proliferation and restrained granulocytic and monocytic maturation, resulting in leukemogenesis [16]. Zou et al. found AML patients with nucleophosmin 1 (NPM1) mutation commonly exhibited higher miR-10b expression compared to NPM1-unmutated AML, and miR-10b upregulation significantly suppressed myeloid differentiation of leukemia cells, and vice versa. KLF was its downstream target gene [17]. However, the clinical value of serum EV-miR-10b in AML remained uncovered. In the current study, we aimed to investigate the clinical significance of serum EV-miR-10b as an indicator for the prognosis prediction of AML.
Relationship between clinicopathological factors and serum EV-miR-10b expression in AML patients
Relationship between clinicopathological factors and serum EV-miR-10b expression in AML patients
WBC, white blood cells; BM, bone marrow; FAB, French-American-British. WHO classification, Type I: AML with certain genetic abnormalities, Type II: AML with myelodysplasia-related changes, Type III: AML related to previous chemotherapy or radiation, Type IV: AML not otherwise specified.
Primer sequence for qRT-PCR
Patients and samples collection
In our study, a total of 95 de novo AML patients and 80 healthy volunteers were enrolled. Of all AML cases, 51 patients were diagnosed with CN-AML. According to the French-American-British (FAB) classification, 8 cases had M0, 17 cases had M1, 25 cases had M2, 14 cases had M4 and 31 cases had M5. According to the WHO classification, 37 patients were AML with certain genetic abnormalities (Type I), 11 were AML with myelodysplasia-related changes (Type II), 15 were AML related to previous chemotherapy or radiation (Type III) and 32 were AML not otherwise specified (Type IV). Based on cytogenetic risk classification, 38 patients were with favorable-risk AML, 42 patients were with intermediate-risk AML, 15 patients were with poor-risk AML. The clinicopathological data of all AML patients were summarized in Table 1. This current study was approved by the Research Ethics Committee of the Third Affiliated Hospital of Sun Yat-Sen University. Informed written consents were collected from all the participants before bone marrow and blood collection. All specimens were handled and made anonymous according to the ethical and legal standards. Overall survival (OS) was defined as the time from diagnosis to death from any cause or the last follow-up. Disease free survival (DFS) was defined as the time from diagnosis to the relapse or the last follow-up.
Extracellular vesicle isolation and qRT-PCR
Peripheral blood from each patient or healthy volunteer was collected in tubes, and then centrifuged at 1500 rpm for 10 min. The serum samples were obtained and stored at
The serum extracellular vesicles were positive for EV/ exosome markers including TSG101, CD63, Flotillin-1 and CD9.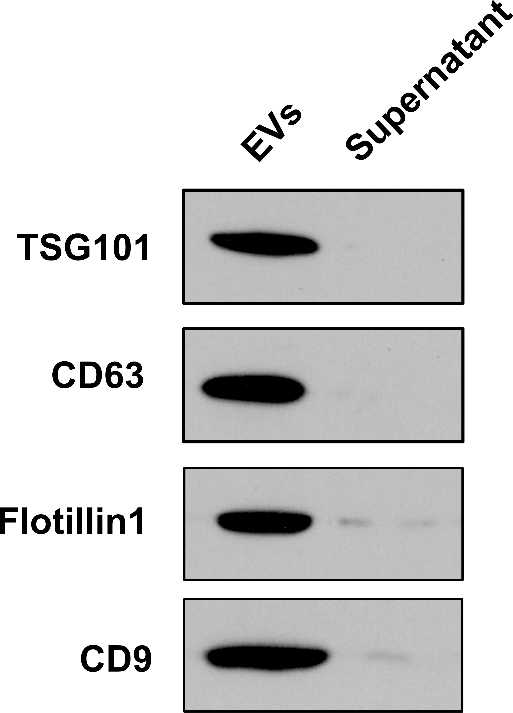
(A) The deregulated serum EV-miRNAs between AML and healthy controls. (B-E) The expression levels of serum EV-miR-10b, miR-542, miR-130a and miR-216b were significantly higher in AML patients compared with healthy controls. (F-H) The expression levels of serum EV-miR-146a, miR-34a and miR-192 were significantly lower in AML patients compared with healthy controls.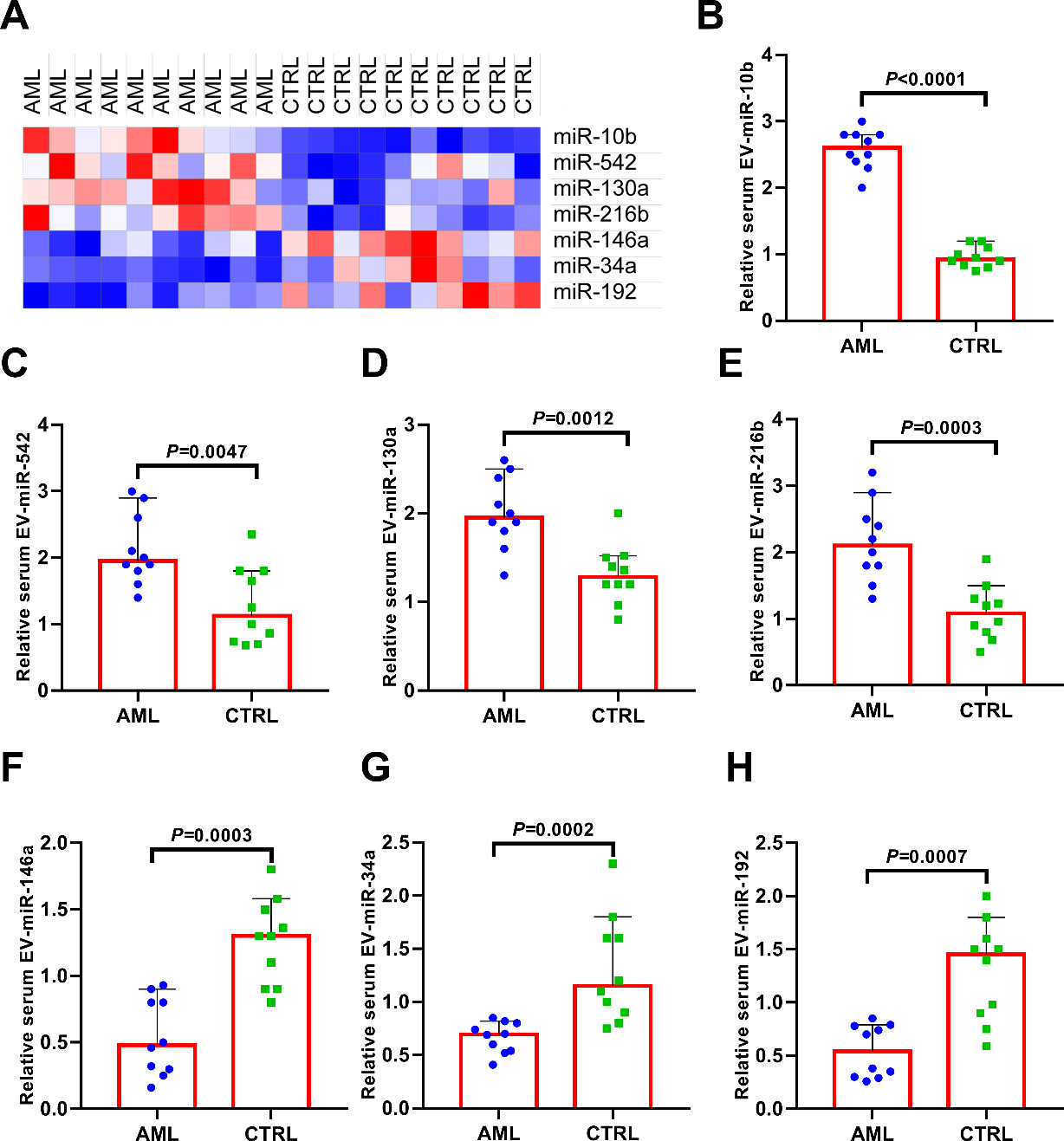
Briefly, EVs isolations were lysed in reducing sample buffer. Proteins were loaded on 8–12% Tris-glycine sodium dodecyl sulfate-polyacrylamide gels (Bio-Rad, Hercules, CA, USA), and electrophoresed. The proteins were transferred to polyvinylidene fluoride membranes and blocked in blocked in 5% non-fat milk in TBST for 1 h at room temperature. Then the membranes were incubated with primary antibodies of CD63 (Abcam, Cambridge, UK), TSG101 (Abcam), CD9 (Santa Cruz Biotechnology, Santa Cruz, CA, USA) and flotillin-1 (Santa Cruz Biotechnology) at 4
Statistical analysis
All statistical analyses were carried out with MedCalc Statistical Software version 16.4.3 (MedCalc Software bvba, Ostend, Belgium) and GraphPad Prism 7.00 (GraphPad Software, Inc., La Jolla, CA, USA). The Mann-Whitney U test or Kruskal-Wallis test were used to compare the differences in serum EV-miR-10b expression between groups. Receiver-operating characteristic (ROC) curves and the area under the ROC curve (AUC) were performed to evaluate the diagnostic accuracy of serum EV-miR-10b. Chi-square test and Pearson correlation analysis were used to assess the association of serum EV-miR-10b expression with clinicopathological variables. Survival curves were constructed by the Kaplan-Meier method, and the log-rank test was applied for comparison. Multivariate Cox regression analyses were performed using the Cox proportional hazards regression model. All differences were statistically significant at the level of
(A) Serum EV-miR-10b levels were significantly higher in AML/CN-AML patients. (B) Serum EV-miR-10b levels were significantly higher in all AML subtypes based on FAB classification. (C) Serum EV-miR-10b levels were significantly higher in all AML subtypes based on WHO classification. (D) Serum EV-miR-10b levels were strongly associated with cytogenetic risk stratification.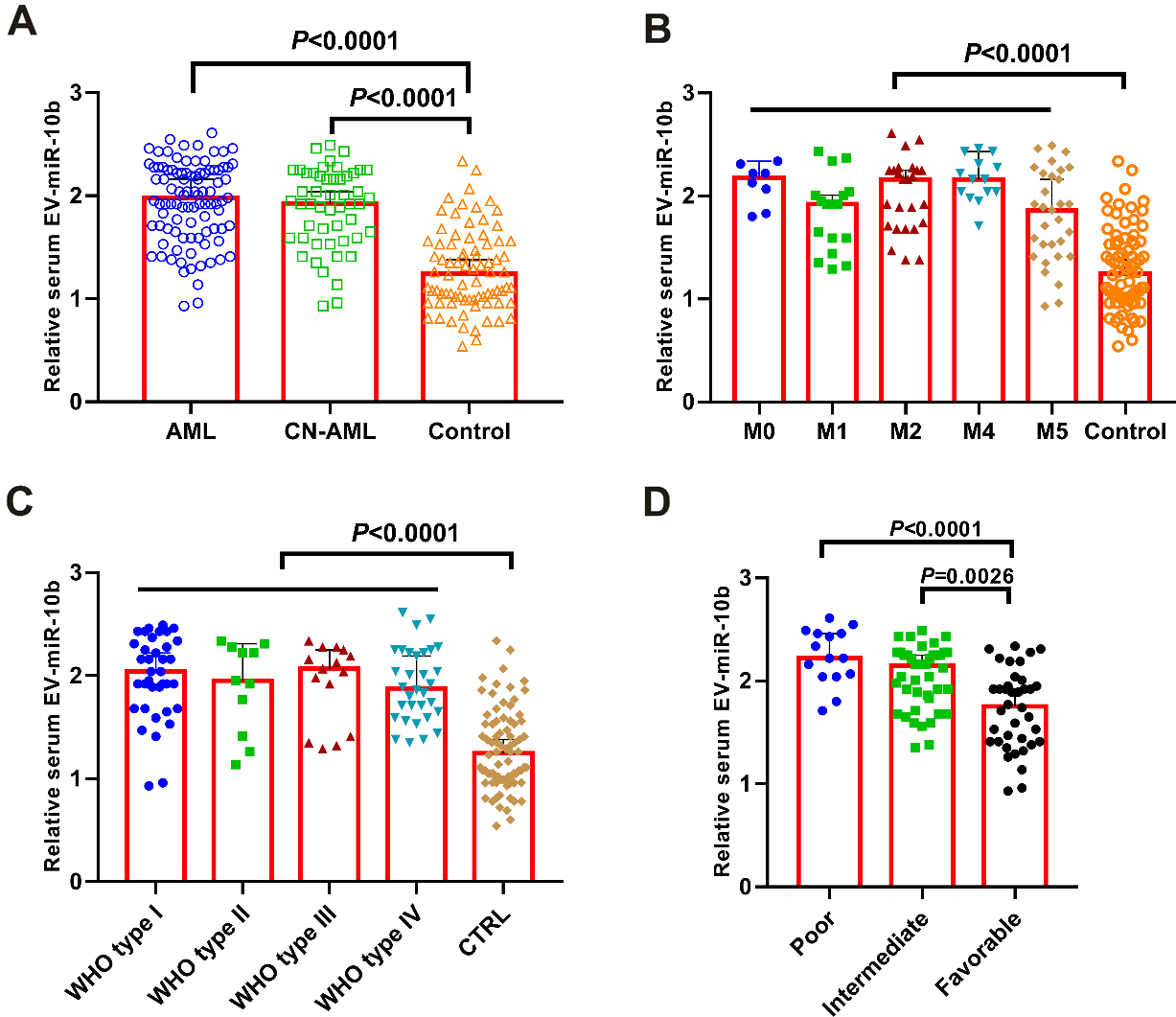
(A-B) Pearson correlation analysis showed that serum EV-miR-10b was significantly correlated with WBC count and blast percentage. (C-D) No significant correlation was found between serum EV-miR-10b level and hemoglobin level or platelet count.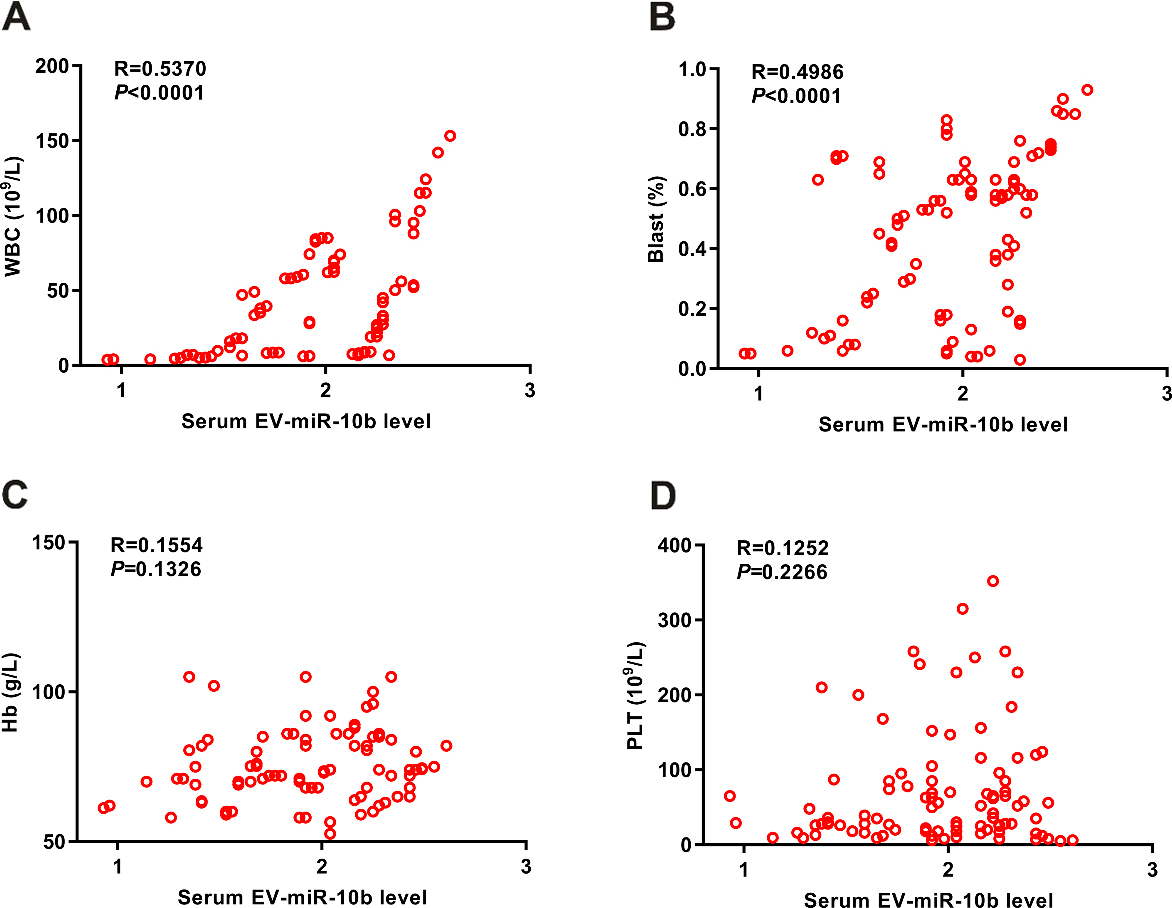
ROC analysis of serum EV-miR-10b for the discrimination of AML patients from healthy volunteers.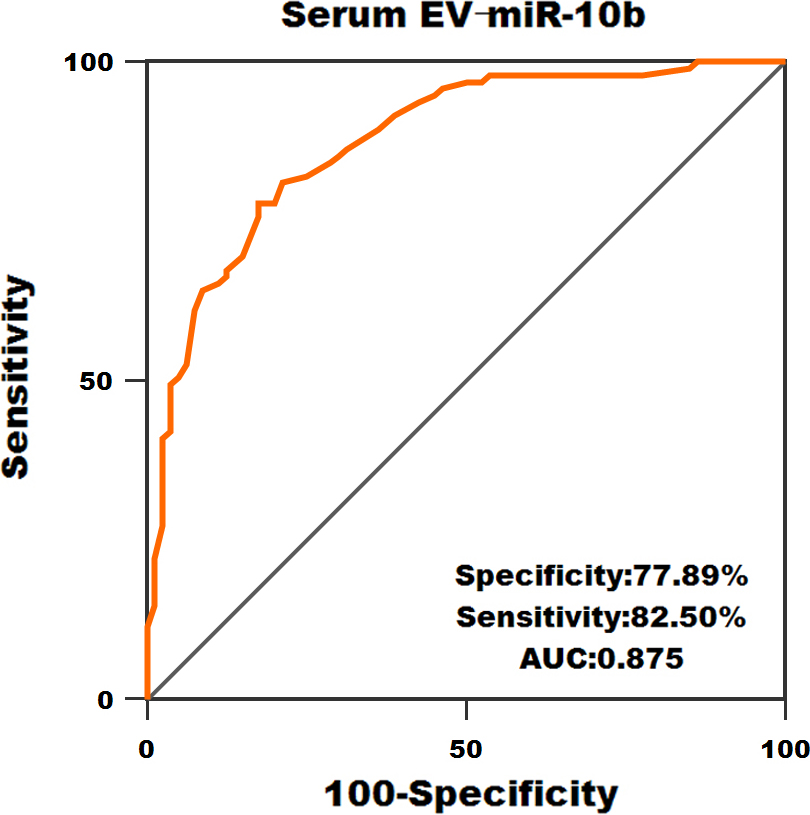
(A) Kaplan-Meier survival curves of OS based on serum EV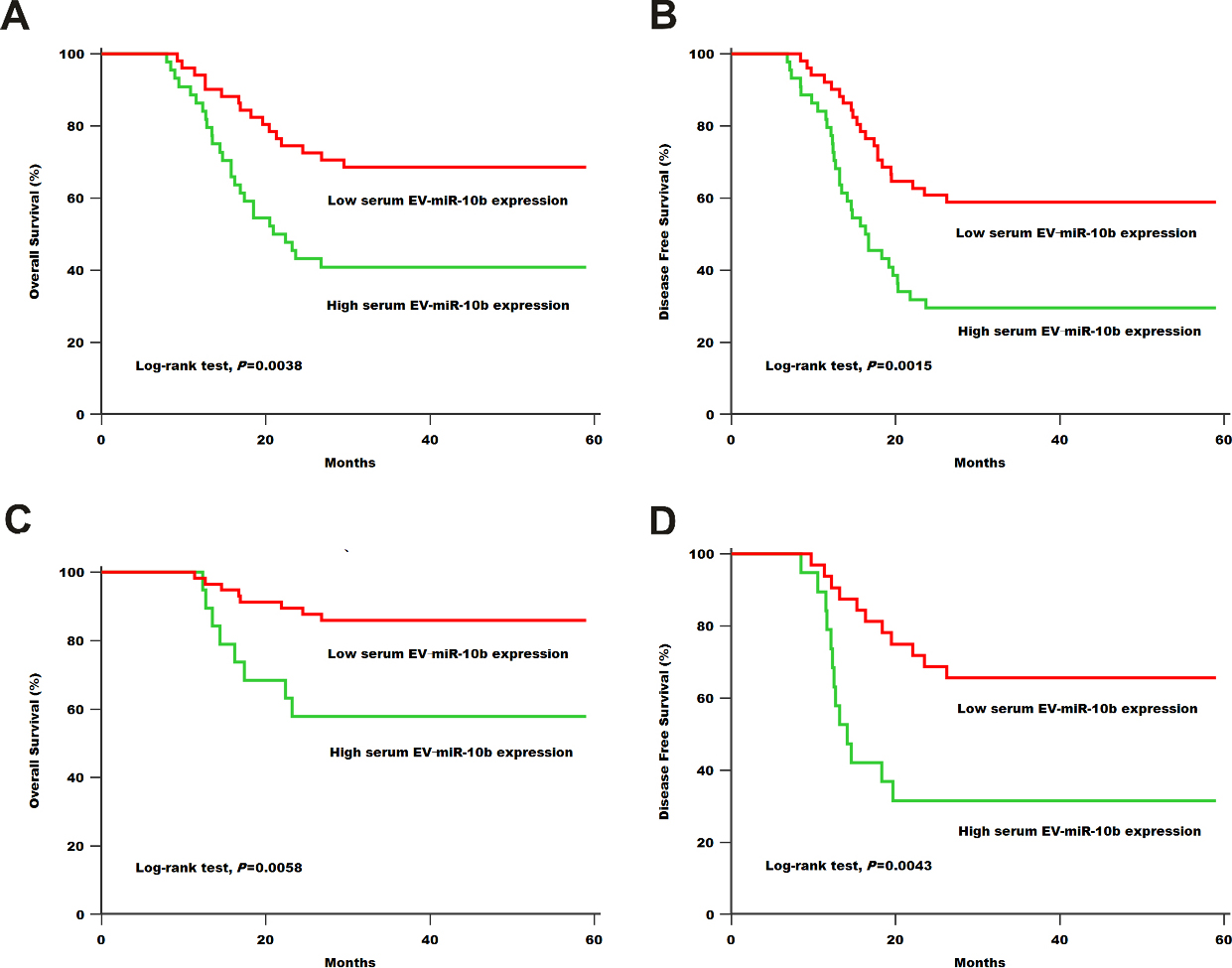
The deregulated serum EV-miRNAs in AML
Our western blot results showed that the EVs we extracted from serum samples were positive for EV/ exosome markers including TSG101, CD63, Flotillin-1 and CD9, while no signal was detected in the supernatant samples (Fig. 1). Then we compared the expression levels of serum EV-miRNAs between AML patients and healthy controls (Fig. 2A). Our data showed that the expression levels of serum EV-miR-10b (
Serum EV-miR-10b was overexpressed in AML patients
The levels of serum EV-miR-10b in AML patients and normal controls were detected by using qRT-PCR. As shown in Fig. 3A, the expression level of serum EV-miR-10b in AML patients and CN-AML patients were significantly elevated compared to the healthy volunteers (both
Pearson correlation analysis was performed to analyze the potential association between serum EV-miR-10b level and WBC, blast, platelet and hemoglobin. Our results showed serum EV-miR-10b level was significantly associated with WBC count (
Subsequently, ROC curve was constructed to determine the diagnostic value of serum EV-miR-10b. As demonstrated in Fig. 5, serum EV-miR-10b could well differentiate AML patients from normal controls (AUC
Association of serum EV-miR-10b expression with clinical features of AML
Table 1 presented the clinicopathological variables of all AML patients recruited in this study. Serum EV-miR-10b upregulation was closely associated with several aggressive clinical features, including WBC (
Multivariate Cox regression analysis for the relationship between serum EV-miR-10b and OS of AML patients
Multivariate Cox regression analysis for the relationship between serum EV-miR-10b and OS of AML patients
HR, hazard ratio.
Kaplan-Meier survival analysis was carried out to assess the prognostic value of serum EV-miR-10b in AML. AML patients in low serum EV-miR-10b expression group showed significantly longer OS/DFS than those in high expression group (
Multivariate analysis for OS revealed WBC (HR 2.24; 95% CI, 1.05–3.43;
Discussion
To the best of our knowledge, this is the first study to explore the clinical significance of serum EV-miR-10b in AML. In this study, we firstly demonstrated that the extracellular vesicles we extracted from the serum samples were positive for EV/exosome markers. Then serum EV-miR-10b expression was found to be markedly elevated in AML/CN-AML patients compared with in normal controls. In addition, high serum EV-miR-10b expression occurred more frequently in AML subjects with aggressive clinical variables. Moreover, ROC curve showed that the AUC for serum EV-miR-10b was 0.875 and yielded a good diagnostic power in discriminating AML cases from normal controls. Furthermore, for all AML patients and CN-AML patients, patients in high serum EV-miR-10b expression group had shorter OS/DFS than those in low serum EV-miR-10b expression group. Finally, serum EV-miR-10b was identified as an independent prognostic factor for OS in AML patients. These data indicated serum EV-miR-10b might serve as a promising diagnostic and prognostic biomarker in AML, and our findings were in line with previous reports [15, 16, 17].
There are several advantages for using serum EV-miRNAs for detecting and predicting the prognosis of AML. Firstly, miRNAs are highly stable in the biofluids such as serum, plasma, saliva and urine, which enable them to become promising biomarker for the diagnosis, prognosis prediction and therapeutic effects monitoring of AML [10]. Secondly, EV-miRNAs are largely derived from cancer cells, indicating that deregulation of EV-miRNAs in the serum samples might be a specific feature of AML [18, 19]. Thirdly, currently bone marrow aspirate and biopsy are part of the routine diagnostic work-up for AML diagnosis. However, these procedures are much more invasive than collecting the serum samples from AML patients.
The reason for selecting miR-10b, miR-542, miR-130a], miR-216b, miR-146a, miR-34a and miR-192 [20, 21, 22, 23, 24] was that these miRNAs have been reported to be deregulated in AML by previous studies. However, the clinical significance of these EV-miRNAs in AML is poorly known. Therefore, firstly, we examined their levels between AML patients and healthy controls with small sample size. The AML patients were randomly selected regardless of the subtypes. Then the most promising EV-miRNA was chosen for further research from these seven deregulated miRNAs. Our results showed that serum EV-miR-10b level was most consistently upregulated in AML patients compared to the healthy controls, which was the major reason for choosing it for further analyses.
The possible reason accounting for the upregulation of serum EV-miR-10b in AML patients might be that cancer cells actively synthesize miR-10b, which are then packaged into exosomes. As tumor cells secrete much more exosomes into the tumor microenvironment or circulation system compared to the normal cells [18, 19], it is reasonable to observe the phenomenon that the expression level of serum EV-miR-10b is significantly higher in AML patients. However, further studies are needed to elucidate the molecular mechanisms driving the increased synthesis of miR-10b in AML. One limitation of our study was that the sample size was relatively small. Large cohort studies are warranted to validate our above findings. Although we showed that upregulation of serum EV-miR-10b was associated with unfavorable prognosis of AML, one single biomarker is not sensitive and specific enough to predict the prognosis for each individual AML patient. Therefore, combining the serum EV-miR-10b with the clinical data as well as genetic profiling information might improve the prediction accuracy. Interestingly, our results also demonstrated that the expression levels of serum EV-miR-542, miR-130a, miR-216b, miR-146a, miR-34a and miR-192 were deregulated in patients with AML. The clinical significance of these serum EV-miRNAs in AML needs further investigation.
Up to now, many studies have demonstrated miR-10b played as an oncogene in various cancer types. For instance, the expression level of circulating exosomal miR-10b was upregulated in patients with pancreatic ductal adenocarcinoma (PDAC), and its level was significantly decreased in post-resection PDAC [25]. In hepatocellular carcinoma (HCC), miR-10b expression was dramatically overexpressed in HCC tissues, and in vitro analysis showed that miR-10b upregulation greatly promoted carcinogenesis through targeting CSMD1 or CADM2 [26]. Bai et al. revealed miR-10b levels were significantly increased both in melanoma patients and metastasis melanoma cells, and its expression was positively associated with worse clinical variables as well as shorter survival [27]. Moreover, miR-10b expression was increased in esophageal squamous cell carcinoma tissues, and overexpression of miR-10b markedly promoted cancer cell motility and invasiveness via degrading KLF4 [28]. Wang et al. found miR-10b expression was dramatically elevated in gastric cancer cell lines, miR-10b knockdown significantly attenuated cancer cell proliferation and migration in vitro by targeting Hoxd10 [29]. In non-small cell lung cancer (NSCLC), miR-10b expression was remarkably upregulated in NSCLC cell line and enhanced lymph node metastasis. In vitro analysis showed miR-10b upregulation stimulated the tumorigenesis [30, 31].
On the other hand, Hou and colleagues reported the tumor suppressive role of miR-10b in cervical cancer. MiR-10b expression was decreased both in cancerous tissues and cell lines, and miR-10b overexpression remarkably suppressed the oncogenic activities of cancer cells by directly silencing IGF-1R expression [32]. More interestingly, the controversial role of miR-10b was observed in colorectal cancer (CRC). MiR-10b levels were significantly increased in CRC tissues. Its upregulation was strongly correlated with aggressive clinical parameters, and miR-10b promoted tumorigenicity by regulating HOXD10 [33, 34]. Whereas, another study by Song and Li reported either miR-10b overexpression or FGF13 downregulation inhibited the carcinogenesis in vitro and restrained cancer cell growth and lung metastasis in vivo [35]. Therefore, the specific role of miR-10b in various tumor types may be linked to the tumor microenvironment.
In summary, the expression level of serum EV-miR-10b was increased in AML and high serum EV-miR-10b level was closely associated with poor prognosis. Thus, serum EV-miR-10b might be a potential diagnostic and prognostic marker for AML.
