Abstract
BACKGROUND:
McKenzie standing trunk extension exercises have been used for the management of low back pain (LBP). However, no study to date has investigated the effect of standing trunk extension postures on spinal height and clinical outcomes.
OBJECTIVE:
To evaluate in subjects with LBP following a period of trunk loading how spinal height, pain, symptoms’ centralization and function outcome measures respond to two standing postures interventions: (1) repetitive trunk extension (RTE) and (2) sustained trunk extension (STE).
METHODS:
A consecutive sample of convenience of people with LBP were recruited to participate in 2-session physical therapy using either RTE or STE in standing.
RESULTS:
Thirty participants (18 women) with a mean age of 53
CONCLUSION:
People with LBP experienced greater spine growth and improvements of pain during standing STE as compared to RTE. People with LBP could use such postures and movements to alleviate their LBP and improve spine height while in a weight bearing position.
Keywords
Background
According to the United States Department of Labor, there were more than one million injuries and illnesses requiring days away from work amongst private industry, state and local government employees. Among these injuries and illnesses, 16.6% were low back related equating to 191,479 low back injuries requiring days away from work [1].
The American College of Physicians and the American Pain Society classified low back pain (LBP) into three categories: (1) nonspecific LBP; (2) LBP potentially associated with radiculopathy or spinal stenosis; and (3) LBP potentially associated with another specific spinal cause. Of these three, lumbar intervertebral disc (IVD) herniation is one of the most common spinal degenerative disorders leading to LBP associated with radiculopathy [2, 3, 4]. In order to better understand the IVD’s role in the development or persistence of LBP and spinal stenosis, there have been many stadiometric studies primarily focused on lumbar spinal height changes associated with various positions and movements [6, 7, 8]. These studies were designed to investigate if spinal height could be restored following spinal shrinkage using various postures. Natural IVD height preservation is so important that the biomedical field has examined the use of growth factors for IVD biologic regeneration [9]. This was done to more naturally preserve IVD biomechanical and physiological function as opposed to surgical disruption.
People spend about 61% of time standing in the work and home environment [1]. Although prolonged weight bearing postures, such as standing and walking, have been associated with decreased spine height [10, 11] some studies reported that seated weight bearing postures could result in spine height gain [12]. Sustained and repetitive lumbar extension postures frequently occur after periods of prolonged unloading such as sleep. These extension postures are periodically repeated throughout the day during activities such as standing and walking [1]. People presenting with directional preferences that include lumbar extension tend to respond well to exercises geared toward trunk extension [13, 14, 15]. Significant and rapid changes in central and distal pain intensity and location have resulted from standing end range trunk extension in patients with low back and referred pain [16]. Additional studies reported that standing back extension exercises resulted in back pain episodes’ prevention and decreased back pain in care workers [17, 18]. Standing exercises have the advantage to be functional and easily performed in work and home settings [19].
Lumbar extension range of motion (ROM) is positively correlated with symptoms’ centralization in LBP patients [20]. Clinicians assess symptoms’ centralization, which refers to symptoms retreating towards the spine midline in response to repeated movements or guided positioning [21, 22]. The operational definition and measurement techniques for centralization have been laid out in several studies [23, 24]. Several methods have been used to increase spinal ROM including static, repeated, passive postures, and proprioceptive neuromuscular facilitation. Both standing and prone lumbar extension postures are effective for treating low back dysfunction syndrome [25]. However, which method is best suited for increasing spinal ROM remains debated [26, 27]. One author found static prone postures to increase ROM more effectively with 30–60 second sustained postures as compared to 15-second postures, but no difference between the effectiveness of 30-second and 60-second postures [28, 29]. Additionally, patients with LBP chose to perform their extension posture for home exercise in standing 80.8% of the time and only 19.2% of the time in the prone position, resulting in similar clinical outcomes where both groups showed equal improvements in lumbar extension ROM [30].
Previous studies investigated the effects of postures and movements in lying (unloaded) or seated positions on spinal height (Owens 2009, Gerke, et al. 2010; Pape 2018). These studies primarily focused on spinal height following static patient positioning and showed that both the lying and supported seated positions resulted in mean spinal height gains of 2 to 5 mm. However, most rehabilitation programs focused on LBP prevention and management use both repetitive and/or sustained spinal extension exercises to improve patients’ outcomes [32, 33]. Such exercises can be performed in lying or standing position. Although patients with acute and recurrent low back and referred pain tend to respond well to directional preference postures [34], subjects with chronic symptoms tend to display greater signs of sensitization, biopsychosocial issues [35], and tend to respond less favorably to directional preferences postures and exercises [36].
No study to date has investigated the effects of standing extension postures on spinal height, pain, centralization and function. Therefore, the purposes of this study will be to evaluate in a sample of LBP patients the effect of standing trunk extension, both sustained and repetitive, following a period of spinal loading, on (1) spinal height; (2) pain; (3) symptoms centralization and (4) functional measures. The results of this study could impact rehabilitation programs that could use standing trunk extension postures at home or in the work environment to grow and/or prevent spinal shrinkage.
Methods
Research design(s)
A pre-test, post-test comparison group design (randomized clinical trial) was used to determine how spinal height changes in response to standing sustained trunk extension (STE) and repetitive trunk extension (RTE) after a period of spinal loading. The study used a 2 (between subjects – type of trunk extension: sustained vs. repetitive)
Power analysis – sample size
Power calculations were performed to determine the sample size required for the study using the spinal height change as the primary outcome measure. The study was designed with the
Pre-study approvals
The Texas Tech University Health Sciences Center Institutional Review Board (IRB) approved this study (L19-024). The trial was registered at
Subjects/specimens
Systematic consecutive sampling of 35 subjects with musculoskeletal LBP were recruited from physician offices, Sports medicine and Physical therapy clinic and the general Fredericksburg community and surrounding areas Our recruitment was inclusive of LBP subjects that demonstrated a directional preference toward trunk extension, regardless of the chronicity of symptoms to increase the external validity of the findings.
Inclusion Criteria were: (1) Ability and willingness to come twice to the physical therapy clinic for approximately 60 minutes each; (2) Subjects with LBP and directional preference in back extension; (3) Age 18–80 [38]; (4) Ability to stand for 5 minutes; (5) Ability to sit for 10 minutes; and (6) Low back pain on Numerical Pain Rating scale (NPRS) of at least 2/10 and less or equal to 9/10 [39]. Exclusion Criteria were: (1) Pregnancy by subject report; (2) history of back surgery or spinal fractures within the last six months; (3) history of spinal fusion or physician’s diagnosis of spinal instability; (4) current history of acute systemic infection, active inflammatory disease, or malignancy; and (5) subjects engaged in legal/compensation claims for their back symptoms.
Consort chart.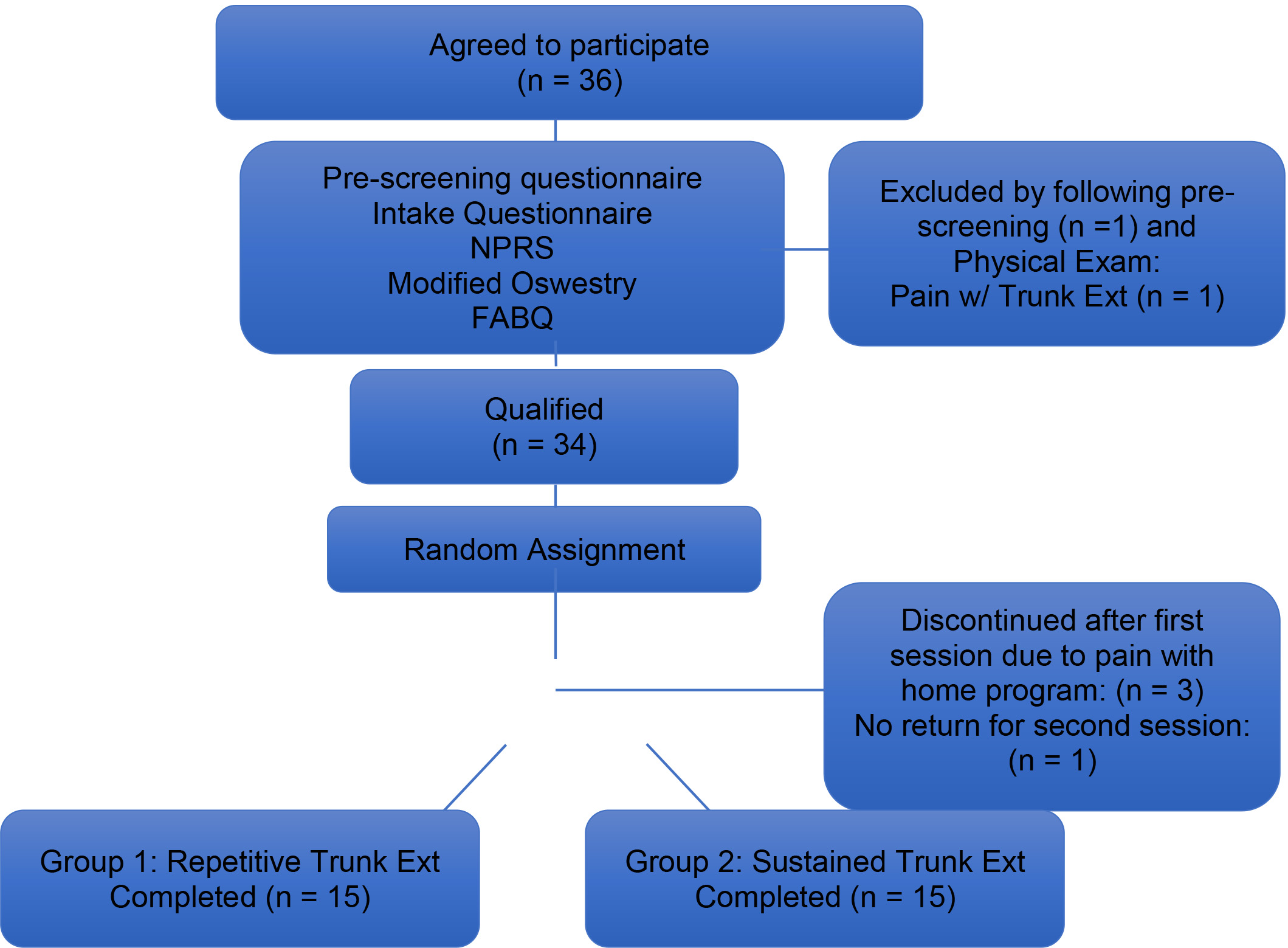
Flow chart of test positions and testing sequence.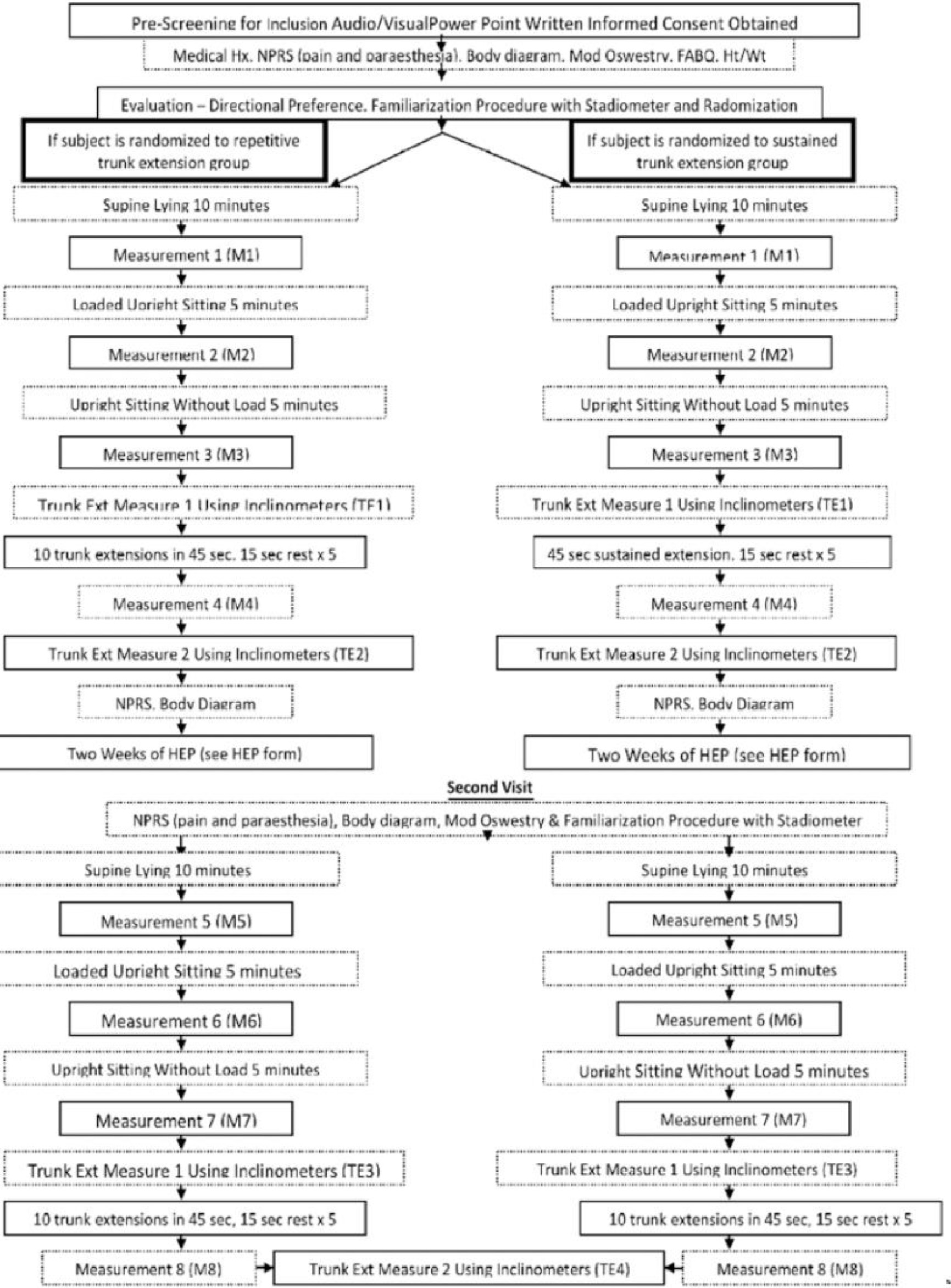
Subjects attended two physical therapy sessions to complete the study.
Session 1
Each participant watched an audio-visual power point presentation explaining the study, test procedures and including a video describing the interventions (standing RTE and standing STE). Written informed consent was obtained. To determine directional preference, the principal investigator (JH) used the guidelines set forth in the directional preference definition [40] and based off of standards set forth in randomized clinical trials [41]. A questionnaire including pertinent medical history was completed. Participants completed (1) a Numerical Pain Rating Scale (NPRS) to rate their current, minimum, maximum and average LBP over the last two days [39] as well as paresthesia signs/symptoms intensity; (2) Body Diagram for indicating location of symptoms; (3) Modified Oswestry LBP questionnaire [42]; (4) Fear Avoidance Belief Questionnaire [43] (Fig. 1). A researcher recorded participant’s height and weight. A Flow chart illustrates study sequence in details (Fig. 2).
Participants meeting the criteria for study inclusion completed a familiarization procedure to determine the consistency to reposition themselves in the stadiometer. Participants able to reposition themselves in the stadiometer with a SD of 1.3 mm or less for five consecutive measurements [31, 32, 44] were included in the study. The stadiometer digital display was covered to blind the researcher performing the measurements.
Starting position for trunk extensions; B: End position for sustained trunk extension that was held for 45 seconds and repeated 5 times (sustained trunk extension group), and for repetitive trunk extensions that were repeated 10 times for a period of 45 seconds followed by 15 seconds break (repetitive trunk extension group).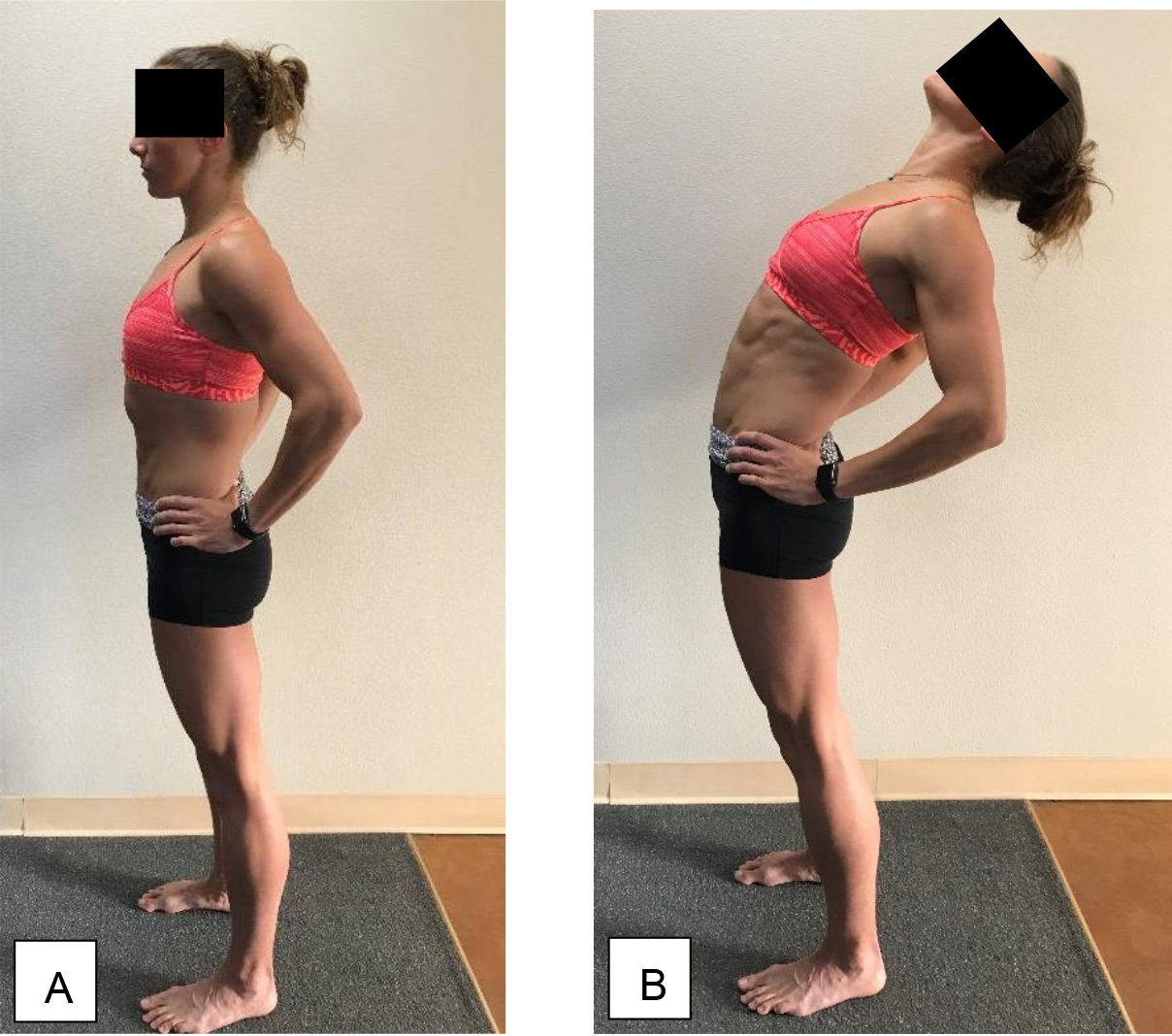
Position of participant – A: for spinal height measurement in stadiometer unit; and B: during spinal loading time in sitting with 5lb on each shoulder.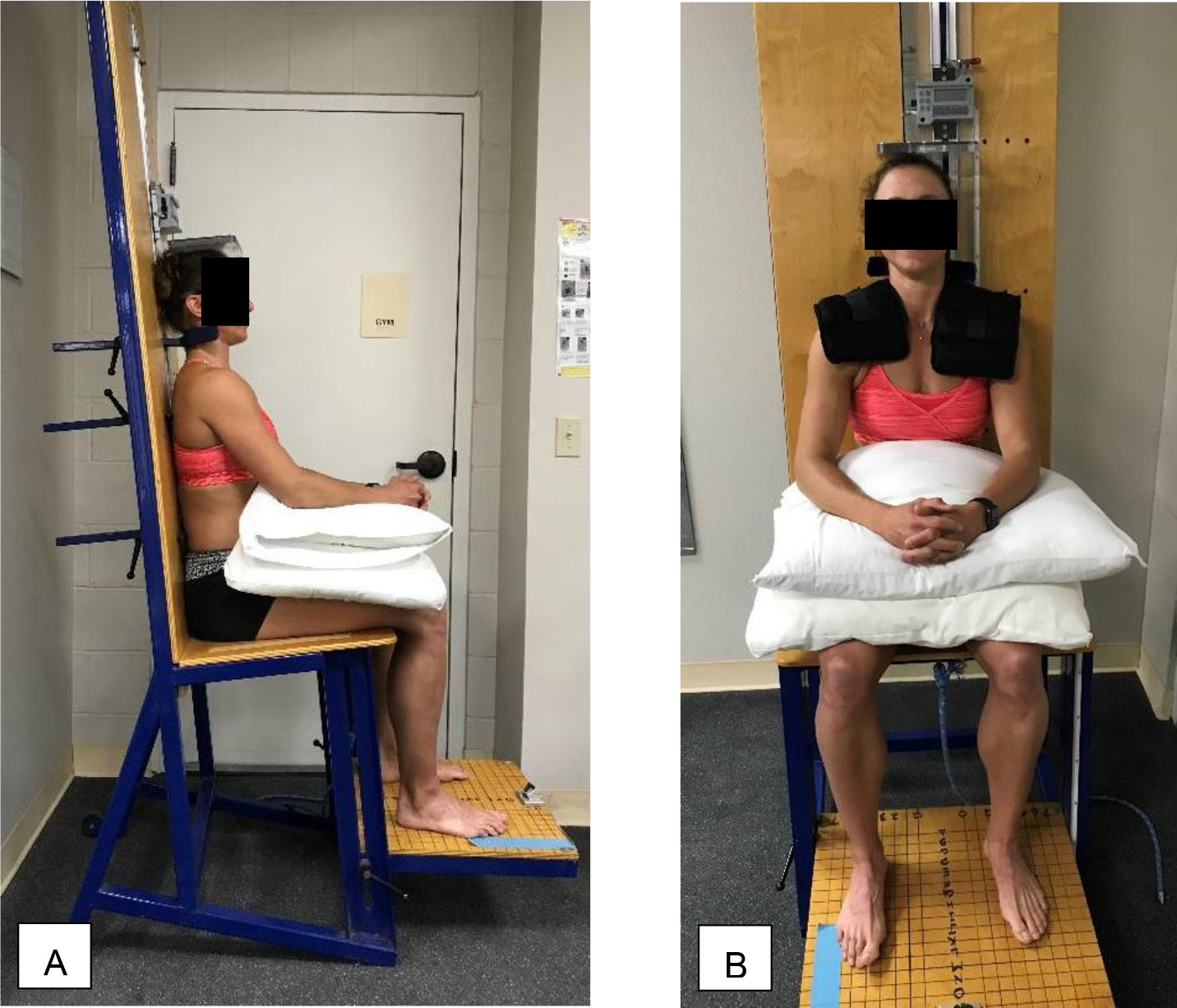
At the beginning of data collection, a randomization plan generator (
The participant repositioned on the stadiometer and spinal height was measured (Measurement 4). Participants scored their low back and lower extremity symptoms using NPRS [40], and mapped their pain on a body pain diagram prior to intervention, immediately after and 2-week following the intervention to determine pain rating and centralization of symptoms [8]. The principal investigator applied a numeric overlay template to the participants’ body diagrams to document the most distal pain location scores between 0 (no LBP) and 6. Higher score indicated a more distal symptoms’ location.
Participants were instructed to continue to use their medications, as prescribed by their primary healthcare provider and not to change them during the follow-up two-week period. A sheet including home exercise instructions was provided to each participant. Instructions included RTE or STE based on random group assignment, performed approximately 5 times per day. Each participant completed a sheet recording home exercise compliance.
Session 2
Participants completed same questionnaires, trunk unloading procedure and four stadiometric measurements as in Session 1. The participants then scored their low back and lower extremity symptoms using NPRS [39], and mapped their pain on a body pain diagram.
Investigator blinding
The principal investigator was involved with data collection, supervised positioning in the stadiometer and stadiometric measurements. The investigator was blinded to the intervention and the stadiometric measurements during the experiment.
Data analysis
Descriptive and inferential statistics were carried out using Excel and SPSS 23.0 for Windows (SPSS, Chicago, IL, USA). Descriptive statistics including mean, median, mode, standard deviation, minimum and maximum values, frequency counts were collected for age, height, weight, body mass index, pain, centralization, function (Modified Oswestry LBP Disability Questionnaire), FABQ, spinal height, and spinal height changes after repetitive and sustained standing trunk extension after a period of spinal loading. To assess differences between the groups for these variables at the beginning of data collection, independent t-tests and Mann Whitney-U were used. Levene’s test and Shapiro-Wilk test of normality were used to test for variance and measurements distribution of spinal height, changes in spinal height, degrees of spinal extension, pain, and function outcomes.
Baseline characteristics of the 30 study participants by group
Baseline characteristics of the 30 study participants by group
Notes: BMI
A Wilcoxon sign-rank test was used to assess differences in spinal height, centralization and pain outcomes improvements following STE and RTE postures. A 2 (between participants – type of trunk extension: STE vs. RTE) x 2 (within participants – time: change at visit 1 and change at visit 2) mixed ANOVA’s examined differences in (1) spinal height change and (2) function outcomes as a result of sustained and repetitive standing trunk extension after a period of spinal loading. Post hoc paired t-tests explored further for significant differences in spinal height, pain and function outcomes between the four conditions. A 2 (between participants – type of trunk extension: STE vs. RTE)
Of the 35 subjects recruited for the study, 34 met all inclusion criteria. One subject was excluded secondary to pain with standing trunk extension upon evaluation after subjectively reporting no pain with this posture on pre-screening questionnaire. Three participants developed pain several days after the first session while participating in the home exercise program and were asked to discontinue the program and no follow up session was scheduled. One participant did not report pain with the home program until the follow up session and at that time, only NPRS, Modified Oswestry and pain body diagram questionnaires were completed. This participant was excluded.
Descriptive statistics including mean
standard deviation for pain, spinal height, function, and median-interquartile range for centralization for visits 1 and 2 changes
Descriptive statistics including mean
Notes: RTE
Thirty participants (18 women and 12 men) randomized into two groups of 15 with a mean age of 59.1
This is the first study to evaluate spine growth during standing extension postures commonly used in Mechanical Diagnosis and Therapy (the McKenzie Method) [46] in a population of people with LBP. Clinicians use such methods across a broad spectrum of ages, pathologies and disabilities. Therefore, this study was designed to avoid exclusion based on age and lumbar pathology as not to limit the generalizability of the results and to better understand the effect of standing trunk extension postures on these populations. Standing trunk extension may be a safer option for cardiovascular patients because of less hemodynamic demand as compared to prone or supine lying trunk extension [46]. Additionally, STE posture can be more practical and easier to achieve for subjects depending on convenience and physical ability. The results indicated that STE posture for 45 seconds repeated five times caused greater spine growth as compared to RTE posture for 10 repetitions repeated five times within five minutes, displaying large effect sizes. Moreover, LBP decreased to a greater extent when the participants did sustained versus repetitive trunk extension in standing. It is possible that the RTE group showed less spinal height increase and pain reduction due to their higher average age and chronicity of symptoms (Table 2) This could be attributable to the biomechanical changes that occur during the spinal degenerative process of a depressurized nucleus and irregular spikes of excessive IVD loading and an increased neutral zone with advancing IVD degeneration [47, 48, 49]. These findings suggest that people that respond favorably to standing trunk extension exercise could use such postures and movements to alleviate their LBP and improve spine height while in a weight bearing position. Four of the 35 participants with LBP (11%) initially recruited for the study did not tolerate the standing trunk extension exercise program and were excluded from the study, indicating that such program may not be appropriate for all patients with LBP. The spinal growth recorded of about 4 mm during five time 45 seconds hold STE posture was similar to that reported previously in the seated slouched position using a lumbar support [51], which suggests that people experiencing pain relief and symptoms’ centralization in such standing posture could adopt it to increase spine height and rehydrate the lumbar IVDs Although the spinal height changes were temporary, as shown in previous studies, new research shows that dynamic loading significantly increases small and large solute transport through the cartilage end-plates. The clinician’s goal is therefore not to sustain spinal height growth but to enhance transport of nutrients into the IVD [51].
Our results support those previously reported in prone position where increased spinal height recovery was greater following prone hyperextension (7 mm) as compared to prone lying (6 mm) [52]. Moreover, both prone [31] and supine hyperextended postures resulted in spinal height increase (6.37
Although lying postures resulted in greater spine height growth of 5 mm [32] and larger decreased in pain and centralization in elderly people with nerve root compression syndromes [8] as compared to our study results, the standing techniques used in our study could be recommended as 57% (17 out of 30) of participants in our investigation reported greater or equal to 2/10 pain improvement (MCID). Such improvements in pain are noteworthy as the participants’ FABQ (Table 2) averaged 23, which indicated a greater risk of reporting no improvement in Oswestry Disability Questionnaire at 6-month and persistent problems [53]. The two groups reported very similar home program compliance at the end of two weeks with the RTE group reporting 91% compliance and the STE group reporting 87% compliance.
The Modified Oswestry resulted in seven participants (23%) reaching the MCID of decreased 12/100 points for the Oswestry LBP questionnaire. No MCID for centralization has been established; however, centralization resulted in a median change of one in both RTE and STE groups from before Session 1 to after Session 2. The RTE group had five subjects and the STE group had seven who had equal to or greater than a twopoint change in their centralization score after two weeks. Future research is needed to investigate the characteristics of those patients that centralized the most with standing extension, which could help guide patient care as patients with lumbar stenosis may not be able to tolerate such standing extension postures.
Limitations of this study include some difference in age and initial Modified Oswestry scores between the groups, a relatively low initial current pain level amongst participants, and no long term follow up. Future studies with longer follow up and recordings of medication usage duration prior to entry in the study are warranted. Additionally, the groups were heterogenous for symptoms’ chronicity, as there were three participants in the RTE group with years of symptoms reported as compared one participant reporting eight years of symptoms in the STE group. The chronic nature of symptoms for these participants may have influenced the outcomes of the study as the RTE group did show less pain reduction although similar improvements in function as the STE group. Future studies including subjects with greater initial LBP would be useful in determining effectiveness in reducing pain.
Conclusion
People with LBP experienced greater spine growth and improvements of pain that were clinically meaningful during standing STE as compared to RTE. These findings suggest that people with LBP could use such postures and movements to alleviate their LBP and improve spine height while in a weight bearing position. Sustained trunk extension may prove more effective in restoring spinal height loss as compared to the RTE intervention and provides alternative ergonomic postural option for people with LBP seeking to rehydrate their lumbar IVDs.
Author contributions
Jeremy J. Harrison: literature review, study design, data collection, analysis and writing.
Jean-Michel Brismée: study design, data analysis and review writing.
Phillip S. Sizer Jr: study design, review writing.
Brent K. Denny: piloting of study, data analysis.
Stéphane Sobczak: study design, and critical review.
Data availability statement
Data are available upon request to the Principal Investigator of the study.
Ethical approval
The Texas Tech University Health Sciences Center Institutional Review Board (IRB) approved this study (L19-024). The trial was registered at
Funding
Not applicable.
Informed consent
All participants voluntarily consented to participate in the study and signed an informed consent form.
Supplementary data
The supplementary files are available to download from
Footnotes
Acknowledgments
We would like to thank the study participants for their willingness to contribute to research and for Sports Medicine & Physical Therapy of Fredericksburg for allowing us to conduct our study.
Conflict of interest
We affirm that none of the authors have financial affiliation (including research funding) or involvement with any commercial organization that has a direct financial interest in any matter included in this manuscript.
