Abstract
OBJECTIVES:
Research investigating the quality of life (QOL) of breast cancer patients undergoing chemotherapy has yielded useful knowledge regarding the effects of cancer treatment on the quality of life of patients. This study reviews the assessment of the quality of life for those diagnosed with breast cancer.
DESIGN:
A systematic review was conducted.
DATA SOURCES:
This systematic review utilized online databases, including PubMed, Web of Science, Scopus, and Google Scholar. A search ranging from 2018 to 2024 was carried out.
REVIEW METHOD:
Medical Subject Headings (MESH) were used for keyword selection along with other target keywords, such as “Quality of life”, “Breast cancer”, “Chemotherapy”, “Treatment side effects”, “Patient experience”, “Psychosocial well-being”, “Physical functioning”, “Emotional distress”, and “Supportive care”. We reviewed and included all English-language publications. A narrative synthesis was conducted to present the results of the studies.
RESULTS:
A total of 300 studies were obtained from the search using the specified keywords. Each result underwent another filtering round after applying the inclusion and exclusion criteria. This process led to a final selection of 20 papers that met the requirements and were included in the systematic review.
CONCLUSION:
The use of instruments to measure the quality of life (QoL) of breast cancer patients is crucial in understanding the impact of breast cancer on patients’ lives, from physical and mental health to social aspects.
Introduction
Patients with breast cancer undergo a variety of treatments, including surgery, chemotherapy, radiation, and hormonal therapy. Patients may receive various treatments based on the specific characteristics of their cancer, such as its type, stage, and size, as well as their demographic and clinical background [1]. The illness’s characteristics and scope determine the treatment approach’s selection. Chemotherapy is a treatment that can eliminate cancer cells, but it may adversely affect healthy cells [2,3].
Cancer patients, especially breast cancer patients, experience considerable QoL changes from chemotherapy. This is because the disease and therapy affect physical, emotional, social, and general health. Fatigue, nausea, vomiting, sleeplessness, appetite loss, and diarrhea might lower QoL. Understanding the disease’s effects and customizing chemotherapy therapies requires assessing a patient’s quality of life. Interdisciplinary, holistic oncological care that addresses cancer’s physical, psychological, and social aspects improves patient and family well-being [4–7].
Chemotherapy significantly impacts the health-related quality of life (HRQoL) of breast cancer patients, leading to a decline in HRQoL scores during treatment. This decline is seen in various aspects of HRQoL, including global health status, physical functioning, role functioning, emotional functioning, social functioning, body image, sexual functioning, and sexual pleasure. Chemotherapy-induced side effects such as fatigue, nausea, vomiting, insomnia, loss of appetite, and diarrhea contributed to this decline despite a decrease in symptoms [8–10].
Chemotherapy worsens physical symptoms such as insomnia, nausea, fatigue, and loss of appetite in breast cancer patients. It also affects daily activities, interpersonal relationships, and self-analysis, increasing emotional and psychological imbalance. Side effects such as fatigue and nausea can affect the patient’s quality of life. Managing these symptoms through medication, lifestyle adjustments, and supportive care can improve treatment and rehabilitation [11,12].
The purpose of this literature study is to review instruments used to assess the quality of life of breast cancer patients. The information obtained will be important for developing methods to improve treatment facilities and facilitate rehabilitation and palliative care to help cancer patients cope with better recovery and improve their quality of life.
The implications of these instruments for the future quality of life of breast cancer patients are multifaceted, encompassing the development of more specific tools, the need for continuous updates to reflect changes in therapies and side effects, and the importance of patient-reported outcomes in clinical trials and research [13–16].
Material and methods
Search strategy and inclusion criteria
We searched four electronic databases: PubMed, Web of Science, Scopus, and Google Scholar. The time interval of our search in this study was from the beginning of 2018–2024. Medical Subject Headings (MESH) were used for keyword selection along with other target keywords, such as “Quality of life”, “Breast cancer”, “Chemotherapy”, “Treatment side effects”, “Patient experience”, “Psychosocial well-being”, “Physical functioning”, “Emotional disturbance”, and “Supportive care”. We reviewed and included all English-language publications.
Study design
All interventional studies, such as randomized clinical trials, clinical trials, and quasi-experimental studies, were included in this review.
Study selection
Search results were imported into Endnote software, thus eliminating duplicate records. The full texts of potentially relevant papers were read to ascertain whether they met the abovementioned inclusion criteria. Two independent reviewers were involved in the execution of this procedure. Any disagreements were resolved through discussion. The study selection process is shown in Fig. 1.
Results
See Table 1.
Discussion
Chemotherapy (CT) side effects and symptoms vary by drug and patient. Studies have examined the effects of CT on quality of life, with some showing that patients who receive CT as a last resort may have better quality of life and more prolonged survival [8].
Silveira FM et al. (2021) found that 79 patients who started chemotherapy at a charity hospital referral institution in Três Lagoas, Mato Grosso do Sul, Brazil, from June 2018 to June 2019 had an average age of 60 years. Study participants with communication issues were excluded. Quality of Life Measures test. European Organisation for Research and Treatment of Cancer Core 30 Quality of Life Questionnaire (version 3). The EORTC QLQ-C30 performed well in two tests. After three months of treatment, physical and cognitive function improved, but emotional function worsened. Three months into treatment, exhaustion, nausea, shortness of breath, loss of appetite, and diarrhea intensified [17].
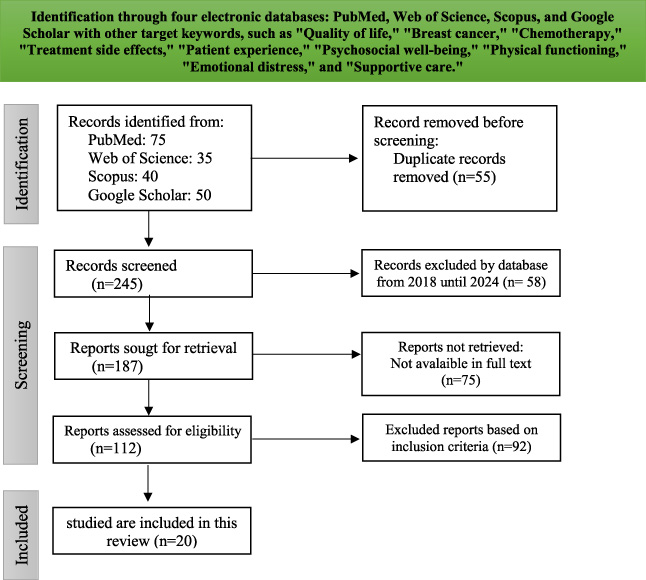
Prisma diagram.
Chemotherapy changed patients’ HRQoL views, lowering global health status and functional measures, according to Binotto et al. (2020). Since chemotherapy side effects are commonly underestimated, this study emphasizes the importance of assessing HRQoL indicators in breast cancer patients. The authors say HRQoL measurement can improve patient care, but its use in clinical practice is complex [18].
Dano et al. (2019) studied 120 patients at the University Hospital Centre Aristide Le Dantec in Dakar, West Africa, from July 2017 to February 2018. Their average age was 45. Half of the patients had metastatic disease, and most had locally progressed disease (stage T3 to T4) and lymph node involvement. Over time, the FACT-B score increased considerably. Nausea and vomiting significantly reduced the FACT-B overall score. This study proved that Senegalese breast cancer patients could use a standardized quality-of-life measure [19].
Studies by Javan Biparva et al. (2023) yielded findings. EORTC QLQ-C30 scored 64.72, FACT-B 84.39, QLQ-BR23 66.33, and SF-36 57.23 in meta-regression of 9012 breast cancer patients. Age directly affects breast cancer patients’ quality of life, with those who completed treatment getting higher scores, according to a meta-analysis. This global systematic study identifies factors affecting breast cancer patients’ quality of life (QoL) and suggests policy changes. Quality-of-life instruments can improve clinical diagnosis, prognosis, monitoring, decision-making, treatment, and follow-up [20].
Characteristics of inclusion studies
The Tikur Anbessa Specialised Hospital in Addis Ababa, Ethiopia, studied the quality of life of 404 breast cancer patients who received at least one chemotherapy cycle. The EORTC QLQ-C30 and breast-specific quality of life questionnaires were employed in the investigation. With most patients rating poorly in emotional, sexual, and financial concerns, the mean quality of life score was 52.98. Education, married status, higher household income, physical and social functioning, decreased fatigue, insomnia, financial troubles, and systemic therapeutic side effects improved quality of life. This study recommends including quality of life assessment in treatment procedures and providing financial aid to breast cancer patients [21].
Youthful breast cancer survivors had a steeper decrease and slower recovery than the general population, according to a Finnish study by E. Roine et al. (2021). Younger survivors declined more throughout therapy and improved slowly but remained below population levels after ten years. At ten years, older survivors were below the population level but approached it in the first five. Both age groups remained below the population level ten years after therapy [22].
A study on axillary care and post-treatment HRQoL in breast cancer patients. APS, or complete axillary lymph node dissection, was performed on 552 individuals. Physical and psychosocial well-being deteriorated considerably for ALND with axillary irradiation compared to APS alone. Both treatments raised arm symptoms, although ALND without radiation increased the least. This study demonstrates that addressing arm symptoms per axilla therapy with patients may improve pretreatment decision-making and management expectations [23].
Quality of life (QOL) is widely examined to understand its impact on cancer therapy. This study used K. Takada et al. (2018)’s Japanese QOL-ACD-B questionnaire for breast cancer. Low QOL-ACD-B ratings before breast cancer surgery (POC) were associated with poor DFS and OS. The study indicated that poor QOL patients before POC had more extensive tumors, cutaneous infiltration, and lymph node metastasis. POC decreased QOL considerably, presumably due to adverse effects. The study observed no significant difference in QOL scores before and after POC, suggesting symptom alleviation enhanced QOL. According to this study, more mental or social QOL elements may affect prognosis [24].
Park et al. (2021) found that higher cancer stage, comorbidities, surgical complications, dissatisfaction with breast surgery, and recurrence, metastasis, or recent secondary malignancy negatively affected health-related quality of life (HRQOL) in US breast cancer survivors. The study also indicated that lower mental T and PROMIS physical scores increased death. These data demonstrate that prognostic and cancer treatment-related factors affect HRQOL in breast cancer survivors and may inform tailored survivorship care [25].
M. Rautalin et al. (2019) compared HRQoL ratings from multiple tools and examined the relationship between cancer-related symptoms and HRQoL in different breast cancer states. Health status was assessed using standard HRQoL instruments such as the 15D, EQ-5D-3L, and cancer-specific EORTC QLQ C30 questionnaires. The 15D assesses mobility, vision, hearing, respiration, sleep, and more; the EQ-5D yields utility and VAS values. The EORTC QLQ-C30 assesses symptoms, function, and quality of life. The study found that varied HRQoL instruments generate varied scores. Apparent ceiling effect on EQ-5D. Poor HRQoL was most often associated with pain and exhaustion in all illness conditions [26].
In a German study of 292 breast cancer (BC) patients, global health status/quality of life (GHS/QoL) decreased after RT and improved 6 weeks afterward before reverting to baseline after 10 years. Role function improved 10 years after diagnosis, but most functional domains decreased or stayed unchanged. HRQoL issues include emotional stress, sleep issues, and exhaustion-plagued breast cancer patients, especially those under 65. Overweight people had poorer Global Health Status/QoL and physical functioning, although living with others enhanced physical functioning and reduced dyspnea and pain. Long-term care may involve specialized screening for cancer patients at risk of psychosocial/other impairments to fulfill unmet health needs [27].
The 2020 Lewandowska et al. study revealed that quality-of-life exams are necessary to assess cancer patients’ psychological, social, and spiritual well-being, including disease symptoms and treatment effects. The study included 800 cancer patients, 60% of whom were women and 40% men undergoing chemotherapy. Although 28% of cancer patients could do typical physical activities, 81% reported severe self-care issues and anxiety/depression [28].
According to Xuan Ng et al. [29], breast cancer patients have trouble reintegrating into society and employment after treatment. The Singapore Breast Cancer Foundation and Akebono-kai in Japan offer comfort and mental health support. Breast Cancer Care in the UK provides extensive cancer treatment information. Breast cancer may be treatable thanks to advances in surgery, radiation, and drugs. Hospital care is holistic, ensuring a supportive journey for patients [29].
A Di Meglio (2022) study of 4,131 breast cancer patients from 2012 to 2015 indicated that the high-risk group had a severe and continuous deterioration in post-chemotherapy quality of life. This is mainly attributable to obesity, inactivity, and tobacco use. Endocrine therapy, younger age, comorbidities, and poverty were risk factors. The results identify patients at risk of quality of life decline and inform personalized interventions, such as early behavioral difficulties and healthy lifestyle support programs [30].
In addition, Aishwarya Sunil Kshirsagar and Surendra Kiran Wani (2020) studied 50 breast cancer patients over 20 who received chemotherapy after surgery. Participants reported excessive pain, exhaustion, insomnia, self-image, sexual dysfunction, hair loss, and systemic therapeutic side effects. This study implies that Indian breast cancer patients’ quality of life should be addressed by healthcare practitioners [31].
Research on depression, symptoms, and functioning in early-stage breast cancer patients. The study included 487 European women aged 35–68 who had completed chemotherapy or begun endocrine therapy. Depression, symptoms, and functioning were associated with a median gQoL at baseline, which improved to 74.9 ± 19.0 after one year. Social functioning, despair, and exhaustion at baseline and emotional functioning and weariness at 12 months are most affected gQoL. This study suggests that low-quality-of-life patients need psychological help and physical function improvement [32].
In 2019, Muhammad Imran et al. at King Abdulaziz University Hospital in Saudi Arabia discovered that patients with an average duration from diagnosis had superior global health status and functional scores [33].
In 2022, Tsui TCO et al. developed global quality-of-life instruments, unlike others. Using the EORTC common cancer instrument (QLQ-C30) and breast module (BR45) dimensions, the study created a new Breast Utility Instrument. QLQ-C30 and BR45 researchers questioned 408 BrC outpatients. Finally, the model contained ten dimensions: physical, role, emotional, social, body image, pain, fatigue, systemic therapy side effects, sexual, arm, breast, and endocrine therapy symptoms [34].
The EORTC QLQ-BR45 questionnaire was examined for validity and reliability among Ethiopian breast cancer patients. The study included 248 participants who completed questionnaires. The findings indicated strong internal reliability, test-retest reliability, and content validity. The questionnaire has an average CVR value of 0.76, Cronbach’s α coefficient of 0.80, and basic reliability norms, except for the arm symptom scale. Seven of the twelve hypothesized scales exhibited positive correlations, showing their utility in assessing the quality of life of breast cancer patients [35].
Despite its qualities, the EORTC QLQ-BR45 needs more studies to determine its responsiveness over time and test-retest reliability at various times [37]. Changes after a phase IV international field study may require additional investigations because the instrument is novel [36].
Over the past decade, generic and particular tools have been used to measure breast cancer patients’ quality of life (QoL). These devices have helped researchers understand how breast cancer affects patients’ physical, emotional, and social well-being. These instruments’ effects on breast cancer patient’s quality of life include the need for more specific tools, ongoing updates to reflect therapy and side effect changes, and the importance of patient-reported outcomes in clinical trials and research [38–40].
The adoption of instruments to assess the quality of life of breast cancer patients receiving chemotherapy has significant implications for future treatment and research. Continuous evaluation, the creation of particular instruments, and the significance of patient-reported outcomes are all critical topics that require attention. Understanding the long-term effects of chemotherapy on QoL will be critical in improving the lives of breast cancer patients.
Footnotes
Acknowledgements
We thank the publication management unit team of the graduate school for assisting in preparing this systematic review.
Ethics committee
Not applicable.
Conflict of interest
Each author declares that he or she has no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangement etc.) that might pose a conflict of interest in connection with the submitted article.
Data availability statement
The data presented in this study are available on request from the corresponding author.
Funding
This article received no external funding.
Authors contribution
UH, MA, and PP study design; UH, MA, and PP databases search and articles selection; All authors participate in the debate and consensus on the articles to be included. UH, ANU, and DIA manuscript writing. AA, ANU, and DIA proofreading of the manuscript.
