Abstract
Stalking is a widespread social phenomenon that, on the one hand, among those affected leads to mental disorders requiring treatment, and on the other is linked to substantial threats of violence, as well as to actual violence towards the victims. In rare cases it even leads to completed acts of homicide. A meta-analysis of 103 studies revealed that at least once in their lives up to 23% of all women and 10% of all men have been affected by stalking [1]. Studies on the impact of stalking on victims indicate that stalking has serious economical, social, medical and psychiatric consequences [2]. Our work group conducted the first, and to date only, study in a German population sample. We found a lifetime prevalence of stalking victimization of 11.6%, whereby women, at 17.3%, were affected much more often than men, for whom we found a prevalence rate of only 3.7% [3,4].
Not yet addressed is the question of how often mentally ill patients have been confronted with stalking. Since under certain circumstances a mental disorder can be a risk factor for becoming a victim of stalking, this question appears meaningful. Specific preliminary findings point in this direction, for example, victims of stalking more frequently have a dependent personality structure among [4], as do general findings that mentally ill patients on the whole are more frequently victims of crime [5,6]. On the other hand, it has already been shown that stalking victimization can be accompanied by substantially impaired psychological well-being [2,7]. A matter of great interest then is whether stalking occurred before or after the onset of the mental disorder. Since stalking correlates with impaired psychological well-being, it also appears to be important to discover the extent to which potential stalking victimization is addressed at all in the course of psychiatric–psychotherapeutic treatment. The current study explores these questions on the basis of a study of a sample of 300 patients admitted consecutively either as inpatients or outpatients to the Central Institute of Mental Health Mannheim (CIMH), Zentralinstitut für Seelische Gesundheit Mannheim (ZI).
Materials and methods
Three hundred psychiatric patients aged 18–80 years and admitted consecutively either as inpatients (295) or outpatients (5) were included in the study. Due to the low number of outpatients, differences between inpatients and outpatients cannot be analysed separately. Patients diagnosed with either a florid psychosis or dementia were excluded from the study in order to avoid systematic biases of the results due to delusions or memory disorders. Aside from these exceptions all other psychiatric diagnoses qualified as inclusion criteria. The study was carried out between May 2005 and September 2005. The stalking experiences of the psychiatric population were compiled by means of the brief version of the Stalking Behaviour Questionnaire (Stalking-Verhaltens-Fragebogen (SVF)) for victims. The SVF was developed by Dressing et al. [4] for use in a study of a German population sample.
The SVF for victims is divided into three sections. Sections A and B apply to all interviewees, Section C only to the victims of stalking. Section A tests the prevalence of stalking. Fifteen items describe typical stalking behaviours, for example, unwanted approaches by an individual. If there is a ‘yes’ answer on a least one item, Section C will be administered. Section B encompasses demographic data such as sex, age, education level and occupation of the interviewee. Recorded as well are the year of the first mental disorder and the date of the first contact to a psychiatrist or neurologist.
Section C contains special questions for victims of stalking. Fifty-one items encompass the date of stalking (present, past), duration, frequency of contact approaches, type of contact initiated, changes in the frequency, respectively the intensity of the stalking behaviour over time, contents of written communications, stalking site, relationship between perpetrator and victim, the stalker's motives, physical attacks, type of attacks, sexual harassment, as well as sexual attacks by the stalker. In addition the effects of stalking, such as anxiety, changes in daily life, physical and psychosocial effects, as well as reactions within the private environment and measures taken by the victim against the stalking are recorded.
The current study thus applies the same definition of stalking as that used in the population study on stalking [4]. Our definition restricted the presence of stalking to multiple episodes of harassment that had to be present over a minimum of two weeks, involved more than one form of intrusive behaviour (unwanted contact behaviours, e.g. loitering, following, entering the victim's home, or unwanted communications: e.g. telephone calls, emails, unwanted gifts) and provoked fear. Violence was defined as physical contact with the victim with intent to coerce or to harm. This definition includes minor forms of violence (e.g. slapping the victim in the face, poking the victim in the stomach). All analyses were carried out with the statistics programme SPSS version 10.0 for Windows. The data were evaluated by means of descriptive statistics (frequencies, means). Pearson's chi2 test was used to analyse the differences in the frequencies of nominally scaled characteristics between the victims of stalking and non-victims. In the case of low cell frequencies Fisher's exact test was used.
Results
Prevalence of stalking in a population of psychiatric patients
Stalking had affected 64 patients, or 21.3% of the total sample, at least once in their lives. The lifetime prevalence to be a victim of stalking was 21.7% among women (30/138), and 21% among men (34/162). At the time of the study six patients were affected by stalking, corresponding to an actual point prevalence of 2%. Only for 6.3% of the victims of stalking (4/64) were the responsible psychiatrists in the hospital aware that their patients were currently or earlier had been the victims of stalking.
The victims of stalking frequently reported having been violently attacked by their stalkers. Such violence occurred in the form of physical and/or sexual attacks: 48.4% of the victims had been physically attacked by their stalkers, 74.2% had been grasped and/or been physically detained against their will, 83.9% had been struck, and 38.7% of those affected had been struck, respectively attacked, with objects. In 54.7% of the cases sexual innuendoes had been made, and 26% of the victims had been sexually harassed.
Socio-demographic characteristics of the sample
The socio-demographic characteristics of the sample are presented in Table 1. The table shows that 21% of the male psychiatric patients and 21.7% of the female psychiatric patients reported having been stalked at least once in their lives. No significant relationship was found between sex and having been stalked (p = 0.874). The average age of the stalking victims in the sample was 42.13 (±11.02) years; non-victims were 44.34 (±14.61) years old (p = 0.188) on average. However, the two groups differed significantly with regard to their level of education (p = 0.029). In the current sample, stalking victims had a lower level of education than did those who were not victims.
Socio-demographic characteristics of stalking victims and non-victims
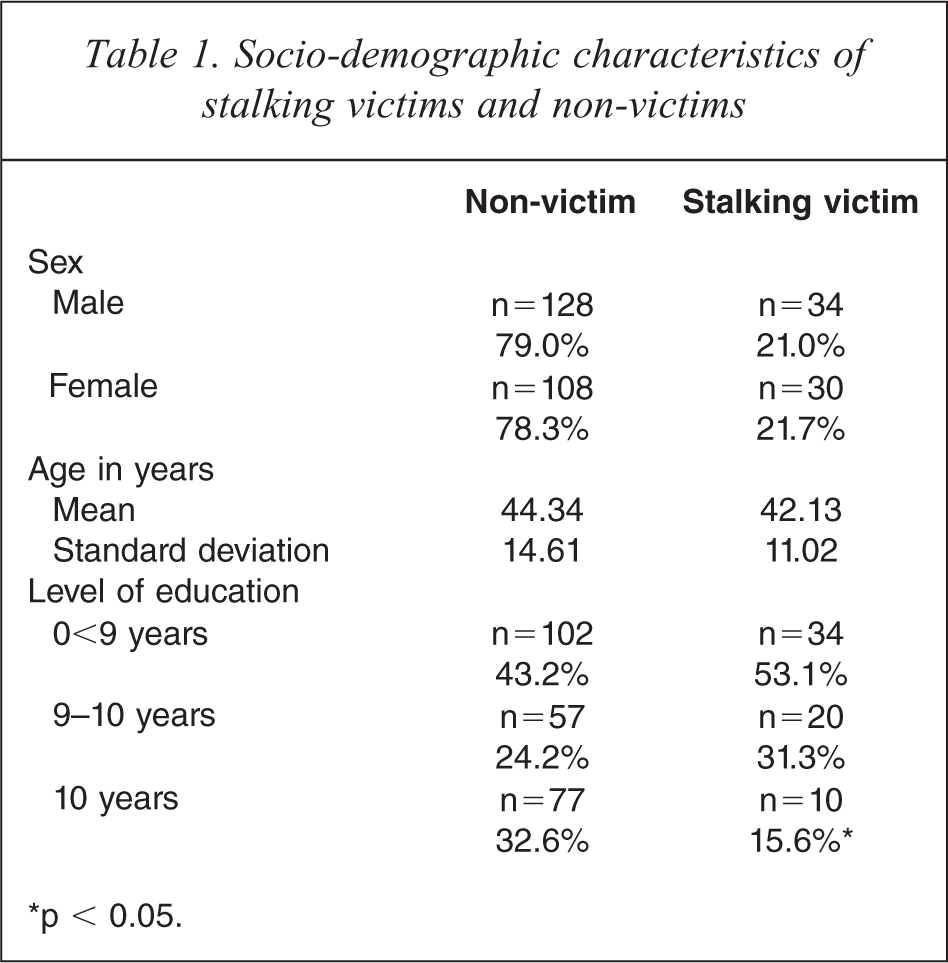
∗p < 0.05.
Duration of stalking and frequency of intrusions
The duration of stalking lasted from a period of several weeks to longer than one year. Of the interviewees 18% had been stalked for one month at the most; 43% had been stalked over several months to 1 year at the most, while for 37.5% of the victims the stalking persisted for at least 1 year or longer.
The frequency of the reported stalking behaviours varied from several times to several times a day: 3% of the victims several times had been subjected to an unwanted approach or unwanted communication, 22% had been stalked several times a month, 42.2% several times a week, 12.5% daily, and 20.3% several times a day. Our definition of stalking encompasses all forms of unwanted contact behaviours that provoked fear (e.g. loitering, following, entering the victim's home) or unwanted communications (e.g. telephone calls, emails, unwanted gifts).
The intensity of the stalking for 20.3% of the victims alternated between phases of severe and less severe harassment, 34% reported a decrease in the stalking over time, for 26.6% the frequency remained relatively constant, while 18.8% experienced an increase in the intensity of the stalking over the duration of the stalking and harassment.
Stalking methods used
Victims reported an average of five different methods of stalking. Most frequent were unwanted telephone calls (65.6%), following (57.8%), loitering in the vicinity (50%), and standing outside the front door (45.3%). For 34.4% of the victims the approach was initiated by a third party, for example by friends, relatives or the employer, 33% reported that questions about them were asked in their personal environment, 67% were sent written communications in the form of letters (29.7%), short message service (SMS) (25%), messages, for example on the car window or on the front door (7.8%), and emails (4.7%). Unwanted gifts such as flowers or chocolates had been received by 22%, 20.3% experienced damage to their possessions by the stalker, and 10.9% reported that the stalker had invaded their residence, 14% reported that orders for wares or services, such as orders to pizza services or tradesmen, had been placed in their names, 14.1% had been followed by car, and 3.1% had been sent objects that induced shock or fear, such as pornographic material, animal body parts, or excrement.
Relationship between perpetrator and victim
In 98.4% of the cases, the victim was acquainted with the stalker. Victims were stalked most frequently by their ex-partners (male and female: 45.3%). In 21.9% of the cases the perpetrator was an acquaintance (m/f), in 4.7% a work colleague, in 4.7% a stranger, and in 3.1%, a family member. Stalking by the ex-partner of their current partner (m/f) was reported by 1.6% of the interviewees, while 18.7% reported having been stalked by other persons.
According to the RECON-typology [8], 45.3% of the cases belong to the ‘Intimate’ group, 50% to the ‘Acquaintance’ group and 4.7% to the ‘Private stranger’ group.
Measures against stalking
Eighty-four per cent of the stalking victims undertook measures against the harassment by their stalkers, 70.4% of the victims talked to their stalker and forbade further harassment, 46.3% sought help from third parties, such as relatives or friends, and 29.9% defended themselves physically against an actual physical attack by the stalker. Eighteen per cent took measures to protect themselves, for example, carrying defence weapons or attending a course in self-defence, 16.7% of those affected tried to escape their stalkers by changing their residence, 1.9% changed jobs, 14.8% applied for an unlisted telephone number and 3.7% installed an answering machine, for example, in order to record messages as legal evidence. Seven per cent requested non-disclosure of information by municipal offices, while only 9.3% consulted a lawyer and only10.9% pressed charges against the stalker with the police. Sixteen per cent of the victims did not undertake any measures against their stalker, either out of fear, sympathy or helplessness.
Diagnoses
Of the stalking victims (n = 64), 46.9% suffered from an addictive disorder, 21.9% from an affective disorder, and 9.4% from schizophrenia; 14.1% had a personality disorder, 4.7% a neurotic, stress or somatoform disorder, and 3.1% some other disorder (Table 2). All of the five outpatients were diagnosed with schizophrenia. Compared to mentally ill patients who had never been stalked, the diagnosis of a personality disorder was significantly more frequent among the mentally ill who were victims of stalking (p = 0.003). Of the nine stalking victims with a personality disorder, seven had an emotionally unstable personality disorder of the borderline type, one victim had a different specific personality disorder, and one person had a combined personality disorder. A trend could be shown for the diagnosis of schizophrenia, which was less common among stalking victims (p = 0.064).
Major diagnoses of stalking victims and non-victims
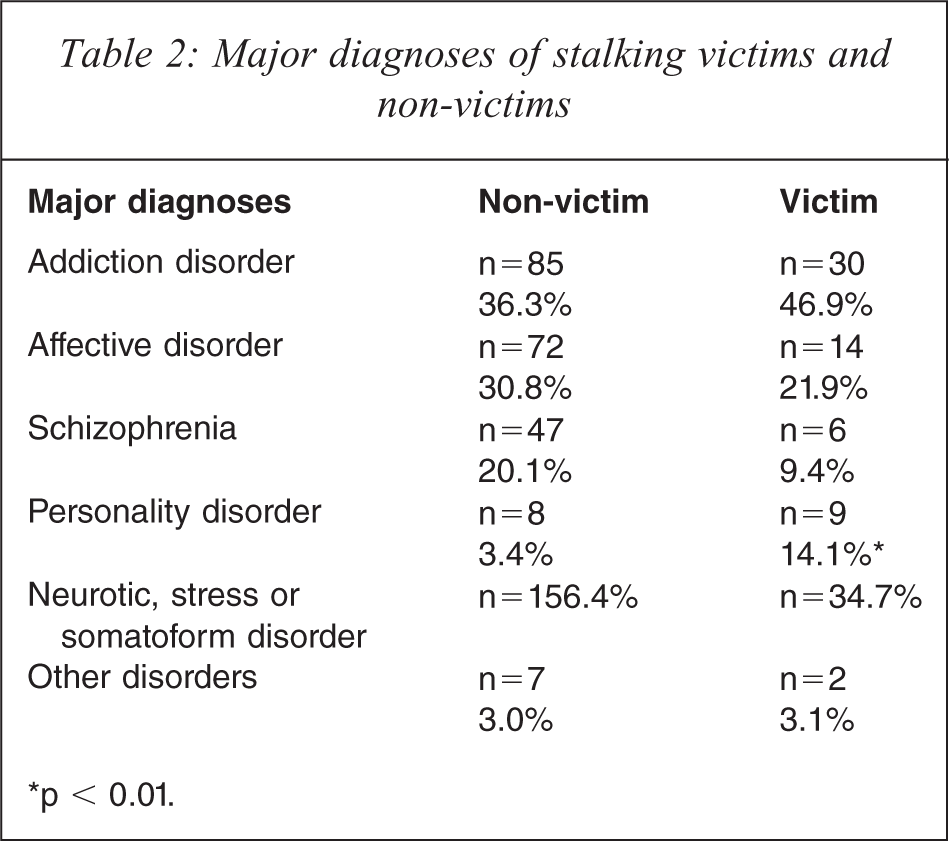
∗p < 0.01.
Of the 64 victims, 67.2% had been mentally ill prior to the stalking event, while 32.8% became mentally ill at a later point in time, after having been the victim of stalking at least once in their lives.
Discussion
In the current study 21.3% of the psychiatric patients had been a victim of stalking at least once in their lives [9]. This finding is twice as high as that in the German population study [4], with a lifetime prevalence of 11.6% (Table 3). Other epidemiological studies reported higher lifetime prevalence rates of stalking victimization: 12–32% among females, and 4–17% among males [2,10,11]. Therefore we cannot ultimately rule out that for unknown reasons rates in the Mannheim community sample were lower than those observed in other community studies. Since we used exactly the same questionnaire and the same definition of stalking in both our hospital sample and in the community study [4], the described difference between the two samples seems to be valid. This notion is supported by the finding of a different gender distribution in the hospital sample that has not been observed in any community study. The lifetime prevalence among women in the current study was 21.7%, and 21% among men. All previously published population studies show that women are significantly more often a victim of stalking than are men. In the general population, female gender is thus the greatest risk factor for stalking. In the psychiatric population studied here, however, it is obvious that men were stalked as often as women were.
Stalking in a community sample in Mannheim compared to a sample of psychiatric patients in Mannheim

The different rates of prevalence and sex distributions in the psychiatric patient population and in the general population may be due on the one hand to a mental disorder, which constitutes an independent risk factor for becoming a victim of stalking. On the other hand, the different rates of prevalence might also be due to a substantial impairment of psychological well-being due to stalking that culminates in a mental disorder requiring treatment.
Several epidemiological studies have proven that the psychological well-being of stalking victims is significantly impaired [7,12]. On the basis of the cross-sectional methods applied in the studies published to date, however, no statements can be made as to the causality; that is, whether the mental disorder is the cause or the result of victimization by stalking. For this reason, in the current study it was also asked whether the stalking had occurred before or after the first manifestation of the mental disorder. Among the majority of the stalked victims in this study, the mental disorder had manifested itself prior to the stalking victimization. Therefore a causal origin of the mental disorder due to the psycho-traumatic consequences of the stalking experience cannot be assumed, at least not for the stalking victims studied here. A different direction of causality should thus be discussed: does the presence of a mental disorder increase one's risk of becoming a stalking victim?
Since stalking is conceived of as a type of criminal activity, and the mentally ill are on the whole more likely to become victims of crime [5,6], it stands to reason to assume that the clearly increased rate of prevalence of stalking victimization in a population of psychiatric inpatients can be explained at least partially by this mechanism.
With regard to the psychiatric diagnoses, personality disorders occurred more frequently among the stalking victims, while no significant differences in the remaining diagnoses were found.
Even if a (co-)causality of the mental disorder due to the stalking victimization cannot be assumed for the majority of the stalking victims in the psychiatric population studied here, since the mental disorder preceded the stalking, a negative influence on the course of the mental disorder due to that additional stressful experience must nevertheless generally be taken into account. However, in only four of the cases were the responsible psychiatrists in the hospital aware of the fact that their patients were currently still being stalked or had been stalked earlier.
Both the duration of stalking and the frequency of intrusions were higher in the psychiatric population than in the community sample in our earlier study [4]. These results show that a victim's mental disorder can modify the appearance of stalking and increase its severity.
In 32.4% of the cases, the psychiatric patients had received written threats. A similar result (34.6%) was also shown in the Mannheim population sample [4]. Several studies found a correlation between threats and stalking violence [13–15]. Harmon
The measures taken by psychiatric patients against the stalking were generally comparable to those found in the Mannheim population sample. The most frequent measure taken by both populations was to talk to the stalker in order to preclude further harassment, whereby the psychiatric patients (70.4%) sought a discussion with the stalker more often than victims from the general population (50%). A further difference between these two samples is that the psychiatry patients filed a complaint with the police less often (10.9%) than the Mannheim population sample (20.5%). However, the frequency in either sample is low. Since the study in the sample of psychiatric patients was carried out two years later, at a time when the counselling programme of the police within the framework of the Mannheim Model Project against Stalking was then well established [18], the even lower number of complaints in the hospital sample is striking. These results indicate that those affected by stalking are still not sufficiently aware of the counselling programme and that mentally ill victims of stalking take advantage of it less often. Therefore the treating psychiatrist should assist mentally disordered victims of stalking in the use of police assistance. The current results make it clear that a greater awareness of the topic of stalking with regard to mentally ill persons is needed and that active counselling should be provided by therapists in cases of specific indications of stalking victimization.
Since the responsible psychiatrists at the hospital were aware of the stalking histories of their patients in only 4 out of 64 cases (at the time of treatment, the patient was either currently still being stalked or had been stalked earlier), the inclusion of stalking as a topic in the case histories of psychiatric patients should be considered in order to identify victims and provide them with adequate counselling and support within the framework of therapeutic treatment.
The results of our study suggest that mental illness should be discussed as an independent risk factor for stalking victimization. Furthermore, our data suggest that stalking in psychiatric patients is more severe in terms of duration, frequency and violence. By no means should these findings be used as an argument to blame the victim, but should instead give rise to greater awareness by psychiatrists. Stalking victimization in psychiatric patients seems to be a common, but in clinical practice underestimated, phenomenon that requires active management.
Footnotes
Acknowledgements
