Abstract
It is estimated that one in five Australians will meet criteria for a mental disorder in any 12-month period [1]. Yet despite the relatively high proportion of individuals who experience mental illness, Australia continues to grapple with the provision of a comprehensive and effective mental health service which meets the needs and demands of the community [2]. In recent years, there have been a number of significant mental health reforms, which have dramatically altered the structure and provision of services across Australia and other Western countries [3]. This has contributed to a growing recognition that Australia's public mental health service may be performing at a sub-optimal level, evidenced by data suggesting that a significant proportion of people experiencing mental illness are not in contact with mental health services [4]. There has also been criticism about the treatment, or lack thereof, of dual-diagnosis clients within the current system [5].
Contemporary Australian research demonstrates that persons with affective disorders are most likely to make contact with mental health services [4]; not surprising perhaps given the relatively high prevalence of these disorders in the community [1]. Conversely, low-prevalence disorders, typically affecting less than 1% of the population, continue to account for a significant proportion of disability in the community. Patients with psychotic disorders are recognized as having high treatment needs, and the effective management of schizophrenia represents a major public health issue [6].
To optimize the provision of cost-effective and accessible services, it is necessary to establish both the ‘need’ and ‘demand’ for them. While need may be expressed by a bottom-up count of community prevalence estimates, demand is better captured by service utilization statistics [2]. For many mental disorders, there will be a marked discrepancy between the number of persons experiencing an illness (‘need’), and the number who make contact with public mental health services (‘demand’). In the schizophrenias, however, it is likely that rates of contact with public health services will closely parallel the true prevalence of disorder in the community, as most individuals come into contact with public services at some point during the course of their illness. For example, recent Australian research that used rates of contact with public mental health services to estimate the lifetime prevalence of schizophrenia, reported an estimated lifetime prevalence of 0.7% [7], a figure broadly consistent with other extant research reporting lifetime prevalence estimates between 0.4% and 0.9%, and point prevalence estimates between 0.2% and 0.5% [8–11]. Therefore, schizophrenia is notable for its relatively stable prevalence across both time and culture, despite significant changes in mental health service, treatment protocols and social structure over time [3,7,8].
Against this background, the present study aimed to measure the number of persons with both high- and low-prevalence disorders identified and treated in the public mental health system in the Australian state of Victoria (population 5 346 480) [12]. Furthermore, the number of persons treated for psychosis in the public mental health system was used to estimate the prevalence of schizophrenia within the community. These estimates were then compared with previous Australian data to explore the temporal stability of schizophrenia prevalence over time [7].
Method
This design involved linking data from two electronic databases: (i) the electoral roll for the Australian state of Victoria, and (ii) the statewide Victorian psychiatric case register (VPCR). The Victorian electoral roll lists the full name, age and gender of all Victorian adults legally registered to vote. Electoral registration is compulsory for all Victorian adults. It is updated monthly to ensure deceased persons are removed from the register [13] and captures over 93% of eligible voters, thus providing a good representation of the state's adult population [14]. Five thousand randomly selected names (2500 men and 2500 women) were extracted from the electoral roll, detailing the full name, gender, and age (within a 2-year age band).
Developed in 1961, the VPCR is considered one of the world's oldest and most comprehensive psychiatric registers [15]. It records virtually all contacts that individuals have with the statewide public mental health system; including details of all diagnoses, admissions, and receipt of treatment services (L. Rimes, personal communication). Diagnoses are recorded by qualified mental health professionals at the time of service discharge or within 1 month of admission, thus representing actual clinical diagnoses that are kept contemporaneous due, in part, to financial incentives to maintain up-to-date records. The International Classification of Diseases (ICD-9 or ICD-10) is used for recording diagnoses [16,17].
The VPCR has undergone a number of revisions with the most recent redevelopment occurring in 2000. Persons with contact with the system prior to, but not since, 2000 have their psychiatric history retained in archive, while any record with post-2000 contacts are listed fully on the contemporary register. The register does not include mental health services provided by general practitioners or by private clinicians, but does include contacts by non-Victorians, including interstate and international citizens. However, contacts by Victorian citizens with services in other Australian states are not recorded (L. Rimes, personal communication). All involuntary admissions and mandated psychiatric treatment services occur in the public sector. As a result, arguably the vast majority of individuals with a schizophrenia-spectrum disorder have contact with the public mental health system at some point during the course of their illness [18]. The VPCR therefore provides a useful estimate of the lifetime prevalence estimate for schizophrenia [7].
The 5000 names from the electoral roll were linked with the VPCR. Using an exact matching procedure, an electoral roll case was matched with a VPCR record if the full name, gender and age category matched completely. As a number of very common names received multiple matches on the VPCR, any name which resulted in more than three matches (n = 84) was removed from the sample. It was also rare, but possible, that one individual may have two separate mental health records listed on the register as a result of human error during data entry. Therefore in cases of duplicate or triplicate matches (n = 22), each case was individually compared on key variables (including full name, gender, date of birth, diagnosis, employment status, education level and marital status) to determine whether the records were of the same individual. All 22 records were judged to be the same case and were collapsed into one case. This reduced the sample to 4916 persons, of whom 610 were identified on the VPCR. However, 86 of these individuals had had no contact with the public mental health system since the database was upgraded in 2000, and their records had been archived. The gender and mean age of the 86 archived records were compared with that of the 520 remaining mental health service users. There were no differences between the proportion of males and females in the archived and the remaining service users (χ2=0.95, df = 1, p = 0.33), however archived cases had a significantly higher mean age than the remaining users (t = −11.75, df = 190.36, p < 0.001). Nevertheless, as it was not possible to extract a detailed psychiatric history for the archived records, these were permanently removed from the dataset, leaving a total sample of 4830. A full psychiatric history for the remaining 520 mental health service users was extracted from the register.
Psychiatric diagnoses were coded into categories of interest, replicating those used in previous Australian research to allow for temporal comparisons to be made [7]. Inclusion criterion aimed to capture the more chronic and severe forms of non-organic psychosis that most closely resembled schizophrenia in clinical presentation. Therefore, ‘schizophrenia’ included all subtypes of the disorder (ICD-9 code 295 and ICD-10 code F20). ‘Schizophrenia-spectrum disorder’ was considered a broader term and included schizophrenia, schizoaffective disorder, schizotypal disorder, shared psychotic disorder, delusional disorders, and unspecified non-organic psychosis (ICD-9 codes 295 and 297, plus ICD-10 codes F20, F21, F22, F24, F25 and F29). The latter excluded organic or transient forms of psychosis, such as substance-induced psychosis, depression with psychotic features, or senile psychotic conditions.
Cases were only included if the initial diagnosis of schizophrenia (or schizophrenia-spectrum disorder) was upheld on at least 75% of subsequent diagnoses, or if there was a clear diagnostic progression over time culminating in a schizophrenia/schizophrenia-spectrum diagnosis. Cases failing to meet this criterion were classified as ‘mixed/other psychotic disorder’. This method has been demonstrated to have good diagnostic reliability [18].
A ‘substance-use disorder’ was defined as any type of substance dependence, substance abuse, or substance-induced disorder, with the exception of nicotine-related disorders. Substance intoxication was not included because acute intoxication is not necessarily indicative of a substance-use problem, however, substance-induced psychosis was.
Once data linkage was complete, the dataset was de-identified by permanently removing the personal identifiers of first name and surname in accordance with ethical guidelines [19]. For those persons with a mental health record, age at 31 July 2008 was calculated from the date of birth, as recorded on the psychiatric register. For persons with no mental health record, age was taken as the lower limit of the 2-year age group provided by the electoral roll (i.e., age 20–21 was coded as age 20). Descriptive statistics were used to characterize the prevalence of psychiatric diagnoses and service utilization.
The study was approved by the human ethics review committees at Monash University, the Victorian Department of Human Services and Victoria Police, in accordance with the Australian National Health and Medical Research Centre guidelines [19]. Data used in this research were not originally collected for the purposes of this study, and the design precluded the provision of informed consent from the individuals whose information was accessed. In recognition of these ethical issues, care was exercised throughout the linkage to ensure that anonymity was maintained and confidentiality upheld. Data were analysed at group level only, so it was not possible for individuals to be identified from the results.
Results
The community sample comprised 4830 cases (2392 males, 49.5%). Their mean age was 39.2 years (SD = 12.4; range 18–63 years). In total, 520 (10.8%, 279 males and 241 females) had made contact with the public mental health system. There were no significant differences in the age (p = 0.35) or gender (p = 0.06) between those with and without a mental health history.
There were roughly equal proportions of men (53.7%, n = 279) and women (46.3%, n = 241) among the 520 who had been mental health service users. Almost half (n = 259) had never married, 29.2% (n = 152) were married/de facto and 15% (n = 78) were separated or divorced. Seven (1.4%) were identified as Indigenous Australians, as compared to 0.6% of the Victorian population [20].
A psychiatric diagnosis was recorded in 320 of the 520 service users (61.5%), therefore 200 people (38.5%) registered on the VPCR had not received a psychiatric diagnosis. Of those who had been diagnosed, 311 had an Axis I diagnosis, and 40 had an Axis II diagnosis (37 personality disorder and three mental retardation diagnoses). A secondary psychiatric diagnosis was recorded in 35.6% (n = 114) of those with a primary Axis I diagnosis and in over 80% (n = 30) of persons with a personality disorder.
The majority of service users (70%, n = 56) who had been diagnosed with a substance use disorder also had a comorbid psychiatric illness. There were relatively few individuals (n = 24) with a substance use disorder in the absence of other psychiatric illness, and only 15.4% of service users (n = 80) had any recorded history of a substance use disorder. Eight of those with a mental illness (20.1%) were diagnosed with comorbid substance use disorders.
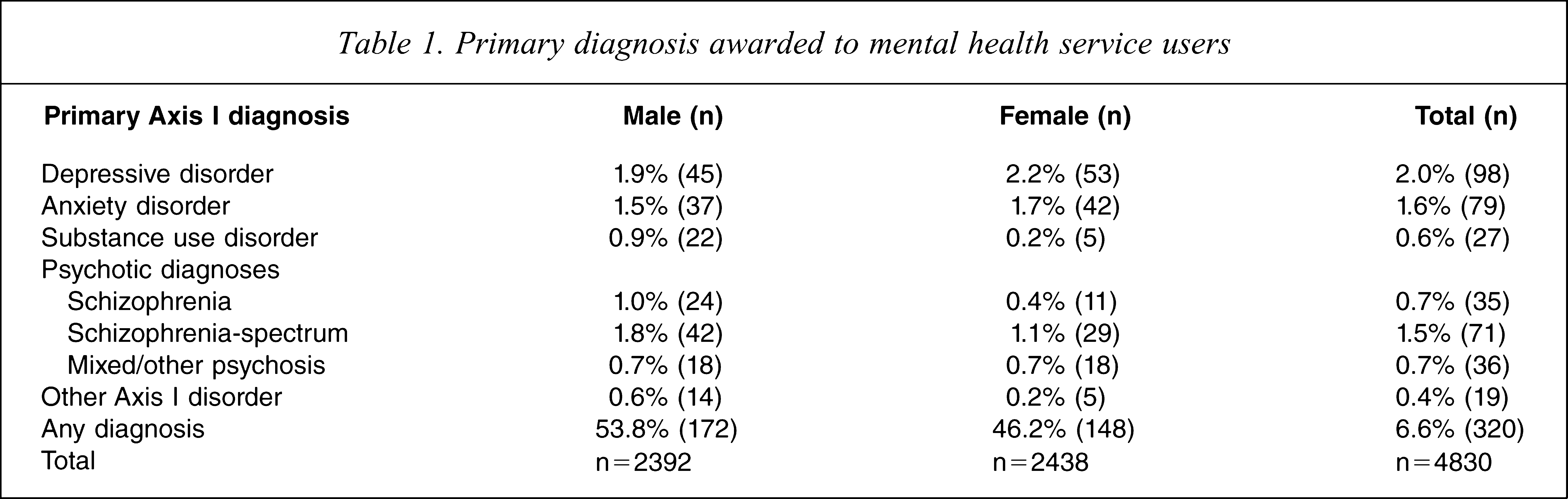
Depressive, anxiety and psychotic disorders were the most common primary diagnoses identified (Table 1). Schizophrenia was diagnosed in 0.7% (n = 35) of the sample, with an additional 0.7% (n = 36) meeting criteria for a schizophrenia-spectrum disorder. Rates of schizophrenia were significantly higher among males (1.0%) than females (0.4%), (χ2 = 5.04, p = 0.03). There were no significant gender differences in the rates of schizophrenia-spectrum disorders (χ2 = 0.02, p = 0.978). The mean age of first schizophrenia diagnosis was 31 years (SD = 9.4) in men and 36 years (SD = 9.4) in women. The mean age of first contact with the public mental health system for those with schizophrenia was 30.1 years (SD = 9.4) in men and 34.1 years (SD = 10.6) in women.
Primary diagnosis awarded to mental health service users
Psychiatric diagnosis or ongoing treatment were provided to 73.3% (n = 381) of those who had contacted the public mental health system, while the remaining 22.9% (n = 119) had no record of diagnoses or treatment. Many of the latter were awarded a non-psychiatric diagnosis pertaining to psychosocial circumstances or other healthcare needs (e.g. ICD-10 code R52.0 ‘acute pain’ or Z59.0 ‘homelessness’), while some were incredibly specific (e.g. code W02 “fall involving ice-skates, skis, roller-skates or skateboard”) [16,17].
The types of services accessed by those who were diagnosed and/or treated by the public system was variable. Over three-quarters (n = 291) had at least one contact with outpatient community services, with an average of 44.4 outpatient contacts (SD = 90.5) per person. Over half (50.6%) of the 12 911 contacts recorded by the sample were attributed to just 6% of these individuals (n = 23); 83% of whom had a schizophrenia-spectrum disorder as their primary diagnosis (n = 19). The age of first contact ranged between 7.7 and 59.9 years, with an average age of 32.5 years (SD = 13.2). On average, the first diagnosis of schizophrenia at 32.6 years (SD = 9.5) (in men, 31 years, SD = 9.4, and in women, 36 years, SD = 9.4).
The most common diagnosis in outpatient mental health services was a depressive disorder, although schizophrenia-spectrum disorders accounted for the majority of more intensive contacts (Table 2). There were few gender differences in service utilization patterns, although most males contacting a psychiatric crisis service were diagnosed with a schizophrenia-spectrum disorder (41.1%, n = 73), while females more commonly presented with depressive illnesses (28.6%, n = 77).
Types of service contacts by persons diagnosed and/or treated for psychiatric disorder
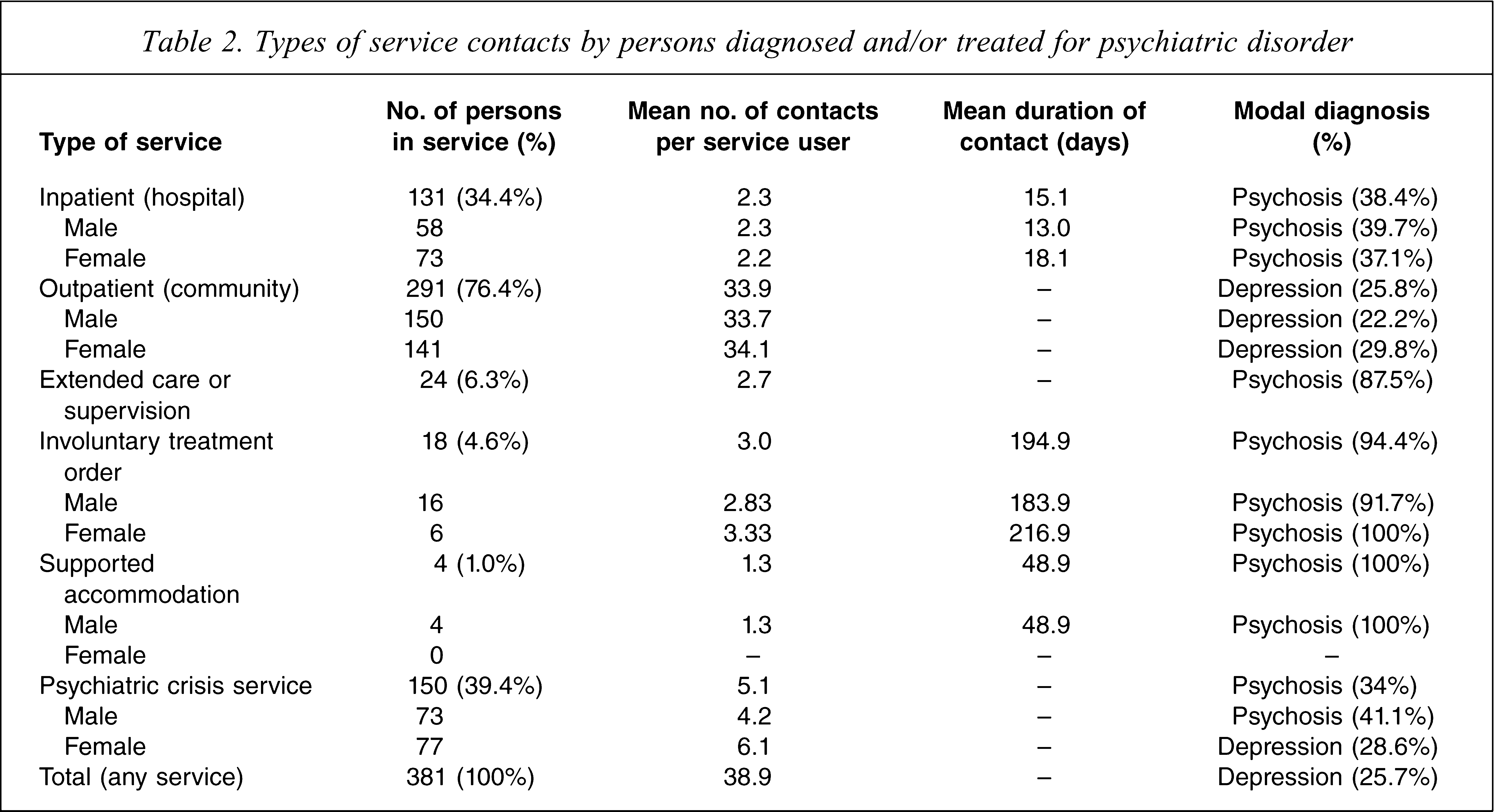
Almost 40% (n = 150) of persons with a history of diagnosis/treatment made at least one contact with the mobile crisis service; this figure rose to 71.8% (n = 50) of people with a schizophrenia-spectrum disorder. Psychiatric hospital admissions occurred in about one-third (n = 131, 34.4%) of those with any history of diagnosis/treatment, and 71.4% of persons with a schizophrenia-spectrum disorder. On average, the first admission occurred at 34.4 years (SD = 10.2) and lasted for 12.4 days (SD = 11.8, median 10 days).
Extended care and supervision contacts were defined as any supported accommodation/continuing care unit, psychiatric rehabilitation, or involuntary community treatment orders. These contacts were relatively rare, with only 6.3% (n = 24) having used these services; 21 of which (87.5%) were diagnosed with a primary schizophrenia-spectrum disorder. The average length of stay in supported accommodation was approximately 6 weeks, and the average involuntary treatment order lasted just over 6 months.
Discussion
The present study examined rates of service utilization in the public mental health system in a sizeable random community sample. The use of a statewide psychiatric case register provided a robust estimate of the number, type and duration of lifetime contacts with the public mental health system in Victoria.
Limitations of the study
Although case-linkage studies are considered methodologically robust, there is an inevitable degree of error attributable to both the original data entry and data-matching procedures adopted [21,22]. The current study used data routinely collected for non-research purposes, thus limiting the breadth, depth and quality of information available. A further consideration using the VPCR is that it does not provide information on suicides, and is an unreliable indicator of self-harm incidents. Notwithstanding these limitations, these data provide a contemporary summary of public mental health service utilization in Victoria.
Use of public mental health services by the community
One in 10 of the random community sample had made contact with the public mental health system at least once, with 6.5% receiving a psychiatric diagnosis at some point. Over one-third of people who made contact with the public mental health service were not given a psychiatric diagnosis. This highlights that community members are making contact with public mental health services for a variety of reasons, many of which apparently fall beyond the scope of psychiatric care. This raises the question of whether the public mental health system is equipped to handle such demand, and whether this demand may be better met by other services.
Conversely, a notable proportion of the community was diagnosed with a high-prevalence psychiatric disorder, but did not go on to receive treatment within the public system. Presumably, this group were primarily treated by private clinicians and general practitioners, as demonstrated in recent Australian research [4]. Using mental disorder prevalence estimates as a basis [1], the current findings indicate that less than 10% of people with a primary diagnosis of anxiety or depression receive their primary treatment from the public mental health system. This pattern of service use is consistent with an increasing shift towards private and community-based care for the high-prevalence disorders following the introduction of Federal government rebates for psychological and psychiatric treatment in 2006 [3,23,24].
Australia's mental health system has undergone a number of changes since the development of the National Mental Health Strategy in 1993 [3]. A decade ago, the average length of an inpatient stay for a patient with psychosis was 6 weeks [25]; today, that figure is less than 2 weeks. In addition, the past 10 years have witnessed a corresponding increase in community-based mental health care in Australia, with 88.7% (n = 63) of patients with a psychotic disorder in the current sample accessing an outpatient treatment service, compared to around 60% 10 years ago. Similarly, the proportion of people with schizophrenia who contacted a community-based psychiatric crisis service has risen from 54% to 71.8% over the same time period [25]. The most intensive outpatient services were almost exclusively accessed by persons with schizophrenia-spectrum disorders. However, the relative absence of high-prevalence disorders within this service should not imply that these individuals do not require high-intensity outpatient care. Rather, it reflects how scarce resources are allocated, with a predominant focus on the provision of intensive services to psychosis patients [23].
Treatment of substance-related disorders in the public system
Despite well-documented comorbidity between substance use and mental disorder [5], the utilization of public mental health services by persons with dual-diagnosis was low. Only 1.6% of the sample had a recorded history of a substance-use disorder, and less than 1% had this as their primary diagnosis. This suggests that public mental health services are not the primary service destination for persons with substance use disorders. Furthermore, those individuals who are treated for substance-use in the public sector are unlikely to have a substance-use problem in isolation from other mental disorders. Nevertheless, there is a noticeable demand for substance abuse treatment, with up to one-fifth of people receiving treatment for mental illness also having a diagnosable substance use disorder.
Typically, drug and alcohol services in Australia are provided in parallel with mental health services, with many individuals receiving separate, yet concurrent, treatment from different services. As a result, too many people with dual diagnosis ‘fall through the cracks’ and fail to receive adequate care for both their mental health and substance abuse needs [26,27]. In light of these concerns, there is growing recognition for the need of an integrated care model to manage effectively the co-occurrence of mental disorder and substance abuse [28]. The present findings support this proposal, demonstrating a clear demand for a more streamlined approach to dual diagnosis.
Estimated lifetime prevalence of schizophrenia in the community
The present study provided a means of estimating the lifetime (period) prevalence of schizophrenia in the community. Consistent with previous international and Australian research, the lifetime prevalence estimate for schizophrenia was 0.7% [7,8,10,11]. This consistency provides support for the temporal stability of schizophrenia prevalence, despite notable changes in both society and the mental health system [3,7].
The mean age of first contact for those with schizophrenia was higher than might be expected, particularly for the women. These data provide some support for the argument that females have a later age of schizophrenia onset than males [29,30]. However, the current findings are somewhat inconsistent with recent Australian data which had a lower age of schizophrenia onset in the mid to late twenties [6]. The reasons behind this discrepancy are unclear. One could speculate that first episodes of psychosis are identified by general practitioners and private clinicians, and that patients with schizophrenia only come into contact with the public system in later years (perhaps in the context of a compulsory hospital admission). Alternatively, there may be some differences in the models of service and diagnostic practices of various jurisdictions which could explain this variation. For example, there is some evidence that particular diagnostic subtypes (such as paranoid schizophrenia) have a later age of onset than other subtypes [29]. A more in-depth examination of the psychiatric case files, and the inclusion of a larger schizophrenia sample, may provide further insight into this apparent discrepancy.
Conclusion
The structure and provision of mental health services in Australia is changing rapidly, with a shift towards fewer public hospital beds, shorter inpatient stays and more community-based services [3,23]. The past decade has seen significant reform in Australia's mental health strategy, and all indications point towards this change continuing [28]. Reforms have led to a concentration of psychotic disorders in the public mental health system at the apparent expense of high prevalence and substance use disorders. Despite affecting less than 1% of the population, schizophrenia-spectrum disorders therefore consume a disproportionate amount of public mental health resources.
Against this background of change, one must consider whether the public mental health service is equipped to deal with the panoply of mental health needs that exist. People continue to make contact with public mental health services for a variety of reasons, many of which fall beyond the scope of psychiatric care. This is contributing to a growing tension between need, demand and supply of mental health services in the community, with mental disorder forming only one component of the demand. Until we find a way to balance these forces, it is likely that we will continue to grapple with the effective management of community-based models of mental health care.
Footnotes
Acknowledgements
