Abstract
Excessive crying and sleep disturbance occur commonly in the first 3 months of life [1–4]. Such problems usually undergo a natural resolution by 3 months [5–7], but in some cases they can continue throughout the first postnatal year and beyond [8–10]. Given that unsettled infant behaviour is known to be associated with a range of later negative child outcomes, including compromised physical development and childhood sleep and behavioural disorders [11–17], the importance of providing effective early interventions is clear.
Evidence suggests that there are relationships between unsettled infant behaviour and infant temperament or organic factors [18–22], and between unsettled infant behaviour, psychosocial/family environment issues and maternal characteristics [23–29]. Early authors focused on the role of maternal psychopathology as a cause for infant sleep disturbance [30,31], but in more recent years it has been suggested that unsettled infant behaviour may also influence maternal mood, and that chronic maternal sleep deprivation associated with unsettled infant behaviour may be a common precipitant for depression in this population [9,32–34]. Overall, most authors agree that persistent infant crying and sleep disturbance develop, and are maintained, through dynamic interactions between infant, maternal and environmental factors [24,35–41].
In Australia, a number of residential mother-infant units have been established to provide interventions for families with unsettled infants. Given the known multi-factorial nature of infant sleep disturbance, these programmes typically utilize a multi-faceted approach. Staffed by multi-disciplinary teams of child and family health nurses, enrolled parent-craft nurses, psychologists, social workers, early childhood workers, psychiatrists and paediatricians, these intervention programmes aim to facilitate improvements in infant, caregiver and environmental domains.
Residential mother-infant intervention programmes have been shown to be associated with positive outcomes. Leeson et al. evaluated outcomes for 20 families (with 23 infants) with infants aged 8–12 months admitted to a residential mother-infant programme in South Australia [42]. One month after the admission, there were significant reductions, compared to pre-admission levels, in the number of times that the infants woke, fed and were awake at night, and there was significant reduction in maternal depressive symptomatology. Three months after the admission, 20 of the 23 babies were reported to be sleeping well. Don et al. examined outcomes for 109 singleton infants (aged <20 weeks) admitted to a mother-infant residential unit in Sydney [43]. These authors observed significant improvements in infant behaviour (time asleep, awake, content and unsettled) by the fourth day of the admission. One month after the admission, there were further improvements in child behaviours, and parents rated their children as less difficult to manage. Fisher et al. followed two samples of families (n= 108 and 81, respectively) for 6 months after an admission to a mother-infant residential unit in Melbourne [44]. Results indicated significant improvements in infant behaviour (crying, fussing, frequency of night-time waking, and sleep and feeding dysregulation) and in maternal mood (depressive and anxiety symptomatology) 1 month after the intervention, with changes being sustained at 6 months. The absence of a control group has been a major limitation of all of these studies because it has meant that it has not been possible to determine the extent to which improvements in infant behaviour were developmentally related. Given the dramatic improvements seen during the very brief interventions (4–5 days), however, it is unlikely that infant gains were attributable entirely to developmental issues.
Hence, when patients are considered as a whole group, it is clear that residential mother-infant intervention programmes are associated with positive outcomes for mothers and infants. Rates of maternal depression and anxiety disorders in residential unit populations are high [25,45,46], however, and it is possible that maternal psychopathology may have an impact on outcomes or that there may be subgroups of women with depression or anxiety who do not benefit from the intervention. To date, this is not an issue that has been well investigated.
Hiscock and Wake conducted a randomized controlled study evaluating the effectiveness of an outpatient behavioural intervention for unsettled infant behaviour compared with written information describing normal infant sleep patterns [34]. Results showed the intervention to be associated with significant improvements in infant behaviour and maternal mood 2 months after the intervention. It was also found that for the subgroup of mothers in the sample with initial Edinburgh Postnatal Depression Scale (EPDS) scores in the clinical range for major or minor depression (i.e. >9), EPDS scores fell in both the intervention and control groups, but the degree of improvement was significantly greater in the intervention group, at both 2 and 4 months. In addition, the only factor that predicted an increase in depression scores was a persistent infant sleep problem. Hiscock and Wake's findings are important because they show a behavioural intervention to be effective in bringing about improvements in infant sleeping problems and maternal depression, whether or not the mother is in the clinical range for depression at the commencement of the treatment [34]. The results of that study, however, were limited by the reliance on self-reported questionnaires to measure depressive symptomatology and infant behaviour, and the fact that the sample included only women recruited from community-based well-baby clinics who self-reported infant behaviour difficulties and it excluded those who were receiving treatment for postnatal depression. It is therefore possible that results may not be generalizable to those with severe infant behaviour difficulties or severe postnatal depression. Further, the fact that it was an outpatient programme means that the generaliz-ability of results to a residential programme is not known. In the only study, to date, to examine differential outcomes of a residential mother-infant programme for mothers with and without depression, Matthey and Speyer examined changes in maternal depression and anxiety symptomatology, maternal bonding to the infant and maternal perceptions of changes in infant behaviours [47]. Results showed significant improvements on all outcome variables at 5 weeks and 4 months after discharge, and showed no differences between women who were high and low on depression or anxiety in terms of the amount of change they perceived to have taken place on the infant-related presenting problem. Once again, that study was limited by its reliance on questionnaire-based measures of psychological symptomatology and by maternal reports of perceptions of improvements in infant behaviour.
To date, there have been no investigations of the differential outcomes of residential interventions for unsettled infant behaviour for mothers with and mothers without a diagnosis of depression or an anxiety disorder. A further limitation of all previous studies has been the reliance on maternal ratings of infant behaviour. The present paper reports two studies that sought to bridge this gap by (i) examining the effect of a residential parent-infant intervention on infant behaviour, maternal depression, maternal anxiety and parenting stress; and (ii) examining the impact of maternal psychopathology (self-reported maternal depressive symptomatology and diagnosed DSM-IV maternal depressive and anxiety disorders) on infant behavioural outcomes of the intervention.
Method: study 1
Participants and procedure
A series of 151 English-speaking mothers with singleton infants aged 0–12 months admitted consecutively to the Karitane Residential Family Care Unit (RFCU) between October 2004 and April 2005 were invited to participate in this study. In total, 104 women (69%) agreed to participate. Of the 47 patients who were asked but did not participate in the study, 35 declined and 12 agreed but were subsequently prevented from participating because of practical constraints associated with the admission or because they went home early. Participants completed self-report measures during the admission and RFCU nurses recorded participants’ infants’ behaviours for the duration of the admission using 24 h infant behaviour charts. The mean ± SD maternal age of participants was 30.90 ± 5.34 years; 93% were in a married or de facto relationship and 44.1% were university educated. The mean infant age was 5.86 ± 3.08 months; 55.3% of infants were first borns and 56.3% were male.
All participants were mailed self-report follow-up measures with pre-paid return envelopes at 1 and 3 months after discharge. Completed questionnaires were received from 73 participants (70.2%) at 1 month after discharge, 65 (89.0%) of whom also returned 3 month questionnaires. Missing data were replaced for the eight participants who returned 1 month but not 3 month questionnaires using the last observation carried forward method, leaving a total of 73 participants for the longitudinal follow up. Women who completed the study (n = 73) were slightly older than those who withdrew or were lost to follow up (n =31, t(102) = 2.35, p = 0.021, d = 0.51), but there were no significant differences between the groups in terms of infant age (t(102) = 1.80, p = 0.076, d = 0.39), parity (χ2(1,103) = 0.635, p = 0.425, w = 0.41), or admission EPDS score (t(98) = 0.740, p = 0.461, d = 0.16).
Measures
Edinburgh Postnatal Depression Scale
The EPDS is a validated 10-item self-report measure for depressive symptoms in the perinatal period [48]. The EPDS yields a maximum score of 30, with higher scores indicating greater symptom severity. EPDS scores > 12 are considered to be indicative of probable major depression and scores between 10 and 12 are considered to be indicative of probable minor depression.
Hospital Anxiety and Depression Scale
The Hospital Anxiety and Depression Scale (HADS) is a validated 14-item self-report scale that was developed to detect states of depression and anxiety in hospital or medical outpatient clinic settings [49]. The seven-item anxiety subscale of the HADS (HADS-A) was used in the current study. HADS-A scores >7 are thought to be indicative of clinically significant anxiety symptoms and scores >9 are thought to be indicative of a probable anxiety disorder.
Parenting Stress Index-Short Form
The Parenting Stress Index-Short Form (PSI-SF) is a validated 36-item self-report measure of stress in the parent-child system [50]. The PSI-SF consists of three subscales: Parental Distress, Parent-child Dysfunctional Interaction, and Difficult Child. Higher subscale and total stress scores indicate greater dysfunction. Total stress scores >90 are thought to be indicative of clinically significant levels of parenting stress.
24 h Child Behaviour Chart
Infant behaviours (awake time, sleeping, crying, screaming, grizzling, feeding) were recorded on 24 h charts similar to those described, validated and used in previous studies [51–54]. The charts were completed by RFCU nurses for the duration of the RFCU admission. A coder (JP), who was blind to maternal EPDS score, examined infant behaviour charts to calculate three variables: (i) total sleep time; (ii) total unsettled time; and (iii) number of night wakings per evening/ night. Total sleep and unsettled times were calculated for the first and last full 24 h days at the unit (i.e. day 2 and day 4, 6 am-6 am). All instances of crying, screaming and grizzling were combined to obtain the total unsettled time; total sleep time included only periods of sleep >12 min; and unsettled behaviours occurring within a 12 min period were considered to represent a single unsettled episode. Night wakings were defined as any awake period during the evening/night time period (i.e. 6 pm-6 am), but wakings occurring within a 12 min period were considered to be the same waking episode. To ensure coding reliability, 10% of the charts were recoded by a second coder (DN; Pearson correlation r > 0.91, p < 0.001).
Analyses
Data were analysed using SPSS for Windows (version 15; SPSS, Chicago, IL, USA). Infant behaviour (total sleep time, total unsettled time, number of night wakings) was analysed across two 24 h time conditions (baseline = RFCU day 2; end of treatment = RFCU day 4), using 2×2 repeated measures ANOVAs, with depression status as the between-subjects factor. There were two levels of depressive status: ‘depressed on admission’ (women with an admission EPDS score > 12) and ‘not depressed on admission’ (women with an admission EPDS score < 13). Maternal functioning (depressive symptomatology, anxiety symptomatology and parenting stress) was analysed across three time conditions (admission, 1 month after discharge and 3 months after discharge) using 2×3 repeated-measures ANOVAs, with depressive status during the admission (defined as given) as the between-subjects factor. McNemar's χ2 tests and binomial distribution comparisons were also used to compare changes in the percentages of patients reporting clinically significant levels of distress at these three time points. Statistical significance was set at p < 0.05 and Greenhouse-Geisser adjustments were made to the degrees of freedom when the assumption of homogeneity of covariance was not met. Effect sizes were calculated for differences between groups on dependent variables, that is, Cohen's d and η2 for continuous variables and Cohen's w for categorical variables. Effect sizes were evaluated using Cohen's descriptors of small (d = 0.2, w = 0.1, η2 = 0.02), medium (d = 0.5, w = 0.3, η2 = 0.13) and large (d = 0.8, w = 0.5, η2 = 0.26) [55].
Results: study 1
Infant behaviour
Of the 104 participants, there were 100 for whom EPDS data were available. Of these, there were 27 (27%) who scored > 12 on the EPDS during the admission and were thus classified as depressed on admission. Table 1 shows the mean infant sleep and unsettled times and the number of night wakings on day 2 and day 4 of the admission, for the total sample, infants of mothers who were depressed on admission and infants of mothers who were not depressed on admission. At baseline there were no significant differences between the depressed and not depressed groups on any of the three infant behaviour variables (sleep time: t(93) = 1.81, p = 0.073, d = 0.42; unsettled time: t(93) = 0.32, p = 0.748, d = 0.08; night wakings: t(92) = 0.09, p = 0.928, d = 0.02).
Study 1: maternal depression status by infant sleep time, unsettled time and number of night wakings (n = 100), and maternal EPDS, HADS-A and PSI-SF scores (n = 70)
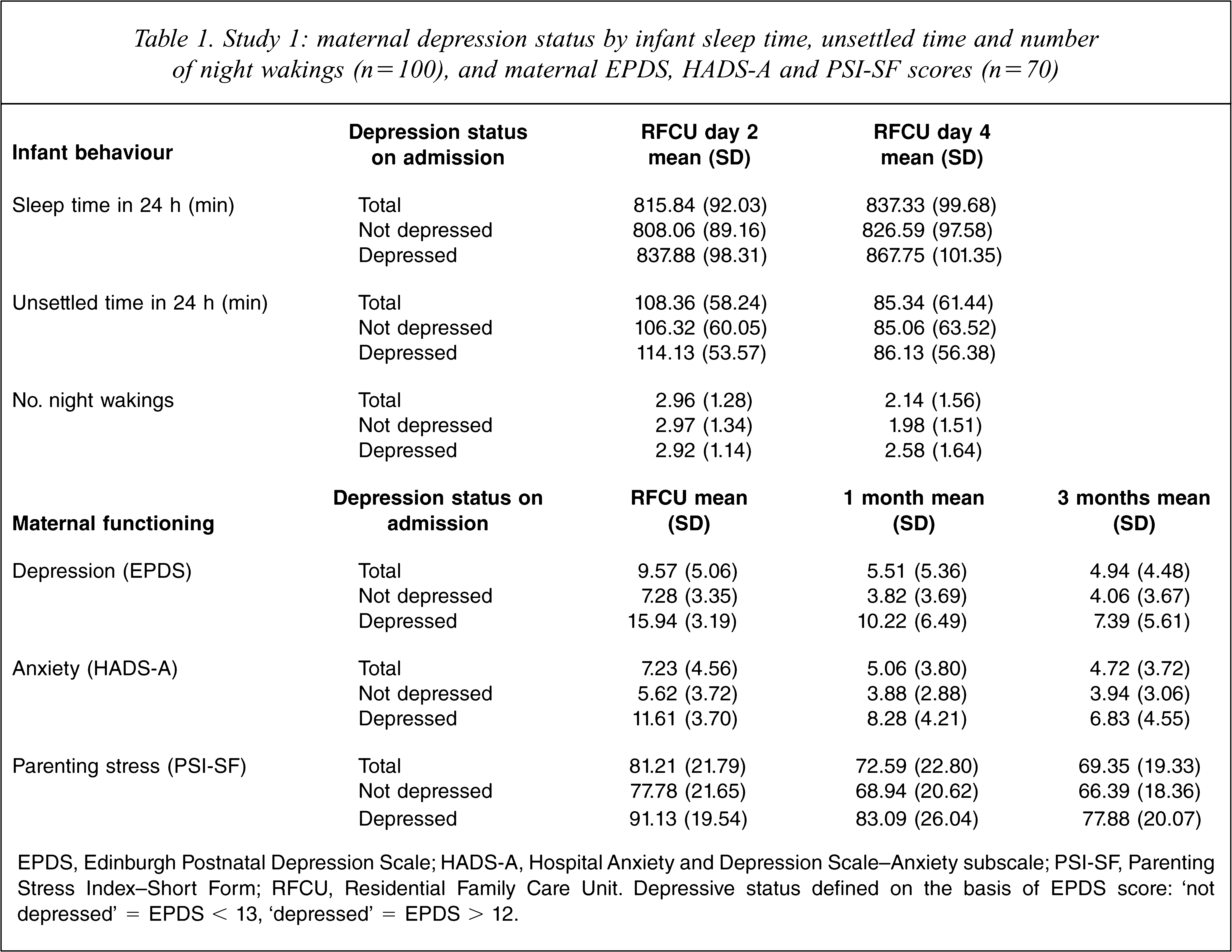
EPDS, Edinburgh Postnatal Depression Scale; HADS-A, Hospital Anxiety and Depression Scale-Anxiety subscale; PSI-SF, Parenting Stress Index-Short Form; RFCU, Residential Family Care Unit. Depressive status defined on the basis of EPDS score: ‘not depressed’ = EPDS < 13, ‘depressed’ = EPDS > 12.
For all three infant behaviour variables, there were significant main effects for time (sleep time: F(1,90) = 5.08, p = 0.027, η2 = 0.053; unsettled time: F(1,90) = 9.51, p = 0.003, η2 = 0.096; night wakings: F(1,88) = 11.11, p = 0.001, η2 = 0.112). This indicates that all infants, whether or not their mother was depressed during the admission, experienced significant increases in the amount of time that they slept, decreases in the amount of time that they were unsettled and decreases in the number of times they woke at night over the course of the admission. In contrast, no significant main effects were found for depressive status (sleep time: F(1,90) = 3.19, p = 0.077, η2 = 0.034; unsettled time: F(1,90) = 0.140, p = 0.709, η2 = 0.002; night wakings: F(1,88) = 0.979, p = 0.325, η2 = 0.011) or time × depressive status (sleep time: F(1,90) = 0.28, p = 0.599, η2 = 0.003; unsettled time: F(1,90) = 0.178, p = 0.674, η2 = 0.002; night wakings: F(1,88) = 2.71, p = 0.103, η2 = 0.030), suggesting that in terms of the degree of improvement in infant outcomes achieved, there were no differences between infants of mothers who were and infants of mothers who were not depressed during the admission.
Maternal depression, anxiety and parenting stress
Of the 73 participants who completed post-discharge follow-up measures, there were 70 for whom baseline EPDS scores were available. Of these, there were 18 (25.7%) who scored >12 on the EPDS during the admission and were thus classified as depressed. The proportions of women classified as depressed at follow up were 11.1% at 1 month and 6.9% at 3 months. The differences between the proportions in the clinical ranges (from baseline) were statistically significant at both time points (p < 0.003). The total EPDS score of women with a likely depressive disorder during the admission had on average fallen by 5.72 EPDS points (SD = 6.65) at 1 month and 8.56 EPDS points (SD = 4.89) at 3 months.
Table 1 shows the mean EPDS, HADS-A and PSI-SF scores at admission, 1 month after discharge and 3 months after discharge, for the total sample, those who were depressed on admission, and those who were not depressed on admission. Significant main effects were found for time on all three outcome measures (EPDS: F(2,132) = 65.13, p < 0.001, η2 = 0.497; HADS-A: F(1.65,107.34) = 39.13, p < 0.001, η2 = 0.376; PSI-SF: F(2,128) = 19.50, p < 0.001, η2 = 0.234), suggesting that all participants, whether or not they were depressed during the admission, experienced improvements in psychopathology. Significant main effects were also found for depressive status on all three outcome measures (EPDS: F(1,66) = 43.34, p < 0.001, η2 = 0.396; HADS-A: F(1,65) = 26.56, p < 0.001, η2 = 0.290; PSI-SF: F(1,64) = 5.90, p < 0.018, η2 = 0.084). It is not surprising that a difference was found for EPDS score, because this was the measure by which participants’ depressive status was classified. Nevertheless, these results do indicate that women who were depressed during the admission were also experiencing significantly higher levels of anxiety symptomatology and parenting stress over the three time points, compared to women who were not depressed. The interaction between depression status and time was significant for the EPDS (F(2,132) = 12.20, p < 0.001, η2 = 0.156) and the HADS-A (F(1.65,107.34) = 8.15, p = 0.001, η2 = 0.111), but not for the PSI-SF (F(2,128) = 0.228, p = 0.797, η2 = 0.004), indicating that those who were depressed during the admission experienced a greater degree of improvement in depressive and anxiety symptomatology over the 3 months compared to those who were not depressed during the admission. Figure 1 shows the maternal EPDS and HAD-A scores at admission, 1 month after discharge and 3 months after discharge, for women who were classified as depressed and not depressed on admission.
Method: study 2
Participants
Two hundred and thirty-three English-speaking women with singleton infants aged 0–12 months admitted consecutively to the RFCU between September 2005 and April 2006 were invited to participate in study 2. A number of patients agreed to participate but were not included in the final sample because they did not complete the structured clinical interview due to insufficient time (n = 25) or because they were discharged early or were absent from the unit for a period of time, resulting in missing child behaviour data (n = 10), and 51 declined. This left a total of 147 study participants (63% recruitment rate). The mean ± SD maternal age of participants was 31.37 ± 5.26 years; 90.8% were in a married or de facto relationship and 40.6% were university educated. The mean ± SD infant age was 5.44 ± 3.20 months; 68.2% of infants were first borns and 57.1% were male.
Procedure
During their admission to the Unit, a psychologist (JP) interviewed participants using the Structured Clinical Interview for DSM-IV diagnosis (research version) (SCID-I) [56]. RFCU nurses recorded infant behaviours for the duration of the admission using a 24 h infant behaviour chart.
Measures
Structured Clinical Interview for DSM-IV diagnosis
The SCID-I is a semi-structured diagnostic interview for DSM-IV disorders [56]. The SCID-I has demonstrated interrater reliability, with reported kappas for diagnosis of major depressive disorder ranging from 0.67 [57] to 0.80 [58]. Kappa coefficients for anxiety disorder diagnoses (general anxiety disorder (GAD), social phobia, obsessive– compulsive disorder (OCD) and panic disorder) ranging from 0.57 to 0.65 have been reported [58]. In the current study, participants were given sections of the Mood episodes module and Optional module (minor depressive disorder) and were asked screening questions relating to current panic disorder, social phobia, specific phobia, OCD, GAD and anxiety disorder not otherwise specified (ADNOS). Corresponding sections of the Anxiety disorders module were given when individuals responded positively to screening questions.
24 h Child Behaviour Chart
The child behaviour charts used in study 1 were also used in study 2. As in study 1, a coder (JP), who was blind to maternal depression or anxiety disorder status, examined infant behaviour charts to calculate total sleep time, total unsettled time and number of night wakings per evening/night. In an effort, however, to obtain baseline and end-of-treatment data as close to the start and end of the admission as possible, in this study total sleep and unsettled times were calculated for 18 h periods on day 1 (12 pm day 1–6 am day 2) and day 4 (12 pm day 4–6 am day 5). All other coding processes were the same as those described for study 1. Again, to ensure coding reliability, 10% of the charts were recoded by a second coder (DN; Pearson correlations r > 0.88, p < 0.001).
Analyses
Data were analysed using SPSS for Windows (version 15; SPSS). Independent samples t-tests were used to examine differences between the disorder and no disorder groups in terms of baseline infant behaviours (total sleep time, total unsettled time and number of night wakings). A series of 2 (disorder) × 2 (time) repeated-measures ANOVAs were used to examine differences in infant behaviours across two time conditions (RFCU day 1 and RFCU day 4), with maternal disorder status as the between-subjects factor. There were two levels of maternal disorder status: disorder (women with either major depression, minor depression or an anxiety disorder) and no disorder (women without major depression, minor depression or an anxiety disorder). Statistical significance was set at p < 0.05 and effect sizes were calculated and evaluated as described for study 1.
Results: study 2
Of the 147 participants, 46 (31.3%) met criteria for major or minor depression, 51 (34.7%) met criteria for at least one anxiety disorder and 73 (49.7%) met criteria for any disorder (depression or anxiety). Mean sleep and unsettled times (in 18 h) and number of night wakings across the two time periods for the disorder and no disorder groups are shown in Table 2. At baseline there were no significant differences between the disorder and no disorder groups for total sleep time (t(138) = 1.63, p = 0.106, d = 0.28) or number of night wakings (t(145) = 1.35, p = 0.178, d = 0.22). Infants of mothers with a disorder, however, were found to be significantly less unsettled on admission than infants of mothers without a disorder (t(117.12) = 2.32, p = 0.022, d = 0.39).
Study 2: maternal psychological disorder status by infant sleep time, unsettled time and number of night wakings (n = 147)
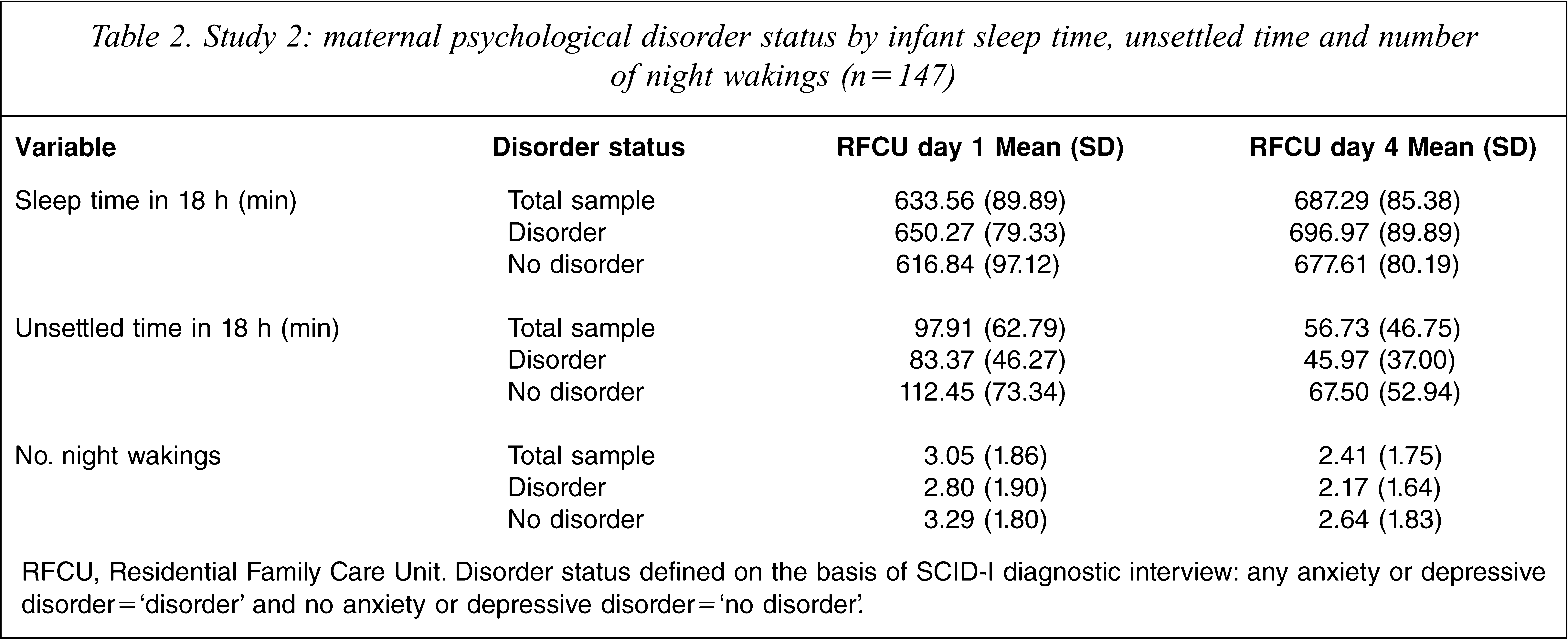
RFCU, Residential Family Care Unit. Disorder status defined on the basis of SCID-I diagnostic interview: any anxiety or depressive disorder=‘disorder’ and no anxiety or depressive disorder=‘no disorder’.
For all three infant behaviour variables there were significant main effects for time (sleep time: F(1,122) = 38.64, p < 0.001, η2 = 0.241; unsettled time: F(1,122) = 57.34, p < 0.001, η2 = 0.320; night wakings: F(1,129) = 12.87, p < 0.001, η2 = 0.09), indicating that all infants, whether or not their mother was diagnosed with a depressive or anxiety disorder, experienced significant increases in the amount of sleep time, decreases in the amount of unsettled time and decreases in the number of night wakings over the course of the 5 day admission. The main effect for disorder was significant for sleep time (F(1,122) = 4.12, p = 0.045, η2 = 0.033) and unsettled time (F(1,122) = 9.90, p = 0.002, η2 = 0.08), but not for number of night wakings (F(1,129) = 3.41, p = 0.067, η2 = 0.03). This suggests that overall, infants of mothers with a disorder were less unsettled and slept longer than infants of mothers without a disorder, but that there were no significant differences between the groups in terms of the number of night wakings. Likewise, no significant effects were found for time × disorder (sleep time: F(1,122) = 0.66, p = 0.417, η2 = 0.01; unsettled time: F(1,122) = 0.48, p = 0.489, η2 = 0.04; night wakings: F(1,129) = 0.02, p = 0.962, η2 < 0.001), indicating similarities between the groups in terms of the degree of change on the three outcome variables.
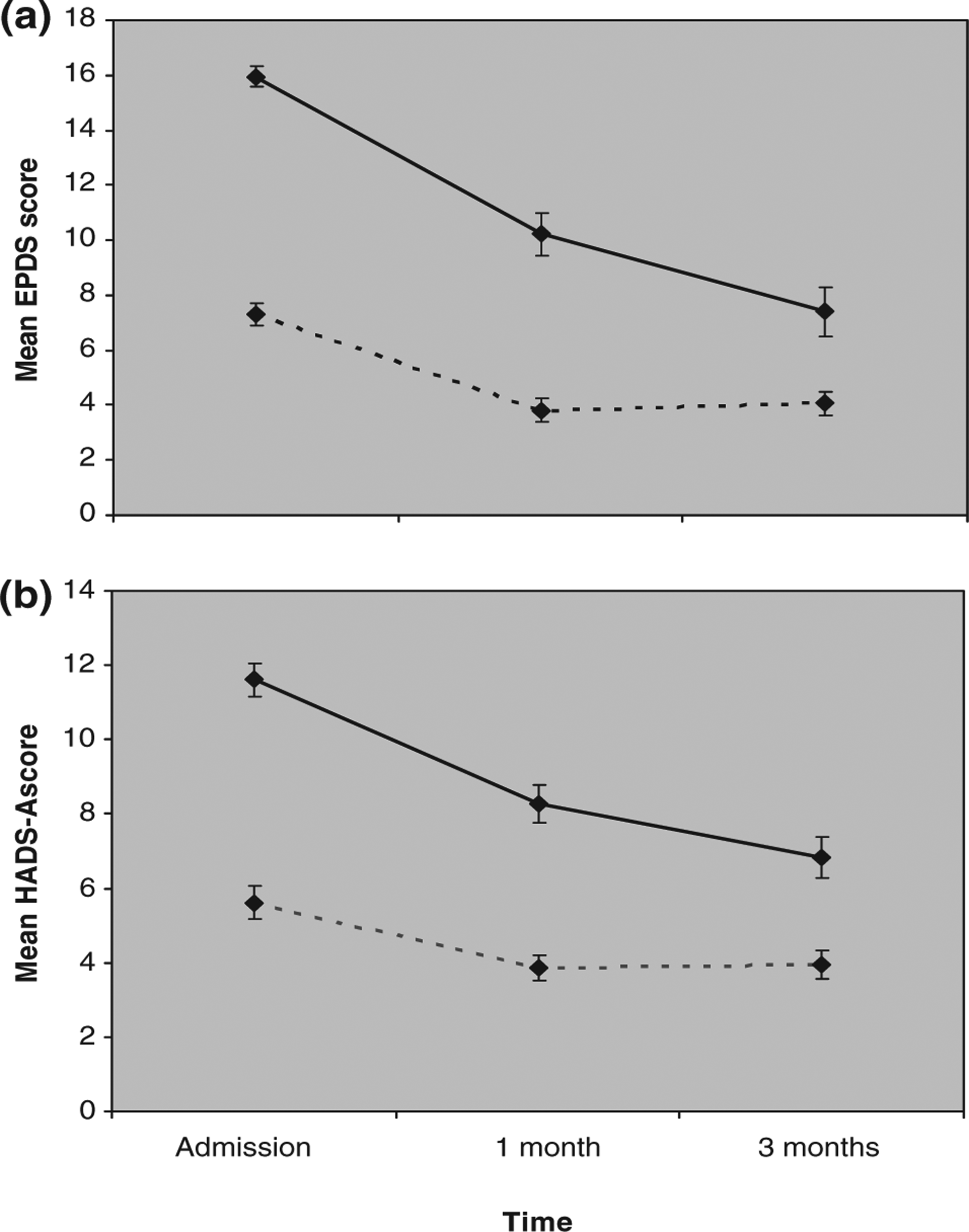
Maternal (a) Edinburgh Postnatal Depression Scale (EPDS) and (b) Hospital Anxiety and Depression Scale-Anxiety subscale (HADS-A) scores at admission, 1month after discharge and 3months after discharge for women classified as (—) ‘depressed’ (EPDS > 12) or (—) ‘not depressed’ (EPDS < 13) during admission.
Discussion
The current paper reports results of two studies that (i) investigated infant and maternal outcomes of a residential mother–infant intervention for unsettled infant behaviour; and (ii) examined the impact of maternal psychopathology on outcomes. The first study showed the RFCU intervention to be associated with significant decreases in the amount of time that infants were unsettled, decreases in the number of night wakings, and increases in the total amount of sleep time. Importantly, these improvements were seen for both infants of mothers who scored above and infants of mothers who scored below the EPDS threshold for major depression during the admission. Results also showed the RFCU intervention to be associated with significant improvements in maternal depression, anxiety and parenting stress: improvements that were again evident both for women who scored above and women who scored below the EPDS threshold for major depression during the admission. The strong and clinically significant gains for women with a probable depressive disorder were evident in the finding that the proportions of participants who scored above the EPDS threshold for major depression fell from 26% at baseline, to 11% at 1 month, and 7% at 3 months, and that the EPDS scores of women with a likely depressive disorder during the admission had on average fallen by 5.7 EPDS points at 1 month and 8.6 EPDS points at 3 months.
The second study confirmed the findings of study 1, again showing that the RFCU intervention was associated with increases in infant sleep time, decreases in unsettled behaviour time and decreases in the number of night wakings. Importantly, these improvements were found for infants of mothers who did meet formal diagnostic criteria for a psychological disorder, as well as for infants of mothers who did not. Interestingly, at the start of the RFCU admission, infants of mothers with a psychological disorder were found to show less unsettled behaviour than those of mothers who did not have a psychological disorder. This suggests that the women in the present study who were suffering from depressive or anxiety disorders may have had a lower threshold for coping and/or seeking help for unsettled infant behaviour, and that infant behaviour was unlikely to have played a primary causative role in the development of their mood disorder. It is nevertheless encouraging to note that infant behaviour improvements were not limited to infants of mothers without a psychological disorder, because it indicates that maternal psychological disorder status does not detract from the effectiveness of the intervention.
Various limitations of the present study must be acknowledged. First, as has been the case in previous studies, given that this study did not have a control group, firm conclusions about treatment outcomes cannot be made. But the fact that the intervention was implemented over such a short time period (5 days) indicates that infant behaviour improvements were likely to be directly attributable to the intervention. In any case, a randomized controlled trial comparing the RFCU intervention to a control condition would still be a worthwhile future research endeavour. Second, recruitment and retention rates in study 1 were not ideal (69% and 62%, respectively). It is also unfortunate that we cannot comment on the women who chose not to take part in the first instance, because systematic differences between these groups may exist. Third, the fact that maternal psychological functioning data in study 1 and infant behaviour data in study 2 were obtained during, and not prior to, the admission means that baseline measures of maternal psychological functioning and infant unsettledness were not true pre-treatment measures. The fact, however, that baseline measurements were taken after the commencement of the intervention suggests that these figures probably represent an underestimation rather than overestimation of the extent of maternal mood and infant behavioural difficulties experienced by participants, thus strengthening the results. Fourth, while there was clear evidence of gains in maternal functioning over the 3 months of follow up, longer-term follow up would be worthwhile. Investigations of child behaviours in the months following discharge would be of particular value, because it is possible that there may be differences in the infant behaviours of women with, and women without, psychological disorders.
These limitations notwithstanding, the current study is important because it not only confirms previous findings about the effectiveness of residential mother–infant programmes for mothers and infants [42–44,47], but also represents a significant extension upon previous studies in its utilization of a structured clinical interview for DSM-IV diagnosis and independent ratings of infant behaviours. In doing so, this study shows the RFCU intervention to be a highly effective means for alleviating both psychological symptomatology and infant behavioural disturbance and, importantly, it shows that these benefits are seen for both women with and women without psychological disorders.
Evidence of widespread exhaustion among mothers with unsettled infants and evidence of improvements in maternal fatigue and psychological functioning following interventions for infant sleep, have led to speculations that maternal fatigue may be a mediating factor in the relationship between infant sleep problems and maternal depression [9,32,33,40,59]. Although the present study did not include any formal assessment of maternal fatigue, given that all participants were mothers attending a tertiary level service for unsettled infant behaviour, fatigue was likely to have been virtually universal in this sample. It is therefore possible that the observed improvements in maternal depression and anxiety were related, in part, to improvements in infant behaviour and thus maternal sleep. As stated in the previous section, however, no definitive conclusions about the reasons for positive maternal psychological functioning outcomes can be made without a randomized controlled study. It must also be noted that almost three-quarters of the women in study 1 scored below the EPDS threshold for likely major depression and that one-half of the women in study 2 did not meet diagnostic criteria for a psychological disorder. Therefore, the fact that such a large proportion of participants were not experiencing clinically significant levels of psychopathology despite probable sleep deprivation and exhaustion, suggests that maternal psychopathology is not accounted for by maternal fatigue alone. Rather, it is likely that other known situational risk and vulnerability factors such as low social support, stressful life events and personal psychiatric history [60–62] also played a role.
Given the known reciprocal relationship between unsettled infant behaviour and maternal psychological functioning [24,35–41] and the multi-faceted programme provided at the RFCU, it is difficult to comment on the effectiveness of individual components of the RFCU intervention or to identify particular reasons for the outcomes observed. Taken together, however, the present results clearly demonstrate the effectiveness of this multi-disciplinary residential mother–infant unit programme in improving both infant behaviours and maternal psychological functioning. There are a wide range of available evidence-based interventions for maternal postnatal depression and anxiety (e.g. cognitive behavioural therapy [63–65], pharmacological treatments [66] and interpersonal psychotherapy [67,68]), but the present results suggest that in cases in which infant unsettledness is also an issue, brief residential mother–infant programme admissions may also offer a very viable and effective treatment option. Psychiatrists, psychologists and general practitioners working in community-based settings should routinely assess for infant behaviour difficulties when conducting post-natal psychiatric and psychosocial assessments; and in cases where unsettled infant behaviour problems are identified, it is recommended that referral to a residential mother–infant programme be considered as a first line of treatment.
Footnotes
Acknowledgements
This research was funded by Karitane and an NHMRC Public Health Postgraduate Scholarship awarded to Jane Phillips. Associate Professor Louise Sharpe is supported by a Senior Research Fellowship from the NHMRC.
