Abstract
Keywords
While suicide and suicide attempts have long been strongly associated with depression and bipolar disorder [1,2], self-mutilation has more often been associated with abnormal personality traits, especially borderline personality disorder (BPD). Many studies confirm the high rates of suicide attempts and self-mutilation in patients with BPD, even when compared to depressed patients without BPD [3]. In an ongoing clinical trial of interpersonal social rhythms psychotherapy for young people with bipolar disorder we have been struck by the high rate of reported self-mutilation.
Using Cloninger's Temperament and Character Inventory (TCI), which assesses four measures of temperament and three domains of character, within the framework of a psychobiological model of personality [4], there are reports that those who make suicide attempts have higher scores on the temperament dimension of harm avoidance [5]. We are not aware of studies that have examined measures of temperament and character in individuals who have a history of self-mutilation. On the TCI, individuals with BPD have consistently been found to score low on the character scale of self-directedness and high on the temperament measures of both harm avoidance and novelty seeking, reflecting approach–avoidance conflict [3,6].
In this paper, using data from a family study on the molecular genetics of depression and personality, we report on the lifetime prevalence of self-mutilation and of suicide attempts in subjects with no mood disorder, major depression and bipolar disorder, and in those with or without BPD. We also examine the temperament and character measures of individuals with mood disorders, bipolar disorders, BPD, self-mutilation and suicide attempts. From these data we explore which diagnostic and personality variables are associated with a history of self-mutilation and of suicide attempts. Finally, we examine the familial pattern of suicide attempts and self-mutilation.
Method
Subjects
The present subjects were recruited for a family study on the molecular genetics of depression and personality. We initially recruited adult probands, who had been treated for depression (regardless of history of bipolarity), and would be willing to participate in a family study of depression. We then asked them to identify two first-degree relatives, preferably parents but otherwise siblings, who might also participate in the study. Our objectives were to recruit family trios to allow family-based association statistical analyses. When the data for this paper were analysed, we had recruited 214 probands and 407 first-degree relatives.
The study had been approved by the Canterbury (New Zealand) Ethics Committee.
Recruitment and screening
Subjects contacted the research team in response to advertisements placed in a variety of locations in the community and by radio advertising. When potential subjects contacted the research team, the details of the project were explained. A screening telephone interview checked that the proband had been treated for depression. If subjects consented, they were offered the options of being interviewed in their homes or within the university department conducting this study.
Questionnaires
Prior to, or following, the clinical interview and obtaining a blood sample for DNA extraction, all probands and relatives completed two self-report questionnaires. This included a 240-item, 5 point Likert scale version of the TCI to assess the four temperament measures and three character measures, inclusive of subscales, in Cloninger's psychobiological model of Personality [4]. The other questionnaire was the General Behavioural Inventory, which assesses depressive, manic and biphasic mood swings [7].
Interviews
All consenting subjects were interviewed by trained interviewers/ research assistants who had appropriate university degrees. All interviews were reviewed by a psychiatrist with a special interest in mood disorders [8], and DSM-IV diagnoses were assigned. If the interview yielded insufficient information to be confident about diagnoses, we utilized further information obtained from family members or, with consent, from medical records.
The interview for axis I disorders was based upon the Mini-International Neuropsychiatric Interview (MINI) [9], but with expansions in the area of alcohol and drug dependence and bipolar disorder. If after the MINI probe for a history of mania or hypomania, subjects had not been diagnosed with bipolar disorder, they were then asked the questions in the Mood Disorder Questionnaire [10]. If subjects affirmed three or more manic symptoms occurring at the same time, they were then further asked about the nature and extent of these ‘manic’ episodes by re-asking the MINI diagnostic criteria including duration, impairment, hospitalization and psychosis. Care was taken to enquire about the longest duration of manic episodes and age of onset. DSM-IV criteria were used to make a diagnosis of bipolar disorder I or II, while bipolar disorder not otherwise specified (NOS) [11] was diagnosed when an individual reported one or more major depressive episodes and a history of recurrent 1–3 day hypomanic episodes.
After the depression section of the axis I interview, all subjects were asked about history of suicide attempts and of self-mutilation. For a history of suicide attempts the probe question was ‘have you ever tried to kill yourself”. The probe question was followed by questions on a number of attempts, method, age, requiring medical treatment, intent, and lethality. For a history of self-mutilation the probe question was ‘have you ever deliberately harmed yourself to relieve tension or feel better’. The probe question was followed by asking about methods (e.g. wrist cutting, burning), number of times and recency.
After completion of the interview for axis I disorders, subjects were then screened for personality traits. The first screener consisted of 12 questions selected to screen for avoidant, obsessive–compulsive, schizoid and BPDs, and were based on earlier research on the structure of personality disorder symptoms [12]. For each personality adjective or phrase a subject was asked whether they would consider themselves to be ‘not at all’ (score=0), ‘somewhat’ (score=1), ‘or very much’ (score=2) a perfectionist, conscientious, stubborn (obsessive–compulsive screener); a loner, content without friends, didn't care what others thought about them (schizoid screener); a worrier, shy, unconfident (avoidant screener); or impulsive, easily angered or having unstable and erratic relationships (borderline screener). If they identified traits as being present they were then asked whether these had caused significant difficulties for them.
Subjects were then asked, in a similar format, 20 questions about their affective temperament [13].
Following these screening questions the interviewer followed up on any potentially positive personality disorder traits by completing the Structured Clinical Interview for DSM-IV Personality Disorders (SCID-II) [14]. Axis II diagnoses were reviewed with the supervising psychiatrist.
Analyses
All data from interviews and questionnaires were entered into a relational database and then transferred to SYSTAT and LOGIT for statistical analyses. Analyses included t-tests, analysis of variance with post-hoc Tukey tests, and logistic regression.
Results
Table 1 lists the demographic and clinical characteristics of the first 621 subjects recruited to the study. It is of note that while 97 gave a history of suicide attempt(s), and 86 a history of self-mutilation, only 37 gave a history of both, which means that there were 60 with a history of suicide attempt(s) without self-mutilation, and 49 had a history of self-mutilation without suicide attempts.
Subject characteristics
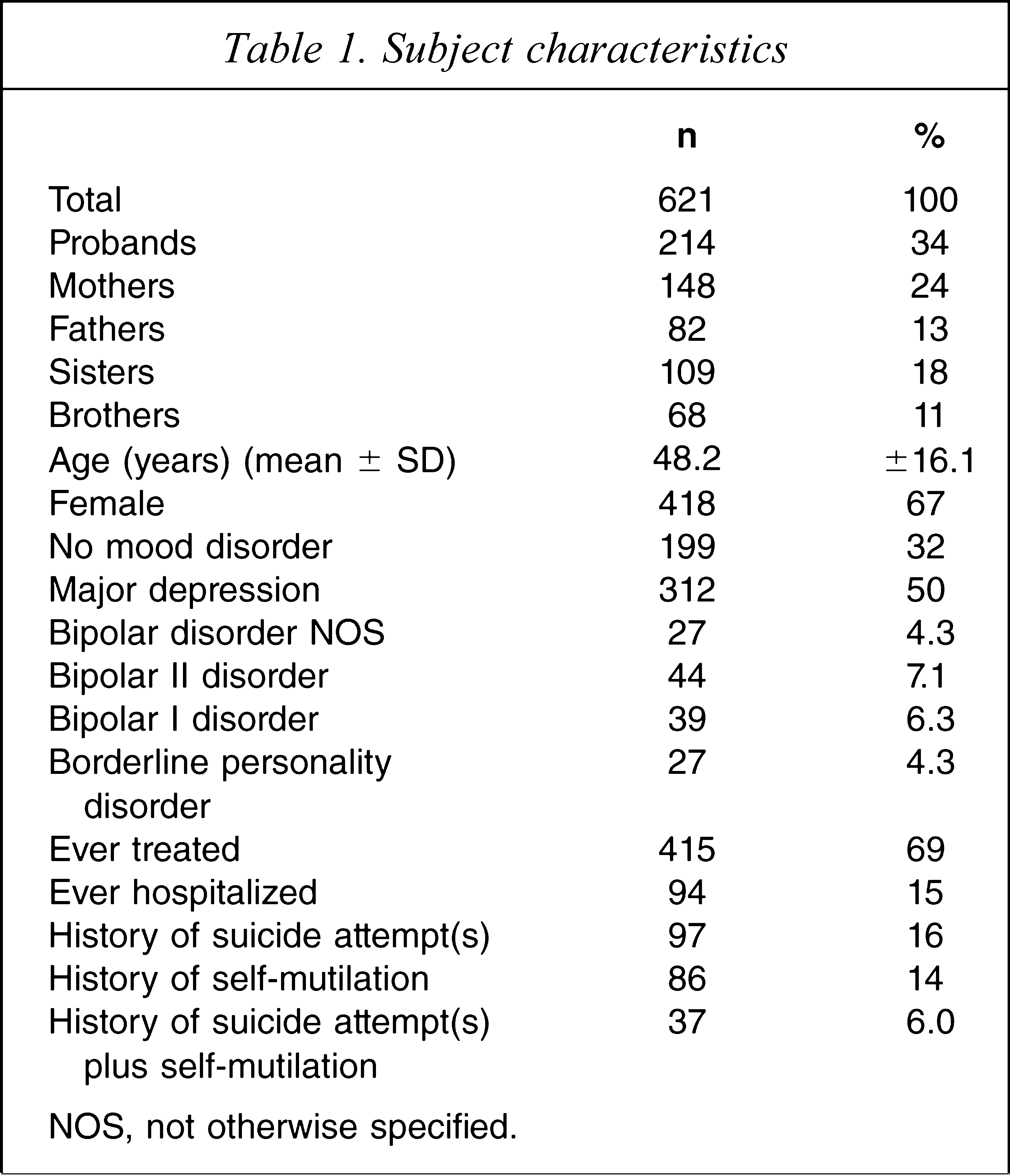
NOS, not otherwise specified.
Table 2 lists the lifetime rates of self-mutilation and of suicide attempts by lifetime diagnoses. With respect to suicide attempts it is notable that the rates varied from 0% in those with no mood disorder diagnosis, to 17% in major depression, and up to 54% in bipolar I disorder. In BPD 52% gave a history of suicide attempt(s). With respect to self-mutilation the rates varied from 2% in those with no mood disorder, to 16% in those with major depression, to 38% in those with bipolar I disorder. In BPD 26% gave a history of self-mutilation, which is lower than the rate in bipolar I disorder. Within those with mood disorders (major depression, any bipolar disorder or bipolar I disorder) a comorbid BPD increases the rate of suicide attempts, but not of self-mutilation.
Lifetime rates of suicide attempts and self-mutilation vs diagnosis
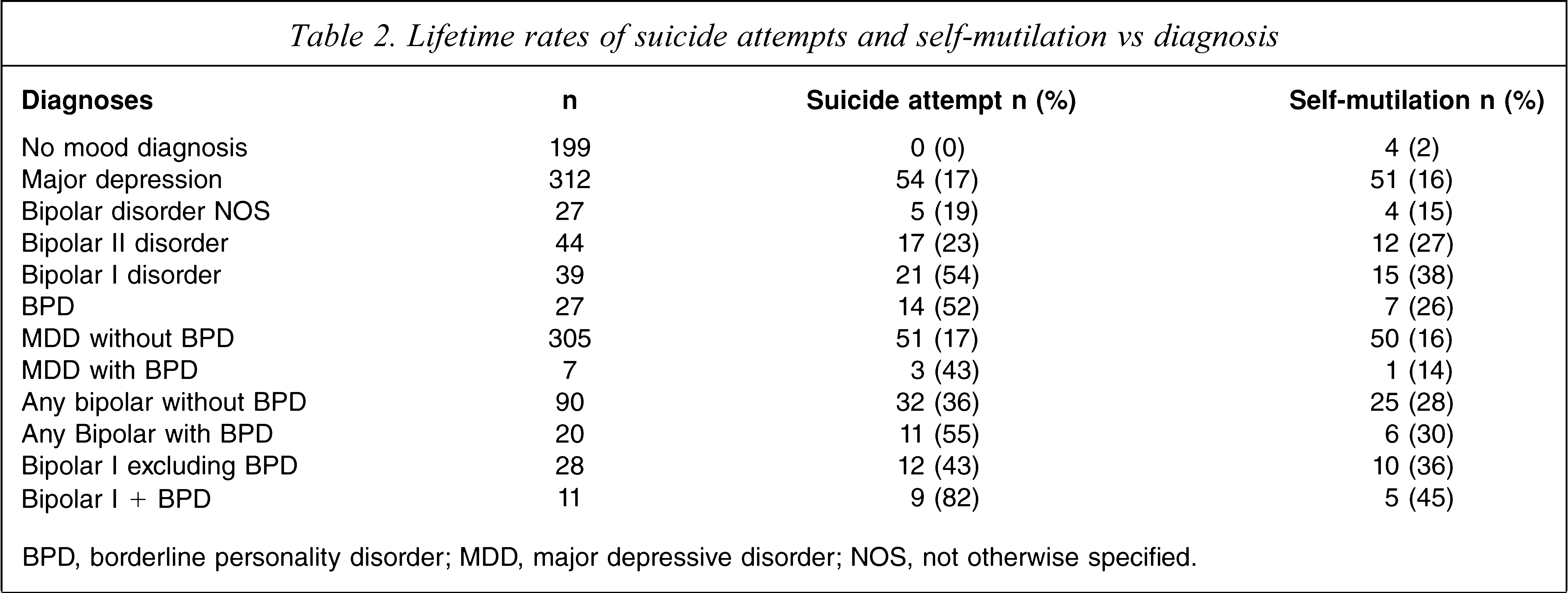
BPD, borderline personality disorder; MDD, major depressive disorder; NOS, not otherwise specified.
Table 3 lists the temperament and character scores by mood diagnoses, BPD, and by history of suicide attempt(s) and self-mutilation. The key findings from Table 3 regarding mood disorders are that both major depression and bipolar disorders are associated with higher harm avoidance and lower self-directedness, while novelty seeking is highest in those with bipolar disorders, intermediate in those with major depression, and lowest in those with no mood disorder. By contrast, self-transcendence is higher in those with any bipolar disorder, compared to those with major depression or no mood disorder. Although the data are not shown in Table 3, self-transcendence was comparable in bipolar I disorder, bipolar II disorder and bipolar disorder NOS; and all were higher than in those without bipolar disorders.
Temperament and Character scores (mean ± SD)

BPD, borderline personality disorder; CO, Cooperativeness; HA, harm avoidance; NS, novelty seeking; PS, persistence; RD, reward dependence; SD, self directedness; ST, self transcendence.
The TCI findings for BPD are comparable to those previously reported [3,6], in that those with BPD had low self-directedness, low cooperativeness and high self-transcendence on their character measures, and had high novelty seeking and harm avoidance on their temperamental measures. For both suicide attempts and self-mutilation, the big differences were the high harm avoidance and low self-directedness. For suicide attempts, but not self-mutilation, there were also smaller differences in relationship to novelty seeking, reward dependence, persistence and cooperativeness.
Multivariate prediction of diagnoses, self-mutilation, and suicide attempts
We initially used multiple logistic regression to predict diagnoses and behaviours from the seven scales of the TCI. For any mood disorder the strongest predictor was high harm avoidance (odds ratio (OR)=1.07, 95% confidence interval (CI)= 1.05–1.09, p < 0.001), with an additional effect of high novelty seeking (OR=1.04, 95%CI= 1.02–1.06, p < 0.001). For bipolar disorders the strongest predictor was high self-transcendence (OR=1.04, 95%CI=1.02–1.05, p < 0.001), but with significant additional effects from high novelty seeking (OR=1.03, 95%CI= 1.01–1.05, p=0.001), low reward dependence (OR=0.98, 95%CI=0.96–1.00, p=0.033) and low self-directedness (OR=0.97, 95%CI=0.96–0.99, p=0.001).
For BPD the predictors were low self-directedness (OR=0.95, 95% CI=0.92–0.99, p=0.004), high self-transcendence (OR=1.05, 95%CI= 1.01–1.09, p = 0.006) and high novelty seeking (OR= 1.04, 95% CI = 1.01–1.08, p=0.013). For self-mutilation the only predictor variable was high harm avoidance (OR=1.04, 95%CI= 1.02–1.06, p < 0.001), while for suicide attempts the strongest predictor was high harm avoidance (OR=1.04, 95%CI = 1.02–1.06, p < 0.001), but with additional effects of high novelty seeking (OR= 1.02, 95%CI= 1.00–1.04, p=0.016), low reward dependence (OR=0.98, 95%CI=0.96–1.00, p=0.021) and low self-directedness (OR=0.98, 95%CI=0.97–1.00, p=0.030).
We then used multiple logistic regression to predict self-mutilation and suicide attempts from diagnostic and temperament and character measures. For self-mutilation the strongest predictor variable was the mood disorder diagnosis (OR = 2.59, 95%CI= 1.65–4.06, p < 0.001), with an additional effect of high harm avoidance (OR=1.03, 95%CI= 1.01–1.05, p = 0.002). BPD was not a significant predictor, and indeed the adjusted OR was <1 at 0.57 (95%CI = 0.19–1.71). For suicide attempts, the mood disorder diagnosis was again the strongest predictor variable (OR = 4.23, 95%CI = 2.65–6.76, p < 0.001), and again only high harm avoidance (OR=1.03, 95%CI= 1.01–1.05, p = 0.003) had a significant additional effect. Again BPD was not a significant predictor, although the adjusted OR was >1 at 1.68 (95%CI = 0.61–4.65).
Familial findings
Because suicide attempts and self-mutilation increased from those with no mood disorder, through those with major depression, to those with bipolar I disorder, we further examined the data of relatives with regard to characteristics of probands with major depression (i.e. excluding probands with any bipolar disorder). For probands with major depression plus suicide attempts, compared to those with major depression but without suicide attempts, the relatives had comparable rates of mood disorders and of suicide attempts. But as can be seen in Table 4, the relatives of probands with major depression plus self-mutilation (vs relatives of those with major depression without self-mutilation) had higher rates of bipolar I or II disorder, with an OR of 3.24 (p < 0.01). Similarly, the relatives of probands with major depression plus self-mutilation had higher rates of self-mutilation (OR=6.83, p < 0.001). Furthermore, this was a consistent finding regardless of whether the relatives had no mood disorder, major depression or bipolar disorder.
Mood disorder diagnoses and self-mutilation in relatives of probands with major depression, vs history of self-mutilation
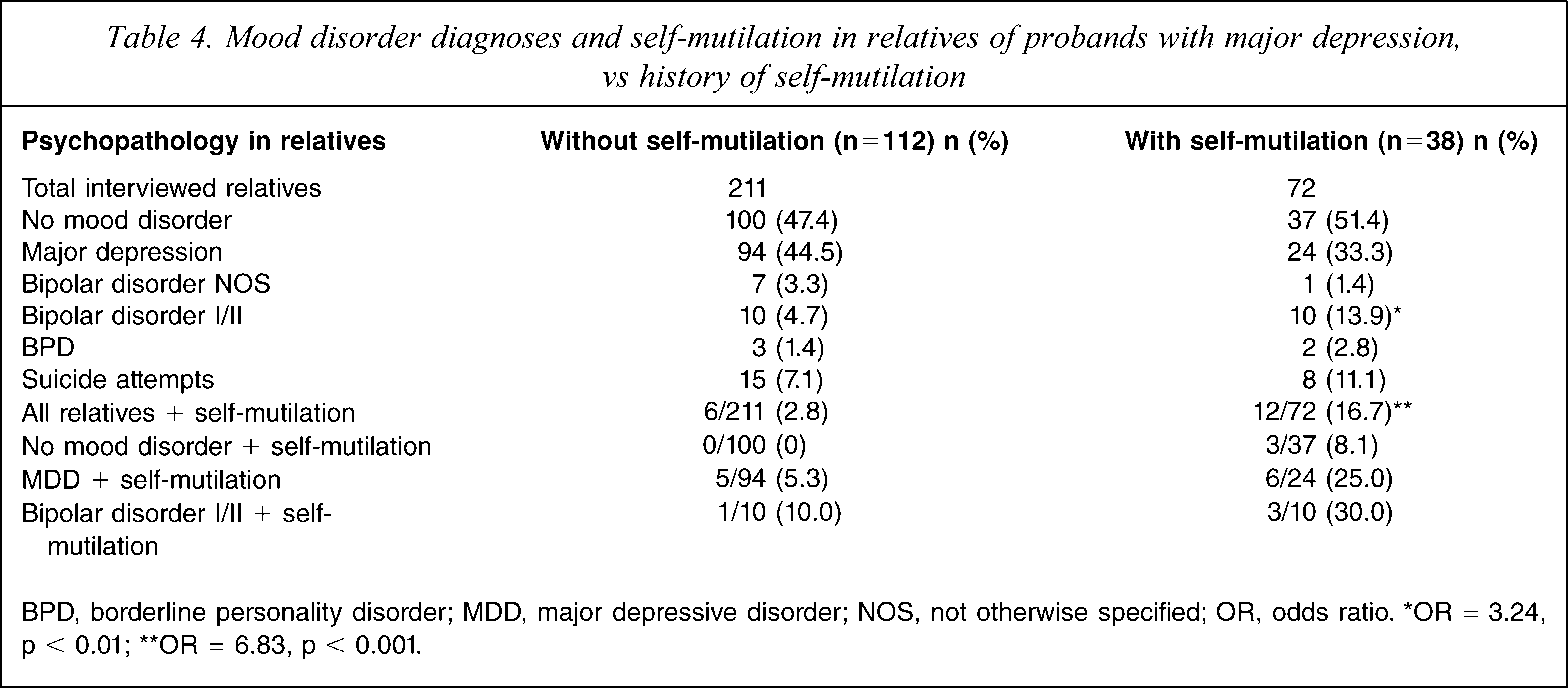
BPD, borderline personality disorder; MDD, major depressive disorder; NOS, not otherwise specified; OR, odds ratio. ∗OR = 3.24, p < 0.01; ∗∗OR = 6.83, p < 0.001.
Discussion
In the present study we have shown that self-mutilation is most commonly observed in subjects with bipolar disorder, and especially bipolar I disorder. Furthermore, relatives of probands who have a history of non-bipolar major depression and a history of self-mutilation have higher rates of bipolar I and II disorders, and have higher rates of self-mutilation. Although subjects meeting criteria for BPD had a 26% rate of self-mutilation (and a 52% rate of suicide attempts), BPD did not predict the presence of self-mutilation, when mood disorder diagnosis and the temperament trait of harm avoidance were included as predictors. Although suicide attempts were also more common in those with mood disorders, and especially those with bipolar I disorder, and were also predicted by mood disorder diagnosis and harm avoidance, relatives of probands who had made suicide attempts did not have increased rates of suicide attempts.
Before discussing further the key findings of the present study, and especially the self-mutilation–bipolar association, we will comment on the strengths and weaknesses of the study. The sample was recruited by advertising for probands treated for depression, and was thus neither a random population sample nor a sample assessed when clinically unwell. More than 80% of those with a lifetime mood disorder were not suffering from a current mood episode when interviewed, and if a subject was clearly unwell when first contacted, an interview was usually delayed until the subject had received appropriate treatment. Across mood diagnoses the rate of being in a current episode was comparable, so higher rates of BPD in bipolar subjects cannot be explained by more being currently unwell. Therefore current mood state should not have been a major confounder in the assessment of personality. Advertising made no comment about bipolar disorder, just that subjects must have been treated for depression, but >100 of the interviewed subjects had a bipolar I, II or NOS diagnosis. Because we aimed to recruit trios for this study, including parents when possible, there is possibly an unknown selection bias as to which relatives, especially in respect to siblings, were selected by probands. It is hard to envisage, however, that key results from the present study could have been due to sibling selection bias.
The definition of self-mutilation may also have impacted upon the results, because the probe question was whether subjects had ever harmed themselves to relieve tension or to feel better. In writing the probe question in this way there was a clear intent to separate the phenomena of self-mutilation from a broader self-harm definition when the intent was suicidal. It could be argued that individuals may harm themselves for a wide variety of reasons and not only to relieve tension or to feel better. We consider, however, that current self-harm data that do not clearly differentiate self-harming behaviours with suicidal intent from self-harming behaviours with the intent to relieve tension or to feel better fail to capture the extent and intent of self-damaging behaviours.
All interviews were completed by trained graduates, usually with psychology degrees, but they were not clinically trained. All interviewers were trained and supervised by one psychiatrist (PRJ), with a long history of clinical and research interest in bipolar disorder, depression and personality disorders [15–18]. Lifetime axis I diagnoses are always subject to concerns about reliability, although usually this is due to underreporting of past episodes [19] and this may be a greater issue for past hypomanic episodes than for past manic or depressive episodes [20]. The most likely effects of underreporting of past episodes is that some relatives with no mood disorder may in fact have experienced a mood disorder, and some subjects diagnosed as having non-bipolar major depression could have a bipolar disorder. It is doubtful that some underestimation of mood disorder diagnoses would substantially alter the associations reported.
Given the use of non-clinically trained interviewers there could be concerns about the diagnosis of axis II disorders. The prevalence rate of BPD in the present sample was 4.3%, which is, as expected, higher than population prevalence rates, but less than seen in clinical samples. The rate of BPD in those with major depression was 2.2%, which is lower than the 8–10% rate we have found in clinical samples [21]. But >80% of those with major depressive disorder were not currently depressed, and the age of the present sample was >10 years older than in the clinical samples; both these factors would be expected to contribute to lower rates of BPD. The rate of BPD in those with bipolar disorders was considerably higher than in those with major depressive disorder, but that is to be expected, and the rates are compatible with previously reported rates [22,23]. The interviewers were blind to the results of the self-report measures, especially the TCI. It is therefore reassuring that those diagnosed as having BPD had the lowest self-directedness scores; along with the lowest cooperativeness and highest novelty seeking and harm avoidance scores. These TCI results thus, in part, validate the BPD diagnoses [3,6].
The TCI results for mood disorder diagnoses are also consistent with other studies, in particular, the high harm avoidance that is associated with major depression and bipolar disorder, and the high self-transcendence with bipolar disorder, but not major depression. The higher novelty seeking from no disorder to major depression to bipolar disorder is consistent with most, but not all, findings [24]. For both those with suicide attempts and self-mutilation, the higher self-directedness scores (than in those with BPD) are suggestive of lower levels of ‘personality dysfunction’ than in those with BPD.
Suicide attempts have been the focus of considerable research, and the present findings that they are associated with mood disorder diagnosis plus harm avoidance largely confirm existing understanding. The present rates of suicide attempts are consistent with other clinical bipolar samples [25].
The most notable results relate to self-mutilation, which is a self-harm behaviour that has not received the same attention as suicide attempts. In part this may be because of the varying terminologies and definitions used in suicide research. Although patients are usually clear that self-mutilation is usually done to relieve tension rather than with an intent to die, the behaviours are sometimes deemed to come under the rubric of self-harm and are not considered independently of suicide attempts. If researchers and clinicians consider that self-mutilation is only a variant of parasuicidal behaviour, then risk factors for self-mutilation will be incorporated into thinking about suicidality. In a current interpersonal social rhythms psychotherapy trial for young people with bipolar disorder we are consistently hearing from these patients that suicide attempts occur with an intent to die, or to escape current despair, when in depressed states, while self-mutilation is to relieve tension when in mixed mood states. Unfortunately, in the present study we did not ask specific questions about the subject's mood state when they made suicide attempts or self-mutilated. We also note that if specific questions are not asked about self-mutilation, then they are seldom volunteered in open questioning or in response to questions about suicidality or safety.
It is of note from the present study that of 86 subjects (14%) who reported self-mutilation, only 37 had also made a suicide attempt, which emphasizes that risk factors for self-mutilation may be very different to risk factors for suicide attempts. For instance, in an earlier study on self-mutilation in depressed patients we reported that a genetic polymorphism of G protein B 3 was associated with self-mutilation [26], but not with suicide attempts. In addition, the highest reported rates of self-mutilation were in bipolar I disorder, and not in BPD.
On the TCI the most notable findings for self-mutilation, apart from the high harm avoidance, was the absence of low self-directedness or low cooperativeness. These findings are congruent with self-mutilation not being associated with personality disorder or dysfunction. In the multivariate prediction of self-mutilation, once mood disorder diagnosis and harm avoidance were included, a BPD made no contribution, and indeed had an OR < 1 for prediction.
The familial findings on self-mutilation in the present study are of particular importance, and require replication and further exploration. First, in the non-bipolar major depression probands with self-mutilation, their relatives had threefold higher rates of bipolar I/II disorder. This threefold increase in bipolar disorder raises questions as to whether there are aspects of the genetics and biology of self-mutilation that are linked to bipolar disorder. It is perhaps interesting that it was a genetic polymorphism of a G protein that we linked with self-mutilation in depressed patients [26], because most psychiatric neurobiological research on G proteins has occurred in the context of bipolar disorder and the mechanism of action of mood stabilizer drugs [27–29]. In addition, self-mutilation, but not suicide attempts, were familial. Thus relatives of non-bipolar major depression with self-mutilation probands had sixfold higher rates of self-mutilation. This occurred across mood diagnoses and it was of note that even three of their 37 relatives with no mood disorder reported self-mutilation. This familial pattern again raises questions about a potential role for genetic factors in self-mutilation. The genetics of suicide has been widely discussed [30], but not the genetics of self-mutilation, except in animals [31].
In the present paper we have reported that there is only a partial overlap between self-mutilation and suicide attempts. Both of these behaviours are associated with mood disorder diagnoses and with the temperament trait of harm avoidance. Self-mutilation, but not suicide attempts, was familial. For clinicians, the most notable findings are the association of self-mutilation with bipolar disorder, and not with BPD. We speculate that the association of self-mutilation with bipolar disorder relates to the presence of mixed mood states. Thus, when clinicians are assessing patients after acts of self-mutilation they should enquire carefully about mixed mood states, which are so easily and often missed [32], and bipolar disorder.
Footnotes
Acknowledgements
This study was supported by project and programme grants from the Health Research Council of New Zealand, by the University of Otago, Christchurch and the Mental Health Division of the Canterbury District Health Board.
