Abstract
Gastric cancer is the second leading cause of cancer mortality worldwide and is projected to rise to tenth in all-cause mortality in the near term. Early detection requires improved sensitivity and specificity of endoscopic imaging with novel methods. The objective of this study was to evaluate the utility of activatable molecular probes for the detection of gastric cancer both in vivo and ex vivo in a preclinical model. Smad4+/− mice, which develop spontaneous gastric neoplasia, were compared to normal wild-type controls. Cathepsin-activatable and matrix metalloproteinase (MMP)-activatable molecular probes were injected 24 hours and 6 hours before imaging, respectively. In vivo imaging was performed using quantitative tomographic near-infrared fluorescence (NIRF) imaging. For validation, ex vivo imaging and histologic examination were performed. Molecular imaging in vivo of Smad4+/− gastric cancer murine models revealed intense activation of both cathepsin B and MMP probes. Ex vivo imaging and histology confirmed that the detected neoplasms were adenocarcinomas and hyperplastic lesions. This study provides proof of principle that the cathepsin- and MMP-activatable molecular probes are activated in the Smad4+/− murine model of spontaneous gastric adenocarcinoma and can be imaged by both in vivo and ex vivo NIRF methods. The cathepsin probe also detects hyperplastic lesions.
GASTRIC CANCER is the second leading cause of cancer mortality, with an expected incidence of over 1 million worldwide in 2010.1–3 Early sensitive and specific detection of gastric cancer is essential for treatment optimization. Traditional endoscopy for gastric cancer screening has several limitations, including the inherent invasiveness, potential complications, and resource use. In addition, standard endoscopy may miss early lesions, as well as yield false-positive results. Yalamarthi and colleagues reported significant rates of missed diagnosis and endoscopist or pathologist errors in gastric cancer patients who had undergone endoscopy within 3 years of diagnosis. 4 Magnification endoscopy, chromoendoscopy, and confocal endoscopy have shown promise in improving detection and potentially avoiding conventional biopsy with histology. 4 The challenges for the next generation of endoscopic imaging are to improve efficiency and to increase sensitivity and specificity for the detection of gastrointestinal tumors.5–7
Molecular imaging of biologic targets, such as cell surface receptors, enzymes, or proteins, provides functional visualization that may help achieve the clinical goals of early detection and characterization.8–11 Among the optical imaging technologies, near-infrared fluorescence (NIRF) imaging has demonstrated promise. Compared to optical imaging at other visible wavelengths, NIRF has the advantages of imaging deeper tissues and minimizing tissue autofluorescence because the major light absorbers (hemoglobin, water, and lipids) have their lowest absorption coefficient in the near-infrared spectral region of 600 to 900 nm.8–10 Activatable probes are substrates of enzymes that are highly expressed in a spectrum of pathologic processes, and a variety of activatable agents were recently developed. Cathepsin-activatable and matrix metalloproteinase (MMP)-activatable probes have been used to detect cancers12–14 and inflammation7,15,16 in mouse models. In our previous study, we demonstrated the ability of the cathepsin-activatable probe to detect precancerous colonic adenomas in murine models. Importantly, discrimination of colonic adenomas within a background of chronic inflammation in an ulcerative colitis mouse model was exhibited using this probe. 17 We also performed NIRF imaging with a capsule endoscope with the goal of combining a noninvasive imaging technique with these activatable probes. 7 Our aim in the present study was to examine whether cathepsin- or MMP-activatable molecular probes can successfully detect and image gastric neoplasia in a Smad4+/− model of spontaneous gastric adenocarcinoma.
Materials and Methods
Animal Models
The study was approved by the Institutional Animal Care and Use Committee (IACUC) of the University of North Carolina at Chapel Hill. Specific pathogen-free (SPF) male heterozygous Smad4m4Mag18,19 mice (Smad4+/−) on C57BL/6 background were provided by Dr. Yijing Chen (Department of Biological Sciences, Kent State University). These mice have targeted disruption of one Smad4 allele. The smad4 protein is a crucial component of signaling by transforming growth factor β (TGF-β), which negatively regulates cell growth and promotes apoptosis of epithelial cells. Studies have demonstrated that loss of Smad4 expression promotes gastric carcinoma.20–22 Xu and colleagues reported that disruption of one Smad4 allele initiates progressive gastric polyposis, dysplasia, and adenocarcinoma in mice. 23 Wild-type (WT) C57BL/6 mice (n = 3) were maintained in our SPF animal facility and used as controls. Water and food were provided ad libitum until 4 days before imaging, when Smad4+/− and WT controls were fed a Nutren 1.0 fiber liquid diet (Nestle Nutrition, Minnetonka, MN) diluted in 1:1 dH2O. Liquid diet was administered to clear the bowel of solid fecal matter, which may autofluoresce or interfere with disease detection. Our preliminary studies confirmed that 4 days on this liquid diet effectively reduced background fluorescence.
Molecular Imaging Methodology
The activatable molecular probes ProSense 680 (mainly targeting cathepsin B) and MMPSense 750 FAST (primarily targeting MMP-9) were obtained from PerkinElmer (Waltham, MA). The probes were administered via retro-orbital injection at the doses recommended by the vendor (ProSense 680, 2 nmol/150 μL; MMPSense 750 FAST, 2 nmol/100 μL) in phosphate-buffered saline. Per guidelines, in vivo imaging was performed 24 hours (ProSense 680) or 6 hours (MMPSense 750 FAST) after the probe injection.
In Vivo Tissue Imaging
The tomographic and planar imaging studies were performed using a fluorescence molecular tomography (FMT) system (FMT 2500 LX, PerkinElmer). Mice were anesthetized and imaged as previously described. 7 Tomographic imaging with the FMT system used a near-infrared laser diode to transilluminate, with signal detection via a charge-coupled device camera. Optical filters allowed excitation of the probes at their respective excitation wavelengths (ProSense: 680 ± 10 nm; MMPSense: 750 nm) and imaging of emitted fluorescence at their emission wavelengths (ProSense: 700 ± 10 nm; MMPSense: 770 nm). The entire imaging acquisition sequence took approximately 3 to 5 minutes per animal model. In addition, two-dimensional (2D) fluorescence reflectance imaging (FRI) was performed with the FMT system using the built-in light-emitting diode (LED) front illuminators and a collection of single camera images.
Ex Vivo Tissue Imaging
Mice were euthanized immediately after live imaging in vivo. Each stomach was resected and then imaged ex vivo with FRI.
Histology
Following in vivo and ex vivo imaging, to confirm that the fluorescent signal originated from the neoplasms, the fresh stomach tissue was fixed in 10% zinc formalin and paraffin embedded. Regions of stomach tissue that yielded signals with activated probe in Smad4+/− mice and corresponding regions from WT controls were sectioned for hematoxylin and eosin (H&E) staining. An experienced pathologist blinded to the sample source categorized the tissue sections as normal, hyperplasia, dysplasia, or adenocarcinoma.
Image and Statistical Analysis
For in vivo imaging data analysis, the fluorochrome quantification of total fluorescence and signal intensity within the gastric region of each mouse was determined using three-dimensional (3D) region of interest (ROI) analysis. Briefly, images were displayed as rotatable reconstructed 3D data sets, allowing views in transverse, sagittal, and coronal planes. The target 3D region was defined by ROI placement in all three viewing planes to delineate appropriate regions of fluorescence within the imaging data set. Image calibration was performed using a threshold applied to all animals equal to 30% of the mean fluorescence in the stomach ROI of normal control mice. This threshold setting minimizes the background fluorescence but allows optical detection of fluorescence signals in activated targets. Fluorochrome concentration in the target tissue was then automatically calculated from the reconstructed images (FMT TrueQuant imaging software, version 2.0.0.19, PerkinElmer) and preacquired calibrations for the specific probe. The results are expressed in total fluorescence calculated as picomoles (specifically, picomole equivalents of activated probe per ROI based on comparisons with calibration standards).
To measure the signal intensity of fluorescence signal, potentially another measure of protease activation in dysplastic lesions, we divided total fluorescence (picomole equivalents of activated probe) by volume of the ROI used for 3D tomographic imaging (fluorescence/volume of ROI). For ex vivo 2D FRI data analysis, identical 2D ROIs were placed on appropriate regions of reflective fluorescence in both WT and Smad4+/− mice stomach tissue, with imaging calibration, as described above.
In vivo FMT data (total fluorescence or fluorescence intensity) and ex vivo FRI data (counts/energy) obtained on individual animals with each of the two probes tested were used to generate the mean of signals (± SE) in observed WT or Smad4+/− mice. Mean signal intensity (SI) was recorded. Data from the Smad4+/− mice and WT controls were compared by Student t-test. The neoplastic lesion to background (normal mucosa) target contrast calculation (TBC) was determined according to published methods. 24 The TBC, expressed as a percentage, represents the ratio of the difference in signal in a macroscopically evident lesion or region of activated probe and grossly normal mucosa divided by the signal in grossly normal mucosa. Regions of normal mucosa were obtained as size-matched gastric mucosa from tissue adjacent to macroscopically evident tumors in Smad4+/− mice or WT mice gastric tissue:
In addition, for in vivo FMT data, we compared signals (total fluorescence and fluorescence intensity) of the ProSense 680 and MMPSense 750 probes. For ex vivo data, we compared FRI and FMT results from ProSense 680 and MMPSense 750 FAST probe activation.
In the statistical analysis, data are expressed as mean ± standard error and compared for significance using the t-test. All statistical analyses were performed using STATISTICA software version 9 (Statsoft, Inc. Tulsa, OK). A p value less than .05 was considered statistically significant.
Results
Detection of Gastric Tumors by Molecular Probes in Smad4+/− Mice
Discrete adenocarcinoma and hyperplastic lesions were successfully detected in the stomachs of each Smad4+/-animal model by both the cathepsin and MMP molecular probes. Figure 1 shows in vivo imaging of a Smad4+/-mouse that yielded signals in the region of the stomach at each of the distinct emission wavelengths for cathepsin (ProSense 680) and MMP (MMPSense 750 FAST) probes. Ex vivo imaging of the stomach using FMT (Figure 1B, with the 3D FMT image displayed on top of the 2D FRI) and FRI (Figure 1, C and D) confirmed significant activation of both the cathepsin- and MMP-activatable probes in regions corresponding to visible gastric tumors. We observed that cathepsin activation and MMP activation in gastric neoplasia were not identical. As shown in Figure 1, C and D, activation of the cathepsin probe was detected in three individual lesions, whereas activation of the MMP probe was observed in only two of the three lesions. Importantly, the tumor localized by the cathepsin probe but not by the MMP probe was a hyperplastic lesion. Lastly, relative SI appears to be greater with the cathepsin-versus the MMP-activated probe.

In vivo and ex vivo imaging of gastric tumors in a Smad4+/− mice injected with activatable cathepsin and matrix metalloproteinase (MMP) probes using fluorescence molecular tomography (FMT) and fluorescence reflectance imaging (FRI). A, In vivo FMT image of Smad4+/− mouse. Region of interest (boxed area) reveals near-infrared fluorescence at specific emission wavelengths for each probe in the anatomic region of the stomach. B, Ex vivo FMT imaging of the stomach from a Smad4+/− mouse shows signal in visible gastric tumors. The 3D FMT image is superimposed on the 2D FRI. C, 2D FRI of gastric tumor activated by cathepsin. D, 2D FRI of gastric tumors activated by MMP. Noted are differences between the two probes: the white arrow demonstrates probe activation with cathepsin but not MMP, and the black arrow shows a neoplasm with cathepsin versus MMP.
Quantitative Comparisons of Cathepsin- and MMP-Activatable Probes In Vivo
For the cathepsin probe, the 3D FMT quantification measured a 2.5-fold greater total fluorescence signal (Figure 2C) and a significant 1.8-fold greater in fluorescence signal intensity in the stomach ROI of Smad4+/− mice versus WT mice (Figure 2D). Similarly, for the MMP probe, 3D FMT in vivo imaging yielded a 3.0-fold increase in total fluorescence (Figure 2G) and a 2.2-fold increase in fluorescence SI (Figure 2H) in the stomach ROI of Smad4+/− mice compared to WT controls.
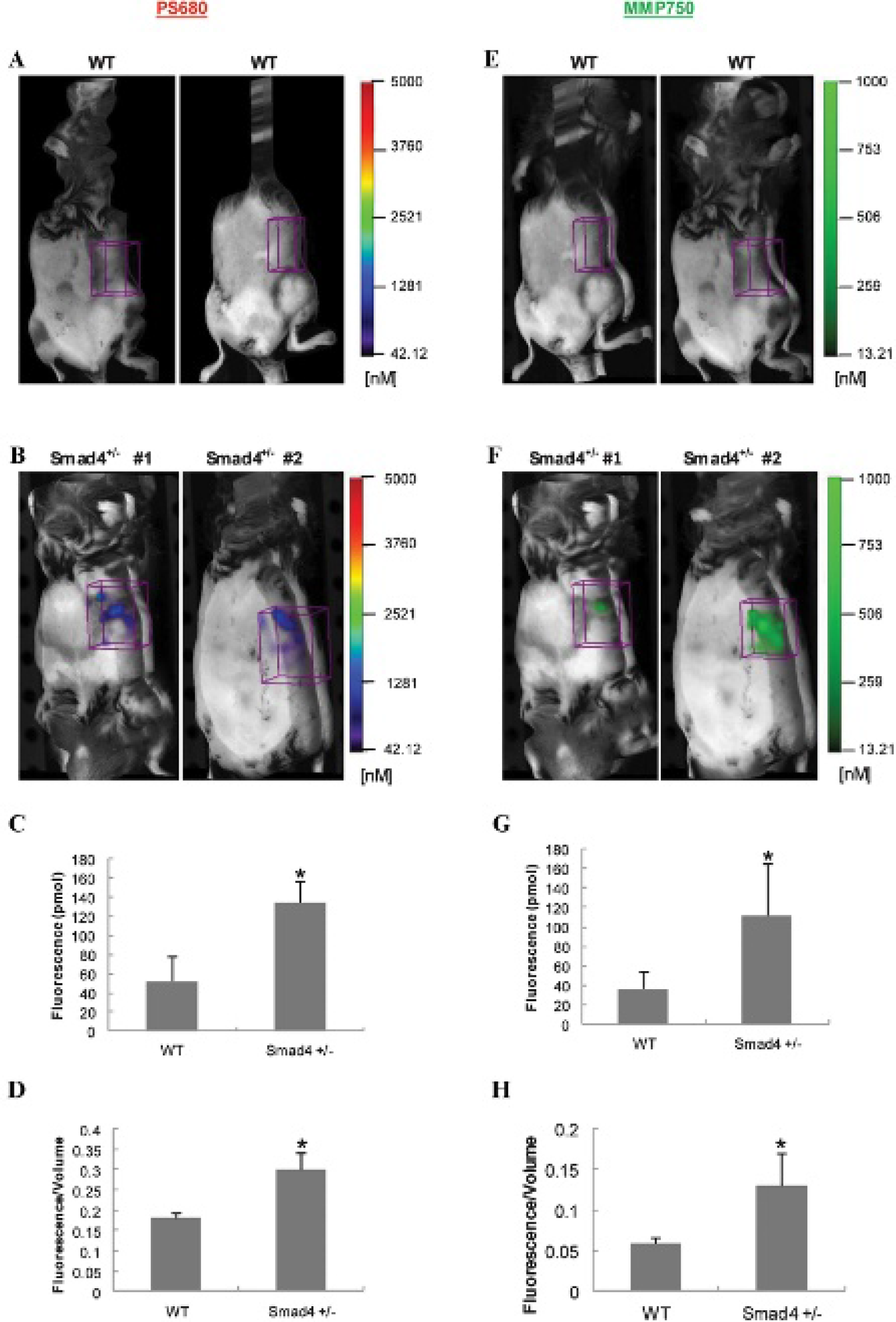
In vivo imaging of wild-type (WT) and Smad4+/− mice injected with cathepsin and matrix metalloproteinase (MMP) probes. Regions of interest were placed in the stomach region from each animal. A, E, Representative images from WT controls. B, F, Representative images from Smad4+/− mice. C, G, 3D quantification of total fluorescence (pmol). D, H, Fluorescence intensity (total fluorescence divided by volume). Histograms show mean ± SEM; n = 4 for Smad4+/− mice and n = 3 for the WT mice; *p ≤ .05 compared to WT mice.
Quantitative Comparisons for Ex Vivo Detection of Gastric Tumors
Ex vivo imaging of freshly dissected stomach from WT and Smad4+/− mice confirmed the ability of detecting tumors by using NIRF probes, cathepsin (Figure 3, A–C) and MMP (Figure 3, D–F). FRI had modest background fluorescence signal in the stomach of WT mice (Figure 3, A and D), but significantly stronger signals were observed in focus regions of the stomach of Smad4+/− mice corresponding to grossly evident tumors (Figure 3, B and E). Mean data for WT versus Smad4+/− mice indicated a significant greater signal in Smad4+/− mouse stomach compared to WT mouse stomach (ProSense 680: 175.81 ± 12.8 vs 91.4 ± 8.0 counts/energy; MMPSense 750 FAST: 96.41 ± 22.9 vs 54.4 ± 4.3 counts/energy). Furthermore, on average, the TBC value indicated an increased protease activity in the region of the tumor in Smad4+/− mice compared to WT: TBC was 92% increased with cathepsin and 77% increased with MMP. (Similar values for TBC were calculated in the comparison of tumor and grossly normal areas in Smad4+/− mice.)

Ex vivo fluorescence reflectance imaging (FRI) of stomach tissue from wild-type (WT) and Smad4+/− mice injected with cathepsin and matrix metalloproteinase (MMP) molecular probes. Stomach tissues were dissected immediately after in vivo imaging and imaged at 680 and 750 excitation wavelengths. Identical regions of interest (circles) were placed on the area of interest in WT and Smad4+/− mice stomach. A, D, Representative FRIs from WT mice. B, E, Representative FRIs from Smad4+/− mice injected with the cathepsin and MMP probes (D). C, F, 2D quantification of total counts (counts/energy) in WT and Smad4+/− mice. Histograms show mean ± SEM; n = 4 for Smad4+/− mice and n = 3 for the WT mice; *p ≤ .05 compared to WT mice.
Histologic Confirmation of Gastric Neoplasia Detected by Activatable NIRF Probes
On dissection, macroscopically evident tumors were present in the antrum of each of the Smad4+/− animal models (Figure 4, A, B), which is consistent with previous findings in these mice. 23 To validate that the fluorescence signals observed with activatable NIRF probes are specific, histology was performed on sections of stomach tissue from Smad4+/− and WT mice. As shown in the representative H&E images in Figure 4 and in Table 1, all Smad4+/− mice showed evidence of tumorigenesis with hyperplastic lesions, dysplastic lesions, and adenocarcinoma. The number of gross lesions matched the number detected with activated probes, with the exception of the lack of MMP probe activation in the hyperplastic lesions.
Summary of Pathology of Individual Tumors Detected by Probes in Smad4+/− Mice


Histologic analysis of gastric tumors detected by activatable probes in Smad4+/− mice. A, Normal stomach. B, Antral tumor. The white arrow points to antral tumors. C–F, Progression of tumor formation from atypical hyperplasia (D), dysplasia (E), and adenocarcinoma (F, G). The black arrow points to the infiltrating lymphocytes. Original magnifications (hematoxylin and eosin stain) ×7.11 for A and B; ×10 for C to F; ×40 for G. An = antrum; Du = duodenum; Fu = fundus.
Discussion
In the present study, we provide proof of principle of the utility of NIRF-based molecular imaging for detection of gastric adenocarcinoma. Specifically, we described the efficacy of NIRF imaging by both in vivo and ex vivo methods with the cathepsin-activatable and the MMP-activatable probes to detect gastric neoplasia in the Smad4+/− gastric cancer mouse model. The MMP probe is activated by gastric dysplasia and adenocarcinoma, whereas the cathepsin probe is activated by hyperplastic lesions as well as dysplastic and adenocarcinoma.
The cathepsin probe is composed of cathepsin substrates, representing preferred substrates for cleavage by cathepsin B compared to other cathepsins. 24 Cathepsin B is a 30 kDa cysteine endopeptidase found mainly in the lysosomes of normal tissues.25,26 It is involved in proteolytic degradation and turnover of extracellular proteins, which is an essential step in cancer invasion and metastasis.27,28 A number of studies have shown that cathepsin B is overexpressed in gastric cancer tissues compared to noncancerous regions.29–31 The MMP probe comprises substrates of MMPs, representing preferred substrates for cleavage by MMP-2 and MMP-9. 10 Evidence suggests that MMP-9 is highly expressed in human gastric carcinoma and can serve as a prognostic marker.6,20,32,33 Thus, detection of elevated cathepsin or MMP activity in regions of gastric dysplasia or cancer is potentially an effective tool for molecular probe–based detection of gastric tumors. Both probes are optically quiescent and undetectable prior to interaction with their respective cysteine proteases. They become activated on protease cleavage, permitting emission of NIRF of sites of protease upregulation and probe activation. The probe activation is visualized at specific times after injection (ProSense 680, 24 hours; MMPSense 750 FAST, 6 hours), which have been shown in studies to permit sufficient concentrations of the agent to be cleaved by cathepsins or MMPs, respectively, in tissues where these enzymes are highly expressed.
The fluorescence imaging technologies FMT and FRI are widely used imaging techniques. FMT permits in vivo detection of specific cellular and subcellular targets 34 because of its advantages of deep tissue penetration and high target to background ratio. In the current study, we tested FMT for in vivo imaging, and the results demonstrated that FMT for activatable NIRF probes is effective for in vivo detection of gastric tumors. We demonstrate and quantify in vivo that both ProSense 680 and MMPSense 750 FAST were activated in the gastric region of Smad4+/− mice at significantly higher levels than in WT control mice.
Our study suggests that the MMP probe is activated by gastric dysplasia and adenocarcinoma, whereas the cathepsin probe is activated by hyperplastic lesions as well as dysplastic lesions and adenocarcinoma. Interestingly, in our previous study of molecular imaging in colon cancer animal models, cathepsin B was not significantly activated in colonic hyperplastic polyps. These differences warrant further study and analyses of molecular and histopathologic features of tumors yielding differing signals with the probes. This finding also suggests important and useful differential sensitivity and specificity of two probes for the detection of gastric neoplasms.
Conclusion
This proof of principle study in murine models demonstrates the feasibility of the use of activatable molecular probes and NIRF imaging to improve detection of gastric neoplasia and cancer. Future studies combining endoscopy or capsule endoscopy with novel molecular probes and imaging techniques may significantly improve gastric tumor detection for future clinical application.
Footnotes
Acknowledgments
We thank Dr. Howard Zhang (Department of Internal Medicine, School of Medicine, Case Western Reserve University) for important input. We acknowledge Kirk McNaughton and the Histology Core Facility of the Department of Cell and Molecular Physiology at UNC-Chapel Hill. We would also like to thank Dr. Hong Yuan from the Biomedical Research Imaging Center (BRIC) and Dr. Weihua Tang of the Department of Pathology at UNC-Chapel Hill.
Financial disclosure of authors: This work was supported by a grant from the University Cancer Research Foundation at UNC-Chapel Hill (to P.K.L. and D.M.), National Institutes of Health grants (DK47769-11 [to P.K.L.], HD058290 to [Y.C.]), CA125588 (to D.M.) and a UO1 grant (CA105417-07).
Financial disclosure of reviewers: None reported.

