Abstract
Pathogenic mycobacteria are highly adapted for survival within host mononuclear phagocytes. This is largely due to the organism's capacity to prevent macrophage activation, block phagosome acidification and maturation, and attenuate presentation of antigens to the immune system. Mycobacterium avium subsp. paratuberculosis (MAP) is one such organism that modulates the ruminant innate immune response. It is the causative agent in paratuberculosis, a chronic progressive granulomatous enteritis in ruminants. MAP initially interacts with cell membrane receptors on bovine mononuclear phagocytes and initiates cell signaling responses and phagocytosis. Mannosylated liparabinomannan (Man-LAM) is a major component of the MAP cell wall that interacts with the cell membrane of mononuclear phagocytes and may be a major virulence factor. Toll-like receptor 2 (TLR2) has been incriminated as major signaling receptor that binds to MAP and initiates signaling though the mitogen-activated protein kinase (MAPK)-p38 pathway. This pathway induces transcription of interleukin (IL)-10. Early production of IL-10 suppresses proinflammatory cytokines, chemokines, IL-12, and major histocompatability factor class-II expression. Both IL-10 dependent and IL-10 independent mechanisms appear to be involved in attenuation of phagosome acidification and phagolysosome fusion. Many of the suppressive effects of MAP on bovine mononuclear phagocytes can be reproduced by exposure of bovine monocytes to Man-LAM. Therefore, MAP Man-LAM-induced TLR2-MAPK-p38 signaling with resultant excessive IL-10 expression has emerged as one of the mechanisms by which MAP organisms suppress inflammatory, immune, and antimicrobial responses and promote their survival within host mononuclear phagocytes.
Keywords
Mycobacterium avium subsp. paratuberculosis (MAP) is the causative agent of paratuberculosis (i.e., Johne's disease), a chronic granulomatous enteritis of wild and domestic ruminants worldwide. 18, 36, 58 Although this has been a sporadic disease problem in the past, concentration of animals as a result of modern farming practices has made paratuberculosis a worldwide epidemic. 43 MAP has also been incriminated as a possible cause of Crohn's disease, a severe progressive granulomatous ileocolitis of human beings estimated to affect 0.15% of the US population. 9, 32, 40 Several lines of evidence support a possible role of MAP as a causative agent in at least some cases of Crohn's disease. The intestinal pathology of paratuberculosis and Crohn's disease is similar. 32 MAP has been identified in intestinal tissue from patients with Crohn's disease by culturing the organisms and by polymerase chain reaction. 32 Additionally, some patients with Crohn's disease respond to antimycobacterial therapy. 14
Mononuclear phagocytes play a pivotal role in the detection and elimination of pathogenic microorganisms and initiation of an adaptive immune response. 8, 11, 51, 87 Despite this, pathogenic mycobacteria have developed mechanisms to survive within mononuclear phagocytes by blocking or modulating macrophage antimicrobial activities. 2, 65, 70 Additionally, the intracellular environment appears to protect the organism from extracellular antimicrobial mechanisms of the host. To fully comprehend the complex host-pathogen relationship, we must understand the complex molecular interactions that occur between the host and the organism. These interactions begin when the cell wall of the organism interacts with cell membrane receptors on the host cell and initiates cell signaling and phagocytosis. The subsequent pattern of proinflammatory and anti-inflammatory signaling, cytokine and chemokines expression/secretion, and phagosome trafficking/maturation determines whether the organism is destroyed or establishes a long-term infection. 70 Other confounding factors include genetic variation in both the host and the organism that alters disease susceptibility/virulence. 62
Early studies provided some clues as to how pathogenic mycobacteria successfully colonize macrophages. Mycobacteria were known to possess highly complex cell walls that provide a formidable permeation barrier and are resistant to degradation. 15 Another key advance in understanding of mycobacterial survival came when it was discovered that phagosomes containing mycobacteria fail to acidify and mature to become phagolysosomes. 4 As a result, the organism survives and replicates within immature phagosomes.
Several pathogenic mycobacteria, including MAP, M. avium subsp. avium (MAA), M. bovis, M. tuberculosis (Mtb), and M. leprae cause disease in mammals. 8, 51, 87 To investigate macrophage responses critical to the survival of mycobacterial organisms, we and others have compared the response of macrophages or dendritic cells ingesting virulent mycobacteria to those ingesting nonvirulent mycobacterial organisms. 30, 51, 59, 76, 89 Because considerably more is know about survival strategies of Mtb, we will begin by discussing general mechanisms associated with virulence among pathogenic mycobacteria. Thereafter, we will focus on the interaction of bovine mononuclear phagocytes with MAP organisms.
Allelic Variation and Susceptibility to Mycobacterial Diseases
Results of many studies have established a link between susceptibility to mycobacterial infection and genotypic variation of the host. 6, 50, 53, 62 Evidence includes susceptibility/resistance of individuals, variation in susceptibility of inbred and knockout mice and immunodeficient families, and association of disease susceptibility with particular nucleotide polymorphisms. Susceptibility is under multigenic control. Genes incriminated include major histocompatibility complex (MHC) class-II, natural resistance associated macrophage protein 1 (Nramp1, also termed SLC11A1), tumor necrosis factor-α, (TNF-α), interleukin (IL)-10, tumor necrosis factor (TNF) receptor, interferon (IFN)-γ and IFN-γ receptor, T-cell receptor, IL-6, and IL-12. 5, 53, 85 Each of these variants result in functional defects in macrophages or dendritic cells. 85 Nramp1 was originally identified as a candidate gene in mice and was shown to control resistance to M. bovis, Salmonella typhimurium, and Leishmania donovani. 84 Later studies have shown that Nramp1 codes for a 12 transmembrane domain integral membrane phosphoglycoprotein that is expressed by macrophages and neutrophils. Nramp1 is constitutively expressed, IFN-γ inducible, and rapidly recruited to the phagosome membrane through fusion with Nramp1-containing vesicles. 17 Susceptibility to mycobacterial infections in mice is associated with a glycine to aspartic acid substitution at position 169 of the putative transmembrane region. 54 The variant molecule in susceptible mice is rapidly degraded and not expressed. 84 Polymorphism of Nramp1 has been identified in humans and cattle. No relationship of allelic variation in Nramp1 to mycobacterial resistance has been identified in cattle but a possible relationship has been identified in goats. 1, 62 However, a quantitative trait loci segregating within families on BTA20 has been linked to susceptibility to MAP infection in cattle. 31
Several cytokine and cytokine receptor mutations have been associated with susceptibility to mycobacterial infections in human beings. These include mutations in IL-10, IL-12, IL-12 receptors, IFN-γ, IFN-γ receptors, TNF-α, and STAT1. 5, 59 Single nucleotide polymorphisms in the promoter regions of cytokine genes have been associated with altered levels of the respective cytokines. 5 These individuals are susceptible to weakly pathogenic mycobacteria, including M. bovis and MAA. 48 Lesions are characterized by poor granuloma formation and progressive infections that may lead to death despite intensive antibiotic therapy. 48 Several TNF-α gene polymorphisms have been reported to influence TNF-α production. 48 Variable rates of TNF-α production have been associated with polymorphisms in the promoter region. For example, a single nucleotide polymorphism at nucleotide −308 has been associated with susceptibility to M. leprae and a variety of other intracellular organisms. 48
Genes located in the MHC complex, including MHC class-I and class-II molecules, are highly polymorphic. MHC class-I and class-II are cell surface glycoproteins essential for cell-to-cell interactions in immune regulation. Despite extensive investigation, few associations between MHC alleles and disease susceptibility have been documented. In screening human populations, HLA-DR2 is most frequently associated with tuberculosis. 53
Cell Membrane Receptor Ligation and Phagocytosis
Mycobacteria have developed numerous mechanisms for entering host mononuclear phagocytes through specific receptor-mediated pathways. 25, 77 Cell membrane receptor-organism interactions activate host cell signaling pathways but do not appear to alter organism gene expression. 13, 67 These cell signaling events precede phagocytosis and thus determine the nature of the macrophage response before the organism enters the cell. 13, 77
Mycobacterial cell wall receptors
The cell walls of mycobacteria contain a variety of molecules, including complex lipoglycans, glycoproteins, and lipoproteins. Major ligants identified on the surface of mycobacteria include lipoarabinomannan (LAM), 19-kDa lipoprotein, and the mycolyl-arabinogalactan peptidoglycan complex. 15 LAM is a phosphatidylinositol-anchored glycolipid containing a mannose core with arabinofuranosyl side chains. Two major forms of LAM occur. A mannose-capped form (Man-LAM) is usually found in pathogenic mycobacteria and a arabinosylated LAM (Ara-LAM) is usually found in nonpathogenic mycobacteria. 70 Man-LAM of Mtb binds to mannose receptors, whereas Ara-LAM preferentially binds to CD14 and initiates signaling via Toll-like receptors (TLRs). 70 Unlike Man-LAM, Ara-LAM induces TNF-α and chemokine production by macrophages. Alternatively, Man-LAM from Mtb inhibits macrophage activation induced by lipopolysaccharide (LPS) and phorbol myristate acetate and inhibits phagosome maturation. 11, 49, 70
The 19-kDa cell wall lipoprotein of Mtb has been reported to signal both through TLR2 and mannose receptors. 23, 57, 60 This molecule inhibits IFN-γ-induced gene expression and MHC class-II expression and antigen processing by murine macrophages in a TLR2-dependent and myeloid differentiation primary response gene 88 (MyD88)–dependent fashion. Alternatively, mycolyl-arabinogalactan peptidoglycan complex inhibits these functions independently of TLR2, TLR4, or MyD88. 60 In addition to preventing induction of specific IFN-γ-responsive genes, the 19-kDa lipoprotein and mycolyl-arabinogalactan peptidoglycan inhibit the capacity of IFN-γ to activate murine macrophages to kill virulent Mtb. 60
Macrophage cell membrane receptors
Host cell membrane receptors potentially involved in phagocytosis include both complement-associated and non–complement-associated integrin receptors, CD14, immunoglobulin Fcγ receptors, scavenger receptors, and mannose receptors. 25, 77 Complement receptors (CR1, CD11b/CD18, and CD11c/CD18) are the major receptors involved in phagocytosis of most mycobacterial organisms, including MAP, MAA, M. bovis, and Mtb. 25, 73, 77 However, other receptors, including mannose receptors and CD14, are also involved. Several studies report complex interactions between receptors in promoting organism phagocytosis. For example, in one study, binding of M. bovis to CD14 of TLR2 initiated “inside-out” signaling that converted low avidity CD11b/CD18 into an active receptor leading to increased organism internalization. 71
Many macrophage surface receptors are involved in cell signaling. 25, 37, 51, 70 These receptors include integrin receptors, TLRs, mannose receptors, CD14, scavenger receptors, and immunoglobulin Fc receptors. 25 Pattern recognition receptors, including TLR2, CD14/TLR4 complex, and mannose receptors appear to play a central role in early recognition and cell signaling in response to mycobacteria. 37, 60 Alternatively, although integrins are centrally involved in phagocytosis, they do not appear to be major components of MAP-induced signaling. 25 Results of several studies indicate that TLR2 may play a key role in initiating inhibitory cell signaling by pathogenic mycobacteria. 3, 37, 69, 80 Mtb attenuates macrophage responses to IFN-γ by blocking a subset of IFN-γ-inducible genes. 3 This effect is mediated through TLR2 but not TLR4 signaling. Some of these effects are mediated through the MAPK-p38 pathway. The mannose receptor has been primarily reported as a receptor for phagocytosis of mycobacteria. 25 However, upon interaction with Man-LAM, the mannose receptor also serves as a cell signaling receptor. 56, 70 Man-LAM has been shown to inhibit LPS-induced IL-12 production by binding to the mannose receptor. 56
Cell Signaling
Both pathogenic and nonpathogenic mycobacteria activate a series of host cell signaling pathways when they engage macrophage cell membrane receptors. 51, 66, 83 These signaling pathways initiate production of a variety of cytokines, chemokines, and antimicrobial metabolites that are critical to the control of mycobacterial infections. Major signaling pathways involved in initiation of inflammation and antimicrobial activity include mitogen-activated protein kinase (MAPK) pathways, phospholipase C, Rho GTPases, protein kinase C, phosphoinositide 3–kinase (PI3-kinase), cytosolic calcium concentration, and Janus kinase (JAK)/signal transducers and activators of transcription (STAT) signaling. 51, 66 The MAPK and JAK/STAT pathways are the major signaling pathways involved in macrophage activation and the inflammatory response and will be discussed here. 51 Other pathways, including phospholipase C, Rho GTPases, protein kinase C, PI3-kinase, and cytosolic calcium, are primarily involved in phagocytosis and phagosome maturation. 51
MAPK signaling pathways
The MAPK cell signaling pathways are a family of highly conserved serine/threonine kinases. 66, 70 The MAPK family is composed of 3 major MAPKs, including MAPK-p38, MAPK-ERK1/2, and MAPK-JNK. The MAPK-ERK1/2 pathway is activated by binding of growth factors and mitogenic factors to cell membrane receptors. The MAPK-p38 and MAPK-JNK are activated primarily by inflammatory and environmental stressors, including osmotic shock, inflammatory cytokines, and LPS, as well as by ultraviolet light. 70 Signaling through the MAPK pathways results in activation of a variety of transcription factors, including SP-1, ATF2, Elk-1, c-Jun, NF-κB, and MEF-2C, which in turn promote production of numerous biologically important transcripts. 51
The global effects of MAPK activation and the interaction of MAPK pathways with other cell signaling pathways are incompletely understood. Insight into the role of MAPKs in inflammation has been gained by use of specific chemical pathway inhibitors, including SB203580 for the MAPK-p38 pathway, PD98059 for the MAPK-ERK1/2 pathway, and SB600125 for the MAPK-JNK pathway. 64 Several studies have addressed MAPK signaling in macrophages during mycobacterial infection. 61, 66, 76, 83 Both pathogenic and nonpathogenic mycobacteria appear to rapidly activate the 3 major MAPK pathways within minutes of binding to macrophage cell membrane receptors. 13, 61, 74– 76, 83 However, key differences in the relative degree of activation of MAPK-p38 and MAPK-ERK1/2 may contribute to the eventual fate of mycobacterial organisms. This is important because MAPK-p38 signaling is primarily responsible for initiating IL-10 expression while MAPK-ERK1/2 signaling is essential for initiation of TNF-α expression. 70, 72, 76 Pathogenic strains preferentially induce MAPK-38 phosphorylation resulting in overexpression of IL-10. 12, 13, 64, 76, 83 The kinetics of MAPK activation may also vary. Murine macrophages infected with virulent MAA rapidly activated MAPK-p38 and MAPK-ERK1/2, but the activation was transient. 66 In contrast, macrophages infected with an avirulent strain had sustained activation of both MAPKs. The transient nature of MAPK activation by virulent mycobacteria may be due to induction of MAPK phosphatase-1 expression, which acts a negative regulator of MAPK pathway activation. 24
In summary, although both pathogenic and nonpathogenic mycobacteria activate all 3 MAPK pathways, the relative intensity and kinetics of activation of these pathways appear to have major effects on the production of inflammatory cytokines and on antimicrobial activity. 66, 76 In particular, the degree and timing of activation of MAPK-38 appears to be important in determining the capacity of mycobacterial organisms to survive within macrophages.
JAK/STAT signaling pathways
JAK/STAT receptors are a group of cell membrane receptors that bind cytokines, including interleukins, interferons, and hematopoietins. 35 Signaling is mediated by receptor oligomerization, which brings JAK kinases into close apposition and allows for tyrosine phosphorylation. Subsequent STAT binding and phosphorylation are essential for initiating signal transduction. Phosphorylation of JAK/STAT1/2 is mediated by binding IFN-γ to its cell membrane receptor. 51 IFN-γ binding to macrophages induces a bactericidal response through several mechanisms, including induction of reactive oxygen and nitrogen intermediates; synthesis of cytokines, including IL-12 and TNF-α; and promotion of phagosome maturation. Pathogenic mycobacteria suppress IFN-γ and JAK/STAT1/2 signaling. 51
In one study using mouse macrophages infected with virulent MAA, infected macrophages had decreased IFN-γ receptors on their cell membrane. 42 In another study using Mtb-infected macrophages, decreased association of STAT with transcriptional coactivators was demonstrated. 81 M. bovis infection of mouse macrophages induced expression of suppressor of cytokine signaling, which binds and inactivates JAK, thereby blocking JAK/STAT signaling. 51 Man-LAM promoted increased activity of tyrosine phosphatases-1 in human monocytes, which is an inhibitor of signaling through the JAK/STAT pathway. 49
Cytokine and Chemokine Production
Production of cytokines and chemokines is a critical factor in development of effective inflammatory and immune responses to mycobacterial infection. 11 However, these responses must be controlled to limit local tissue injury and prevent systemic inflammatory responses. 52 Therefore, both proinflammatory and anti-inflammatory cytokines are produced to regulate the inflammatory response. Additionally, regulatory T cells limit the extent of the immune response. However, some pathogenic microorganisms dysregulate the inflammatory and immune responses by inducing selective overexpression of inhibitory cytokines and thus abrogating inflammatory and immune responses. 8, 11, 51, 87 IL-10 and transforming growth factor-β (TGF- β) are the major inhibitory cytokines produced by macrophages. 16, 47, 88
IL-10
IL-10 is an immunomodulatory cytokine produced by a variety of cells, including monocytes/macrophages and T and B lymphocytes. 34 This cytokine plays a pivotal role in immune responses by suppressing macrophage activation and antimicrobial activity, by enhancing Th2-type immune responses, and by suppressing Th1-type immune responses. 28– 30 IL-10 is thought to suppress Th1-type immune responses largely through inhibition of IL-12 production by macrophages. 34, 94 IL-10 also inhibits cytokine production and antigen presentation by macrophage and dendritic cells. 34 Macrophages and dendritic cells in response to Mtb and MAP produce large amounts of IL-10 and depressed T-cell/IFN-γ responses in pulmonary tuberculosis were shown to be associated with IL-10 production by monocytes. 34 In vitro, IL-10 downregulates the production of IL-12 by monocytes infected with Mtb or MAP and inhibits the proliferation of IFN-γ producing T cells and γδ T cells. 34
TGF-β
TGF-β has multiple inhibitory effects on inflammatory and immune responses. TGF-β has been reported to inhibit IFN-γ production, suppress dendritic cell maturation and differentiation, decrease MHC class-II expression, and suppress organism killing by macrophages. 89, 90, 97
IL-12
Production of IL-12 by macrophages and dendritic cells is essential for induction of a Th1-type immune response that is essential for control of mycobacterial infections. Early studies in the murine model of tuberculosis clearly demonstrated that IL-12 and IFN-γ were both necessary for protection against Mtb infection. Mice deficient in the p40 component of IL-12 or in IFN-γ were both highly susceptible to Mtb infection. 68 Exogenous supplementation of IL-12 at the onset of disease led to reduction in bacterial burden and delayed the lung pathology in the relatively susceptible Balb/C strain of mice. 68 However, IL-12 supplementation did not lead to enhanced protection in IFN-γ-deficient knockout mice indicating that IFN-γ is downstream of IL-12 and is the effector molecule mediating protection in the host. 27, 68
TNF-α
TNF-α plays an important role in regulating the pathology associated with pathogenic mycobacteria. 7, 10 TNF-α exists in both soluble and membrane-bound forms and signals through TNF-α receptor. Mycobacterial infection leads to TNF-α secretion by macrophages, dendritic cells, and T cells. 10 Secretion of TNF-α by Mtb-infected macrophages is a potent mechanism to induce killing of organisms via generation of reactive nitrogen intermediates. 10 TNF-α also induces apoptosis of Mtb-infected alveolar macrophages, and thereby indirectly contributes to reduction of bacterial burden. 11 The requirement for TNF-α in host defense against Mtb infection was demonstrated in studies in which mice treated with anti-TNF-α antibody became more susceptible to bacille Calmette-Guérin (BCG) infection and exhibited malformed granulomas. 7 Mtb infection of mice lacking TNF receptor or neutralization of TNF-α activity in mice also led to the failure to control bacterial replication resulting in enhanced susceptibility.
Macrophage Antimicrobial Activity
A major mechanism by which mycobacteria survive within macrophages is by inhibiting phagosome acidification and phagolysosome fusion. 4, 78 Normally, nascent phagosomes undergo a stepwise maturation process that involves fusion with early and late endosomes and finally with lysosomes. This sequential interaction with endosomes involves acquisition and exchange of both membrane and luminal contents. 22 These interactions are highly controlled events involving ATPase N-ethyl-maleimide-sensitive factor (NSF), soluble NSF attachment proteins (SNAP), and vesicle and target membrane SNAP receptors (SNARES). 86 SNARE-to-SNARE interactions between endosomal membranes result in lipid bilayer fusion. 86 This process is under the control of Rab GTPases. Rab5 is acquired by early phagosomes and Rab7 is acquired later, just before phagosome-lysosome fusion. Rab5 has been shown to stimulate fusion of early phagosomes with endosomes, whereas, Rab7 stimulates fusion of more mature phagosomes with endosomes and lysosomes. 44 Within the phagolysosome, toxic compounds such as defensins, nitric oxide, oxygen radicals, and proteases degrade the phagocytized organisms. As this process proceeds, the phagosome becomes acidified. This process is dependent on the activity of vacuolar H+ ATPases within the phagosome wall.
Phagosomes of virulent mycobacteria fail to mature. This is indicated by failure to obtain late endosome markers, including lysosome-associated membrane proteins-1 (LAMP-1), LAMP-2, LAMP-3 (i.e., CD63), and Rab7, and retention of early endosome markers, including Rab5 and transferrin receptors. 4, 8, 76, 78, 96 The persistence of transferrin receptors appears to be associated with continuous exchange of these receptors with the cell surface. As a result, the continued uptake of transferrin may provide a source of iron for mycobacterial growth. 78
The exact mechanism used by mycobacteria to resist phagosome maturation is uncertain but may involve several factors. Inhibition of phagosome maturation and phagosome-lysosome fusion may be mediated, in part, by the direct effects of mycobacterial lipids intercalating into the phagosome membrane, thereby altering the physical properties of the membrane. 79 Alterations in cell membranes that have been identified include decreased membrane fluidity, increased aqueous permeability, and inhibition of transmembrane protein movement. 79 A mycobacterial sulfolipid has been shown to impair phagosome fusion and antigen processing when coated onto yeast particles. 4, 79 Intracellular calcium and PI3-K signaling are essential for phagosome maturation. Cytosolic calcium, by regulating the activities of 2 effecter proteins, calmodulin and serine/threonine protein kinase, alters phagosome maturation by modulating membrane fusion between phagosomes and lysosomes. Mtb has been shown to interfere with calcium and PI3-K signaling with resultant blocking of phagosome maturation. 51 Man-LAM has been incriminated as the major mediator of these inhibitory activities. 51 Man-LAM has also been shown to inhibit other macrophage antimicrobial functions. 49, 51 Additionally, recruitment of coronin 1 to the mycobacterial phagosome appears to be directly involved in preventing lysosome fusion. 45
The role of the MAPK pathway in phagosome maturation is incompletely understood. Recent studies have demonstrated that the endocytic pathway and MAPK-p38 signaling are interconnected. 28 This study reported that signaling through the MAPK-p38 pathway blocks the association of EEA1 and LAMP-3 with late endosomes. 28 Blocking the MAPK-p38 pathway caused phagosomal acidification and enrichment of the late endocytic markers lysobisphosphatidic acid and CD63 on mycobacterial phagosomes. These findings suggest that MAPK-p38 activity contributes to the arrest of Mtb phagosome maturation and demonstrate a negative regulatory role of MAPK-p38 in phagolysosome biogenesis.
Phagosomes containing pathogenic mycobacteria also have substantially higher pH compared with those containing nonpathogenic or killed organisms. 4, 78 Decreased phagosome acidification has been associated with lack of H+-ATPase pumps in the phagosome membrane. The role of H+-ATPases in phagosome acidification is supported by studies in which M. bovis BCG-containing phagosomes were acidified by addition of cofactors that activated vacuolar H+-ATPases. 33 In addition, pathogenic mycobacteria produce alkalinizing factors, including glutathione synthetase and urease. 33
Pathogenic mycobacteria also block antimicrobial activity within the phagosome, including nitric oxide and oxygen radicals. 20, 29 Mtb organisms block the association of inducible nitric oxide synthase with the phagosome membrane by altering the scaffolding protein EBP50 that normally binds inducible nitric oxide synthase to the cytoskeleton. 20
Apoptosis
Macrophages infected with mycobacteria tend to activate apoptotic pathways, resulting in cell death. 51 However, pathogenic strains of mycobacteria induce lower levels of apoptosis compared to less pathogenic strains. For example, bovine monocyte-derived macrophages had a greater percentage of apoptotic cells when incubated with the less pathogenic organism MAA than when incubated with the bovine pathogen MAP. 90 One factor thought to attenuate apoptosis is Man-LAM. 51 Man-LAM antagonizes apoptosis by preventing an increase in cytosolic calcium concentration. Cytosolic calcium is thought to facilitate apoptosis by increasing the permeability of mitochondrial membranes. This promotes release of pro-apoptotic products such as cytochrome c. 51 Man-LAM also stimulates phosphorylation of Bad a pro-apoptotic protein. Phosphorylation of Bad prevents the molecule from binding to the anti-apoptotic proteins Bcl-2 and Bcl-XL. Free Bcl-2 prevents release of cytochrome c from mitochondria. 51
Pathogenic mycobacteria also limit apoptosis by inhibiting TNF-α expression and releasing soluble TNFR2 that neutralize TNF-α activity. 51 This is accomplished primarily through overexpression of IL-10. 34, 76, 88 IL-10 not only suppresses TNF-α synthesis but also induces release of soluble TNFR2. 51
Antigen Presentation
Pathogenic mycobacteria, including MAP, Mtb, and M. leprae, appear to interfere with antigen presentation by inhibiting activation of proteolytic enzymes in the phagosome as well as alter expression and distribution of MHC class-I and class-II and coregulatory molecules. 30, 57, 65, 91 Macrophages infected with pathogenic mycobacteria have decreased cell surface MHC class II and fail to upregulate MHC class-II expression in response to IFN-γ. 91 Antigen processing may also be inhibited by neutralization of phagosomal proteinases. Phagosome membranes contain aspartic and cysteine proteinases that degrade antigens to peptides that can be presented to T cells. A major proteinase in the phagosomal membrane is cathepsin D. In early phagosomes, cathepsin D is present as a proenzyme that is activated as the phagosome matures. In phagosomes containing live mycobacteria, cathepsin D, and perhaps other proteolytic enzymes, remain in an inactive form. 30 Alternatively, in phagosomes containing dead organisms, cathepsin D is present in an active form. Therefore, inhibition of cathepsin D activation appears to be an active process.
Several mechanisms have been associated with inhibition with antigen presentation. IL-10 causes decreased antigen presentation to T cells that is associated with downregulation of MHC class II, CD80, CD86, and ICAM-1 on the macrophage cell membrane. 55 Interference with MHC class-II expression and antigen processing has also been attributed to the 19-kDa cell membrane lipoprotein of Mtb. 57 The activity of the 19-kDa lipoprotein on antigen processing is dependent on TLR-2. The 19-kDa lipoprotein is characterized by an N-terminal lipo-amino acid, N-acyl-S-diacylglyceryl cysteine that has immunomodulatory activity. Mtb may also impair the transport of newly synthesized MHC class-II through the endocytic processing compartments thus inhibiting the formation of peptide-loaded MHC class-II heterodimers. 57
Survival Tactics Defined for MAP Organisms
Compared to Mtb, relatively little is known about the molecular interactions that are critical for the survival of MAP organisms within bovine mononuclear phagocytes. To investigate these responses, we and others have compared the response of bovine monocytes or monocyte-derived macrophages ingesting MAP organisms to those of mononuclear phagocytes ingesting MAA organisms. 76, 89, 90– 92, 96 MAP and MAA are closely related organisms that are 93% conserved at the nucleotide level. 41 Although some strains of MAA are pathogenic in various species and can be isolated from bovine feces, MAA is rarely recognized as a pathogen in cattle. 21
Initial studies established that bovine monocyte-derived macrophages lacked the capacity to kill MAP organisms but were able to kill approximately half of MAA organisms within 72 to 96 hours. 92, 98 Other studies used DNA microarray technology to screen for differential expression of thousands of genes when bovine monocytes or peripheral blood mononuclear cells (PMBC) were infected with MAP. 82, 89, 90 These results were compared to results for uninfected monocytes, monocytes activated with IFN-γ and bacterial LPS, or monocytes infected with MAA. Additionally, PBMC gene expression from MAP-infected cows has been compared to PBMC from uninfected cows. 19 Each of these studies revealed a variety of differentially expressed genes associated with inflammation, cell structure, cell signaling, apoptosis, and transcription factors. When MAP-infected monocytes were compared to uninfected or MAA-infected monocytes, MAP-infected monocytes had greater expression of anti-inflammatory cytokines, suppressor of cytokine signaling, and apoptosis inhibiting genes and had lesser expression of MHC class-II, certain endosomal and lysosomal membrane components, and protein kinase cell signaling molecules. 89, 90 In other studies comparing gene expression by PMBC from MAP-infected and uninfected cows, MAP-infected cows had twice as many downregulated genes as upregulated genes suggesting that MAP-infected cows had suppressed PBMC function. 19 Results of these studies indicate that MAP may induce a net anti-inflammatory response; inhibit macrophage cell signaling, antigen presentation, and apoptosis; and alter endosome and lysosome structure and function.
MAP and MAA organisms differentially regulate cytokine expression by bovine mononuclear phagocytes. 89, 90, 92 Bovine mononuclear phagocytes incubated with MAP expressed larger amounts of IL-10 and transforming growth factor-beta mRNA and lower amounts of IL-12, TNF-a, and IL-8 compared with cells ingesting MAA. Therefore, MAP-infected mononuclear phagocytes tend to produce relatively large amounts of anti-inflammatory cytokines and small amounts of proinflammatory and proimmune cytokines.
Results of subsequent studies indicated that cellular responses were initiated when MAP or MAP cell wall components interacted with host cell membrane receptors. 77, 93, 96 These receptor interactions were particularly critical to host responses because they induced an early response that preceded phagocytosis. A major signaling receptor incriminated in susceptibility to MAP infection was TLR2. Alternatively, MAA did not appear to signal through the bovine monocyte TLR2 receptor. 26, 77, 96 TLR2 has been shown to activate the MAPK-p38 pathway and may activate the NF-κB pathway as well. 95 Both pathways initiate IL-10 transcription. Early and excessive expression of IL-10 would be expected to suppress both the inflammatory and immune responses to MAP infection. 34, 46, 63 The effects of IL-10 in suppressing immune responses is highlighted by results of a study in which adding a neutralizing anti-IL-10 antibody to bovine PBMC obtained from cows with paratuberculosis resulted in a 23-fold increase in IFN-γ secretion in response to johnin purified protein derivative. 16
In addition to failing to initiate inflammatory and immune responses, bovine mononuclear phagocytes fail to initiate a robust antimicrobial response when infected with MAP organisms. 92, 98 MAP organisms are rapidly phagocytized and sequestered within phagosomes, but like other pathogenic mycobacteria, phagosomes containing MAP fail to acidify and form phagolysosomes. 73, 76, 96 MAP-containing phagosome have almost complete failure to acidify phagosomes even 18 hours after phagocytosis. 96 Compared with MAA, MAP-containing phagosomes fail to mature to phagolysosomes as determined by lower amounts of CD63 on the phagosome. 96 Results of several studies indicate that the block to phagosome acidification and phagosome maturation may involve TLR2 receptor signaling, MAPK-p38 activation, and IL-10. 76, 88, 96 Preincubation of bovine monocyte-derived macrophages with anti-IL-10 resulted in phagosome acidification and killing of some MAP organisms. 88 Likewise, preincubation of bovine monocytes with an inhibitor of the MAPK-p38 pathway decreased IL-10 expression and induced phagosome acidification and MAP killing. 76 Finally, preincubation with a neutralizing anti-TLR2 antibody resulted in increased phagosome acidification, phagosome maturation, and killing of MAP organisms. 76 Because adding anti-TLR2 antibody did not decrease IL-10 protein concentration in culture supernatants, TLR2 may have a IL-10-independent role in altering phagosome acidification and maturation. These results are consistent with results of other studies indicating that MAPK-p38 signaling across the phagosome wall blocks phagosome acidification and phagolysosome fusion. 28
Antigen presentation is also attenuated in MAP-infected macrophages. We investigated cell surface expression of MHC class-I and class-II molecules on bovine monocyte-derived macrophages infected with MAP or MAA. 91 Phagocytosis of both organisms resulted in a marked and persistent decrease in expression of MHC class-I and class-II molecules within 12 to 24 hours after phagocytosis. When IFN-γ was subsequently added, MHC class-I and class-II expression was increased in MAA-infected macrophages but remained low in MAP-infected macrophages. Additionally, microarray studies indicated that MHC class-II expression was downregulated in MAP-infected macrophages. 89, 90 Irreversible downregulation of MHC expression could contribute to the paucity of T-cell infiltrates and tubercle formation observed in Johne's disease lesions. 18
To further investigate the immunosuppressive mechanisms of MAP on bovine mononuclear phagocytes, we evaluated the effects of isolated cell wall components on bovine monocytes, including Man-LAM and 42 lipoproteins (unpublished data). Of these, Man-LAM appeared to be the major virulence factor. Man-LAM derived from MAP had substantially different effects on bovine monocytes than have been reported for Man-LAM from other pathogenic organisms. Man-LAM from MAP induces marked expression of both IL-10 and TNF-α by bovine monocytes, indicating that both proinflammatory and anti-inflammatory cytokine expression were stimulated. This difference may relate to different receptor interactions. IL-10 expression was attenuated by adding anti-TLR2 but not a mannose receptor inhibitor indicating that Man-LAM may interact with TLR2 receptors. In further studies, we evaluated the effects of Man-LAM on the interaction of bovine monocytes with MAA organisms. We found that preincubation of MAA with Man-LAM inhibited phagosome maturation and reduced the capacity of bovine monocytes to kill MAA organisms. Preincubation of monocytes with an inhibitor of MAPK-p38 but not anti-IL-10 ameliorated the inhibitory effects of Man-LAM on organism killing. As in previous studies, these data suggest that MAPK-p38 signaling across the phagosome membrane may be important in regulating phagosome maturation. 28 These results support the hypothesis that Man-LAM is a major virulence factor in mycobacterial survival within bovine mononuclear phagocytes and that MAPK-p38 is a major signaling pathway involved in inhibiting phagosome maturation as well as in initiating IL-10 expression.
Potential Applications to Paratuberculosis
The interaction of MAP with TLR2 receptors with resultant MAPK-p38 signaling, and rapid and excessive IL-10 expression has emerged as one of the major mechanisms by which MAP organisms suppress macrophage activation. The capacity of Man-LAM in initiating IL-10 expression and inhibiting phagosome maturation and organism killing provides evidence that this molecule is a major virulence factor. These findings have several potential applications to the clinical disease. First, these results suggest that studies of allelic variation in TLR2 or the IL-10 promoter may be informative in detecting genetic susceptibility to paratuberculosis. Second, these results could be used to intelligently design vaccine strains that lack cell wall components that interact with TLR2. Because Man-LAM appears to be the major inducer of IL-10 expression, Man-LAM-deficient forms may serve as vaccine candidates. Chemical treatments of MAP have been described to generate organisms that are deficient in Man-LAM and other cell wall components. 39 Third, this hypothesis can be tested in vivo. Recent development of several reproducible models will facilitate in vivo studies of the pathogenesis of paratuberculosis. 38 Quantifying the number and types of inflammatory cells and the expression/production of IL-10 in the intestinal wall at various stages of infection should be informative.
Conclusions
MAP organisms are highly adapted for survival within bovine mononuclear phagocytes. When they contact bovine mononuclear phagocytes they induce rapid and excessive IL-10 expression but minimal TNF-α or IL-12 expression. After phagocytosis, mononuclear phagocytes generate little nitric oxide, and phagosomes fail to acidify or fuse with lysosomes. Mononuclear phagocytes also have attenuated apoptosis and reduced MHC class-II expression consistent with altered antigen presentation. MAP-infected mononuclear phagocytes are also refractory to activation by IFN-γ or LPS. Therefore, MAP effectively interferes with macrophage activation and antimicrobial responses at multiple sites (Table 1).
Mechanisms presently known or suspected by which Mycobacterium avium subsp. paratuberculosis organisms suppress the antimicrobial response of bovine mononuclear phagocytes ∗ .
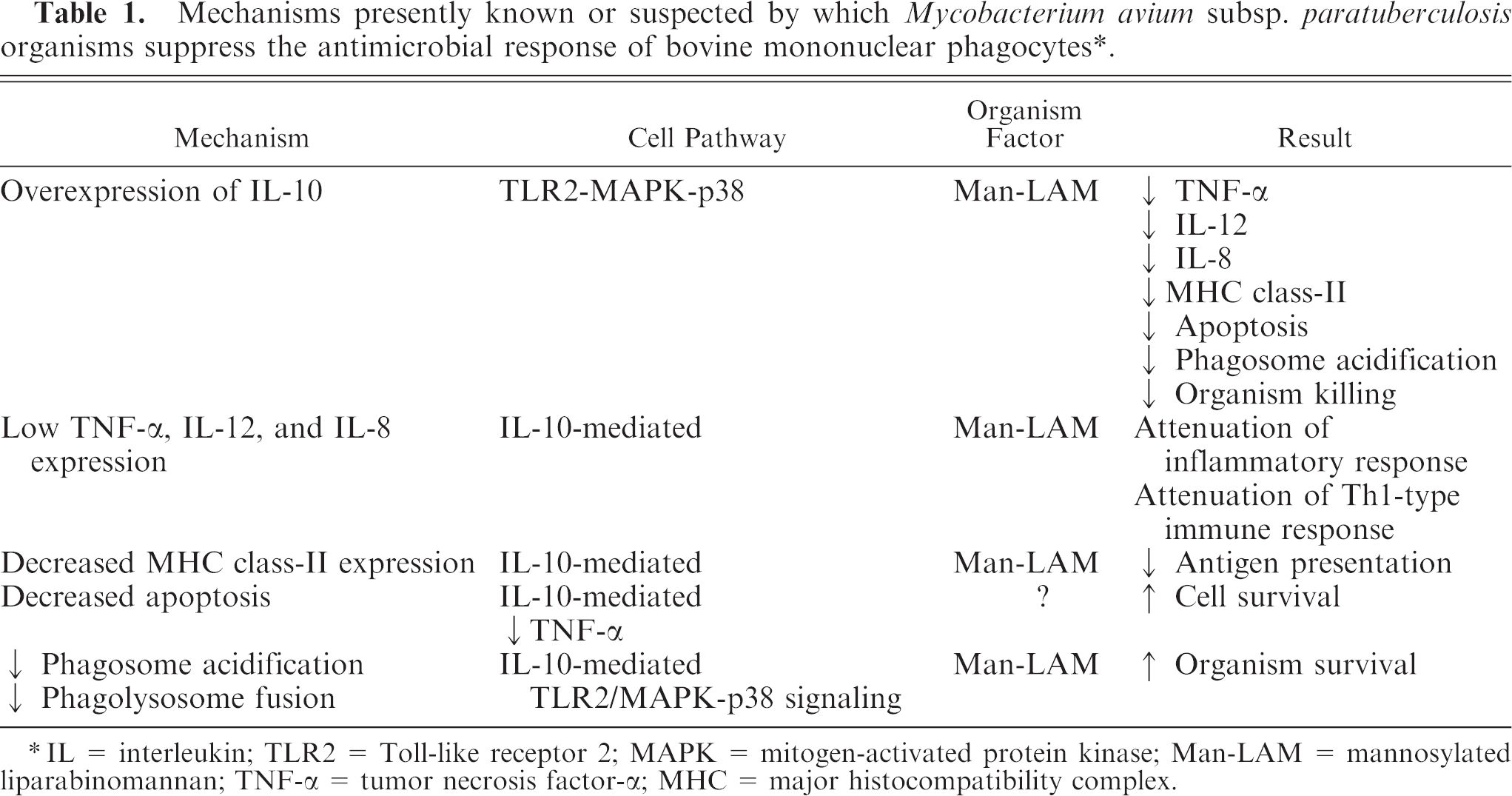
IL = interleukin; TLR2 = Toll-like receptor 2; MAPK = mitogen-activated protein kinase; Man-LAM = mannosylated liparabinomannan; TNF-α = tumor necrosis factor-α; MHC = major histocompatibility complex.
Results of several studies have highlighted the importance of interaction of MAP with cell membrane TLR2 receptors and signaling through the MAPK-p38 pathway in suppressing antimicrobial responses in bovine macrophages. Although other pathways are undoubtedly involved in survival of MAP within bovine mononuclear phagocytes, the TLR2-MAPK-p38-IL-10 pathway appears to play a significant role. Man-LAM appears to be a major virulence factor involved in mediating these events within bovine mononuclear phagocytes.
