Abstract
An evaluation of histologic findings in full-thickness biopsies from the gastrointestinal tract (GIT) from 64 dogs with chronic GIT disease symptoms was performed. In the majority of cases (38/64; 59%), intestinal lymphangiectasia and mucosal edema of unknown etiology were present. In 10 dogs (16%) an eosinophilic colitis, either alone or together with gastritis and/or enteritis, was found. In 5 dogs (8%) lymphocytic-plasmacytic enteritis or enterocolitis was diagnosed. Five dogs (8%) had an intestinal T-cell lymphoma. Samples from the remaining cases were histologically normal or did not allow for a final diagnosis. In contrast to reports about findings in endoscopic biopsies (which often are of varying quality or inadequate for diagnosis), in the majority of cases of this study, examination of full-thickness biopsies from the GIT allowed us to make a definitive histopathologic diagnosis. Furthermore, the study revealed that transmural biopsies are very helpful for diagnosing lymphoma.
Keywords
Chronic gastrointestinal diseases in dogs, such as inflammatory bowel disease (IBD), food allergy, and neoplasms, are mainly characterized by persisting or intermittent clinical symptoms of diarrhea, vomiting, or weight loss lasting more than 3 weeks. 4, 10 Histopathologic evaluation of biopsies from the gastrointestinal tract (GIT) is an important tool in the diagnosis of chronic GIT diseases. Especially in IBD a definitive diagnosis can only be made based on histopathologic analysis of GIT biopsy specimens. 3, 5, 9, 10, 14 One of the most common types of IBD in dogs is lymphocytic-plasmacytic enteritis (LPE). 3, 9 It has been suggested that LPE may have a patchy distribution throughout the GIT. 10 So far, except from descriptions of histopathologic findings in endoscopic duodenal and colonic biopsies, information on the occurrence of LPE in other segments of the small intestine (SI), i.e., jejunum and ileum, has not been available. There are only a few reports available, mainly limited to findings in samples taken endoscopically, describing the histopathologic appearance of GIT biopsies from dogs suffering from chronic GIT symptoms. 6, 11– 13
The main purposes of this investigation were 1) to compare the diagnostic value of full-thickness biopsies with endoscopic biopsies as reported in the literature and 2) to study the distribution of LPE throughout the GIT.
GIT samples were obtained from 64 dogs during the years 2000 to 2004. Prior to histopathologic diagnosis, all dogs of this study had been clinically suspect of having IBD because of anamnestic and clinical data presenting the main clinical symptoms of diarrhea and/or vomiting. In all dogs, symptoms had been present for at least 3 weeks up to 5 years. Dogs in which nodular GIT tumors were recognized clinically were excluded from this study. Fifteen dogs of various breeds and sex, euthanized for diseases unrelated to the GIT, served as controls (age range: 1 month to 17 years; mean age: 6 years). Transmural biopsy samples from diseased and control dogs were collected from the fundus region of the stomach, duodenum descendens, mid-jejunum, ileum, and colon descendens by using a 4-mm biopsy punch (GE Healthcare; Garbsen, Germany). From one diseased dog, 2 jejunal samples were available. Tissue samples were formalin fixed and paraffin embedded, and sections were examined histologically. In cases with lymphoma, immunohistochemistry was performed with antibodies against human CD3 and human CD79a molecule as described elsewhere. 7 For cases with LPE or enterocolitis, a histologic grading system was used. 4
Biopsy samples of control dogs showed a regular histologic architecture as described elsewhere. 3, 14 In 9 of 15 control dogs (60%), mild lymphangiectasia (LA) was present in the submucosa of the stomach (n = 3), accompanied by transmural LA of the colon wall in 1 of these dogs. One dog displayed mild transmural LA in the ileal biopsy. In 2 dogs dilated lacteals were present in all layers of the duodenum and, additionally, in the submucosa of the colon. Mild transmural LA was found in only 3 dogs, and mild edema was found in the lamina propria of the colon in only 1 dog.
In 5 of 64 dogs (8%) (mean age: 7 years; age range: 3 to 10 years), mild or moderate LPE was diagnosed in at least 1 of the SI tissue samples (Figs. 1, 2). In 3 of these cases, 1 of the SI biopsies had a normal histologic appearance. Mainly affected were the duodenum and jejunum (4/5) followed by the ileum (1/3) or colon (1/4). Only in the duodenum of 1 dog did the moderate lymphocytic-plasmacytic infiltration extend into the submucosa. In all cases, mild or moderate dilation of lacteals and mild mucosal edema was present in the small intestinal samples examined.
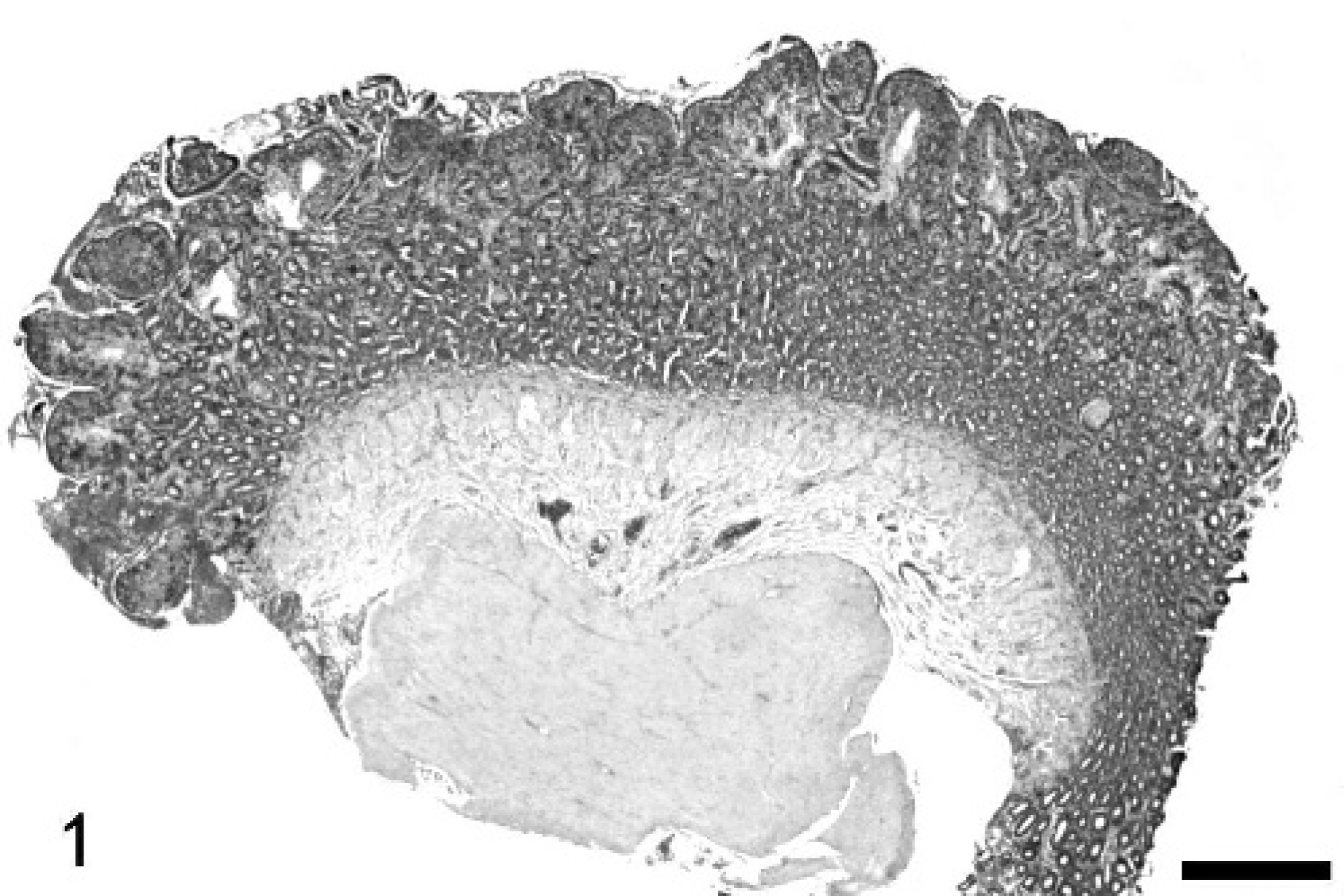
Duodenum, lymphocytic-plasmacytic enteritis; dog. Transmural biopsy with villous blunting and shortening. HE staining. Bar = 1600 μm.
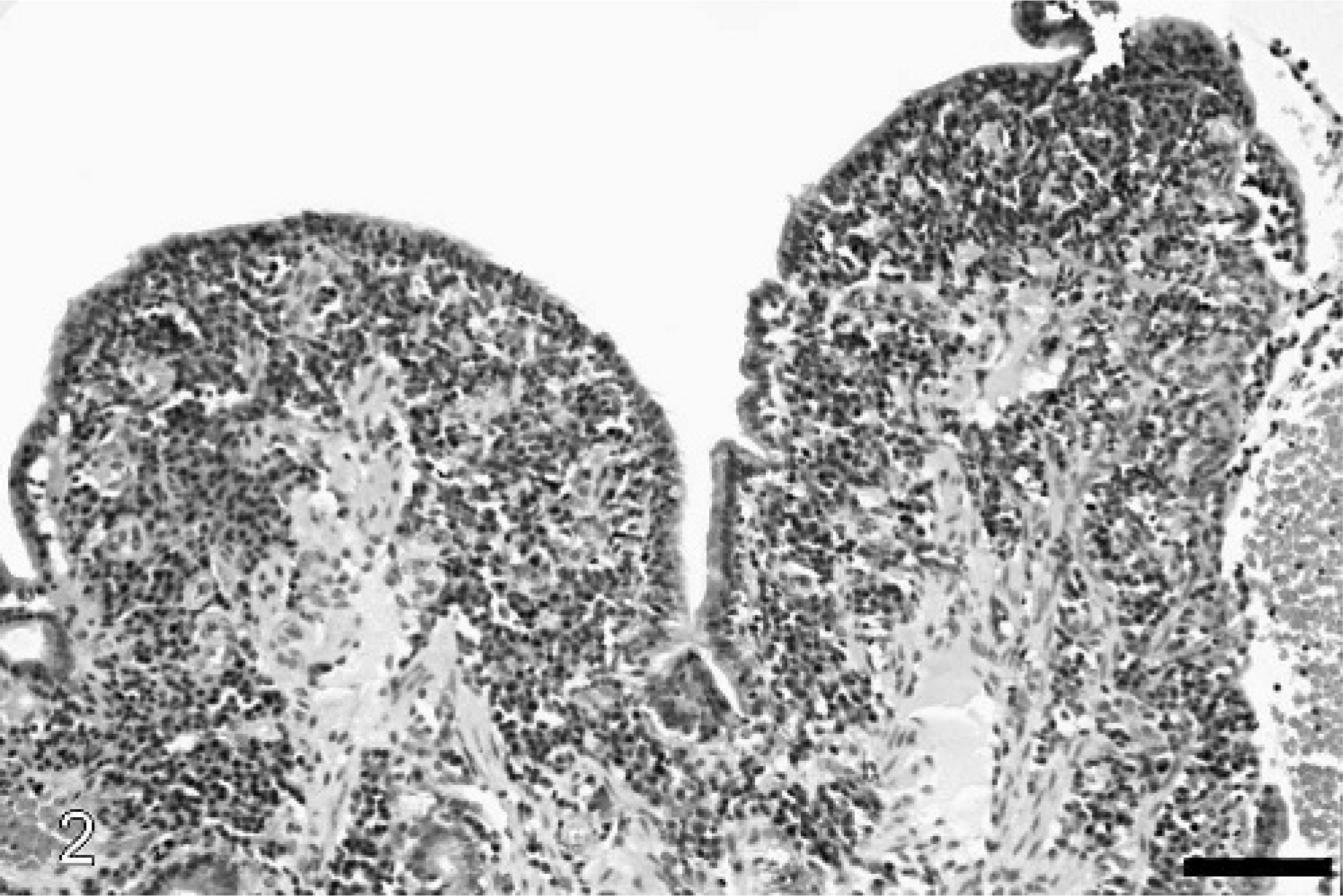
Duodenum, lymphocytic-plasmacytic enteritis; dog. Higher magnification of Fig. 1 displaying villous blunting and shortening with increased numbers of lymphocytes and plasma cells in the lamina propria. HE staining. Bar = 200 μm.
In 10 of 64 dogs (16%) (mean age: 4.2 years; age range: 1 to 7.7 years), an eosinophilic inflammation of the GIT was diagnosed. Evaluation of these 10 cases revealed that in 8 of them the colon, either alone (4/8) or together with the SI (2/8) or together with the stomach and SI (2/8), was affected. In all cases, increased numbers of eosinophils were found in the mucosa. In 3 dogs, an infiltration with eosinophils was present in the submucosa, and another 3 dogs had a transmural distribution. In all cases, slight to moderate LA was present in the lamina propria mucosae of biopsies from the SI and, except from 1 dog, there was also mild to moderate edema of the mucosa.
In 38 of 64 dogs (59%) (mean age: 5 years; age range: 1 to 15 years), varying degrees of LA of the lamina propria of the SI mucosa was the major histopathologic feature (Figs. 3, 4). Twenty-nine of 38 dogs (76%) displayed transmural LA. In the majority of these cases (n = 20) the SI was affected by transmural LA. In 35 of 38 dogs (92%), LA of the small intestinal mucosa was accompanied by slight or moderate mucosal edema. In 1 dog with severe transmural LA, a lipogranulomatous lesion was observed.
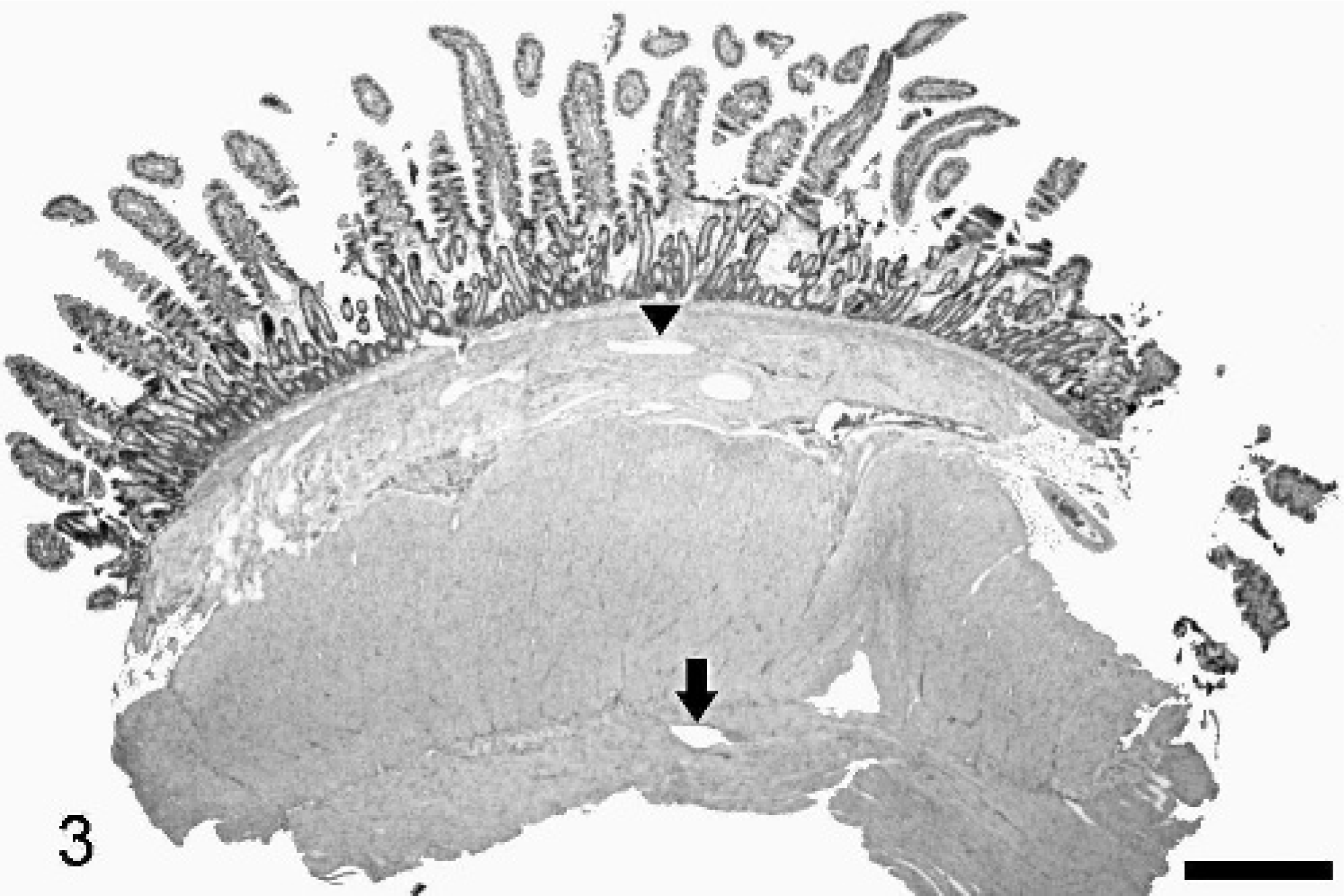
Jejunum, intestinal lymphangiectasia; dog. Full-thickness biopsy displaying transmural lymphangiectasia (arrow and arrow-head). HE staining. Bar = 1600 μm.
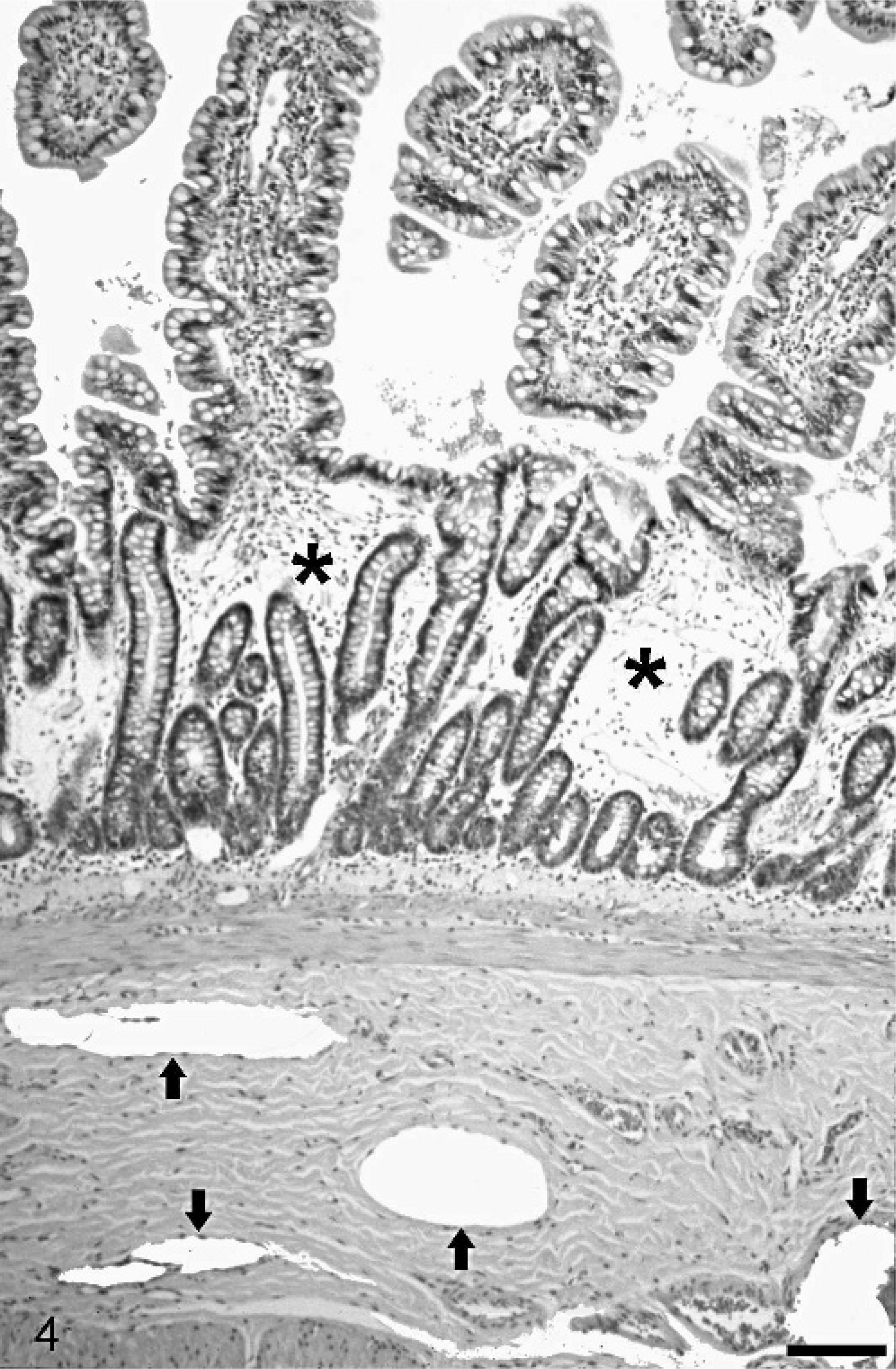
Jejunum, intestinal lymphangiectasia; dog. Higher magnification of Fig. 3 displaying severe submucosal lymphangiectasia (arrows) and mucosal edema (asterisks). HE staining. Bar = 280 μm.
In 5 of 64 dogs (8%) (mean age: 8 years; age range: 3 to 10 years) intestinal T-cell lymphoma was diagnosed. In these cases, 1, 2, or all 3 biopsies from the SI were affected while stomach and colon samples had a normal histologic appearance. In 2 cases neoplastic infiltration extended into the submucosa and in 2 other cases transmural infiltration was observed. Epitheliotropism of tumor cells was noted in 4 of 5 cases, affecting the duodenum (3/4), jejunum (2/4), and ileum (2/4). More than 95% of tumor cells were positive for CD3 antigen. Only a few cells were positive for CD79a antigen, interpreted as preexisting infiltrates. Mild to moderate LA of the lamina propria mucosae was a common feature in all cases and was present throughout all layers in 3 dogs. Edematous changes of these 3 dogs were only observed in the mucosa of the jejunum of 1 dog. In the 1 dog from which 2 intestinal jejunal biopsies were taken, neoplastic infiltration was visible in only 1 of the 2. In 2 dogs localizations adjacent to the lymphomas displayed a mild increased infiltration with mature nonneoplastic lymphocytes and plasma cells in the ileum or colon, respectively.
No histopathologic lesions were found in biopsies from 2 of 64 dogs (3%) (mean age: 3 years; age range: 1 to 5 years).
In 4 of 64 dogs (6%) (mean age: 4 years; age range: 2 to 9 years), no final histopathologic diagnosis could be made because the samples from the SIs only consisted of small parts of the lamina propria mucosae without villi and because biopsies from the stomach and colon were histologically unremarkable.
In the present study, examination of full-thickness biopsies from 64 dogs with chronic GIT disease symptoms allowed us to make a definitive histopathologic diagnosis in 60 cases (94%). In 5 of 64 dogs (8%) IBD, i.e., LPE or enterocolitis, was present. In these dogs, histopathologic findings largely resembled those described by other authors. 3, 4, 9, 10 In a study evaluating endoscopic biopsies from the SI of 383 dogs with chronic diarrhea, LPE was diagnosed in a considerably higher percentage of cases (24%) than in the present study (8%). 13 It has been pointed out by other authors that a universally accepted set of criteria or standardized grading system for evaluating intestinal mucosal specimens is missing and that the diagnosis of IBD remains largely subjective on the basis of evaluation of the cellularity of the lamina propria. 5, 15 In a recent study, substantial interobserver variations between pathologists evaluating tissue sections from intestinal biopsies from dogs and cats were detected. 15 Therefore, it can not be excluded that the discrepancy between the percentages of cases diagnosed to be affected by IBD in a former investigation and our study may be due to interobserver differences. 13 In 3 of 5 LPE cases, one SI sample had a normal histopathologic appearance, indicating regional variability of the lesion in the intestinal tract.
In this study, eosinophilic inflammatory changes were found in 10 dogs (16%). The cause of chronic eosinophilic inflammatory GIT disease of dogs is not known. Dietary sensitivity, such as food allergy and intolerance, has been proposed but not proved as a cause of eosinophilic gastroenteritis in dogs. According to several authors, it can occur as an idiopathic disease and therefore may be classified as a variant of IBD. 3, 5 Histopathologic changes in biopsies from the GIT are not pathognomonic for food allergy. 2
In the majority of the cases of this study (59%), the predominating histopathologic finding was intestinal LA without apparent increase in cellularity, which in 29 of 38 cases (76%) was transmural and in 35 of 38 cases (92%) was associated with edema of the lamina propria. The cause of intestinal LA and edema in these animals is not clear. Edema of the intestinal lamina propria may be a possible artifact occurring in endoscopic biopsies of dogs and cats. 13 Because LA was only observed in 3 of 15 controls and was mild and because edema was only noted in 1 of 15 controls, we believe that the LA observed in symptomatic dogs is unlikely to be an artifact of biopsy. The LA observed in these control dogs could be reasonably ascribed to the conditions for which they were euthanized, namely right-sided aorta, liver cirrhosis, and multiple abdominal masses. Intestinal LA in dogs can be a primary disorder (congenital or idiopathic) or secondary to lymphatic blockage by neoplastic or inflammatory infiltrates. 8, 10 The LA and edema noted in IBD cases of this study were probably associated with inflammatory infiltration. In the 38 other cases without increased cellularity or other lesions, however, the cause was not clear. It is possible that LA may have been due to vascular changes induced by certain mediators released from inflammatory cells not visibly increased in numbers (e.g., mast cells). The finding that lipogranulomatous lesions were only seen in 1 of our cases with intestinal LA further supports the view of other authors that they most likely are a consequence of lymphatic fluid stasis with chronic leakage of lipid-laden chyle, rather than a cause of lymphatic obstruction. 8, 14
In 8% of the cases of this study, an intestinal T-cell lymphoma was diagnosed. One of the most important differential diagnoses of intestinal lymphoma is LPE, and in many cases the only certain way to diagnose a neoplastic infiltration of the intestinal wall is to demonstrate the transmural spread of the neoplastic lymphoid cells. 14 The results of the present study clearly demonstrate the advantage of transmural biopsies for the diagnosis of intestinal lymphoma, especially in cases in which lymphoma cells are well differentiated. In 4 of 5 cases, diagnosis of intestinal lymphoma could be made easily because extension of the neoplastic process into deeper layers of the intestinal walls was found. In 1 case of our study examination of 2 available, jejunal biopsies revealed that infiltration with lymphoma cells was only present in 1 of these samples, indicating that intestinal lymphoma can have a patchy distribution. This finding also demonstrates the advantages of sampling more than 1 biopsy if possible. It has been reported that intestinal lymphoma in dogs can arise on the basis of LPE. 1, 3, 10, 14 Interestingly, in 2 dogs with lymphoma we found an infiltration of lymphocytes and plasma cells resembling mild LPE and lymphocytic-plasmacytic colitis, respectively, being present in samples obtained from adjacent intestinal segments, possibly indicating progression of IBD to intestinal lymphoma in these 2 cases.
In samples from 2 dogs with chronic clinical symptoms of GIT disease, no histopathologic findings were observed. These dogs may not have had histologic changes, or biopsy samples may have been taken away from lesional areas. In relatively few cases of this study (6%), it was impossible to make a final histopathologic diagnosis. For intestinal tissue specimens obtained endoscopically, it is very well known that the quality of samples can vary widely and that they are often inadequate for diagnosis. 13, 14 In 1 of these investigations it was reported that 23% of specimens obtained endoscopically from the SI of dogs with chronic diarrhea was unsuitable for examination. 13 From the results of this study, in which only transmural biopsies were available, no final conclusions can be drawn as to whether full-thickness samples obtained during laparotomy are of superior diagnostic value compared with endoscopic biopsies.
In conclusion, examination of full-thickness biopsies from all segments of the GIT allowed us to make a definitive diagnosis in the majority of cases in this study (94%). The inclusion of submucosal and deeper tissues within the biopsy was particularly helpful in the diagnosis of intestinal lymphoma
Footnotes
Acknowledgements
We thank Mr. K.-P. Kuhlmann for excellent technical assistance. This work was supported by the Deutsche Forschungsgemeinschaft (HE 1548/4-2).
