Abstract
Sacrococcygeal teratoma (SCT) is a germ cell tumor that can occur in newborns and infants. This case study centers on a 10-month-old girl, who presented with bruising over the lumbosacral area, after a fall. The initial examination in the emergency medicine department was normal, but the patient returned with persistent swelling and prominent vasculature. A sonographic examination demonstrated a Type IV SCT, which was further confirmed with additional diagnostic imaging. Type IV SCT is an internal growth that can be challenging to diagnose. This patient case illustrates the importance of an early diagnosis of SCTs, which can be detected with sonography. A thorough sonographic evaluation of the pelvis, by using varied ultrasound transducers and patient positions, can be helpful in identifying sacral pathology.
Sacrococcygeal teratoma (SCT) is a congenital tumor that arises in the sacral and coccyx region. 1 It is considered the most common germ cell tumor in newborns and infants. The incidence of these tumors are approximately 1 in every 40 000 births and has a 3.1:1 female-to-male ratio, in prevalence. 2 Type IV SCTs are rare entities and are particularly challenging to diagnose because they are difficult to find on physical examination. 3 Typically, sacral teratomas are benign masses but the incidence of malignancy increases with delay in surgical resection. 4 This patient case examines the benefit of using a curved ultrasound transducer, with a lower frequency, when examining the lower lumbar region. Curved ultrasound transducers provide a wider field of view and allow for deeper penetration of the acoustic beam. 5 Utilizing various patient positions and ensuring a fully distended urinary bladder can also be helpful, to improve visualization. This case report presents a Type IV SCT, in a 10-month-old girl, which initially presented with bruising over the lumbosacral area, after an incidental fall.
Case Report
A previously healthy 10-month-old girl came into the emergency medicine department (ED) presenting with bruising and prominent blue veins, over the sacrum. The parent reported the infant had fallen on her buttocks earlier that day. The ED providers reported a normal physical examination. The patient has a history of urinary tract infections (UTI), the most recent was reported 2 months prior, to this ED visit. A radiograph was ordered but never completed on this patient. Upon the provider’s reassessment, the patient’s pain had improved and was now controlled with non-steroidal anti-inflammatory drugs. The patient was discharged from the ED and referred to their primary care provider (PCP) for continued surveillance.
Nine days later, the patient returned to the ED, based on PCP’s recommendation for persistent lumbosacral swelling and prominent vasculature. The parents reported constipation and straining with bowel movements, over the past week. In addition, the patient was now refusing to ambulate. The ED providers initiated their assessment and a soft tissue sonogram, of the lumbosacral region, was ordered. The initial images were taken with the patient in a prone position using an IU22 ultrasound equipment system (Philips, Ultrasound, Bothell, WA) and a high frequency linear 12-5 MHz (L12-5) transducer, with a superficial setting. A soft tissue mass with hypoechoic components and irregular shape was visualized (See Figure 1A). Despite adjusting settings, with the L12-5, attenuation limited visualization of the deep margins of the mass (See Figure 1B). The sonographer addressed this diagnostic challenge by switching to curved transducers (C9-4 and C5-1), with lower frequencies. Lower frequencies have longer wavelengths that can travel deeper into tissues with less attenuation, enhancing the ability to see deeper structures. 5 The wider field of view from a smaller transducer footprint and deeper penetration of the acoustic beam allowed for improved visualization of the mass, which could now be seen abutting the sacrum (See Figure 2). To further increase visualization, the patient was placed in the supine position to evaluate the most caudal extent of the mass, in relationship to other pelvic structures. The urinary bladder was filled to improve the acoustic window. The mass’ relationship to the sacrum, its complexity, and mass effect on the bladder, ureters, and rectum were now evident (See Figure 3).
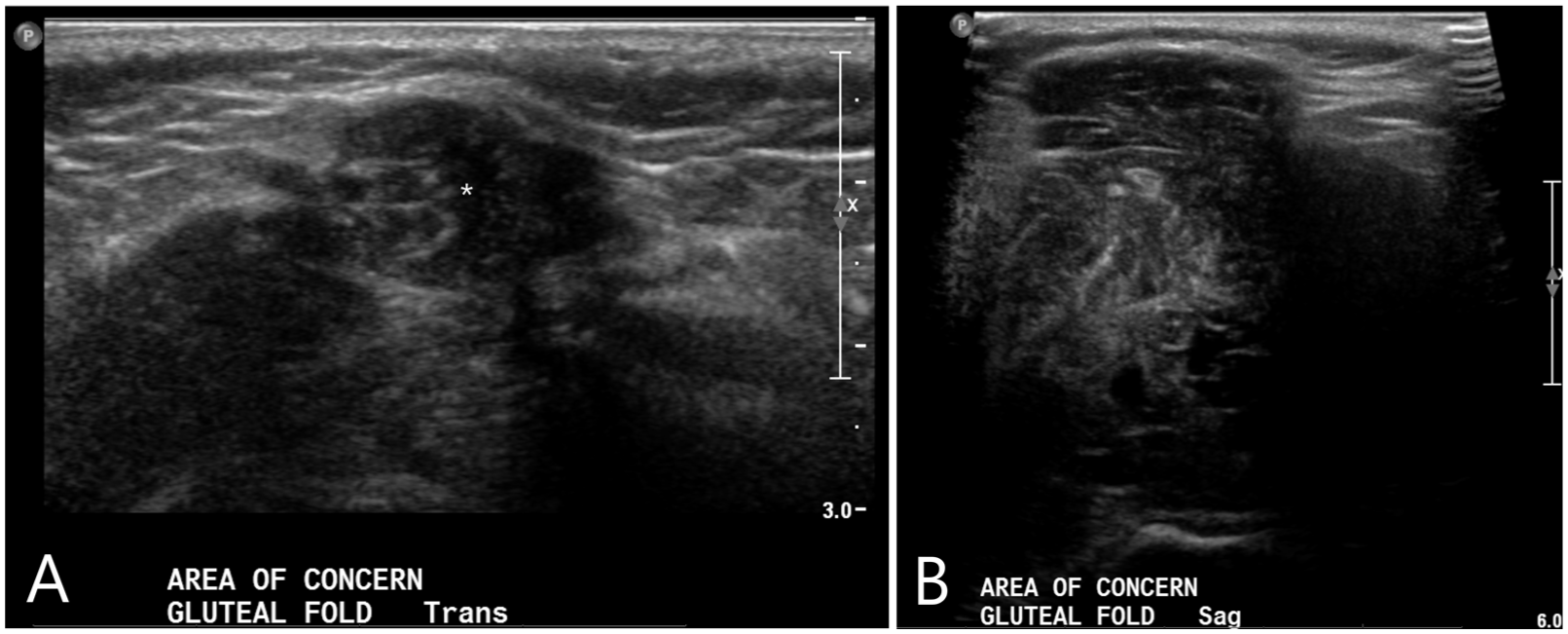
The sonogram, denoted with an (A), demonstrates the use of a high-frequency linear transducer in the gluteal fold and shows a complex soft tissue lesion (marked with an asterisk). Adjustments were made to the sonographic image, denoted with a (B), by increasing the depth and extend the field of view. It is important to note that the deeper extension of the lesion was limited by attenuation.
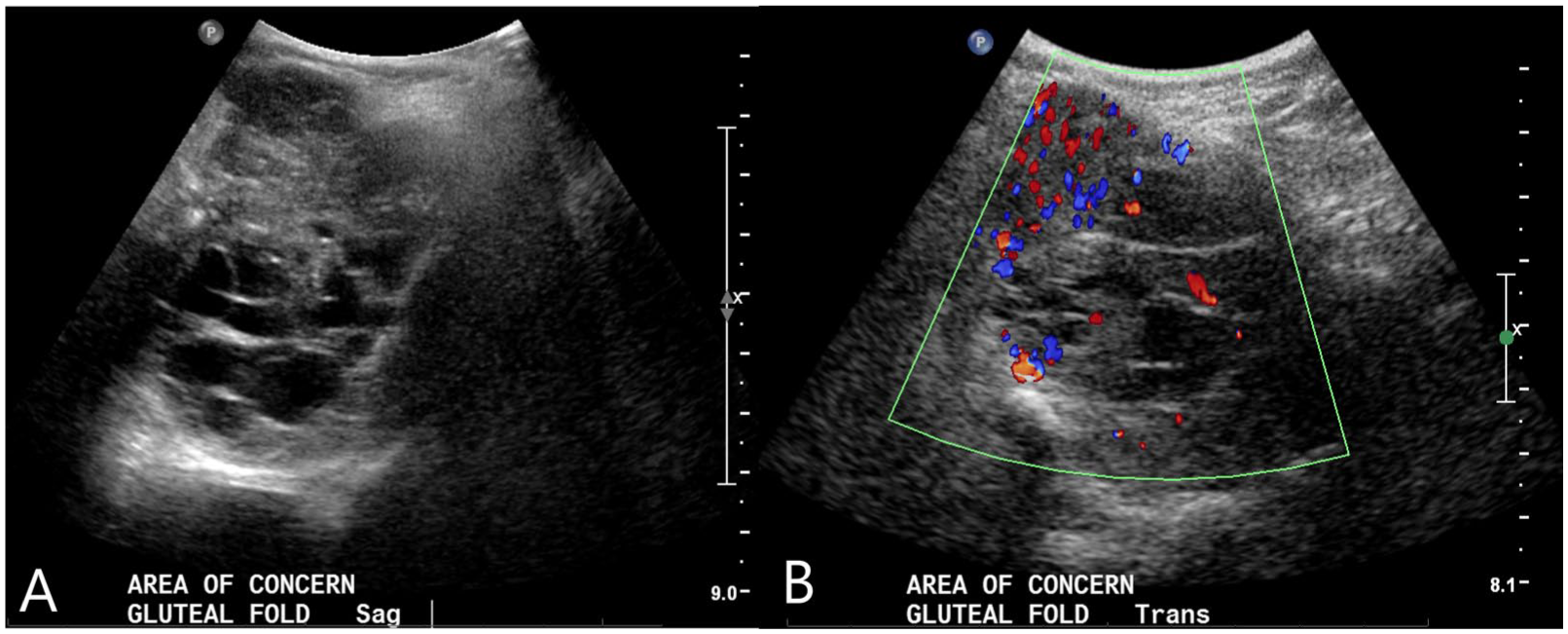
The sonographic image created with the curved transducer shows the deeper extent of the mass demonstrating additional complexity with solid and cystic components (labeled as image A). Color Doppler shows increased internal vascularity, a finding more consistent with a mass and not a complex fluid collection (labeled as image B).
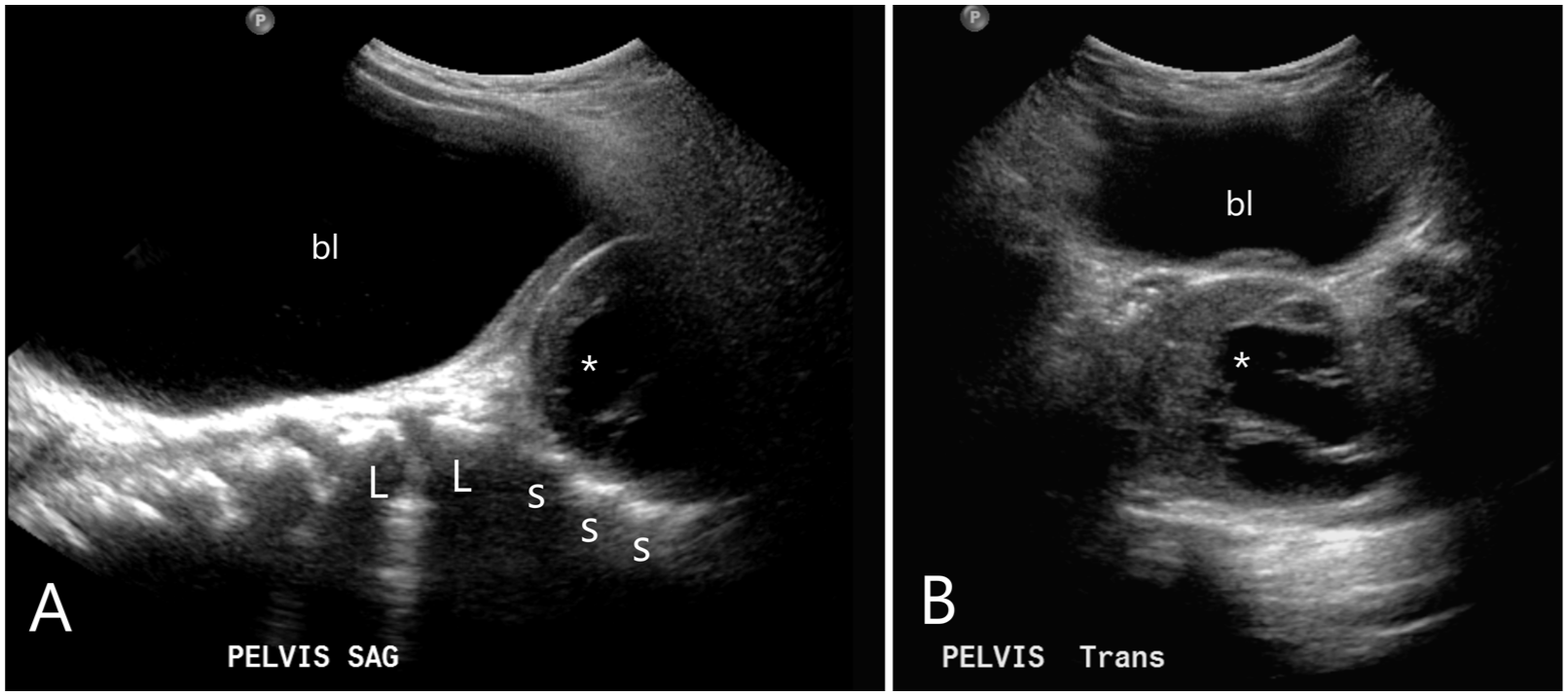
The sonogram, denoted as image (A), shows a well distended urinary bladder (labeled “bl”) providing a good acoustic window to visualize the mass (marked with an asterisk) abutting the sacral elements (marked as “s”) and the lower portion of the lumbar spine (L). The sonogram, denoted as image (B), shows the mass (marked with an asterisk) in the transverse plane posterior to the bladder (noted as “bl”).
Using only the linear transducer, initial measurements of 2.7 cm × 1.2 cm × 1.8 cm risked pathological misinterpretation. The reported measurement after switching transducers was 7 cm × 3 cm × 4 cm. Superficially, the teratoma would be described as a complex soft tissue lesion. Looking deeper revealed a hyper-vascular mass with multiple cystic spaces. The demonstrated characteristics of increased blood flow, heterogeneous components, cystic change, and areas of potential necrosis indicated an increased risk of malignancy (See Figure 2). The additional steps taken by the sonographer provided supplementary information to demonstrate that this was not a fluid collection or abscess. The added images enabled the radiologist to confidently diagnose the mass as a Type IV sacrococcygeal teratoma, based on its characteristic findings. Consequently, the patient was admitted to the hospital and additional imaging was ordered. A radiograph showed a soft tissue density that projected over the rectum and sacrum. Computed tomography (CT) (See Figure 4) and magnetic resonance imaging (MRI) (See Figure 5), completed on the second day of admission, confirmed the presumed diagnosis and findings. The MRI measurement of the mass was 7.3 × 4.5 × 5.6 cm and showed it extending into the spinal canal through the left S1-S2 neural foramen, where the nerve roots were displaced. There was abnormal marrow signal and fracture of L3 suggestive of metastases.
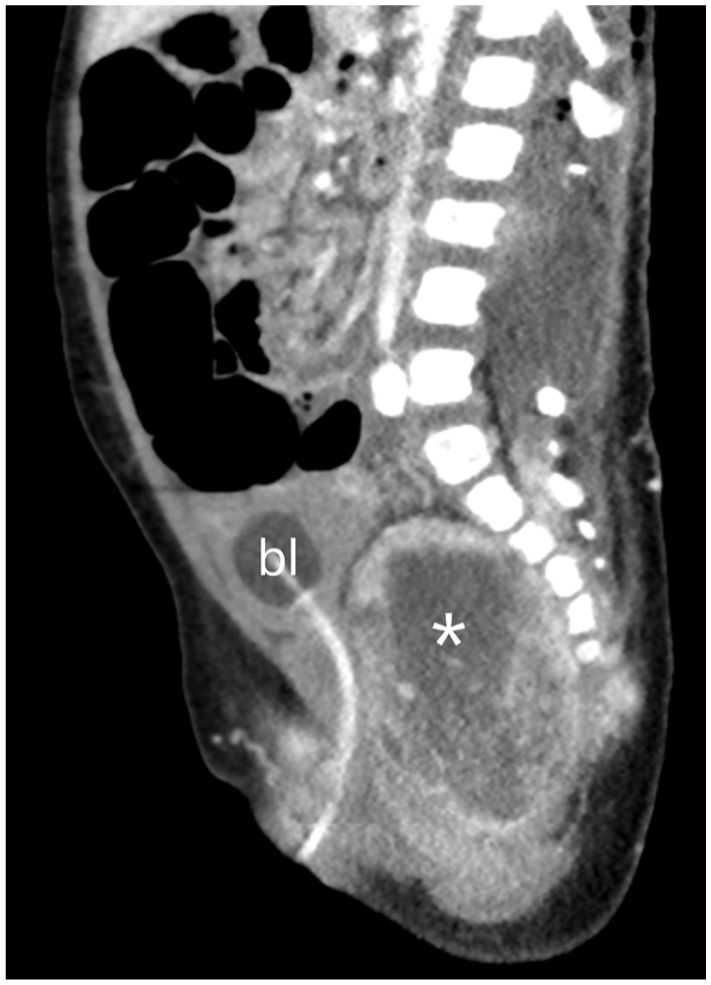
A sagittal reformatted computed tomographic image shows a heterogeneously enhancing presacral mass with large cystic components (marked with an asterisk). The urinary bladder (marked as “bl”) is displaced anterior and localized with urinary catheter in place.
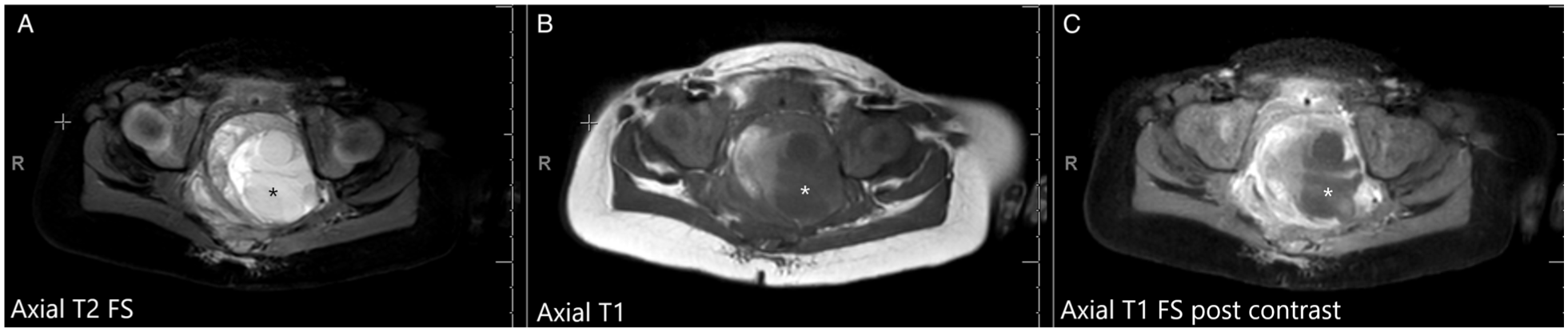
The MRI image, marked as (A), is an axial T2 slice with FS sequence, through the pelvis and demonstrates a presacral mass that is heterogeneous but overall T2 bright. T2 bright areas suggest a cystic component. The bladder is displaced anteriorly, marked by the presence of a urinary catheter. The MRI, image (B), is an axial T1 pre-contract image at the same level demonstrates portion of the mass along the right aspect to be T1 bright consistent with gross fat suggestive of a teratoma. The MRI, image (C), is an axial T1 FS post contrast image at the same level demonstrates the non enhancing areas confirming fluid component within the mass, greatest along the central and left aspect of this lesion.
On the second day of admission, a laminectomy of L2-L4 was performed due to severe cauda equina compression. Neurosurgical specimen was collected but was inconclusive for tumor specificity. However, there was a notable alpha-fetoprotein (AFP) level of 9696 consistent with a germ cell tumor. This instigated placement of a totally accessible venous access device (PORT), a repeat tissue biopsy, to determine treatment plan, and positron emission tomography (PET) examination.
On the fourth day of admission, the open tissue biopsy resulted in a mixed malignant germ cell tumor. The PET scan showed metastases in the lungs, liver, spine, and spinal canal (See Figure 6). The patient was treated with cisplatin-based chemotherapy consisting of six cycles of cisplatin, etoposide, and bleomycin (PEB treatment), administered intravenously. The surgical resection of the teratoma was performed 3 months later. The patient responded well to the treatment.
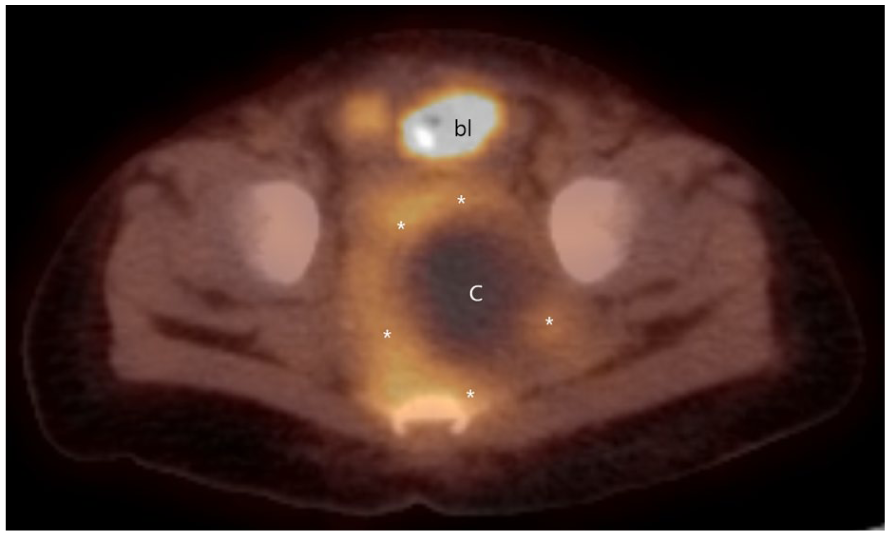
An axial positron emission tomographic (PET) image shows the bladder (marked as “bl”) is displaced anterior. Large presacral mass demonstrates increased FDG activity peripherally (denoted with an asterisk) with central necrotic component versus fluid component (marked as “C”).
Discussion
Sacrococcygeal teratomas represent the most common type of germ cell tumor in newborns and infants. 1 As the term implies, the tumor involves the sacrum and coccyx, adjacent or attached to the periosteum. 1 The origin is hypothesized to stem from embryonic germ cells located in Hensen’s node, which results in the layers developing in the genital organs, during the segmentation process. 6 Under microscopic evaluation, SCTs contain diverse types of epithelia, along with cystic and solid components. 6
There are four types of SCT, classified by Altman et al, 3 each characterized by their location and extent into surrounding tissue, in standard anatomical position. The characteristic differentiators as described by Altman et al, 3 as follows: Type I SCT is primarily external and compromises the posterior sacral region, Type II SCT has external visualization but with a significant intrapelvic component, Type III SCT is a predominant intrapelvic mass with minimal externality, Type IV SCT is internally located in the presacral area with no external component. The presacral region can be defined as the area anterior to the coccyx and the sacrum.
Determining the relationship of the mass to the sacrum can be challenging when examining the patient with sonography, in the prone position. Maintaining contact while scanning over the sacrum, along with a limited field of view, can be a constraint. It is recommended to take supine images of the pelvis, to gain a wider field of view, therefore providing greater contextual information for the interpreting radiologist. If the mass is large enough and the patient has a full urinary bladder, the inferior portion of the spine can be visualized with adequate depth. If the sonographer can further angle the transducer inferiorly, then the relationship of the mass to the sacrum, bladder, and other landmarks can be better demarcated.
Employing various transducers, with different frequencies enables a comprehensive assessment, ensuring that both superficial and deep structures are adequately visualized. Using both high- and low-frequency transducers can be expanded, by using both linear and curved transducers. While the linear transducer will provide greater resolution and characterization of the mass, the curved transducer delivers a greater field of view and allows the interpreting physician confidence in describing location and potential areas of mass effect. When combined with different acoustic windows, color Doppler, and patient positioning, a comprehensive evaluation provides the interpreting physician with the additional detail, to make the diagnosis. Particularly, adding supine images with a full urinary bladder enhances the acoustic window, offering additional supporting diagnostic information. This diagnosis is heavily reliant on complementary diagnostic imaging techniques that are used.
Historically, according to Altman, the most common misdiagnosis was myelomeningocele. 3 Differential diagnosis to consider include rectal abscess, lymphangioma, lipoma, hamartoma, ependymoma, chordoma, peroneal cysts, rectal prolapse, schwannoma, neuroblastoma, and rhabdomyosarcoma.3,4,7 The importance of considering differential diagnoses and understanding the potential for misdiagnosis, especially in cases where symptoms overlap with other conditions, cannot be understated.
Clinical presentation of Type IV SCTs, often involve vague symptoms, such as a palpable mass or abdominal distention. Laboratory findings may include non-specific elevation in alpha-fetoprotein (AFP) levels.1,3,4 Although typically asymptomatic, if symptoms arise it is generally caused by mass effect on neighboring organs. 1 This mass effect can lead to bowel and urinary bladder dysfunction, lymphatic, or venous obstruction, lower extremity paralysis, among other symptoms. 8 Urinary retention and constipation are rare but can occur. 1 In the late stages of disease progression, teratomas can cause pain and constipation. 3
Current evidence would suggest that malignant transformation increases over time. Teratomas diagnosed between 0 and 2 months, after birth, have a malignancy rate between 7% and 10% for females and males, respectively. 3 Both sexes show conversion to malignancy with diagnostic delay, males more progressively than females. 3 In Altman’s analysis, when the diagnosis of the teratoma was delayed past 2 months of age, the incidence of malignancy increased to two-thirds of males and about half of females. Early detection typically improves prognosis, increasing the likelihood of successful resection and reducing complications. Delayed identification may result in malignant degeneration and a larger, more challenging tumor to resect, affecting both surgical outcomes and long-term prognosis. 1
Treatment for SCT consists of surgical resection of the mass and compromised anatomy. 1 Benign teratomas can be managed through excision of the mass, however, malignant teratomas are treated with a multimodality approach including neoadjuvant chemotherapy (PEB treatment). 4 The surgical outcome and prognosis of SCT are favorable. 1 The recurrence rate after surgical resection has been estimated as 10% to 15%. 9 Patients are then monitored for relapse for several years through AFP checks and digital rectal examination. 1
Conclusion
This case report serves to aid in the early diagnosis of Type IV SCTs, using sonography as the primary imaging technique. In the hands of a skilled sonographer, sonography is an excellent diagnostic tool for postnatal screening, to aid in the diagnosis of Type IV SCT. When examining the lower lumbar region, using a curved transducer with a lower frequency supplies a wider view and allows for deeper penetration, which increases visualization. The sonographer can place the patient in a supine position and fill the urinary bladder to further enhance visualization and the acoustic window, respectively. The current case highlights the importance of conducting a thorough investigation while scanning with changing depth, transducers, patient position, and acoustic windows.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval for this study was waived by Phoenix Children’s Institutional Review Board as it was determined that it did not meet the definition of human subject research (IRB-24-225).
Informed Consent
Informed consent was not sought for the present study because all case data was de-identified and/or aggregated and followed ethics committee or IRB guidelines (also referred to as the Honest Broker System).
