Abstract
Cardiac auscultation is an integral element of bedside cardiovascular assessment, offering valuable clinical insights. Complementing this, echocardiography serves as a powerful diagnostic imaging tool that enables detailed structural and functional visualization of the heart. Understanding various auscultatory findings and their correlation with corresponding echocardiographic features can enhance cardiac sonographers’ insight into a wide range of cardiovascular conditions. This is an introduction for cardiac sonographers on how foundational knowledge of cardiac auscultation can be integrated into an echocardiographic examination. The focus is on the first heart sound (S1), serving as a starting point to bridge auscultatory findings with imaging correlations. The findings from M-mode, pulse wave Doppler of atrioventricular valve inflows, and tissue Doppler of the mitral and tricuspid valve annuli can be systematically integrated with the characteristics of a patient’s S1. Such awareness can guide sonographers to explore relevant findings more intentionally during the examination and hopefully contributing to improved diagnostic accuracy.
Since echocardiography emerged, it has revolutionized cardiac diagnosis. Historically, ever since the invention of the stethoscope in 1816, cardiac auscultation has been an indirect cardiac diagnostic tool. While auscultation provides valuable insights into the underlying hemodynamics and valvular function, echocardiography has been used for direct investigation of heart sounds. A cardiac sonographer can directly visualize the events leading to detected heart sounds and add that to the assessment while completing the full echocardiographic examination. This approach facilitates a better understanding of cardiac diseases and enhances diagnostic accuracy by using both indirect and direct analyses of relevant echocardiographic findings.
This symposium examines the first heart sound (S1) and its variations, as a foundation to connect auscultation with corresponding echocardiographic features. During the methodical performance of an echocardiographic examination, it is possible to systematically incorporate the characteristics of a patient’s S1 with relevant imaging features.
The First Heart Sound
The S1 is not widely discussed from a cardiac sonographer’s perspective. S1 signals the end of ventricular diastole and the onset of ventricular systole. 1 It is not a single sound but rather has two distinct components. There is a louder mitral component (M1) corresponding to the mitral valve closure. This is followed by the tricuspid component (T1) corresponding to the closure of tricuspid valve.2,3 Audibly via stethoscope, the two components effectively merge into one sound, the S1.
S1 characteristics in an individual patient can be correlated with specific echocardiographic findings. To fully understand these correlations, it is also important to review the patient’s 12-lead electrocardiogram (ECG), with particular attention to the PR interval duration, 4 presence of bundle branch block, evidence of ventricular hypertrophy, and heart rhythm abnormalities. In addition, the heart rate itself can influence the audible loudness of S1. The auscultatory features of the S1 include loudness or intensity, location of S1 on the chest, separate audibility of M1 and T1 components, and presence or absence of beat-to-beat variability.
Parasternal Views
Mitral valve closure at the time of the S1 can be visualized by the cardiac sonographer. Ventricular contraction, causing an increase in left ventricular pressure leading to mitral valve closure, can be visualized with detail on echocardiography. Echocardiographers can observe the movement and position of valve leaflets in relation to the onset of ventricular contraction. This can give information regarding the timing and intensity of S1 and correlate these findings with mechanical events in the heart. Mitral valve leaflets approach closure right before ventricular contraction begins at the end of diastole. Loudness of S1 is influenced by the left ventricular function. 5 S1 intensity decreases when there is myocardial depression because of the decreased rate of intraventricular pressure development.
M-mode echocardiography is a valuable tool due to its high temporal resolution. Understanding of auscultatory findings was reinforced by research specifically using M-mode echocardiography. The mitral closure point on M-mode tracings coincides with S13 (See Figure 1). The QRS complex on ECG is a marker for S1, as illustrated. M1 occurs approximately 60 ms, and T1 approximately 90 ms after the onset of the QRS complex on the ECG. To measure the time intervals in milliseconds accurately by M-mode, one must maximize the sweep speed. 3
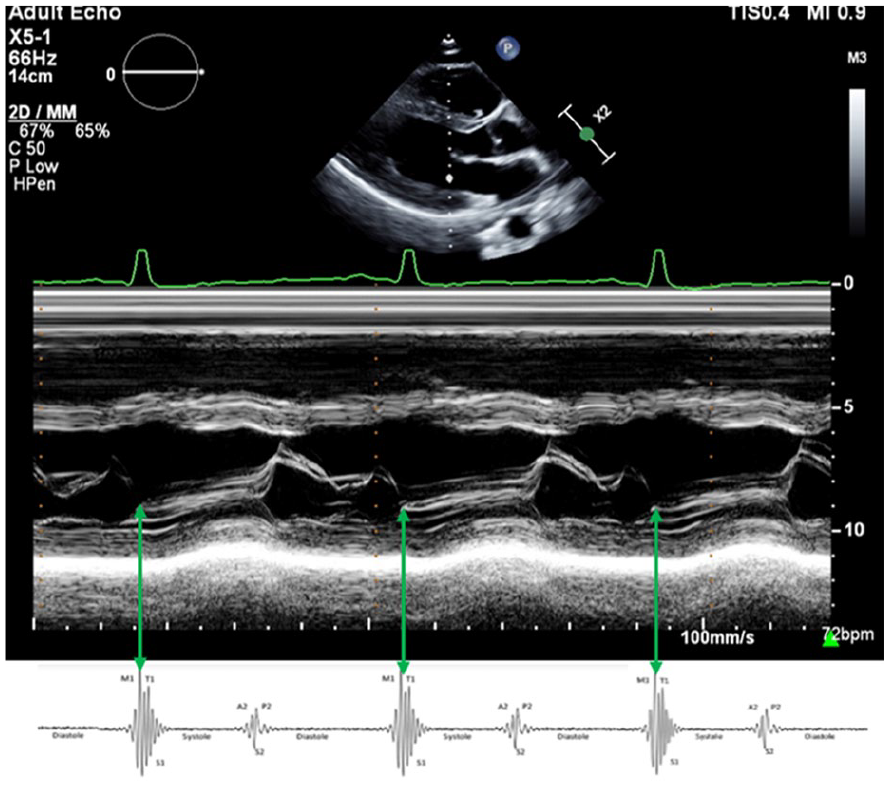
The image provided, illustrates the relationship between the timing of mitral valve opening on M-mode at mitral valve level and the first heart sound; Mitral and tricuspid components (M1 and T1) of the first heart sound correspond to mitral valve closure, represented by the C-point on the M-mode tracing indicated by green arrows.
Apical Views
When recording the S1, it is common to discover multiple components. From the perspective of the sonographer, it is easy to visualize and assess mitral and tricuspid valve closure. Mitral, aortic, tricuspid valve opening, and closure can be correlated to the Doppler tracings of the corresponding valve (See Figure 2). Also, by putting the sample volume between the mitral and aortic valves, it is possible to get both aortic and mitral Doppler signals in one tracing to have a better visualization and timing of valvular events with respect to S1 (See Figure 3).
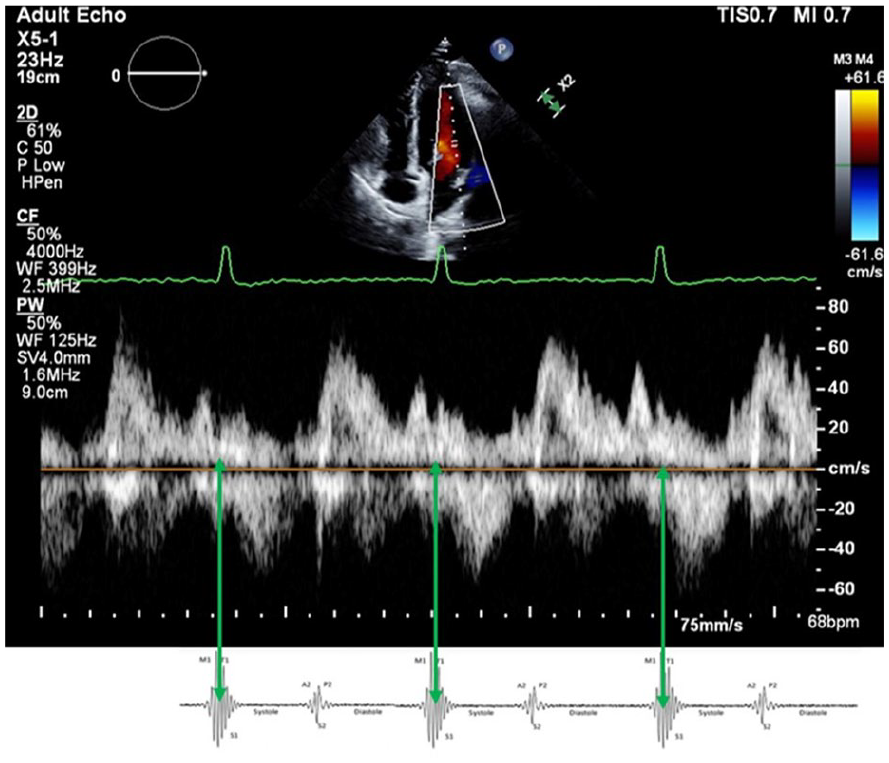
The image provided demonstrates the relationship between the first heart sound (S1) and mitral inflow Doppler tracings. S1 occurs at mitral valve closure and precedes systolic ejection, as indicated by green arrows.
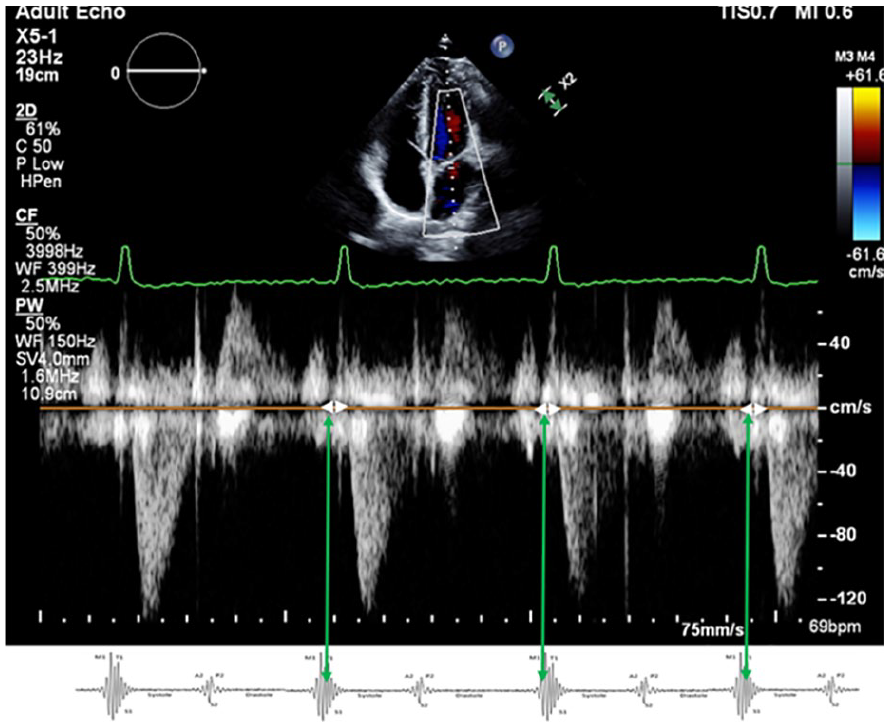
This image illustrates the correlation between the isovolumic contraction time (IVCT; indicated by white arrowheads) and the components of the first heart sound. S1 marks the onset of IVCT, as shown by the green arrow. The Doppler tracing was obtained using pulsed wave Doppler with the sample volume placed between the aortic and mitral valves in an anteriorly angulated apical four-chamber view.
Simultaneous multiple components can be demonstrated on tissue Doppler tracings of the mitral and tricuspid annulus around the time of the isovolumic period. The middle components of S1 in the phonocardiogram are the mitral closure component and the tricuspid closure component. Preceding that there is another component that can be thought of as an atrial component. Following that there is a component that can be considered as an ejection component. An increased isovolumic contraction time and decreased left ventricular ejection time are common findings in patients with left bundle branch block (LBBB). 6 Isovolumic contraction time can be assessed from mitral annular tissue Doppler tracings (See Figures 4 and 5). Left ventricular ejection time (See Figure 6) and stroke volume estimation are also part of the routine transthoracic echocardiographic protocol. The S1 occurs right before the ejection.
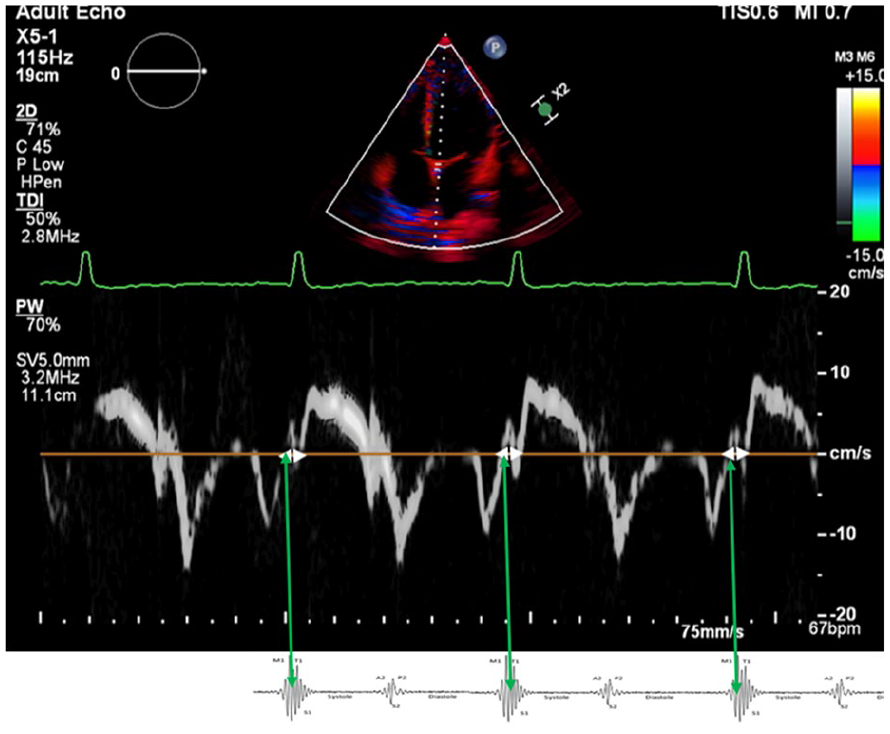
An example image is provided that Illustrates how tissue Doppler imaging at the mitral annulus can demonstrate the correlation between the isovolumic contraction time (IVCT; between white arrowheads) and the first heart sound. The green arrows indicate S1, corresponding to the onset of IVCT.
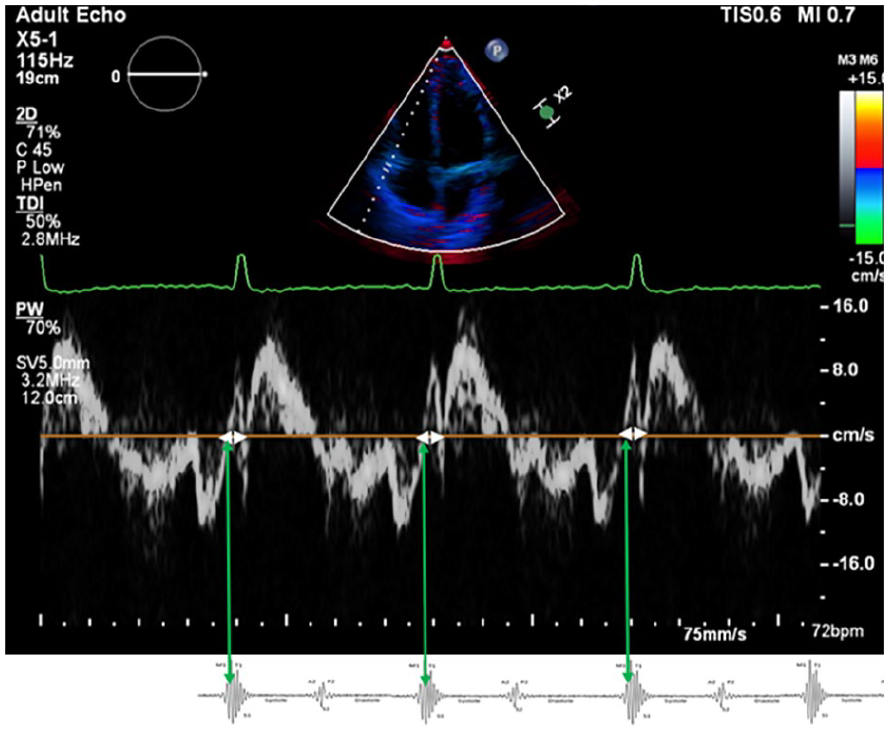
This image demonstrates how tissue Doppler imaging at the tricuspid annulus can demonstrate the correlation between the isovolumic contraction time (IVCT; between white arrowheads) and the first heart sound. The green arrows indicate S1, marking the onset of IVCT.
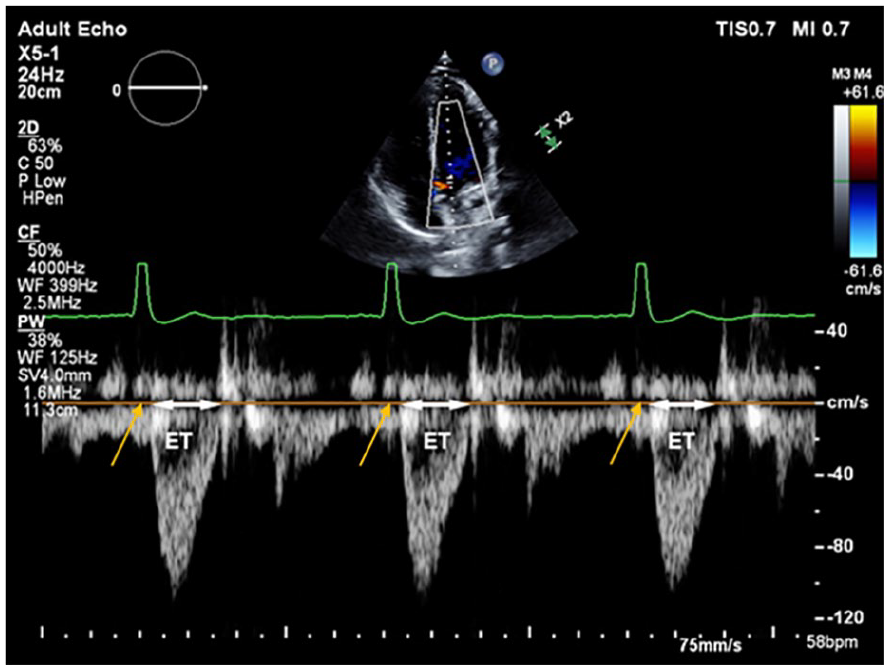
This image illustrates how ejection time (ET) is measured from pulsed wave Doppler spectral tracings of left ventricular outflow. The first heart sound (S1) is heard just before the onset of ventricular ejection, corresponding to the time marked by yellow arrows.
In addition, in the process of recording the S1, there are multiple components that are attributed to ejection. For a cardiac sonographer, these phenomena are not obvious in the sense of displaying prominent valve closure. Instead, multiple phenomena recorded on echocardiography can be related to the ejection of blood from the right and left cardiac chambers that influence sounds that are components of S1. What is familiar is the ejection click of a bicuspid aortic valve. Perhaps less familiar but more frequent in a clinic setting is the ejection sound into the aorta in patients with disorders such as hypertension. A rare disorder with classic valuable findings is the entity of pulmonic valve stenosis, 7 where the behavior of the ejection click in early systole and its relation to respiration is pathognomonic for the disorder. These right-sided ejection sounds are found to coincide with the completion of pulmonary valvular opening, whereas the M1 and T1 components of S1 coincide with closure of the respective atrioventricular valves.1 –3
Closely coupled ejection clicks and atrial gallops can amplify and expand the duration of the first heart sound.
Ejection Clicks
It is important to note the location on the chest where the S1 is best heard and the point of being most audible. Normally, S1 is best heard in the mitral area at the left ventricular apex, where it is possible to palpate the left ventricular impulse. Sonographers often use this point to place their transducer and obtain the apical images from that point. However, in the case that the S1 is more audible at the upper right sternal border, there may be an early systolic ejection click closely coupled to the first heart sound that is contributing to the increased loudness (See Figure 7). For the sonographer, this means looking for a bicuspid aortic valve, and for a dilated aorta.2,8,9
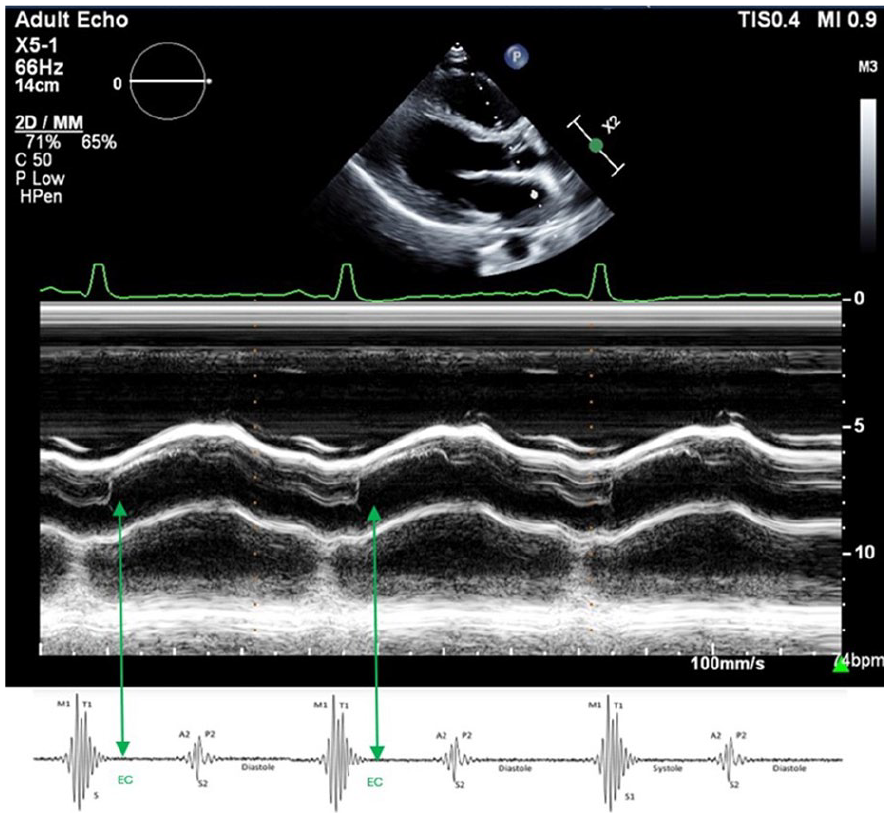
This example demonstrates the timing of the ejection click (EC), which is typically heard right after the first heart sound (S1). This can be mistaken for a loud S1 when it merges with S1.
Atrial Gallops
The bell of the stethoscope is meant to be pushed into the chest and then gently pulled back while maintaining a seal that excludes room noise. When the bell is placed in the mitral area for auscultation, the listener should be paying attention to the loudness of the S1 while pushing in and subsequently pulling back the bell. If the S1 is more audible with a light stethoscope bell pressure, there may be an atrial gallop closely coupled with the S1.
The fourth heart sound (S4) or atrial gallop occurs after the late diastolic reopening of the mitral valve because of atrial contraction 2 causing a disproportionate rise in left ventricular end diastolic pressure. Atrial gallops are found in older patients, hypertensive patients, and patients with left ventricular hypertrophy on echocardiography and on ECG. On M-mode echocardiography, S4 is closely related to the “A” point of mitral valve motion 2 (See Figure 8), right before S1.
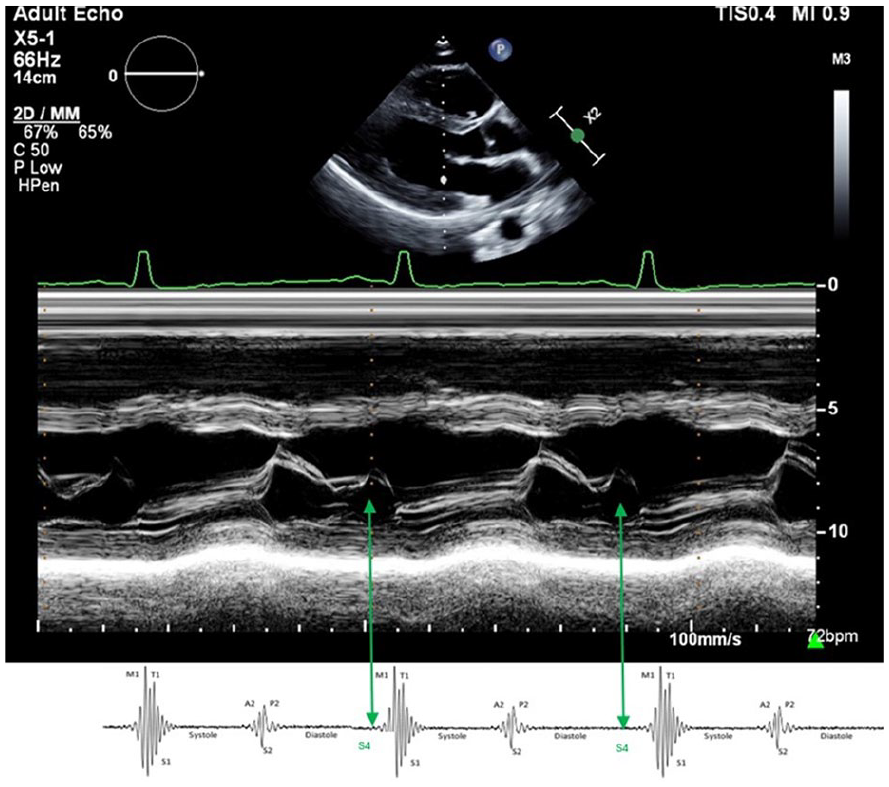
Demonstration of the relationship between the fourth heart sound (S4) and the “A” point on M-mode at the mitral valve level (indicated by green arrows). S4, which coincides with atrial contraction (A point on M-mode), occurs just before the first heart sound (S1) and may be mistaken for a loud S1 when the two are closely spaced.
Bundle Branch Block
When it comes to right and LBBB, things are not necessarily intuitive from one to the other. It is agreed upon and clinically important that patients with right bundle branch block (RBBB) exhibit abnormal first heart sounds with abnormal splitting. 10 Since electrical impulses are conducted normally through the LBBB, left ventricular contraction occurs slightly earlier than right ventricular contraction, where conduction is relatively delayed. This delay in right ventricular activation leads to later closure of the tricuspid valve, resulting in a split S1, with separate audible mitral and tricuspid components. Split S1 is best heard at the apex or along the lower left sternal border.
Conversely, the LBBB is still puzzling and does not follow the opposite rule of the RBBB. For the cardiac sonographer, the importance of the LBBB is that, in addition to the electrical abnormality, the sonographer is also expected to recognize the fact that the presence of an electronic pacer effectively results in an LBBB with all its associated consequences for the heart sounds.
The fascinating finding of an LBBB is that it does not affect splitting of the S1, but rather it affects the loudness. 11 The intensity of S1 may decrease when there is an LBBB.
S1 and Myocarditis
Myocarditis is a rare complication in certain oncology and rheumatological patients. Cancer patients being treated with immune checkpoint inhibitors can develop myocarditis. Scleroderma patients may also develop myocarditis in the course of their disease. Myocarditis is potentially lethal and needs to be recognized for prompt treatment.
It is said that echocardiography is the front-line tool for the diagnosis of myocarditis and needs to be followed by other diagnostic testing, such as cardiac magnetic resonance imaging and endomyocardial biopsy. However, these patients may be followed on a regular basis for a long time. The use of serial echocardiograms may be impractical.
An auscultatory finding on a routine follow-up visit in these patients may be the fact that the intensity of the S1 has decreased when compared with prior visits. Cardiac symptoms and signs lack specificity to diagnose myocarditis, due to the diversity of clinical presentations. However, a combination of new cardiac symptoms with elevated cardiac enzymes and perhaps the decreased intensity of the S1 may then prompt a referral for an echocardiogram. Thus, the S1 can serve as a valuable clue in the early diagnosis of myocarditis 12 and could play a key role in the clinical follow-up of such patients.
Further Exploration
As an introduction to the S1, only the first heart sound and related components are described. However, further exploration of echocardiographic correlation with the different heart sounds, especially the second heart sound (S2) and its components will enable cardiac sonographers to have an even better understanding of many diseases.
Recent studies have explored ways to improve the diagnostic accuracy of heart sounds by integrating auscultatory findings with echocardiographic analysis. Zhao et al 13 published an article that introduced the inclusion of a heart sound diagnosis with echocardiography reports (HSDreport). In their work, they suggested that the indirect use of heart sounds from auscultation, as part of the echocardiography reports, assists in the prediction of pediatric congenital heart disease. As part of their study, researchers introduced a new dataset using advanced machine learning models that integrated heart sounds with comprehensive echocardiographic information and enhanced the reliability of the heart sound diagnosis. They demonstrated the feasibility of using heart sounds to infer information from echocardiography. 13
Conclusion
Knowledge of auscultatory findings and their correlation to the different echocardiographic sets of information could help to improve sonographer’s understanding of many disease conditions. This includes valvular heart diseases, bundle branch blocks, and myocarditis. The characteristics and variations noted should be interpreted after correlating with other clinical findings. It is also important to know the 12-lead ECG to have a good understanding of cardiac events. These are some of the key skills that will help enhance the diagnostic confidence of a cardiac sonographer and prompt them to explore in the right direction while performing the studies.
Footnotes
Acknowledgements
I thank Dr. Daniel Shindler, Professor of Medicine, Robert Wood Johnson Medical School for his valuable support and guidance during the development and review of this article.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
