Abstract
Objective:
The purpose of this study was to determine the quality and effectiveness of a structured, competency milestone-based pediatric sonographer onboarding program and continuing educational curriculum and to ascertain if these experiences influence their professional development, job satisfaction, and retention.
Materials and Methods:
A survey was distributed to the sonographers in a single echocardiography laboratory. The anonymized data were collected and analyzed to generate descriptive statistics.
Results:
There were 36 sonographers who responded (80%) and 15 (42%) training with the new onboarding curriculum. The majority reported a positive feeling of preparedness for independent practices (80%) with hands-on teaching, timely feedback, and case-based learning rated as the most effective teaching methods. Physician feedback was preferred over sonographer trainer feedback. Most sonographers perceived the advancement of their knowledge as important for professional growth, job satisfaction, and retention.
Conclusion:
A structured onboarding program for new hires based on competency milestones was effective in preparing pediatric cardiac sonographers for independent practice. Hands-on bedside training, timely constructive feedback, and case-based learning should be included in the curriculum to ensure high-quality teaching. Physician engagement is highly valued and should be incorporated into the workflow. This study may suggest that continuing education helps positively influence the sonographer’s attitudes toward professional development, job satisfaction, and retention.
Transthoracic echocardiography is the mainstay of diagnosis and surveillance for pediatric congenital heart disease and requires a high level of technical and interpretive expertise by the performing sonographer. 1 The technical aspect involves the procedural skills for performing the echocardiogram and obtaining all the relevant images. The interpretive expertise includes understanding the relevant anatomy and physiology and being able to combine this information with the images obtained to deduce clinically relevant findings. This combination of skills requires specialized training and continuous education and is essential to maximize diagnostic accuracy and reduce the risk of adverse outcomes.2,3 In addition to the challenges of mastering a complex skillset, the sonographer workforce is under added pressure, due to chronic staff shortages and work-related musculoskeletal injuries, resulting in higher attrition rates than other allied healthcare professions.4 –6
The diagnostic medical sonographer had its origin in the 1960s, around the inception of clinical echocardiography. Despite this, there is great variability in the education and training of sonographers. Echocardiographic education has drastically changed in the last few decades from textbooks with still images to live multimedia resources. The American Society of Echocardiography has released guidelines for the education of the cardiac sonographer; however, no widely accepted standardized educational curriculum exists for pediatric cardiac sonographer training and ongoing education beyond graduation from a sonography program.7,8 A growing body of literature demonstrates the benefit of a blended approach for education utilizing web-based modules coupled with classroom activities and hands-on simulation. This combination promotes the retention of knowledge, the development of an individual’s cognitive and psychomotor skills, and mastery of the pediatric echocardiogram in a low-risk environment.9 –15
There is a considerable gap in the literature addressing the education of the cardiac sonographer. Recently, the echocardiography laboratory at Texas Children’s Hospital developed a structured new hire onboarding program and comprehensive, yet diverse continuing education curriculum, to improve competency and prepare sonographers for independent practice. Texas Children’s Hospital is a tertiary care pediatric facility with the echocardiography laboratory providing services for the main medical center, as well as several regional practices. The purpose of this study was to ascertain the quality and effectiveness of a new structured, competency milestone-based new hire onboarding program and continuing educational curriculum. Additionally, it was important to determine if these experiences influence the sonographer’s professional development, job satisfaction, and retention.
Materials and Methods
Onboarding Program
The new hire onboarding program utilizes competency-based performance development (CBPD) to provide clear expectations of the cognitive, interpersonal, and technical skills required for the new sonographer to function successfully and independently in their role following orientation. The program consists of three phases of increasing complexity coupled with frequent assessment and feedback (See Figure 1).
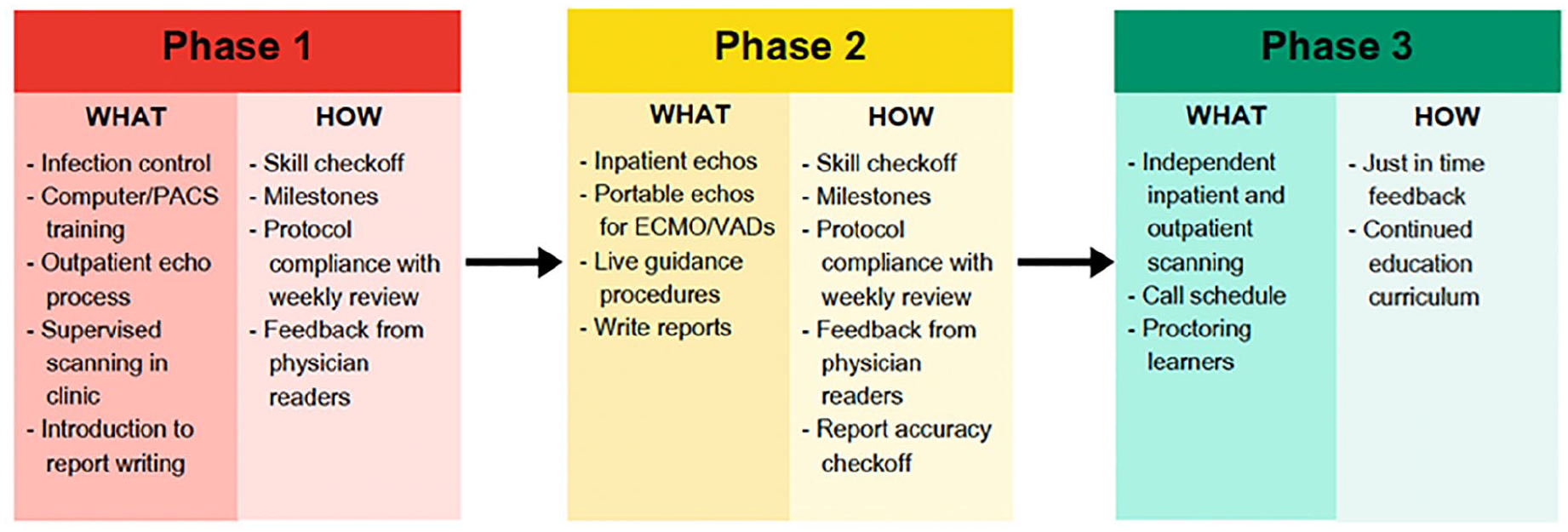
This diagram provides an overview of the new hire onboarding program that consists of three phases of increasing complexity, coupled with frequent assessment and feedback.
Phase 1 typically spans 3–6 months and encompasses essential centralized onboarding requirements, alongside initial scanning and reporting training. The lead sonographer educator conducts regular once-weekly check-ins for skill assessments and milestone evaluations. Phase 1 skills include demonstrating proficient transducer and equipment selection, mastering standard imaging views, accurately identifying intracardiac anatomy, and conducting echocardiographic testing. This included two-dimensional and M-mode imaging, as well as color and spectral Doppler. An example of a Phase 1 milestone involves successfully performing a complete normal cardiac echo and generating a report within a 1-hour timeframe.
Phase 2 lasts approximately 3 months and delves into more complex scanning of cardiac disease both within the laboratory and throughout the hospital. During this phase, the trainees must document anomalies encountered during their examination, to ensure exposure to a variety of congenital heart disease. This would include but not limited to tetralogy of Fallot, atrioventricular septal defect, transposition of the great arteries, hypoplastic left heart syndrome, truncus arteriosus, tricuspid atresia, pulmonary atresia, and coarctation of the aorta. In addition to frequent check-ins every third week with the lead sonographer educator with respect to Phase 2 skills, such as navigating throughout the hospital campus and recognizing pathological changes in cardiac anatomy. Additionally, the reading physician also provides real-time feedback on the technical quality and interpretation of the studies. A Phase 2 milestone consists of comparing 25 preliminary reports to the final report to identify discrepancies. The goal is to achieve < 10% major discrepancies, with major discrepancy defined as two or more degrees of change (e.g., mild regurgitation being reported as severe regurgitation, or a small ventricular septal defect being graded as a large defect). At the end of Phase 2, a comprehensive assessment is performed to evaluate the trainee’s readiness for independent performance by incorporating feedback from the physician readers, lead sonographers, and self-reported competency and comfort level by the trainee.
The final phase, Phase 3, facilitates the transition of the sonographer into a full-time role with independent inpatient and outpatient scanning responsibilities, participation in the call schedule, and mentoring of other learners. Phase 3 offers continual learning opportunities with “just in time” feedback and integration of the structured continuing education curriculum.
Continuing Education
The continuing education curriculum incorporates a variety of learning methodologies to accommodate a diverse group of learners (See Figure 2). Bedside teaching and “just in time” feedback encourage timely instruction while prioritizing patient-centered care. These methods allow for a hands-on experience and individualization of the curriculum to meet the needs of the sonographer.
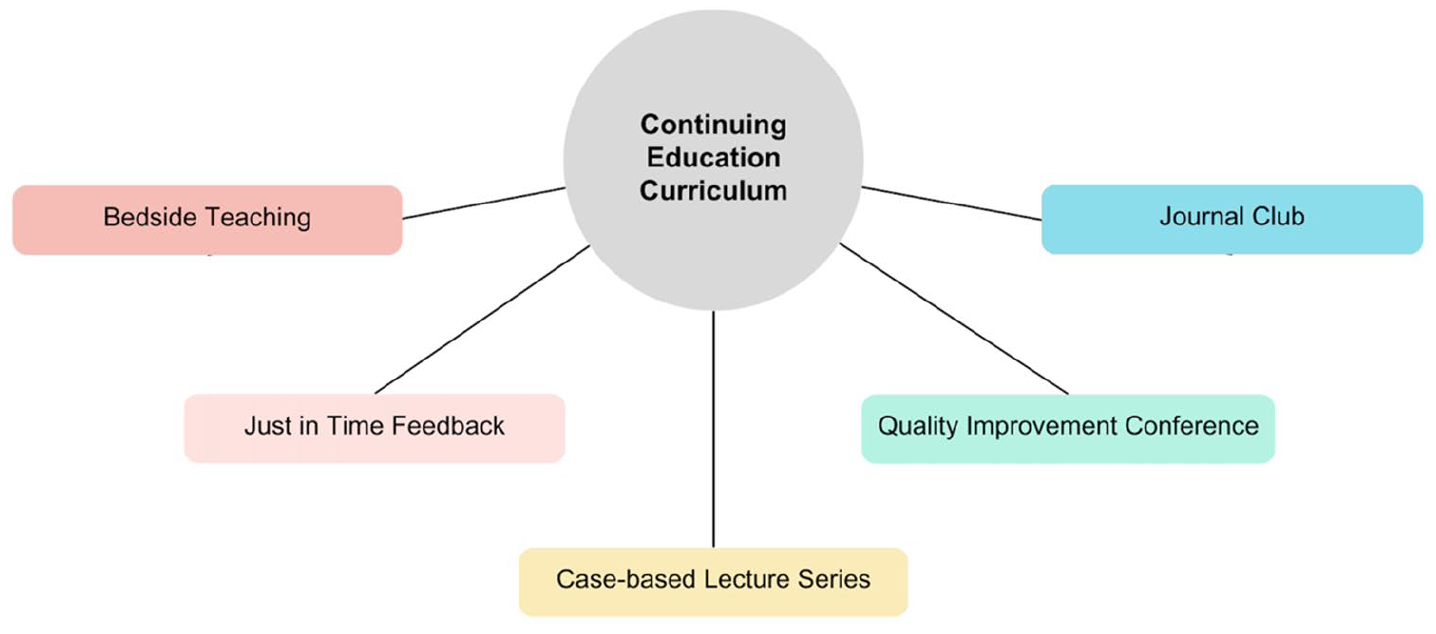
This diagram provides an overview of continuing education curriculum incorporating a variety of learning methodologies to accommodate a diverse group of learners.
Group education included a weekly case-based lecture series that focuses on a patient case to encourage a review of echo images that illustrate the best techniques and interpretation while applying this information to relevant real-life scenarios. This program feature promotes the development of their analytic, communicative, and collaborative skills while advancing content knowledge.
In addition, a quarterly quality improvement case review was incorporated to evaluate technical and interpretive errors and promote collective and collaborative learning, as well as, a journal club that promotes critical appraisal of new literature, while advancing evidence-based practices.
Conduct of Study
A cross-sectional online survey was designed to investigate the new onboarding training program and continuing education curriculum. An 18-question survey was created and distributed with study data collected and managed using REDCap (hosted at Texas Children’s Hospital) electronic data capture tools managed at Texas Children’s Hospital.16,17 The survey invitation was deployed via email to all the cardiac sonographers at Texas Children’s Hospital Heart Center and remained open for 2 weeks. There were no incentives offered for participating in the study. The survey was reviewed by experienced sonographers and physicians prior to its use. The survey consisted of both multiple-choice rating questions utilizing the Likert scale and free-text answer questions designed to meet the objectives above. The effectiveness of onboarding was evaluated by sonographers ranking the methods of training that best prepared them for independent practice following the completion of training. The effectiveness of the curriculum was evaluated by sonographers ranking the methods that best contributed to an advancement in their learning. All data collected was anonymous. This study was considered a quality improvement project therefore, it was considered exempt from internal review and approval.
Statistical Analysis
Descriptive statistics were used to summarize the trainee characteristics, training duration, and sonographer responses for this study.
Results
Of 45 sonographers in the laboratory, 36 completed survey responses were received (80%). Many respondents have been practicing cardiac sonography for more than 5 years (25/36, 70%). Fifteen sonographers (42%) trained with the new onboarding curriculum with most of those sonographers rating their training duration as appropriate (87%), with a positive feeling of preparedness for independent practice afterward (20% very prepared, 60% prepared). The frequency (81% just right) and quality (36% excellent, 44% good) of continuing education were rated positively (See Figure 3). Figure 4 depicts the rating of effectiveness of the various methodologies used for onboarding and education. Hands-on bedside teaching, timely constructive feedback, and case-based learning were rated as most effective. The participating sonographers also preferred physician teaching and feedback. Overall, most sonographers perceived that their knowledge base advanced because of access to multiple sources of educational training which they found important for their professional growth, job satisfaction, and job retention (See Figure 5). These sources included access to outside educational resources (society memberships and scientific conferences), training in new skills such as 3-D echo, and continuing education within the lab.
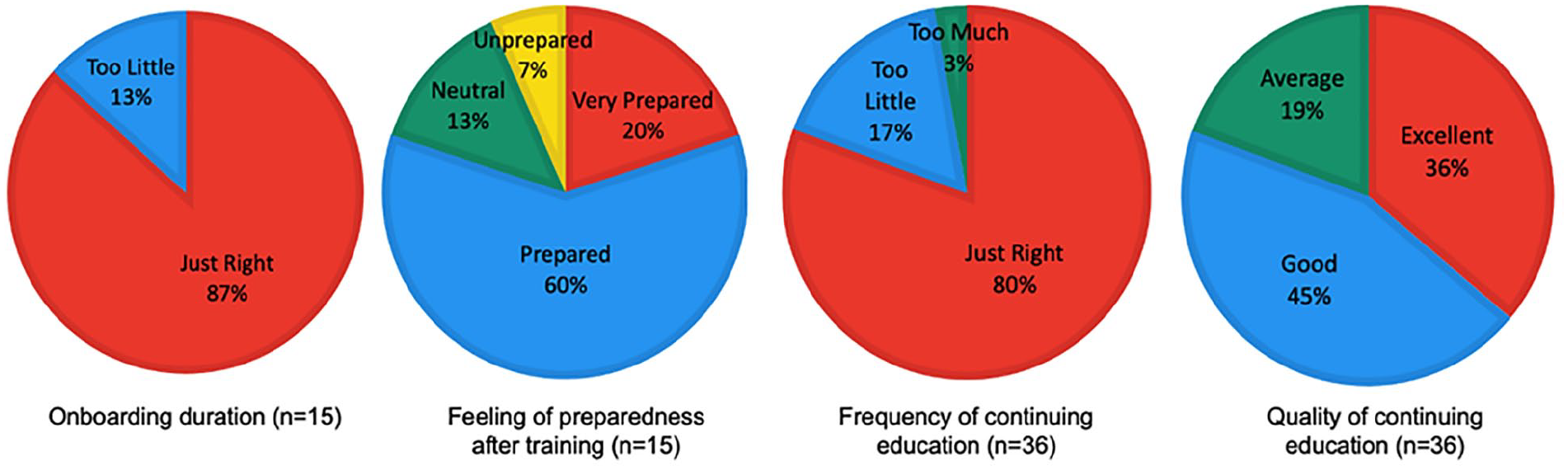
A pie chart is provided, which shows how sonographers rated onboarding duration (far left), feeling of preparedness, after onboarding training (middle left), frequency of continuing education (middle right), and quality of continuing education (far right).
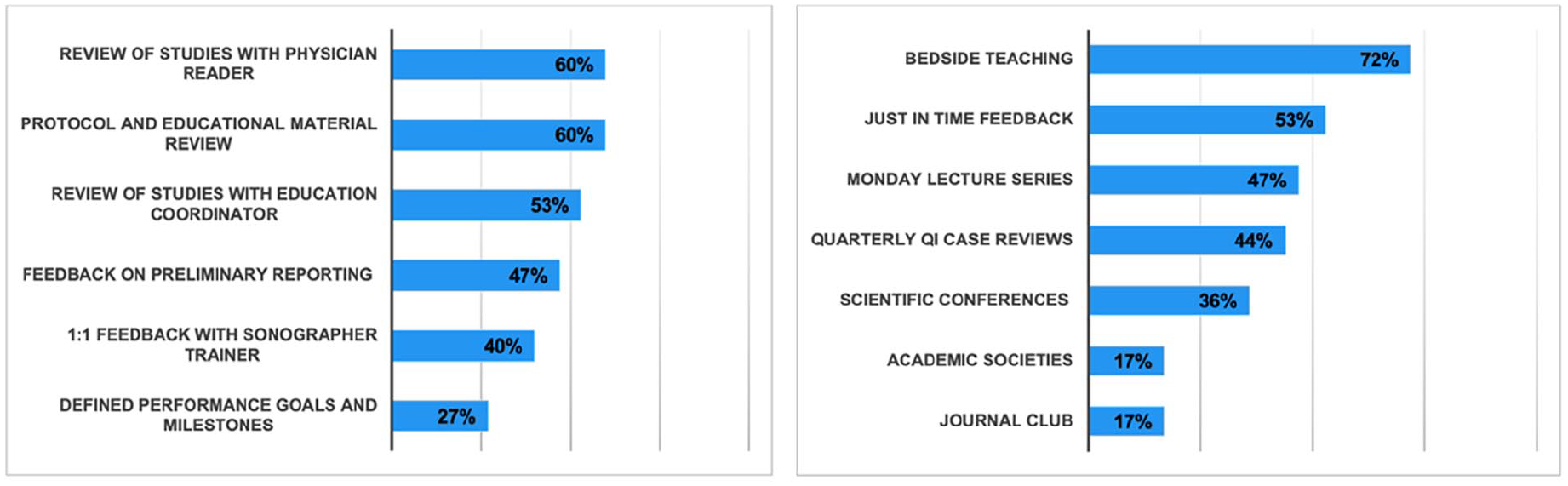
This bar chart indicates how sonographers perceived the most effective onboarding (left) and educational opportunities (right). The numbers represent the percentage of sonographers rating the method as most effective.
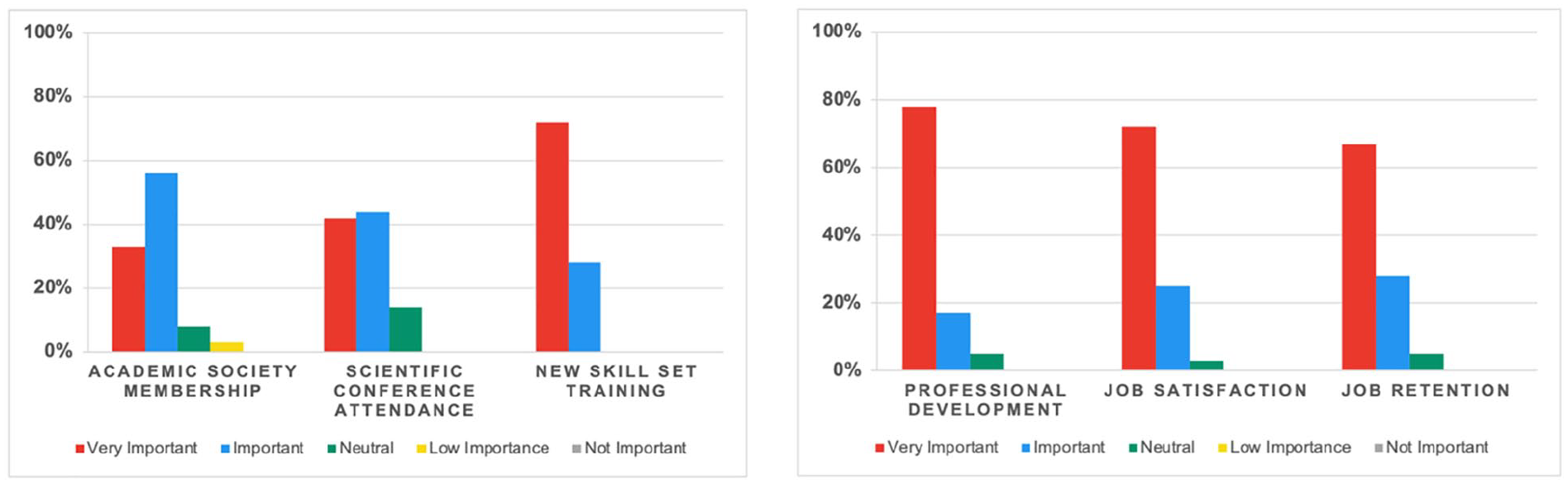
This bar chart indicated how sonographers rated the importance of access to education from external sources such as academic societies and journals, attending scientific conferences, and exposure to new skills for the advancement of knowledge (left). An additional bar chart provides how sonographers perceived the importance of education in their professional development, job satisfaction, and retention (right).
Discussion
The field of cardiac sonography is constantly evolving with increased demand for educated and well-trained sonographers to be able to perform the two-core skill sets of procedural technique and interpretive skill. This role is crucial in pediatric cardiology, where the echocardiogram remains the predominant modality used for the diagnosis and follow-up of congenital heart disease. Furthermore, the diverse anatomy, physiology, and complexity of congenital heart disease and consequently the palliative strategies demand a significant breadth and depth of the sonographer’s knowledge base. Sonographer education has evolved from primarily “on-the-job training” to formal education through a sonography educational program. However, further efforts are still needed in areas lacking such as standardized onboarding and continuing education, following graduation. New pediatric cardiac sonographers are required to negotiate a steep learning curve on the job as they are exposed to various pathology and surgical repairs. This is particularly evident in tertiary care centers where the patient population is most complex. To be successful, as a pediatric sonographer, it is important to stress continued on-the-job learning and training.
Education in echocardiography integrates theoretical understanding with practical application. This program aligns with the current evidence advocating for a blended approach to cater to a diverse group of learners.13,14 Traditional educational techniques, particularly beneficial for grasping ultrasound physics and cardiac anatomy, establish a robust foundation. This approach proves most effective for introducing trainees to fundamental concepts at the onset of the onboarding process, facilitating the formation of their knowledge base. Hands-on simulations, workshops, and bedside instruction offer realistic and valuable avenues for trainees to augment their skills and cultivate confidence within a secure environment.10,11 Such experiential learning proves indispensable for trainees, as they progress toward autonomy. This starts as part of their onboarding and continues as they refine their abilities and continue their professional journey. Drawing from the findings in this study, the inclusion of hands-on bedside training, timely constructive feedback, and case-based learning in cardiac sonography proved to ensure the delivery of high-quality education. While overall being receptive to the different methodologies of this educational curriculum, the survey responses highlighted a few logistical areas for improvement that could further bridge the gaps in attendance and participation. These included avoiding educational sessions on Monday, due to the higher volume of studies in the lab, reserving an hour over lunch for case discussions, and expanding in-person educational offerings for the satellite locations.
In response to the evolving and demanding educational landscape, numerous health professions have embraced active learning through peer-assisted learning, as supplementary approaches alongside faculty/expert-led methods. Peer-assisted learning capitalizes on cognitive and social congruence, fostering a shared knowledge base and the ability to articulate concepts in ways that resonate with peers. 18 Particularly beneficial at the onset of a program, such approaches help navigate the transitional challenges associated with assuming new role responsibilities. Zhang et al 19 and Aquino et al 20 evaluated peer versus faculty-led learning methods and highlighted the effectiveness and positive impact of integrating peer-assisted learning strategies, alongside faculty-led learning into the medical education curriculum. Based on these findings and the experiences within the current study’s curriculum, it would seem that the two strategies should be used in a complementary fashion to promote well-rounded education of the pediatric sonographer. Physician engagement in teaching is highly valuable and should be incorporated into the workflow and staffing plan. Physician faculty may be better able to provide education on the clinical correlation of the echo data with other imaging techniques, as well as contextualize procedural decision-making and patient outcomes. To further emphasize the importance of physician involvement, the most common survey feedback that was received from the participating sonographers was to incorporate a physician interpreter, as a point person for education, that can address questions, provide feedback on image quality, identify areas for improvement, and explain the essential images required. This was expressed in order to properly address the clinical question stated and integrate this when examining various pathologies. However, to address some of the challenges hindering faculty engagement in the workflow, it was important to recognize the practicality and value of peer-assisted learning, as well as endorse its incorporation, as a key educational strategy.
To maintain and enhance their professional proficiency, healthcare professionals must partake in continuing education and training. Employees who actively engage in skill development or training are more inclined to remain in their current positions compared with those who do not. 21 In addition to fostering role commitment and job satisfaction, continuing professional education enriches the employee’s knowledge, skills, confidence, and sense of coherence, thereby increasing employee retention.21,22 For new employees, particularly inexperienced sonographers, pairing them with a mentor can also have a profound impact on retention. While existing studies primarily focus on other healthcare professionals such as nurses, research specific to sonographers suggests similar findings, highlighting the positive influence of continuing education and skill acquisition on attitudes toward professional development, job satisfaction, and retention.
The findings of this study are impactful in suggesting that the implementation of a structured onboarding process and continuing education with physician participation are worth the investment of resources for the professional advancement and satisfaction of our sonographers. This is particularly relevant given the high rate of attrition among sonography professionals and projected workforce shortages for the foreseeable future. 23
Limitations
It is important to acknowledge the limitations in this quality improvement study, including single-center evaluation, a small number of sonographers, and the subjective nature of the survey. The future success of this institution’s onboarding and continuing education process will be measured by tracking sonographer advancement, academic participation, and retention.
Conclusion
A structured onboarding program for new hires, based on graded achievement of competency milestones, was effective in preparing pediatric cardiac sonographers for independent practice. Hands-on bedside training, timely constructive feedback, and case-based learning should be included in the curriculum to ensure high-quality teaching. Physician engagement is highly valued and should be incorporated into the workflow. This study also suggests that continuing education and learning new skills help positively influence the sonographer’s attitudes toward professional development, job satisfaction, and retention.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval was not sought for the present study because ethical approval was not required per institutional policy.
Informed Consent
Informed consent was not sought for the present study because no patient data were collected, survey participation was voluntary, and responses were anonymous. It was also deemed a quality improvement activity and therefore exempt from review.
Animal Welfare
Guidelines for humane animal treatment did not apply to the present study because no animals were used during the study.
Trial Registration
Not applicable.
