Abstract
Objective:
The purpose of this mixed-methods study was to gather benchmark data on curricular content related to imaging of transgender patients. In addition, the intent was to explore program directors’ opinions on the need to include this content in the curriculum.
Material and Methods:
An online survey was emailed to all directors (n = 982) of accredited imaging programs in the United States.
Results:
In total, 331 (34%) program directors participated in the survey. Fifty-six percent currently do not include this content in their curriculum and 67% reported no discussion of adding the material. There was a modest and significant positive correlation between the program directors’ perceived level of knowledge, regarding imaging transgender patients, and their perceived importance of including this material in the curriculum (r = 0.370; P < .001). Positive (55%), negative (7%), and neutral themes (38%) emerged from the qualitative data analysis.
Conclusion:
These findings were consistent with literature regarding a lack of curriculum specific to transgender patients. Program directors recognized the need to include this content, although barriers exist related to readiness to implement, limited faculty knowledge with the material, and lack of educational resources. Program directors are seeking strategies and resources to guide the integration of this material into the curriculum.
Keywords
The term transgender refers to people whose identity does not agree with cultural expectations related to the sex they were assigned, at birth.1,2 Approximately 1.6 million (0.6%) adults in the United States identify as transgender. 2 As the transgender community continues to grow, the need for appropriate education for medical imaging and radiation therapists becomes more critical to reduce disparities in treatment and access to care. 3 A lack of transgender information in health care professional curricula has also become more apparent.4,5
The health care professional community has a mandate to ensure cultural competence and patient-centered care.4,6 Data from the National Transgender Discrimination Survey in 2014 found 48% of transgender adults have delayed or avoided medical care. This compared with 29% of lesbian, gay, and bisexual adults, as well as 17% of heterosexual adults who delayed or avoided care. 7 Most often, these patients cite costs, fear of discrimination, and previous negative experiences with health care providers as reasons for delays.1,7
Aside from mandates to offer culturally competent care, there is a need to improve health care access and experiences for transgender patients. A health professionals educational program is the foundation upon which this type of education begins. 8 Maley and Gross 5 stated that exposure to lesbian, gay, bisexual, and transgender (LGBT) health issues, through both didactic and clinical education, is a significant method for affecting students’ knowledge, attitudes, and behaviors. To prepare students to provide quality care for these patients, it is important for a health professional’s educational program to include topics related to the needs of transgender patients.
Literature Review
Multiple databases (EBSCOhost, Medline, CINAHL, PsycINFO, and EMBASE) were searched to identify relevant literature on transgender issues in imaging, radiography, sonography, and radiation therapy education. More than 80 articles were sorted by relevance, with the preliminary research focused on those more relevant to this study’s search and purpose. A review of the literature noted the importance of faculty education in terms of curricular revisions. Few of the studies evaluated or discussed specific methods for preparing faculty.
Studies documented instructional approaches, within medical education, which were tailored to prepare students to care for diverse populations, such as transgender patients. Clark et al. 9 noted the need to evaluate transgender-related curricula based on the type of curricular opportunities being offered, student perspectives, and educator preparedness. Curriculum opportunities such as health fairs, community partnerships, presentations, and panel discussions are a few examples of the documented instructional approaches in the literature.3,8–10 In other cases, students were provided this content, primarily in clinical rotations.11,12 While this method can improve learning through actual experience, it is often inconsistent. When exploring student perspectives, possible topics include awareness of transgender students enrolled in the program and how to better meet their needs, student comfort levels in caring for their future patients, and student feedback on the transgender curriculum at their institution. Surveys of medical schools reported that only five hours of instructional content was dedicated to LGBT needs over the four-year curriculum. 13
Fewer studies have addressed faculty preparedness. Maley and Gross 5 reported on previous studies of faculty. In one study, 72% of nursing faculty did not feel prepared to teach LGBT content; another study revealed 62% of nursing faculty had never taught content related to LGBT topics. Lim et al. 8 identified perceived barriers to integrating LGBT health topics into the curriculum. These barriers included limited time in curriculum, limited guidance on how to integrate LGBT topics, and limited knowledge among faculty on health-related topics for these patients.
In 2011, Obedin-Maliver et al. 13 reported on the total hours of LGBT-related content in US and Canadian medical schools. On average, five combined hours were allowed to address these health care topics. Still, the number of required hours in medical schools dedicated to LGBT patients varied widely. Further, the authors found most (66.7%) of preclinical content, related to the LGBT health, was interspersed throughout the curriculum; only 24.2% of schools responding had dedicated modules for LGBT content. Mandap et al. 11 evaluated curriculum in pharmacy schools for educational content regarding the LGBT community. They found only 18% of schools were preparing faculty to teach LGBT content and recommended the development of strategies and resources to assist faculty and curriculum committees to teach LGBT content.
Medical school content, reviewed by Obedin-Maliver et al., 13 consisted primarily of lectures or small groups addressing LGBT content in the clinical setting. According to Brennan et al., 14 several strategies could help to improve students’ mastery of lesbian, gay, transgender, and queer/questioning (LGBTQ+) topics. These include classroom LGBT patient panels that address interactions with health care personnel and potential scenarios. In addition, they suggested group projects or written papers that discuss personal experiences along with exercises to clarify students’ beliefs. 14 These can also include case studies aimed at meeting specific mental and physical health needs of LGBT patients and simulation exercises to address barriers to LGBT care and their health concerns. 14
Some studies in health care education have reported unwillingness, inability, or even bias on the part of faculty concerning transgender topics.8,15 Educator preparedness often begins with an evaluation of educator knowledge, as well as experience with and readiness to teach transgender health issues. It is important to also consider the current state of the curriculum regarding transgender topics and how to most effectively incorporate this information into the curriculum.
The purpose of this study was to gather benchmark data on curricular content related to imaging of transgender patients from accredited medical imaging and therapeutic science (MITS) programs in the United States. The study also explored the opinions of program directors concerning the need to include medical imaging of transgender patients in the curriculum and how to prepare faculty.
Materials and Methods
This mixed-methods research was conducted by medical imaging and therapeutic science faculty at a midwestern academic health sciences’ center. A literature search as well as a survey instrument gathered data on program directors’ current curricula related to transgender patients, attitudes toward inclusion of curriculum related to imaging of transgender patients, and methods for training faculty on transgender topics. An institutional review board (IRB) approval was granted (IRB 136-19-EX).
Participants
The study population included MITS program directors from the United States and accredited by the Joint Review Committee on Education in Radiologic Technology (JRCERT) for radiography, magnetic resonance imaging (MRI), nuclear medicine, and radiation therapy education. In addition, responses were gathered from sonography program directors accredited by the Commission on Accreditation of Allied Health Programs (CAAHEP). Geographical information was collected using the four statistical regions outlined by the US Census Bureau (see Figure 1). 16
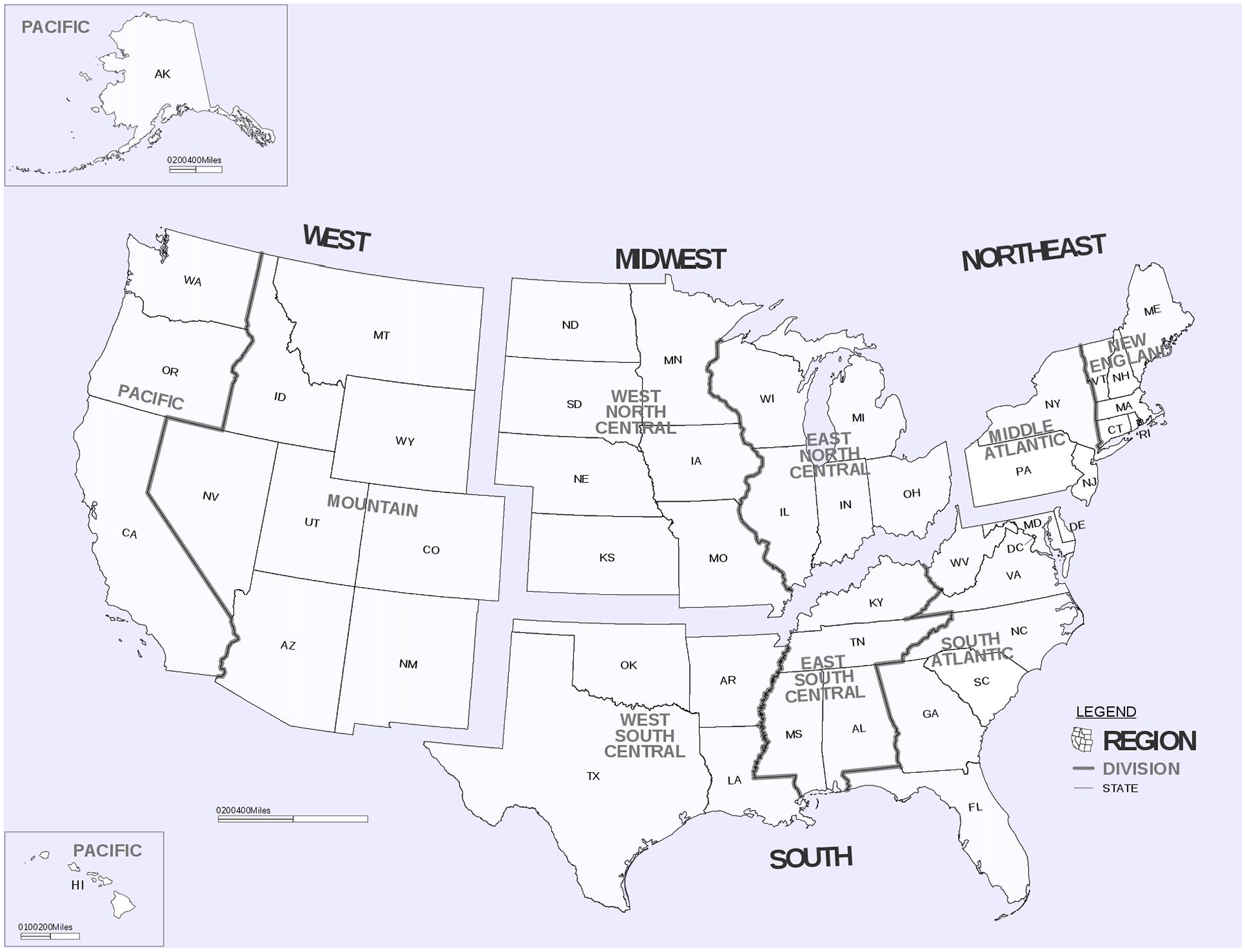
Census regions and divisions of the United States.
Survey Instrument
A total of 982 program directors of JRCERT- and CAAHEP-accredited programs received invitations to participate by email and a link to a RedCap Survey. The survey instrument was a modified version of the one by Lim et al., 8 which was originally designed to assess nursing faculty knowledge, experience, and readiness to teach LGBT health in baccalaureate nursing programs. Lim et al. 8 granted permission to modify and use the survey to meet the needs of the current study. The faculty co-chairs of a campus LGBTQ+ employee alliance group piloted the survey for accuracy and understanding. Edits were made to clarify wording and improve the order of questions. The 32- to 35-question survey (depending on skip patterns) included multiple-choice, short-answer, and rating questions.
The first two questions gathered information regarding type of imaging program(s) directed by the respondent. The third question asked, “Does your program curriculum currently cover topics related to medical imaging of transgender patients?” From there, a skip pattern separated programs currently covering topics related to medical imaging of transgender patients from those reporting not covering the topic. Directors responding “yes” were asked 32 additional questions, those responding “no” were asked 31 additional questions, and those responding “I do not know” were asked 30 additional questions. These questions gathered information on the importance of adding transgender topics in the curriculum, the readiness of programs to add this information, and teaching strategies used when adding transgender topics to the curriculum.
Data Collection and Analysis
Surveys submitted with a least one page of the survey completed were included in the results. The data were analyzed following American Association for Public Opinion Research guidelines for counting partial interviews as respondents. 17 Survey data were quantified initially using appropriate descriptive statistics with frequencies and percentages for categorical responses, as well as means and standard deviations for continuous response measures. Program directors who oversee more than one imaging program were asked to identify the largest program they direct. Further responses from these individuals were classified under their largest program during all analyses conducted by program type.
Tests for associations between continuous measures were conducted using Pearson correlation coefficients, and tests for association between categorical response variables were performed with either Pearson chi-square tests or Fisher exact tests. Differences on continuous outcome measures between pairs of respondent groups were tested with t tests, and differences across three or more groups were assessed with analysis of variance (ANOVA) models. All analyses were conducted using STATA v16.0 (StataCorp, College Station, TX). Qualitative data were collected with the final survey question. The results were compiled and reviewed following Creswell’s qualitative analysis procedure. This involved the organization of the data, a preliminary read-through, coding and organizing of themes, data representation, and interpretation. 18
Results
Of the 982 survey invitations sent, 14 email messages were returned as undeliverable, 630 directors did not respond, and 7 surveys were submitted as incomplete. This provided a response rate of 34% (n = 331). As respondents progressed through the survey, a total of 26 respondents did not advance to page 2 (n = 305) and an additional 10 participants did not progress to the third and final page of the survey (n = 295).
Fifty-six percent (n = 184/331) of the program directors responding currently do not include topics related to medical imaging of transgender patients; 41% (n = 137/331) include this information in the curriculum, and 3% (n = 10/331) did not know whether transgender information is included. Of the programs that include content related to imaging of the transgender patient, 66% (n = 90/137) believe the content is sufficient to meet the needs of an entry-level medical professional, with a mean of 2.8 hours devoted to this content. Mean hours varied by program type, with radiation therapy programs reporting the highest number of hours (4.3) and nuclear medicine programs reporting the lowest number of hours (2.0) (see Table 1).
Inclusion of Transgender Content in Curriculum and Average Hours.
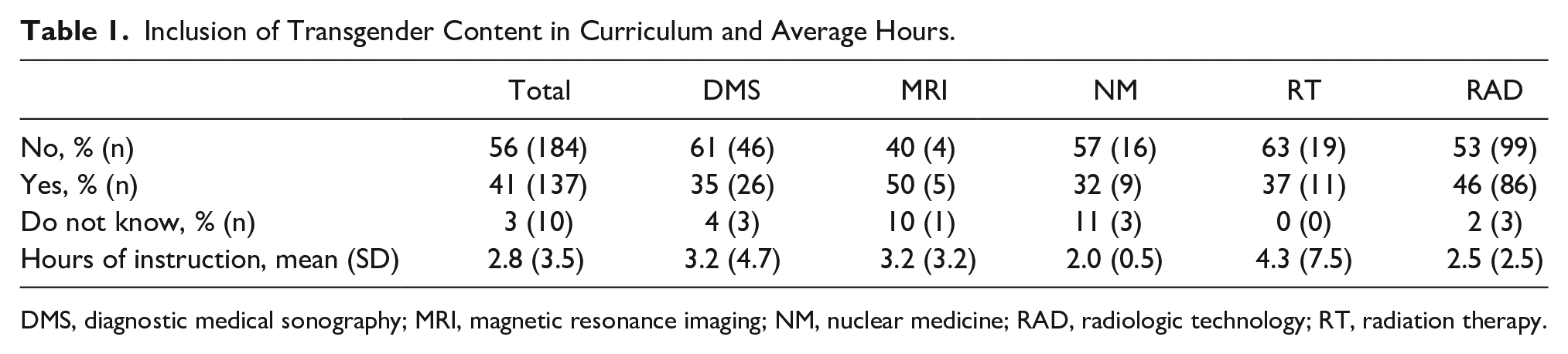
DMS, diagnostic medical sonography; MRI, magnetic resonance imaging; NM, nuclear medicine; RAD, radiologic technology; RT, radiation therapy.
Program directors rated their professional knowledge on transgender topics using a rating scale from 0 to 10, with 0 being “not at all important” and 10 being “critically important,” resulting in a mean (SD) of 5.0 (2.7). This rating was fairly consistent across geographic regions. There was a modest and significant positive correlation between the program directors’ perceived level of knowledge regarding imaging transgender patients and their perceived importance of including this material in the curriculum (r = 0.370; P < .001). Nearly 60% of program directors had cared for a transgender patient during their professional career, but no association was found between this experience and the perceived importance of including transgender imaging in the curriculum (P = .77).
Those program directors who currently do not include didactic material on transgender imaging reported various states of inclusion readiness. Sixty-seven percent (n = 123/183) reported no discussion of adding the material to the curriculum, 23% (n = 42/183) had discussed the content addition but had taken no action, 5% (n = 9/183) reported currently taking action but not ready to implement, and 5% (n = 9/183) would be including the material in the near future. Also, among those not including transgender imaging in their curriculum, 73% said it had not been mentioned during a departmental meeting in the past two years, 20% said it had been mentioned one or two times, and 7% reported it had been mentioned three times or more.
Most respondents stated in the past two years, they had not read articles regarding transgender care in a professional journal (52%, n = 172/331). Nor had most attended a presentation at a local/regional conference (75%, n = 249/331) or attended a presentation at a national conference (76%, n = 250/331) related to the medical imaging of transgender patients. The distribution of these “no” responses was highest in the South region for the categories of professional journal articles (64%) and presentations at local/regional conferences (88%). The number of “no” responses for learning about transgender topics through presentations at national conferences was highest in the Northeast region at 87%. Respondents from the Northeast region reported the highest percentage of positive responses for learning about transgender topics in journal articles (60%) and through local/regional conference presentations (31%). The West region contained the highest percentage of respondents who noted attendance at transgender-related presentations at a national conference (32%).
Program directors rated providing faculty development and training that incorporated transgender topics, using a rating scale from 0 to 10, with 0 being “not at all important” and 10 being “critically important.” The mean (SD) importance rating was 6.4 (3.2). Similar scales were used to rate the importance of individual strategies for developing faculty readiness. Review of accreditation requirements (6.7, SD = 3.2) and identification of curricular gaps (6.3, SD = 3.1) were rated the most important strategies in developing faculty readiness when this new material was added. Using transgender-specific clinical sites (4.2, SD = 3.2) and increasing the diversity of the faculty roster (4.1, SD = 3.1) were rated the lowest of importance (see Table 2).
Numerical Rating of Strategies for Faculty Development and Training Regarding Transgender Topics.

Respondents were asked to select the teaching strategies they had implemented to integrate topics on the medical imaging of transgender patients into their curriculum. Of the respondents with curricular content in place, the most common strategies listed were lectures (45%; n = 138/304) and clinical experiences (23%; n = 70/304). Other strategies, in decreasing order of use, included handouts, invited speakers, online resources, and case studies. Thirty-nine percent (n = 120/304) of those responding had no teaching strategies in place (see Table 3).
Implemented Strategies for Imaging of Transgender Patients Curriculum (n = 304). a
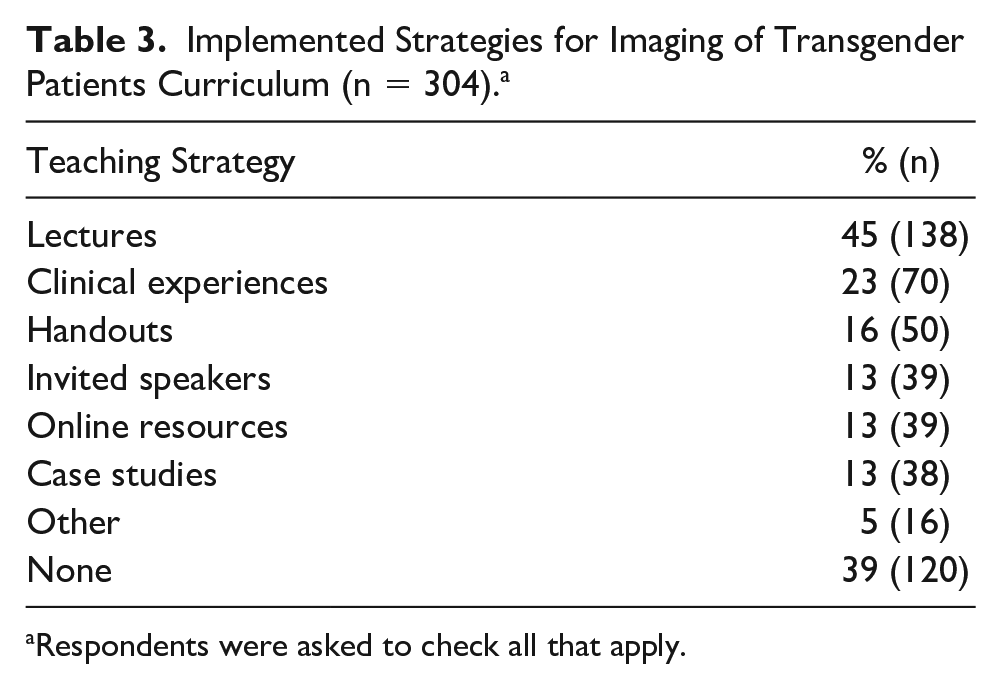
Respondents were asked to check all that apply.
The final page of the survey gathered demographic data. No significant association was found between the perceived importance of including transgender topics in the curriculum and the program director’s academic degree, age, race, sex, or directorship tenure. An association was noted between the perceived importance of including transgender topics in the curriculum and the program director’s academic rank. The results demonstrated that associate professors were highest (7.5), followed by other (7.0), assistant professors (6.9), instructors (6.1), and professors (5.8).
Directors from all four US census regions responded to the survey with 18% (n = 52) from the Northeast, 31% (n = 90) from the Midwest, 37% (n = 109) from the South, and 14% (n = 41) from the West. No significant association was noted between the region and whether transgender topics were incorporated into the curriculum. Likewise, there was no significant association between the perceived importance of including transgender topics in the curriculum by region or between region and how program directors rated the importance of transgender faculty development. An association was found between the region and whether transgender topics were being discussed in departmental meetings. This association was highest in the West at 54% and lowest in the South at 29%.
The final question on the survey allowed participants to include additional comments related to medical imaging of the transgender patient. Ninety of 295 (31%) participants shared comments on this final question. The comments were coded into three categories: positive (55%, n = 50/90), neutral (38%, n = 34/90), and negative (7%, n = 6/90). Themes emerging in the positive category included appreciation for addressing the topic, support for content inclusion in the curriculum, and requests for resources or information to enable faculty to begin including these topics in their curriculum. Neutral themes focused on the current topics taught in their curriculum; providing respectful, quality care for all patients; and the understanding that there is no need to treat anyone differently. Negative themes were few but included association with political views, past experiences, and disregard for the topic in general.
Discussion
This study is one of the first to provide benchmark data on the curricular content for imaging the transgender patient in JRCERT- and CAAHEP-accredited programs. Of the program directors responding, more than one half (56%) currently do not include topics related to medical imaging of transgender patients in their curriculum. This finding is consistent with the literature reported by other health care education programs.4,5,8,11 Although current transgender patient content is lacking in program curricula, some health professions educators recognized the need to address the issue.4,8,13 Still, this study found the integration of content on imaging transgender patients, which had not been discussed by 60% of respondents’ faculty department meetings in the past two years.
Program directors believed in the importance of incorporating imaging content related to transgender patients into their curricula, yet lacked knowledge and resources. The mean numerical rating for self-reported professional knowledge regarding the topic was 5.0. The mean rating was particularly low among MRI (2.3) and radiation therapy (3.9) program directors. This is in line with reports in the literature of limited health care faculty knowledge or opportunities for development.8,11 The low ratings for surveyed program directors could relate to the majority of them having little exposure to this topic through professional journals and local/regional/national conferences. This could be coupled with the fact that this curricular content is not being discussed at departmental meetings.
In regard to faculty preparedness to teach transgender-related imaging topics, 67% of respondents reported they have not had discussions regarding adding this content to their curriculum. In addition, 39% reported having implemented no strategy for integrating topics related to medical imaging of transgender patients into their curriculum. The literature regarding faculty readiness varies among professions. A survey of nursing faculty reported more than two-thirds felt unprepared to teach LGBT health content. 19 Lim et al. 8 reported 62% of nursing faculty had not taught this type of content. Educators in undergraduate medical education reported increased readiness, with 67% of faculty reporting they are willing and able to teach LGBT-related content. 13
Sixty-six percent of respondents who do include transgender topics in the curriculum believe the content is sufficient to meet the needs of an entry-level medical professional. The programs reported they spend an average of 2.8 hours devoted to this specific content. The literature notes an average of 5 hours dedicated to this type of content in medical schools, 13 2.12 hours in nursing schools, and 1 to 3 hours in pharmacy schools.8,11 In addition to these quantitative findings, voluntary comments noted that program directors were seeking guidance on how best to include imaging of transgender patients into their curriculum.
To provide initial guidance, it is important to evaluate the current strategies in place for teaching MITS students about transgender content. Program directors reported lectures (45%) were currently the most common strategy. Other strategies used in MITS programs include clinical experiences, followed by handouts, invited speakers, online resources, and case studies. Obedin-Maliver et al. 13 reported most LGBT content taught in medical schools was in the form of lectures or small groups in clinical settings. Few of the strategies, reported by these survey respondents, matched those that Brennan et al. 14 found to be helpful for students learning LGBT topics (e.g., classroom panel discussions, group projects, case studies, sharing personal experiences, and simulation exercises).
Nearly one-fourth of program directors relied on experiences in clinical rotations to educate students on transgender patient imaging, which could be problematic. Clinical experiences are an inconsistent teaching method, as encounters with transgender patients can vary across students’ clinical rotations. Teaching methods and approaches of clinical instructors versus established curriculum can also be inconsistent. As Lim et al. 8 reported, seamless integration requires competency-based clinical instruction and interprofessional collaboration. Likewise, use of invited speakers and online resources might be highly inconsistent based on individual research methods. Helping program directors and faculty members identify established resources could assist in their preparedness.
Faculty education is an important component to revising curricula to include topics related to medical imaging of transgender patients in the classroom. The importance of providing faculty development and training, related to incorporating transgender imaging topics, was rated 6.4 on a scale of 0 to 10 (e.g., 10 represented being critically important and 0 not at all important). Davy et al. 15 concluded nonhostile and open health care environments can be created for LGBT patients when content is dispersed across the curriculum for medical, health, and social care students by knowledgeable faculty. The authors also note a lack of time and resources and an unwillingness or inability of faculty to teach LGBT-related topics as barriers to including these topics in the curriculum. Training for health students at both undergraduate and postgraduate levels should address taking a proactive role, avoiding assumptions about patients’ sexual orientation, and applying the knowledge to health care practice. The authors suggest faculty use community-based learning and interprofessional training as strategies for incorporating these topics into the curriculum.
Limitations
Fifty-six percent of survey respondents reported they do not include transgender topics in their curricular content. These results could be high based on the population who found value in completing the survey. The result could also be underreported because program directors who do not perceive this as important may be less likely to complete the survey. In particular, some program directors with lower participation such as in MRI (n = 22) and nuclear medicine (n = 32) might not be as accurately represented as are those with higher response rates, such as in radiography (n = 193).
Based on a lack of faculty knowledge in regard to transgender issues, some respondents may have misinterpreted the survey questions, as acknowledged in the open comments. Some respondents admitted general disregard for the topic and might have therefore misinterpreted the objective meaning of some questions.
Conclusion
The results of this study suggest inclusion of curriculum related to imaging of the transgender patients may be lacking in MITS educational programs. The delivery of the curriculum varies, among program directors surveyed, by hours spent on transgender topics and teaching strategies used. Program directors recognized the need to include or improve their curriculum. Faculty education will play an important role in adding or revising curriculum related to medical imaging of transgender patients. It will likely begin with a review of accreditation requirements and identifying gaps in the curriculum. The survey revealed that program directors may be seeking guidance on how best to include these topics in the curriculum. Further research should address specific resources and methods for preparing faculty, in accredited educational programs, to teach topics related to the imaging of transgender patients.
Footnotes
Acknowledgements
The authors acknowledge Teresa Odle, BA, ELS, for her writing assistance with this manuscript. The assistance was funded by the Joseph C. Anderson, MD, and Darlene Anderson Distinguished Professorship of Imaging Sciences.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
