Abstract
Objective:
The aim of this study is to determine whether a one-hour image-rich didactic lecture given to sonographers can successfully teach them the TI-RADS (Thyroid Imaging, Reporting and Data System) lexicon, to improve their recognition of malignant thyroid nodules.
Methods:
A one-hour image-rich didactic lecture on TI-RADS was designed that encompassed the diagnostic criteria for thyroid malignancy and technical tips to better demonstrate thyroid nodules. A lecture was presented to 34 sonographers across multiple sites. The study examined the effects of the lecture by comparing the results of a pretest, an immediate posttest, and a two-week delayed posttest.
Results:
All 34 sonographers participated in the lecture intervention and each assessment. The prelecture assessment scores ranged from 13% to 73% with an average of 46%. Immediately after the lecture, the assessment scores ranged from 27% to 100%, with an average of 77%. Two weeks after the lectures, scores ranged from 27% to 93%, with an average of 70%. Compared to the pretest, there was a statistically significant increase in average scores immediately after and two weeks after the lecture.
Conclusion:
It is critically importance to have a reliable, noninvasive method to identify thyroid nodules that have a greater chance of malignancy. A didactic lecture could successfully teach, result in knowledge retention, and increase sonographers’ confidence in the TI-RADS lexicon.
Thyroid nodules are a very frequent finding on a sonogram, the most appropriate and widely used initial imaging study for suspected thyroid pathology. The reported prevalence of thyroid nodules in adults is at least 60% on sonography, in contrast to physical examination, which detects thyroid nodules in 5% to 10%.1,2 Most of those nodules are incidentally discovered on sonography and, when sampled with fine-needle aspiration biopsy, are benign. 3 In addition, many malignant nodules are clinically indolent. In South Korea, a screening thyroid sonography program resulted in an increase in the incidence of papillary cancer in their population, yet mortality remained very low.4,5 Similar results from the United States have led some to call the thyroid cancer detection not an epidemic of disease but rather one of diagnosis. 6 Thus, many malignant thyroid nodules are clinically quiescent and prone to overdiagnosis. These factors result in a large number of unnecessary thyroid biopsies, which increases medical costs and patient anxiety. There is even a clinical trend for active surveillance in low-risk thyroid cancer.7,8 Hence, most thyroid nodules do not require fine-needle aspiration or biopsy.6,9
Frequently, a patient is encountered with a multinodular gland, and performing biopsies of multiple thyroid nodules is time-consuming, decreases departmental throughput, and increases patient anxiety. 8 The question often arises as to whether and which nodules need follow-up or biopsy. Therefore, there is a need for a system to more accurately classify thyroid nodules as to their benign or malignant characteristics. The goal of standardizing report terminology is to guide management and reduce the large number of unnecessary biopsies. Several professional societies have tackled the question of which nodules have a high likelihood of malignancy and warrant biopsy. In 2015, the American College of Radiology published a white paper to standardize terminology for sonographic reporting of incidental thyroid nodules. 1 This system was termed TI-RADS (Thyroid Imaging, Reporting and Data System) and was modeled on BIRADS (Breast Imaging-Reporting and Data System). More recently, an additional article published methodology for risk stratification of thyroid nodules to identify the most clinically significant nodules to reduce the number of biopsies performed on benign nodules. 8 TI-RADS attempts to address this conundrum by stratifying thyroid nodules by their sonographic appearance and size. The goal of this system is to decrease the number of benign biopsies while biopsying those nodules that are malignant in appearance.
TI-RADS categorizes thyroid nodules as benign, minimally suspicious, moderately suspicious, or highly suspicious for malignancy based on five imaging features: composition, echogenicity, shape, margin, and hyperechoic foci. For composition, nodules can be classified as cystic (least suspicious), spongiform, mixed cystic and solid or almost completely solid (most suspicious). For echogenicity, nodules can be classified as anechoic (least suspicious), hyperechoic, or isoechoic, hypoechoic, or very hypoechoic (most suspicious). For shape, the lesion can be wider-than-tall (not suspicious) or taller-than-wide (suspicious). Margin may be smooth (least suspicious), ill-defined, lobulated or irregular, or extra-thyroidal extension (most suspicious). Hyperechoic foci may be classified as none or large comet-tails (least suspicious), macrocalcifications, or rim calcifications or punctate hyperechoic foci (most suspicious). Each of these features is assigned a point value that, when summated, provides a grade for each nodule. The grade and size of a nodule determine the management recommendation (e.g., surveillance, fine-needle aspiration [FNA], no follow-up necessary). The recommendations are based on the higher risk of thyroid cancer with a higher TI-RADS grade. For example, TR1 is associated with cancer risk of 0.3% and TR5 with a risk of 35%. 7 The recommendation of the committee is that if multiple nodules are visualized, only the four highest-scoring nodules are reported. 8
Sonographers are generally the first members of the imaging team to examine the patient. They are tasked with selecting and capturing images of the four most suspicious thyroid nodules in the patient with a multinodular gland. 8 If TI-RADS is to become the standard for the evaluation and management of thyroid nodules, it is essential that the sonographers become knowledgeable about the imaging features that aid in differentiating benign from malignant nodules, as described in the TI-RADS lexicon. It is equally important for the sonographer to incorporate the technical recommendations described in the TI-RADS system to optimize image quality and standardize the way nodule measurements are obtained. The purpose of this study was to determine whether a one-hour image-rich didactic lecture given to sonographers can successfully teach the TI-RADS lexicon. The purpose was to improve sonographers’ recognition of malignant nodules, using these criteria.
Methods
The study population included sonographers with 5 to 25 years of experience working in inpatient and outpatient settings at five different sites at two neighboring medical centers that serve an inner-city, urban population. Five board-certified attending physicians (sonologists), with 10 to 40 years of experience, presented a one-hour didactic lecture of the TI-RADS lexicon to the sonographers in the form of a PowerPoint presentation at each site. The 36-slide presentation defined TI-RADS criteria for assessing thyroid nodules and included numerous relevant images. Multiple types of thyroid nodules with each of the five major characteristics (composition, echogenicity, shape, margin, and hyperechoic foci) were depicted, and technical tips were offered to enhance image quality. The lecture was highly interactive, with multiple opportunities for sonographers to provide comments and ask questions. Cognitive load was reduced by clarifying the aim of the lecture and its direct relevance to the sonographers’ day-to-day work, as well as creating PowerPoint slides with minimal verbiage, high-yield images, and imaging tips.
An image-rich 15-question multiple-choice examination was administered to the sonographers before the lecture (pretest), immediately after the lecture (immediate posttest), and two weeks postintervention (delayed posttest) (Figure 1). Each administration was supervised with a closed book format. The pretest and two posttests had the identical questions in a randomized order. A survey was given to the sonographers immediately following the two-week posttest to evaluate their opinion of the efficacy of this educational initiative and to self-assess their confidence applying TI-RADS in their future patients with thyroid nodules. Results of the quiz were given to the sonographers after the two-week posttest.
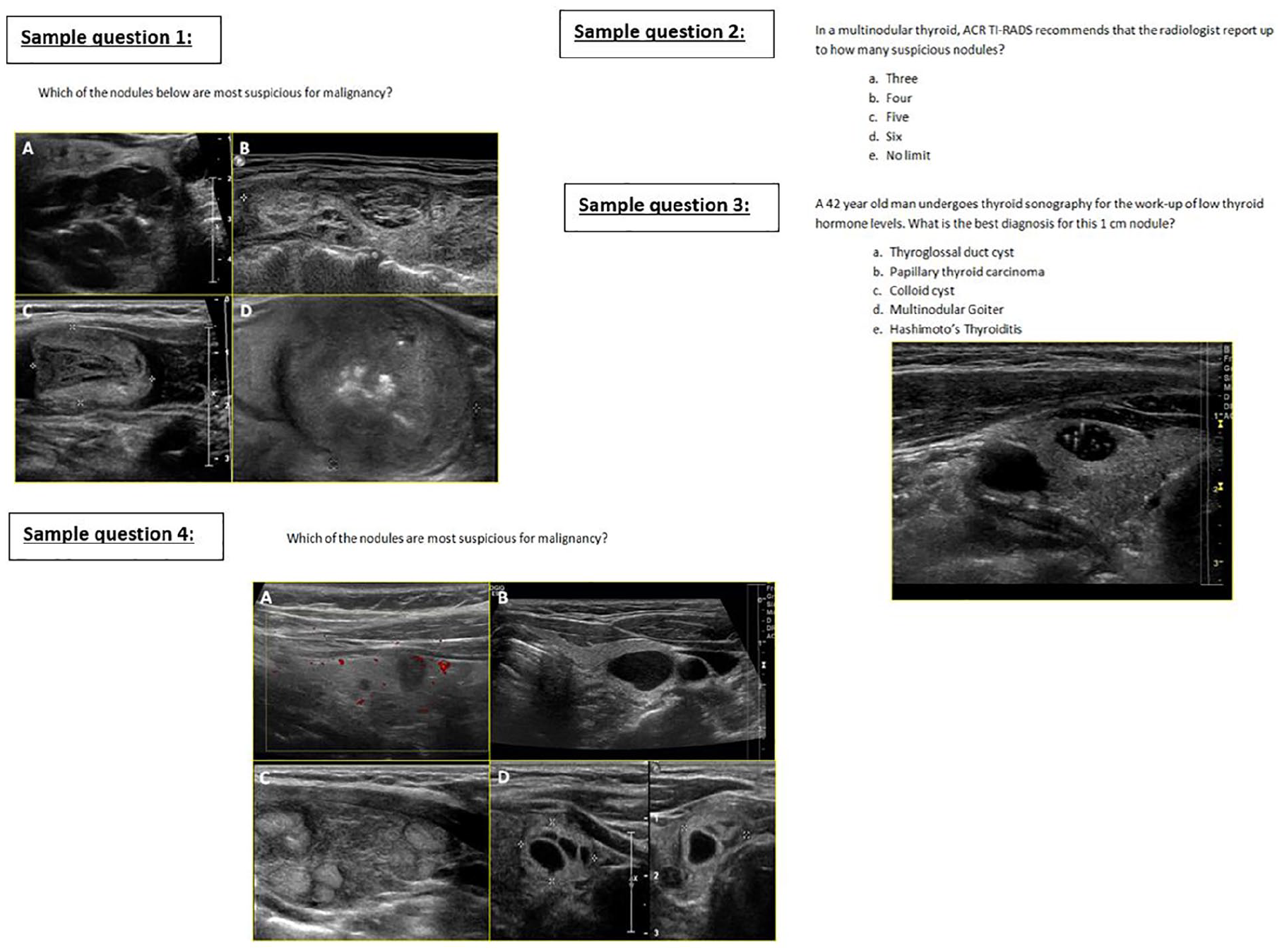
Four representative sample questions from the image-rich 15-question multiple-choice examination are shown above.
Statistical Analysis
Each sonographer in the study was assigned a unique identifying number, which preserved anonymity. Descrip-tive statistics are provided in terms of mean and standard deviation. The matched-pair t test was used to compare pretest scores to both immediate posttest and delayed posttest. Two-tailed P values ≤.5 were considered statistically significant.
Results
Thirty-four sonographers participated in the study. All 34 participated in the lecture intervention, and each took a pretest, immediate posttest, and two-week delayed posttest. The prelecture assessment scores ranged from 13% to 73% with an average of 46%. Immediately after the lecture, the assessment scores ranged from 27% to 100%, with an average of 77%. Two weeks after the lectures, scores ranged from 27% to 93%, with an average of 70% (Figure 2a). Compared to the pretest, there was a statistically significant increase in average scores immediately after and two weeks after the lecture (P = .00001 and <.00001, respectively) (Figure 2b). At both the immediate and two-week delayed posttest, the sonographers learned and retained knowledge, as evidenced by gains in test scores on the 15-question multiple-choice tests.
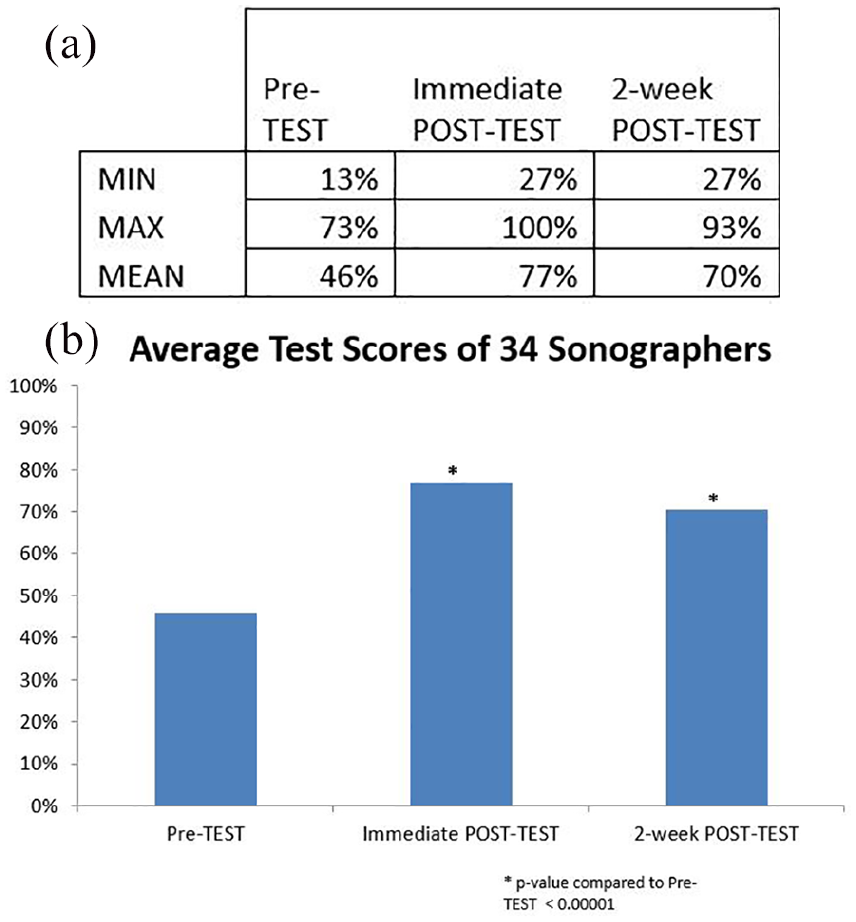
Of the 34 sonographers who participated in the lecture intervention, each took a pretest, immediate posttest, and two-week delayed posttest. Range and mean test scores are shown in (a) with average scores.
Pos intervention survey demonstrated that over 90% of participants agreed or strongly agreed that the lecture presented concepts in a clear and concise manner. As a result, they felt more confident identifying malignant nodules, as well as able to apply what they learned in the TI-RADS lecture. They also indicated that the postlecture quizzes were helpful in reinforcing the TI-RADS concepts (Figure 3).
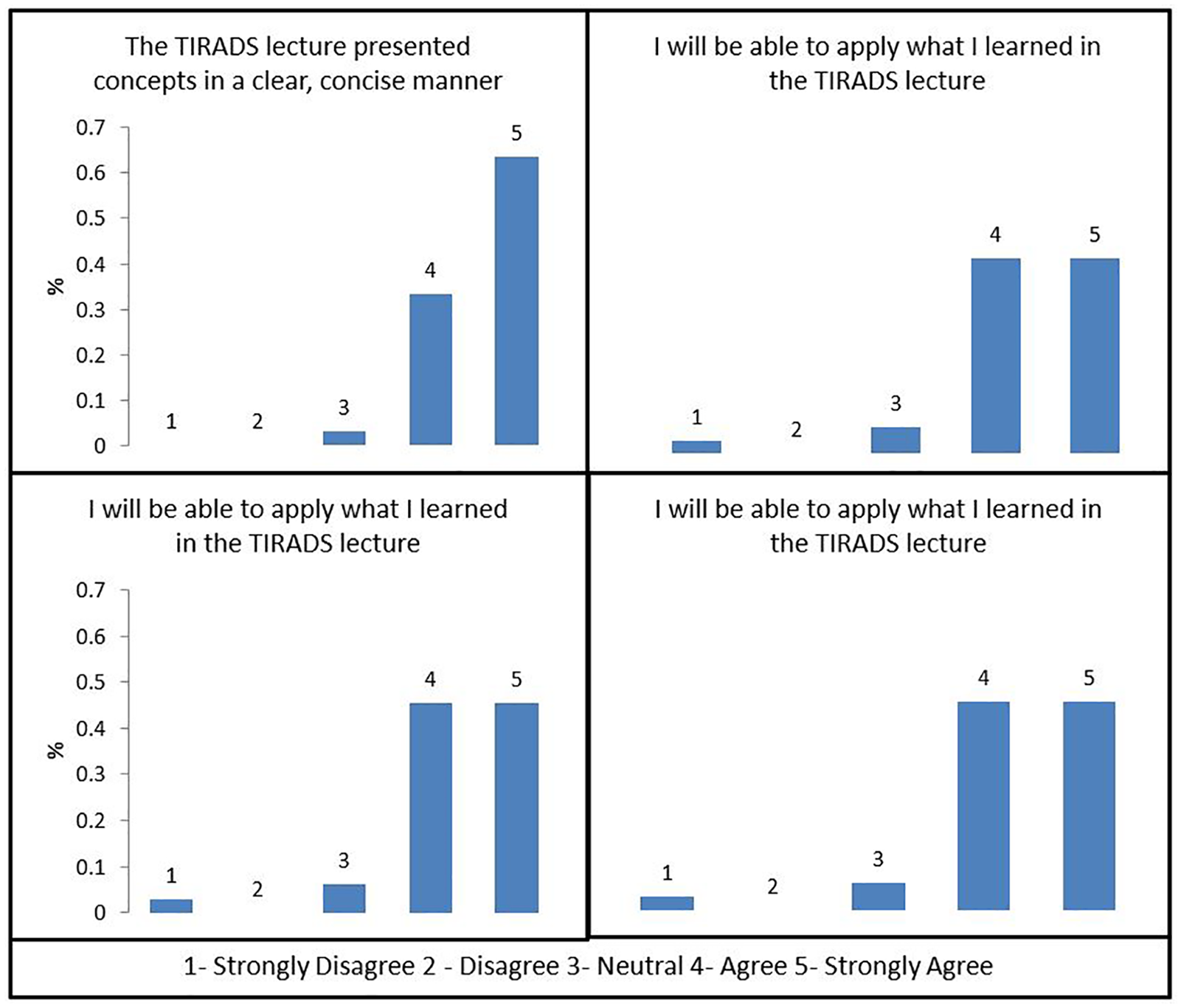
Postintervention survey demonstrated that over 90% of participants agreed or strongly agreed that the lecture presented concepts in a clear, concise manner, and they felt more confident identifying malignant nodules. They were able to apply what they learned in the TI-RADS (Thyroid Imaging, Reporting and Data System) lecture and that the postlecture quizzes were helpful reinforcing TI-RADS concepts.
Discussion
Sonographers are generally the first members of the imaging team to examine the patient undergoing a thyroid sonogram. The job of the sonographer is to select and capture images of the four most abnormal thyroid nodules for review. Therefore, it is essential that they be well versed in the salient imaging features involved in the TI-RADS lexicon. 8 Thus, if TI-RADS is to be adopted successfully, the sonographer must understand the TI-RADS criteria and technical recommendations.
A didactic lecture is often the first and easiest way to familiarize a large group of individuals with new information in a timely fashion. A recent study demonstrated the effectiveness of teaching novice medical students the basics of sonography knowledge and skills using a live lecture format prior to hands-on training. 10 Similarly, the current study results showed a significant increase in test scores when comparing the pretest scores to both the immediate and delayed posttest scores after a didactic lecture was presented. Moreover, the results of the Likert surveys demonstrate that the vast majority of sonographers felt that the intervention increased their knowledge in recognizing malignant-appearing thyroid nodules and that they would be able to apply their newfound knowledge in the clinical setting (Figure 3). This educational imitative shows that a didactic lecture can successfully result in knowledge retention and increases sonographers’ confidence in the TI-RADS lexicon. It would appear that this is the first study to demonstrate the efficacy of a didactic lecture in effectively educating sonographers to use the TI-RADS system. Future research to assess the efficacy of a didactic lecture in delivering this information as compared to more active educational strategies is planned.
One of the limitations of this analysis is that the questions on the pretest, immediate posttest, and delayed posttest were identical. This was intentionally done to create equivalent tests. Thus, there may been recall bias, as the question stems and responses were similar in nature. The correct answers were not given to the sonographers until after the delayed posttest. Another limitation is the heterogeneity of the study group due to different levels of experience of the many sonographers at various clinical sites. Also, the delayed posttest was administered only two weeks after the didactic lecture, which may overexaggerate the knowledge retention effect. Future studies are necessary to determine whether the effects of this educational initiative would result in long-term knowledge retention.
This reported experience demonstrates the use of a didactic lecture as an effective way to teach sonographers the TI-RADS lexicon for the purposes of implementation into clinical practice. The use of TI-RADS, to standardize characterization of thyroid nodules to guide clinical decision making, specifically if and when to perform follow-up and biopsy, cannot be effective without educated sonographers. Sonography is an inherently operator-dependent specialty, and with TI-RADS, it is the sonographers who decide which four nodules to characterize and document in each thyroid lobe. It is incumbent upon the radiologist to inform sonographers about new initiatives such as the TI-RADS lexicon in an effective manner. Although many thyroid nodules will not neatly fit into all of the TI-RADS categories, it is important that the sonographer know the basic concepts that distinguish between benign and malignant pathology, as well as technical tips for optimizing image quality. Adoption of TI-RADS will hopefully provide a more reliable noninvasive method to identify biologically aggressive thyroid nodules. Future research will attempt to assess how well sonographers are applying the knowledge acquired in a classroom setting to their daily practice. This will be particularly important as thyroid sonogram reports begin to reflect the TI-RADS risk stratification system.
Footnotes
Acknowledgements
We thank Dr. Kenny Ye for the review of statistical analysis.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
