Abstract
Background:
Transvaginal sonography (TVS) is considered a simple and generally accepted method for detecting uterine anomalies. With TVS, the uterus can be clearly visualized, but so far, the diagnostic accuracy of TVS varies across different studies. This retrospective study was devised to evaluate the accuracy of a sonographic diagnosis of endometrial polyps in a Ukrainian hospital.
Methods:
This was a single-center retrospective study of woman who underwent TVS and had hysteroscopy or dilation and curettage for endometrial pathology. A cohort of 156 women were included in this yearlong study. A comparative analysis was based on the preoperative diagnosis, according to TVS, compared with the postoperative histopathology results.
Results:
The overall sensitivity, specificity, positive predictive value, negative predictive value, and accuracy of TVS in diagnosing endometrial polyps were 69%, 51%, 73%, 46%, and 63%, respectively.
Conclusion:
This retrospective study provided data on the lack of accuracy for a sonographic diagnosis of endometrial polyps. This was based on 26% of women whose diagnosis was not confirmed by histology. A false-negative result occurred for 54% of women who had polyps that were not detected at the preoperative stage. These data raise the question of the feasibility of further invasive procedures based on a single TVS study.
An endometrial polyp is a focal proliferation of the endometrium, which consists of glandular tissue, stroma, and blood vessels. 1 Endometrial polyps are frequently found during routine preventive transvaginal sonography (TVS) in women without clinical symptoms (Figure 1). 2 Although most endometrial polyps are asymptomatic, for patients with symptoms, the most frequent manifestation is abnormal uterine bleeding.3,4
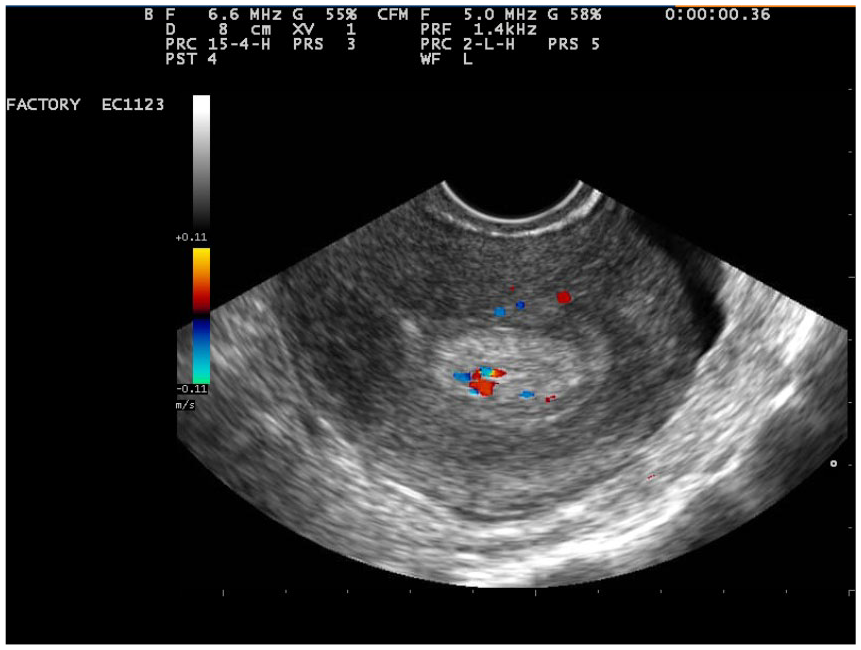
Transvaginal sonogram of an endometrial polyp.
The prevalence of endometrial polyps varies depending on the diagnostic method and population; it has been reported to be present in 12% to 14% of women. 5 As endometrial polyps are often asymptomatic, their true prevalence in the general population remains unknown. 6
Although endometrial polyps are usually benign, the risk of malignancy is still a possibility that should be considered. The American Association of Gynecologic Laparoscopists (AAGL) estimates that the incidence of malignant endometrial polyps ranges from 0% to 12.9%, depending on the subgroup of patients. 7
Despite extensive research, endometrial polyps remain a diagnostic and therapeutic problem. TVS is considered a simple and common method for detecting uterine anomalies.8–10 With the help of TVS, the uterus can be clearly visualized; therefore, the universal application of TVS has led to an increased detection of endometrial polyps in symptomatic and asymptomatic women. However, the diagnostic accuracy of TVS still varies across different studies, 11 and the need for routine polypectomy is still the subject of discussion.6,12–14
The present study was performed to assess the diagnostic accuracy of TVS for detecting endometrial polyps. This study had the potential to determine the proper role for sonography in the diagnosis of endometrial polyps and the feasibility of further invasive procedures based on the diagnostic result.
Methods
This was a single-center retrospective study of woman who underwent TVS from January 2017 to January 2018 at a Ukrainian hospital. This cohort of patients also underwent hysteroscopy or dilation and curettage for their endometrial pathology. According to the standards that exist in Ukraine, the preoperative endometrial diagnosis was based solely on the results of TVS.
All women who met the inclusion criteria during the one-year period constituted the study’s participant cohort. A retrospective analysis of age, parity, pre- and postoperative diagnosis, results of TVS, hysteroscopy, and biopsy was performed. Sonographic assessment was performed by certified sonologists from various medical units. A TVS was completed on all patients during the proliferative phase of the menstrual cycle. A histopathology examination was completed in the pathoanatomical departments of either a regional hospital or university hospital (at the request of the patient) by qualified pathologists. The ethical commission of the hospital that sponsored the research approved the study protocol.
The evaluation criterion was based on the sensitivity and specificity of TVS for the diagnosis of an endometrial polyp. A comparative analysis of the preoperative diagnosis, according to TVS, was compared with the postoperative diagnosis from the corresponding histopathologic examination. The clinical standard for comparing the pre- and postoperative results was confirmed by the pathologist’s report. Cases with indeterminate histopathologic results were excluded from the study. The data were entered into a MS Excel spreadsheet, and means, sensitivity, specificity, positive and negative predictive values, positive and negative likelihood ratio tests, and diagnostic accuracy were calculated. A Fisher exact test was used to calculate the differences between categorical variables. An alpha level was set a priori at P < .05.
Results
A retrospective study of 266 cases was conducted, and 156 cases were selected to analyze the accuracy of diagnosis of endometrial pathology. A total of 110 patients who underwent invasive interventions due to submucous myomas or uterine intrauterine synechia and those who had no histopathological data that could serve as the comparison criteria were excluded.
A retrospective analysis showed that in 121 cases of 156 invasive interventions due to endometrial pathology, hysteroresectoscopy was conducted, and in 35 cases, dilation and curettage was performed.
According to the TVS results, the patients were divided into two groups before the procedure. The first group included 97 women with a preoperative diagnosis of endometrial polyps. The second group was composed of 59 women for whom an intrauterine intervention was performed due to alternate indications.
Demographic characteristics of the patients with respect to the presence of endometrial polyps are presented in the Table 1. Both patient groups were statistically similar in age, gravidity, and parity (Table 1).
Demographic Characteristics of Patients.
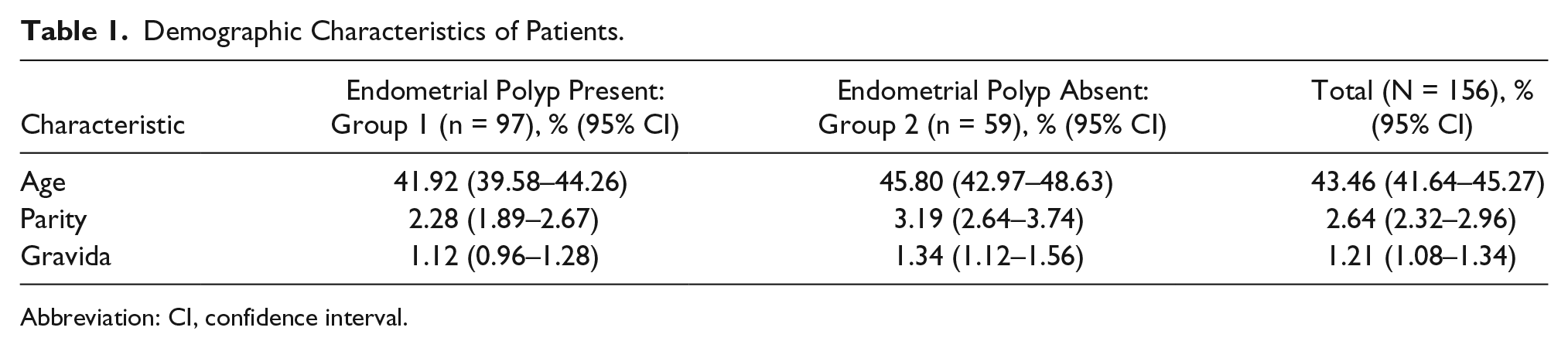
Abbreviation: CI, confidence interval.
In the first group of 97 women, an endometrial polyp was detected by TVS and the diagnosis was confirmed by histology in 71 women. The positive predictive value was 73.19% (95% confidence interval [CI], 63.07%–81.44%), and the false-positive value was 26.8%. In the second group of 59 women, the absence of an endometrial polyp was observed in 27 people, so negative prognostic value was 45.76% (95% CI, 54.73%–70.41%), and false-negative value was 54.23%. The sensitivity, specificity, positive likelihood ratio, negative likelihood ratio, and diagnostic accuracy of TVS for the diagnosis of endometrial polyp were 68.93% (95% CI, 59.06%–77.69%), 50.94% (95% CI, 36.84–63.94%), 1.41 (95% CI, 1.04–1.90), 0.61 (95% CI, 0.41–0.90) and 62.82% (95% CI, 54.73%–70.41%), respectively.
Discussion
TVS is considered a noninvasive diagnostic imaging procedure. It is relatively painless and can be performed both at the hospital and at an outpatient department. However, the accuracy of the TVS technique, according to the results presented, suggests a lack of reliability. This conclusion was based on the large number of questionable results reviewed, which did not completely eliminate or confirm the presence of an endometrial polyp. However, patients who have a TVS diagnosis of an endometrial polyp should undergo invasive treatment, so that the diagnostic accuracy can be definitely confirmed (Figure 2). However, this study did indicate that in more than a quarter of cases (26.8%), the histopathologic report, which is the gold standard, did not confirm the diagnosis of an endometrial polyp. This would suggest that there is a capacity for these women to choose another, possibly noninvasive treatment method. This study also confirms the need to develop and improve methods for diagnosing endometrial polyp.
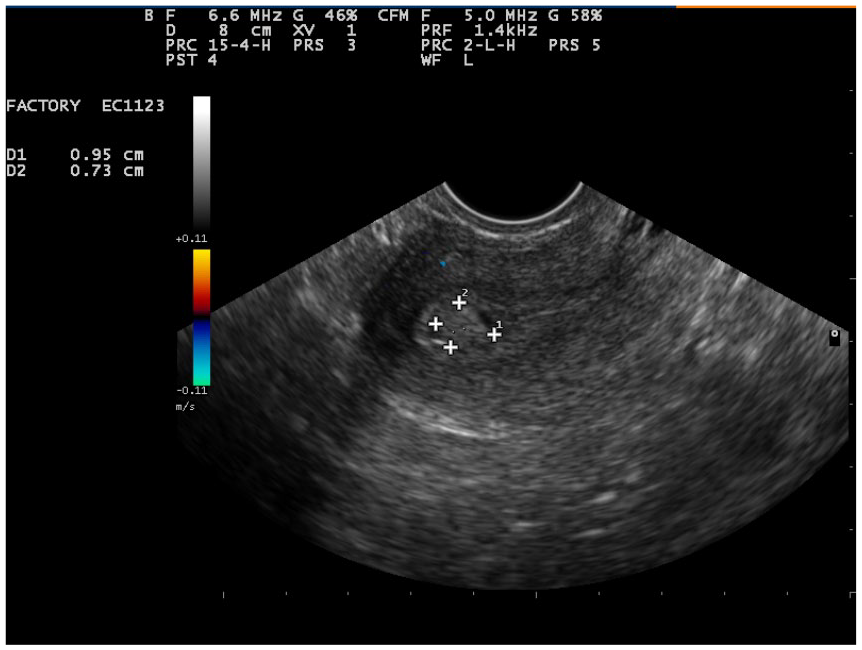
Transvaginal sonogram of an endometrial polyp.
This retrospective study of 156 patients with suspected endometrial pathology, diagnosed with TVS, demonstrated the insufficient accuracy of the TVS diagnosis of endometrial polyps. Given that 26% of the cohort’s diagnoses were not confirmed histologically, there was a false-positive result. In addition, 54% of these participants did not have an endometrial polyp, which was detected at the preoperative stage, so a false-negative result was noted. These data raise the question of the feasibility of further invasive procedures on the basis of a single TVS examination.
Data on the sensitivity, specificity, positive predictive value, and negative predictive value of TVS in the diagnosis of endometrial polyps are listed in Table 2.
Comparison of Sensitivity, Specificity, Positive Predictive Value (PPV), and Negative Predictive Value (NPV) of Transvaginal Sonography in the Diagnosis of Endometrial Polyps.
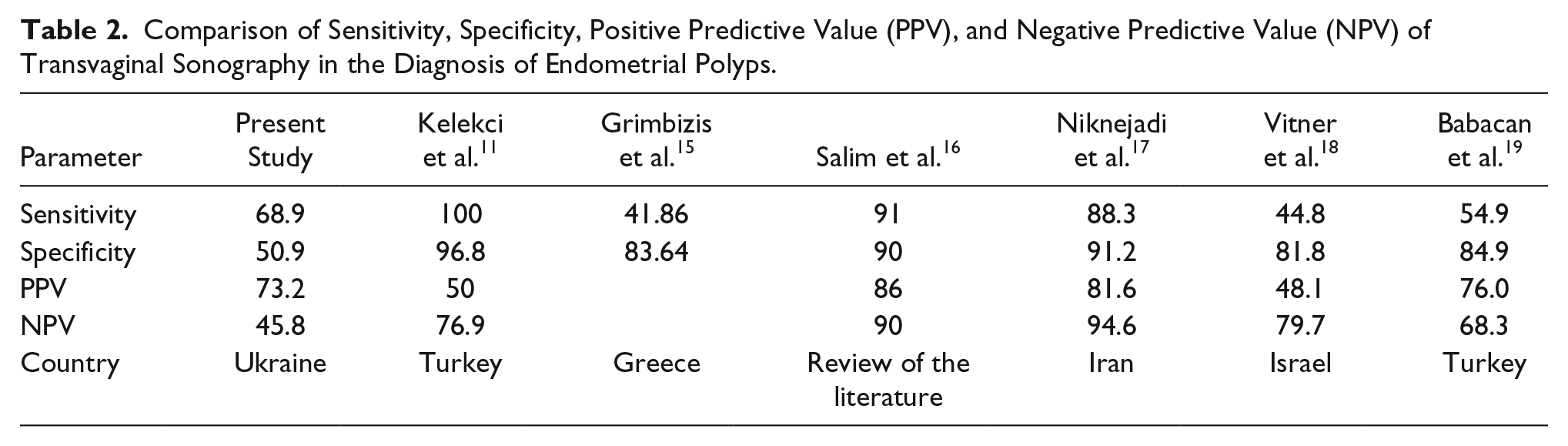
The sensitivity of the TVS method in the present study was comparable with the data published by other investigators.11,15–19 With recent improvement in technology, we expect sensitivity of TVS to be increased. However, it is important to note that in the past, when the quality and type of ultrasound equipment were inferior, the sensitivity of the method appeared to be higher. As an example, a Turkish publication indicated a decrease in the sensitivity of TVS from 2005 to 2014 by 45.1% and specificity by 11.9%.11,19
The specificity of the technique, which reflects the correctness of identifying a negative result (in this study, the absence of an endometrial polyp), was low, and it may be 1.7 times lower than in other reported studies. This is concerning and would indicate the need for further research to avoid having patients without an endometrial polyp being improperly classified in this way.
These data are confirmed by the negative and positive prognostic value of the TVS technique, which by its positive value was comparable to other studies and the sensitivity of the present study. The negative prognostic study was low, however, consistent with the specificity index, which confirms the insufficiency of the TVS technique for accurate diagnosis. It also has the potential to exclude patients from an interventional hysteroscopic examination.
Saline contrast sonohysterography (SCSH) is an alternative sonographic method in which the uterine cavity is distended with saline and allows the radiologist to distinguish focal from diffuse pathological conditions of the endometrium. 20 SCSH is an inexpensive, painless TVS enhancement that obviates the need for diagnostic hysteroscopy in complicated patient cases. 21 SCSH could potentially be used as a diagnostic method to stratify women with endometrial polyps for further diagnostic workup and treatment. 22 When combining TVS with saline in the endometrial cavity, diagnostic accuracy is significantly increased. 21 Іn the study by Aslam et al., 19 when comparing just TVS versus sonohysterogram in detecting endometrial polyps, there was a 92.9% sensitivity and 89.7% specificity, compared to only a 71.4% sensitivity and 67.7% specificity using only TVS. 23 SCHS could enhance the diagnostic accuracy of TVS in the assessment of endometrial polyps.
Conclusion
The main concern for clinicians and patients considering the diagnosis of an endometrial polyp, detected on TVS, is the accuracy of the imaging result. The clinician and patient are concerned with whether the likelihood that an endometrial polyp really exists and whether surgery is needed. The current study provides a cohort level of evidence that would indicate a rather less than accurate method for diagnosing endometrial polyps for patients in this Ukrainian hospital. This cohort study would suggest that there might be a need to provide patients with an array of diagnostic options so that an informed decision can be reached. It would be important for the clinician and the patient to have additional diagnostic information as to whether to undergo surgical hysteroscopy and not based solely on the results of a TVS. More diagnostic evidence is needed to determine the necessity for adding SCSH before hysteroscopy.
Footnotes
Acknowledgements
We thank Nataly Tovstolytkina for her friendly help with polyp TVS images.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study protocol was approved by the ethical commission of the maternity hospital.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Data Availability Statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to restrictions (their containing information that could compromise the privacy of research participants).
