Abstract
Pediatric pain remains frequently under-recognized and inadequately managed in emergency departments (EDs), particularly in low- and middle-income countries (LMICs), leading to significant physical and psychological harm. This narrative review synthesizes current evidence on pediatric pain management in LMIC emergency settings, highlighting both established practices and emerging innovations. Established approaches include pharmacologic interventions such as acetaminophen, NSAIDs, and opioids and cost-effective non-pharmacologic methods like distraction, guided imagery, and parental involvement. Despite their demonstrated benefits, implementation in LMICs is hindered by limited provider training, restricted access to essential analgesics, and cultural misconceptions about childhood pain. Emerging innovations involve task-shifting models to expand workforce capacity, digital and AI pain assessment tools, and context-adapted community interventions. Improving pediatric pain care in LMICs demands a multifaceted strategy integrating culturally adapted assessment tools, equitable access to analgesics, scalable non-pharmacologic interventions, and sustainable workforce development supported by technology-driven solutions.
Keywords
Introduction
Pain is a prevalent and distressing symptom among children presenting to emergency departments worldwide, serving as an indicator of potential physiological and psychological sequelae. 1 Studies indicate a high prevalence of pain in pediatric ED populations, with estimates ranging from 55% to 75% of patients experiencing moderate to severe pain.2,3 A persistent concern is the documented discrepancy between child or parent-reported pain intensity and healthcare provider assessments, which often leads to underestimation and undertreatment.4,5 Effective pediatric pain management is crucial not only for immediate relief but also to mitigate long-term risks, including the development of chronic pain patterns and procedural anxiety. 6
Accurate assessment is foundational, utilizing tools ranging from self-report scales like the Visual Analog Scale (VAS) to observer-based instruments like the FLACC (Face, Legs, Activity, Cry, Consolability) scale for non-verbal or younger children. 7 Management employs a multimodal approach, integrating pharmacologic and non-pharmacologic strategies. While high-resource settings utilize a broad analgesic arsenal including intranasal fentanyl and opioids, access in LMICs is frequently constrained. 8
Despite global advancements, profound disparities persist in low-resource emergency settings. Challenges include critical shortages of essential medicines, a lack of trained healthcare professionals, inadequate pain assessment protocols, and deeply rooted cultural beliefs that minimize childhood pain expression.9,10 Furthermore, robust evidence on the efficacy, safety, and feasibility of pain management interventions specifically within LMIC contexts remains scarce. 11
This narrative review aims to synthesize the current understanding of pediatric pain management with a dedicated focus on low-resource emergency settings. Its unique contribution lies in its specific synthesis for LMIC EDs, critically examining the intersection of 2 pivotal, yet underexplored, solutions: (1) the potential of AI-driven and digital health innovations for assessment and management, and (2) the scalability of task-shifting and training models to bridge the human resource gap. By integrating evidence on barriers, established practices, and these emerging innovations, this review provides a comprehensive framework for advancing equitable pediatric pain care.
Methods
This state-of-the-art narrative review was conducted to summarize and critically appraise current evidence on pediatric pain management in low- and middle-income country (LMIC) emergency settings. The methodology was designed in accordance with guidance for developing rigorous and practical narrative reviews. 12
Epidemiology and Burden of Untreated Pediatric Pain in LMICs
Acute pain is a ubiquitous presentation in pediatric emergency settings globally. Multicenter studies report high prevalence rates; for example, a study in Spain found 53.1% of children in the ED experienced pain, with abdominal and limb pain being most frequent. 13 In pre-hospital settings, the vulnerability is pronounced: an Irish study found 41.4% of children transported by ambulance were in pain, yet only 26% received pre-hospital analgesics, highlighting a critical care gap. 14
A consistent and troubling theme across settings is the discrepancy between clinician and patient/parent pain assessments. Healthcare professionals often underestimate severity, directly contributing to inadequate management and negative treatment experiences. 15 This assessment failure is the first step in a cascade of negative outcomes.
Inadequate pediatric pain management inflicts significant harm. Beyond immediate suffering, it elevates parental stress and increases the risk of distress and heightened pain perception during future medical procedures, particularly in young children. 16 Poorly managed acute pain can impair basic functions; a post-tonsillectomy study noted 75% of children exhibited behavioral changes, with majority experiencing sleep and feeding difficulties due to pain. 17
Persistent systemic and cultural barriers perpetuate this burden. A survey revealed approximately one-third of physicians believed analgesics could mask symptoms in acute abdominal conditions, reflecting enduring misconceptions that impede effective pain relief. 18 This underscores that the challenge is not solely one of resource availability, but also of knowledge, attitude, and systemic protocol.
Barriers to Accurate Pain Assessment and Intervention in LMIC Settings
Effective pain management is predicated on accurate assessment, which faces multifaceted barriers in LMICs stemming from cultural, professional, and systemic factors.
Pharmacologic Pain Management in Pediatric LMIC Emergency Settings
Pharmacologic management in LMIC EDs is constrained by a nexus of financial limitations, logistical inefficiencies, and regulatory barriers, creating a landscape of inequitable access and suboptimal use. 24
Accessibility of Pharmacologic Agents
Essential analgesics, particularly opioids, are often unavailable due to strict regulatory controls stemming from concerns about misuse and diversion. Morphine, the gold standard for severe pain, is frequently underutilized due to these restrictions, lack of prescriber training, and bureaucratic procurement hurdles. 25 While acetaminophen and NSAIDs are more widely available, they are insufficient for moderate-to-severe pain. 26
Fragile supply chains and poor infrastructure lead to frequent stock-outs, especially in rural facilities. Disparities are stark between urban and rural access, with even basic analgesics sometimes lacking in remote areas. 27 A critical issue is the paucity of pediatric-appropriate formulations (eg, liquid suspensions), forcing healthcare workers to manipulate adult dosages, which increases the risk of dosing errors. 28
Efficacy, Safety, and Practice Gaps
A pervasive problem is
Alternative Routes of Administration
When intravenous access is difficult, alternative routes are vital.
Abbreviations: IV, intravenous; IN, intranasal; IM, intramuscular; GI, gastrointestinal.
The evidence base for pharmacologic interventions in LMICs is notably weaker than in high-income countries, relying heavily on observational data and extrapolation. This underscores an urgent need for context-specific clinical trials to establish robust, feasible guidelines for LMIC emergency settings.
Non-Pharmacologic Pain Management Strategies in LMICs
Non-pharmacologic interventions are indispensable in LMIC EDs. They are typically low-cost, scalable, and can be used synergistically with pharmacologic methods to improve overall comfort and outcomes. 37
Family-Centered and Community-Based Approaches
Integrating families is a powerful, no-cost strategy. Parental presence, soothing talk, and holding provide emotional security, reducing a child’s fear.
43
Community-based interventions can bridge cultural gaps by thoughtfully integrating evidence-based practices with accepted traditional healing methods. While some traditional practices offer psychological comfort, collaboration is needed to ensure safety and efficacy, promoting adherence through cultural resonance. 45 Key strategies are summarized in Table 2.
Abbreviation: TENS, transcutaneous electrical nerve stimulation.
Widespread implementation requires focused training for healthcare workers, community awareness campaigns, and the systematic inclusion of these techniques in clinical protocols to reduce over-reliance on scarce pharmaceuticals.
Task-Shifting and Training Initiatives for Pediatric Pain Management in LMICs
Task-shifting delegating specific clinical tasks to less-specialized health workers is a necessary strategy to address the critical shortage of pediatric pain specialists in LMICs, particularly in rural areas. 46
Digital and AI-Based Innovations for Pediatric Pain Assessment and Management
Digital and AI technologies offer promising tools to overcome traditional barriers to pain assessment and management, though their application in LMICs is nascent and faces specific challenges.
• • • • •
Therefore, while digital/AI tools hold immense potential, their implementation must be preceded by feasibility studies, cost-benefit analyses, and the development of supportive infrastructural and governance systems (Figure 1).
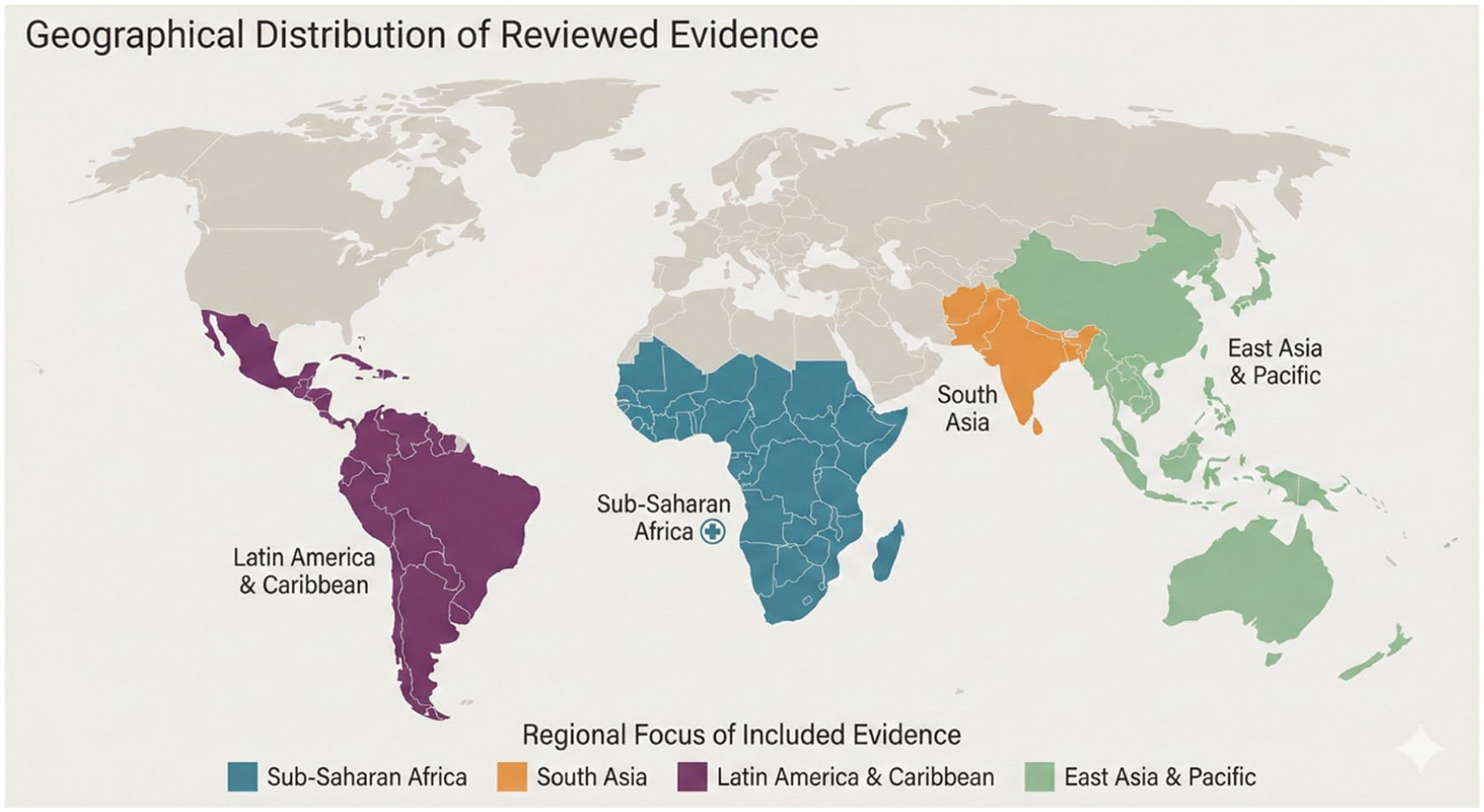
Geographical distribution of reviewed studies/interventions by LMIC region.
Future Directions and Policy Recommendations for Scaling Pediatric Pain Management in LMICs
Transforming pediatric pain care in LMICs requires coordinated action across clinical practice, health systems, and policy. The conceptual framework in Figure 2 outlines this multi-level approach.

Conceptual framework for improving pediatric pain management in LMIC emergency settings.
Health Systems Strengthening
Workforce Development
Research and Innovation Priorities
Conduct multicenter pragmatic trials within LMICs to establish context-specific efficacy and safety data for pharmacologic and non-pharmacologic interventions.
Support the co-design and validation of culturally adapted pain tools and feasible digital/AI solutions with local stakeholders.
Investigate sustainable financing models and implementation strategies for scaling successful pilot programs.
Global and National Policy Action
Study Limitations
This narrative review has several limitations. Methodologically, the exclusion of non-English literature and reliance on primary databases (PubMed, Scopus, Google Scholar) may have omitted relevant studies published in local journals or gray literature. The narrative synthesis approach, while comprehensive, precludes quantitative meta-analysis and formal assessment of evidence strength.
Substantively, the available evidence base itself has gaps. There is a relative scarcity of high-quality randomized controlled trials conducted within LMIC emergency settings; much of the data is observational or extrapolated from high-income contexts. The reviewed literature on cutting-edge innovations like AI and VR predominantly stems from high-resource settings, limiting direct applicability to LMICs without further validation. Furthermore, significant heterogeneity exists across the vast spectrum of LMICs in terms of culture, health system structure, and resources, challenging the generalizability of any single recommendation. These limitations highlight the critical need for more context-specific, high-quality research in this field.
Conclusion
Pediatric pain in LMIC emergency departments is a pervasive, undertreated problem with profound consequences. Barriers are multifactorial, spanning drug shortages, workforce gaps, cultural misconceptions, and fragile systems. This review synthesizes a dual pathway forward.
Immediate, practical gains are achievable at the bedside: implementing routine pain assessment with adapted tools, empowering families, utilizing non-invasive analgesic routes (IN/IM), and deploying low-cost non-pharmacologic techniques like distraction and comfort positioning.
Sustained improvement, however, demands systemic commitment. This includes strengthening analgesic supply chains, expanding the workforce through supervised task-shifting with rigorous training, and explicitly integrating pediatric pain management into national emergency care policies and financing frameworks. Digital innovations offer promise but require ethical, locally validated, and feasible implementation strategies.
Ultimately, achieving equity in pediatric pain relief is a matter of justice. Providing effective pain management is not merely a clinical best practice but a fundamental human right of every child. Closing the gap between current reality and these imperative demands concerted global action, context-sensitive innovation, and unwavering political will to prioritize the relief of suffering for the most vulnerable.
Footnotes
Author Contributions
M. Alsabri is considered first author and the corresponding author. M. Alsabri proposed the project and contributed to the conception, formulation, and drafting of the article, and reviewed and revised the manuscript. M. Alaswad is also is considered first author. M. Alaswad also contributed to formulation, and drafting of the article, and reviewed and revised the manuscript. EA, ESM, MMA, SR, and OJO participated in writing and revising the final manuscript. All authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data synthesized in this review are from previously published studies, which are cited.


