Abstract
Just like the DIPSI Guidelines for GDM in India, we must have a rapid screening tool like POC-A1c, which gives an estimate of long-term hyperglycemia and helps early detection. Traditional gold standard methods may delay the diagnosis for an indefinite time, as we have seen in our observations that of those who did not opt for POC-A1c, about 34% did not turn up even after three months. We infer that random capillary blood glucose (with a history of meal timings) of more than 140 mg% using POC-A1c helps in instant diagnosis accuracy of about 93%, or exclusion and necessary action can be taken immediately compared to traditional gold standard methods.
It also saves time and is cost-effective as no preparation is required, transportation can be avoided, and it also removes the stress or burden of being positive immediately. We know the important role of POC-A1c in treatment intensification or deintensification in the management of known T2DM patients. We also know that POC-A1c is not recommended for the diagnosis of DM by ADA, but evidence suggests we can opt for RPG and POC-A1c to screen and confirm or exclude T2DM.
At the same time, we also recommend large-scale cross sectional studies to recommend POC-A1c as a tool for early screening and diagnosis and definitely reconfirmation is always possible and can be recommended.
Background
Type 2 diabetes mellitus (T2DM) is increasing globally, and delay in the diagnosis of T2DM is about 4–7 years following the onset of hyperglycemia. As per ADA 2023, about 22.9% diabetics are undiagnosed in the USA. 1 In India, 2019 estimates showed that 77 million individuals have diabetes in India, which is expected to rise to 134 million by 2045 and approximately 57% of these individuals remain undiagnosed. 2 So there is a need to have a rapid screening tool to diagnose T2DM earlier in high-risk and susceptible individuals.
Objective
The aim was to understand whether “POC-A1c” helps early diagnosis of diabetes.
Methods
Random high-risk persons (obese, first-degree relatives of people with T2DM, those having acanthosis nigricans, and attendants of patients of T2DM) were chosen and offered free capillary blood glucose, and 100 individuals whose random capillary blood glucose was more than 140 mg% were offered POC-A1c.
Results
Out of those 100 persons, 66 opted for POC-A1c and 34 refused any further testing; still they were advised fasting plasma glucose and glycated hemoglobin (A1c) tests.
All abnormal values were advised to be reconfirmed by traditional gold standard fasting plasma glucose FPG and A1c.
These persons were classified as follows as per ADA criteria:
Normal (A1c < 5.7) Prediabetic (A1c 5.7–6.4) Diabetic (A1c > 6.5)
The following were the results:
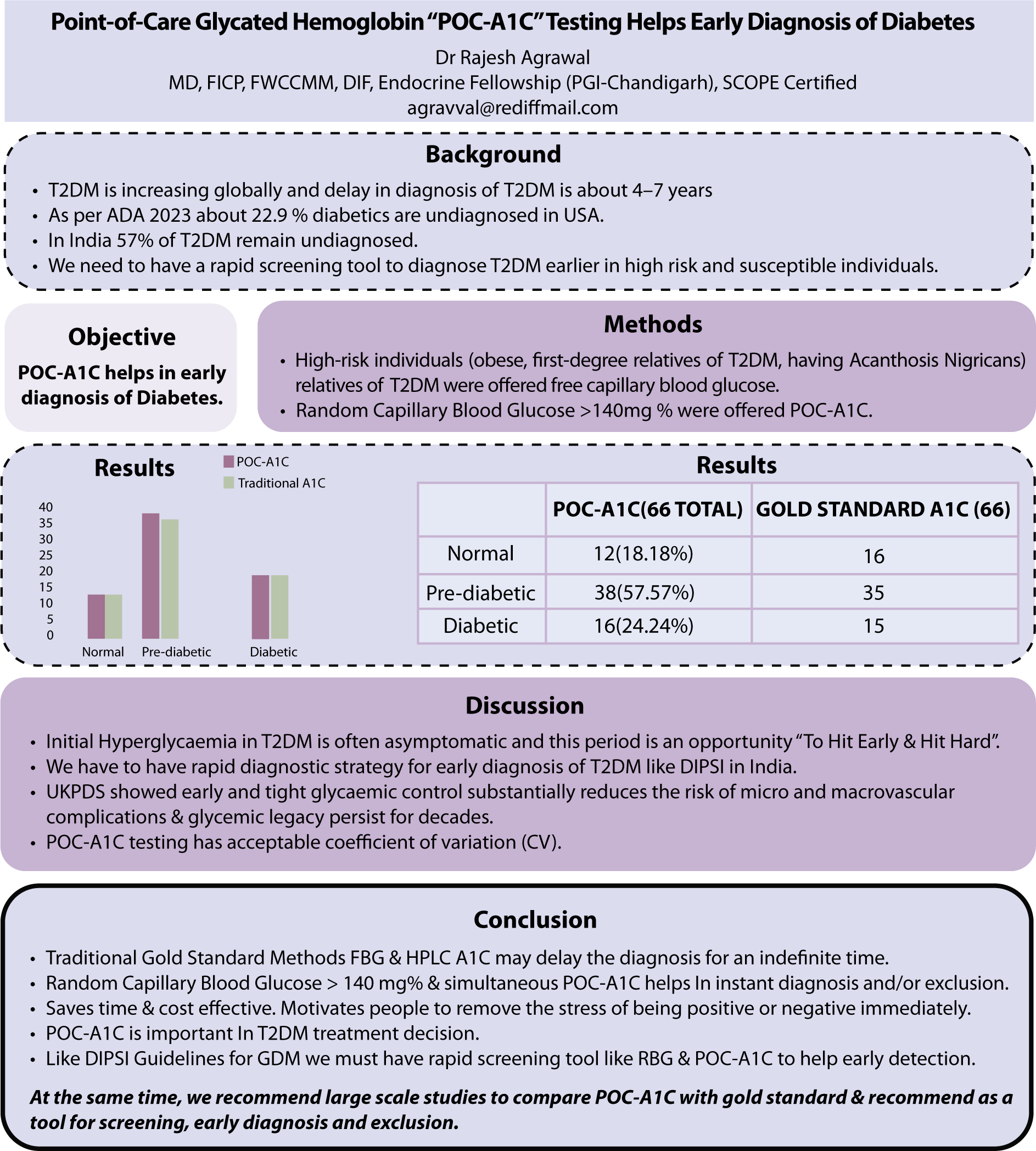
A total of 100 high-risk individuals 66% opted for POC-A1c 38/66 (57.57%) were prediabetic (A1c > 5.7 but < 6.4) 16/66 (24.24%) had A1c of 6.5 and above in the diabetic range 12 (18.18%) were in the normal range of A1c < 5.7.
So, a total of 54 persons out of 66 had abnormal values, and they were advised to get gold standard markers such as FPG and lab A1c.
Fifty-four individuals [prediabetic (38) plus diabetic (16)] got traditional gold standard FPG and lab A1C tests done, and results were in accordance with POC-A1c.
35/38 (92.1%) prediabetics by POC-A1c were found to have prediabetes.
15/16 (93.7%) diabetics by POC-A1c were found to have diabetes.
4 (7.4) were normal, which means a false positive.
Remaining high-risk candidates did not turn up even after three months, who did not opt for POP-A1C and five who opted but did not turn up.
Discussion
As per the ADA, in the USA, 38.4 million people have diabetes (11.6% of the US population); 29.7 million have been diagnosed and still 8.7 million people (22.8% of adults) are undiagnosed. 1
In India, 2019 estimates showed that 77 million individuals had diabetes, which is expected to rise to 134 million by 2045, and approximately 57% of these individuals remain undiagnosed, 2 which is quite a huge difference when compared to 22.8% in the USA.
So we have to have a different and rapid diagnostic strategy for early diagnosis of T2DM, just like the DIPSI criteria for the diagnosis of GDM (nonfasting 75 g post-glucose challenge) in India. 1
We are aware of the fact that the initial period of hyperglycemia in T2DM is often asymptomatic and it is an opportunity “to hit early and hit hard” to reverse or prevent the progression of T2DM and address cardiovascular and other risk factors. 3
In fact, up to 25% people already have diabetes-related micro- and/or macro-vascular complication at diagnosis.4-7
The United Kingdom Prospective Diabetes Study (UKPDS) demonstrated that early and tight glycemic control substantially reduces the risk of micro and macro-vascular complications, and myocardial infarctions and glycemic legacy persist for decades after diagnosis compared to those in whom initial tight control was not achieved. 8
Here, in our observational study, important points to be remembered are that we have chosen high-risk individuals on the basis of anthropological measures and random capillary blood glucose (RCBG) of more than 140 mg%, while most of the diagnostic criteria are on the basis of venous plasma glucose. Keeping this factor in mind, if we can screen and diagnose T2DM earlier, the time lag between the onset and diagnosis of DM will be reduced to minimum. In a study of 1,333 individuals randomly chosen from 63,305 individuals who had participated in an opportunistic screening program, RCBG was performed and the cutoff was 140 mg%; the conclusion was that Asian Indians with RCBG > 110 mg/dl at the time of screening can be recommended to undergo definitive testing to confirm or exclude the diagnosis of DM. 9
Tight glycemic control of DM is the need of the hour, and for that, we need to do frequent POC-A1c testing, which has an acceptable coefficient of variation (CV).
A total of 618 EDTA whole blood testing over a wide range of HbA1c values (4.0%–15% HbA1c) was performed, and 97.1% of the POC results and 94.5% of routine laboratory results fell within the target value of ±6% of the NGSP reference method results.
The total imprecision of the POC HbA1c results ranged from 0.74% to 2.13% CV across the measurement range compared to 0.81%–3.23% CV for the routine laboratory methods.
The accuracy and precision of the Afinion POC HbA1c method were comparable to those of the laboratory HbA1c methods supporting the FDA’s recent approval of the Afinion HbA1c Dx device for use in the diagnosis of diabetes. 10
Comprehensive care of patients with diabetes requires frequent A1c, and research indicates that the use of POC HbA1c testing can affect patients’ A1c results in the short term. This study illuminates perceptions of HCPs and patients regarding the impact of POC HbA1c testing on diabetes management.
The POC HbA1c test has many benefits in the clinical care of patients with diabetes including the following:
One-to-one feedback Proactive patient education Increased collaboration between patients and providers Improved patient adherence
However, logistical issues, such as the machine’s accuracy and cost factors, could be significant barriers to implementation. 11
Conclusion
Just like the DIPSI Guidelines for GDM in India, 12 we must have a rapid screening tool like POC-A1c, which gives an estimate of long-term hyperglycemia and helps early detection. Traditional gold standard methods may delay the diagnosis for an indefinite time, as we have seen in our observations that of those who did not opt for POC-A1c, about 34% did not turn up even after three months. We infer that random capillary blood glucose (with a history of meal timings) of more than 140 mg% and POC-A1c help in instant diagnosis and the accuracy is about 93%, or exclusion and necessary action can be taken immediately compared to traditional gold standard methods.
It also saves time and is cost-effective as no preparation is required, transportation is avoided, and it also removes the stress or burden of being positive immediately. We know the important role of POC-A1c in the treatment intensification or deintensification in the management of known T2DM patients. We also know that POC-A1c is not recommended for the diagnosis of DM by ADA, but evidence suggests we can go for RPG and POC-A1c to screen for and confirm or exclude T2DM. At the same time, we also recommend large-scale cross-sectional studies to recommend POC-A1c as a tool for early screening and diagnosis, and definitely reconfirmation is always possible and can be recommended.
Footnotes
Acknowledgements
We acknowledge with folded hands, the work done by all the researchers, authors whose references are cited here.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval and Informed Consent
No ethical approval or informed consent was required.
Funding
The author received no financial support for the research, authorship and/or publication of this article.
