Abstract
Brown tumors, though rare, are significant manifestations of hyperparathyroidism, often presenting with multifocal osteolytic lesions and occasionally leading to pathological fractures. This case report details the presentation and management of a 38-year-old male with multifocal brown tumors, including a right tibial fracture, and provides a comprehensive literature review. The patient exhibited multiple osteolytic lesions in the legs, thighs, and forearms, alongside elevated serum calcium and parathyroid hormone (PTH) levels. Management included conservative fracture treatment, surgical resection of the parathyroid adenoma, and postoperative rehabilitation. Follow-up revealed significant tibial fracture healing and reduction in the size of osteolytic lesions. This report underscores the importance of timely diagnosis and comprehensive management to prevent complications and improve outcomes in patients with multifocal brown tumors.
Plain Language Summary
Brown tumors are rare but important signs of a condition called hyperparathyroidism. They can cause multiple weak spots in the bones, sometimes leading to fractures. This report discusses a 38-year-old man with several brown tumors and a fracture in his right leg, and reviews similar cases in medical literature. We examined the patient, took X-rays, conducted lab tests, and performed surgery. We also reviewed other cases from medical literature to understand more about brown tumors and how to treat them. The patient had multiple weak spots in his leg, thigh, and forearm bones, along with high levels of calcium and a hormone called parathyroid hormone (PTH) in his blood. Treatment involved managing the fracture without surgery, removing a growth on his parathyroid gland, and helping him recover post-surgery. Follow-up showed the leg fracture healing well and the weak bone spots getting smaller. Quickly identifying and treating brown tumors is essential to prevent complications and help patients get better. Proper management of hyperparathyroidism can lead to significant improvements in health.
Keywords
Introduction
Brown tumors are benign osteolytic lesions associated with hyperparathyroidism, particularly in primary and secondary cases. 1 Known as osteitis fibrosa cystica, they result from excessive osteoclastic activity and fibrous tissue proliferation due to elevated parathyroid hormone (PTH) levels. 2 While brown tumors can affect any bone, they predominantly involve the ribs, pelvis, and long bones of the limbs. 3 The prevalence of brown tumors in primary hyperparathyroidism cases is approximately 3%–5%, while secondary hyperparathyroidism cases have a prevalence of about 1.5%. 4 Multifocal brown tumors are exceptionally rare, occurring in fewer than 2% of cases. 5 Recognizing and appropriately managing these lesions is critical to prevent complications, such as pathological fractures, and to ensure optimal patient outcomes. This case report illustrates the clinical course of a patient with multifocal brown tumors and discusses the diagnostic and therapeutic challenges associated with this condition.
Case report
A 38-year-old male with a history of parathyroid adenoma and hyperparathyroidism presented with multiple osteolytic lesions in both legs, thighs, and forearms. He reported progressive pain and swelling over the past 2 years, which impaired ambulation. Recently, he sustained a right tibial fracture at a brown tumor site following a minor fall.
On physical examination, marked swelling and tenderness were observed over the right tibia, along with palpable masses in the thighs and forearms (Figure 1). Radiographs confirmed osteolytic lesions consistent with brown tumors and a fracture in the right tibia (Figures 2 and 3). Laboratory investigations revealed elevated serum calcium (11.5 mg/dL) and significantly increased PTH levels (220 pg/mL). While no apparent diagnostic challenges arose in this case, cases with nuanced biochemical profiles may require additional diagnostic steps due to similarities with other bone lesions.
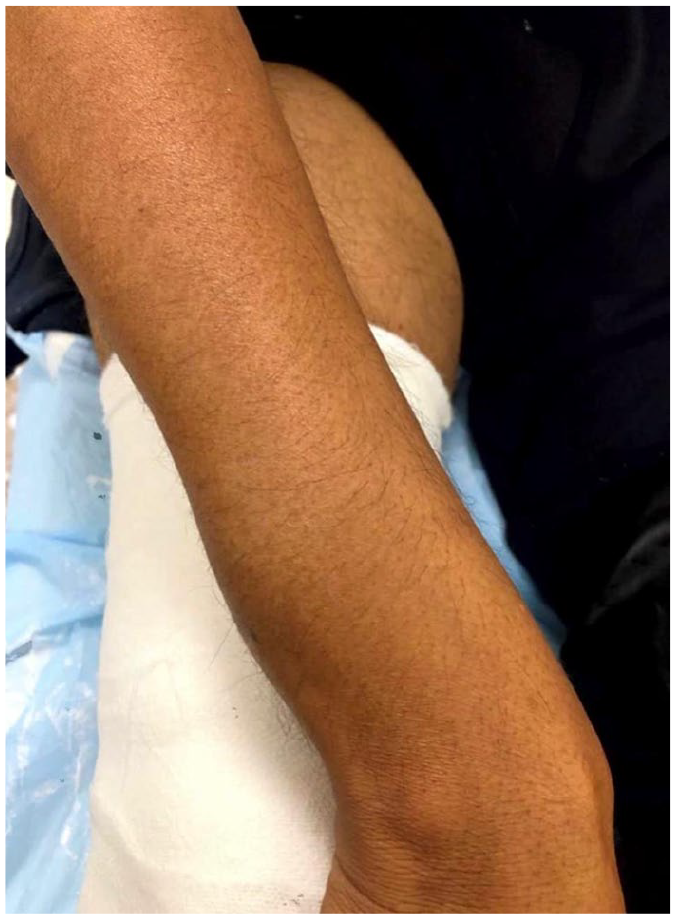
Clinical image of forearm showing swelling in the distal aspect.
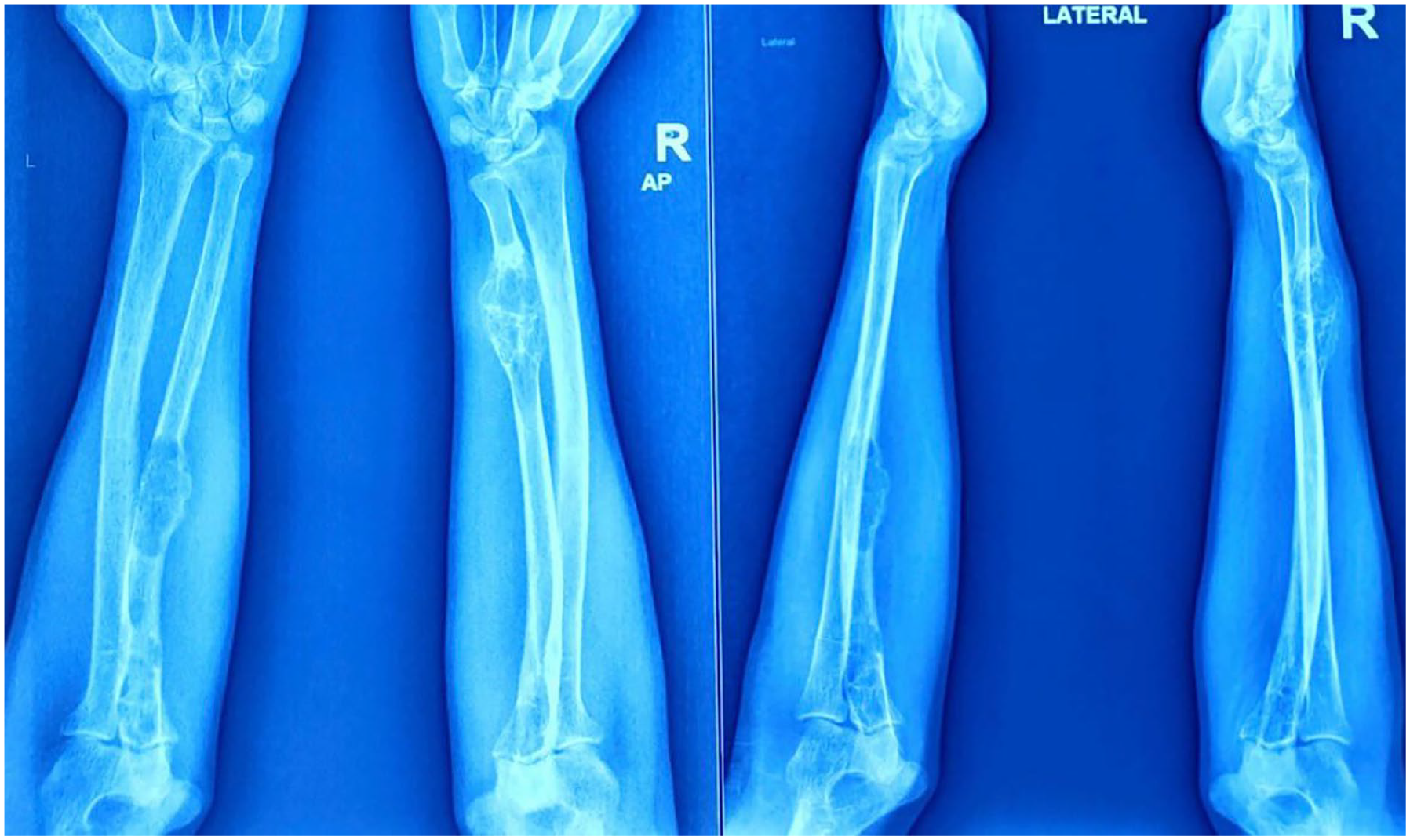
X-ray of both bone bilateral forearm (antero-posterior and lateral views) showing lytic and cystic.

X-ray of pelvis with both hips and thigh (antero-posterior views) showing lytic bony lesion in right.
A biopsy was performed, showing fibrous tissue proliferation that replaced normal bone marrow and trabeculae, accompanied by numerous osteoclast-like giant cells scattered within the fibrous stroma. In addition, hemosiderin deposition was noted due to the lesion’s hemorrhagic nature. These findings confirmed the presence of a brown tumor.
The tibial fracture was managed conservatively through immobilization in a plaster cast (Figure 4) for 6 weeks, with regular radiological monitoring to ensure alignment and fracture reduction. The patient was scheduled for parathyroid adenoma resection, which was performed successfully, addressing the hyperparathyroidism. Postoperatively, he received calcium supplements and bisphosphonates to manage transient hypocalcemia commonly observed post-parathyroidectomy.

Pathological fracture through brown’s tumor in right leg, being managed conservatively.
The patient was advised to avoid weight-bearing on the right leg until complete fracture healing was confirmed. Six months of follow-up included monitoring serum calcium and PTH levels, assessing tibial fracture healing, and evaluating the status of other brown tumors. The fracture healed in approximately 6 weeks (Figure 5), with physical therapy initiated to aid strength and mobility restoration. Six-month follow-up imaging indicated a fully healed tibial fracture (Figure 6) and a reduction in the size of some osteolytic lesions post-parathyroidectomy.

Six-week follow-up X-ray of right leg showing healed fracture.
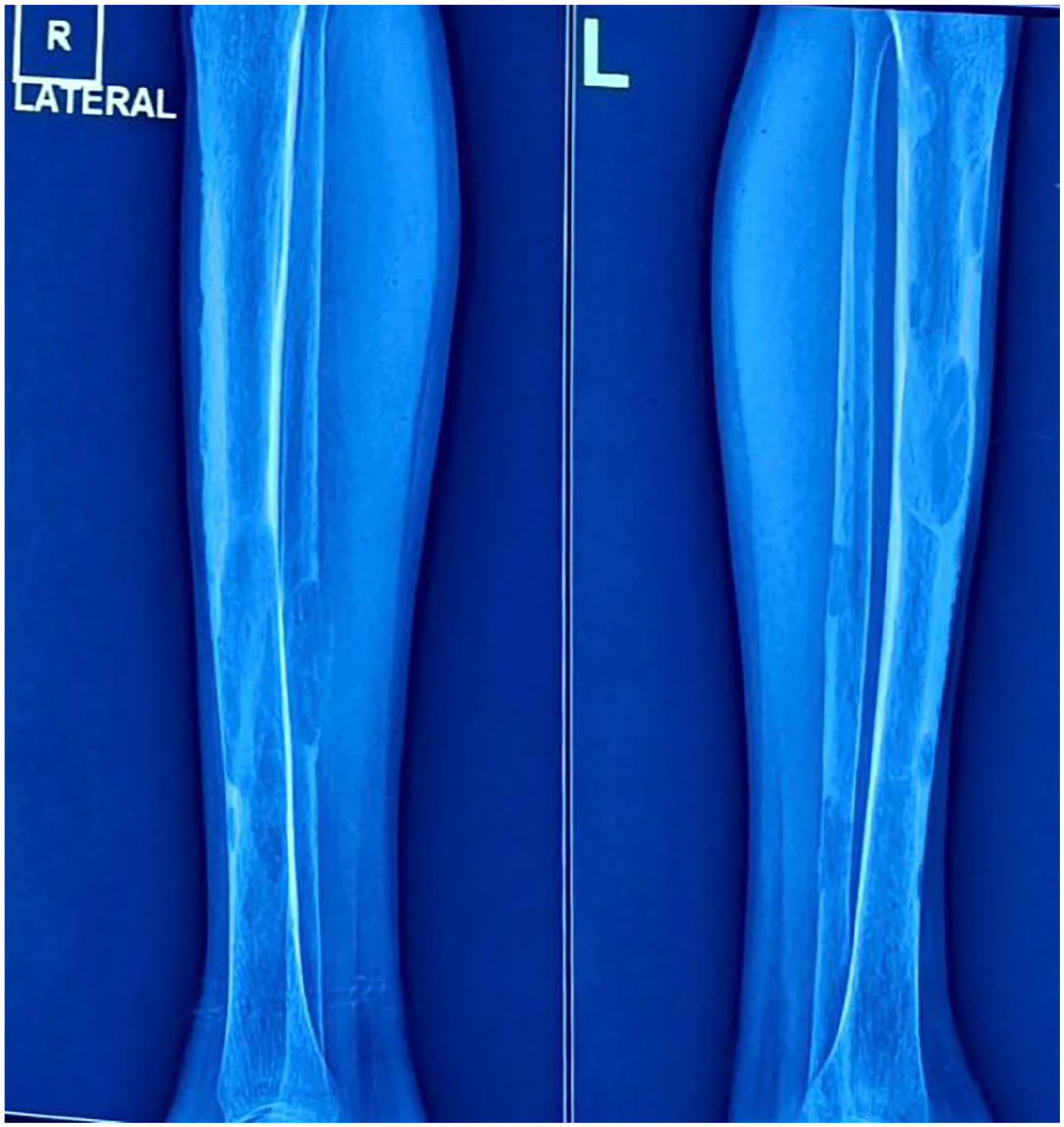
Six-month follow-up X-ray of both legs showing complete bony union of right leg fracture.
Discussion
Brown tumors, arising from excessive osteoclastic activity and fibrous tissue proliferation, are significant complications of hyperparathyroidism. 6 They frequently occur in primary hyperparathyroidism, often caused by parathyroid adenomas, and can also arise in secondary hyperparathyroidism, especially in patients with chronic kidney disease. 7
While the prevalence of brown tumors in primary hyperparathyroidism is around 3%–5%, secondary hyperparathyroidism cases see about 1.5% prevalence. 8 Multifocal brown tumors are rare and can present diagnostic challenges, as they may resemble metastatic bone disease or other osteolytic conditions. 9 In regions such as the United Kingdom, cases of brown tumors with atypical features would warrant multidisciplinary discussion with a bone sarcoma unit and cross-sectional imaging before biopsy to avoid potential misdiagnosis and unnecessary biopsy of malignant or metastatic bone lesions. 10 This approach highlights the importance of imaging in differentiating benign brown tumors from possible malignant or metastatic lesions.
Biochemical reference ranges are critical in the differential diagnosis of brown tumors. Elevated serum calcium levels (typically 8.5–10.2 mg/dL) and PTH levels (reference range: 10–65 pg/mL) are indicative of hyperparathyroidism. 11 When diagnostic uncertainty exists, reliance on biochemical markers alone may lead to a diagnostic error, particularly if a metastatic deposit or primary bone malignancy is suspected. Instead, cross-sectional imaging should be integrated into the assessment to better identify bone lesions suggestive of malignancy, thereby guiding subsequent biopsy decisions.
Current literature gaps and need for standardized management
The diagnostic approach to suspicious bone lesions associated with hyperparathyroidism lacks standardization, particularly in cases presenting with atypical biochemical and radiographic findings. This case reinforces the necessity of a comprehensive imaging-based diagnostic protocol for brown tumors, especially in cases where malignancy is a differential consideration. Future studies should focus on refining imaging protocols and evaluating multidisciplinary approaches to improve diagnostic accuracy and minimize unnecessary interventions. 12
Orthopedic management and follow-up
Treating brown tumors involves addressing hyperparathyroidism, typically through parathyroid adenoma resection in primary cases or calcium-lowering agents in secondary cases. 13 Orthopedic management focuses on stabilizing pathological fractures and curettage of lesions when needed. Bisphosphonates may support hypercalcemia management and reduce bone resorption. 14 Table 1 provides a comparative overview of various studies on multifocal brown tumors, summarizing lesion locations, management approaches, and patient outcomes.
Comparative analysis of studies on multifocal brown tumors.

This case illustrates the complexity in diagnosing and managing multifocal brown tumors in patients with hyperparathyroidism. Timely intervention is essential to prevent complications such as pathological fractures. Regular monitoring and comprehensive management of hyperparathyroidism can lead to significant improvement in patient outcomes. Further research is warranted to develop standardized diagnostic and therapeutic protocols, especially for atypical presentations of multifocal brown tumors. 15 Atypical presentations of brown tumors with normal biochemical ranges pose diagnostic challenges. Multidisciplinary consultation with a sarcoma service and imaging-based assessments are vital to differentiate these from malignant or metastatic lesions. As highlighted in the literature, collaboration with specialized units improves diagnostic accuracy and avoids unnecessary interventions. 16
Conclusion
This case report highlights the importance of early diagnosis and comprehensive management of multifocal brown tumors associated with hyperparathyroidism. Proper management of the underlying hyperparathyroidism is crucial to prevent complications and improve patient outcomes. Regular monitoring and follow-up are essential to ensure successful treatment and recovery. Further studies should aim to establish standardized guidelines to enhance the diagnostic and therapeutic approach for multifocal brown tumors.
